Abstract
Background
Trigeminal neuralgia (TN) in elderly or medically complex patients poses significant management challenges due to medication side effects, comorbidities, and limited tolerance for invasive surgery.
Cases
This case series described two elderly patients with multiple comorbidities and medically refractory TN who underwent CT-guided Gasserian ganglion injection after declining or being unsuitable for microvascular decompression or radiofrequency ablation. Both procedures were performed under CT guidance using 2% lignocaine and 8 mg dexamethasone, with no procedural complications. Patient 1 reported reduced pain intensity and medication reliance, while Patient 2 experienced complete pain relief lasting eight months, requiring a repeat injection with similar benefit. This minimally invasive approach provided meaningful symptom control, improved quality of life, and preserved independence, with a low side effect profile. Although analgesia is often temporary, repeat injections are feasible.
Conclusion
CT-guided Gasserian ganglion injection appears to be a feasible and potentially effective therapeutic option for elderly patients with TN who are unable to tolerate pharmacological treatment. Nevertheless, the current evidence base remains limited, and well-designed controlled studies are required to more clearly establish its safety and efficacy.
This is a visual representation of the abstract.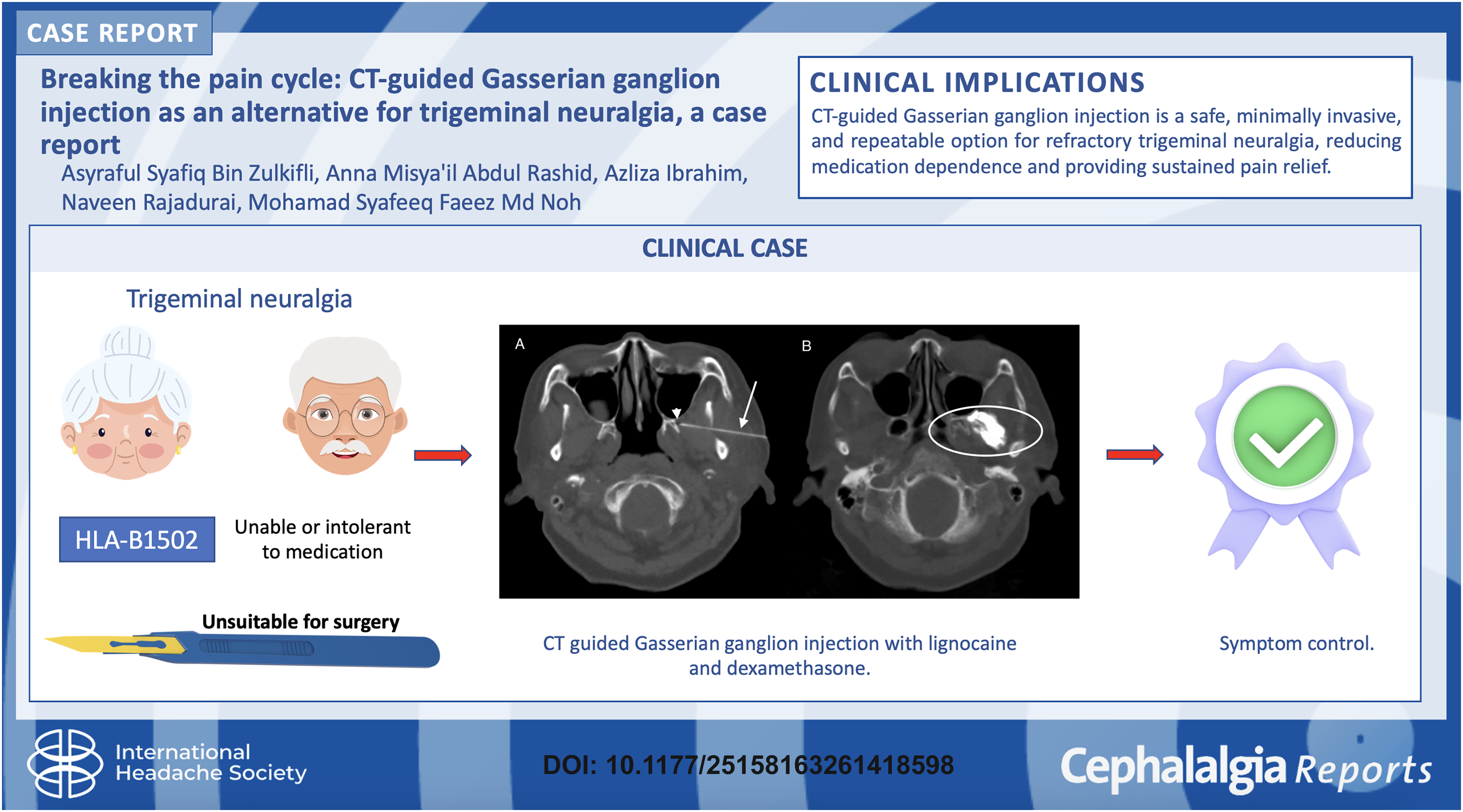
Introduction
Trigeminal neuralgia (TN) is a neuropathic pain disorder of the fifth cranial nerve, characterised by recurrent unilateral paroxysms of severe, electric shock-like pain lasting from a fraction of a second to 2 minutes, often triggered by innocuous stimuli within the trigeminal distribution and without neurological deficit. 1 The most common cause of classical TN is vascular compression at the root entry zone, usually by the superior cerebellar artery, and high-resolution magnetic resonance imaging (MRI) helps detect neurovascular contact and exclude secondary causes.1,2
Pharmacological therapy is the first-line treatment for TN, with carbamazepine and oxcarbazepine being the most effective agents. Their use, however, is often limited by side effects such as sedation, dizziness, hyponatraemia, and ataxia, particularly in older adults, and by genetic risks such as HLA-B*1502 associated Stevens–Johnson syndrome. 3 When medications are ineffective or poorly tolerated, surgical options like microvascular decompression (MVD), Gamma Knife radiosurgery, or radiofrequency thermocoagulation (RFTC) may be offered, but frail elderly patients often decline due to anaesthetic and recovery risks. 4
In such cases, CT-guided Gasserian ganglion (sensory ganglion of trigeminal nerve) injection could provide a minimally invasive alternative, delivering corticosteroid often with local anaesthetic via the foramen ovale under CT guidance. This technique can offer temporary but meaningful pain relief with a low complication rate, making it suitable for elderly or medically complex patients. 4
