Abstract
Free jejunal flap transfer is common in head and neck reconstruction, but necrosis remains a complication. A 77-year-old man underwent total pharyngo-laryngo-esophagectomy, bilateral neck dissection, and free jejunal flap transfer. We anastomosed 3 arteries (facial, transverse cervical, and superior thyroid) and 1 vein (jejunal) because the recipient site’s arterial status was poor. On day 2, ultrasonography and visualization revealed that the anastomosed vein was obstructed in the cranial jejunum but the remainder was viable. The region recovered by day 7 and the patient began oral intake on day 30. Ultrasonography revealed that the anastomosed jejunal vein showed no waveform, the facial and transverse cervical arteries showed arterial waveforms, and the superior thyroid artery showed a retrograde venous waveform. The flap had survived because the blood exited through the superior thyroid artery and vein. Thus, additional vascular and arterial anastomoses are options for free flap survival if the vascular status is poor.
Introduction
Free jejunal transfer is widely performed in head and neck reconstruction, but flap necrosis caused by anastomosed vessel occlusion remains a serious complication. 1 To reduce the risk of flap loss, additional vascular anastomoses are sometimes performed. However, it is not clear how additional anastomoses increase the chance of flap survival. We report on the survival of a free jejunal flap despite obstruction of the only anastomosed vein on postoperative day 2.
Case Presentation
