Abstract
Death literacy is an emerging concept within academic and social spheres, reflecting increasing recognition that people need to be better prepared for death and dying. The extent to which key features of death literacy are embedded in policies indicates how death and dying are framed and prioritised. Therefore, how the term ‘death literacy’ and its components have been adopted in UK governments’ policies required exploration. This study aimed to analyse post-2015 UK state-level (Westminster) and national (England, Northern Ireland, Scotland and Wales) policies to explore how death literacy is framed and described. A document analysis of policies was conducted using the READ approach, comprising reading materials, data extraction, data analysis and distilling the findings. UK and national governments’ and health services’ websites were searched. A thematic policy analysis was conducted, mapping content to Noonan et al. – features of death literacy (knowledge, skills, experiential learning and social action). Key findings were outlined in a narrative format. Initially, 11,063 records were screened, 59 documents were eligible for data extraction and a final 22 papers were selected. Findings included that death literacy was not explicitly referenced, despite key features of death literacy being present. These elements focused on knowledge and skills relating to death and dying, including publics’, caregivers’ and professionals’ understanding of end-of-life processes, predominantly relating to the skills of healthcare professionals. The policies also incorporated social action through community engagement and support. Elements of experiential learning, including coproduction of health services, were only referred to minimally. Despite no explicit reference to death literacy, key features were evident within UK policies, which focused on knowledge and skills relating to death and dying through palliative and end-of-life care processes. Future policies should explicitly outline a consolidated approach to death literacy, with the aim of improving experiences and preparedness relating to death, dying and end-of-life. These should embed strategies to implement multi-level, cross-departmental, and new public health approaches that addresses systemic inequalities, and to enhance experiential and socially focused initiatives.
Plain language summary
Why was the study done? Death literacy involves key features including knowledge, skills, social action and learning through experience relating to death, dying and end-of-life. As populations are increasingly ageing, there is a need to be better prepared for death and dying. How key features of death literacy are described in policies reflect how death and dying are prioritised by governments. Therefore, it was important to find out how ‘death literacy’ is described and how its key features have been used in UK governments’ policies. What did the researchers do? Researchers studied UK (Westminster) and national (England, Northern Ireland, Scotland and Wales) policies written after 2015. They looked for how features of death literacy are described. The results are described using the four main features as key themes. What did the researchers find? There were an initial 11063 policy records found on UK nations’ government and NHS websites. After examination, 22 policies were found to be relevant to death literacy. The term death literacy was not used in any policies. However, the four features of death literacy were presented. The policies mainly described how the public, families, carers, and healthcare professionals could improve understanding and skills relating to death and dying. They also described how people could help others in their communities when facing death and dying. There was only a minimal mention of learning through experience, which included content about how the public can help develop services. What do the findings mean? Features of death literacy in UK policies focused on the development of knowledge and skills relating to death and dying through health services, mainly focusing on healthcare professionals. Therefore, more focus on community and social approaches to understanding and supporting death and dying, also learning through experience could be included in future policies.
Introduction
Death literacy is an emerging concept within academic and social spheres. Recently, the COVID-19 pandemic brought public discussions of death and dying to the fore. During this time, public attitudes towards death and dying were explored in United Kingdom based studies in 2021 and 2023.1,2 This research highlighted a lack of public understanding of what death and dying entail, as well as how to discuss it and cope with it. It also reported low levels of public awareness of how to access palliative care, advance care planning (ACPs), bereavement support and of relevant terminology. This emphasises insufficient knowledge of the death system, which is described as ‘the interpersonal, sociocultural, and symbolic network through which an individual’s relationship to mortality is mediated by his or her society’. 3 Other research illustrates that most people do not know how to support people who are dying. 4 These knowledge and skills deficits are also apparent among those who work directly with people experiencing end-of-life, including health and social care professionals. 5 Thus, where death literacy is inadequate, it can negatively impact the quality of life and death, and the psychological and practical experiences of those dying and bereaved.6–8 Death literacy is thus important in supporting the development of effective end-of-life care strategies and support systems, reducing fears and uncertainty associated with dying, and improving access to palliative care.
Current international concepts of death literacy tend to be shaped around experiential learning from first-hand experiences, knowledge exchange or public and community forms of education.9,10 Death literacy usually intersects with health, social care, community and educational contexts, where its key facets are often formally discussed and developed. In line with these facets is the seminal definition of death literacy, which is described as ‘a set of knowledge and skills that make it possible to gain access to understand and act upon end-of-life and death care options’. Four key features of death literacy described by Noonan et al. 11 comprise:
Knowledge: Factual understanding of palliative care, medical services, medication and equipment, public health policies relating to death, for example, death certificates, also end-of-life planning processes, for example, wills and funerals.
Skills: Refers to the confidence and ability to talk about death, dying and bereavement with others, and in providing care to the dying or dead, negotiating and conversing with professionals about dying and death.
Experiential learning: Participation in end-of-life care and accessing information from networks.
Social action: Sharing knowledge about the death system within networks and the ability to put it into practice (e.g. compassionate communities).
These features of death literacy are important in identifying priorities that could be embedded in policies. However, the extent to which the term ‘death literacy’ and its components have been explicitly adopted in official policies requires further exploration.
