Abstract
Background:
Providing specially trained volunteer navigators is one promising strategy for supporting the increasing number of family caregivers who are caring for children living with medical complexity.
Objective:
The objective of this study was to develop consensus on the role and competencies required for volunteer navigators who support caregivers of children living with medical complexity.
Design:
This was a mixed-method study using modified e-Delphi and focus group methods. In phase 1, a modified e-Delphi survey with 20 family caregivers and a focus group with 4 family caregivers were conducted to develop consensus on their unmet needs and the potential roles of a volunteer to meet those needs. In phase 2, a modified e-Delphi survey was conducted with experts to develop consensus on the volunteer competencies required to meet the roles identified by family caregivers in phase 1.
Results:
Findings from phase 1 resulted in 36 need-related items over 8 domains: communication, daily life and chores, emotional support, information and knowledge, respite, support with decision-making, and sharing the caregiving experience. Concerns about the volunteer role included the potential lack of commitment in the absence of remuneration, the complexity of the child’s condition that was beyond the role of a volunteer, and a preference for support from individuals they knew. Findings from the phase 2 Delphi survey with professionals resulted in 22 competencies, derived from the roles identified in phase 1, that would be required of volunteers who wished to support these family caregivers.
Conclusion:
This study provides insight into a role for volunteers in meeting the needs of family caregivers of children living with medical complexity. A volunteer with lived experience and adequate preparation can assist with meeting some of these important needs. Further research is required to better understand the feasibility and acceptability of such a role.
Introduction
A growing number of children are born with medically complex conditions, and because of more sophisticated treatment options, many of these children survive for years and even into adulthood. Children living with medical complexity are defined by ‘high family-identified needs; complex chronic disease necessitating specialized care; functional disability; or high healthcare utilization’ (p. 518). 1 From 2015 to 2016, over 97,000 children living with medical complexity were identified across Canada. 2 They have a range of diverse conditions, such as neurological impairments, cancer, and cardiovascular or gastrointestinal disease. 2 Higher survival rates of infants born prematurely or with perinatal or congenital anomalies are further contributing to this growing population.3,4
Children living with medical complexity, not only those experiencing symptom burden, can benefit from a palliative approach to care. Pediatric palliative care (PPC) is defined as an ‘active and total approach to care provided to children with life-threatening conditions and their families from the time of recognition or diagnosis of disease, throughout the illness, at the time of death and beyond’ (p. 156). 5 PPC, however, is often poorly understood or accepted. 6 This care is often invisible care; few are comfortable with thinking about palliative care, let alone palliative care for children. To date, palliative care, as a medical subspeciality and area of research, has focused primarily on the needs of older persons, and this established practice may not be transferable to the unique needs of children and their families. 7 The relative invisibility of PPC has meant that some families feel marginalized and misunderstood in their daily struggles to provide care. Furthermore, the boundaries between definitions of medical complexity and palliative care are notoriously complex.
Few parents expect to provide supportive care to a child living with medical complexity or feel prepared to do so. Such care requires significant commitment and expertise on the part of the caregiver. Parents who fulfill the role of family caregiver take on what is often an overwhelming and all-consuming task. The child’s condition and complex treatment regimes can have a significant impact on the quality of life of the entire family. Evidence to-date highlights the support caregivers require to be able to function well in their responsibilities.
Emotional, spiritual, and decision-making support
Becoming a caregiver for a child living with medical complexity necessitates a shift in identity from that of simply being a parent to that of being both a provider of health-related care and a parent. Parents are expected to learn and perform complex medical regimes on a daily basis. Emotional support has proved to be a key factor in guiding family caregivers toward this identity reconciliation.8,9 Families require emotional support throughout the caregiving experience and into the bereavement period. It is not uncommon for parents to feel abandoned by healthcare professionals once their child has died.8–10 Even though pediatric healthcare services are designed to be family-centric, these services may no longer be extended after the child, the focus of care, has died. These feelings of abandonment on the part of family may be exacerbated when they are confronting deep grief, ‘emptiness’, ‘emotional survival’, and a need for ‘re-adaptation [. . .] to the outside world’ (p. 12). 8 This emotional support into bereavement experience is particularly important considering the fatigue experienced by many family caregivers, a consequence of the 24/7 care provision during their child’s palliative trajectory.8,10 Such fatigue from caregiving has been reported as lasting for months and even years for some parents. 8
Furthermore, families caring for a child living with medical complexity at home have identified a need for spiritual and existential support.11–15 Developing a meaningful narrative around what is happening to their family is an important part of family caregiver support. Families typically find this support through extended family, associations dedicated to their child’s illness, local churches, pastoral care, and chaplains specialized in children ministries.14,15 Studies to-date indicate that this existential and spiritual support, and consequent meaning-making, assists in mediating decision-making conflict and helping families cope into bereavement.14,15
Finally, family caregivers of children living with medical complexity live with a heavy and often unwieldy burden of decision-making with serious impact on the entire family. These decisions range from everyday choices about how to manage their many day-to-day tasks to major decisions regarding medication or life-sustaining treatment for their child.9,10,15,16 An important part of making these decisions is having access to good information for making an informed decision. However, caregivers report encountering challenges in getting relevant, accessible, and clear information regarding a range of topics.15,17 This necessary information includes, but is not limited to, providing symptom management at home, accessing financial information, and finding services to assist them.9,13,14 Support in finding this information, and in making the multiple decisions required of their role, is an integral part of family caregiver well-being.