Case 1
A woman in her sixties with a history of repaired congenital heart disease, dyslipidemia and diabetes, presented with a 10-month history of left-sided facial pain. The pain was described as severe, shooting in nature and associated with facial numbness especially at the left V1 distribution. She reported that the intermittent facial numbness was predominantly in the left V1 distribution, occurring during pain paroxysms, with no continuous background pain, dysesthesia, burning pain, or persistent sensory disturbance between attacks. The pain was exacerbated by lying on her left side and scored 8 out of 10 on the visual analogue scale (VAS).
Neurological examination was unremarkable. Cranial nerves III, IV, and VI were intact, and motor function in all limbs was preserved. Initial laboratory investigations were unremarkable, but MRI of the brain revealed superior cerebellar arteries abutting the cisternal segment of the trigeminal nerves bilaterally, without distortion of the nerve anatomy.
She was diagnosed with idiopathic TN according to the International Classification of Headache Disorders (ICHD-3) and began medical therapy. Multiple pharmacologic agents were tried, including amitriptyline, pregabalin, gabapentin, lamotrigine, and adjunctive agents like mecobalamin and alpha lipoic acid. However, these medications provided only partial relief and were associated with excessive sedation. Carbamazepine was not prescribed due to a positive HLA-B*1502 genotype, increasing the risk of severe skin reactions.
MVD was recommended based on imaging evidence of neurovascular contact; however, the patient declined due to the invasive nature of the procedure, which required craniotomy and general anaesthesia. Being unmarried and living alone, she was concerned about the prolonged recovery period, potential post-operative pain, and the need for assistance during rehabilitation. Given these factors, she was referred to the interventional radiology (IR) team and consented to undergo CT-guided Gasserian ganglion injection, a less invasive and more practical option for her circumstances.
Case 2
A man in his seventies with long-standing diabetes mellitus, hypertension, dyslipidaemia, stage IIIB chronic kidney disease, and a history of unprovoked left lower limb deep vein thrombosis presented with a 6-month history of severe right-sided facial pain especially over the V2 and V3 distribution, scoring 9‒10 on the VAS and significantly impairing daily activities. He was diagnosed with Idiopathic TN as the MRI of the brain did not reveal underlying structural abnormality.
While awaiting the HLA-B*1502 genotype result, lamotrigine was initiated but discontinued within weeks due to a generalised maculopapular rash. Pain persisted with VAS score of 7, despite trials of pregabalin, gabapentin, and topiramate. Therapeutic doses could not be achieved owing to side effects; even on a twice-daily dose of gabapentin alone, he experienced profound drowsiness. Carbamazepine was not started in view of his HLA-B*1502 status that later returned positive.
