Abstract
Introduction
The World Health Organization's Multi-Professional Patient Safety (PS) Curriculum (WHO-MPSC) was introduced in 2011, which made PS content easily available for nursing educators to integrate into their own curricula. With the exception of a few developed countries that have their own PS frameworks, many countries have yet to fully integrate PS concepts in pre-licensure healthcare education. The literature reveals numerous challenges when attempting to integrate new patient safety (PS) concepts. Due to the lack of updated synthesis and appraisal of these challenges, a synthesis of findings from the literature was deemed timely and significant. Hence, a literature review was carried out to comprehensively understand the challenges.
Methods
An integrative review was conducted by searching electronic databases for the years 2011–2022. The Cumulative Index of Nursing and Allied Health Literature (CINAHL), MEDLINE databases and Google Scholar were searched. The search terms were barriers, challenges, nursing students and PS education.
Results
Twenty reviews met the inclusion criteria. Through this review, investigators were able to identify 5 major categories of challenges (educators’ characteristics, administration, programme structure, curriculum, theory–practice gap) and 17 individual challenges of PS education implementation.
Conclusion
The theory-practice gap, curriculum development, and programme structure are areas that should be targeted by curriculum developers in nursing education. Furthermore, it was revealed that there is a need for further research on topics such as resistance to change and individual innovativeness among nurse educators.
Introduction
Ensuring patient safety (PS) has been erroneously centralized on the notion of improving individual performance and absolute correctness. 1 This was challenged by ‘The quality chasm’, a series of reports on healthcare safety in the United States by Institute of Medicine. In 2000, the first report, ‘To Err is human’, shifted the approach to solving PS issues from ‘naming and shaming’ the individual to making robust systems that could prevent human error. 2 This report insisted on the need to accept human fallibility in healthcare workers, which can be considered the cornerstone of the PS paradigm shift. Since then, many studies have shown the importance of introducing these new concepts and competencies of PS into healthcare professional education.3–6 The abovementioned new PS concepts include but are not limited to human factors (HFs), system factors in error, learning from error, reporting adverse events and root-cause analysis.
Since the early 2000s, PS has been a priority in healthcare education, which can be largely attributed to the quality chasm series, mandates from healthcare professional bodies and the World Health Organization (WHO). There has been a common agreement to add PS concepts in healthcare curricula. Gradually, some countries have developed their own PS education frameworks, such as Quality and Safety Education for Nurses (QSEN) 7 in the United States and the Canadian Patient Safety Education Programme (PESP). 8 The World Health Organization's Multi-Professional Patient Safety Curriculum (WHO-MPSC) 9 was introduced in 2011, and this made PS content easily available for anyone to refer and integrate into their own curricula. However, it became apparent that the integration of PS content has not achieved the momentum as expected, particularly in low- and middle-income countries. 10 With the exception of a few developed countries having their own PS frameworks, many countries have yet to fully integrate PS concepts in pre-licensure healthcare education. Hence, PS education is still considered an emerging trend. 11
It is important to understand why some countries are facing challenges when trying to integrate PS concepts. Challenges are described as something new and difficult that requires great effort and determination to overcome. 12 There is an inherent resistance to change or adopt a new movement. 13 There can be numerous challenges to change a particular behaviour and gain acceptance of a new practice. Some of the challenges highlighted in the literature regarding the adoption of PS concepts include a saturated curriculum, lack of training for nursing educators and theory-practice gap. It is vital to identify what are the challenges and why those challenges arise, in order to mitigate these challenges. Most importantly, for institutions which are planning to integrate PS, this understanding will provide a proactive understanding of what to anticipate. Hence, a literature review was planned to comprehensively understand the challenges.
