Abstract
Different methods have been reported to reconstruct groin defects brought about by hidradenitis suppurativa (HS); however, it has been challenging to achieve favourable outcomes that serve both cosmetic and functional purposes. In this report, we present a case of a groin HS defect that was reconstructed using a combination of abdominal flap and gluteal thigh flap (GTF). A 47-year-old female patient underwent extensive excision of the infra-umbilical abdominal and bilateral groin HS, resulting in a defect that was reconstructed using a combination of abdominoplasty, skin grafts, and bilateral GTFs. The use of the GTF in this reconstruction has achieved beneficial outcomes.
Introduction
Hidradenitis suppurativa (HS) is a chronic, relapsing, inflammatory disease caused by follicular occlusion usually in the axillary, inguinal, and perineal areas. 1 Clinical manifestations include painful subcutaneous nodules, sinus formation, and scarring. 1 It is hypothesized that the friction within these areas leads to terminal follicular infundibular occlusion, causing inflammation. 1 Initial treatment includes antibiotics, steroids, and biologic and hormonal therapies; however, surgery is frequently chosen for better outcomes and includes punch debridement, incision and drainage, and excision. 1 The resulting defect is repaired using secondary intention, skin graft, or regional flap. 1 In this report, we report reconstruction using abdominoplasty and posterior thigh flap.
Case Report
A 47-year-old female patient presented with a 2-year history of severe lower abdominal, inguinal, and perineal HS with massive suppurative lesions, sinuses, and scarring. She was a non-smoker and had a history of diabetes mellitus and hypothyroidism. She did not complain of micturition difficulties or fever. She had to abstain from sexual intercourse due to chronic groin pain and discharge, which significantly affected and ended her marriage, causing her to go through depression. Furthermore, she had bilateral hip movement restriction. Previously, she had a right axillary HS defect that was reconstructed using a parascapular flap. She was initially treated