A 77-year-old man with hypopharyngeal cancer (T4a N2b M0), who had received 70 Gy radiation for laryngeal cancer 14 years before this surgical intervention, underwent a total pharyngo-laryngo-esophagectomy, bilateral neck dissection, and free jejunal flap transfer. The patient had no other significant medical history. Revascularization was achieved by anastomosis of 3 arteries and 1 vein. After anastomosing the jejunal artery and vein to the facial artery and internal jugular vein, 2 additional arterial anastomoses of the superior thyroid artery and transverse cervical artery were performed because the recipient site vascular status was poor; that is, repeating intraoperative artery thrombosis and spasms (Figure 1).
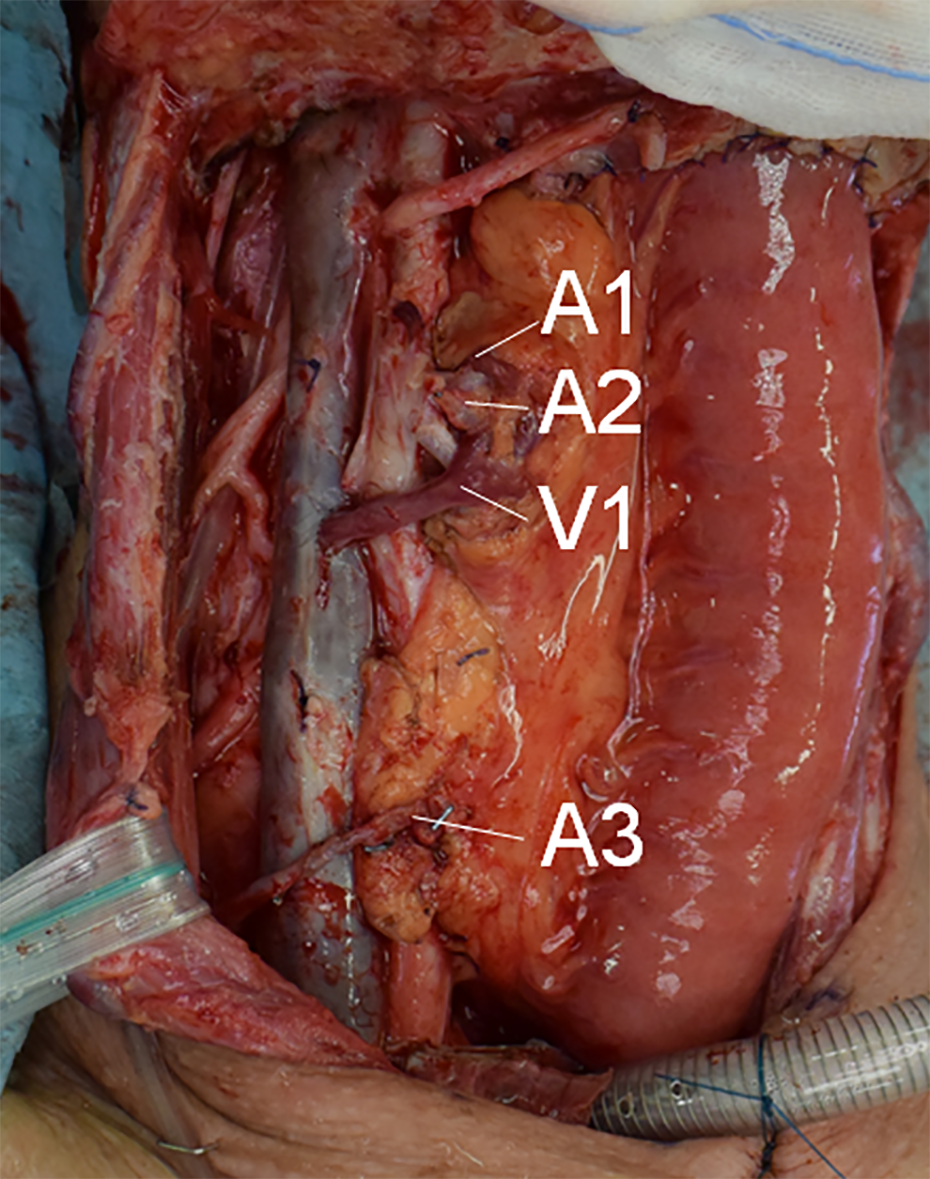
A free jejunal transfer was performed by anastomosis of 3 arteries and 1 vein. The jejunal artery and vein were anastomosed to the facial artery and internal jugular vein, respectively, and then 2 additional arteries—the superior thyroid artery and transverse cervical artery—were anastomosed because the recipient site vascular status was poor. A1, facial artery; A2, superior thyroid artery; A3, transverse cervical artery; V1, internal jugular vein.
On postoperative day 2, the patient spat blood. Ultrasonography showed that all of the anastomosed arteries were flowing, but the anastomosed vein was obstructed (Figure 2). A computed tomography (CT) examination revealed a large dead space below the stiff neck skin, and that the arteries in the mesentery were enhanced but the vein was not (Figure 3). We opened the wound directly above the dead space. The mesentery was red and swollen, a small area of the cranial portion of the jejunum was purplish, and the caudal portion of the jejunum was reddish (Figure 4). Because the main portion of the jejunum seemed to be alive, we did not reoperate.
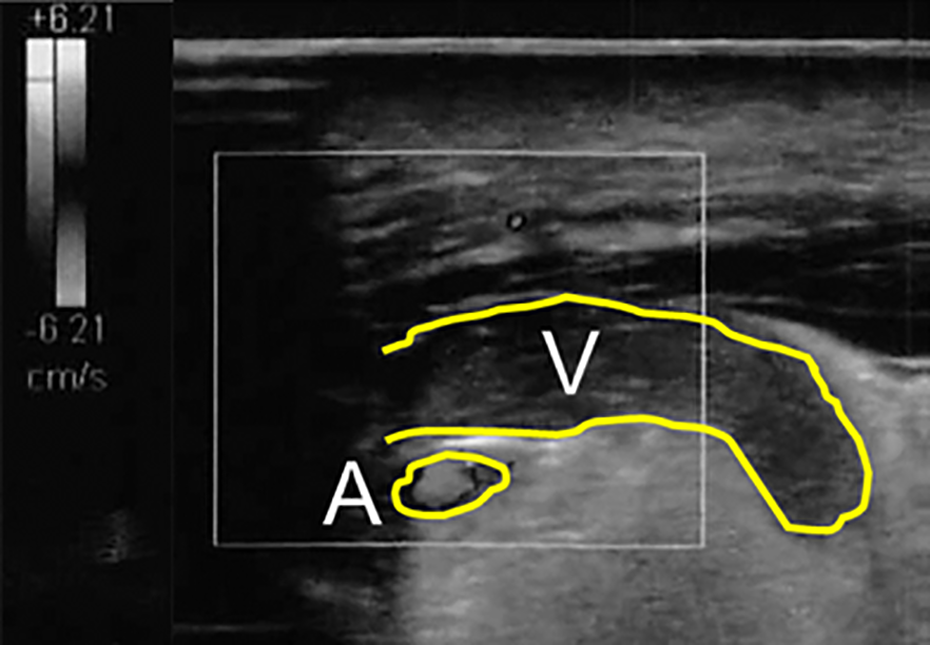
Ultrasonography on postoperative day 2. All anastomosed arteries demonstrated blood flow, but the anastomosed vein was obstructed. V, anastomosed vein; A, anastomosed artery.
