Abstract
Horse related injuries include falling from a horse, being stepped on by a horse, kicks, or bites. Bites are rare and often associated with fatalities. We present a case of a 41-year-old healthy female who suffered a complete amputation of her right nipple and abrasion of the areola following a horse bite. We managed the nipple injury as a full-thickness skin graft, similar to that of a compromised nipple in a reduction mammaplasty or mastopexy case. Barring a lack of projection and minor hypopigmentation, the nipple had normal sensation with no scar contracture. Overall, the patient was happy with her final outcome. With a healthy, minimally contaminated wound bed, and lack of poor wound healing risk factors, we believe that treating a nipple amputation as a full thickness skin graft in the emergency setting results in aesthetic outcomes, sensation, and patient satisfaction comparable if not superior to other means of nipple reconstruction in adults.
Introduction
Engineered for power and speed, horses can inflict serious injuries to humans while riding, grooming, feeding, or tacking. 1 Falling from a horse (60%), being stepped on by a horse (11%), kicks (11%), or bites (3%) often result in extremity fracture(s) and/or head injuries. 1,2 Nonfatal horse-related injuries account for approximately 100, 000 emergency room visits per year in the United States. 3 The most common nonfatal areas of injury are the face (23.2%), lower extremity (22.2%), and upper extremity (21.5%). 3
For horses, biting is a form of offensive behavior, which may be due to a change in group composition or housing structure. 4 Not only are horse bites rare, they are also highly associated with fatalities. 5,6 Bites generally involve the limbs and cause trauma ranging from minor superficial contusions, abrasions, or lacerations to severe crushing or tearing injuries with damage to deeper structures. 7,8 Interestingly, previous case reports have even detailed donkey/horse bites that have led to ear 9,10 , nasal, 8 and penile 11 amputations. Following adequate debridement, cleansing, and antibiotic prophylaxis, early primary repair and reconstructive procedures can achieve acceptable aesthetic outcomes. 9 If immediate reconstruction is not feasible, primary closure with delayed reconstruction is preferred. 11
Acquired non-oncologic breast defects are rare, and are often the result of traumatic injuries such as deep burns. 12 Here we present a novel case of a nipple amputation due to a horse bite to the breast, treated surgically with full-thickness grafting of the amputated nipple.
Case Presentation
A 41-year-old healthy, non-smoker, female presented to the emergency department with a complete amputation of her right nipple secondary to a horse bite earlier that day (Figure 1). She reported trying to put a bridle on a horse that was blind in one eye. Fortunately, she had been wearing a thick shirt and a vest. The horse’s teeth did not fully penetrate the patient’s clothing and thus did not come into contact with her skin. With the exception of the nipple amputation and areolar abrasion, no other cutaneous injuries were sustained. Treatment options discussed were primary closure, healing via secondary intention or reconstruction via full-thickness grafting of the nipple. The patient consented to full-thickness grafting of the amputated part after her options and the risks and benefits of each, were explained. Pre-operatively she understood that with any of the treatment options, asymmetrical appearance to the contralateral nipple, altered pigmentation, altered or lack of sensation, and inability to breastfeed were likely. The patient was prepped and draped in a sterile fashion. The wound was irrigated. The nipple was debrided, irrigated and debulked sharply. A 4-0 chromic gut suture was used to suture the nipple in situ (Figures 2 and 3) and a bolster dressing consisting of Xeroform, Bactigras, and moist gauze was secured using a 3-0 nylon suture. The patient was prescribed an antibiotic (amoxicillin-clavulanic acid) and instructed to leave the dressing intact until her follow-up with the surgeon.