Fink 14 defines literature review as ‘a systematic, explicit, and reproducible method for identifying, evaluating and synthesizing the existing body of completed and recorded work produced by researchers, scholars, and practitioners’. We could identify three (3) such literature reviews done on PS education. Sheehan et al. 15 identified both barriers and opportunities related to HF implementation through a systematic review on HF and PS in undergraduate education in health care . Barriers identified were, the lack of shared safety language, lack of faculty expertise in PS as well as the lack of an appropriate HF-based competency framework to guide curriculum development. Opportunities included increased organizational collaboration between academic and clinical settings with respect to PS teaching. An integrative literature review conducted by Tella et al. 16 has identified which PS content is being taught to nursing students at both clinical and academic settings. Her study reiterated that curriculum content is fragmented, and highlighted the importance of nurse educators’ response towards students’ errors at clinical placements. Mansour, 1 claimed that according to nursing students and faculty members’ perception, there is a need for PS friendly nursing curricula and there is a vacuum in existing curricula that need to be filled with PS content. He also highlighted the existence of theory-practice mismatch with regard to PS education. Wu & Busch 17 has listed out challenges of PS implementation, including but not limited to, all the challenges mentioned above.
All the systematic literature reviews on PS have been conducted before the WHO-MPSC was published about ten years ago. New synthesis of evidence remains due. After the publication of WHO-MPSC, many countries initiated integrating PS in their healthcare curricula. It can be hypothesized that new challenges might have emerged during the last decade. In all three literature reviews mentioned above, the main objective has not been to identify challenges of PS implementation; nevertheless, during the course of analysis, they have identified certain challenging issues related to PS education.
Due to the lack of updated synthesis and appraisal of the aforesaid challenges, a synthesis of findings from the literature was timely and significant. Through this review, the research team was able to identify 5 major categories and 17 challenges of PS education implementation. This will be explained in detail in the results section. We were able to further analyse the most reported challenges and propose means to mitigate these challenges. We could also identify areas for future research. The evidence gathered can be utilized by individuals or educational institutions to develop a proactive strategic plan to overcome these challenges.
Methods
Design of the study
Aveyard 18 recommends incorporating a review question, specific methods or strategies in the literature search, appraisal and analysis of the literature, results of the review, and a discussion with recommendations for practice to develop a comprehensive literature review. Booth et al. 19 reiterate the same by suggesting that a literature review should be carried out systematically in 4 steps, which they acronym as ‘SALSA’, Search, Appraisal, Synthesis and Analysis.
The question leading this review was, ‘what are the common challenges faced by individuals and institutions when attempting to integrate PS concepts in nursing curricula?’. The purpose of this review was to synthesize existing knowledge on the challenges of PS education for nursing students. The ultimate aim was to systematically identify the challenges of integrating PS into nursing education to provide direction for future action and investigation.
An integrative review (IR) was conducted because the purpose of the review resonated well with the intention of conducting an IR rather than other available literature review models. The IR is a distinctive form of research that uses literature to create new knowledge. 20 As elucidated by Toronto & Remington, 21 ‘the term IR is often used interchangeably with systematic review; however, there are distinct differences between them … A systematic review has a single narrowly focused clinical question, usually formulated in a PICO (P = population, I = intervention, C = comparison, O = outcomes) format and may include meta-analysis. An IR looks more broadly at a phenomenon of interest than a systematic review and allows for diverse research, which may contain theoretical and methodological literature to address the aim of the review … An IR does not include statistical synthesis methods whereas a systematic review statistically synthesizes data’.
Search methods and strategies for the identification of studies
IRs combine data from theoretical and empirical literature as well as experimental and non-experimental research to understand a phenomenon of concern holistically. This study utilized a systematic approach to database searching as emphasized by Aveyard. 18
The data search and screening were performed from October to December in 2022. The databases searched for related literature included MEDLINE, CINAHL and Google Scholar. Search limitations included were, by year 2011–2022 (10 years post introduction of WHO-MPSC), English language, and academic journal articles. The reference lists of the included studies were also reviewed to find additional articles. Google Scholar was used as a complimentary database to find literature with the support of ‘Publish or Perish’ software. 22 Keywords for the search included challenges, barriers, PS, and nursing education. To increase precision in the search process, the Boolean term AND was used to separate the keywords.
Covidence, a web-based collaboration software platform for literature reviews, was used to manage the screening process. 23 The system mandated that the two reviewers independently screen the titles and abstracts of all the retrieved documents to check the inclusion criteria. A full-text review was performed independently by two reviewers, and studies were excluded based on mutually agreed exclusion criteria.
