Abstract
This is the first report of pilomatrix carcinoma in a man with C282Y myotonic dystrophy type 1. This pilomatrix carcinoma had originally presented as a rapidly growing recurrence of a histopathologically confirmed pilomatrixoma, removed a year prior. On examination, the fungating mass had measured 10 × 23 cm. A wide local resection with removal of suspicious lymph nodes was preformed, and the resulting defect was reconstructed with a latissimus dorsi myocutaneous flap and skin graft. Histologic investigation of the excised mass confirmed the diagnosis of pilomatrix carcinoma. This is the first reported case of pilomatrix carcinoma in a patient with a genetic condition that often presents with scalp pilomatrixomas. Potential implications of myotonic dystrophy on developing pilomatrix carcinoma are discussed.
Introduction
Pilomatrix carcinoma is an extremely rare malignant tumor that was first identified by Lopansri and Mihm in 1980. 1 This malignant tumor arises from hair follicle matrix cells, from which it gets its name. Contrary to original descriptions, pilomatrix carcinoma can be locally aggressive and has the potential for recurrence and significant morbidity. Regional lymph node and systemic metastases occur in approximately 13% of the reported cases. 2 -6 Clinically, pilomatrix carcinoma often presents in the head and neck region as a non-tender, firm dermal swelling, although it can be found all over the body. 3,5,7 -11 Pilomatrix carcinoma has been shown to have a male predominance and most commonly occurs in the fifth to seventh decade of life. 6 Given its rarity, the pathogenesis of pilomatrix carcinoma and its predisposing risk factors remains unknown. One hypothesis is that pilomatrix carcinomas arise from malignant transformation of pre-existing benign pilomatrixomas. Pilomatrixomas are benign tumor of hair follicle cells, are far more prevalent than pilomatrix carcinomas, and have been associated with a number of genetic conditions, including myotonic dystrophy (DM).
Myotonic dystrophy is the most common adult muscular dystrophy, primarily associated with myotonia and muscle weakness, although other clinical features have been documented. 12 Myotonic dystrophy is categorized into DM type 1 and DM type 2, depending on the affected gene. Both types are a collection of autosomal dominant, multisystemic diseases that arise from unstable nucleotide repeat expansions in the untranslated regions of 2 unrelated genes. 12 Of the two, DM type 1 is more common. 13 It is well reported that patients with DM are at an increased risk of developing tumors, with pilomatrixomas being the most common. 12 To date, no report of pilomatrix carcinoma developing in patients with a genetic condition has been published in the literature. To the best of our knowledge, we present the first documented case of pilomatrix carcinoma in a patient with DM.
Case Report
A 36-year-old Caucasian male, with heterozygous C282Y DM type I presented to the clinic regarding a possible recurrence of a lesion on his left posterior scalp. A previous biopsy confirmed pilomatrixoma had been excised from the same location a year prior with clear margins. Within 2 months of the lesion presentation, it had grown rapidly with bleeding, discharge, and drainage. With the exception of occasional pain over the area of the mass, no other symptoms were reported by the patient. On examination, the patient had a 10 × 12 cm hemorrhagic, fungating cutaneous mass with peripheral ulceration and purulent discharge, on his left occipital scalp (Figure 1). No occipital or cervical lymphadenopathy was appreciated on clinical examination. Due to the appearance, growth, and location of this lesion, a malignant transformation versus possible de novo malignancy of pilomatrix carcinoma was suspected. Complete surgical excision was recommended.