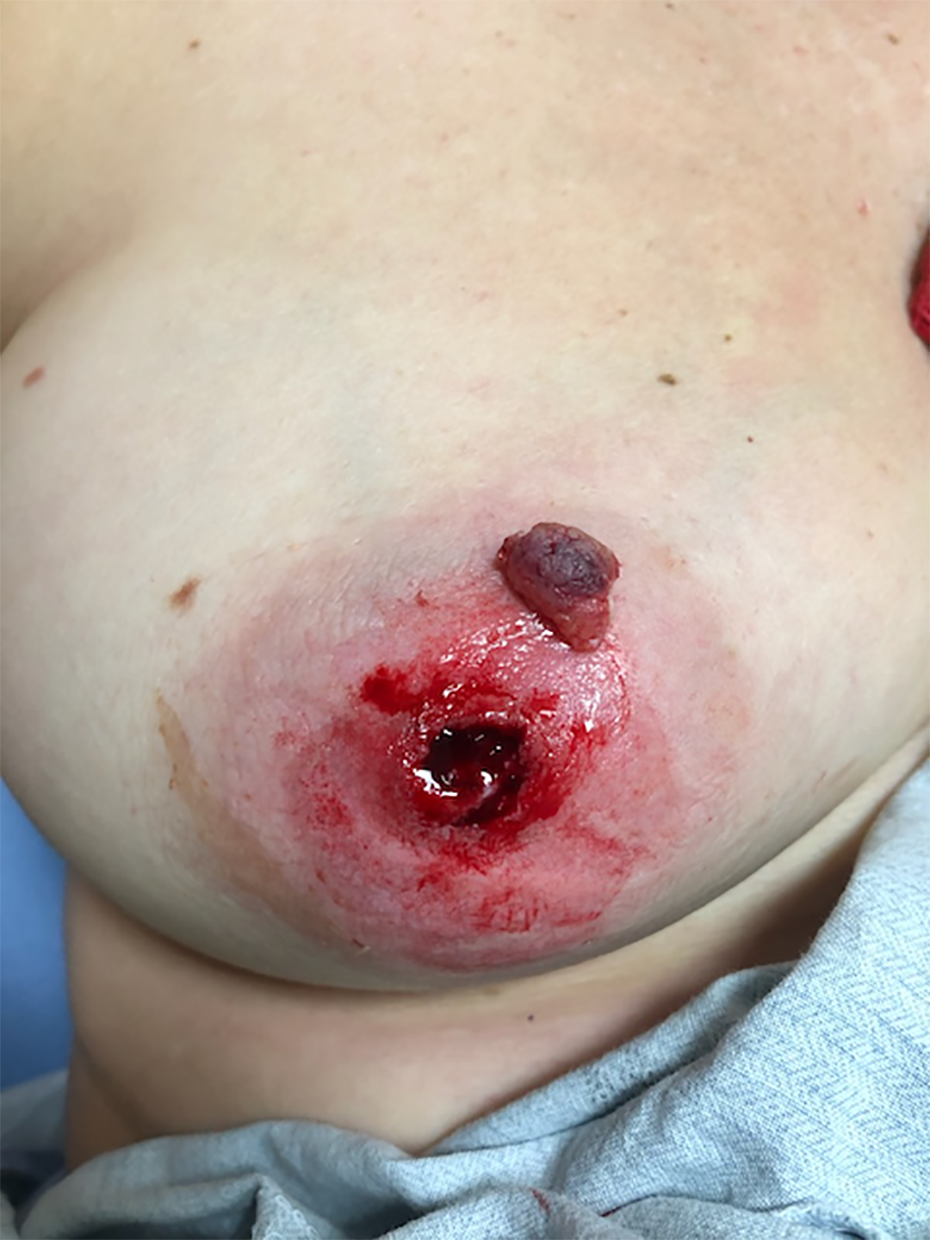
Emergency department presentation of complete nipple amputation.
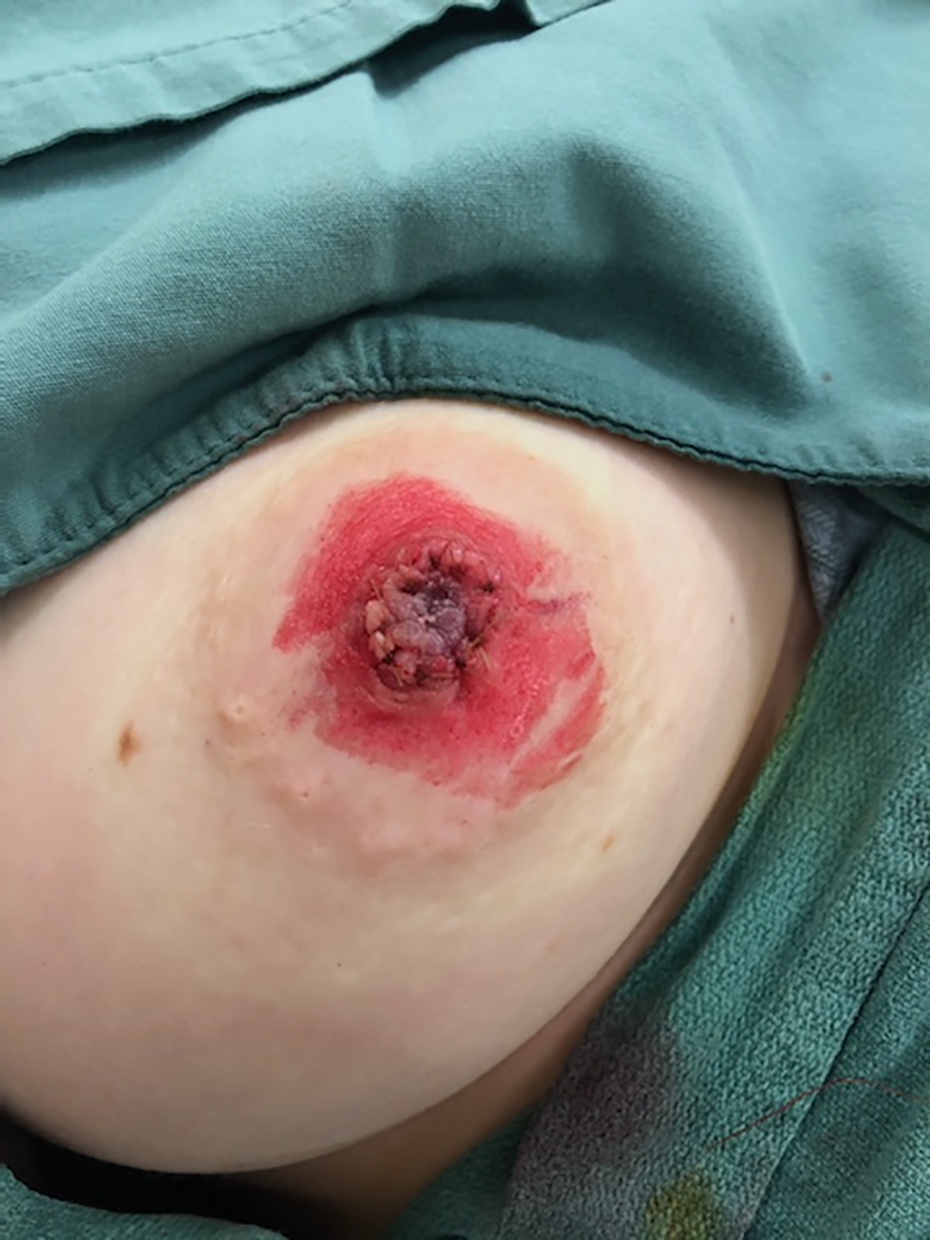