The pain progressively worsened, disrupting sleep and interfering with mastication. Due to the unbearable pain and unsuitability for MVD, he was referred for a CT-guided Gasserian ganglion injection by the IR team.
Treatment and outcome
Both patients underwent CT-guided Gasserian ganglion injection under sterile conditions. The patients were positioned supine (head-first) with the head slightly extended. CT image acquisition included the temporal bone and paranasal sinus region to identify the pterygoid plates on the affected side. The lateral pterygoid muscle is then delineated, and its apex ‒ which lies just inferior to the Gasserian ganglion and shared innervation via the V3 ‒ is selected as the target region. Under serial CT fluoroscopic guidance aided by the scanner's laser beam, local anaesthesia (i.e., 2% lignocaine) is administered subcutaneously at the puncture site. A 22-gauge spinal needle is advanced along the laser trajectory toward the apex of the lateral pterygoid muscle using thin-slice (≈2.4 mm) CT guidance (Figures 1 and 2). Once the target is reached, 8 mg of dexamethasone is injected through a short connecting tube and low-osmolar contrast medium is subsequently introduced to confirm accurate needle placement. A post-procedural CT scan was then performed to verify correct delivery and to exclude any immediate complications; which included transient facial numbness, jaw weakness, altered corneal reflex, cheek swelling, bruising, and temporary pain exacerbation. However, neither patient experienced any of these adverse effects immediately after the procedure or during subsequent follow-up.

(A) The needle (white arrow) and its trajectory towards the apex of the left lateral pterygoid muscle (white arrowhead). (B) Contrast is seen outlining the lateral pterygoid muscle, which confirms correct placement of dexamethasone and low osmolar contrast media (LOCM) (white oval).

(A) The needle (white arrow) and its trajectory towards the apex of the right lateral pterygoid muscle (white arrowhead). (B) Contrast is seen outlining the lateral pterygoid muscle, which confirms correct placement of dexamethasone and low osmolar contrast media (LOCM) (white oval).
At two weeks post-procedure Patient 1 reported a reduction in pain score from 8 to 4, that persisted up to 4 months. Pain paroxysms were less frequent and less intense, allowing her to reduce medication use to two to three times per week on an as-needed basis. At this lower frequency, side effects were tolerable, and she was able to resume normal daily activities independently. At the time of reporting, follow-up for Patient 1 remains short-term, as the procedure was performed recently; longer-term outcomes are still being monitored. Patient 2 on the other hand, experienced complete cessation of pain following the procedure. At the two-week review, he required no oral analgesics and was functioning independently. This benefit persisted for eight months after the first injection, after which he underwent a second injection with equally effective results. Satisfied with the outcome, he declined more invasive, potentially curative surgical interventions. Table 1 summarizes the outcomes for both patients in comparison.
Summary of key outcomes before and after CT-guided Gasserian Ganglion injection.

Discussion
Managing TN in elderly or medically complex patients is challenging, as oral pharmacological agents often cause central nervous system side effects such as sedation and dizziness that increase fall risk and functional decline. The presence of the HLA-B*1502 allele further limits options, as carbamazepine and related drugs carry a high risk of severe cutaneous adverse reactions. Symptoms often worsen over time and become less responsive to escalating doses or combination therapy, making treatment complicated. 5
When medications are ineffective or poorly tolerated, procedural options such as MVD, stereotactic radiosurgery (e.g., Gamma Knife), and percutaneous rhizotomy techniques (e.g., RFTC, glycerol rhizolysis, and balloon compression) are typically considered.2,6,7 Contemporary guidelines place MVD as the first-line surgical option for classical TN with neurovascular compression, offering the highest likelihood of durable, medication-free relief. Nevertheless, the procedure entails a craniotomy with microsurgical separation of the compressing vessel ‒ typically the superior cerebellar artery ‒ from the trigeminal root, and placement of a protective Teflon pledget. While long-term pain relief rates exceed 70–90%, MVD carries risks of cerebrospinal fluid leak, hearing disturbance, stroke, and infection, which increase with age and comorbidity.2,7,8 Consequently, many frail or elderly patients decline MVD due to anaesthesia exposure, recovery demands, and its invasive nature.