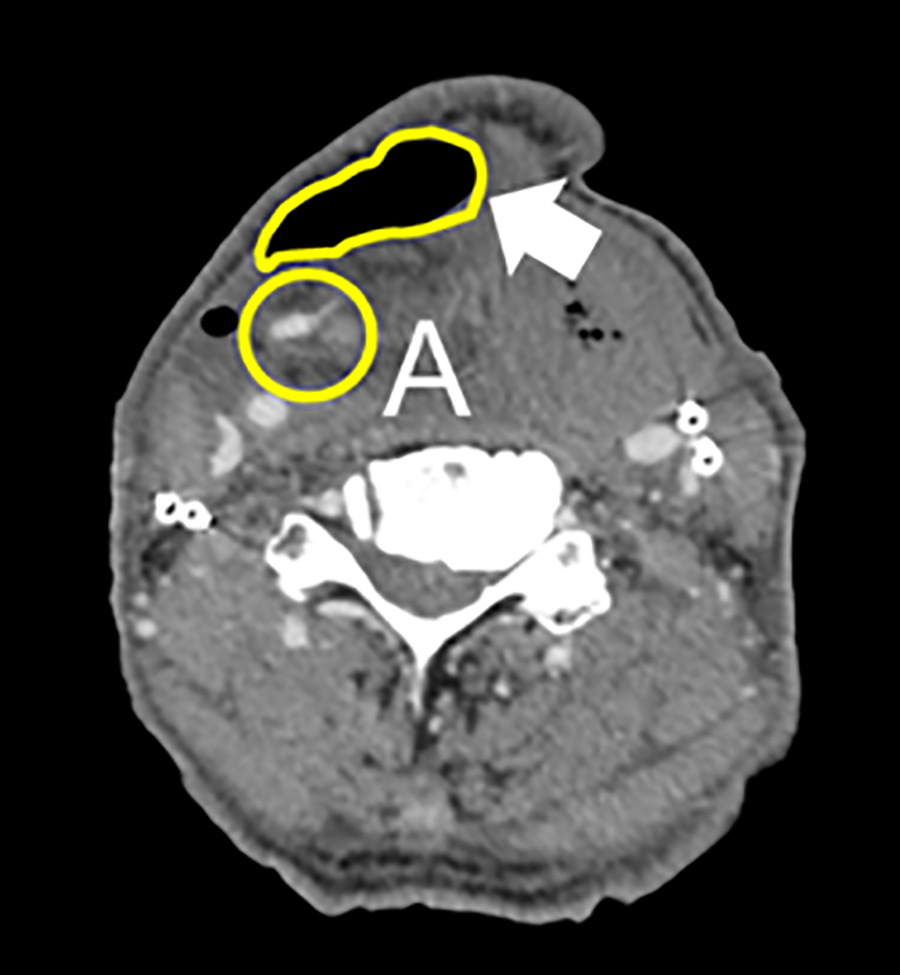
CT examination on postoperative day 2. A large dead space was observed below the stiff neck skin (arrow). Arteries in the mesentery were enhanced but the vein was not.
