Abstract
Introduction:
Congenital symmastia is notoriously difficult to treat. Many management approaches have been reported but none seem to address the root cause of the anatomic deformity and may result in significant scarring.
Method:
We propose a minimally invasive approach to treating congenital symmastia with good results and minimal scarring by liposuction and use of a fibrin sealant.
Conclusion:
Liposuction of the pre-sternal area and injection of fibrin sealant as an adhesive with post-operative pressure garment support worked well to create and maintain a good cleavage.
Introduction
Symmastia is a medial confluence of the breasts. 1 It consists of 2 forms, namely iatrogenic/acquired and congenital. 2 Iatrogenic symmastia 3,4 is a complication arising from breast augmentation, whereas congenital symmastia is abnormal proliferation of subcutaneous tissue in the intermammary web crossing the sternal midline. It is a relatively rare condition and only a few cases have been reported. 5
Both forms are difficult to manage; however, effective options for correction of iatrogenic symmastia are well documented in the literature (capsulorrhaphy, neo-subpectoral pocket dissection, and acellular dermal matrices). Several surgical approaches in treating congenital symmastia have also been reported and include breast reduction with or without liposuction, intermammary quilting, and resection of the medial breast tissue and fixation using dermal matrix), but there is no gold standard of treatment. 6 -9 We present a novel approach in treating symmastia by liposuction of the pre-sternal fat and application of a surgical adhesive to attempt to obliterate the dead space, thereby recreating the cleavage.
Case
A 20-year-old female was referred to our plastic surgery department for consultation regarding a lack of cleavage (Figure 1). Clinical examination revealed a moderate congenital symmastia. Computed tomography reported “a natural symmastia” between T3 and T7 with fatty tissue but no breast glands (Figure 2). The patient wore C cup brassieres and was happy with the size and volume and did not wish for invasive surgery.
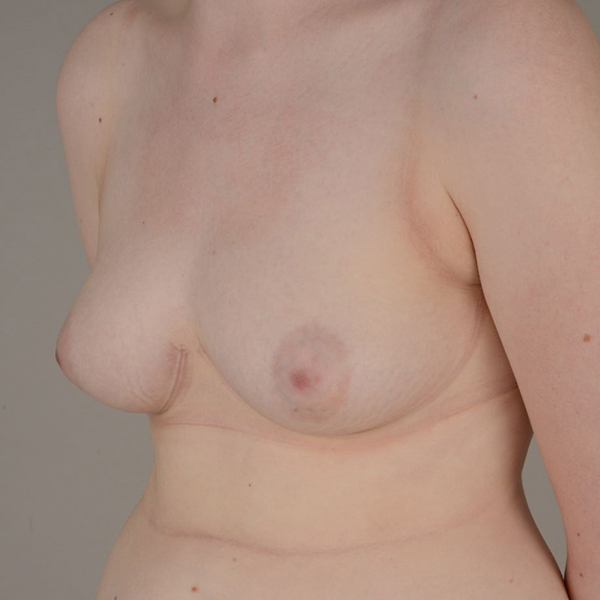
Mild congenital symmastia in a 20-year-old female.
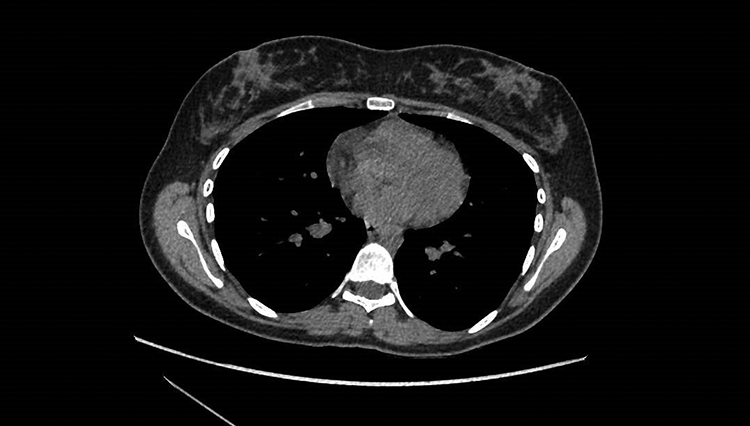
Computed tomography imaging depicting the extend and size of the symmastia.
