Abstract
The Canadian Charter of Freedom and Rights asks us to be mindful of cultural or religious requests when providing healthcare, however alternative medicine is not commonly considered during acute burn resuscitation despite the value patients may place in it. We present a case study of a 46-year-old Amish gentleman with 22% TBSA (TotalBody Surface Area) deep thermal burns who requested traditional Amish burn wound treatment administered by his community elders while an inpatient at our academic burn centre. This case report illustrates the possibility of successful burn wound healing while respecting the traditional cultural beliefs of a patient and his community. Very little is found in the literature to date that describes the blending of traditional and novel treatments in an academic centre, and this largely unstudied area of medicine may present an opportunity for innovation and further discussion about the incorporation of alternative medicine in burn care.
Introduction
The Canadian Amish population was estimated around 5600 in 2019, with the large majority of communities based in Ontario. 1 Similar to Canadian Mennonites, these Anabaptist groups share core Christian beliefs and practices that maintain a unique rural way of life with minimal to no use of technological tools or electrical amenities. Due to these cultural differences from modern society, adults and children are at increased risk of burn injury with higher exposure to open flames, combustible substances, and scalding water. 2,3
Within these communities, traditional home remedies and supplements are often favored over modern medical care, guided by religious roots and cultural separation from present-day society. Significant medical costs are avoided when possible as communities typically do not have private insurance or pay into the provincial healthcare systems; communal resources are paid out for medical services. Resistance and litigation from medical professionals regularly frustrate Amish and Mennonite patients, whose traditional remedies are often met with dismissal. As a result of their cultural beliefs and need to minimize costs, patients often leave hospital early against medical advice in order to allow community elders to use traditional medicine for healing. Herbal products have been used topically in the care of burn wounds for centuries, and have been shown to stimulate burn wound healing. 4 The use of traditional Amish medicine in the treatment of burn wounds in an academic centre has not been previously described.
Case Description
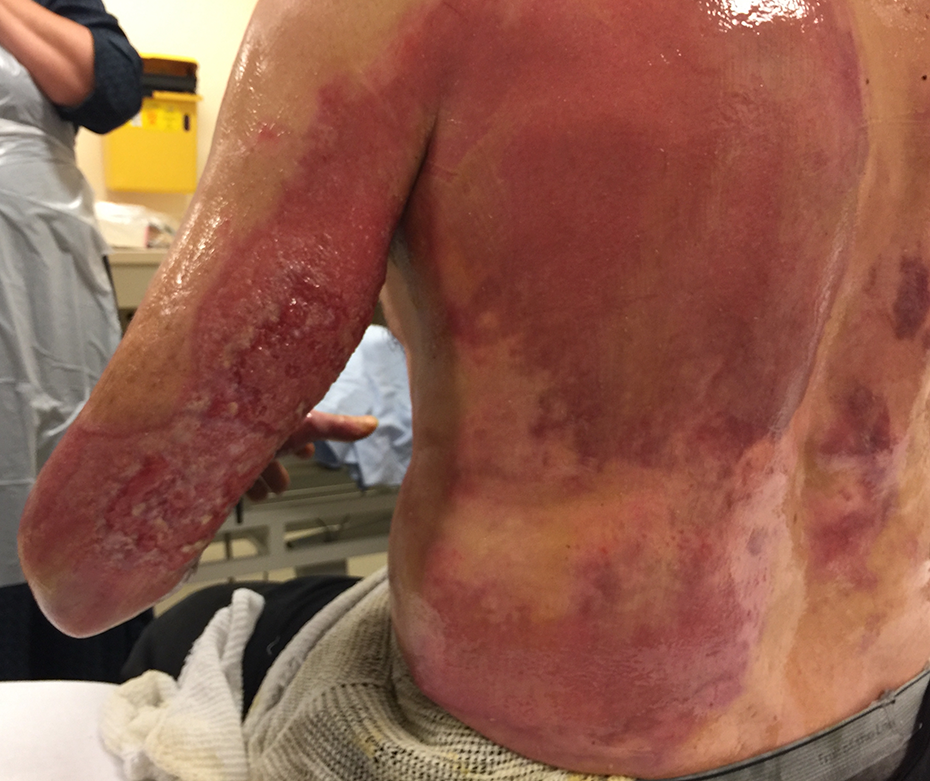
An otherwise healthy 46-year-old Amish man was pulling out of his driveway when a high-speed motorcycle collided with his tractor, resulting in a gasoline explosion. He sustained 22% TBSA superficial partial, deep partial, and full thickness burns which were most extensive on his left back and extending to the medial and posterior left arm and forearm (Figures 1 and 2). His mixed depth burns were further distributed in smaller areas on the chest, hands, and bilateral forearms.