Nipple sutured in situ with a 4-0 chromic gut suture.
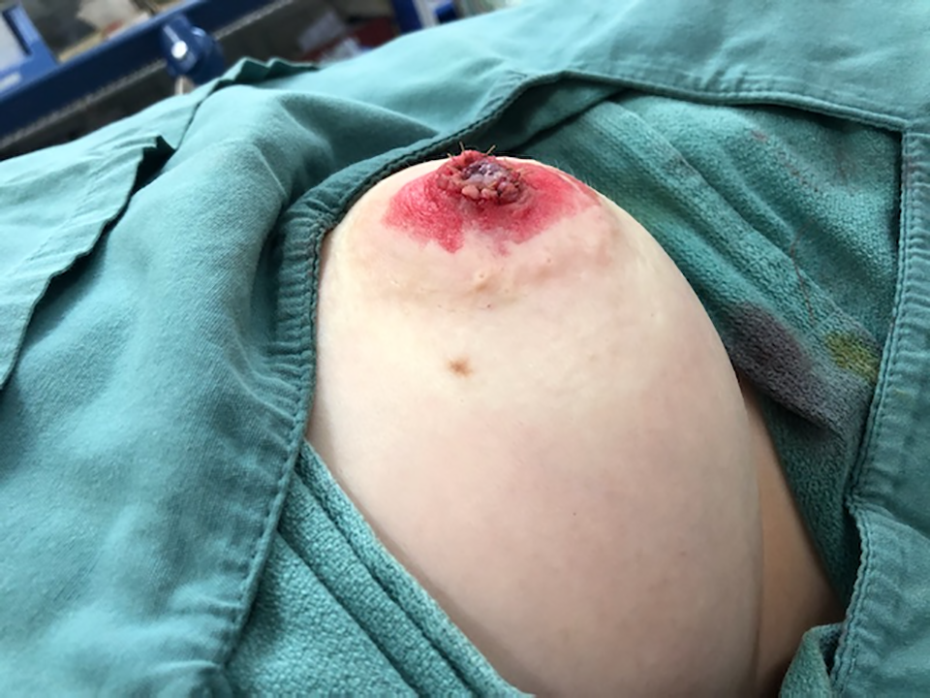
Nipple sutured in situ with a 4-0 chromic gut suture.
