Abstract
Paramedian forehead flaps (PMFFs) are commonly performed procedures for the reconstruction of complex nasal defects and require multiple stages predicated on when the interpolated pedicle is no longer required to provide perfusion to the neo-nose. As the presence of the pedicle is disfiguring, the flap is therefore divided ideally as soon as safely possible, but that determination is challenging. Recently, a novel device that uses near-infrared spectroscopy (NIRS) to measure tissue oxygen saturation has been developed and may provide an accurate and cost-effective tool to assess tissue perfusion. Here we present the use of this technology in the management of 2 patients who underwent successful oncologic nasal reconstructions using PMFFs. Using the device as a clinical adjunct, we measured tissue oxygen saturation values in the flaps before and after pedicle division, which assisted us in deciding when to safely divide the flaps, as well as with post-division management, particularly when a low tissue oxygen saturation reading ultimately necessitated the use of nitroglycerine past to improve flap perfusion in one of our patients. Interestingly, the values we recorded corresponded well to previously published cut-off values for adequate tissue perfusion, which have to date only been reported for free flaps. To our knowledge, this is the first description of the use of NIRS in the division of PMFFs, which we overall found to be a useful and reliable adjunct to a clinical examination in assessing flap neovascularization.
Keywords
Introduction
The paramedian forehead flap (PMFF) is a mainstay in the reconstruction of complex nasal defects. 1 They require an essential delay between initially raising the flap to cover a defect and the division of the pedicle in order to allow for neovascularization of the flap from the recipient tissue bed. 2 Although necessary, the delay between stages of a PMFF reconstruction leaves patients with a prominent pedicle that interpolates from the supratrochlear source artery at the brow level and passes over intact skin to cover the destination defect of the nasal tip, ala, sidewall, or other missing subunits. This extra-anatomic trunk can affect functional aspects of daily life, such as driving and wearing glasses, as well as causing some patients to socially isolate themselves due to cosmetic concerns. 3,4 This presents a management challenge to the surgeon, in that the patient desire to minimize the delay period must be balanced with the time required for sufficient flap neovascularization.
In current practice, the PMFF pedicle remains connected for approximately 3-4 weeks, after which the surgeon assesses whether there is sufficient neovascularization for division. 5 Some surgeons prefer an intervening flap thinning stage to minimize the bulk of the reconstruction, thus increasing the intervening time. 5 Neovascularization is traditionally assessed through a clinical examination of flap perfusion after temporarily occluding the pedicle manually and assessing capillary refill, colour, and temperature. 2 Confirmation of adequate neovascularization avoids premature division that could lead to necrosis of the flap, thus impacting patient outcomes and requiring additional surgery. To aid in decision making, various adjunctive technologies to assess tissue perfusion exist, including indocyanine green (ICG) angiography, microdialysis, and laser Doppler flowmetry. 6
We present the use of a novel device developed in Alberta, Canada that uses near-infrared spectroscopy (NIRS) to measure tissue oxygen saturation (StO2), which we had previously used in a prospective cohort study on skin flap necrosis. 7,8 This handheld highly portable device allows for almost instantaneous measurements of StO2, which are obtained by holding the device 30 cm from the surgical site and pushing a button. It can be easily incorporated into both the clinic and the operating room (OR), with minimal disruption to the surgical workflow. Use of the device is also non-invasive for patients, as it does not require contact or the use of injectable dye.
Following are reports of 2 patients undergoing oncologic nasal reconstructions using PMFFs with the aid of a NIRS device, the Kent KD203 SnapshotNIR (Kent Imaging Inc, Calgary) as a clinical adjunct to prospectively assess flap perfusion and tissue viability pre, intra and post-operatively, including clinical follow-up assessment. This device is already approved by Health Canada for measuring tissue oxygenation, therefore institutional ethics approval was not required for use of the device. To our knowledge, the application of this technology in the division of a PMFF has not been previously described in the literature, which has thus far primarily focused on flap inflow and outflow issues, rather than assessing neovascularization.
Case Presentations
Patient 1
An 87-year-old female underwent Mohs excision of a basal cell carcinoma that created a complex defect inclusive of the nasal tip and left ala (Figure 1). Following excision, she was brought into the operating room for evaluation and reconstruction of the defect, which required auricular extranatomic cartilage grafting, a right PMFF, and a full thickness skin graft applied to the raw surface of the PMFF.