Aims
This study sought to understand how death literacy is described and framed within UK policies. It aimed to analyse recent (from 2015) UK state level (Westminster) and national (England, Northern Ireland, Scotland and Wales) policies explicitly referring to death literacy or implicitly describing the knowledge and skills related to death, dying and end-of-life.
Question
How is death literacy described across governement policies across the four UK countries?
Objectives
Outline policies relevant to death literacy in the United Kingdom.
Describe how death literacy and its key features are framed and described across the UK governments’ policies.
Analyse and summarise the main cross-cutting themes of these policies relating to death literacy.
Assess how these policies align with Noonan’s et al. 11 features of death literacy.
Explore commonalities and differences in policies between the countries.
Summarise opportunities for future policy and research.
Methods
A document analysis review was conducted to examine the cross-cutting components of UK government and national policies that describe death literacy and prescribe how it is applied in practice. The UK focus of this review is based on the recognition that while the United Kingdom has overarching state policies, it also comprises three country’s devolved parliaments and England, which may differ in cultural attitudes and political approaches towards how policies relating to death literacy are shaped. It therefore offers a multi-level perspective of death literacy in policies within a specific geographical location and distinct cultural contexts. It should be noted that all countries share core elements of the National Health Service (NHS), despite most of the responsibility of health and social care being separately decided at national levels. Likewise, there tends to be no difference between the UK-wide government and England’s governmental policies. UK government policies describing legal matters usually pertain to England and Wales, but health and social care policies usually relate to England only.
A document analysis approach was chosen due to its role in methodological and data triangulation. Document analysis entails finding, selecting, appraising and synthesising data contained in documents. 12 The READ approach was adapted for this document analysis process. This is a systematic procedure for collecting documents and gaining information from them in the context of health policy studies at any level (global, national, local, etc.). The steps consist of (1) reading materials, (2) extracting data, (3) analysing data and (4) distilling findings. 13
Reflexivity
The team of authors is UK based. The lead author is a social scientist with a background in policy and qualitative studies within health and care contexts, with experience of palliative and end-of-life research. The second author is an anthropologist with research experience in the making of care in medical settings. The third author is a medical sociologist with a background in health literacy and the death literacy theme team lead.
Search strategies
A search strategy was developed in line with the keywords related to the inclusion criteria outlined below. The following government and healthcare websites were searched for official policy publications using the following search terms: ‘Death literacy’, ‘death’, ‘dying’, ‘end-of-life’ and ‘palliative care’.
United Kingdom and devolved governmental websites were searched for relevant policy documents, including: (https://www.gov.uk/), Northern Ireland (https://www.northernireland.gov.uk/), Scotland government (https://www.gov.scot/) and the Welsh government (https://www.gov.wales/).
NHS websites: NHS England https://www.england.nhs.uk/, NHS Northern Ireland https://www.health-ni.gov.uk/, NHS Scotland https://www.scot.nhs.uk/ and NHS Wales https://www.nhs.wales.
Additionally, backwards and forwards searches of policies’ content were used to find other relevant policies not directly available via these searches.
Inclusion criteria
The following types of policy documents were included:
UK government, country level governments, and health and care policy documents which explicitly discuss ‘death literacy’ or literacy relating to end-of-life or discuss education, learning, skills, practice guidance or understanding relating to death, dying or end-of-life.
Documents written by government departments or public health services which describe the overall vision of governments and/or policy direction; strategies; or official guidelines which outline how to achieve this vision, or frameworks and delivery plans, which cover the detailed operational planning to deliver on strategies; official instructions on discussing, delivering or recording end-of-life information or skills, national policy; priority setting; call to action; statement of intent documents; Government Acts and White Papers.
The search focused on documents, defined as national, overarching policies from a government or national health service directly relevant to or specifically focused on death literacy (relating to the public; bereaved; health; care; social work or other associated professionals or patients, caregivers or the public or public institutions).
Contains content relating to death processes and death systems before, during and after death.
Published from 1 January 2015 to 14 May 2025, representing policies within the last 10 years.
Exclusion criteria
Policy documents focused on other areas of death relating to health or social care practice and not discussing elements of death literacy (e.g. knowledge, skills, etc.)
Policy documents incorporated within or superseded by more recent policy documents, unless they provide additional information not already covered elsewhere.
Policy documents at a smaller area-level (e.g. regional geographical area) within a country or specific context (e.g. only relevant to the COVID-19 pandemic only).
Policy documents created, for example, by arm’s length bodies such as Public Health Wales or Public Health Scotland.
Any other policy document that did not fit within our categories, including reports; audits; information only; case studies, research with no policy intent; documents relating to national programmes; workforce performance funding arrangements; procurement or infrastructure.
Targeted searches of each database were conducted by the lead researcher. Each term was searched separately within the general websites, using a publication function where available, and relevant filters, for example, date, document type. Then the titles and descriptions of each record were screened in accordance with the inclusion criteria, seeking specific content relating to death literacy including implicit descriptions of knowledge, skills, training and learning relevant to death, dying, palliative care and end of life.
