Abstract
Sweet’s syndrome, also known as acute febrile neutrophilic dermatosis, is an uncommon dermatological condition characterized by sudden onset, painful, erythematous/violaceous papules, plaques and ulcers, and specific histopathologic findings. Ulcers commonly present on the trunk, neck, hands and typically respond to systemic corticosteroid treatment. Here, we present a case of a 63-year-old woman with Sweet’s syndrome that presented with a thumb ulcer resembling a soft tissue infection. The thumb lesion was refractory to management for an infection and tissue pathology was consistent with a Sweet’s lesion. The patient was intolerant to first line therapy of oral prednisone, but the lesion was initially responsive to topical clobetasol and maintenance therapy of oral dapsone. This case emphasizes the importance of a careful history, examination, workup and maintaining a broad differential diagnosis to prevent misdiagnosis. We also demonstrate the potential effectiveness of initial topical treatment for problematic Sweet’s lesions when systemic steroids are contraindicated.
Introduction
Acute febrile neutrophilic dermatosis, eponymously known as Sweet’s syndrome, is an uncommon dermatological condition characterized by a combination of clinical symptoms, physical exam features and pathologic findings. 1,2 The etiology of Sweet’s syndrome is unclear, although it can be categorized into classical/idiopathic, malignancy-associated, and drug-induced. 1,3,4 Cases of Sweet’s syndrome are distributed worldwide with no racial predominance, and commonly present in middle-aged women with a 4:1 female to male ratio. 1,2 Classically, patients with Sweet’s syndrome may feel and look acutely unwell, presenting with an abrupt onset of recurrent fevers, painful red-purple papules, nodules, plaques, and ulcerations. The distribution is often asymmetrical with involvement of the upper extremities, face, and neck. 1 Skin lesions may develop concurrently with fever or be delayed in their appearance by several weeks. Skin histopathology demonstrate dense neutrophilic infiltrate without vasculitis. 1,2,4 -6 Associations with Sweet’s syndrome include drug-induced (classically associated with granulocyte colony stimulating factor), minor trauma, upper respiratory or gastrointestinal tract infection, malignancy, paraneoplastic syndromes, pregnancy and underlying autoimmune diseases, suggesting an irregular hypersensitivity response. 1,2 First-line treatment of Sweet’s syndrome is generally systemic corticosteroids. Topical steroids, intralesional steroids, colchicine, potassium iodide, systemic immunosuppressants, dapsone, and biologics have also been used for this condition. 1,7
Here we discuss the case of a middle-aged woman with a large Sweet’s ulcerated plaque of the thumb masquerading as an infection whose initial successful treatment was with topical corticosteroids due to intolerance of oral prednisone.
Case Report
A 63-year-old woman with a known history Sweet’s syndrome was referred to the plastic surgery service with a one-week history of evolving cellulitis and possible abscess of the left thumb. As described by the patient, the lesion began as a small boil that rapidly enlarged over 3 days. She initially received oral cephalexin from her family physician with a presumptive diagnosis of cellulitis. However, she presented to her local emergency department after a failed response to 48 hours of antibiotic treatment. Throughout this episode she had regular fevers with a maximal temperature of 39.3°C, although taken in context of regular fevers associated with her existing diagnosis of Sweet’s syndrome. On examination, there was an ulcerated, friable, exquisitely tender violaceous plaque on the dorsum of her left thumb overlying the proximal phalanx (Figure 1). The lesion was spongy in texture with no discrete fluctuance. Juicy-looking papules, nodules, and plaques were present on her forehead, while similar lesions on the neck were eroded (Figure 1). Clinical examination and radiographs ruled out associated flexor tenosynovitis and septic arthritis. Range of motion was restricted however, due to tenderness. White blood cell count was normal at 9.8 (109/L) and c-reactive protein was moderately elevated at 75.8 (mg/L).
