Abstract
Ledderhose disease, or plantar fibromatosis, is a rare benign disorder of fibrous proliferation in the plantar aponeurosis. It is known to be highly associated with Dupuytren disease of the hand by sharing similar symptomatology and treatment methods. This case study explores a presentation of Ledderhose disease in a 56-year-old male with concomitant Dupuytren contracture. The patient underwent surgical excision resulting in symptomatic relief with regained function. This case highlights diagnostic measures, association with Dupuytren disease, and both surgical and nonsurgical treatment methods of Ledderhose disease.
Introduction
Ledderhose disease, also commonly known as Dupuytren of the foot or plantar fibromatosis, is a rare benign disorder of fibrous proliferation in the plantar aponeurosis. 1,2 It is well defined in the medial or central region of the plantar fascia, causing painful nodules. 2,3 It is only in rare instances that Ledderhose disease causes toe contractures. Patients with Ledderhose present with pain and swelling of the foot and inability to ambulate if the disease is left to progress without treatment. 4
Although first described by Georg Ledderhose in 1897, the etiology of the disease is still unknown. 2 Current theory suggests the pathology may be a compensatory response to mechanical forces. 5 Ledderhose disease has an estimated incidence of 1 to 2 per 100 000 and is more common in males. 6 It is often associated with Dupuytren disease of the hand and Peyronie disease of the penis. This subset of diseases shares similar symptomatology in different anatomical regions as well as different patient demographics. 7 Further, immunohistochemical and ultrastructural studies have shown that both Ledderhose and Dupuytren diseases share similar fibroblast and myofibroblast composition, suggesting that they are different expressions of the same disorder. 8 Diabetes mellitus, liver disease, alcohol abuse, epilepsy, and repeated trauma have all been frequently described in association with development of lesions in all 3 conditions. 1,5,9,10 Ledderhose and Dupuytren diseases have shown the highest association, ranging from 2% to 25% concomitance rate. 3,6,9,11
One of the most challenging aspects of treatment in both Ledderhose and Dupuytren disease is symptom recurrence described by either continuous pain or failure of conservative measures. A recent systematic review of the literature reported a 69.3% recurrence rate after operative intervention. 7 Despite a vast array of options for both conservative and surgical approaches, no gold standard intervention exists. As with Dupuytren disease, a treatment algorithm that factors disease severity, patient preference, and concern for recurrence should be utilized in the management of Ledderhose disease. 5 We present a case in which both diseases occurred concomitantly and the patient achieved symptomatic relief with surgical intervention.
Case Report
A 56-year-old Caucasian male presented to our institution with a 5-year history of bilateral palpable nodules within the medial plantar region. The patient reported an increase in size and tenderness over the past 6 months, particularly after standing or ambulating for long periods. The plantar pain was accompanied by bilateral ankle pain which induced alterations in gait. This caused significant occupational limitations related to prolonged ambulation.
Of note, the patient also had a history of severe Dupuytren contracture. He was treated surgically with palmar fasciectomy 8 years prior but unfortunately developed a recurrent contracture in the left long finger proximal interphalangeal joint (PIP) joint. He denied pertinent past medical history but did report daily alcohol consumption.
Clinical examination revealed a 4 × 5 × 5 cm lesion of the medial left plantar surface which extended just proximal to the first metatarsophalangeal joint. The mass was tender, erythematous, soft, and multilobular with no overlying skin or sensation changes. A nearly symmetrical lesion was located on the right foot measuring 3 × 4 × 5 cm. No imaging modalities were utilized to further evaluate the lesions. Due to worsening pain and limitations in daily living, surgical excision of these plantar fibromas was offered. The patient elected to undergo intervention for the more symptomatic lesion.
A curvilinear incision was made over the right lesion, followed by sharp dissection with tenotomy scissors to raise skin flaps. First, a localized area of fibrosis was identified. Meticulous dissection was undertaken to isolate the scar tissue from underlying tendon and microvascular structures which are visible in Figure 1. Then, once isolated, the mass was fully excised as demonstrated in Figure 2. The wound was irrigated and closed with 4-0 Nylon suture. Pathology results confirmed the diagnosis of plantar fibromatosis.
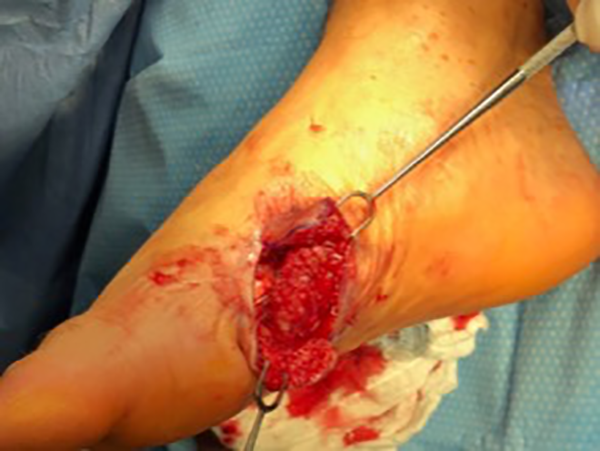
Planter fibromatosis in situ.