Tangible support
Caring for a child living with medical complexity entails an overwhelming number of tasks that require many hands. Practical supportive needs include assistance with caring for other children, juggling multiple medical appointments, accessing information, completing household chores, and obtaining caregiver respite.9,10,15,17,18 Caregivers particularly need practical support with cooking, cleaning, grocery shopping, and housekeeping. 8 The task of communicating the status and needs of the ill child to multiple healthcare providers, community support services, and family can in itself be an overwhelming role.11,12,16 Although family caregivers are often aware that there are services available to assist them, finding and accessing those services can be an additional burden. 8 Furthermore, such services can be expensive, and hence inaccessible for families who are not wealthy. 8
Family caregivers further struggle with balancing care for their children living with medical complexity and the care of their other children, which can lead to a fragile family life.8,9 The intensive and pressing reality of their child’s needs requires consistently rearranging the home-life, which can disrupt the activities of other children. 9 Frequent and unanticipated hospitalizations and recurrent, time-arduous appointments make it difficult to attend to other children in the home.9,18 This in turn can leave caregivers feeling discouraged and distressed about their parenting abilities. 9 These family caregivers struggle to reconcile these feelings amidst the commitments required by their children living with medical complexity. 9
Support for families to balance routine and home-life is crucial to the well-being of family caregivers; respite therefore can play an important role in decreasing caregiver self-reported stress and worry.13,19 In one case, the recognition of the need for family caregivers to have time with their other children led to the establishment of a short-break respite program for families of children with palliative needs. 18 This consisted of having a trained facilitator come to the home to provide care for the child with palliative needs. 18 This intervention gave family caregivers the opportunity to spend quality time with their other children, which in turn improved home stability and improved the quality of life of family caregivers. 18 Similar findings have been demonstrated in other respite interventions. For example, in one study, the majority of family caregivers indicated that respite helped them to maintain home routines. 14 Finding ways to provide support for family caregivers of children living with medical complexity is an important focus of family-centric care.
Volunteer navigation
A potential avenue for helping family caregivers is through volunteers who focus on providing support. In the context of adults living with life-limiting illness, hospice volunteers have a long legacy of providing support. More recently, a volunteer navigator role has developed to expand the scope of the hospice volunteer. 20 This model, called Nav-CARE (Navigating-Connecting, Advocating, Resourcing, Engaging) provides additional training to hospice volunteers to enable them to provide assistance for the day-to-day challenges experienced by persons living with declining health at home with an emphasis on improving their quality of life.20,21 Nav-CARE has been implemented and evaluated in multiple sites across Canada with good impact. Volunteers feel well-prepared and satisfied in their role; older persons and families who have participated in the program have indicated that having a volunteer navigator has improved their engagement with life, their ability to manage their illness, and their overall quality of life. 21 Such results may hold promise for a similar model that can assist family caregivers of children living with medical complexity. The research described in this paper is a first step in preparing such an adaptation. The purpose of this study was to inform the creation and development of a volunteer role and competencies to support caregivers of children living with medical complexity.