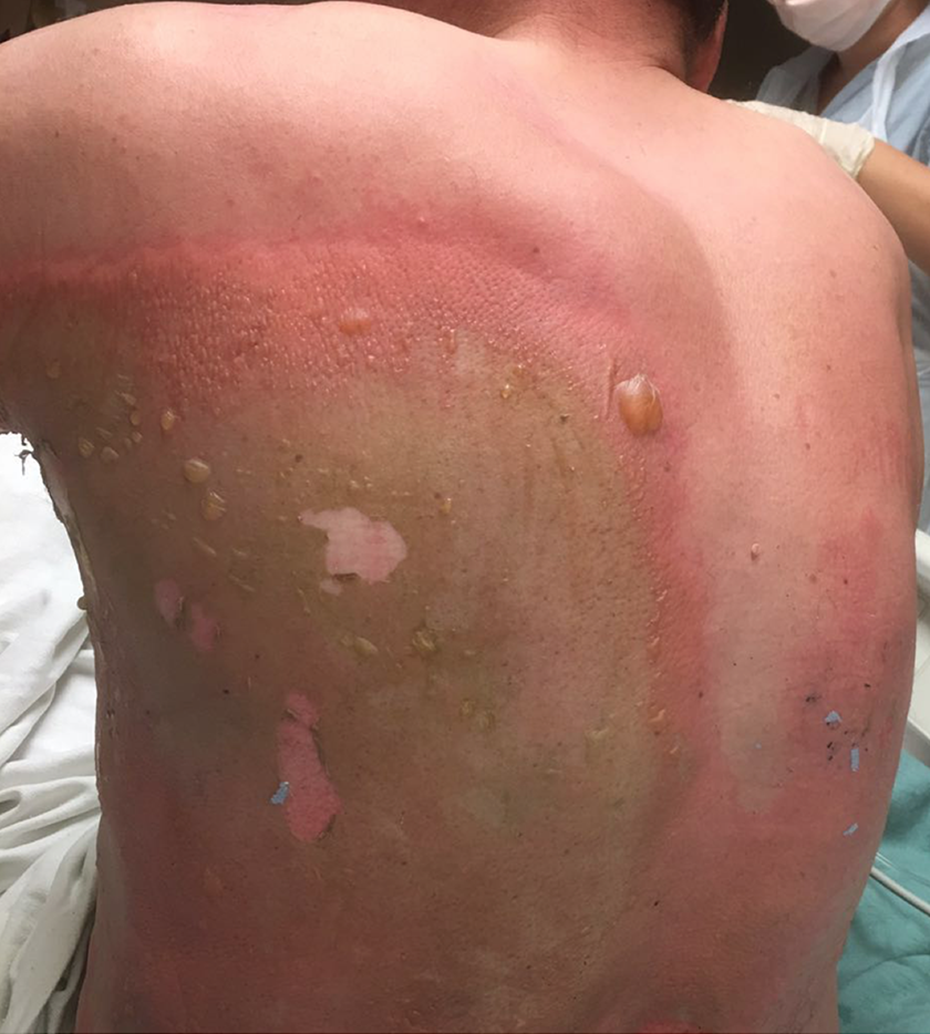
Extensive burns on patient’s back, day of the burn injury.