Inclusion and exclusion criteria
Inclusion criteria
Original research papers (positivistic, hermeneutic and mixed methods), literature reviews, editorials and discussions about PS education and the challenges of integrating safety education into nursing curricula were included. Articles that generally addressed PS education without identifying challenges or barriers. Articles published without peer review. Research abstracts that did not provide access to the full text of the article. Studies that are not related to polished undergraduate education. Studies that have not been within the time limit (2011–2022) Research was only on medical education or any other allied health discipline. Nursing education-related articles that are not without any relevance to PS
Exclusion criteria
At each review cycle, Covidence synthesized the overall outcome and presented the articles with conflicts for further discussion and resolution.
Twenty (20) full-text papers were retrieved and included in the study. Eighteen (18) studies were from the keyword search and two (2) were included by manual searching of the references in relevant full-text articles (Figure 1). The list of articles was exported into an excel sheet. Themes emerging while reviewing articles were documented against the articles. First, the researcher reviewed each article several times to identify potential and actual barriers or challenges mentioned. An excel matrix was created to record the basic study details such as author, title, published year, etc. Challenges are listed in a ‘findings or conclusions’ column. Results were then analysed inductively to identify major categories and subcategories.
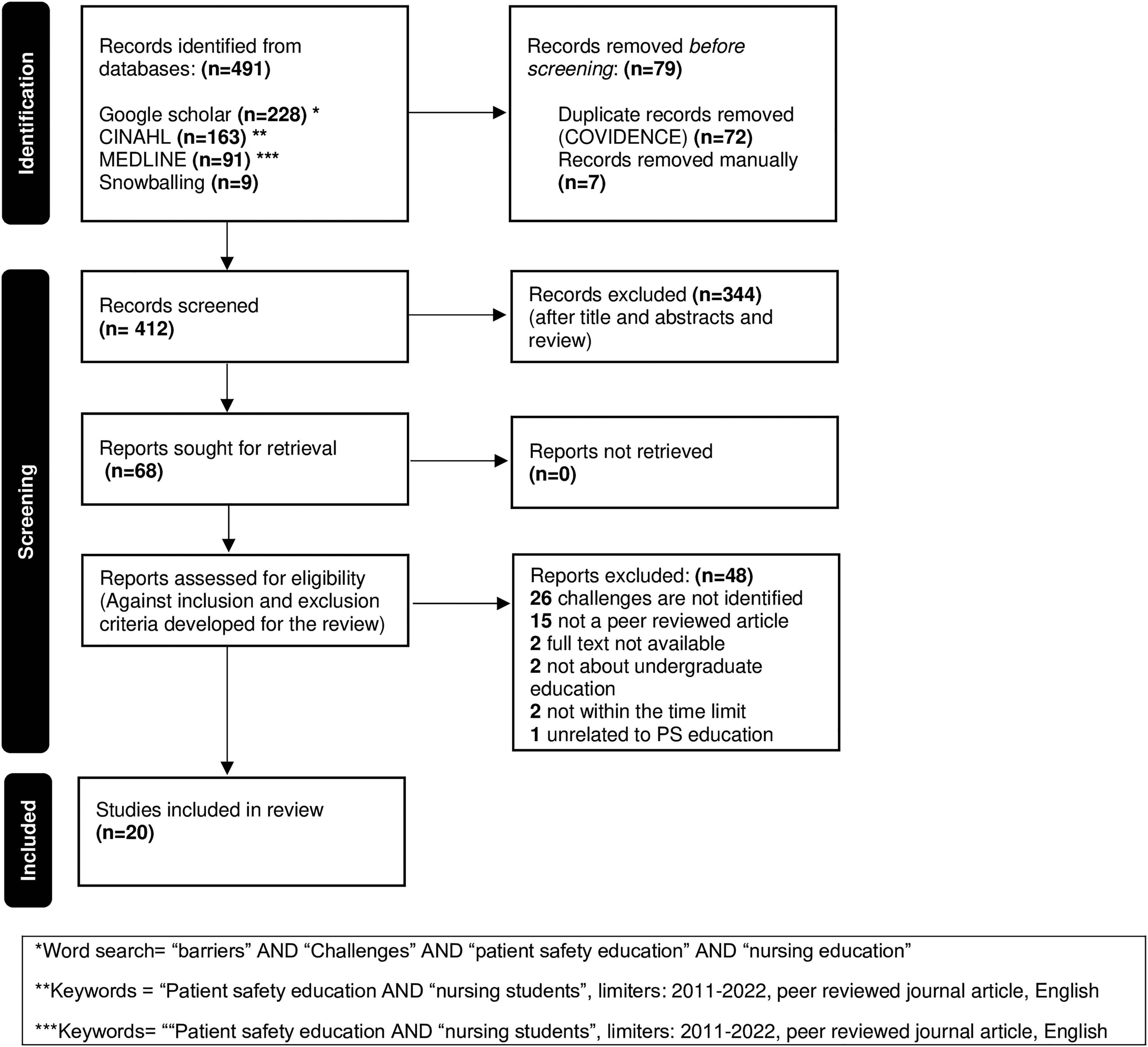
PRISMA flow diagram for article selection. From: Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ 2021;372:n71. Doi: 10.1136/bmj.n71. For more information, visit: http://www.prisma-statement.org/ ( 24 ).