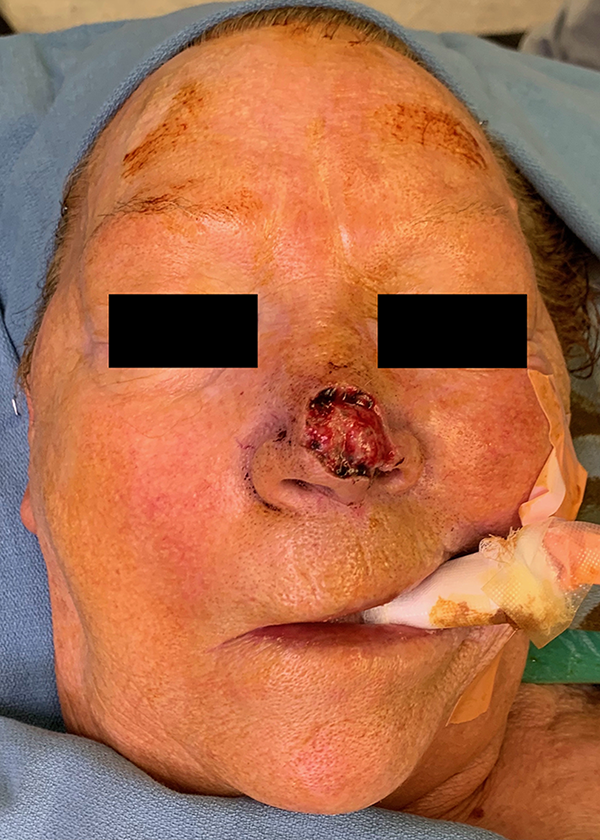
Pre-reconstruction image of the first patient.
The patient returned to the OR 33 days following the first procedure for division of the pedicle and inset of the flap. The NIRS device was used to image the flap prior to pedicle occlusion and initial StO2 measurements ranged from 73-84% (Figure 2). The pedicle was occluded with a Penrose drain and the flap appeared to perfuse well clinically, with good colour and capillary refill. Repeat StO2 measurements decreased to between 68-78% (Figure 3) with pedicle strangulation. After several minutes of continued occlusion, we were satisfied that the flap was perfused independently. The pedicle was then divided; the flap was inset; StO2 measurements remained between 68-78%.
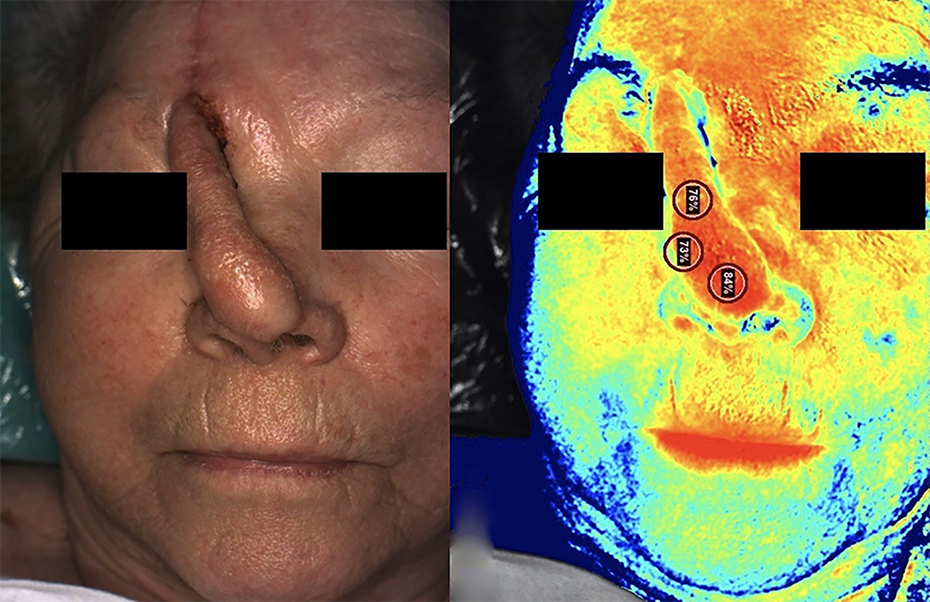
Pre-operative images of the first patient prior to pedicle occlusion showing (left) the colour image and (right) the corresponding StO2 image.