Methods
Research approach
This was a mixed-method study completed in two phases. Phase 1 aimed to develop consensus on the needs of family caregivers of children with medical complexity to inform the role of a supportive volunteer. A modified e-Delphi survey was delivered over two rounds and a subsequent focus group was conducted with family caregivers to develop consensus on their unmet needs and the potential roles of a volunteer to meet those needs. The focus group was conducted to explore in-depth the needs described on the survey and to identify additional need-related items for round two of the phase 1 e-Delphi. The purpose of phase 2 was to determine what competencies would be required of a volunteer to fulfill the roles as described by family caregivers in phase 1. A competency refers to the knowledge, skills, or abilities required to fulfill a role. A modified e-Delphi survey, delivered over two rounds, was conducted to develop consensus on the volunteer competencies required to meet the roles identified in phase 1. Reporting of the study process was guided by the CREDES criteria adapted from Junger et al. (Supplemental Appendix B, Figure B1).
Sample and recruitment
In phase 1, current or past family caregivers of children living with medical complexity were recruited through email via convenience and snowball sampling. Potential participants were identified through a children’s hospital network, specifically through a research liaison who shares research opportunities with families. To be eligible for the study, caregivers had to have performed medical treatments in the home, attended frequent medical appointments, and have devoted significant unpaid time to caring for the child. To confirm eligibility, caregivers who were interested in participating were asked to contact the study team and had an initial phone call to screen for the above points before proceeding. Family caregivers who participated in phase 1 were invited to take part in the focus group; four persons volunteered to participate. In phase 2, professionals with expertise in palliative care, pediatrics, and/or navigation were recruited via email through existing relationships with academics and healthcare professionals.
Data collection and analysis
Phase 1 used a modified e-Delphi process and focus groups. The initial survey was populated with a list of caregiver needs identified from a rapid review of the literature (the Delphi modification) and delivered via a Qualtrics™ online survey. The rapid review included 15 studies that explored the needs of family caregivers of children living with medical complexity and potential interventions to meet those needs. The methods of this review are attached as a Supplemental File (Appendix A). The phase 1 modified e-Delphi survey was piloted with two individuals who had previous caregiving experience before it was implemented with participants.
On the modified e-Delphi survey, participants were asked to rate how important it was to them to have a volunteer assist them meet each need on a scale of 1–5. Participants also had the option to add additional needs using an open-ended question format. Descriptive statistics were run on all items to determine consensus. Consensus was defined as items that had a mode of 3 or greater on the five-point scale, items which then continued into the second round of the e-Delphi survey. Items with bimodal distributions were handled through as follows: (1) If means were assessed as ⩾3 and ⩾50% of participants rated the role as ⩾3, then the role was included into the subsequent round or final list of roles. (2) Exceptions to 1 occurred if the study team deemed that a particular bimodal distribution may be constitutive to social factors (e.g. socioeconomic status or family dynamics), and as such, these roles were included into the subsequent round or final list of roles.
The focus group with family caregivers was conducted between round one and round two of the phase 1 e-Delphi and occurred virtually via a secure Zoom Video Communications, Inc platform using a semi-structured interview guide. The focus group was digitally recorded, transcribed verbatim, and analyzed using thematic analysis. 22 Additional needs identified by participants through the focus group were added into the second round of the survey. Data collection and analysis for the second round repeated the process used in the first round without the addition of a focus group. However, it is important to note that although additional items were added based upon the focus group findings, these items did not necessarily become part of the final consensus if they were not rated highly on the second round survey.
Phase 2 used an e-Delphi process to develop consensus on the competencies that would be required of volunteers based upon the volunteer roles identified by caregivers from phase 1. Participants in phase 2 were provided with the eight categories of family caregiver needs that a volunteer could meet as developed from phase 1 and asked to provide competencies (e.g. knowledge, skills, and abilities) that volunteers would need to meet those roles. These competencies were then analyzed thematically and provided back to participants in round two. In this round, participants were asked to rate the importance of the competencies developed in round one on a scale of 1–5 to determine consensus; competencies that received a mode of 3 or greater constituted the final set of competencies. These inductively developed competencies were further categorized into sub-competencies (general domains of learning) and learning objectives (more focused learning). Here it is important to note that the competencies were developed based upon expert knowledge of what was realistic for a volunteer to do in a supportive navigation role.
Ethics
Ethical approval was obtained through the UBC Behavioural Research Ethics Board [H21-00066]. All participants provided written informed consent to participate in the study.
Results
Twenty family caregivers participated in phase 1 of the e-Delphi survey, and 18 of those completed both rounds one and two. Four of those 20 family caregivers participated in the focus group (see Table 1 for demographic information). All family caregivers were female and mothers, half of whom were sole care providers of their children. Eight professionals participated in the phase 2 e-Delphi competency development, seven of those participated in both rounds one and two.