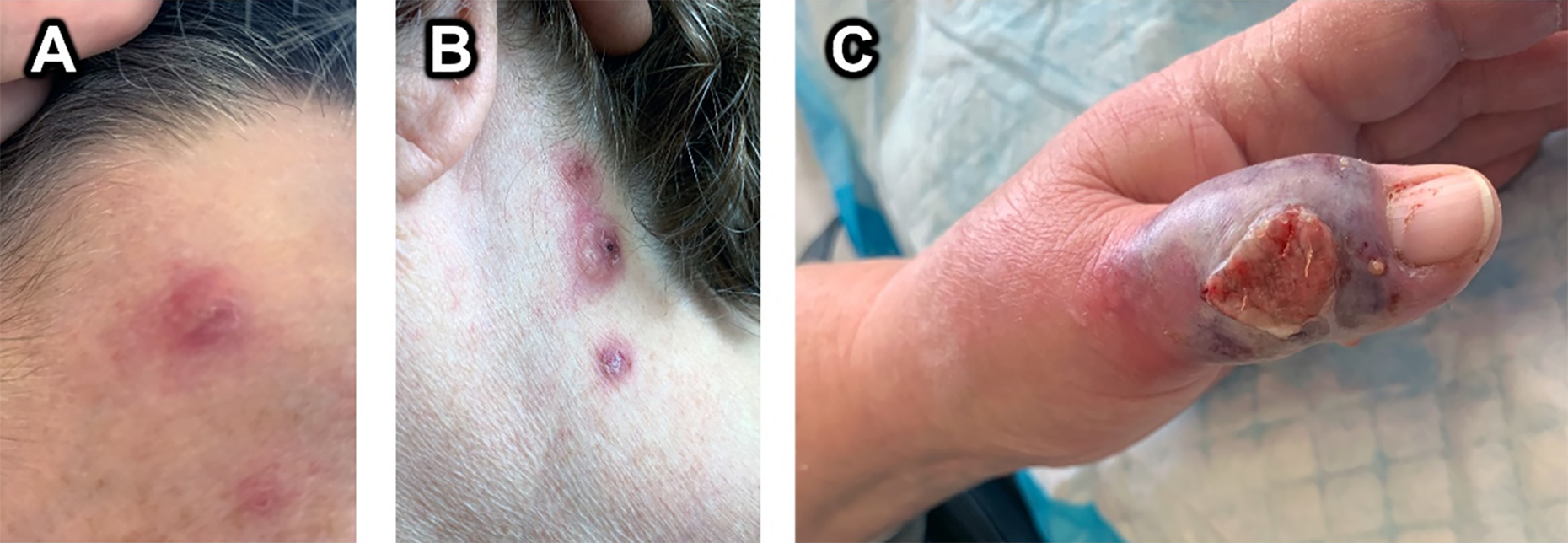
Presentation of Sweet’s lesion on left thumb, referred as concern for infection. This patient had been diagnosed with Sweet's syndrome 2 years prior after multiple episodes of recurrent inflammatory lesions throughout her body. Characteristic Sweet's lesions at the time of presentation were on the patient's right forehead (A) and left neck (B). The lesion of concern (C) features a raised, exquisitely tender, ulcerative mass with surrounding erythema.
Initial management at the first encounter included obtaining wound swabs for culture and sensitivity, arranging for community wound care and intravenous antibiotics, and tissue biopsy given the atypical examination characteristics of the lesion. Early follow-up 3 days later showed no clinical improvement with intravenous antibiotics and no bacterial growth on any of the cultures that were obtained (including tissue culture). Histopathology of the biopsied lesion reported dense neutrophilic inflammation, necrosis, thrombosed vessels, and fibrin deposition. In other regions of the lesion there was lymphohistiocytic inflammation in the mid to deep dermis, and a mixed inflammatory infiltrate in the papillary dermis including lymphocytes and neutrophils. The epidermis showed acanthosis and subtle spongiosis. No organisms were identified with Periodic acid-Schiff (PAS), Gram, or Grocott special stains. When considered in this clinical context, these pathologic features were consistent with a Sweet’s lesion.
The patient’s dermatologist was consulted to provide recommendations of systemic treatment. Unfortunately, this patient had a reliable and recurrent history of hematemesis from oral prednisone in the past and was therefore contraindicated. Prior to systemic treatment with dapsone, workup to rule out paraneoplastic syndromes was undertaken. In the interim, with few alternatives, the patient was prescribed topical clobetasol ointment and foam dressing which resulted in good initial and long-term response (Figure 2). Prior to initiating systemic therapy 14 days later, the lesion had largely resolved, was far less symptomatic and the wounds re-epithelialized. Further maturation of wound healing and recovery of thumb range of motion took place in the following weeks. The patient’s affected thumb at 6 months following initiation of treatment can be seen in Figure 3.