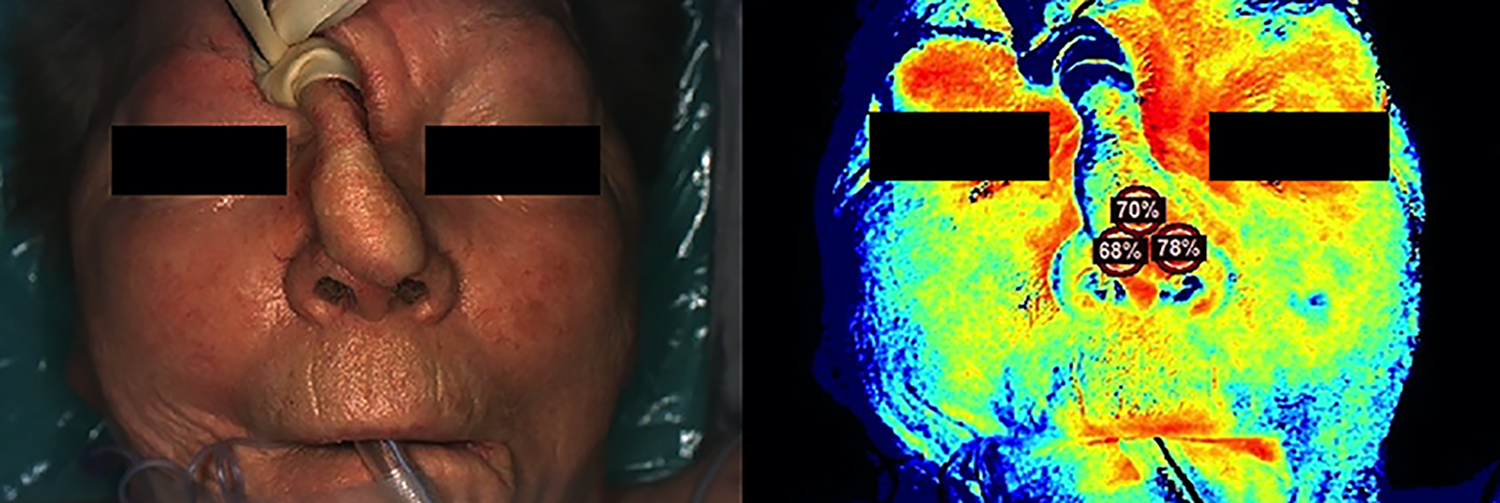
Intra-operative images of the first patient during pedicle occlusion, showing (left) the colour image and (right) the corresponding StO2 image.
Careful flap assessment was carried out in the post anaesthesia recovery unit (PACU). Repeat StO2 measurements were 65% in the distal portion of the flap but decreased to 36% in the area closest to the divided pedicle (Figure 4), while on clinical examination, this portion of the flap appeared pale. Considering this low tissue oxygen saturation close to the value of less than 30% that represents vascular compromise in free flaps, the abrupt drop in oxygen saturation of greater than 20% from the operating room, as well as the flap’s pale appearance, we decided to use nitroglycerine paste to improve perfusion. The patient was discharged home and presented to follow up 2 days later. On examination, perfusion of the superior portion of the flap had normalized, exhibiting good colour and capillary refill; the rest of the flap continued to appear well perfused. A final set of NIRS images demonstrated an increase in StO2 ranging between 72-79% (Figure 5). The patient’s further follow up appointments were uneventful, and the flap healed without complications (Figure 6).
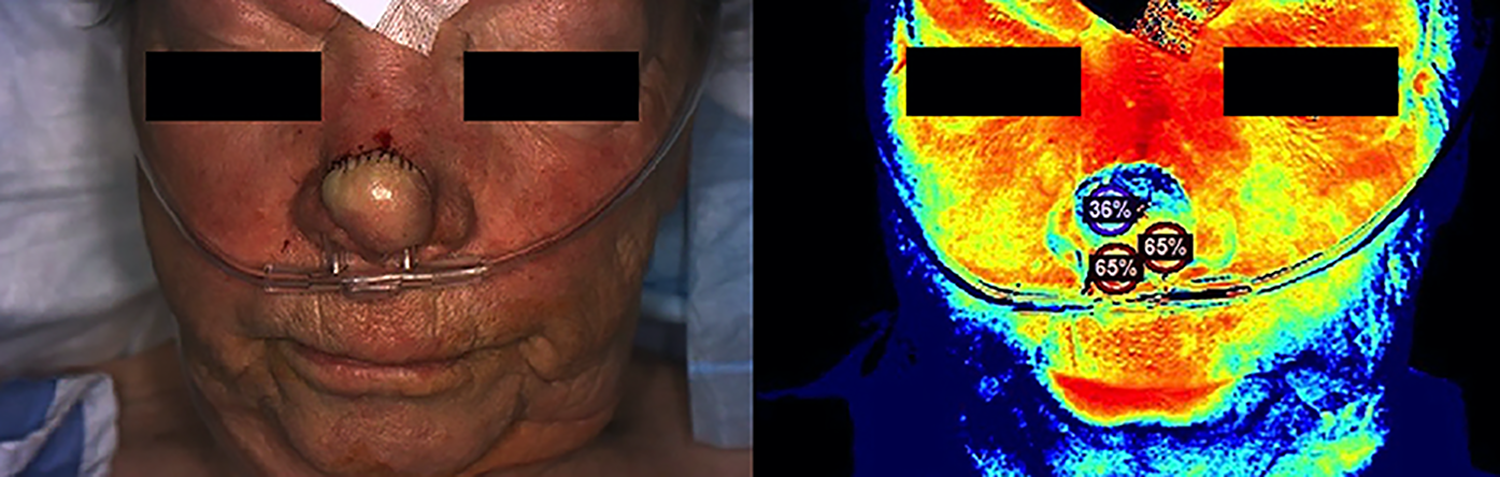
Post-operative images of the first patient in the PACU, showing (left) the colour image and (right) the corresponding StO2 image.