Family caregiver demographic information.

Phase 1: Initial identification of needs
Family caregivers in phase 1 were presented with 37 items developed from a rapid review of the literature over seven domains of needs: communication, daily life and chores, emotional support, information and knowledge, respite, support with decision-making, and sharing the caregiver experience. In the first round of responses, 28 of 37 items had modes of 3 or greater (see Supplemental Appendix C), indicating the caregivers felt these were important needs that could be met by a volunteer, and so were carried into the second round. Three roles were bimodally rated (some rated is poorly and others highly) and met qualifications to continue into the second round. Nine items that were excluded in round one was: communicating about my child’s health with extended family; communicating my child’s health needs with my other children; communicating my child’s health needs with my friends; taking care of pets; doing creative activities to reflect on experiences; connecting me with spiritual or faith-based providers; helping to take my family on special outings; helping set up virtual appointments; and sharing the caregiving experience on social media. Notably, none of the items in the domain of information and knowledge were deleted.
Focus group: Additional identification of needs
The focus group provided rich data about the needs experienced by these family caregivers. Participants discussed challenges with communicating their child and families’ unique needs to health providers. They were particularly frustrated when they had to reiterate their child’s condition to multiple care providers and over a short period of time. ‘Every 12 hours it was a different doctor. Every 12 hours I had to explain exactly what his condition was and what his baseline was. It was ridiculous’ (FCG). Participants also described feeling frustrated with complex medical terminology used by some health providers, describing such language as ‘bewildering and inaccessible’. Communicating with family could also be challenging if family members were unable or unwilling to understand the complex reality caregivers were facing. ‘I have to turn the family down all the time. . .I think sometimes they think that I’m just a party pooper and there isn’t an understanding on what kind of care he needs’ (FCG).
A prominent discussion in the focus group surrounded participants’ desire for more support in their daily-life activities and household chores. This included support with personalized tasks such as house cleaning, meals, and a range of family-centered activities. ‘I would love to have more of a deep clean. Like, someone to come in and wash the floors, that would be a huge help’ (FCG). Participants described the burden of feeling as though they were ‘triaging all day’ and facing an ‘endless pileup of tasks’. ‘It’s just hard to even make breakfast sometimes. That’s just normal for some people and they take it for granted. But, it’s hard’ (FCG). Participants suggested that having support with their daily life and chores would sometimes be more helpful than having support with caregiving for their child living with medical complexity. The importance and nature of respite constituted an important part of the focus group. Participants spoke enthusiastically of the respite available through the pediatric hospital and hospice. Respite for their other children was seen as particularly beneficial. ‘There was one point where we had a girl who volunteered to help to watch my 1-year old twins. It was amazing. I looked forward all week to that morning and for me not to feel guilty because my twins were being neglected’ (FCG).
Emotional support was another theme within the focus group interview. Participants spoke of the isolation of caregiving and wishing for someone who would just listen to them or for a support line they could call during crisis moments. ‘There needs to be a help line where caregivers can phone in those crisis moments and you can just unload and then never have to see that person again’ (FCG). Finding information about resources was particularly time-consuming and burdensome. ‘I found there’s no one telling you where resources are. I need to call like a hundred people’ (FCG). Much of their information came from other caregivers or through happenstance. Caregivers described having to search out multiple sources and continually ask questions to get the information they needed, and even then, they often missed out on resources that were available to them. ‘I didn’t realize my child had a social worker’ (FCG). Similarly, participants spoke of the importance of the pediatric care providers to their assistance with decision-making. However, they cautioned that such assistance needed to be embedded within an intimate knowledge of the family situation. Finally, participants spoke of how much they relied upon other caregivers for sharing their experiences. However, they cited some of the underlying challenges that can happen among caregivers such as poor boundaries, overcommitment to supporting other parents while juggling their own demands, and social contexts that can quickly become focused on the negative. ‘There’s always the danger that another parent will start phoning you out of despair. . .I’d get calls sometimes at midnight. . .after a while I just couldn’t do it’ (FCG).
