Abstract
Resection of neoplastic chest wall lesions is associated with high surgical morbidity and can result in complete full thickness defects. Defects can be challenging to reconstruct and require a multidisciplinary surgical approach. The goals of chest wall resection are to optimize oncological outcomes while also minimizing functional disturbance. We report a novel technique, using a Titanium and Polymethyl-methacrylate (PMMA) construct for an antero–lateral chest wall reconstruction following resection of a locally recurrent malignant Phyllodes tumour. This approach to reconstruction provides stability, allows chest wall excursion and minimizes post-operative pain.
Introduction
The technical aspects of oncologic chest wall surgery can be simplified by dividing the operative approach into two separate but distinct components; resection and reconstruction. Optimizing both oncologic and functional outcomes is crucial for patient management, and consequently the technical considerations of each aspect must be thought of in turn. 1
In general, chest wall reconstruction consists of two parts: skeletal reconstruction and soft tissue coverage. 2 There are several synthetic, biologic and metallic materials available for chest wall reconstruction; each with its own advantages and disadvantages. 3 Coverage of the prosthesis with durable vascularized tissue is essential to prevent infection or chest wall extrusion. The tissue should be robust enough to withstand radiotherapy, which may be required either in the adjuvant setting or in the event of recurrence. Furthermore, consideration should be given to the cosmetic result, particularly in the region of the female breast.
The priorities of chest wall reconstruction include restoration of functional and structural integrity, preservation of pulmonary mechanics, avoidance of chest wall contraction, prevention of scapula trapping (particularly when resection involves ribs five and six), protection of underlying mediastinal organs following sternal resection, and an acceptable cosmetic result. 2,4 Therefore, a multidisciplinary approach, including consultation from thoracic surgeons, surgical oncologists, plastic surgeons, as well as medical and radiation oncologists is essential.
Technique
We report a 59–year–old female patient who presented with a locally recurrent malignant Phyllodes tumor of the left breast. Previous subcutaneous mastectomy and lateral chest soft tissue resection had left a positive deep margin on the anterolateral chest wall. There was also an incidental metastatic deposit in a single ipsilateral axillary tail lymph node. The patient was presented and discussed at a multidisciplinary meeting and advised to undergo chest wall resection with reconstruction.
Pre–operative consultation with a radiologist was necessary to determine the extent of both the soft tissue and bony resection margins. The initial pre–operative computed tomography (CT) scan of the chest, with the original tumor in–vivo, was superimposed onto the most recent post–resection CT scan. The surgeon was then able to ascertain the required surgical margin.
Method of Surgical Resection
Surgical resection commenced with excision of the previous pedicled latissimus dorsi myocutaneous flap (LDMF), including soft tissue margin, with preservation of the thoracodorsal vascular pedicle for later soft tissue reconstruction. A level I-III left axillary lymph node dissection was then performed. The surgeon then resected three ribs (four to six in continuity with serratus anterior over ribs three to seven). This was done to ensure an adequate surgical margin (> 1 cm) and reduce the risk of further local recurrence. 1 A 28-French chest drain was then inserted. The resultant defect measured 7 cm. Typically, resections less than 5 cm do not require stabilization of the chest wall. 5 However, anterior chest wall defects greater than 5 cm, posterior defects more than 10 cm or a resection including more than three ribs, require skeletal reconstruction. 5
Method of Reconstruction
Chest wall reconstruction commenced using Polypropylene mesh sutured to the inner layer of the lateral rib defect with 2 cm of overlap. Neo-ribs were fashioned on the back table prior to implantation using Polymethyl-methacrylate (PMMA) shaped to approximate the dimensions of the resected rib segments; with a few millimeters of space at each end. After the PMMA hardened, each neo-rib was held against the locking Titanium plate (Synthes MatrixRIB ™ Fixation System, Johnson and Johnson, USA) with bone reduction forceps (Figure 1) to ensure correct separation of the anterior and posterior rib segments. Plates were then bent and cut to traverse the defect so that there were three screw holes overlapping both the anterior and posterior remnants of the resected ribs. These were fixed using bicortical locking screws. The neo-ribs were then screwed to the center of the Titanium plate with two locking screws (slightly short of full thickness) to form the semi-rigid neo-rib constructs (Figure 2).