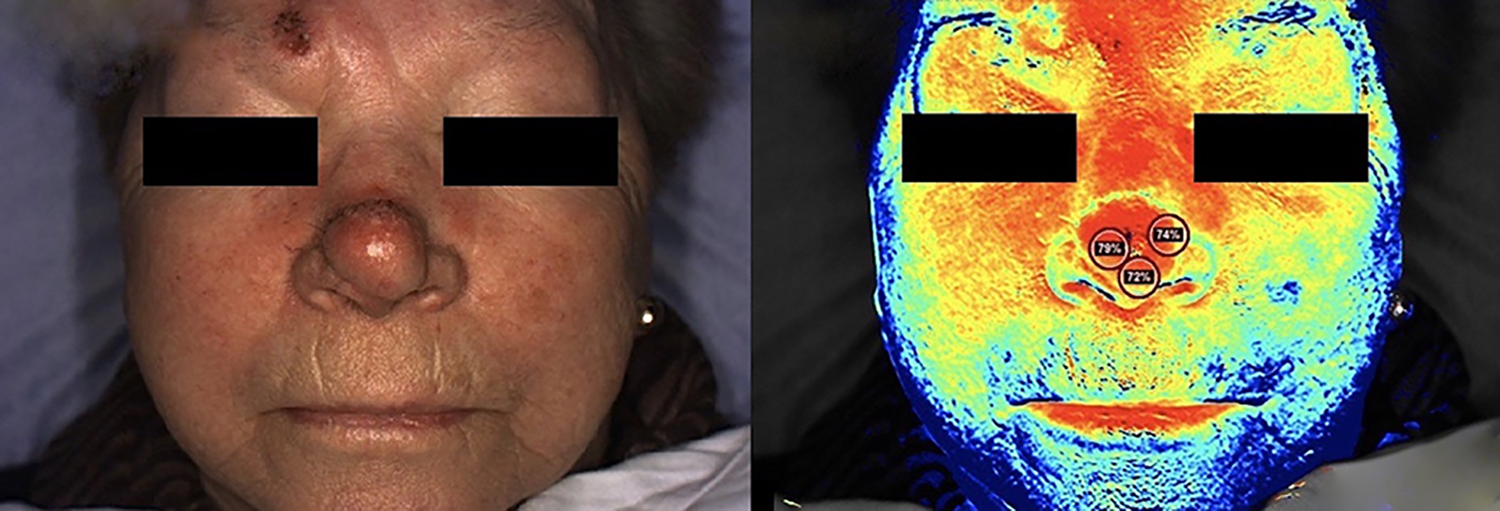
Follow-up images taken 2 days post-operatively of the first patient, showing (left) the colour image and (right) the corresponding StO2 image.
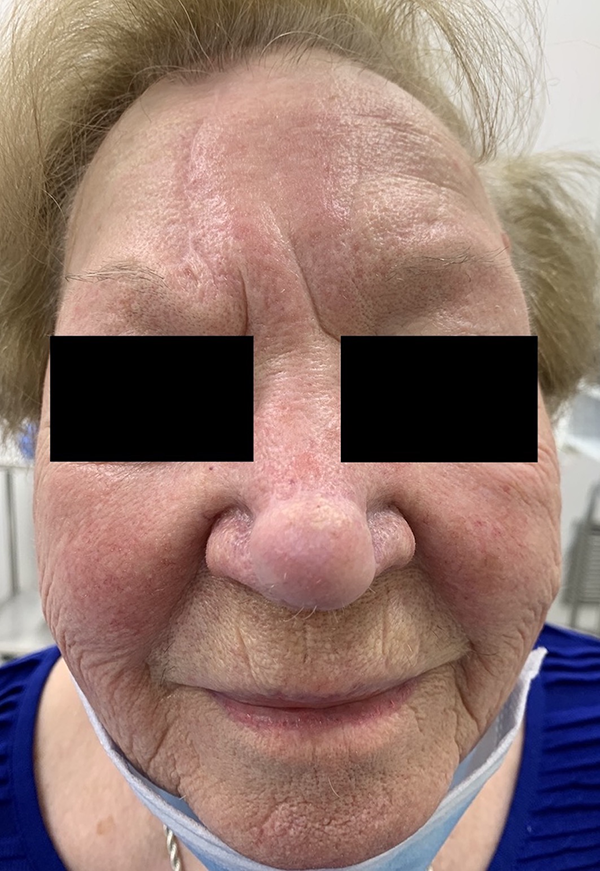
Five-month follow-up image of the first patient.
Patient 2
A 65-year-old female underwent Mohs excision of an in-situ melanoma that created a defect inclusive of right nasal lining, ala, columella and nasal tip (Figure 7). She had her lining reconstructed with a bi-pedicled bucket-handle flap and a septal artery mucoperichondrial flap. Auricular cartilage was used to provide support, and a left PMFF, cover. A retro-auricular full thickness skin graft covered the raw surface of the PMFF.