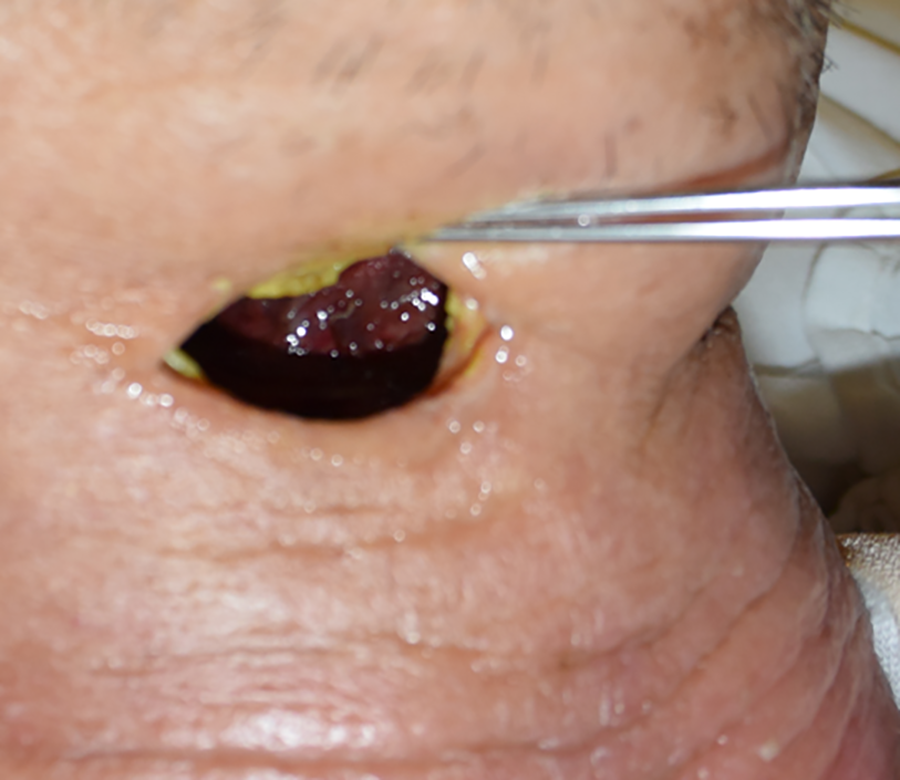
Postoperative day 2. We opened the wound directly above the dead space on postoperative day 2. A small area of the cranial portion of the jejunum was purplish, and the caudal portion of the jejunum was reddish. We did not reoperate immediately because the main portion of the jejunum seemed to be alive.
The purplish area of the jejunum became reddish and the mesentery shrank gradually. On postoperative day 7, the purplish area of the jejunum was the same color as the other areas (Figure 5). On postoperative day 14, the patient started oral intake of water, and no leakage was observed. He then started oral intake of a soft diet on postoperative day 30.
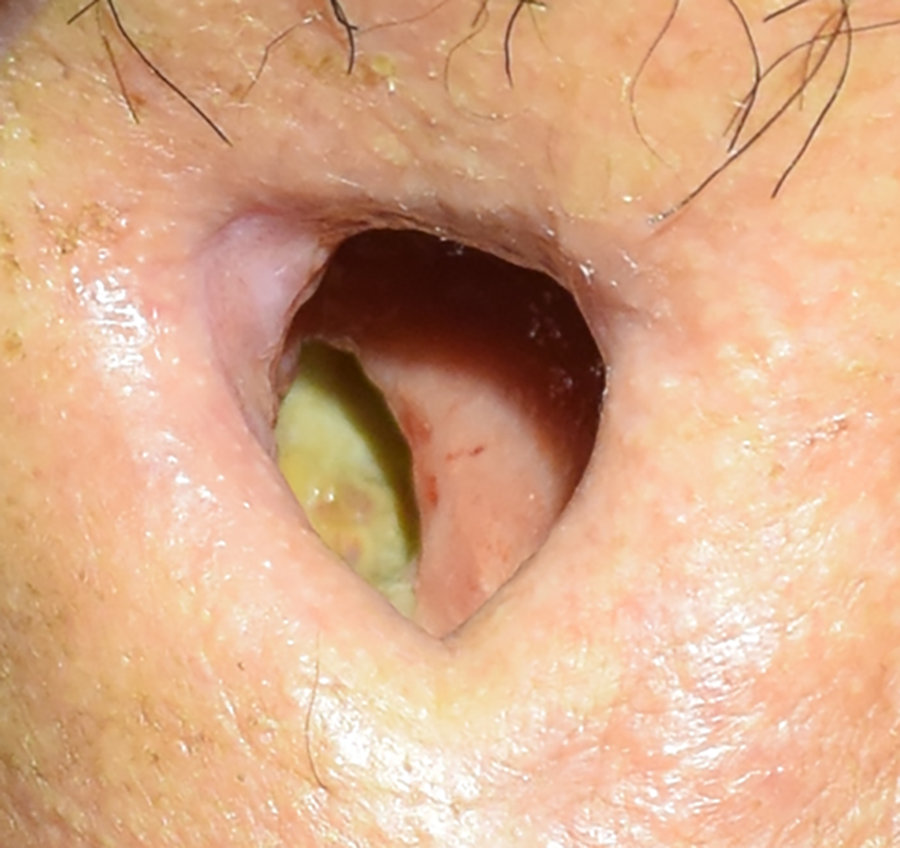
Postoperative day 7. The purplish area of the jejunum had become reddish as in the other areas of the jejunum.