Search results
After screening 10,711 records, 63 duplicates were removed and 137 papers were eligible for full-text reading. Four policy documents were unable to be retrieved. Then, 133 were read in full. At this stage a further 74 documents were removed due to a lack of relevant content. Fifty-nine documents were eligible for data extraction. A further 36 documents were excluded for the following reasons: not specifically detailed enough about death literacy (n = 19); advice or resource document only (n = 5); superseded by another document (n = 3); case study (n = 2); not authored by government organisation (n = 2); research summary or report (n = 2); programme updates (n = 1); full text unavailable (n = 1); and a restricted document (n = 1). A final 22 policy documents were suitable for analysis. Figure 1 PRISMA document outlines the search results. 14

PRISMA flow diagram.
Data extraction
The following data from each policy document was extracted into a table comprising author(s)/year published, document type, target population, main aim and or vision, research evidence referenced and key recommendations relating to death literacy, available in Table 1 policy characteristics.
Policy characteristics.
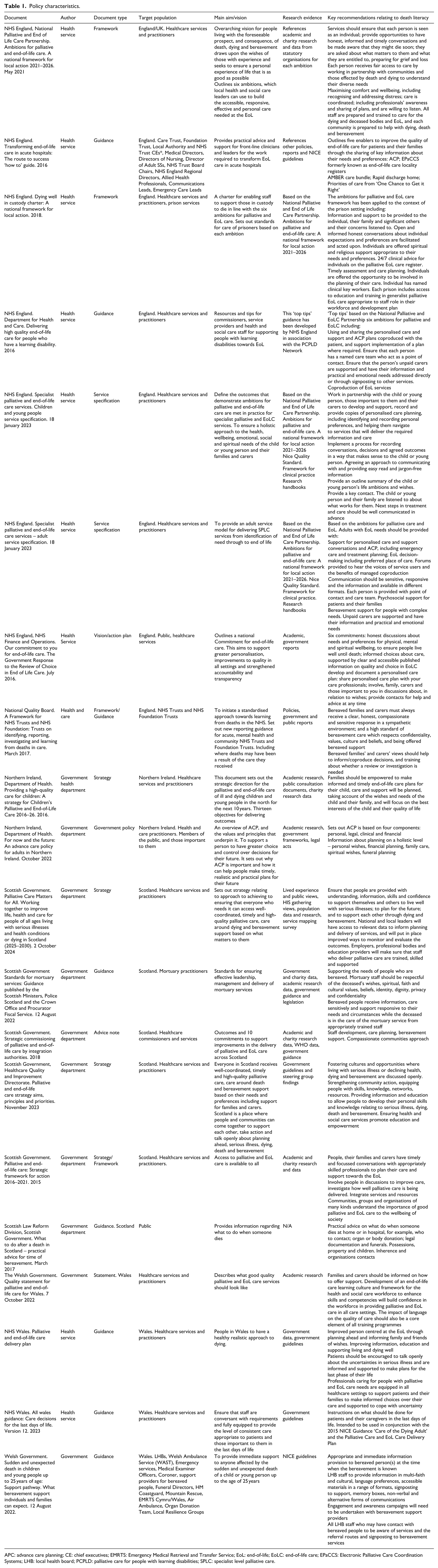
APC: advance care planning; CE: chief executives; EMRTS: Emergency Medical Retrieval and Transfer Service; EoL: end-of-life; EoLC: end-of-life care; EPaCCS: Electronic Palliative Care Coordination Systems; LHB: local health board; PCPLD: palliative care for people with learning disabilities; SPLC: specialist level palliative care.
Analysis
Thematic content analysis was conducted, which involves a form of pattern recognition within the data. 15 The lead author coded all policy documents and the second author separately double coded 25% of the documents. The documents were examined for content relating to Noonan et al. 11 four elements of death literacy, that is, knowledge; skills; experiential learning; and social action and mapped against these elements in line with the researchers’ interpretation. In some cases, content was associated with these themes but may not strictly align with Noonan’s description (e.g. skills relating to healthcare professionals’ death literacy). Any additionally relevant content relating to death literacy was inductively analysed and was also coded into themes. Key codes were compared, then final themes and sub-themes were agreed by consensus. NVivo v.14 was used to manage the data analysis Lumivero, version 14.
Key themes from the policy documents were synthesised and are presented in a thematic narrative format. Table 2 illustrates how the key thematic components of death literacy compare across the varying UK policies.
Comparisons between policies: England/ UK, Northern Ireland, Scotland and Wales.

Source: Page et al. 14 This work is licensed under CC BY 4.0. To view a copy of this license, visit https://creativecommons.org/licenses/by/4.0/.
APC: advance care planning; EoL: end-of-life; EoLC: end-of-life care.
NCP 2021 = National Palliative and End of Life Care Partnership – Ambitions for palliative and end-of-life care: a national framework for local action 2021–2026, May 2021.
NHS England 2015 = NHS England – Transforming end-of-life care in acute hospitals: the route to success ‘how to’ guide, December 2015.
NHS England 2024 = NHS England – Dying well in custody charter: a national framework for local action, 19 June 2024.
NHS England 2017 = NHS England, Department for Health and Care – Delivering high-quality end-of-life care for people who have a learning disability, 2017.
NHS England 2023a = NHS England – Specialist palliative and end-of-life care services: children and young people service specification, 18 January 2023.
NHS England 2023b = NHS England – Specialist palliative and end-of-life care services – adult service specification, 18 January 2023.