with antibiotics and underwent multiple incisions and drainage, which provided temporary relief. However, her condition recurred. On physical examination, her vital signs were normal and extensive scarred tissue was observed extending continuously from the lower abdominal region to the perineum (Figure 1A). Laboratory results showed the following: a haemoglobin count of 94 g/L, indicating anaemia, a slightly elevated white blood cell count (12.4 × 109/l), and a haemoglobin A1c level of 12.4%, suggesting poorly controlled diabetes. Her blood glucose levels were controlled by the medical team during her admission. Although she did not complain of any urinary symptom, her urinalysis showed leucocytosis and nitrates, indicating urinary tract infection. She was diagnosed with extensive inguinal HS and admitted to the surgical ward.
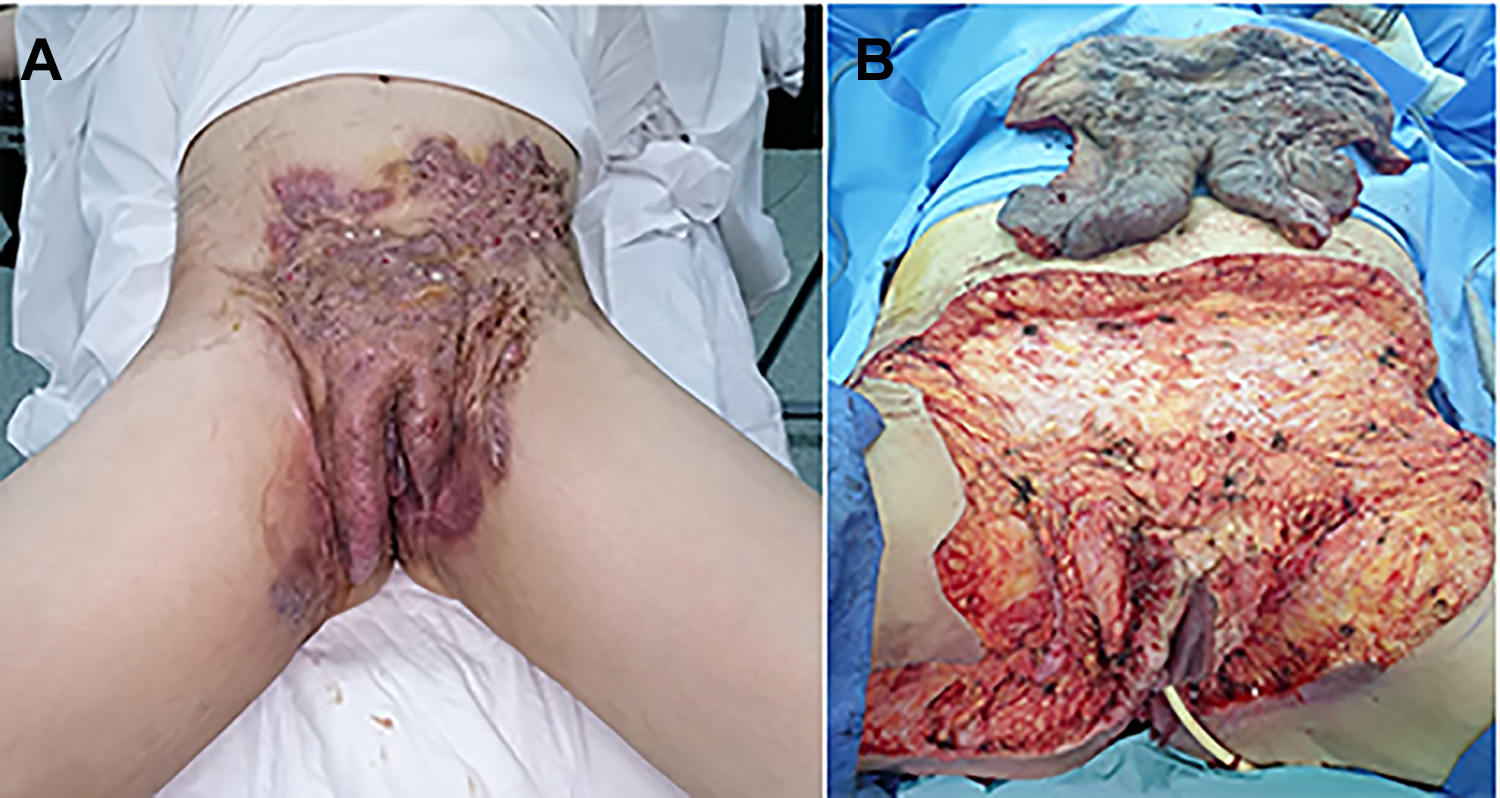
A, Preoperative assessment: extensive pelvic hidradenitis. B, Post excision of the extensive hidradenitis suppurativa lesion.
Extensive excision and debridement were performed. The specimen, measuring 25 × 20 × 3 cm (Figure 1B), was sent for microbiology and histopathology analyses, which confirmed the diagnosis of HS. Post-operatively, the patient was transfused with 2 units of packed red blood cells since her haemoglobin level was 80 g/L. Wound dressing was done daily for 1 week followed by reconstructive surgery. Colostomy was not considered as the scar tissue and the planned flap were far from the anus and the gluteal region.
Marking
With the patient lying in the prone position, the greater trochanter and the ischial tuberosity were highlighted. The midpoint between the ischial and greater trochanter marks the entry point of this descending branch of inferior gluteal artey (Figure 2). The axis of the flap was marked from the midpoint between the ischial tuberosity and the greater trochanter to the midpoint of the popliteal fossa. To preserve the blood supply of the flap, the limit of the dissection was marked 2 cm below the midpoint between the ischial tuberosity and the greater trochanter, and the endpoint of the flap was marked 10 cm above the popliteal crease.