Postoperative ultrasonography revealed that the anastomosed jejunal vein showed no waveform, the facial artery and transverse cervical artery showed an arterial waveform, and the superior thyroid artery showed a venous waveform (Figure 6). We concluded that the free jejunal flap had survived because the blood from the facial artery and transverse cervical artery flowed out retrogradely through the superior thyroid artery and into its companion vein even though the anastomosed jejunal vein was obstructed.
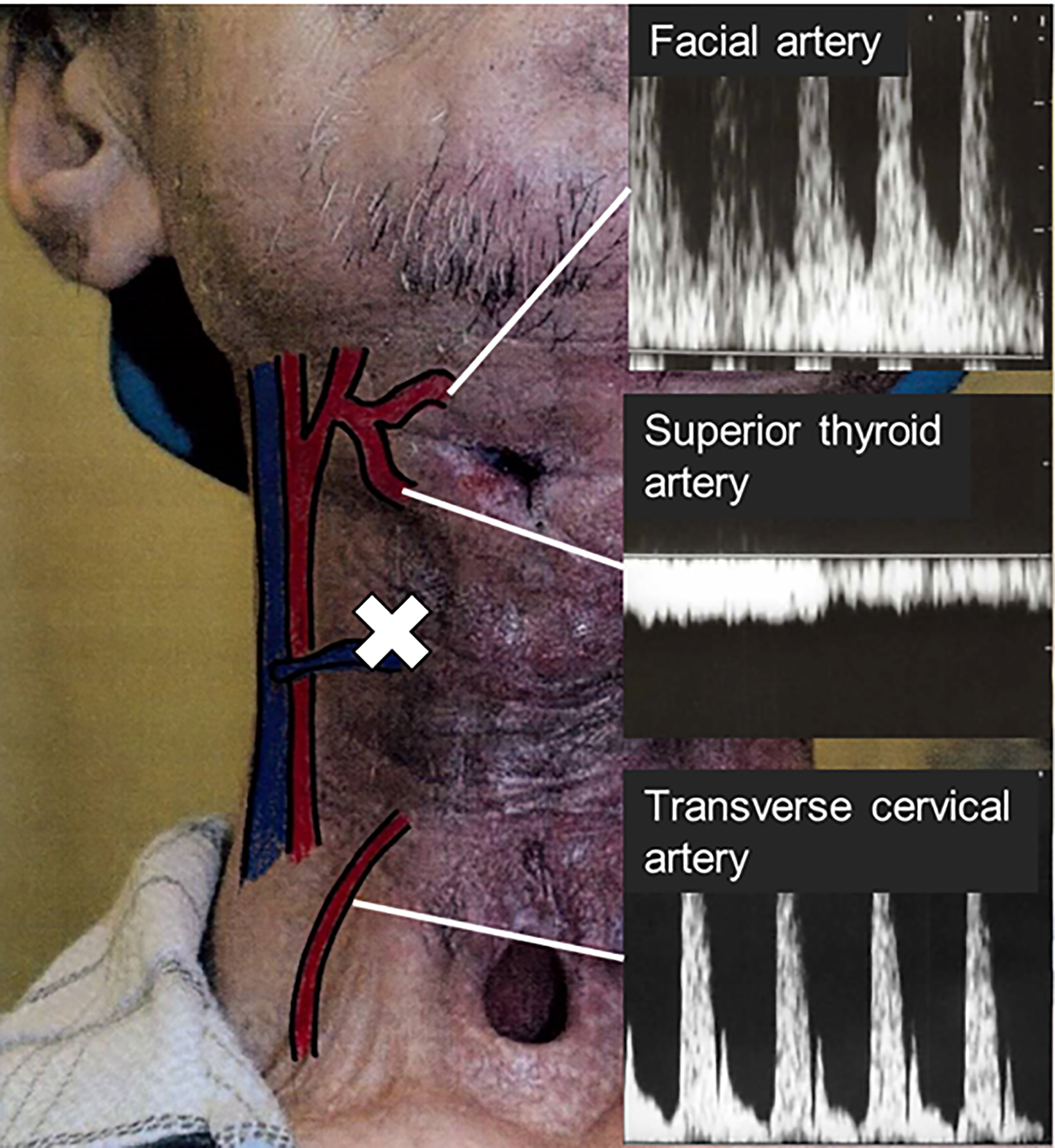
Postoperative ultrasonography. The anastomosed jejunal vein showed no waveform (white cross). The facial artery and transverse cervical artery showed an arterial waveform. The superior thyroid artery showed a retrograde venous waveform.
Discussion
This case raises 2 important clinical issues. The first is that a free jejunal flap with 3 arterial anastomoses survived despite the only anastomosed vein being obstructed on postoperative day 2.
The total necrosis rate is less than 5% for a free jejunal flap. Necrosis is caused mainly by vascular thrombosis and loss of axial blood supply. 2 Survival of a free jejunal flap after interruption of a vascular anastomosis without surgical revision has been reported only 4 times in the recent literature. 3-6 The flap survived after venous thrombosis in 1 case 3 and after loss of axial blood supply in 3 cases, 4 -6 and the flap survived after neovascularization in all cases.
