Abstract
Carpal tunnel syndrome (CTS) is a neuropathy brought about by the entrapment and compression of the median nerve as it travels through the carpal tunnel. The hallmark of classic CTS is pain or paraesthesia (numbness, burning, or tingling) in the palmar aspect of the first 3 digits, as well as the radial aspect of the fourth digit. Although idiopathic in nature, many risk factors have been attributed to the development of CTS. These factors include diabetes mellitus, acromegaly, thyroid disease, rheumatoid arthritis, pregnancy, the use of steroids, and the repetitive use of hand and wrist. The prevalence also seems to be higher in obese women. In literature, trauma, foreign body, tumors, or anatomical variations are considered to be infrequent causes of CTS.
A rare form of CTS is the acute carpal tunnel syndrome (ACTS) that presents mainly after injuries to the upper extremities. The patient typically acknowledges trauma to the wrist secondary to a foreign body at the time of injury. In some cases, small fragments may penetrate the wrist and remain unnoticed causing acute neurological symptoms. In literature, there were limited studies that reported the development of ACTS secondary to missed foreign bodies following trauma. This report presents a case of ACTS sustained following a penetrating foreign body (pellet) to the right wrist. Removal of the foreign body resulted in complete recovery with no neurological sequelae.
Introduction
Carpal tunnel syndrome (CTS) is a neuropathy brought about by the entrapment and compression of the median nerve as it travels through the carpal tunnel. The hallmark of classic CTS is pain or paraesthesia (numbness, burning, or tingling) in the palmar aspect of the first 3 digits, as well as the radial aspect of the fourth digit. Although idiopathic in nature, many risk factors have been attributed to the development of CTS. These factors include diabetes mellitus, acromegaly, thyroid disease, rheumatoid arthritis, pregnancy, the use of steroids, and the repetitive use of hand and wrist. The prevalence also seems to be higher in obese women. 1 In literature, trauma, foreign body, tumors, or anatomical variations are considered to be infrequent causes of CTS.
A rare form of CTS is the acute carpal tunnel syndrome (ACTS) that presents mainly after injuries to the upper extremities. 1 The patient typically acknowledges trauma to the wrist secondary to a foreign body at the time of injury. In some cases, small fragments may penetrate the wrist and remain unnoticed causing acute neurological symptoms. 2 In literature, there were limited studies that reported the development of ACTS secondary to missed foreign bodies following trauma.
This report presents a case of ACTS sustained following a penetrating foreign body (pellet) to the right wrist. Removal of the foreign body resulted in complete recovery with no neurological sequelae.
Case
A 53-year-old gentleman, not known to have any medical illnesses, presented to our clinic on January 05, 2020, with the complaint of 2 days history of numbness in the right thumb and index finger and a feeling of a solid mass in his right wrist. The patient was attempting to clean his air gun and an accidental fire was shot, thus sustaining a penetrating injury to the right hand a week prior to presentation. There was no neurological deficit at the time of injury. An ultrasound scan was performed and it confirmed the presence of a foreign body measuring 0.2 × 0.8 cm in dimensions, seated very close to the flexor retinaculum of the right hand at the level of the wrist with associated mild reactive edema of the surrounding tissues. A baseline Anterio-Posterior X-ray of the right hand was also performed which showed a radiopaque foreign body on the volar aspect of the proximal right hand in relation to the carpal bones and carpometacarpal joint. There were no bony injuries or fractures seen.
Upon physical examination there was a puncture/entry wound, 2 × 2 mm in size, in the center of the palm (halfway between the thenar and hypothenar eminence), around 2 cm distal to the distal wrist crease. There were no signs of reduced sensation in the right hand. All finger movements were found to be normal and the thenar motor function was intact.
The patient underwent exploration and retrieval of right palm foreign body (pellet) on January 19, 2020. He was operated upon under general anesthesia with proximal tourniquet to achieve hemostatic control. Fluoroscopic guidance with portable Computed-Radiography X-ray was used to aid in localization of the pellet (Figure 1). Magnification was achieved with the help of magnifying loupes. A linear incision was performed at the level of flexor retinaculum and was extended proximally. Intraoperative findings showed right palm foreign body (pellet) at the level of carpal bones. The pellet was found embedded in the median nerve with epineural swelling, but no injury to the nerve itself (Figure 2). The pellet was retrieved carefully (Figure 3). A repeat imaging was done following the extraction that confirmed complete retrieval of the foreign body (Figure 4). Closure of skin was done with 3/0 ethilon, after hemostasis with bipolar diathermy.