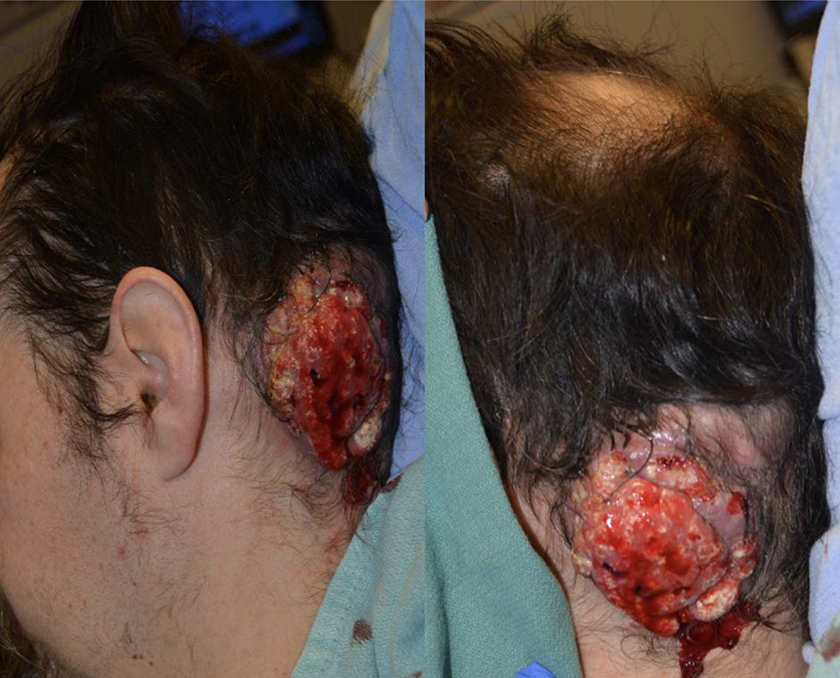
Fungated mass of left posterior scalp, measuring 10 × 12 cm.
A computed tomography (CT) scan was obtained for surgical planning. Results of the CT scan suggested a deeply infiltrative mass extending to the periosteum, without evidence of cortical skull bone invasion. One slightly rounded homogenously enhancing lymph node was identified in the left neck at the level Va, measuring 13 × 11 mm. This lymph node was noted by radiology to be potentially concerning of malignancy, should the pathological finding of the scalp lesion be malignant in nature. No preoperative biopsy was completed. After discussion with the patient, primary surgical treatment was recommended.
A wide local excision of the primary tumor was completed with excision of the lesion including the periosteum and an elective lymph node biopsy of levels II-V. The defect was reconstructed with a musculocutaneous latissimus dorsi free flap. A split thickness skin graft was used to cover exposed muscle not covered by the skin paddle.
The excised mass was sent to pathology in 2 specimens labelled as “left scalp” and “left small soft tissue tumor occipital area,” along with left neck level II-V lymph nodes. Pathologic examination of the “left scalp” specimen reported an 8.3 × 3.0-cm tumor with multiple calcified nodules and soft pink cystic nodules. There were concerning features of highly aggressive pilomatrixoma including high mitotic counts, focal necrosis, and partial tissue islands extending into surrounding soft tissue and inducing desmoplastic reaction. Surgical margins were noted to be negative, with the closest being 2 mm from the deep margin. A second tumor with features of a pilomatrixoma was also noted. Perineural and lymphovasular invasion was not identified. The specimen labelled “occipital scalp” showed calcified subcutaneous nodule that was determined to be pilomatrixoma. All 34 resected neck lymph nodes were negative for malignancy. This case was then presented for a second opinion from an expert dermatopathologist for review. The diagnosis of the “left scalp” specimen was subsequently changed to pilomatrix carcinoma, as the dermatopathologist believed there was sufficient invasive features for the diagnosis of pilomatrix carcinoma.
The patient’s postoperative course was unremarkable other than loss of a small portion of the skin graft covering the transferred latissimus dorsi muscle, which required debridement and an additional spilt thickness skin graft. The remainder of the reconstruction healed without complication (Figure 2).
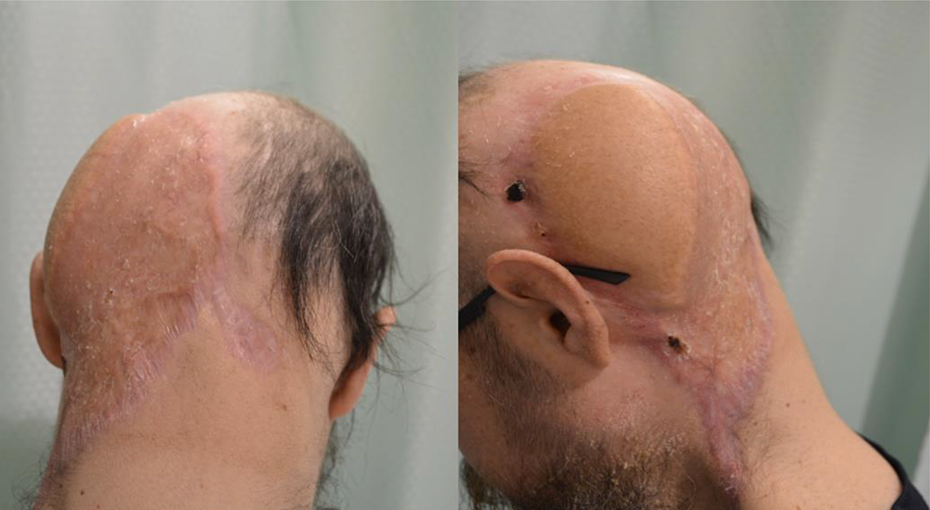
Postoperative free flap and skin graft healing.