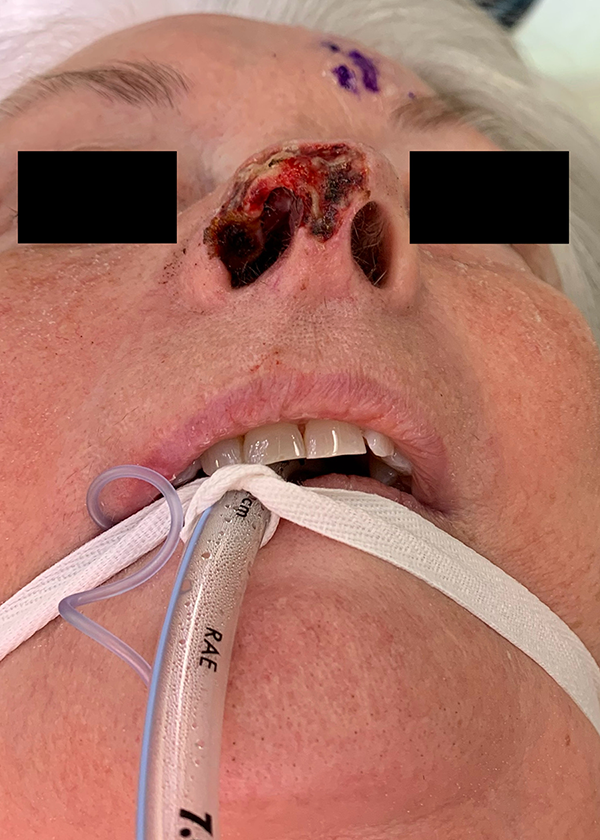
Pre-reconstruction image of the second patient.
The patient presented at 22 days after the first procedure to evaluate if the PMFF pedicle was ready for division. When the pedicle was temporarily occluded, the flap appeared pale and not sufficiently neovascularized for division. A decision was taken to proceed with her OR scheduled the following day, accepting the possibility of just thinning the flap and keeping the pedicle intact for a later division. When the patient returned to OR the next day, the flap was imaged using the NIRS device. Initial StO2 values read 80-81% (Figure 8); the pedicle was then occluded with a Penrose drain and appeared clinically better perfused compared to the previous day. When imaged with the pedicle occluded, StO2 measurements had decreased to 65-69% in the distal portion of the flap, and 59% in the area nearest the pedicle (Figure 9). Continued occlusion of the pedicle persisted for several minutes and the flap continued to have good colour and capillary refill; repeat StO2 measurements further decreased to between 44-62%. We were satisfied that the flap was perfused independently of the pedicle, so we elected to proceed with pedicle division. The pedicle was divided, and the flap was thinned and sutured into place. StO2 measurements remained between 44-62% following division.
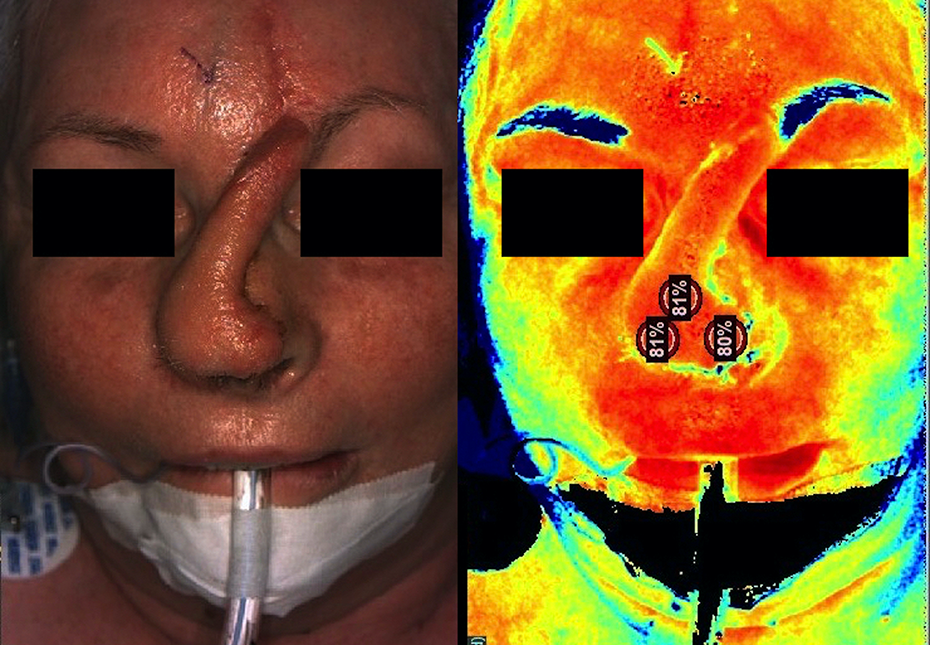
Pre-operative images of the second patient prior to pedicle occlusion showing (left) the colour image and (right) the corresponding StO2 image.