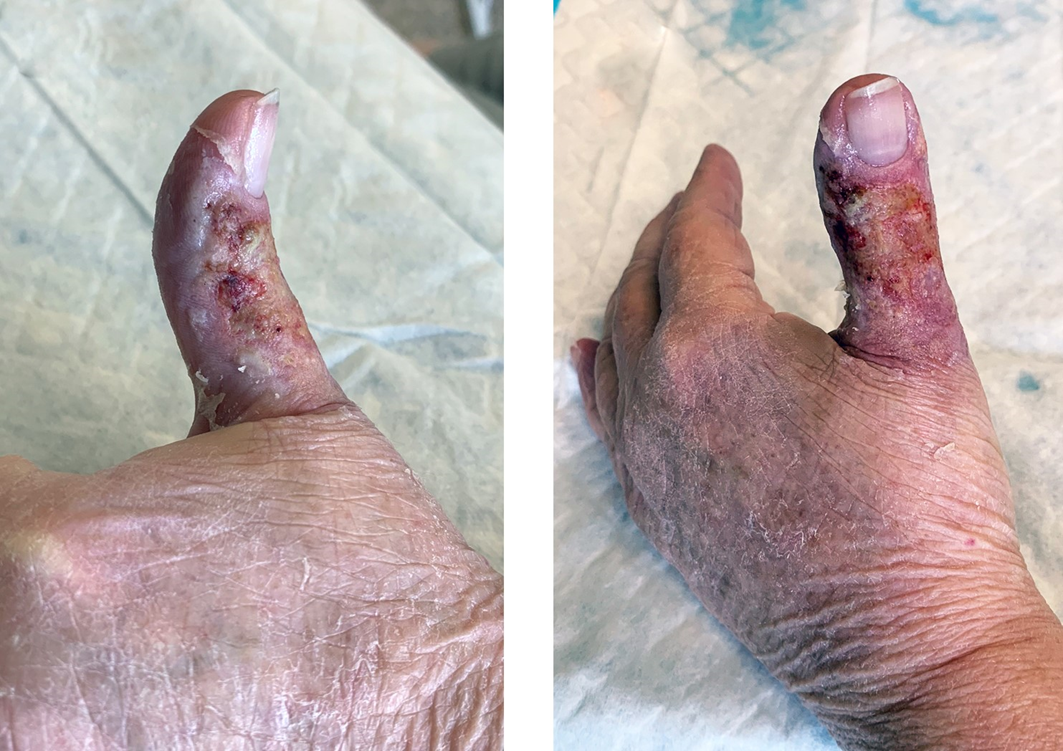
Result of clobetasol application for 13 days along with daily wound care prior to dapsone treatment.

Appearance of affected thumb 6 months following initiation of treatment.
Discussion
Sweet’s syndrome is an uncommon, inflammatory dermatological condition characterized by sudden onset of painful erythematous lesions, fever, and specific histopathologic features. 1,2 The distribution of lesions typically occurs on the neck, face, and upper extremities; however, it is important to recognize atypical presentations such as the one demonstrated by this case.
This case depicts a patient with an established diagnosis of Sweet’s syndrome presenting with an atypical lesion on the thumb initially referred as an infection. Histopathology confirmed a neutrophilic lesion consistent with Sweet’s syndrome, later to be successfully treated with topical corticosteroids given her underlying adverse reaction to oral prednisone. This case illustrates several points specific to the initial management of lesions localized to the hands. First, in acute care environments that manage high volumes of soft tissue infections such as a plastic surgery clinic, it is important for the provider to always keep the differential diagnosis open in atypical scenarios and obtain tissue pathology as part of the work up when necessary. Moreover, this patient also presented with similar papules, nodules, and plaques on her forehead and neck, suggesting that the cause may be systemic rather than localized. Second, this case demonstrates that topical corticosteroids, while less preferable to systemic options, can be used to acutely settle Sweet’s lesions on the hand until systemic therapy with second line agents can be initiated. This observation has not been reported widely in the literature.
Walling et al. and others have reported case series of hand lesions featuring dense neutrophilic infiltrate and have proposed that Neutrophilic Dermatoses of the Dorsal Hand (NDDH) be a recognized subset of lesions presenting in Sweet’s syndrome (see note 1). 8-10 Histologically, these lesions are indistinguishable from atypical pyoderma gangrenosum and pustular vasculitis of the hand and may represent a spectrum of the same disease entity. 8 Its reputation of an infectious mimicker was emphasized in a 49 patient series reported by O’Halloran and colleagues who were referred to either plastic surgery, dermatology or internal medicine clinics. 11 In nearly all reports, diagnosis was established based on very consistent clinical features: lack of clinical response to antimicrobial therapy, tissue pathology featuring dense neutrophilic infiltrate in the dermis without vasculitis, negative cultures, fevers, leukocytosis, and elevated inflammatory markers.
Topical corticosteroids often play an adjuvant role in the treatment of Sweet’s syndrome, and have been found to be effective in treating localized Sweet’s lesions. 1 However, the use of topical corticosteroids as a first-line option in treating these localized lesions is underreported in the literature, as most case reports of localized Sweet’s lesions in the hands have been effectively treated with systemic corticosteroids. 1,7-9,11 In our patient, topical clobetasol was administered prior to systemic dapsone therapy, to which her lesion largely resolved. Administration of clobetasol was an important action to take, as work up for paraneoplastic syndromes and malignancy is required prior to initiating systemic therapy and can cause treatment delays.
Our patient’s presentation was consistent with existing reports of NDDH, a localized manifestation of Sweet’s syndrome. We extend the existing literature on this variant of Sweet’s syndrome and emphasize the importance of a careful history, examination and workup (including tissue pathology when necessary), as this condition may be mistaken for an infection. In addition to infection, the differential for this presentation should include other neutrophilic disorders (e.g., pyoderma gangrenosum, erythema elevatum diutinum), and malignancy. Furthermore, topical corticosteroids can be considered a first-line option to treat localized lesions when systemic corticosteroids are not tolerated, or while workup for paraneoplastic syndromes and malignancy is being conducted.
Footnotes
Consent
The patient presented in this case provided consent for her information and images to be published.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