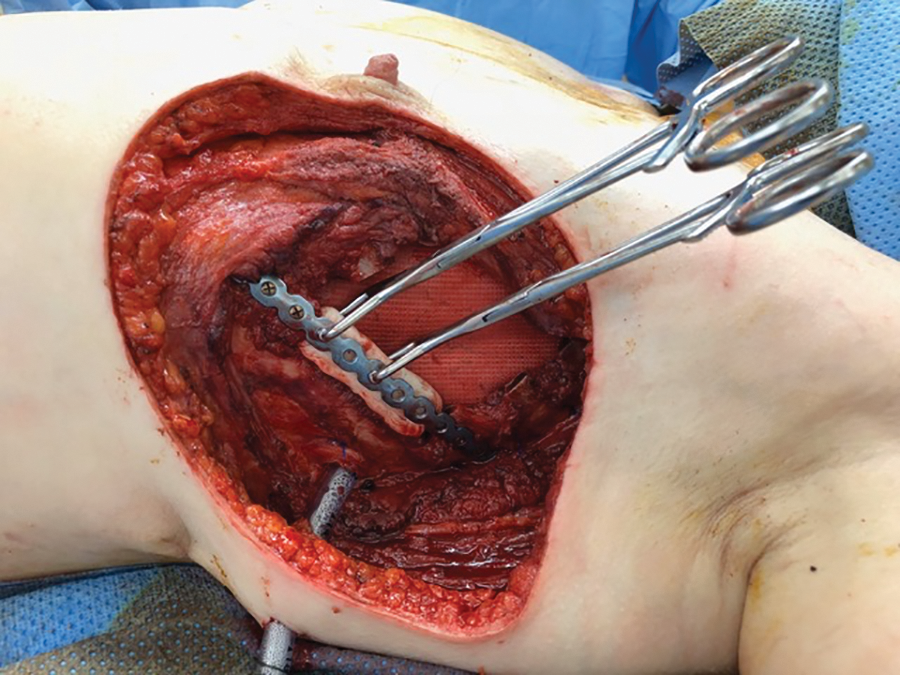
After the Polypropylene mesh layer is sutured inside the chest wall defect with 2-3 cm overlap, bicortical locking screws fix the Titanium rib plate to the resected ribs. The first of the neo-ribs is held in place with reduction forceps prior to securing to the Titanium plate.
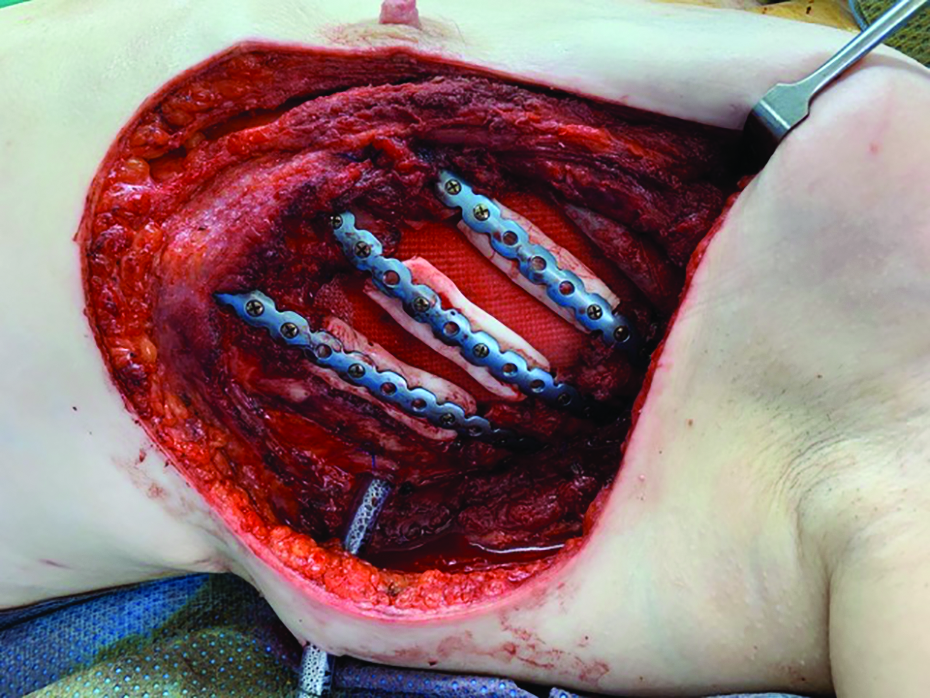
Prior to soft tissue reconstruction, all neo-ribs are secured in place.
Following skeletal reconstruction, the breast and lateral chest soft tissues were reconstructed with a free deep inferior epigastric artery perforator (DIEP) flap (Figure 3). The patient had minimal post-operative chest wall discomfort, despite significant chest wall resection. At six-month follow-up, the patient remained well and disease free.