We considered different approaches guided by a literature search, but none seem to offer the ideal of a good outcome with minimal scarring. We decided on a new approach, using a surgical fibrin sealant: Tisseel (Baxter) which is used as an adjunct to haemostasis and standard surgical techniques to prevent leakage. The patient was consented, and she underwent surgery as planned.
Procedure
Our management followed a 2-step approach. The aim of our surgical approach was to remove the excess pre-sternal fat and the second step was to compress the dead space to produce a deeper cleavage.
The pre-sternal fat was liposuctioned via a small inferior medial incision and 100 mL was obtained. Thereafter, we prepared the Tisseel following the manufacturer’s guideline and 4 mL was injected into the area via a wide bore cannula to best reach the apex of the space and compressed for 10 minutes (Figure 3). We noticed a significant reduction of the pre-sternal area with good adherence of tissues, forming a normal breast footprint (Figure 4).
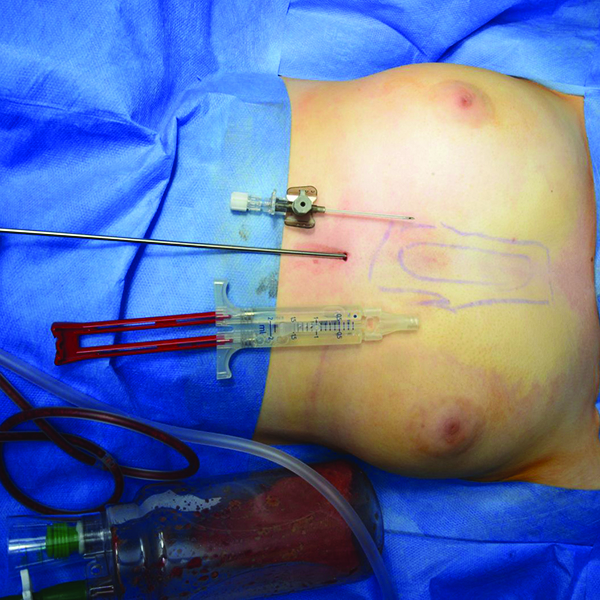
Liposuction of the pre-sternal fat, application of Tisseel and compression.
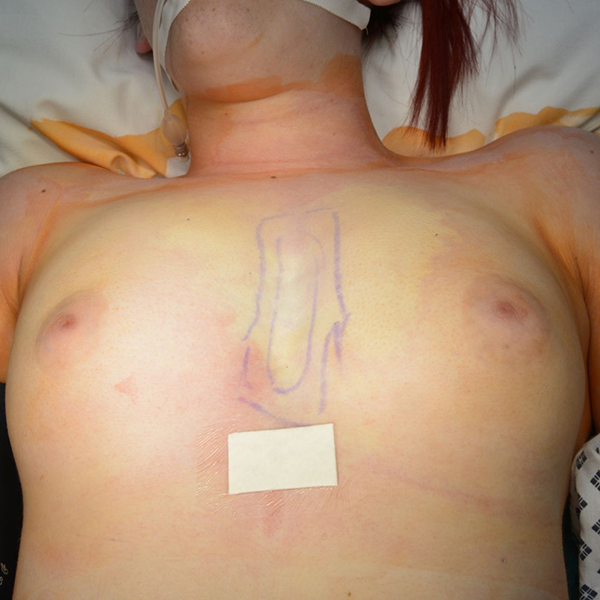
Results post compression and prior to application of bra (with bolster).
Post-operatively, she was provided a custom-made foam bolster to facilitate pre-sternal compression and an overlying support garment similar to a reversed sports bra. The design of the garment is similar to that of the Thongbra Inc, (Berlin, Maryland, USA) but was actually developed independently by our pressure garment therapist for a case of burn injury–related symmastia treated several years previously.