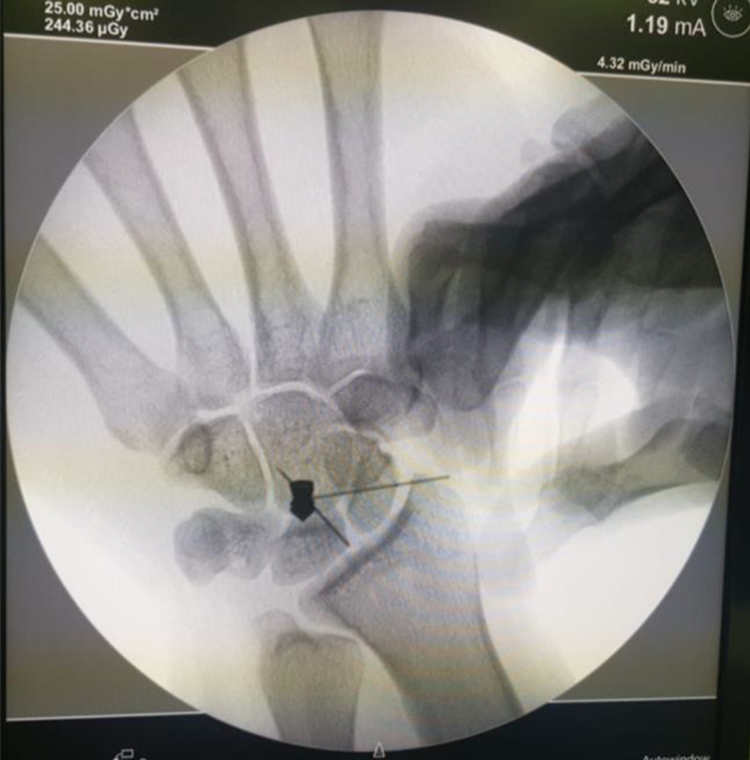
Pre-operative Anterio-posterior Computed-Radiography X-ray of the right wrist with needle localization of the foreign body.
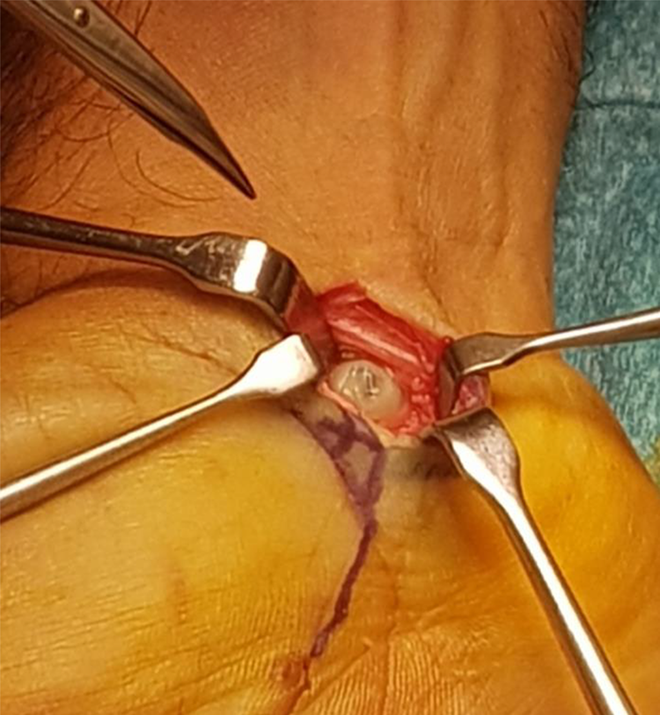
Intraoperative image of the foreign body embedded within the median nerve.
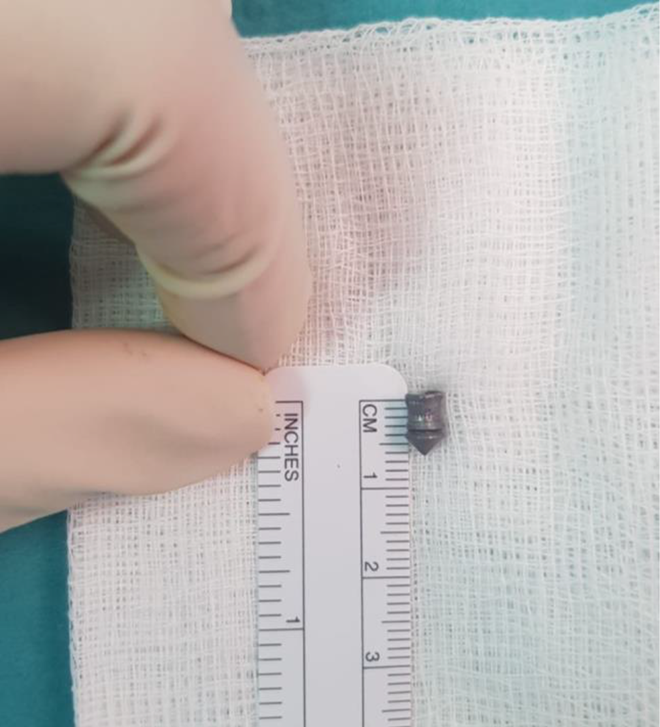
The pellet post retrieval measuring around 6 mm.