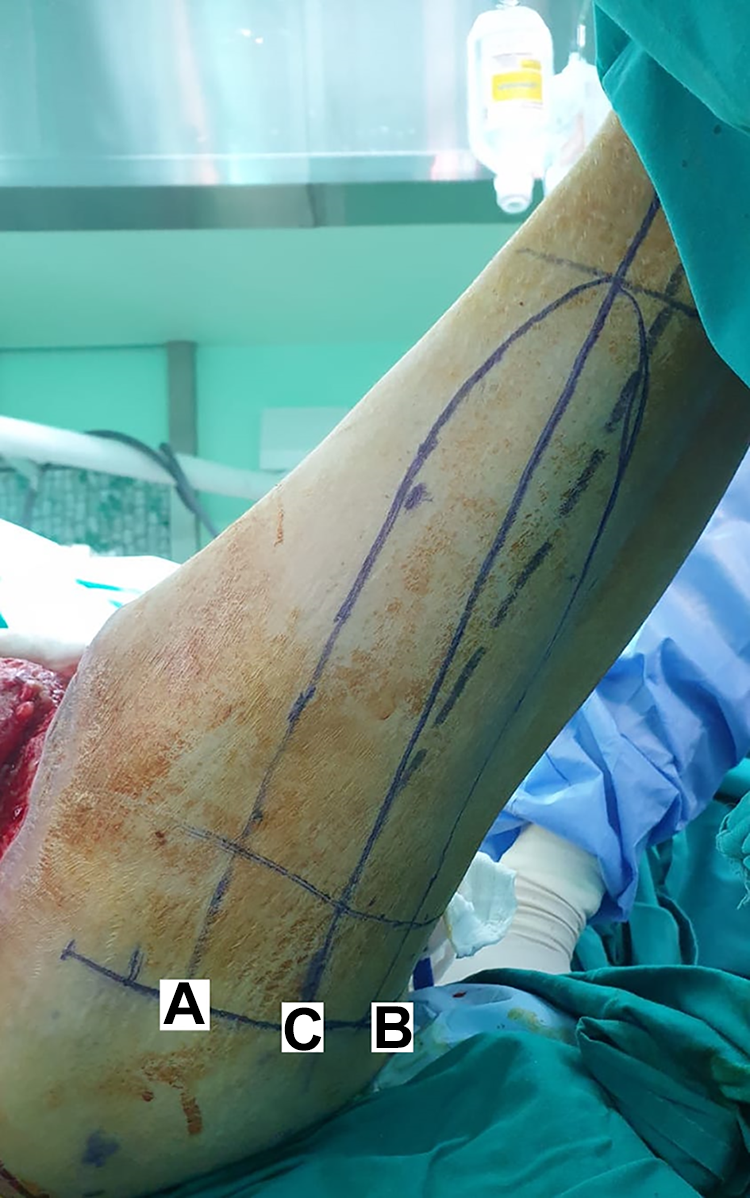
Preoperative marking. A, Ischial tuberosity. B, Greater trochanter. C, Midpoint between (A) and (B), that is, the entry point of the descending branch of inferior gluteal artey.
Surgical Technique
Under general anaesthesia, preoperative markings were made, and the patient was positioned in an exaggerated lithotomy position to increase perineal exposure. A circular incision was made around the umbilicus and the umbilical stalk was transected to the skeleton. The abdominal wall was dissected just anterior to the rectus sheath and up until the xiphoid, sparing the lateral sides. This mobilized the abdominal flap and was left to be used later.
An incision was made bilaterally on the posterior thigh to obtain the 2 gluteal thigh flaps (GTFs) after identifying the descending branch of inferior gluteal artey (Figure 3). Each flap was elevated and rotated to cover the ipsilateral groin and labia majora. The 2 flaps were then sutured together above the anterior vulvar commissure to reconstruct the mons (Figure 4). The abdominal flap was retracted inferiorly and fixed to the underlying abdominal wall. There was a 10 × 5-cm defect between the abdominal flap and the distal edges of GTFs. This exposed area was repaired using a split-thickness skin graft harvested from the left thigh. Two subcutaneous drains were then kept bilaterally in situ. There were no intraoperative complications, and the procedure took approximately 5 hours.