At the first follow-up appointment, post-operative day (POD) 4 the full-thickness nipple graft was intact, with no signs of graft loss or infection. Wound care was arranged for daily dressing changes. At POD9, graft necrosis was present, though superficial (Figures 4 and 5). At 4 weeks post-operatively, some projection was maintained (Figure 6). However, the central third of the grafted nipple appeared necrotic, and debridement of the necrotic tissue was performed (Figure 7). Daily dressings were continued, and the patient cleansed the wound daily with soap and water. The last follow up occurred at 7 months post-injury and reconstruction. Compared to the contralateral nipple, the reconstructed nipple lacked projection and had minor hypopigmentation (Figures 8 –10). The patient reported similar sensation (with the ability to discriminate sharp versus dull) to the contralateral nipple. The patient volunteered that she was happy with her outcome. Nevertheless, the patient was offered options for augmentation of nipple projection (with fat grafting versus dermal graft versus injectable filler), which she declined. Informed consent was obtained from the patient for publication of photography in scientific journals.
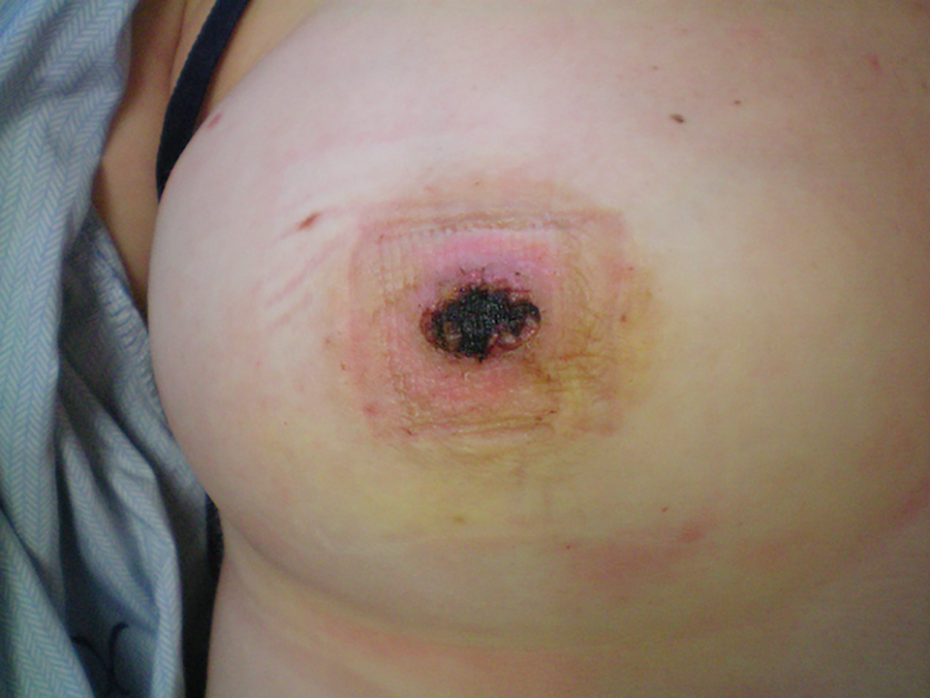
At 9 days post-injury and reconstruction, superficial graft necrosis was seen (frontal view).