NHS England 2023 = NHS England – Addressing palliative and end of life care, 31 October 2023.
UK Gov 2016 = Department of Health, NHS Finance and Operations. Our Commitment to you for end-of-life care: the government response to the review of choice in end of life care, UK Government. July 2016.
NQB 2017 = National Quality Board – A framework for NHS Trusts and NHS Foundation Trusts on identifying, reporting, investigating and learning from deaths in care, March 2017.
NI Gov Jan 2022 = Northern Ireland, Government, Department of Health. A strategy for children’s palliative and end-of-life care 2016–26, 21 January 2022.
NI Gov 2015 = Northern Ireland Government, Department of Health, Social Services and Public Safety – Regional Bereavement Guidance on evidence-based, holistic care of parents and their families after the experience of miscarriage, stillbirth or neonatal death, December 2015.
NI Gov Oct 2022 = Northern Ireland Governnment, Department of Health – For now and the future: an advance care policy for adults in Northern Ireland, October 2022.
SG 2024 = Scottish Government – Palliative Care Matters for All Working together to improve life, health and care for people of all ages living with serious illnesses and health conditions or dying in Scotland (2025–2030), October 2024.
SG 2022 = Scottish Government – Standards for mortuary services: guidance published by the Scottish Ministers, Police Scotland and the Crown Office and Procurator Fiscal Service, 12 August 2022.
SG 2018 = Scottish Government –Strategic commissioning of palliative and end-of-life care by integration authorities, May 2018.
SG 2023 = Scottish Government, Healthcare Quality and Improvement Directorate – Palliative and end-of-life care strategy: aims, principles and priorities, November 2023.
SG 2015 = Scottish Government – Palliative and end-of-life care: strategic framework for action 2016–2021, 2015.
SG 2017 = Scottish Government, Law Reform Division, Scottish Government – What to do after death, March 2017.
WG 2022a = Welsh Government – Quality statement for palliative and end-of-life care for Wales, 7 October 2022.
WG 2022b = Welsh Government – Sudden and unexpected death in children and young people up to 25 years of age: support pathway. What bereavement support individuals and families can expect, 12 August 2022.
NHS Wales 2017 = NHS Wales – Palliative and end-of-life care delivery plan March, 2017.
NHS Wales 2023 = All wales guidance: care decisions for the last days of life, version 12, 2023.
Consider, if feasible to do so, reporting the number of records identified from each database or register searched (rather than the total number across all databases/registers).
If automation tools were used, indicate how many records were excluded by a human and how many were excluded by automation tools.
Results
Key themes, sub-themes and minor themes from the data are presented in Table 3, these are described in a narrative form in relation to Noonan’s four key elements below, these comprise: Knowledge; Skills; Experiential learning; and Social action.
Themes and sub-themes.
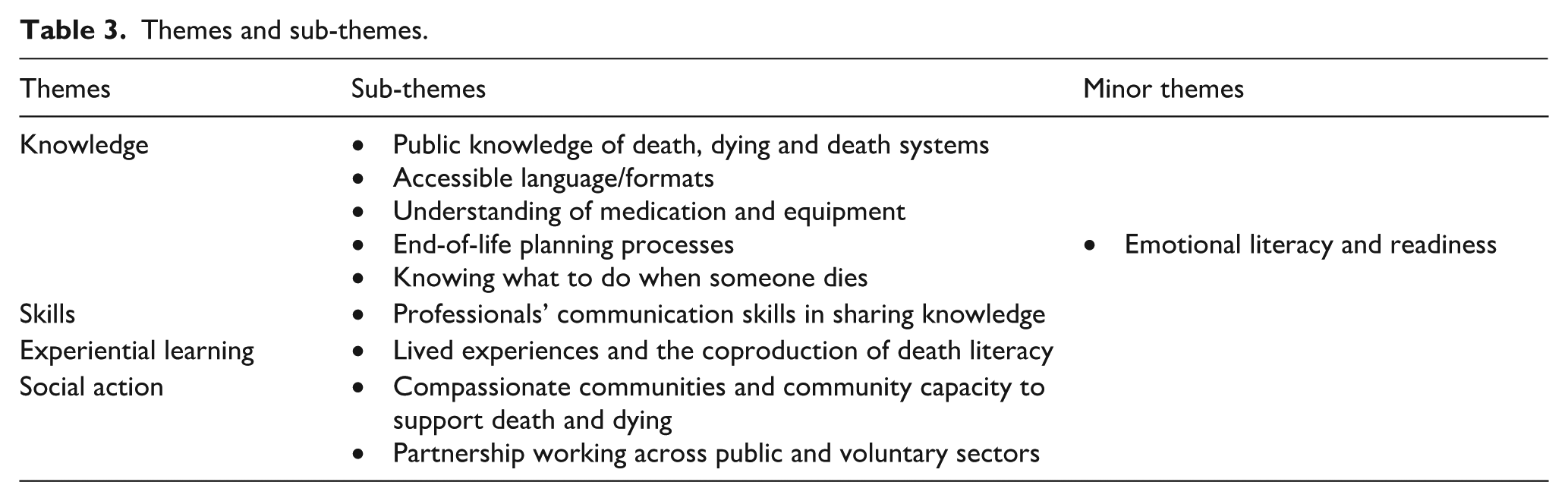
Knowledge
Public knowledge of death, dying and death systems
The need to raise public awareness about death and dying are explicitly acknowledged in English and Scottish policies.16–18 Specific attention is provided to encouraging people with a learning disability to develop their awareness about death and dying. 19 A Welsh Government policy also states that people in Wales should have a healthy realistic approach to dying. 20 However, there are limited examples across these policies of how public awareness has been or could be facilitated. The need to promote public awareness of advance care or future care planning, which tacitly implies a need for recognition of death and dying is highlighted across all four nations.19–22
Commitments to support the public provision of information and dialogue regarding dying and end of life are explicitly stated, they refer to leadership in supporting organisations, 16 commissioning of public sector bodies outside of health and care including educational organisations,18,22 and third sector initiatives to facilitate open conversations.20,23 There is an emphasis on utilising media of all types 16 to support people in discussing death 19 and signposting to information using healthcare resources. 22
Accessible language/formats
There was acknowledgement within the policies that information presented to the public needs to be fully accessible and adapted to people’s varying needs. This includes providing information and communication in varying formats,20,22,24 for example, for people with learning disabilities and those who may use non-verbal communication19,24 and those that require sign language and interpreters. 25 Also, provision for those who do not have English as a first language.24,26
Understanding palliative care and medical services