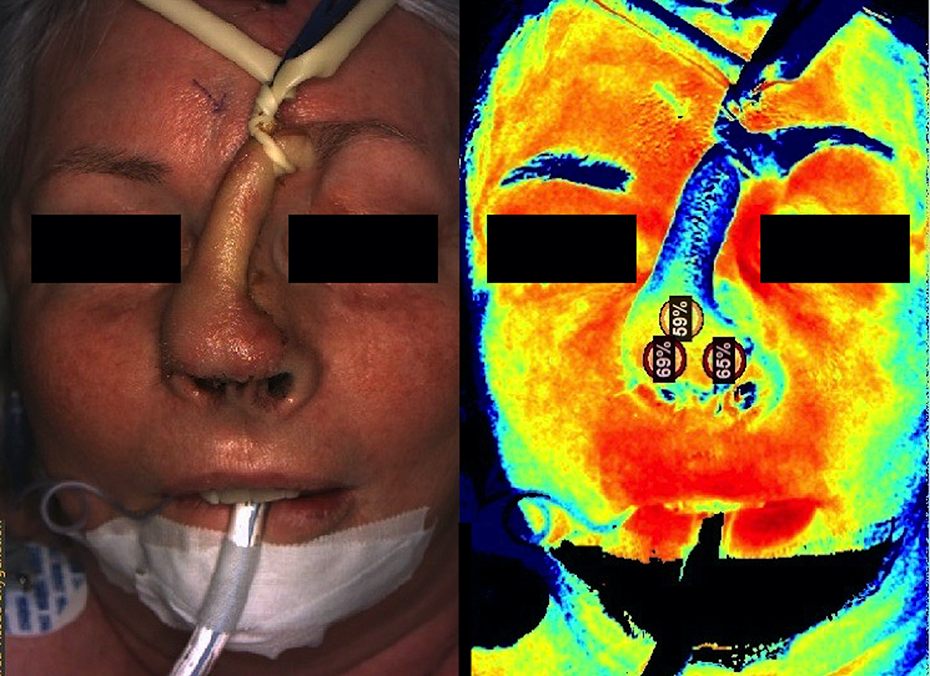
Intra-operative images of the second patient during pedicle occlusion, showing (left) the colour image and (right) the corresponding StO2 image
Careful flap assessment was again carried out in the PACU. The flap looked mildly congested, but the StO2 measurements were reassuring between 42-43% (Figure 10). After discharge, the patient presented to follow-up 2 days later and a final set of NIRS images were obtained. StO2 measurements had increased to between 64-76% (Figure 11); clinically the flap continued to appear well perfused. The patient’s further follow-up appointments were uneventful, and the flap healed without complications (Figure 12).
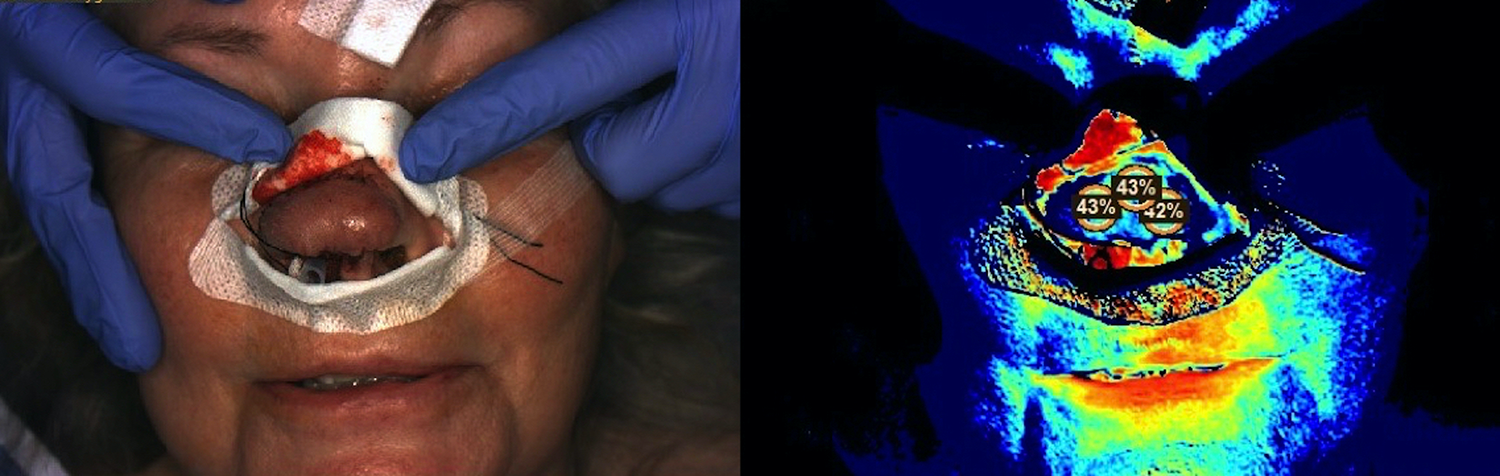
Post-operative images of the second patient in the PACU, showing (left) the colour image and (right) the corresponding StO2 image.