Phase 1: Consensus on needs
Sixteen additional items were added to round two based upon family caregiver feedback in round one and data from the focus group. The following eight items were rated as unimportant (mode <3) in round two: planning for trips and travel; doing activities with me or my family to manage stress; helping with conversations about our emotional well-being and experiences; staying at the hospital with me and my child; discussing decisions about where to care for my child; coming to hospital appointments with me and my child; coming to general appointments with me and my child; supporting my child emotionally during appointments. The final family caregiver consensus on needs that could be met through a volunteer role included 36 items over 8 domains (See Table 2 for phase 1 results).
Phase 1: Final consensus on needs that could be addressed by a volunteer.

Bimodal distributions. The smallest value is shown.
Results from Likert scale of 1–5: (1) not at all important, (2) slightly important, (3) moderately important, (4) very important, (5) extremely important.
Nature of desired help
An additional objective of the modified e-Delphi survey and focus group with family caregivers was to determine the nature of help desired from a volunteer. Caregivers cited the importance of previous caregiving experience and/or training, and the traits of being compassionate, emotionally intelligent, and family-centric. Gender and age were not relevant considerations. When asked about their desired interactions with a volunteer, participants recommended regular visits on a schedule determined by the caregiver and over sufficient duration so that the volunteer could develop a relationship with the family. In home, virtual, and hospital visits were all acceptable possibilities. Concerns about the volunteer role included the potential lack of commitment in the absence of remuneration, the complexity of the child’s condition that was beyond the role of a volunteer, and a preference for support from individuals they knew as part of their social circle.
Phase 2: Competency development
The first round of the phase 2 e-Delphi, in which competencies were developed inductively, resulted in the development of 20 competencies with 62 learning objectives over 8 domains. In round two, the competencies were given back to the participant panel of experts to determine relevance/importance. No learning objectives were rated as less than 3 (moderately important in round two). Eight roles were bimodally rated (some rated it poorly, others highly), and met qualifications to continue to the final list. The study team minimally reorganized the sub-competencies in the final table to produce a set of 22 sub-competencies overarching 62 associated learning objectives for volunteer navigation curriculum development (See Table 3 for phase 2 results).
Phase 2: Final consensus on volunteer competencies and learning objectives.
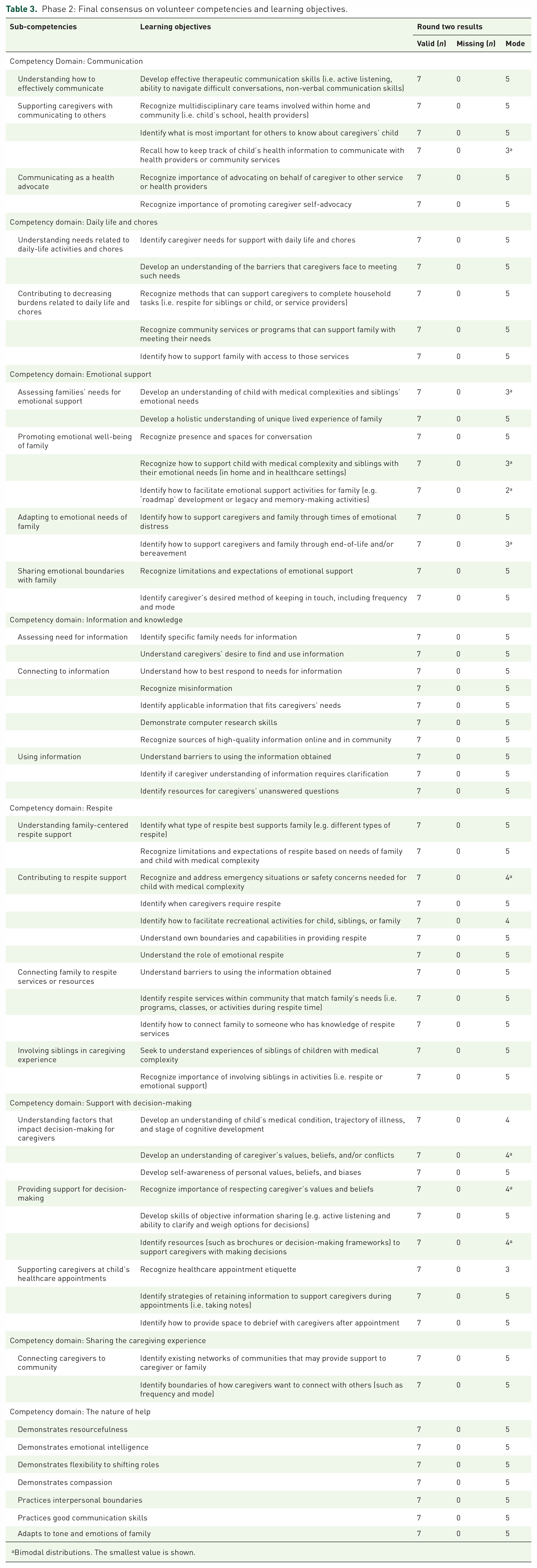
Bimodal distributions. The smallest value is shown.