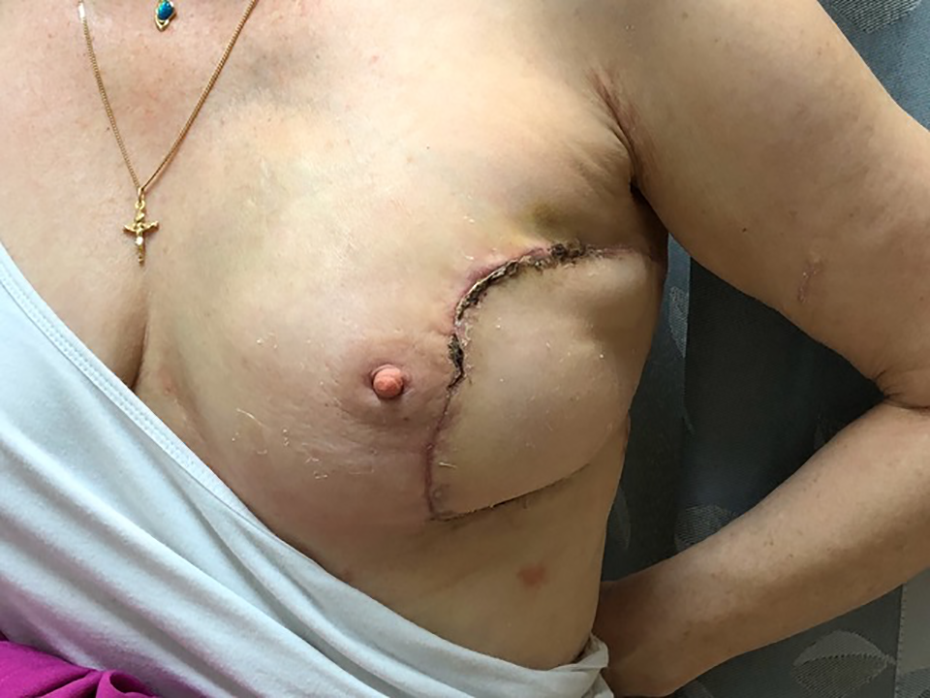
The chest wall three weeks after reconstruction with a DIEP flap to reconstruct breast and lateral chest wall soft tissue defects.
Comment
When managing chest wall tumors that require complex resection and reconstruction, a multidisciplinary approach affords the best chance of success. From an oncological perspective, the extent of chest wall resection required should not be limited by the size of the resulting defect. 4 While any attempt at chest wall reconstruction demands an understanding of both the functional and structural aspects of the final defect and chest wall anatomy.
To achieve both objectives, we developed an approach that combined PMMA with Titanium locking plates. This technique allowed reconstruction of each rib to its normal dimensions to avoid collapse inwards, whilst also permitting independent movement of each rib; allowing normal chest movement. Our approach re–created the anatomical chest wall and reduced chest wall instability. Chest wall stabilization in patients with a large flail segment reduces the incidence of pulmonary complications and duration of ventilatory support. 6 The approach described offers a semi-rigid repair that can be modified to any size, shape, or contour of chest wall defect, while preventing paradoxical movements and chest wall deformity.
Locking Titanium plates provides greater stability, however if there is only a short gap between locked independent sections e.g. adjacent screws either side of a simple fracture, then this can result in a zone of high stress, potentially leading to fracture of the plate over time. In the approach described, this problem is avoided by virtue of the PMMA neo-rib spanning the length of the resected interval. Furthermore, if a fracture was to occur, then the metal plate would be held away from the underlying Polypropylene mesh and lung by the neo-rib, preventing any damage to underlying structures. Other commonly described approaches to rib reconstruction include PMMA neo-ribs secured by suturing pockets between two layers of Polypropylene mesh or other flexible permanent material. However, this approach does not provide rigid reconstruction of the rib and is therefore less stable and likely to allow some paradoxical movement.
A recent experimental study 5 aimed to identify the optimal material for chest wall reconstruction in terms of mechanical behaviour and resistance. Among the tested materials (PMMA, Titanium, Steel and native ribs), PMMA was superior in terms of mechanical behaviour, malleability, and the capacity to customize and weight a prosthesis. When compared to metal, PMMA exhibited better biocomparability with the natural resistance of the native ribs. Additionally, when placed under maximal stress, the PMMA matched native cortical bone.
In summary, rigid reconstruction of rib segments can be achieved with a combination of locking Titanium plates and PMMA neo-rib segments over a flexible permanent or absorbable material. Using this approach, we have shown that chest wall function and form can be restored.
Footnotes
Acknowledgements
We thank the patient for providing consent for images to be used in reporting of this manuscript
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