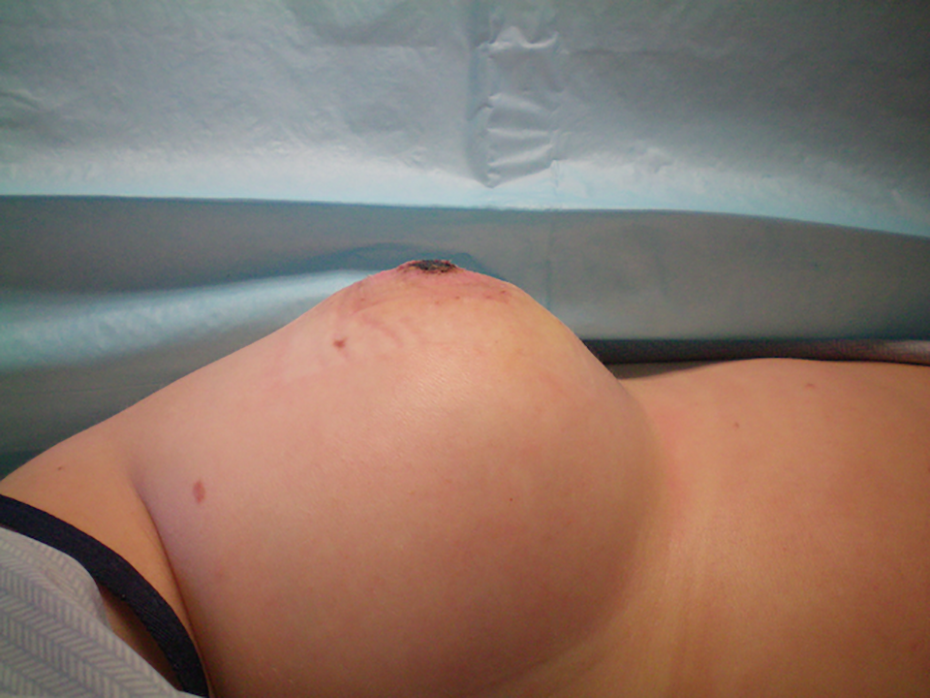
At 9 days post-injury and reconstruction, superficial graft necrosis was seen (lateral view).
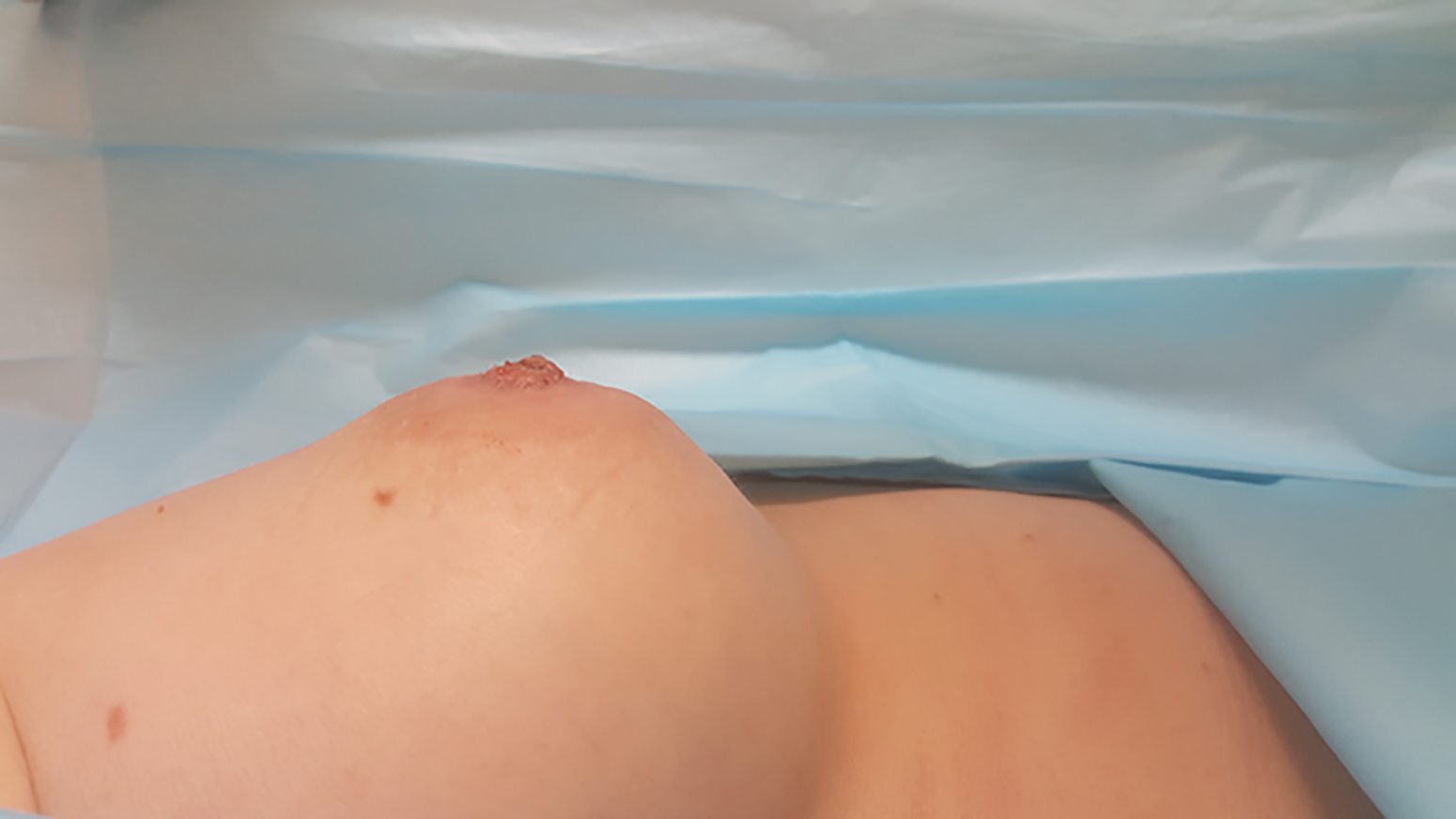
At 4 weeks post-injury and reconstruction, there was preservation of some projection.