Policies across the UK emphasise that knowledge about palliative care and medical services is required by members of the public. There is a specific mention of the need for training and educational opportunities for caregivers and community members in providing palliative care and care for people at end-of-life. Examples of these initiatives are highlighted, including End-of-life Aid Skills for Everyone (EASE) and Last Aid. 22 Likewise, there is an emphasis on professionals sharing key information with caregivers when some is dying, including how to access facilities, practical help at home, in hospital or other settings 27 or how to provide care.26,28 Providing explanations and opportunities to discuss and record decisions around hydration and nutrition (including artificial provision) are also expected to be offered by health and care services. 27
Understanding of medication and equipment
Providing information and skills training for caregivers and community members with an understanding of medical equipment, devices and procedures are referred to as a means to allay fears of treatments and support practical application.19,22
End-of-life planning processes
A need for the public to understand and consider planning processes relating to end of life including wills, funerals and finances were explicitly mentioned across UK policies.16,20–22,29–31 This includes information about financial support for funerals,22,31 hospices helping with funeral planning 32 and the broad role of funeral directors. 25
Personalised planning for end of life was emphasised across all countries, each advocating that everyone approaching the end of their life should be offered opportunities for informed discussion and care plans (anticipatory care, future care and advance care plans).18,20,21,23,27 These included death in transit plans 33 emergency care and treatment plans, treatment escalation plans and cardiopulmonary resuscitation decisions.21,26,28 The Northern Ireland Government highlights the need for parents and families to be kept informed about the plan of management of their care before, during and after the loss of their baby. 30 A multi-disciplinary approach to ACP and anticipatory care planning with patients and families, service providers, educators, policymakers and commissioners was highlighted by Scottish Government. 17 Ensuring opportunities are provided for preferences to be expressed through ACP is emphasised by NHS Wales. 27
Knowing what to do when someone dies
Across UK nation’s policies there was a stated need for people to access information regarding knowing what to do when someone dies, including at home.22,27,31 Likewise, how bereaved people should be made aware of what happens when deaths involve the police,24,25,31 legal matters including death certificates,30,31 the role of the medical examiner 27 and if an investigation needs to take place into a death. 34 Information is provided about how to organise funerals,24,30,31 financial matters30,31 and how to deal with mass and social media. 30 Policies are available which specifically relate to sudden or unexpected deaths, 31 including guidance describing the bespoke processes and information that should be provided regarding the death of a child, including burial or cremation and the involvement of a coroner.24,30
Guidance for the public relating to discussing organ or whole-body donation was provided for each of the four countries.21,27,29,31 At different timepoints since 2013, these countries developed an ‘opt out’ approach to presumed consent and the need to educate people on their rights. Presumed consent was enshrined in law in the following years: Wales, 2013; England, 2019; Scotland, 2019 and Northern Ireland, 2023.
Ensuring that people know how to access bereavement services is prioritised across the four nations’ policies.25,27,29–31,34 By comparison the National Palliative and End-of-life Care Partnership policy mentions the need for bereavement support but not the need for how to access it. 16
Emotional literacy and readiness
There is some recognition that support for the emotional facets of death and dying is needed by those approaching end of life16,19,22,30 and their caregivers, 32 including signposting to appropriate information 33 and support for bereaved families, including parents.23–25,30,31,34 This included health and care professionals enacting empathetic approaches, and families being offered immediate information about support after the death of a child with the aim of reducing the need for traumatic grief support. However, further details of the emotional support required to improve death literacy are generally lacking prioritisation across the other policies.
Skills
A significant proportion of the focus of the policies concentrated on the skills of professionals (health, care, community, etc.) and how they should gain knowledge of death systems and processes in order to provide appropriate care at end of life or enable patients and caregivers to become more aware of death and dying. Policies from across all four countries outlined the expectations, education and training that are required to improve death literacy among staff, patients and the public.