Discussion
The purpose of this study was to inform the development of a volunteer role and competencies to support caregivers of children living with medical complexity. The following discussion will contextualize the findings in relation to the literature in three areas: family caregiver knowledge, communication, and decision-making; support with daily life and chores; and respite and emotional support with a specific focus on the role of the volunteer.
Knowledge, communication, and decision-making
Caregivers of children living with medical complexity face barriers to accessing information related to caring for their child and family.15,17 This lack of information makes it difficult for caregivers to communicate with others and participate fully in decision-making.10–12,16 In this study, caregivers described a range of unmet needs related to receiving information and knowledge, communicating their child and families’ needs to others, and feeling supported with decision-making.
Luke et al. 23 evaluated how a patient navigator could support parents of children living with medical complexity and found that most calls received by the telehealth patient navigator came from parents who were searching for information and resources. In the study reported here, one of the highest-rated categories in the e-Delphi survey surrounded volunteer roles that could support caregivers with finding information and resources related to their child and families’ care. Notably, all of the volunteer roles in this category were rated as greater than or equal to moderately important in both survey rounds. Furthermore, in the qualitative data, caregivers described difficulty in the search for information and knowledge, often at great cost of personal time and energy. Volunteers who are knowledgeable about the resources available for family caregivers could help to bridge these gaps in information.
This study identified the importance of improving access to the expertise that comes from other caregivers with similar lived experience of caring for a child living with medical complexity. Caregivers explained that much of their knowledge came from other parents or ‘word of mouth’. This finding supports previous literature citing the importance of peer-to-peer support for finding information.24,25 For example, Kelly et al. 24 explored how caregivers of children with complex care needs utilize peer-to-peer support through a private Facebook group. Caregivers most often utilized the group to meet their informational needs. 24 Caregivers also shared knowledge of health services and resources, such as upcoming webinars, academic articles, or news posts. 24 As such, persons with lived experience of being a caregiver for a child living with medical complexity may be particularly effective as volunteer navigators.
Previous literature indicates that caregivers face challenges when communicating with others about their child’s status and care, and this is especially true in regards to communicating with caregiver’s healthy children.26–28 Multiple studies describe how caregivers attempt to protect their children from difficult details about their sibling’s illness. 29 In turn, children return this silence, because of this discomfort and the attendant feeling that their parents have enough to worry about.26,28 This ‘reciprocal silence’ between parents and their healthy children can be detrimental to maintaining a transparent and open-relationship (p. 6). 2 During the focus group interview in this study, caregivers discussed how they were unsure of the best way to communicate with their healthy children, especially during times of distress when their sick child’s health was deteriorating. Notably, research with community-based hospice palliative care volunteers suggests that volunteers can act as a mediator for channeling information between patients and other family members.30,31 In this study, despite a thorough discussion in the focus group, the role of supporting communication with siblings did not meet inclusion criteria within phase 1. 32 Caregivers did highly rate ‘supporting my other children with being involved in the caregiving experience’, which could imply a willingness for the volunteer role in facilitating spaces for improved communication. However, this discrepancy along with the paucity of further literature on interventions or services addressing communication with siblings highlights the need for more research on this complex experience.