Literature reviews and expert opinion papers selected for retrieval were assessed for methodological validity using The Joanna Briggs Institute's (JBI) quality assessment tools.25,26 Qualitative studies, quantitative studies, mixed method studies were assessed using Mixed Methods Appraisal Tool (MMAT), version 2018. 27 Two reviewers (AD and KD) conducted quality appraisal of the manuscripts independently and blinded to each other's ratings. Disagreements were discussed and resolved by consensus. No article was excluded due to lack of quality.
Results
Characteristics of the included studies
Twenty studies were finalized for the thematic analysis. These consisted of a vast range of study designs, which included surveys, interviews, focus group discussions, editorials, discussion papers, evaluation reports, literature reviews, systematic reviews and multi-method descriptive studies (Table 1). Five (5) major themes and seventeen (17) sub-themes emerged from these studies (Table 2). Table 3 provides an overview of the challenges identified in each article.
Characteristics and key findings of included studies
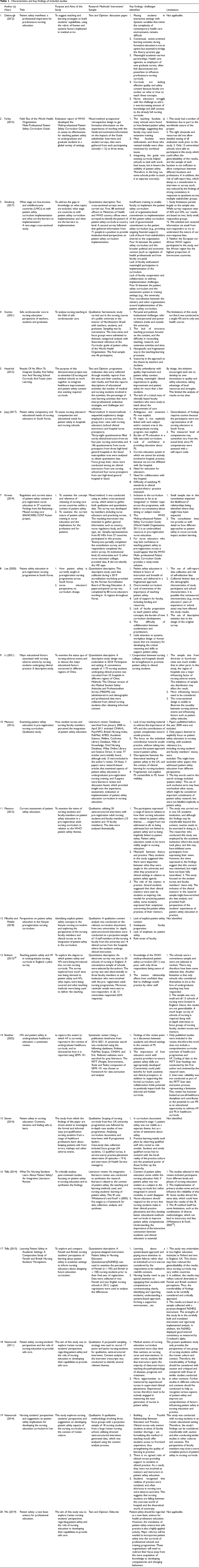
Characteristics and key findings of included studies

Major themes and sub-themes.

An overview of challenges identified.