Professionals’ communication skills in sharing knowledge
The need for all health and care professionals providing care in end of life and palliative settings to be appropriately trained to signpost to relevant services that support people’s spiritual, emotional, practical and financial needs relating to end of life was prescribed.23,26,28,33 This specifically included signposting via accessible information 35 to grief and bereavement, counselling, mortuary services and where appropriate police services.24,25,30
Ensuring that patients and caregivers are made aware of a single point of access, including key contacts or workers for their information needs when nearing the end of life was described by all countries.19,24,26,28 This included knowing who the senior or lead clinician is providing care for them, and the need for a 24/7 single point of access to advice about end-of-life care.23,35 There was particular focus on the importance of this provision for families caring for a person at home whose death is imminent. 20 People bereaved by a sudden or unexpected death should be provided with bereavement coordinators or advisors for bespoke support and information.24,34
The need for open and honest discussions about death, dying and bereavement is emphasised and highlights the importance of interpersonal communications between information providers and receivers.16,17,22,23,34,35 Palliative care and other health professionals (such as a bereavement midwife) should receive training in sensitive communication skills with people who are at end-of-life, their family and caregivers,26,28,30,34 and respond appropriately to their preferred wishes and cultural, spiritual needs, identities and beliefs.25,30 Training is also advocated to enable professionals to listen to and support people to make informed decisions at their end of life relevant to their personal needs and preferences.16,18,21,23,26,28,30 There is recognition that professionals should help empower people to take control at the end of life 16 through appropriate information provision to support decision-making,17,21,25,26 including parents regarding end-of-life plans for their child 29 or where perinatal or neonatal death has occurred. 30
The need to ensure that people understand the nature of their illness (diagnosis), prognosis, likelihood of dying or of a death was highlighted.16,19,26,28,35 There was a recognition of the specific information needs of parents of children who are dying and providing pre-birth diagnosis. 29 Underserved groups were also recognised as requiring diagnostic information in bespoke and accessible ways. 16 Likewise, that these conversations need to be timely and focused at appropriate timepoints,16,18,34 where possible before a person’s condition is incurable, 19 and to ensure ACPs are offered. 21 Information about the reasons for decisions, changes to treatments, health status and death should be promptly communicated and carefully explained to caregivers.16,17,25,30,33
There is also recognition that local health, care and voluntary organisations, including mortuary staff, need appropriate up-to-date knowledge and practical skills that enable them to play their part in good end of life and post-death care.16,25 This includes equality training in order to understand and respond to wider determinants of people’s experiences towards the end of life and during bereavement.17,25
Experiential learning
Lived experiences and the coproduction of death literacy
Limited references are made throughout the policies relating to public participation in end-of-life and how these experiences shape death literacy. The references that are made relate to coproduction (including the co-designing of services for end-of-life care), which were considered important.16,17,19,23,33,34 This includes co-producing bereavement skills training for healthcare staff. Enhancing experiential approaches could enable people with lived experience of dying or supporting those through end-of-life to inform the death system and thus enhance death literacy among the public and professionals.
Social action
Compassionate communities and community capacity to support death and dying
The compassionate communities’ model was explicitly referenced within the National Palliative and End-of-life Care Partnership and Scottish documents. It was understood as a method towards supporting people to feel ‘ready, willing and confident to have conversations about living and dying well’ which would ‘help dying and bereaved people be better supported and ensure that they do not become isolated from their communities’. Here, it is suggested that local organisations find ways to offer support and training by working alongside families and communities. 16
Scottish policies encouraged an ethos that the end-of-life is the responsibility of the whole community. 32 The Scottish Government (2024) stated that people should be enabled to have the understanding, information, skills and confidence to support themselves and others to live well with serious illnesses, and this could enable people to plan for and discuss death and dying more openly. 22 In turn, this could strengthen community action and networks of care.17,32 In this respect, improving components of death literacy is understood as a means to improve end-of-life care.
Partnership working across public and voluntary sectors
It was recognised that communities and public services need assistance to work alongside one another, to open up discussions about death, and provide support. These partnerships can help to meet diverse cultural, and faith needs, which enable minority groups to obtain specialist support in the community.16–18,22,23,32 For example, NHS England recommended using circles of friends (people who understand the person’s needs) for those with a learning disability to support decision-making in community. 19 The Welsh Government encourages the use of peer support, and community events for people to discuss their bereavement experiences and needs. 24 Scottish documents highlighted well-established training and community-led education opportunities, which aimed to improve people’s experiences of death and dying. These included the Good Life Good Death Good Grief initiative set up by The Scottish Partnership for Palliative Care.22,32 This initiative and others across the UK highlighted how community and volunteer groups provide bespoke resources and expertise, including social networks, financial advice and support groups.26,28 It was also recognised that volunteer recruitment needed to be more integrated with other public and community services. 16 This includes developing relationships with hospice and outpatient services, inpatient units as a necessary step in improving end-of-life care and understanding. 19 Storytelling conducted by volunteers was recommended as a method to share and reflect both challenges and positive accounts of end-of-life care. 16 Other examples of pre-existing initiatives referenced in these policies included the Byw Nawr (Live Now), a local charity in Wales, aimed to drive forward public conversations around death and dying. 20 Compassionate Inverclyde in Scotland was a multi-agency, community-wide initiative which aimed to build a compassionate community. 32 Dying Matters led by the National Council for Palliative Care a UK-wide coalition aimed to support changing knowledge, attitudes and behaviours towards dying, death and bereavement, by encouraging people to talk about their wishes regarding death and dying. 16 In this sense, volunteer groups and charities were framed as a way of enabling the public to gain more awareness, community care and involvement in death and dying.