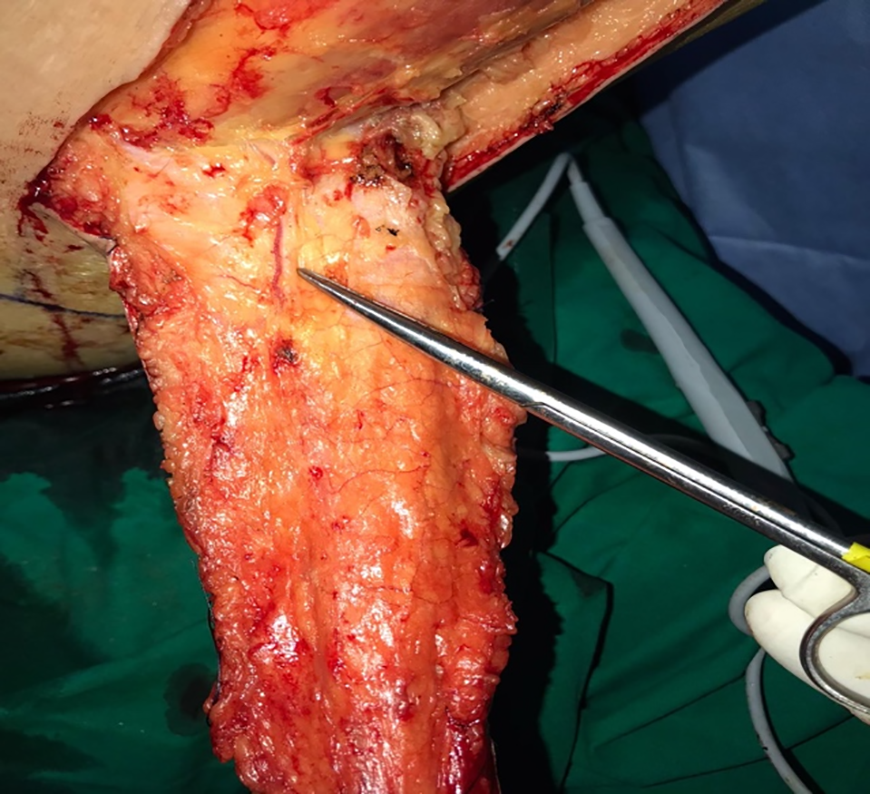
Descending branch of inferior gluteal artey.
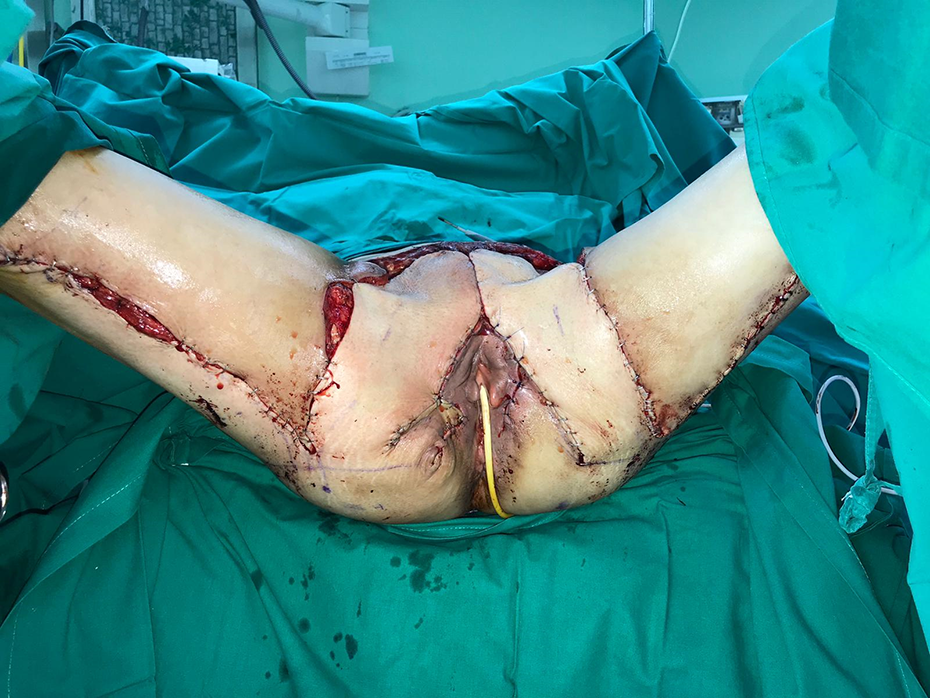
Reconstructive intraoperative result.