Upon consultation with a multidisciplinary tumor board, adjuvant external beam radiation was recommended. After complete healing of the patient’s skin graft was achieved, the patient underwent a 5-week course of treatment, totaling 55 Gy, without complications.
Discussion
Although rare, the morbidity and mortality of pilomatrix carcinoma is not insignificant. Between 50% and 60% of cases recur after surgical excision, and a number of cases have reported patient mortality directly attributed to the disease. 9,11,14,15 Due to its rarity, pilomatrix carcinoma is not well understood. This first reported case of pilomatrix carcinoma in a patient with pre-existing DM may provide insight into risk and tumorigenesis, especially in patients with DM.
At the time of this report, there are multiple reported cases that support both the de novo and the malignant transformation of pilomatrixoma hypotheses on the origin of pilomatrix carcinoma. There have been a number of patients who presented with a rapidly growing pilomatrix carcinoma without previous pilomatrixoma, suggesting a de novo transformation. 2,4,6 In contrast, there are multiple reported cases with patients who developed pilomatrix carcinoma on a background of histopathologically confirmed pilomatrixoma. 9,16 -18 From these reported cases, it is likely that both pathways exist in the tumorigenesis of pilomatrix carcinoma. Similarly, in our case, it is unclear whether the pilomatrix carcinoma arose de novo or from malignant transformation of a pilomatrixoma. Although our patient had a previous diagnosis of pilomatrixoma, it was shown to be excised with clear margins prior to the presentation of the pilomatrix carcinoma. Interestingly, DM is one of a number of genetic conditions that have been shown to have an increased association with both malignancy and pilomatrixomas.
Although this is the first reported case of pilomatirx carcinoma in a patient with DM, an association between DM and pilomatrixoma is well established and was first reported in 1965 by Cantwell and Reed. 19 Since the first report, pilomatrixoma has become the most frequently described neoplasm in patients with DM and occurs with greater prevalence in patients with DM than in the general population. 12,20 In addition, there have been reports of multiple pilomatrixomas in several members of the same family who have DM. 20 -31 The brother and mother of our patient both had DM with multiple pilomatrixomas. The exact mechanism that underlies this association is not yet known, although one hypothesis is that mutations in the CATNNB1 gene that codes for beta-catenin is involved. Beta-catenin is a downstream effector in the Wnt-signalling pathway that is involved in cell differentiation, proliferation, and adhesion. 32,33 In fact, activating mutations in beta-catenin regulation have been observed in 75% of pilomatrixomas, suggesting an association of the two. 21 Although this mechanism is not proven, considering both DM and pilomatrixomas are uncommon conditions, it is unlikely that this association between the two is a chance occurrence.
In addition to pilomatrixomas, patients with DM are at a higher risk of developing malignancies. It is believed that this predisposition also stems from an upregulation of beta-catenin via the Wnt pathway, although the specific mechanism has not been elucidated. 12 Multiple cohort studies have found that patients with DM have as high as a 2-fold increase in developing certain malignancies when compared to the general population. 34 -36 Thymoma is the most commonly associated malignancies, although there have also been reports of colon, endometrium, ovary, and brain malignancy. 34 -36 Despite the variation in the specific cancers found, the reproducibility of this finding across 3 separate cohort studies suggests credibility in the observation of increased malignancy in DM.
Given the association of DM with pilomatrixoma and potential malignancy, the presentation of malignant pilomatrix carcinoma in a patient with DM is not surprising. However, this is the first documented case in the literature of pilomatrix carcinoma in a patient with a pre-existing genetic condition. This may be partially attributed to the overall rarity of pilomatrix carcinoma. Given the findings of this case, the authors suggest excision of pilomatrixomas and careful surveillance in the DM population. Further investigation is needed to more fully explore the relationship between DM and pilomatrix carcinoma.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Statement of Human and Animal Rights
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helskinki Declaration of 1975, as revised in 2008.
Statement of Informed Consent
Informed consent was obtained by the patient discussed in this manuscript.