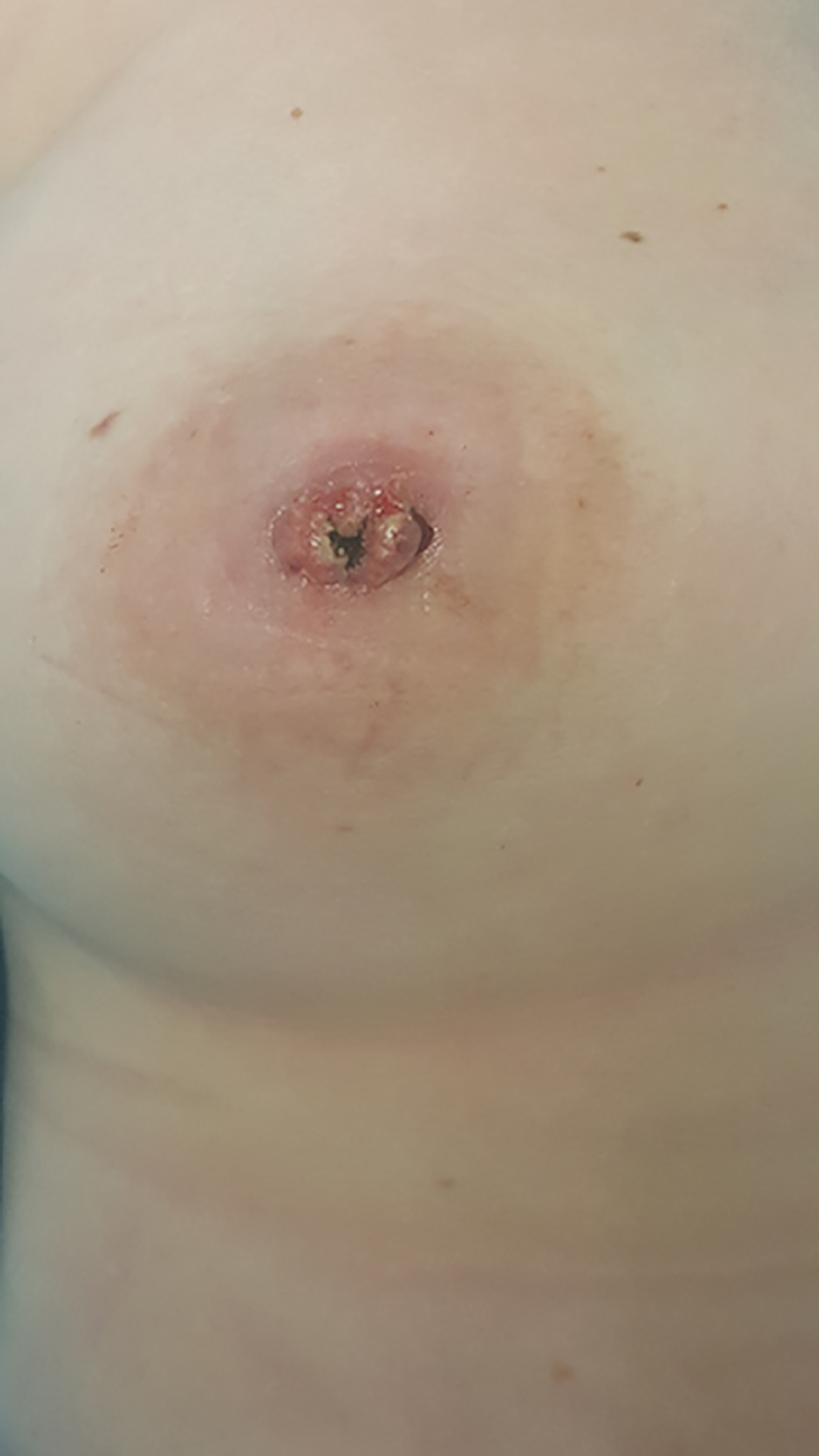
At 4 weeks post-injury and reconstruction, there was necrosis of the central aspect of the grafted nipple.