Family caregivers experience decision-making burden, ranging from everyday choices to life-altering decisions.8,9,15,16 In the focus group interview, caregivers described the uncertainty and fear they experienced surrounding transitionary periods in their child’s life. Specifically, caregivers described concerns with deciding what is reasonable for their child as they grow. These findings are congruent with previous literature which suggests that the needs of children living with medical complexity can shift greatly as they grow older, and decision-making can be particularly difficult during adolescence and transition into adulthood. 31 During this transition time, family caregivers tend to adopt protective behaviors, which can lead to personal fatigue and health deterioration. 9 Whether or not such precautionary measures are necessary or reasonable can be difficult for caregivers to discern, suggesting that the opportunity for caregivers to consult with a volunteer who has lived experience of these transitionary periods may be beneficial.9,16
Support with daily life and chores
Caregivers of children living with medical complexity experience a complicated home-life.8,9,18 Part of this complexity arises from the difficulty of integrating care for their children living with medical complexity with practical activities, such as cooking, cleaning, grocery shopping, and housekeeping. 8 Participants in this study described the challenges of managing their everyday lives while simultaneously meeting the needs of their children living with medical complexity. Caregivers explained how tasks, which to an outsider’s perspective may seem relatively simple, can cause considerable stress and pressure simply because of the sheer volume of things that must be done. In the e-Delphi survey, the majority of volunteer roles related to supporting caregivers with their daily life and chores were rated as important in both survey rounds. Specifically, roles related to support with housekeeping and meals were rated as extremely important to caregivers, which aligns with previous literature that caregiving for children living with medical complexity can increase the difficulty of performing and completing household tasks.8,9,18,33
Assistance with transportation and completing household tasks was perceived to be particularly helpful by caregivers in this study. Similarly, Campbell et al. 33 aimed to describe burdens faced by caregivers of children with a severe epileptic condition and identified that providing transportation and completing additional household tasks were particularly burdensome. Part of this burden is that these tasks compromise the extent of care they can provide for their children living with medical complexity as well as their normal children. Caregivers in the study expressed significant stress and guilt from being unable to optimally meet their healthy children’s needs. Factors such as time-arduous appointments and unexpected hospitalizations make it difficult for caregivers to provide due attention to other children in the home.9,18
Participants in this study suggested that a volunteer could help with their daily life and chores in many different ways. This can include helping caregivers get more time to complete those tasks themselves, having help with finding external resources for meeting those needs, or having a volunteer contribute to supporting caregivers’ healthy children. For example, some caregivers expressed that in certain situations it would be more helpful to have support with their everyday activities than to have traditional respite. This was further described by another participant who reflected on how a volunteer who had no previous caregiving experience (a high school student) was still able to provide relief and support through helping with small tasks such as folding laundry or making lunches.
Overall, having a volunteer who could help caregivers access support with their daily life and chores was a prominent aspect of the study findings. Despite the evident need for more support, few studies explore how caregivers can be better supported with non-caregiving related tasks, despite caregivers finding these unmet needs as extremely important in this study. This suggests a need for more comprehensive understandings of how the burdens of some everyday activities as a caregiver could be met by a volunteer.
Respite and emotional support
Parents who are caregivers for children living with medical complexity may experience adverse mental and physical health effects including stress, sleep deprivation, anxiety, and depression, while simultaneously facing a myriad of other personal burdens such as loss of work and deterioration of relationships.33–35 In this study, such effects were reported by caregivers as they described intersecting unmet needs related to respite and emotional support.
Respite provision is an essential service for families of children living with medical complexity; such care provision relieves caregivers of their caregiving responsibilities for a period of time. 19 Respite was consistently rated as one of the most important needs of caregivers in both e-Delphi survey rounds and the group interview. This included more traditional respite roles (someone to watch my child with medical complexity so I can sleep or leave the house) and indirect respite roles (someone to take my other children on special outings). Previous literature on respite typically focuses on a traditional model where caregivers get a break from caring for their child with medical complexity.36,37 However, participants in this study cited other opportunities to provide significant respite by freeing them to spend more time with their children living with medical complexity without worrying about tasks left undone. They further expressed that one of the major challenges in accessing traditional respite is finding someone who either (1) has expertise with caregiving and is comfortable/able to provide respite care to families of children with medical complexity, or (2) is willing to train on their child’s specific needs. Training inexperienced respite providers is sometimes too onerous to be worth it to caregivers.
Developing a volunteer role in the area of respite must take into account the unique needs of each family caregiver. The complexity of the child’s needs may make it difficult for volunteers to provide respite in the traditional sense. However, there are numerous tasks that are within the scope of the volunteer that can alleviate the burdens experienced by these caregivers. One interesting role that emerged in this study was ‘someone to help us create a roadmap to manage all our needs’. There is little empirical literature that explores this family-centered approach to care-coordination for a child with medical complexity, merging a family’s household and caregiving tasks. Most literature focus on the health-related needs of children living with medical complexities, such as hospital appointments, school, and extracurriculars.33,38 For example, Adams et al. 39 and Kuo et al. 38 describe a parent-created care-map for a child with medical complexity, displaying the multifarious activities that caregivers manage surrounding their child’s care alone. Volunteers could play a significant role by helping families to create a similar map that describes the constellation of family needs, and then having families describe the needs that could best be met within the volunteer role.