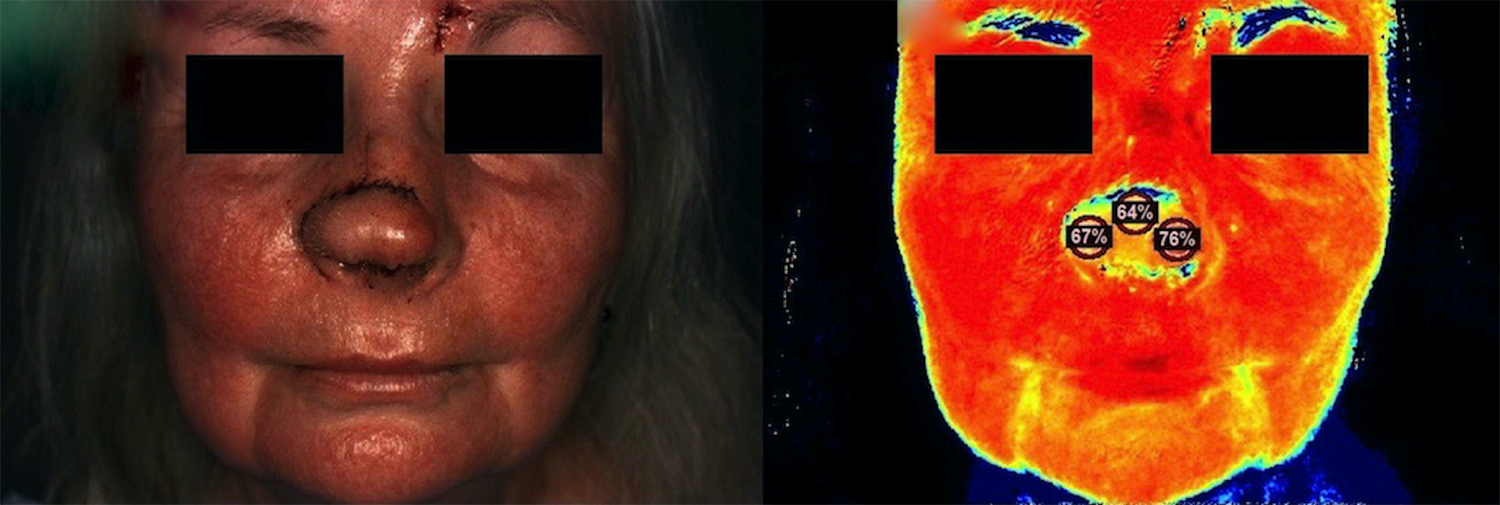
Follow-up images taken 2 days post-operatively of the second patient showing (left) the colour image and (right) the corresponding StO2 image.
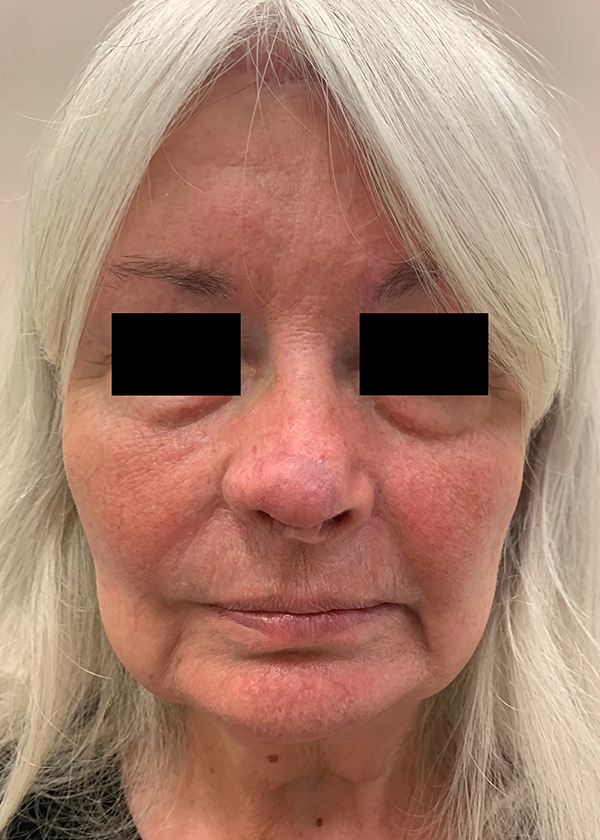
17 month follow-up image of the second patient. The photo shows the outcome following two staged revisions for debulking and shaping.
Discussion
The PMFF, an axial patterned flap supplied by the supratrochlear vessels, is a workhorse flap for the reconstruction of complex nasal defects. 3 A delay between the stages of a PMFF reconstruction is essential, as it allows for neovascularization of the flap from the recipient nasal tissue bed, while maintaining a blood supply from the pedicle. 2 There is a time honoured prescribed wait time of 3-4 weeks between stages, however this timeline can vary from 2-6 weeks depending on both surgeon preferences and patient factors. 2,4,5 Although necessary, this delay is not without concerns from patients. 100% of respondents in a survey study of patients who had undergone nasal reconstruction with PMFFs found the trunk to be “very disfiguring,” and 63% agreed that its presence greatly impeded their daily activities. These concerns resulted in all but one of the patients wishing that the trunk could be divided at 1 week, instead of the typical wait time. 4 Both of the patients reported here also found the trunk to be disfiguring, and one isolated herself from her friends, family, and the public for the duration of her reconstruction. The second patient avoided going out in public.