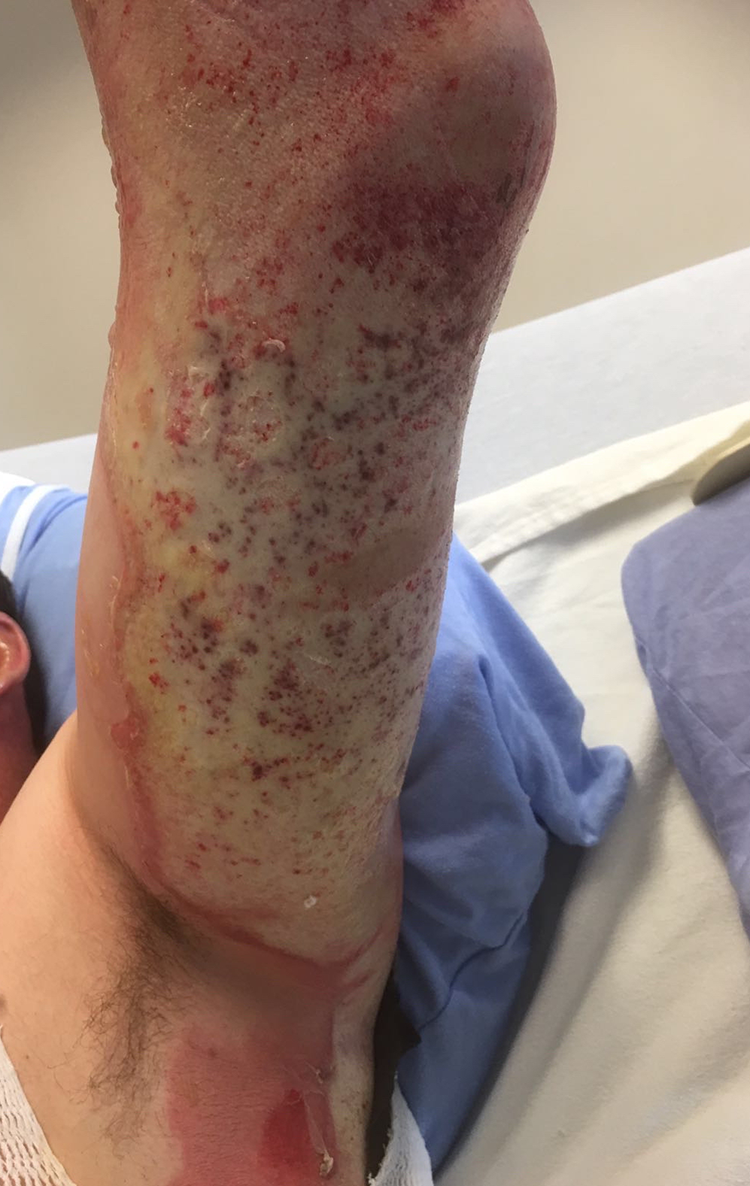
Extensive burns on patient’s left posterior arm, the day of the burn injury.
He was transported to our Burn Centre and his burns were debrided at the bedside, where the appropriate Parkland formula resuscitation was also administered. Full and deep partial thickness burns were dressed with silver sulfadiazine on his left back and arm while the rest were dressed with Acticoat®. The dressings were removed for assessment 2 days after admission. Our recommendation was for early excision and grafting of the deep partial and full thickness burns of his left arm and back, while continuing silver dressings elsewhere. The patient declined the recommended dressing and surgical treatment, emphasizing his preference to trust his elders. They suggested a traditional treatment of his burn wounds, avoiding surgical intervention and using dressings of cold compressed olive oil and burdock leaves.
Extensive discussion with our multidisciplinary team and hospital leadership ensued, and the patient ultimately decided to undergo traditional Amish burn treatment with the compromise that frequent monitoring would take place by our team on the burn unit. When a small cellulitis developed on his left inner arm, the patient and his elders were agreeable to treatment with antibiotics, which was effective. Administrative approval was received from the hospital, and while an inpatient in our academic burn unit his elders applied extra virgin olive oil and Amish Burn & Wounds™ (B&W) Ointment to all burns, covering them with prepared burdock leaves every 12 hours (Figures 3 and 4). After 8 days, as an outpatient at home, this dressing was applied to all burns for 6 weeks. No debridement or cleansing of the burn sites took place with dressing changes, simply reapplication of fresh dressings. A thick, beige pseudo-eschar formed on the wound as it healed, making serial assessment a challenge (Figures 5 and 6).