A comparison of the UK policies
Key commonalities and differences in policies across England, Northern Ireland, Wales and Scotland are summarised in Table 2. A principal finding is the absence of the term ‘death literacy’ across all policy documents, despite its component elements being described. The number of documents that describe features of death literacy relating to each nation broadly reflects the size and capacity of each country to develop policy. Each country has focused on different elements of the death system. English and UK policies are often interchangeable, thus cover a wider remit of policy objectives than Northern Irish, Scottish and Welsh policies. Likewise, Westminster (UK government) has reserved powers over several non-devolved policy areas, including in health, for example, medicines in England and Wales, which can make country specific policymaking complex and requires partnership working. 36 Across UK government and English focused policies, death literacy promotion is advocated in relation to varying initiatives including raising public awareness through leaders and media channels, and partnerships between community groups, third sector and public sector organisations. However, all countries’ policies focus primarily on the role of healthcare professionals, gaining and imparting knowledge of end-of-life processes to patients and their caregivers. Northern Irish policies which highlight elements of death literacy focused principally on ACPs, palliative care for children, and support and information for bereaved parents, reflecting that Northern Ireland has the highest child mortality rate in the United Kingdom. 37 While highlighting the importance of palliative care and end of life, Scottish policies also recognise the role of wider organisations, including mortuary services, and the need for public awareness of death and dying, and skills for caregivers at the end-of-life coupled with a stronger emphasis on compassionate communities and public health approaches. Demonstrating an acknowledgement that a significant proportion of death education occurs in local communities, and the need to reduce structural inequities. This is particularly pertinent as people in Scotland die younger than in any other Western European country. 38 Also, Scotland has integrated health and care functions, which potentially enable a more holistic approach to death and dying. 39 Welsh policies focused on understanding death and dying through the lens of palliative care and end-of-life processes, facilitated through NHS professionals. This reflects the increasing need to provide palliative care to the oldest population in the United Kingdom. 40 These Welsh policies are underpinned by the Wellbeing of Future Generations Act, which sets out the legal requirements of public bodies to plan for the needs of an increasingly ageing population. 41
Overall, although UK governments’ policies address broader features of death literacy, including social action, compared to health services’ policies, death literacy is consistently framed around the role of health systems and institutions. Likewise, this review illustrates the variability of priorities across the UK’s countries, indicating that a partnership approach to policy development is expedient to ensure a coproduced and multi-level approach to death literacy. This should recognise the interdependency between the national governance structures, health, care, local services and the public to ensure practical implementation.
Discussion
Key findings
This policy document analysis review provides an overview of how death literacy is described across UK government policies. It highlights how the term and key components of death literacy are integrated and compared across these policies. This provides a lens to understand how death literacy is framed within political spheres and policy agendas. Death literacy as a term was not explicitly mentioned in any of the governmental policies. However, its key components were evident (e.g. knowledge, skills, experiential learning and social action, as described by Noonan et al. 11
Due to the medical and palliative care focus of the policies, there is significantly less reference to the role of experiential learning. This reflects prior observations from Noonan et al. noting the dominance of the medical approach to death. 11 Similarly, there is a focus throughout the policies on the roles of healthcare professionals in relation to death literacy, which are not explicitly mentioned in Noonan et al. 11 four features but can be associated with the knowledge and skills categories. This prevalence does, however, reflect that most people in the United Kingdom will gain access to knowledge related to death and dying through health and care services. Likewise, while some documents mention coproduction, there is minimal elaboration on how experiences and social networks can shape understanding and enable people to utilise skills they have acquired when someone dies. This demonstrates elements of death literacy that require significantly more policy attention. There is also some focus on social action, including compassionate communities, and voluntary organisations, although synergy between the grassroots, community approaches, population-wide initiatives and service provision could be further developed.
Death literacy in political spheres
Despite the absence of the term ‘death literacy’ among government policy documents, there is evidence of its use by elected representatives in the United Kingdom within other government documents. A Welsh Senedd cross party inquiry report of the experiences of palliative and end-of-life care in the community during the COVID-19 pandemic in 2023, recommended that ‘the Welsh Government should support greater death literacy within communities in Wales, encouraging higher levels of advance planning for end-of-life, alongside improving support for bereaved people’. This would involve ‘investing in hospices as experiential learning sites; addressing inequalities; and ensuring that workforce strategies prioritise the wellbeing, staffing, education and training needs of those working across the full spectrum of palliative and end-of-life care’. 42 Likewise, The House of Commons’ Health and Social Care Committee, recommended the establishment of a national strategy for death literacy relating to the assisted dying bill. The UK government’s responded that there was no plan to establish a national strategy for death literacy in January 2024. 43 These reports illustrate the need for UK-wide and devolved governments to recognise the importance of death literacy and embed it into their policies and strategies. While the absence of the term ‘death literacy’ does not necessarily prevent elements of it from being prioritised across policies, consistent explanations and application of the term would provide a more cohesive understanding of its component parts and their significance in improving preparation for and experiences relating to death and dying.
