Abstract
One of the major dental esthetic and functional problem that occurs frequently in patients is due to gingival recession which is the apical shifting of the gingival margin from its normal position, ultimately leading to exposure of the root surface along with pain, sensitivity, plaque retention, gingivitis, loss of attachment, and root caries posing a challenge for the clinicians. This case report presents a case of total root coverage with laterally positioned flap technique for the treatment of recession defect in mandibular tooth with complete remission of dentine hypersensitivity and excellent esthetic and functional outcomes.
Introduction
Periodontal therapy is aimed toward the reestablishment of health, masticatory functions and/or the esthetics. 1 Gingival recession is defined as the exposure of the root surface caused by apical displacement of the gingival margin past the cementoenamel junction and is highly prevalent worldwide. 2 It presents one of the most common esthetic and functional problems of the periodontium and also one of the most complex regarding the etiology and the treatment modalities. 3
The etiology of gingival recession is multifactorial and the key agents regularly involved in the development of recession defects are destructive periodontal disease, 4 mechanical trauma 5 (i.e., traumatic toothbrushing and intraoral piercing trauma), anatomical conditions 6 (i.e., areas with thin band of attached gingiva, muscular inserts adjacent to the gingival margin, root prominence, inadequate thickness of alveolar bone plate, malpositioned tooth, faulty restorations, 7 high frenum attachment, and uncontrolled orthodontic movements). 4
Grupe and Warren, 8 in 1956 introduced the laterally positioned flap (LPF) technique which is one of the most predictable methods designed to solve the problem of isolated gingival recession and root denudation. However, its success is governed by the surgical design, technique involved 9 and presence of factors such as thick keratinized tissue and tissue biotype which greatly influence the final outcome. Studies revealed a positive prognosis with higher amount of baseline keratinized tissue and gingival thickness of 0.8 to 1.2 mm. 10
The aim of the present case report was to evaluate the efficacy of a modified LPF technique in treating a case of isolated gingival recession.
Case Report
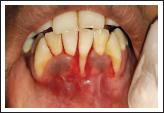
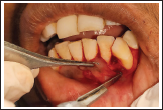
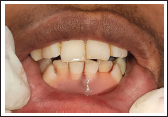
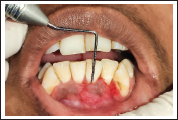
A 22-year-old female patient reported to the Department of Periodontology, Career Post Graduate Institute of Dental Sciences and Hospital, with chief complaint of receding gums and esthetic concerns along with hypersensitivity in lower front tooth region since 5 to 6 months. The patient had no relevant past dental and medical history. Intraoral examination revealed Miller’s class-II gingival recession in relation to 31 (marginal tissue recession extending to mucogingival junction and no loss of interdental bone was revealed on the intraoral periapical radiograph) (Figure 1). Recession defect depth was 4 mm and clinical attachment loss was 5 mm (Figure 2). The thickness of keratinized tissue was measured about 1.6 mm by penetrating the endodontic file with a stopper on gingival tissue perpendicularly in relation to the underlying bone surface, under local anesthesia. No carious lesions or significant wear was exhibited on the exposed root surface. The interproximal space was filled with papilla to the contact points with absence of black space. No occlusal trauma or mobility was detected with respect to the involved tooth.
IOPAR irt 31, 32, 41, 42.
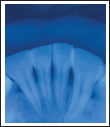
Pre-op View Showing 4 mm of Recession Defect.
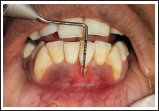
Presurgical Protocol
Patient was motivated and educated and instructions regarding oral hygiene were given. Scaling and root planing was performed thoroughly and re-evaluation of the patient was done after 1 month. Informed consent was obtained from the patient after explaining her about the surgical procedure.
Surgical Technique
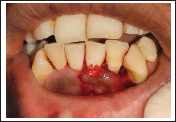
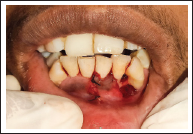
After proper isolation and anesthetizing the surgical site using 2% lignocaine hydrochloride with adrenaline (1:80,000). The exposed root surface was scaled and planed using curettes to remove plaque debris and surface irregularities (Figure 3). Root biomodification was done with the help of Diode laser (810 nm) (Figure 4). A “V” shaped incision was made using #15 BP scalpel blade around the area of recession defect and an external bevel incision was given mesially in relation to 31 followed by de-epitheliazation (Figure 5).
Root Planing of Denuded root.
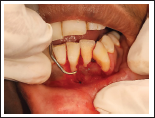
Root Biomodification Done by Diode LASER.
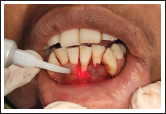
Recipient Bed Preparation.