We suggest 2 possible mechanisms to explain why the flap survived despite venous occlusion in our patient. The first is neovascularization, such as that reported in the 4 reports noted above. Yoon et al. reported that neovascularization occurs as early as postoperative day 6 in a free cutaneous flap but that a jejunal flap needs more time for complete neovascularization than a skin or muscle flap. 7 In one previous report, 3 the free jejunal flap survived for at least 5 weeks after the operation despite venous occlusion. 3 In another report, the free jejunal flap survived for at least 10 days after the operation despite the loss of the axial blood supply. 4 In our patient, the venous anastomosis was obstructed on postoperative day 2 and postoperative contrast CT showed no neovascularization. We conclude that venous neovascularization was not responsible for flap survival in this patient.
The second possible mechanism for flap survival is that an anastomosed artery may have become a drainer; that is, arterial blood flowed into the flap through the facial and transverse cervical arteries and flowed out through the superior thyroid artery (Figure 7). Postoperative ultrasonography revealed that the facial and transverse cervical arteries showed arterial waveforms, which suggested that the arterial blood flowed into the jejunum in an antegrade fashion through these vessels. Postoperative ultrasonography showed no waveform in the anastomosed jejunal vein and a retrograde venous waveform in the superior thyroid artery. These findings suggest that the blood passed through the jejunal arcade, flowed out retrogradely through the superior thyroid artery, and finally flowed into its companion vein.