Death literacy gaps in policies
The policies in this review offer nominal reference to the underlying reasons for a lack of death literacy, and few incorporate public health or community approaches. Specifically, there is minimal recognition of barriers faced by people from underserved communities, with often poorer access to hospices, healthcare services and educational opportunities. 44 Importantly, those from the most socio-economically deprived areas of the United Kingdom and underserved groups often face issues relating to death and dying at a younger age, compared to the general population.45,46 This highlights how different groups and individuals may gain death literacy through diverse methods. It is therefore essential that approaches to improve death literacy, reflect individuals and groups differentiated and multi-faceted needs, circumstances and contexts. This requires policy approaches which recognise and address underlying structural barriers to accessing appropriate support and services relating to end-of-life. Rather than merely focusing on communities’ knowledge and skills deficits, ‘new public health approaches’ could be implemented, which emphasise equity, empowering people as active participants, addressing the broader social determinants of health, and local solutions tailored to specific populations.8,47 Cross-departmental and multi-disciplinary, multi-level approaches to death literacy are therefore required, which involve incorporating the wide range of services and approaches that can enhance support and knowledge, at individual, community and institutional levels. The Scottish Partnership for Palliative Care advocates this cross-departmental approach. 48 This approach encompasses state-provided services (health, care, education) working alongside workplaces, family and community networks, and the media to support open attitudes and behaviours towards death and dying. Policymakers should also consider death literacy promotion throughout the life-course. This could involve expanding grief education which will be implemented in English schools in 2026, and bereavement training for teachers in Northern Irish schools, to include wider education about death and dying, across all UK countries. 49
Previous research demonstrated how public health approaches, including community-based activities in varying global contexts, can improve understanding and experiences at end-of-life and relating to palliative care.50–52 Public Health England developed a Public Health Dying Well Community Charter and accompanying toolkit to improve community support in the face of life-threatening and limiting illnesses, caregiving and bereavement, which utilises partnerships between public and third sector organisations. 53 The Academy of Medical Sciences, UK, developed a ‘departure lounge’, a short-term immersive installation based in a shopping centre in London, UK. This provided information and encouraged discussion with the public about death and dying. 54 However, these have mainly been localised rather than nation-wide initiatives and are not always specifically aimed at improving death literacy. Nonetheless, integration of these community-based approaches into government policies could provide a basis to develop evidence-informed country-wide initiatives.
While some policies address the emotional realities of death and dying, most focus on the practical knowledge and skills required to understand processes and the death system, including ACPs and cardiopulmonary resuscitation decisions. Further emphasis on emotional aspects and support could help address some fundamental barriers to death literacy such as fears of triggering challenging emotions in others when discussing death. 55 However, public health and NHS support information across all four countries recognise the need for emotional support for people who are bereaved after someone has died by suicide or an unexpected death. This illustrates a more holistic approach to death literacy, which could be expanded to all of those dealing with death and dying.56–59
Articulating the purpose of death literacy is also fundamental to improving policy approaches. This may include underpinning approaches with aims of increased awareness, practical, psychological and emotional preparedness and wellbeing, improving end-of-life care and acceptance of death and dying.
Strengths and limitations
This policy review provides an in-depth, multi-faceted comparative analysis of how elements of death literacy are framed and described within recent UK policies. It illustrates gaps within current UK policies, particularly in relation to experiential and wider public and community-based approaches to death literacy. It highlights areas for future policies to focus on, to provide a more holistic approach to enabling societal wide death literacy.
This study was limited however, as it was restricted to governmental policies, legislation and official guidance, post-2015. Some policies were unable to be included due to their restricted nature, even where they had relevant content. However, wider political discussions and initiatives are published regarding death literacy, illustrating some growing recognition of the issue within political spheres that have yet to influence formal policies.
Policy implications
This review illustrates that future UK policies could be enriched by embedding death literacy explicitly through a consolidated set of proposed actions, with the aim of improving public and services preparation for death, dying and end-of-life. Cross-departmental, multi-national and coproduced approaches to policy could help establish wider understanding and application of death literacy and its component elements in practice. There is a need to incorporate public health and social approaches to death literacy which reach beyond the health and social care systems to the wider social sphere and build on social capital, and pre-existing knowledge and skills. Policies integrating community and educational initiatives and approaches could support death literacy across populations but also require acknowledgement of diverse needs and cultures, and that address structural inequalities which prevent equitable access to information and support across the life-course. Further research which compares varying international approaches to death literacy, could help develop an international understanding of best practice and inform future policies.
Conclusion
Death literacy as a term was not explicitly stated in any official UK nation’s policies. However, key components of death literacy including informing and developing public’, caregivers’ and healthcare professionals’ knowledge and skills around death and dying were evident. Future policies should explicitly outline a consolidated approach to death literacy, with the aim of improving experiences and preparedness relating to death, dying and end-of-life. These should embed strategies to implement multi-level, cross-departmental, and new public health approaches which addresses systemic inequalities, and enhance experiential and socially focused initiatives.
Footnotes
Acknowledgements
We would like to thank Marie Curie for funding this study.
Author contributions
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: D.H.H., J.R., M.E. are funded by Marie Curie (Grant 523838).
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
Data are available upon reasonable request.