Despite cosmetic concerns, the pedicle cannot be divided until adequate neovascularization is achieved. Premature division can result in flap necrosis that can lead to further disfigurement, psychological stress, re-operation, and increased healthcare utilization. 9 Although the risk of flap necrosis in a PMFF is low, some studies report a rate of up to 5.4%, more commonly in patients who are smokers. 9- 11 Classically, neovascularization is assessed with a clinical examination of flap perfusion after the pedicle is occluded, based on colour, temperature, and capillary refill. 2 Along with a clinical assessment, adjunct methods of assessing tissue profusion exist, with ICG angiography and SPY technology being the most commonly described in PMFFs. Herein, we present the use of NIRS to measure StO2 as a practical and cost-effective tool in the assessment of PMFF perfusion.
NIRS was first described in 1977 by Jobsis 12 as capable of measuring tissue oxygenation and haemoglobin content through the application of optical spectrometry. To calculate a measurement of StO2, the concentrations of both oxygenated and deoxygenated hemoglobin are determined using their know absorption spectra. 13,14 To date, previous studies involving NIRS have largely focused on postoperative free flap monitoring and have demonstrated promising clinical results through the early detection of vascular compromise due to arterial occlusion or venous congestion. 13,15,16 To detect postoperative vascular compromise, criteria first proposed by Keller of StO2 < 30% or Δ StO2 decrease/h > 20% (sustained for more than 30 minutes), 17 have now been widely accepted as standard thresholds for free flaps. 15 In terms of the intraoperative use of NIRS, Hill et al recently determined that compared with baseline StO2 measurements, a mean intraoperative StO2 reduction of 17.5% following flap inset was ultimately associated with areas of skin flap necrosis. 8 It is important to note that the use of NIRS in evaluating tissue perfusion in PMFFs differs from its use in free flaps, which in the latter situation aims to detect an arterial or venous occlusion rather than assess neovascularization. Interestingly though, these free flap cut-off values corresponded well to our patients, most notably our first patient, where poor perfusion on clinical exam was reflected by a tissue oxygen saturation of 36%, which is just above the free flap cut-off value for vascular compromise. Although further research is needed, we learned from our first case that the free flap cut-off values for vascular compromise may hold true for identifying issues with neovascularization in PMFFs.
Of the adjuncts available to assess tissue perfusion, ICG angiography with SPY technology is the most commonly described in the PMFF literature. Its use in PMFFs was first described in case studies where patients underwent pedicle division based on ICG confirmed perfusion, 6,18 while later studies described the use of IGC angiography to minimize the wait time to 2 weeks between stages. 19,20 Although effective, use of ICG angiography is not without limitations. With an upfront cost of around $300 000 USD, it also requires recurrent spending on disposables such as the injectable dye, and it can increase operating time due to its more cumbersome manipulation in the surgical field. The need for injectable dye is also an additional invasive procedure for the patient and cannot be used in patients with allergies to iodine or shellfish. 6 When compared to ICG angiography, NIRS has several advantages. The device reported here costs $29 000 USD and the only recurrent cost is a sterile drape. As the device is handheld, it can be easily manipulated in the surgical field. Obtaining a reading from the device is near instantaneous, further saving time in the OR and allowing for clinical decisions to be made quickly. Use of the device is non-invasive for the patient, as there are no injectables or exposures. The portability of the device is another advantage in that it can be used throughout the reconstruction process, including pre-operatively, immediately postoperatively, and during follow up visits, increasing its utility beyond the OR.
The use of NIRS is not without limitations. The application of NIRS as described here in a PMFF reconstruction differs from its previous applications, which aimed to detect flap inflow or outflow issues, rather than assessing flap neovascularization. As this is a novel use of the technology, research is needed to determine postoperative threshold values that represent inadequate tissue perfusion. Intraoperatively, future work is also required to determine threshold values of StO2 following pedicle occlusion, prior to division and inset, that constitute a concern with neovascularization.
In this case report, we have demonstrated the utility of NIRS in the successful division and post-operative evaluation of PMFFs in 2 patients. Additional studies are needed to further confirm reliability and establish clearer threshold values in order to facilitate its incorporation into routine practice.
Footnotes
Statement of Human and Animal Rights
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2008 (5). Informed consent was obtained from all patients for being included in the study.
Statement of Informed Consent
Both participants provided written informed consent for their information and images to be published in this case report.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The authors received financial support from the Iona Martin Melanoma Fund for costs associated with the publication of this article.