The patient wore her bra continuously for 6 weeks and when reviewed in clinic and her cleavage has retained. She continued to wear the garment for a further 6 weeks during the day only (Figure 5).
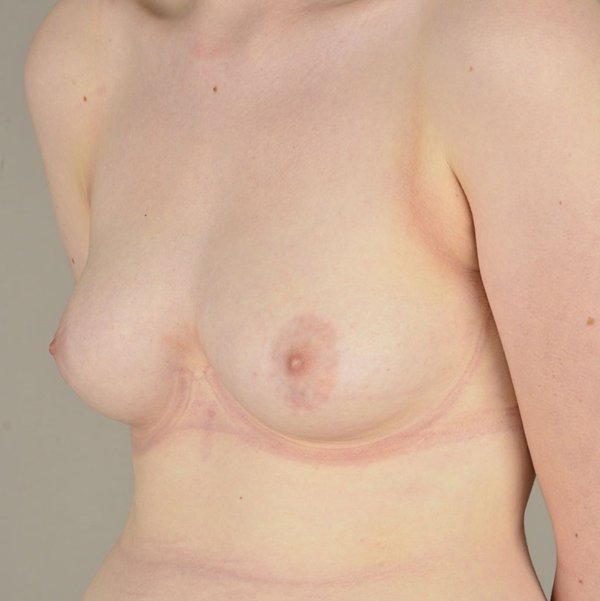
Results 12 weeks post-operatively.
Conclusion
Currently, the majority of treatments reported result in significant scarring and may need further procedures. We were able to improve the cleavage by correcting the pre-sternal fatty tissue and the breast footprint through a minimally invasive and easy to perform procedure with no recurrence at 4 months. Our patient was extremely happy with the outcome.
Supplemental Material
Supplemental Material, Supplemental_Figure_1 - A Simple and Novel Approach in Treating Congenital Symmastia (Using Tisseel in a 2-Step Approach)
Supplemental Material, Supplemental_Figure_1 for A Simple and Novel Approach in Treating Congenital Symmastia (Using Tisseel in a 2-Step Approach) by Bismark Adjei, Susie Z. Yao, Ashraf Mostafa and Ommen Koshy in Plastic Surgery Case Studies
Supplemental Material
Supplemental Material, Supplemental_Figure_2 - A Simple and Novel Approach in Treating Congenital Symmastia (Using Tisseel in a 2-Step Approach)
Supplemental Material, Supplemental_Figure_2 for A Simple and Novel Approach in Treating Congenital Symmastia (Using Tisseel in a 2-Step Approach) by Bismark Adjei, Susie Z. Yao, Ashraf Mostafa and Ommen Koshy in Plastic Surgery Case Studies
Supplemental Material
Supplemental Material, Supplemental_Figure_3 - A Simple and Novel Approach in Treating Congenital Symmastia (Using Tisseel in a 2-Step Approach)
Supplemental Material, Supplemental_Figure_3 for A Simple and Novel Approach in Treating Congenital Symmastia (Using Tisseel in a 2-Step Approach) by Bismark Adjei, Susie Z. Yao, Ashraf Mostafa and Ommen Koshy in Plastic Surgery Case Studies
Supplemental Material
Supplemental Material, Supplemental_Figure_4 - A Simple and Novel Approach in Treating Congenital Symmastia (Using Tisseel in a 2-Step Approach)
Supplemental Material, Supplemental_Figure_4 for A Simple and Novel Approach in Treating Congenital Symmastia (Using Tisseel in a 2-Step Approach) by Bismark Adjei, Susie Z. Yao, Ashraf Mostafa and Ommen Koshy in Plastic Surgery Case Studies
Footnotes
Authors' Note
This study was presented at The European Society of Plastic, Reconstructive and Aesthetic Surgery Meeting (ESPRAS) 2018 in Limassol, Cyprus (Poster presentation).
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Statement of Informed Consent
Informed consent has been given by the patient for publication of the clinical images, which have no patient identifiers on them and the patient cannot be identified from the images.
Statement of Human and Animal Rights,or Ethical Approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