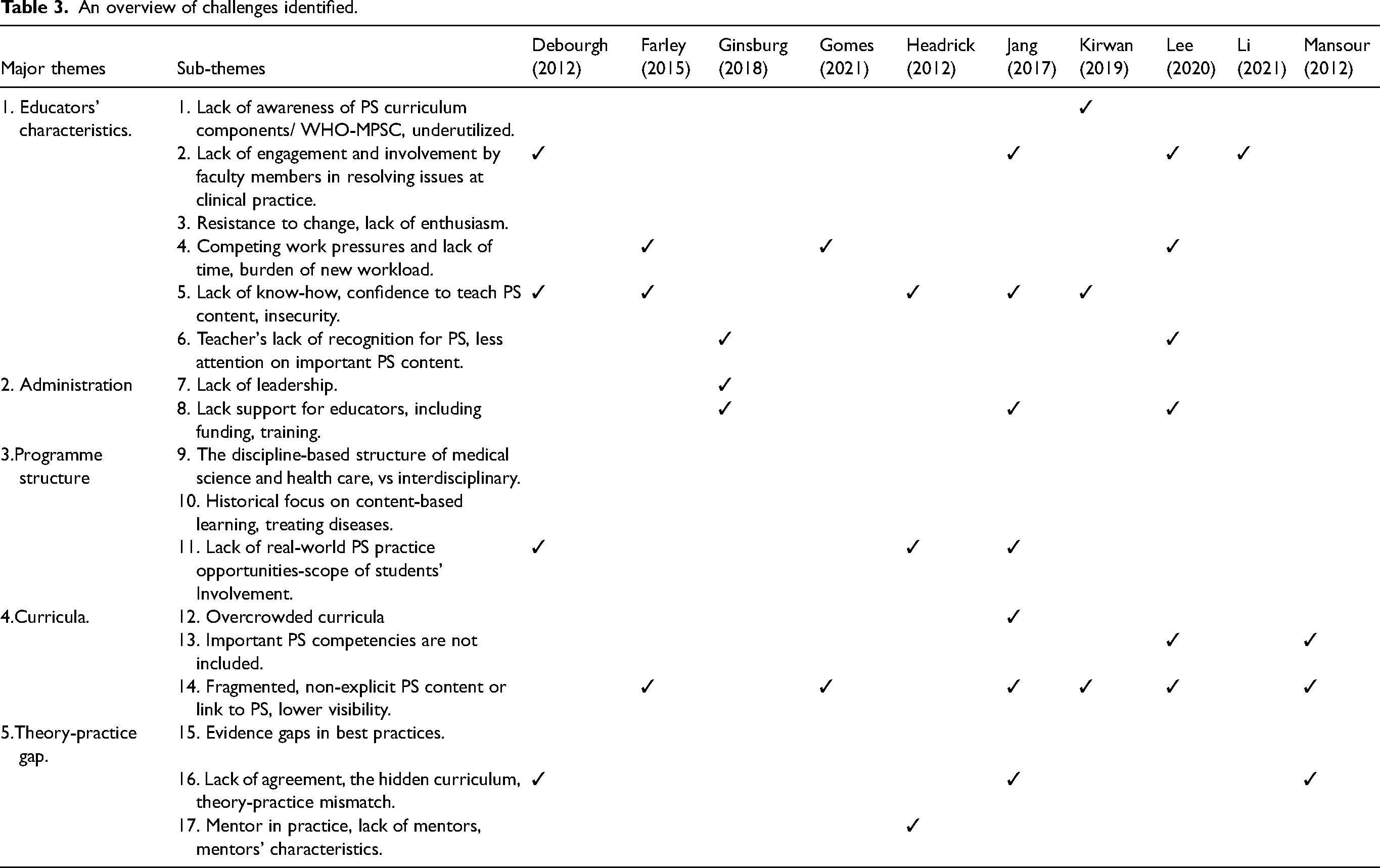

An overview of challenges identified continued.