The emotional toll of caregiving for children living with medical complexities that has been documented in previous literature was also reported in this study.40–42 Emotional support is dual faceted: support for the emotional aspects of caregiving and support for the emotional well-being of the caregivers themselves. Although these two facets of emotional support are, of course, intertwined, there has been less emphasis in the literature on the emotional well-being of the caregiver. 43 As the mental health of caregivers is intrinsically tied to health outcomes of their families, there is an urgent need to have emotional support systems in place for caregivers. 44 In this study, caregivers expressed a desire to be heard and listened to when sharing their experiences, and they especially wanted to do this within a safe space where they would be understood and supported without judgment or blame. A volunteer with lived experience of caring for a child living with medical complexity could potentially meet this need, as previous literature suggests that peer-to-peer support presents a particularly safe space.24,45 However, the importance of emotional boundaries when engaging in such spaces also emerged in the focus group, a finding which was not evident in the literature reviewed. While caregivers highlighted the fulfilling nature of being able to provide information and support to others, they also described how they can come to ‘feel depleted’ when other caregivers are asking for ‘more of their time outside of workshop settings’ or are reaching out for support during times of distress. It is possible that a volunteer with lived experience could breach boundaries to also seek support for their own child or for managing personal grief. As such, support with establishing and respecting emotional boundaries may be an important aspect of training volunteers to meet caregivers’ needs for emotional support and sharing their experiences with others.
In summary, caregivers in this study faced intersecting needs related to family caregiver knowledge, communication, and decision-making; support with daily life and chores; and respite and emotional support. A volunteer with lived experience and adequate preparation can assist with meeting some of these important needs. There are limitations to these findings. First, the sample size of caregivers for the phase 1 e-Delphi was small and homogeneous. The sample was made up entirely of mothers, half of whom were sole caregivers. This is important to note in terms of transferability of the findings. What has been described is in essence the family caregiving experiences of mothers, and of those caring for their children alone. More work needs to be done exploring the family caregiving experiences of fathers. Second, there was no face-to-face interaction in either phase 1 or phase 2 in which participants would meet to discuss discrepancies, which is a common practice in e-Delphi methods. This is an important limitation because there was some disagreement between the e-Delphi and focus group conclusions in phase 1 and the expert panel in phase 2 did not include some competencies that family caregivers felt were an important role in phase 1. Third, volunteers were not part of the study sample and so their input was not obtained either in determining family caregiver needs or the volunteer competencies required to meet those needs. However, it is important to note that the expert panel included persons overseeing volunteers who worked in navigation roles with adults. We anticipate that these limitations will be addressed in future research in which we explore the feasibility and acceptability of this new role. This current study was meant to be a first step in the construction of these competencies and we anticipate that they will be further refined in future studies.
Conclusion
The number of children living with medical complexity is on the rise due to advances in treatment. As a result, parents as family caregivers are called upon to provide ever more sophisticated and intense care in the home for these children. There is a robust body of evidence about the tangible and emotional needs of these caregivers, but to-date there are few interventions designed to provide support in the home for these families. In this study, we began preliminary explorations of a volunteer role for family caregivers of children living with medical complexity. Consensus was developed on volunteer roles that could assist caregivers in the home and on a set of competencies to prepare volunteers for that role. Our next steps will be to create curriculum to prepare volunteer navigators based upon these competencies. In subsequent research we will conduct a pilot study in which volunteer navigators will be partnered with family caregivers of children living with medical complexity to assist them in the home over time. This pilot study will explore the feasibility and acceptability of the volunteer navigation intervention along with preliminary outcomes. Supportive and cost-effective interventions for this group of caregivers can make a long-term impact on child and family health and well-being.
Supplemental Material
sj-docx-1-pcr-10.1177_26323524231209060 – Supplemental material for Developing competencies for volunteer navigators to support caregivers of children living with medical complexity: a mixed-method e-Delphi study
Supplemental material, sj-docx-1-pcr-10.1177_26323524231209060 for Developing competencies for volunteer navigators to support caregivers of children living with medical complexity: a mixed-method e-Delphi study by Robyn Thomas, Barbara Pesut, Hal Siden, Michael Treschow and Gloria Puurveen in Palliative Care and Social Practice
Footnotes
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