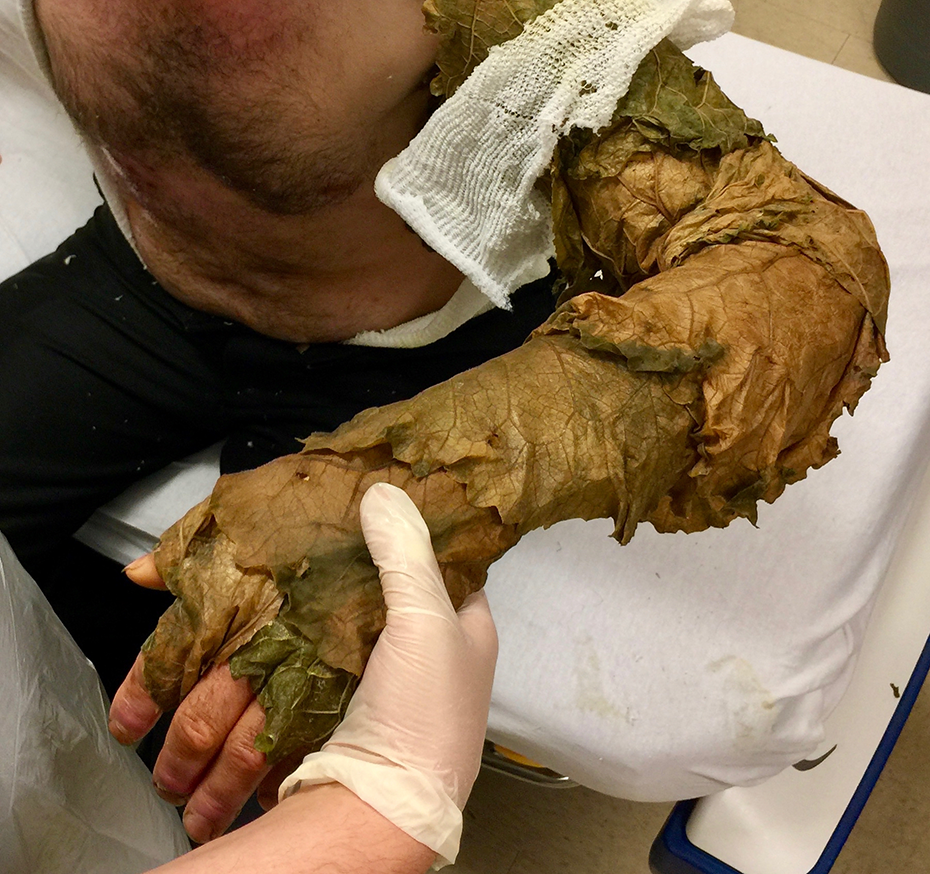
Burdock leaf dressing, applied to patient’s arm.

Drying the burdock leaves, which would be used for wound dressings.
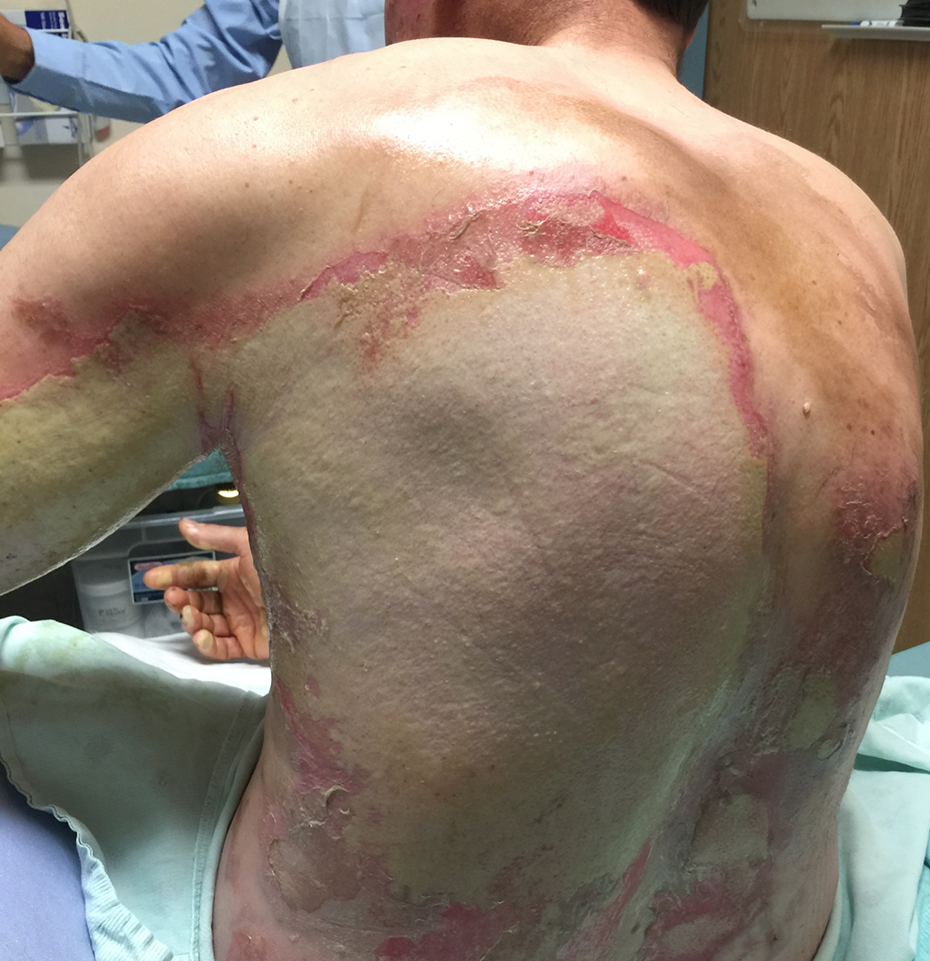
Post burn day #7, showing the thick, beige pseudo-eschar on the back.
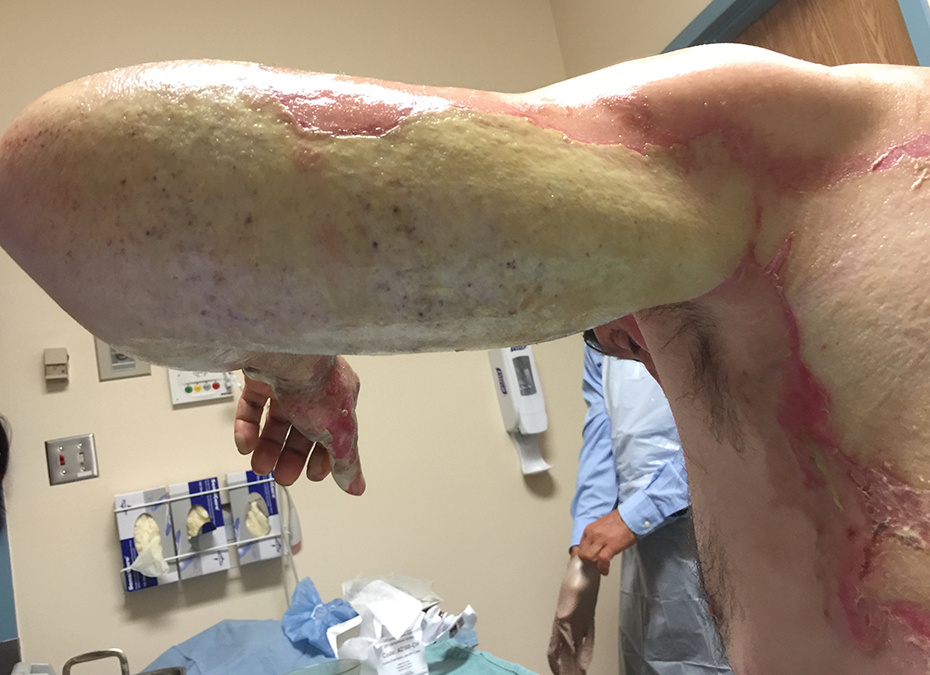
Post burn day #7, showing the thick, beige pseudo-eschar on the posterior arm.
Four weeks following the burn, significant healing had taken place on the back and hypergranulation tissue had formed on the left arm (Figure 7). Bi-weekly visits with the burn specialists occurred for 3 months for close assessment of wounds and physiotherapy needs.