Post-Reconstructive Surgery
The patient was made to rest in the frog-leg position at a 45° elevation. She was immobilized for the first 4 days. She was administered a broad-spectrum antibiotic (4.5 g of piperacillin/tazobactam) and a low-molecular-weight heparin (40 mg of enoxaparin sodium), and the drains were in place for 15 days. She was kept on urinary catheter for the first 4 days which was removed after bladder training. There were no labial spreading, micturition difficulties, or hygiene issues. Dressing was changed every other day using Inadine dressing. She was then discharged and scheduled for a follow-up at the surgical outpatient clinic. Although improvement was noted, a 4 × 4 cm distal central part of the abdominal flap became necrotic, needing debridement under local anaesthesia. The wound healing was satisfactory (Figure 5A and B). Her hips range of movements improved dramatically after the surgery.
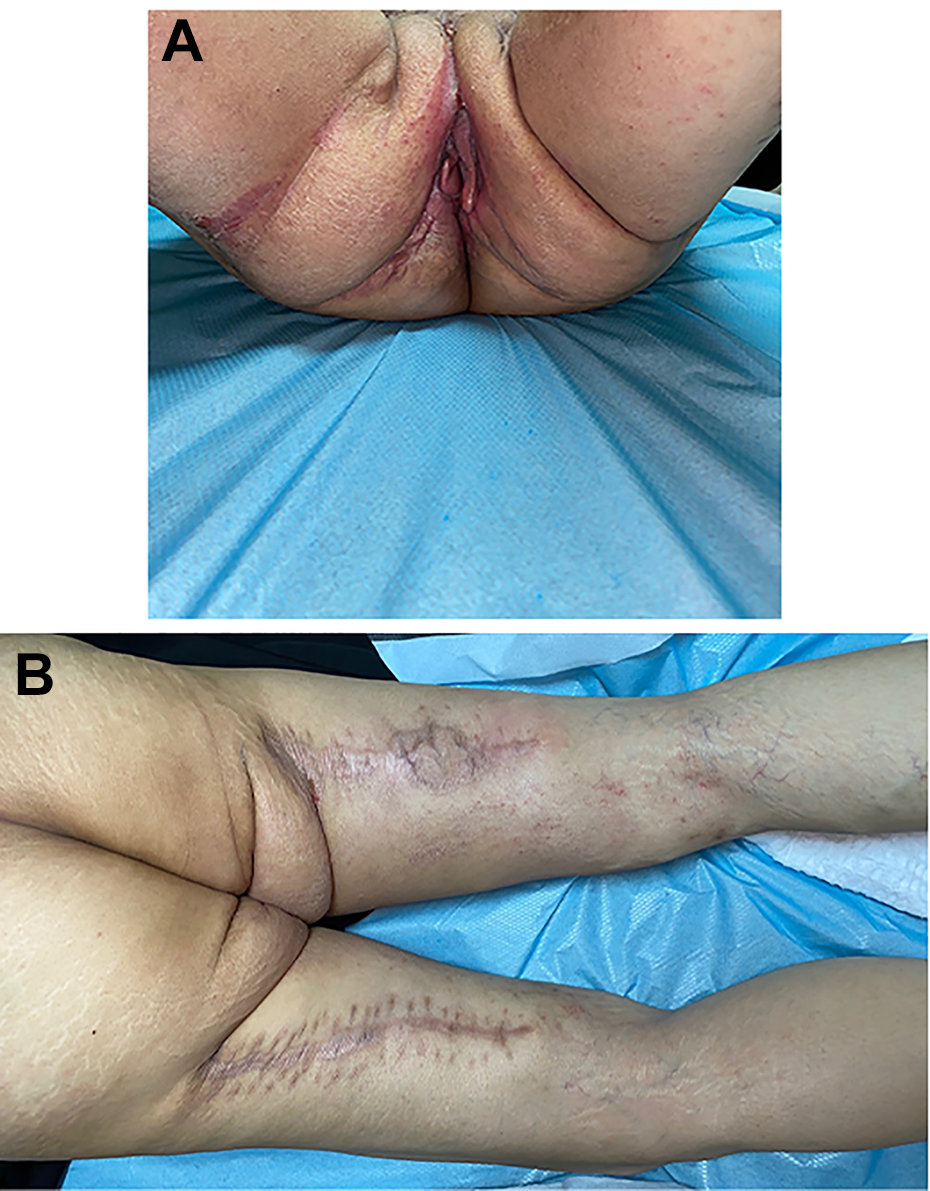
A and B, Six months post-operative result.