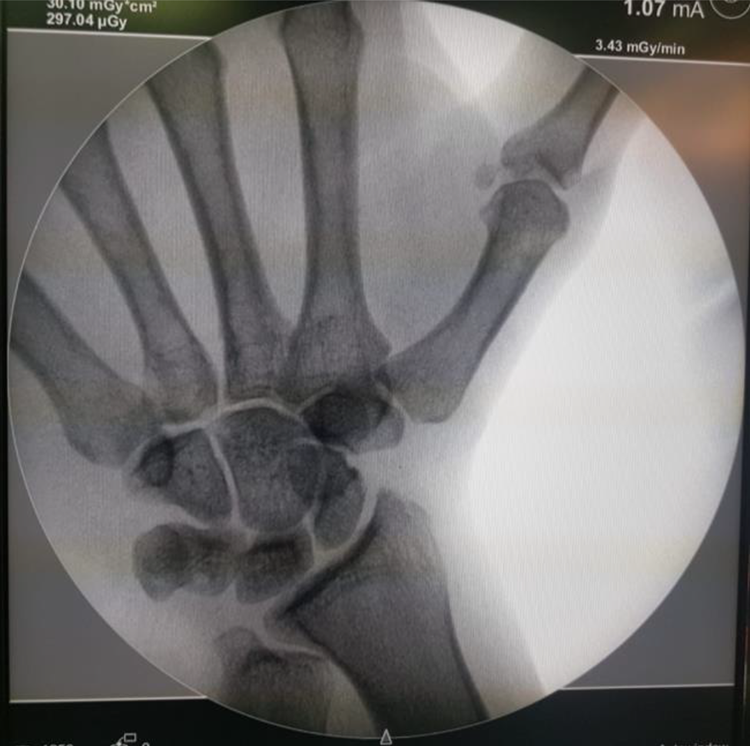
Post-operative Anterio-posterior Computed-Radiography X-ray of the right wrist.
Post-operatively, both motor and sensory functions of the right hand were checked and were intact. The patient was discharge in a stable condition and close follow-up.
He was reviewed in clinic 2 day after the operation. He reported no numbness in the median nerve distribution of the right palm, and there was no motor deficit. The wound was clean and stitches were intact. The stitches were removed after 10 days from the operation, and the patient showed complete resolution of symptoms.
Discussion
Carpal tunnel syndrome is a chronic neuropathy that is progressive in nature, often occurring over the course of weeks or months, eventually resulting in the impairment of hand function. Acute carpal tunnel syndrome on the other hand develops rapidly within days. Foreign bodies, hematomas, or mass lesions should always be excluded in patients who present with a short history of symptoms. 1
Injuries to the median nerve secondary to foreign bodies are most likely to cause immediate symptoms of numbness, paraesthesia, reduced sensation, or motor dysfunction. 2 Nonetheless, some foreign bodies may remain undetected and asymptomatic for long period and thus might lead to a variety of complications that include abscess formation, chronic discharging wound, necrotizing fasciitis, granulomas, migration of body, neurodeficits, or vascular events. 3
Precise preoperative localization of the foreign body is vital for successful surgical retrieval. Despite thorough physical examination, physicians may still miss up to 38% of foreign bodies. 1 Manual examination (palpation) and radiological investigations should always be performed for an accurate diagnosis of suspicious foreign bodies. 4
The choice of radiological imaging varies according to the foreign body material. Radiopaque objects are easily detected on plain films. Difficulty arises with radiolucent objects, such as wooden splinters. In these cases, an ultrasound, computed tomogram (CT), or infrequently magnetic resonance imaging) can be done. These modalities can also be beneficial in providing further information regarding the exact location of retained body and its relationship to the nearby structures. 2,3 This can guide the surgeon in his approach to surgical exploration. Some studies advise for ultrasonography as a first-line imaging for radiolucent objects, while CT scan to be done in cases of complex injuries. 1
Correct localization of foreign bodies is crucial to a successful surgical retrieval. Surgical exploration followed by removal of the body is the treatment of choice. These surgeries are mostly done as a day case procedure, under local anesthesia/block. Failure to accurately locate the object can result in long manipulations, and might cause extensive soft tissue injury. 4 In some literature, the use of intraoperative ultrasonography for an accurate localization has been recommended to increase the chance of a successful surgery, reduces operative time, and minimizes soft tissue manipulation. 3
Conclusion
The aim of this case report is to highlight the fact that foreign bodies should always be considered in patients who present with acute symptoms of pain in the hands following history of trauma. Thorough examination and proper imaging for an accurate localization, followed by surgical exploration are essential to prevent future complications.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Statement of Human and Animal Rights
All humans in the study have been approved by the appropriate ethics committee and therefore have been performed in accordance with the ethical standards.
Statement of Informed Consent
All persons gave their informed consent prior to their inclusion in the study.