Patient’s arm and back 4 weeks post burn.
Fourteen months post-burn he demonstrated significant hypertrophic scarring of the deep burns near his left elbow with 20 degrees contracture, but self-described no significant functional deficit including with overhead reach (Figure 8 and 9). Disabilities of the Arm, Shoulder, and Hand (DASH) Questionnaire yielded a score of 6/100, gaining points due to mild shoulder stiffness and moderate difficulty in activities requiring free active range of motion. Although the scar outcome was suboptimal through the lens of a plastic surgeon, at 2 years the patient was happy with the result of his care and had no interest in scar contracture release or any revisionary procedures.
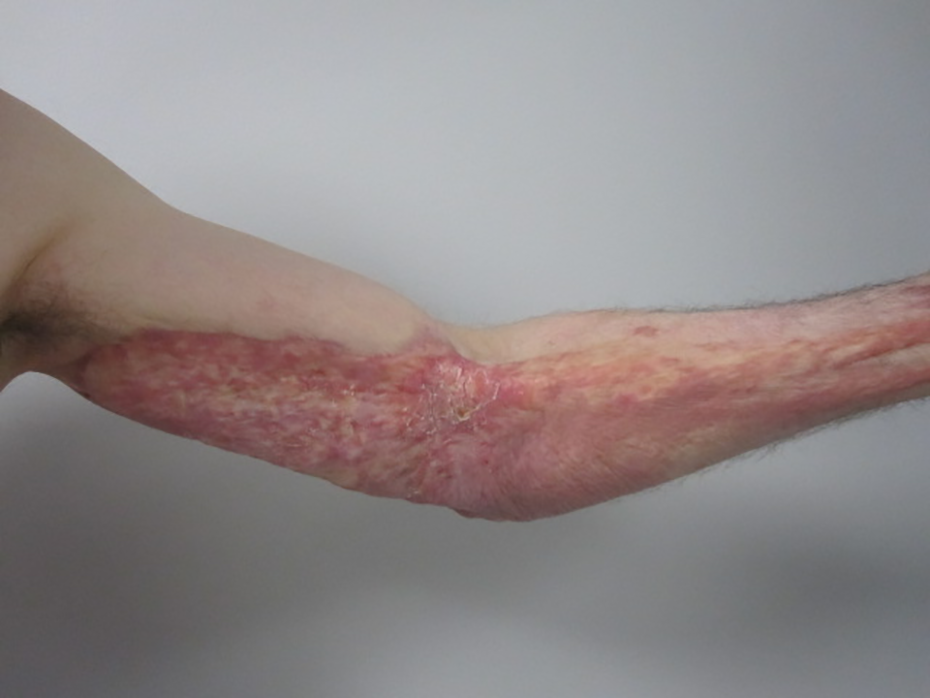
Patient’s left arm 14 months post burn.
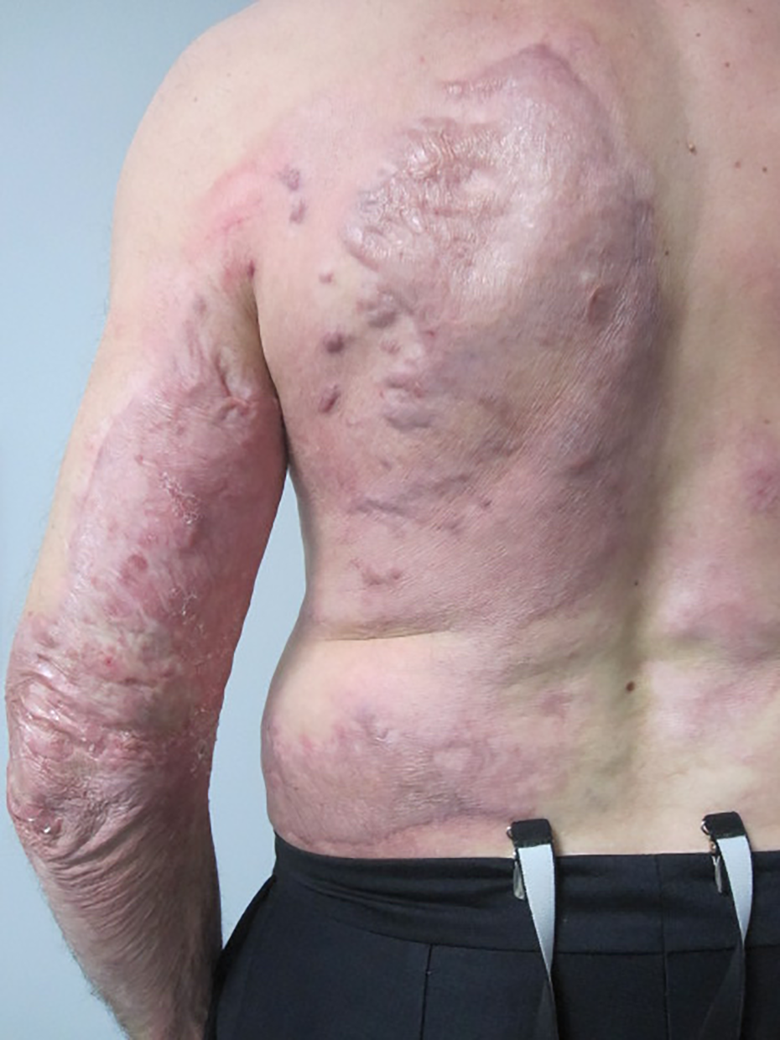
Patient’s back 14 months post burn.
Discussion
This case exemplifies cooperation between modern and alternative medicine that is both safe and successful. An excellent functional outcome was achieved, while remaining within the bounds of the patient’s traditional values and beliefs. Patient safety was consistently the focus of treatment discussions, understanding that close monitoring allowed for intervention by the plastic surgery team should complications occur. Given the challenge of incorporating 2 different theories of medicine, we attribute success to strong communication between the plastic surgery team, community elders, and the patient.
Throughout his healing process, our patient was clear in his goals of care, which included both mitigating cost and returning to work. We were able to achieve an outcome that met these priorities, despite the patient leaving hospital sooner than recommended. Through the trusting relationship built between our burn unit team and the community elders, the patient continued to return for outpatient follow-up which was an integral part of maintaining patient safety and successful healing.