Discussion
Surgical management of HS leaves a large wound for which primary closure may not be possible. Wound healing can occur 1 of 3 ways: secondary intention, skin grafting, or flap reconstruction. Healing by secondary intention is preferred when wounds cannot heal after surgery, become infected, or when flaps and grafts become necrotic. 2 However, it has high rates of dehiscence at wound margins; furthermore, it requires several weeks of dressing and has a substantial risk of scar contracture and infection. 3-5
Although skin grafting is a relatively simple procedure that can reduce the risk of complications, it has been shown to cause morbidities. The procedure our patient underwent caused a significantly large defect and required a skin flap to repair and restore the sexual and excretory function of the perineal region. 6 Rapid healing is paramount, and the risk of scar contracture needs to be minimized since the perineal region is highly mobile and at increased risk of infection. Skin grafting is excluded as an option for several reasons. First, they run the risk of scar contracture, which can impair hip mobility. Second, they require complicated dressing that can cause defaecation difficulties. Third, there is delayed healing, implying long-term bed rest. 4 Finally, skin graft-shrinkage may cause dysfunction (i.e., labia majora dehiscence). This leaves flap reconstruction as the best option for groin reconstruction.
Here, we used the posterior thigh flap, which was first described by Hurwitz in 1979. 7 It is used to repair different types of defects in the gluteal, perineal, and inguinal regions 7,8 and is based on the fasciocutaneous perforator of the descending branch of the inferior gluteal artery. It is a transposition flap that is centered on the mid-posterior axis of the thigh, extending from the inferior margin of the piriformis muscle up to the popliteal region, and the width is based on skin laxity to allow primary closure, making it suitable for large defects. 9
The most commonly used flaps are the gluteus maximus and gracilis. The gracilis flap, however, has high complication rates and poor distal skin island reliability, and only its thin portion is used to fill the apex of the defect as it is tethered in the thigh by the pedicle. 7 The gracilis muscle can also be difficult to identify and isolate, especially in obese patients. 7 Furthermore, the perineal region has high shearing forces that easily disrupt the skin paddle vascularity. 7
The GTF presents several advantages over the other flaps. First, the pedicle is close to the defect, making it easier to rotate into the perineal wound. Second, the fascial pedicles are supple and durable, allowing for easy rotation. Finally, it has sensory cutaneous innervation, allowing for vaginal reconstruction. 7 It also has low postoperative morbidity and is widely accepted by patients despite open donor-site scarring. 8 Its main reported disadvantage is distal posterior thigh numbness, but this has shown to decrease over time and is well tolerated. 7 The method used for reconstruction (GTF) restored the anatomy of the external female genitalia by ensuring the presence of a wide vaginal orifice and restoring micturition, thus improving body image and self-esteem. Aesthetically, our patient was satisfied with the outcome.
Conclusion
Perineal HS can cause severe pain and discomfort, and chronic cases often require surgical excision. Depending on its extent, perineal surgery can result in a substantial skin wound, which is best managed with flap reconstruction, having rapid wound closure and minimal scar contracture risk. GTF use is recommended because of ease of manipulation, presence of sensory cutaneous innervation, and favourable patient outcomes.
Footnotes
Informed Consent
Written informed consent for patient information and images to be published was provided by the patient.
Authors Note
Mahmoud A. Abdullatif is also affiliated from Department of Plastic Surgery and Burn, Faculty of Medicine, Al-Azhar University, Almokhayyam Aldaem Street, Nasr City, Cairo, Egypt.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