At 7 months post-injury and reconstruction, the reconstructed nipple had minor hypopigmentation.
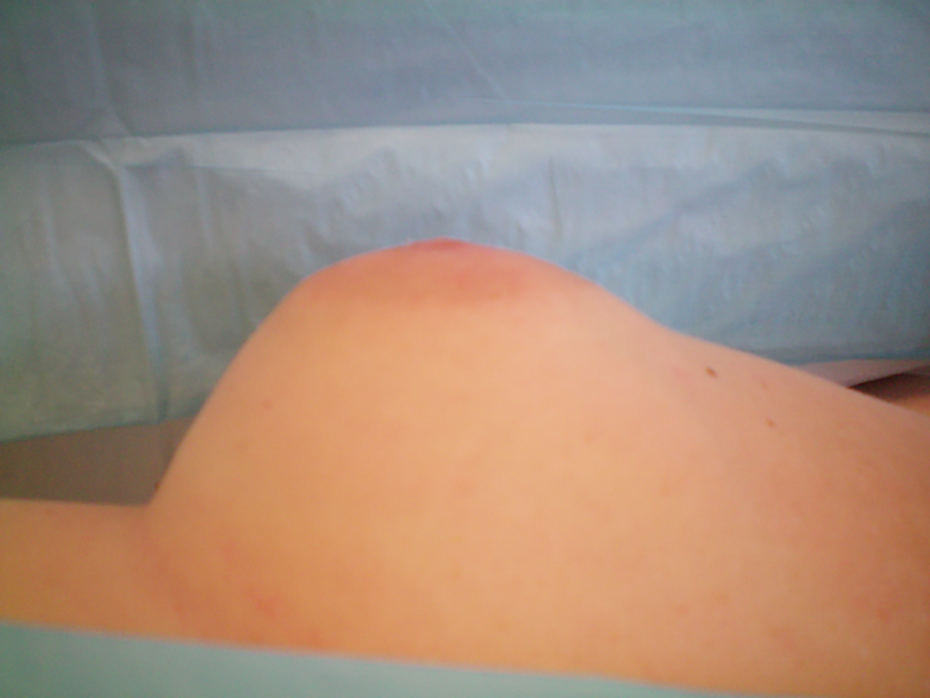
At 7 months post-injury and reconstruction, the reconstructed nipple lacked projection.
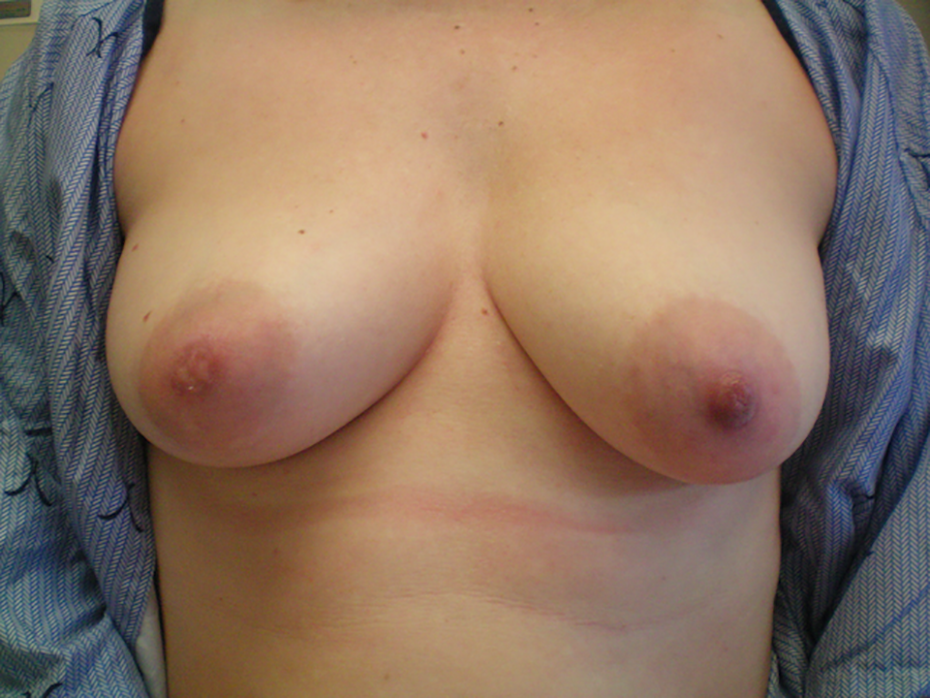
Comparison of the reconstructed nipple and healed areola to the contralateral side at 7 months post-injury and reconstruction.