Access to Gamma Knife and other stereotactic techniques is often limited by the need for specialised equipment, neurosurgical expertise, and dedicated facilities, which are typically available only in high-volume tertiary centres. 6 On the other hand, RFTC, glycerol rhizolysis, and percutaneous balloon rhizotomy are minimally invasive but neuroablative procedures; where RFTC delivers controlled thermal energy to lesion pain fibres, glycerol rhizolysis uses anhydrous glycerol for chemical neurolysis, and balloon rhizotomy achieves mechanical compression of the trigeminal root.7,9 Although these techniques provide rapid and often substantial pain relief, they carry risks of facial numbness, corneal anaesthesia, and anaesthesia dolorosa, and their availability is further constrained by technical demands, procedural costs, and concentration of expertise in specialised centres, limiting access for patients in many regions.9,10
Nerve blocks for TN remain an underused therapeutic option despite evidence of their effectiveness in providing rapid and sustained pain relief. 11 Targeted injections of local anaesthetics, often ultrasound guided, into peripheral trigeminal branches can effectively interrupt pain transmission, with relief often lasting weeks to months, exceeding the expected pharmacological duration of the drug.12,13 These procedures are minimally invasive, repeatable, and carry a low risk of adverse effects, with reported complications typically rare and mild.14,15
By contrast, CT-guided Gasserian ganglion injections are technically less complex than percutaneous ablative procedures, as they do not involve lesioning of the nerve and therefore carry a lower risk of permanent sensory deficits, anaesthesia dolorosa, or corneal complications.13,16 As compared to peripheral nerve blocks, their effect often lasts longer, between three to 6 months. These injections can often be performed by trained IRs in secondary care centres, expanding access beyond highly specialised neurosurgical units. The procedure typically involves percutaneous needle placement through the foramen ovale under CT guidance, followed by the injection of corticosteroid and local anaesthetic, offering pain relief with minimal downtime and without the need for general anaesthesia.12,13
This approach has been reported to provide clinically meaningful pain reduction, particularly in elderly or medically fragile patients for whom more invasive surgical options are unsuitable. 15 In addition, the shorter procedural time, lower consumable cost, and reduced need for postoperative monitoring make CT-guided Gasserian ganglion injections a more accessible and cost-effective intervention in many healthcare settings. Despite these advantages and favourable outcomes, the technique remains underused, often overshadowed by MVD. In the absence of access to RFTC, this procedure offers an effective, well-tolerated, and practical alternative that can significantly improve quality of life.
Although this minimally invasive approach avoids the risks of major surgery and offers an option for patients who are not suitable for or decline surgery, it is not curative, and its efficacy may diminish over time, often requiring adjunct therapies or repeat injections. Furthermore, high-quality randomized controlled trials comparing nerve blocks to other interventions are lacking, and questions remain regarding optimal dosing, duration of benefit, and long-term outcomes, underscoring the need for larger, well-designed studies.
Conclusions
CT-guided Gasserian ganglion injection may represent a safe, minimally invasive option for elderly or medically fragile patients with refractory TN who are unsuitable for or decline surgery. As illustrated in this case series, the procedure provided meaningful, though temporary, pain relief with a low complication rate, reduced reliance on systemic medications, and helped preserve patient independence. While these findings are encouraging, they should be interpreted with caution given the limited sample size. Larger, prospective studies are warranted to further evaluate the efficacy, durability, and safety of this technique and to define its role within the broader treatment algorithm for TN.
Key findings
CT-guided Gasserian ganglion injection is a potentially safe, minimally invasive option for elderly or medically fragile patients with TN who are unsuitable for or decline surgery.
This technique can provide meaningful and sustained, pain relief, reduce dependence on systemic medications, and help preserve functional independence.
The procedure can be safely repeated if symptoms recur and has a low complication rate when performed by trained operators.
Despite its favourable safety profile and accessibility in many centres, this intervention is underutilised and should be considered in multidisciplinary management discussions for refractory TN.
Footnotes
Acknowledgements
The authors thank the Director of Hospital Sultan Abdul Aziz Shah, Universiti Putra Malaysia for supporting the publication of this case report.
ORCID iDs
Ethical considerations
According to institutional policy, ethics approval is not required for case report publications. All patient identifiers were removed to ensure confidentiality, and the report was prepared in accordance with institutional and journal policies governing case report publication.
Consent to participate
Written informed consent for participation and publication was obtained from both patients, including permission to use clinical details and anonymized images.
Consent for publishing
Final approval of the article: All authors agree to publish with Cephalalgia Reports.
Author contributions
Asyraful Syafiq Bin Zulkifli contributed to data collection, analysis and interpretation and writing the article. Anna Misya'il Abdul Rashid contributed to concept and design, analysis and interpretation and writing the article. Azliza Ibrahim contributed to data collection and analysis and interpretation. Naveen Rajadurai contributed to critical revision of the article. Mohamad Syafeeq Faeez Md Noh contributed to concept and design and critical revision of the article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
The data used for this article may be obtained from the authors with a reasonable request.