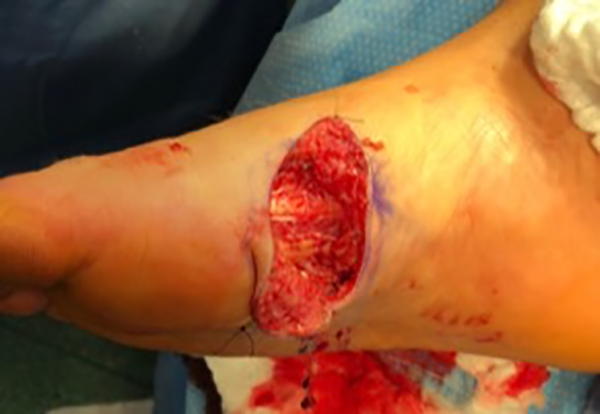
Wound bed after full excision of mass.
The patient returned to clinic 2 weeks postoperatively, and the incision was noted to be healing well with no evidence of infection. He reported mild tenderness but required no narcotic medication for pain control. A small hematoma was present which resolved without intervention. Sutures were removed 4 weeks postoperatively. The patient’s final visit at 6 weeks showed a vast improvement in pain compared to his preoperative baseline. No signs of recurrence were observed.
Discussion
Ledderhose disease is a benign condition most notably characterized by local proliferation of fibrous tissue in the plantar fascia or plantar aponeurosis. 12 Diagnosis of Ledderhose disease is usually a clinical diagnosis and requires no further testing, but correlating clinical findings with radiology and histology can help significantly in confirming the diagnosis, as the differential includes plantar fasciitis, leiomyoma, rhabdomyosarcoma, and liposarcoma. 6,13 Griffith et al demonstrated that sonographic visualization between the lesion and the plantar fascia was the most useful finding to exclude possibilities of neuroma or soft tissue tumors. 8 Magnetic resonance imaging (MRI) has also proved to be useful in showing deep extension of advanced lesions into the musculature, although the cost and effectiveness of sonography make it the preferred option for diagnosis. 3 Therefore, MRI may be more appropriate as a tool for surgical planning by accurately defining the extent of the lesion to permit complete surgical resection. 14
Histologic findings of myofibroblast proliferation with elongated oval-shaped nuclei and deposition of type III collagen can further strengthen the diagnosis for plantar fibromatosis. Clinicopathological studies have classified Ledderhose disease into 3 stages: (1) proliferation with increased fibroblast activity, (2) involution with physical nodule formation, and (3) residual stage with collagen maturation and tissue contracture. 2,9 It is particularly interesting to note that these pathologic stages correlate linearly with the progression of Dupuytren disease. The palmar fascia of Dupuytren patients is defined by myofibroblast influx and concentration of type III collagen, leading to cord formation and contracture. 5 Unlike Dupuytren disease, however, contracture in Ledderhose seems to be rare. This is attributed to the anatomic nature of the plantar fascia which is divided by thinner and more insignificant longitudinal slips than those of the palmar fascia, thereby avoiding the flexion deformity of the toes. 15 Not surprisingly, both diseases share common treatment methods consisting of a combination of nonsurgical and surgical measures.
Nonsurgical treatment involving intralesional steroid injection, collagenase clostridium histolyticum injection, anti-inflammatory drugs, radiotherapy, orthoses, stretching, or physical therapy should first be considered. 1,7 There have been several studies demonstrating the effectiveness of radiotherapy, including its capacity to prevent progression of both Dupuytren and Ledderhose disease when applied early in the course. 16 Mella et al have formulated a simplified treatment algorithm incorporating patient-, disease-, and intervention-related factors. 5 If a patient develops recurrence less than 1 year from a nonsurgical treatment, the algorithm suggests the patient would benefit from an operative approach. In cases of aggressive recurrence or inhibition of daily activities, surgical treatment is indicated. 2
Surgical treatments have been shown to mitigate pain. Methods include local resection, wide excision, subtotal, or complete fasciectomy. Partial fasciectomy and wide excision have been shown to produce the lowest recurrence rate. 7 One-centimeter margins of normal aponeurosis are recommended to ensure complete excision of affected fascia and reduce the possibility of relapse. 2 Surgery is not without risks, however, and patients are vulnerable to complications such as skin necrosis, infection, plantar neuroma, and nerve laceration. 9 The treatment plan can be individualized and should incorporate key patient information such as number and dimension of lesions, previous history of disease, patient’s personal risk factors, financial concerns, and effect on daily living.
The aforementioned patient was offered surgical excision, given the debilitating nature of his pain and the well-circumscribed nature of his lesions. He experienced significant unilateral symptomatic relief and reportedly wishes to undergo contralateral fasciectomy in the near future. This case highlights the value in holding a high index of suspicion for associated disease processes throughout the plastic surgeon’s clinical evaluation. The patient’s Ledderhose disease was diagnosed and successfully treated after his presentation for recurrent Dupuytren contractures. A thorough examination includes appreciation of not only Ledderhose disease but other ectopic disease such as Garrod’s pads or Peyronie disease. 5
Conclusion
Ledderhose disease is a benign proliferative condition of the plantar aponeurosis that can cause significant debilitation and dysfunction. We present a case of Ledderhose disease that was diagnosed in conjunction with recurrent Dupuytren disease. The patient was offered surgical excision and experienced symptomatic relief with improved function. This case serves to underscore the association of Ledderhose disease with a prevalent plastic surgery disease process as well as the potential benefit of surgical intervention.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Statement of Human and Animal Rights
Research was conducted according to the World Medical Association Declaration of Helsinki.
Statement of Informed Consent
Written informed consent for patient information and images to be published was provided by the patient.