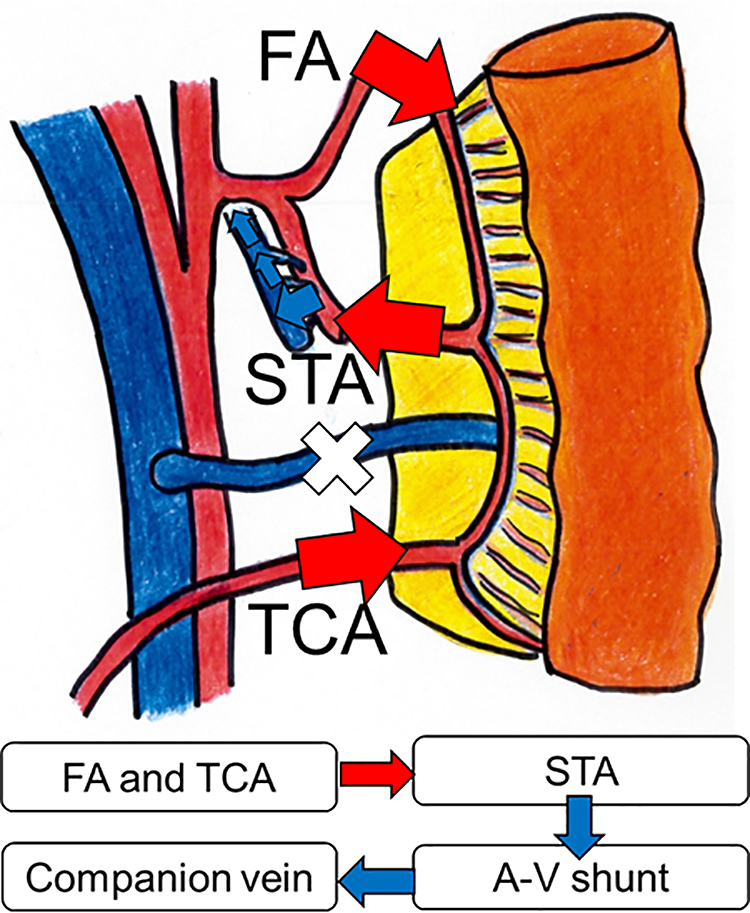
A proposed mechanism to explain flap survival. The blood flowed in through the facial artery (FA) and transverse cervical artery (TCA), flowed retrogradely out through the superior thyroid artery (STA), and finally flowed into its companion vein through an arteriovenous (A–V) shunt.
We propose that the blood flow from the superior thyroid artery to its companion vein must have passed through an arteriovenous shunt (A–V). Sekido et al. reported that, in a free radial forearm flap transfer for tongue reconstruction, blood in an anastomosed artery flowed in both an antegrade and retrograde fashion because of venous congestion. 8 The reports cited above and our findings suggest that the free jejunum flap survived in our patient because an anastomosed artery became a drainer through an A–V shunt and because of blood flow through a companion vein of the superior thyroid artery. We conclude that the second mechanism—an anastomosed artery had become a drainer—is the more likely explanation for the survival of the flap in our patient.
The second important clinical issue is that additional vascular anastomosis is a potential surgical option if the vascular status is poor and that an additional arterial anastomosis might be more useful for free flap survival than additional venous anastomoses. One arterial and one venous anastomosis are usually performed in the microvascular free flap transfer, but additional vascular anastomoses may be performed to reduce the risk of flap loss in some patients. However, it remains controversial whether additional vascular anastomoses are better for flap survival. 9,10
In our patient, the free jejunal flap survived because the blood flowed out retrogradely through the superior thyroid artery, which was 1 of 3 anastomosed arteries, and through its A–V shunt and companion vein. This suggests that an additional vascular anastomosis can function as a safety valve if the other anastomosis is obstructed. An additional vascular anastomosis may therefore be a surgical option if the vascular status is poor.
Others have discussed whether an artery or vein is more useful for an additional anastomosis to ensure flap survival. 11 In our case, if a single arterial anastomosis and multiple venous anastomoses are performed, the anastomosed veins do not exhibit retrograde flow and the flap cannot survive when the arterial anastomosis is obstructed because of the presence of valves in the veins. The additional arterial anastomosis also makes the blood flow faster in the flap and lessens the risk of thrombosis. 10,12 By contrast, the additional venous anastomosis slows the blood flow in the flap, which increases the risk of thrombosis. Based on these findings, we conclude that additional vascular anastomosis is a surgical option if the vascular status is poor and that an additional arterial anastomosis might be more useful for free flap survival than additional venous anastomoses.
Footnotes
Ethical Statements and Informed Consent
All procedures followed were in accordance with the ethical standards of the national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. Informed consent was obtained from all individual participants involved in the study.
Declaration of Conflicting Interests
The author declared no potential conflicts of interest with respect to the research, authorship, or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Statement of Human and Animal Rights
This article does not contain any experimental studies with human or animal subjects.
Statement of Informed Consent
Written, informed consent was obtained from the patient included in this case report.