Burn healing is a complex process which can be delayed at any stage by infection, making topical antimicrobial therapy an important consideration in treatment. 4 The burdock plant is shown to have anti-inflammatory, antimicrobial and analgesic properties, and has been used around the world for the treatment of many conditions for centuries. 5,6 By contrast, the B&W™ Ointment contains many natural ingredients that have been individually studied in wound care, but the ointment itself has not been studied for effectiveness. 7 Together, steamed burdock leaves and B&W™ Ointment are used for primary burn care in many Amish and Mennonite communities. 7 Similar to the application of topical antimicrobial agents in modern medicine, local skin reactions resulting from burdock leaves can occur. 4,8 Although fortunately not required in our patient, community elders will often change the dressing material to another type of leaf such as lettuce or plantain to mitigate this reaction. 8
The patient and his community elders anecdotally described the dressing changes as minimally painful and generally very well tolerated. This was confirmed by a pilot study by the Amish Burn Study Group looking at this traditional approach of dressings, suggesting it as an acceptable alternative treatment to conventional burn care for first and second degree burns. 7 Although the assistance required for such frequent changes is extensive, the community often comes together to assist with care, embracing a “more hands make for less work” mentality.
Conclusion
This case report of a 46-year-old Amish male with major burns admitted to our facility illustrates the success of incorporating traditional and novel treatments in burn care. In accordance with the Canadian Charter of Freedom and Rights we strove to uphold excellent medical care while respecting our patient’s cultural and religious values, using modern fluid resuscitation and antibiotic therapy with traditional wound dressings. With the effort of all team members in the patient’s circle of care, including both medical professionals and community elders, safe burn care and healing was achieved. Further discussion and analysis is needed to continue advancing the partnership of alternative medicine in burn care.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article .
Statement of Human and Animal Rights
All human and animal rights were respected in the research and manuscript development of this paper.
Statement of Informed Consent
Written Informed consent was obtained from the patient and it is securely stored.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