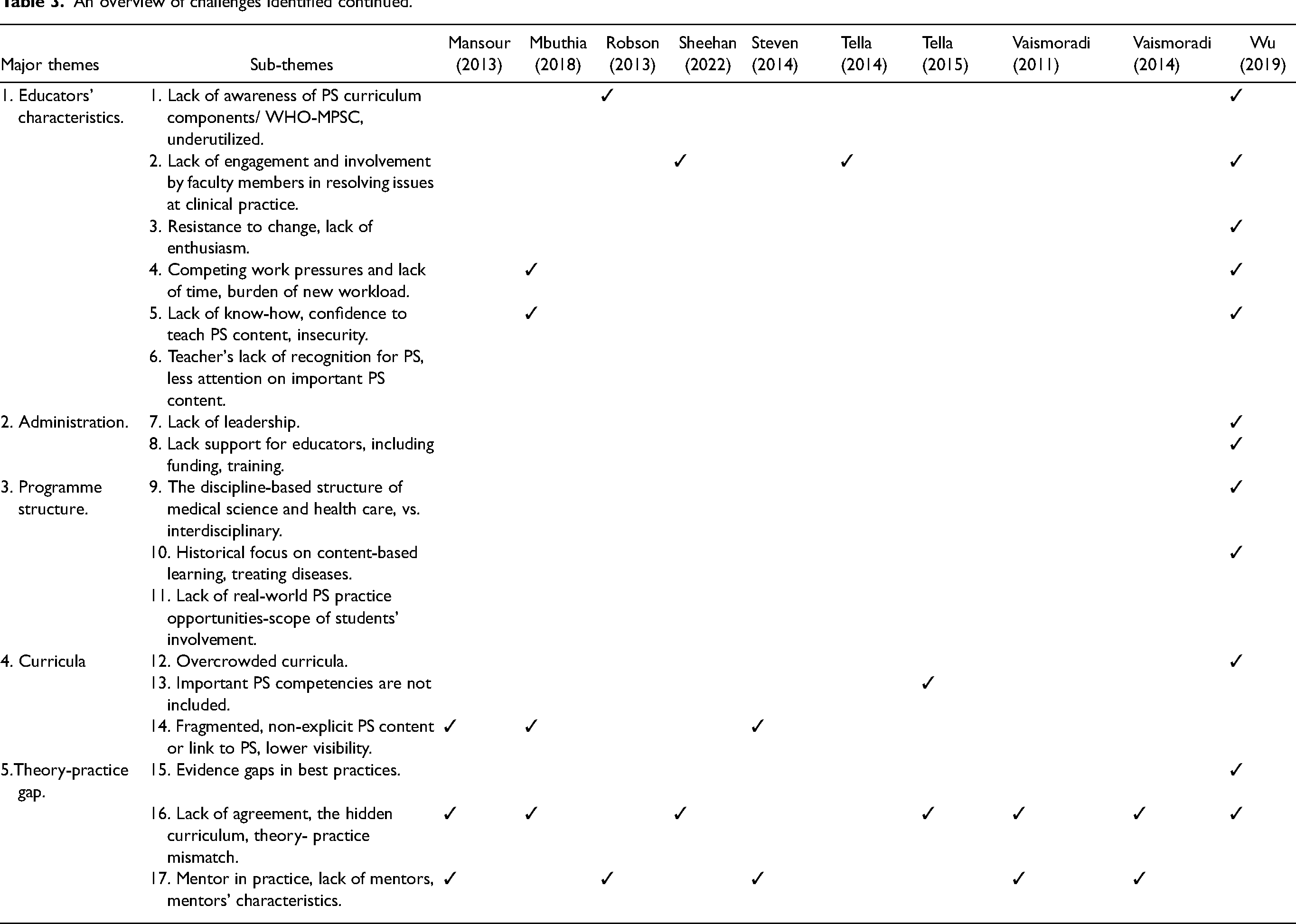

One of the common challenges identified in the literature is the tendencies of nurse educators to embrace or deviate from PS education. They almost act as the gatekeepers of deciding which PS concepts are reaching the students. Their awareness of the new PS concepts, readiness to embrace new ideas and confidence to teach are among the sub-themes identified.
Administration
The importance of support from administration to encourage PS education has been identified. Lack of leadership to embrace new PS content, funding and providing training opportunities have emerged from the literature as challenging administrative traits.
Programme structure
While acknowledging the importance given to simulations and their role as a medium of knowledge transfer, a lack of real-world opportunities to experience PS issues first-hand has been identified. In reality, healthcare teams work as teams and handle PS issues as teams. Due to the prevalence of disciplinary-based teaching, providing a realistic training experience has become a challenge.
Nursing curricula
One of the most frequently identified challenge is the non-explicit, fragmented nature of the PS content in nursing curricula. This challenge is worsening by the saturated curricula in use for pre-licensure nursing training.
Theory-practice gap
The existence of hidden curricula for PS, as with the rest of the clinical practices, and clinical mentors’ reluctance to endorse theoretical aspects of PS education has been identified as challenging. Hence, finding clinical mentors who are championing PS education is a need of the hour.
Discussion
The purpose of this IR is to synthesize existing knowledge on the challenges of PS education for nursing students.