Pedicle Flap Preparation
Satisfactory width of attached gingiva with minimal loss of bone was present at the periodontium of the donor site with no dehiscence or fenestration. A split thickness flap was reflected, half way close to the recession by giving sharp dissection using #15 blade and a periosteal elevator was used with blunt dissection to reflect the remaining half as full thickness flap. An undermining incision through the periosteum was performed at the base the entire flap for final elevation. Passivity of the flap was obtained by giving a cut back incision at the base of the flap (Figure 6) and placement of Chorion membrane was done after trimming it according to the defect size (Figure 7). The width of the flap was broader than the recipient site to cover it completely and attach it to the connective tissue around the tooth root.
LPF Elevation and Cut Back Incision Given at the Base of the Flap.
Chorion Membrane Placement Done.
Transfer of Flap
Flap was slid laterally to cover the recession defect and adapted properly without tension. Suturing was done with 4-0 silk suture to secure the flap and hold the tissues tightly against the tooth surface (Figure 8).
Sling Suture Placement.
Placement of Periodontal Dressing
Barricaid was applied and cured to protect the surgical site (Figure 9).
Barricaid Placement.
Postoperative Instructions
Postoperative instructions were given in written form. Medication of 500 mg of Amoxicillin TDS for 5 days and 400 mg of Ibuprofen BD for 3 days along with 0.2% Chlorhexidine mouthwash BD for 14 days was prescribed. Patient was instructed not to brush teeth around the surgical site during the first month after surgery followed by gentle tooth brushing with soft-bristled toothbrush. No complain of any discomfort was reported by the patient and healing was found satisfactory. Excellent colour matching with adjacent tissues with steady results at surgical site were obtained. Same results were found at 3 months follow-up (Figure 10).
Three Months Post-op View With Total Root Coverage.
Discussion
In addition to esthetic correction, complete root coverage helps in resolution of hypersensitivity and prevention of root abrasion. 11 The original lateral pedicle flap procedure 8 advocated the use of a full thickness pedicle flap being moved laterally for covering the denuded root surface but this technique was associated with increased risk of donor site’s osseous tissue exposure. Since then, various modifications were proposed, the first of which was by Grupe in 1966 12 who introduced the submarginal incision so as to avoid the risk of denudation at the donor site. This modification was evaluated by McFall in 1967 13 and Smukler in 1976 14 and it yielded a success range of 69% to 72%. Staffileno in 1964 15 replaced the original full thickness pedicle flap with partial thickness, thereby maintaining the donor area covered by periosteum. Corn in 1964 16 did a cutback incision at the base of the flap, followed by Knowles and Ramfjord in 1971 17 who performed a free graft to cover the donor area.
However, most of the root coverage procedures heal by long junctional epithelium rather than new attachment and regeneration has been observed only in the most apical portion of the lesion 8 which predisposes to high chance of recurrence. It has been reported that the use of mechanical instrumentation (scaling and root planing) leaves behind a smear layer, thereby affecting the cell reattachment which compromises the process of periodontal regeneration and repair and can also serve as a microbial growth reservoir. To overcome this, techniques such as root biomodification were introduced which aim to detoxify, decontaminate and demineralize diseased root surface, to expose the dentinal tubules and dental collagen which are supposed to be chemoattractants for periodontal fibroblasts so as to favor the joining of the Sharpey’s fibers with root collagen. Studies18, 19 have shown promising results with the use of lasers in periodontal therapy (root biomodification) to remove the smear layer and diseased cementum so as to favor new attachment and enhance the periodontal regeneration.
Placental allografts, comprised of amniotic and chorion tissues, have gained a lot of popularity over the years due to their unique inherent properties. The human chorion membrane inherits nonimmunogenic, antibacterial and anti-inflammatory properties and has also shown to enhance healing of the wound. Its matrix comprises of various growth factors such as basic fibroblast growth factor, keratinocyte growth factor, and transforming growth factor- β, making it the ideal allograft material for periodontal regeneration. 20
Advantages of using lateral pedicle graft over the other root coverage procedures are its simplicity, requirement of only a single surgical site and good vascularity of the pedicle. It offers an excellent colour matching of the graft with the adjacent tissues as observed in the present case. Whereas, the disadvantages associated this technique are the need of thick keratinized attached gingival tissue, probable sequelae of dehiscence or fenestration at the donor site and its limited application to only 1 to 2 teeth. Moreover, tension at base of distal incision and too narrow pedicle often result in cases of failure to cover the denuded surface.
Conclusion
A successful outcome was obtained by this technique with no surgical complications during or after the procedure. The lateral pedicle flap is a safe and feasible option for the surgical correction of isolated gingival recession and can be used to repair the defects of gingiva. The continuity and integrity of the zone of attached gingiva can also be re-established. However, it is important to emphasize that this case report is short term and that further clinical studies with larger sample sizes are required to provide solid evidence of complete root coverage by this modified LPF technique.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Statement of Informed Consent and Ethical Approval
Necessary ethical approval and informed consent was received and obtained respectively before initiating the study from the patient.