Discussion
Breast asymmetry can be a result of breast cancer, trauma, or embryologic, hormonal, or idiopathic factors. 13 Restoring the form of the breast has known positive effects including improvement of: psychosocial and sexual well-being, satisfaction with their breasts, body image, and self-esteem. 14
Many methods of nipple reconstruction have been described in the context of breast reconstruction, including: nipple sharing, local flaps, autologous or heterologous augmentation, prosthesis, or 3D tattoos. 15 Local flaps are most commonly used, and may be classified as: centrally based flaps, subdermal pedicled flaps, or pull out/purse string flaps. 16-18 The most common complications are partial and total nipple necrosis, loss of projection, and donor site morbidity. 15 Loss of projection results from retraction forces, scar contracture, and reduced blood flow, which leads to tissue contraction and shrinkage. 16 Notably, patient satisfaction following nipple reconstruction is often high, regardless of the technique employed. 19
While there are several methods available for nipple reconstruction, we opted to preserve the original nipple by treating the amputated nipple as a full thickness skin graft. We believe that this amputated nipple maintained viability via the basic principles of skin grafting: plasmatic imbibition, inosculation, and revascularization. 20 Management of this amputated nipple is similar to the intraoperative management of a nonviable nipple in a reduction mammaplasty or mastopexy. In these cases, irreversible ischemia of the nipple is an indication for conversion from the nipple as a pedicle flap to a full thickness skin graft. 21 Survival of the graft is then dependent on adequate blood supply at the recipient site. 21 These salvage procedures have been associated with satisfactory aesthetic outcomes. 22
As a full thickness skin graft, the nipple was particularly susceptible to partial or complete graft failure due to greater soft tissue requiring nourishment. 20 To decrease this risk, the nipple was debulked prior to grafting, likely at the cost of decreased nipple projection. Similar to the presented case, a literature review found that loss of projection following NAC reconstruction was found to have no significant impact on patient satisfaction. 17 In the case of a healthy wound bed, lack of poor wound healing risk factors, and absence of a crush injury, we suspect that treating a nipple amputation as a full thickness skin graft resulted in aesthetic outcomes, sensation, and patient satisfaction comparable if not superior to other means of nipple reconstruction in adults.
Bite injuries to the breast are rare, with only a few previously reported cases. Similar to our case, Shen et al 23 described the reconstruction of a completely amputated nipple following a human bite in a 26-year old female. The amputated nipple was reshaped for reconstruction along with a fascial flap and closed with a purse string suture. This resulted in good symmetry and improved shape and colour in comparison to either a local or distant flap.
In the pediatric population, Ho Quoc et al. 12 reported reconstruction of a breast amputation following a horse bite in an 8-year old female, resulting in inadequate skin envelope and breast volume, in addition to amputation of the NAC. With fat grafting and nipple reconstruction using a bifoliated flap and areolar tattooing, the authors reported symmetric volume, natural texture, and improved sensation without any complications. The reconstructed breast underwent symmetrical breast development. In contrast, Miyata et al. 24 reported a nipple amputation after a dog bite in a 6-year-old, which was treated with suturing the nipple as a graft. While it was partially depigmented and there was no projection, full sensitivity was regained. Ten years later, scar revision was performed with 2 Z-plasty procedures to correct the flat nipple. Authors noted that as secondary sex characteristics appeared, due to nipple and areolar enlargement, pediatric breast injuries became more pronounced.
While previous attempts have been made at nipple reconstruction following bite injuries, this case is the first (to our knowledge after literature review) where an amputated nipple was managed successfully using the principles of full-thickness skin grafting in an adult.
Take Away
As an alternative to other means of nipple reconstruction, nipple amputation injuries can be treated as a full thickness skin graft in the emergency department in the appropriate scenario. This case report demonstrated adequate graft take, acceptable recovery of sensation, and good patient satisfaction.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Statement of Human and Animal Rights
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2008.
Statement of informed Consent
Informed consent was obtained from the patient in the study, including for the purpose of publication in scientific journals.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