This review identified seventeen (17) challenges from the literature that were categorized under educators’ characteristics, administration, programme structure, curriculum, and theory-practice gap. Out of the 17 challenges, the highest number of papers identified the following challenges,
Theory-practice mismatch, the hidden curriculum and lack of agreement Fragmented, non-explicit PS content, lower visibility. Lack of engagement and involvement by faculty members in resolving issues in clinical practice. Lack of know-how, confidence in teaching PS content and insecurity of the faculty. Mentors in clinical practice: lack of mentors and mentors’ characteristics
Several researchers17,28–34 have found insufficient training of faculty members to be a major challenge in integrating PS education into nursing curricula. Wu & Busch
17
argue that existing faculty may feel uncomfortable with teaching material outside their own discipline and expertise. Similarly, Jang & Lee
35
report that nursing educators express a desire for didactic lectures on PS concepts. To address this issue, Kirwan et al.
33
highlight the WHO Multi-Professional Patient Safety Curriculum Guide as a ready-made solution for meeting the training needs of faculty members. The lack of trained faculty can also contribute to the non-explicit and fragmented nature of PS in the curriculum.
If faculty members were adequately trained, they would understand the importance of PS education and could make the PS content more visible in the curricula. The literature highlights two main issues in this regard:36,37 First, when PS content is integrated into existing modules, it often lacks visibility and is overshadowed by other topics.1,32,38 Second, when PS content is presented as a separate module, there is a fear among teachers that students might perceive it as separate from their other learning, thereby neglecting the importance of PS in all modules.36,39 A possible solution to this dilemma is to introduce PS as a separate module or topic while clearly emphasizing to students that PS must be practised in all other modules and clinical settings. The objective of this module will be to consolidate fragmented PS concepts and practices to ensure visibility and comprehensiveness. If other modules already allocate considerable time to specific PS concepts, they can be briefly mentioned while focusing on unique concepts that require highlighting, such as HFs, error reporting, and root cause analysis.
Insufficient training of faculty members can also lead to a lack of involvement in PS issues within clinical settings. To enable faculty members to champion PS in both academic and clinical settings, they need to be empowered with adequate knowledge and experience in PS. Another factor contributing to this distance between academia and clinical practice is the non-practicing state of some academics. This lack of clinical engagement diminishes their confidence and credibility in assuming clinical responsibilities. Researchers have called for improved connectivity between hospitals and academia.15,40,41 Nurse educators have identified the difficulty of collaboration between academicians and practitioners as a barrier to incorporating PS into their curricula. 42 This issue has two facets: health organizations and clinical staff feeling powerless or disconnected in influencing nursing curricula 28 and academic staff feeling limited due to a lack of affiliation with hospitals. 32 To address these challenges, the authors suggest officially appointing qualified clinical staff as extended faculty members and providing affiliations to academic staff at hospitals, thereby empowering them and providing legislative protection and coverage.
The theory–practice mismatch is a recognized issue not only in PS but also in other clinical subjects.43,44 While clinical environments provide the ideal setting for practicing and refining competencies, the initial exposure to theory and procedural knowledge occurs in academic institutions. 28 Nursing students have voiced concerns that theory lessons are often oversimplified and fail to consider the complexities of real clinical practice. 38 While it is unrealistic to replicate actual clinical scenarios entirely in the university setting, attempts have been made through simulation to bridge the gap. It is crucial to clearly communicate this distinction to students, preparing them for the greater complexities they will encounter in the actual work environment.
The theory-practice mismatch leaves students feeling unprepared and low in confidence, as nurses doubt their abilities. 38 To mitigate this, it is important to convey to them that nurses do not expect the same level of confidence from students as they would from registered nurses. Students are expected to learn through observation, assistance, and gradually performing tasks based on assessment by senior nurses. Students have also observed that the realities of practice can be outdated, with shortcuts taken in nursing care due to time constraints. 45 Implementing evidence-based practice (EBP) in a realistic and context-specific manner is essential. Factors such as lack of resources, including water supply, waste segregation options, safety equipment, and limited hospital capacity, have been identified as hindrances and compromises to PS in hospitals. 36 It is crucial to strike a balance between what is perfect and what is practical, selecting approaches that suit the needs and context of the situation.
Connectivity between academia and clinical practice can help bridge the theory–practice gap. Collaborative efforts not only support the formal curriculum but also have the potential to positively influence the informal and hidden curricula. 15 The characteristics of clinical mentors can either facilitate or hinder students’ inclination toward practicing PS. Challenges in this area include the lack of available clinical mentors and mentors who do not prioritize PS practices. 34 Students expressed their enthusiasm to learn under the guidance of skilled nurses. 45 However, not all clinical nurses are effective mentors.39,46 Effective communication between academia and clinical staff is crucial in establishing mentoring support from experienced nurses. It is also important to have realistic expectations of mentors, and academic staff should be able to identify critical areas where a clinical mentor can provide support and guidance.
Wu & Busch 17 suggest that ‘resistance to change’ is a challenge when integrating PS content into curricula. However, there is a lack of in-depth studies specifically evaluating this aspect, particularly concerning faculty members. On the other hand, ‘innovation adoption’ is considered the opposite of resistance to change, as discussed by Rogers 13 and Hurt, Joseph & Cook. 47 Hurt, Joseph and Cook's concept of individual innovativeness (II) refers to an individual's willingness to change. Previous research has shown a relationship between innovation adoption and individual innovativeness. Originally studied in the field of marketing and business to understand consumer behaviour in adopting new products, the concept of innovativeness has been expanded to higher education48,49 and other contexts such as management. 50
Given the highly personal nature of II, it is reasonable to assume that the level of II among educators could significantly impact PS education as well. Therefore, it is recommended to conduct an in-depth study to investigate how the individual innovativeness of nurse educators affects the integration of PS into curricula. Such a study would provide valuable insights into the role of educators’ willingness to change and innovate in promoting effective PS education.
Conclusion
This study aimed to systematically identify the challenges reported in the literature when integrating PS into existing nursing curricula. Our approach involved utilizing various databases, with a specific focus on the 10-year period following the introduction of the WHO-MPSC in 2011. The synthesis of international literature yielded highly insightful results.
However, it is important to acknowledge the limitations of this study. First, our search was restricted to MEDLINE, CINAHL, and Google Scholar, potentially overlooking relevant evidence present in other search engines. Second, the review only considered studies published in English, potentially excluding valuable evidence published in other languages. Additionally, the chosen search terms, such as ‘challenges’ and ‘patient safety education,’ may have inadvertently omitted studies using alternative terms such as ‘barriers’ to discuss similar phenomena.
Despite these limitations, the study demonstrates several strengths. Notably, we established specific inclusion and exclusion criteria to ensure a systematic approach to article selection and minimize bias. We employed validated appraisal tools and had two independent reviewers assess the data quality individually, thus enhancing the study's rigor. Furthermore, the adoption of a two-reviewer system for screening and appraising the selected articles further enhanced the reliability and objectivity of the findings.
This study contributes novel insights to the literature by synthesizing challenges related to the education of nurses in PS and proposing strategies to overcome these challenges. It also identifies the need for further research on topics such as resistance to change and individual innovativeness among nurse educators. Furthermore, it highlights areas such as the theory-practice gap, curriculum development, and programme structure that should be targeted by global nursing education curriculum developers.
Footnotes
Acknowledgements
We would like to acknowledge all the researchers whose articles were included in the current review and the generous support by Mrs. PBMS de Silva at Monash Center for Health, Research and Implementation.
Author contributions
This review's conception and design are by DMAP. Provision of study materials and collection, assembly of data and analysis and interpretation of the data were done by DMAP and KP. DMAP drafted the article. Critical revision of the article for important intellectual content and final approval of the article was done by SSP.
Availability of data and materials
All extracted data and relevant materials are included in this article itself.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethics approval and consent to participate
The corresponding author has received ethical approval for the main study ‘A critical realist analysis of nursing educators’ concerns about patient safety education in Sri Lanka’, which this is a part of, from the Ethical Review Committee at Faculty of Graduate studies, University of Colombo (FGS/ERC/2022/013).
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work is a part of the MPhil leading to PhD study conducted by the corresponding author. The study is funded by a University Grants Commission – Sri Lanka's research grant, UGC/VC/DRIC/PG2018(II)/SJP/01.
