Abstract
A 36-year-old male who suffered severe frostbite injuries to both feet presented with an estimated total body surface area at around 4%. These injuries resulted from the patient travelling from his town by foot, with a temperature of −10°C during 4 days. On route, he received rewarming therapy followed by thrombolysis that was initiated as the duration of the warm ischemia period resided under 24 hours. Immediately after the procedure, the feet recovered clinically up to the distal toes. Saturation revealed normal values. Thrombolysis ceased after 9 hours and angiography showed adequate perfusion of the toes. Three hours later, pedal pulses at the toes were lost. Subsequently, the patient developed blisters and progressive necrosis of the toes to midfoot. Both feet were managed expectantly and were dressed, but the conditions of both feet worsened and the tissue turned into full-thickness necrosis. The decision was made to amputate a month after thrombolysis.
Keywords
Introduction
In the past few years, the rate of frostbites has been increasing due to several factors. Many of the victims are individuals who are homeless and alcohol and/or drug consumers and some of them are affected by mental illness. 1 Also, increasing outdoor activities and sports during the winter is a risk factor, especially for those not taking appropriate protection. 2 The most common sites that are affected are fingers, toes, hands, feet, and to a lesser extent nose and ears. 3
Several factors play a role in determining the severity of cold injuries. The most important ones include exposure to cold temperatures, typically starting from −2°C, wind chill factor, and duration of exposure to cold. 4 The lower the temperatures and more time exposed to cold weather will result in more severe injuries.
The mainstay of frostbite treatment is rapid rewarming of the injured site using water at around 40°C, then covered with a protective dressing for few weeks. In cases of severe injuries with presence of necrosis, surgery is typically delayed to allow the necrotic tissues to demarcate, which allows amputating only devitalized tissues. 5
The pathophysiologic pathways of frostbite injury include direct damage to the cell by cold and ice crystals and tissue ischemia due to the development of thrombi and embolic events. 5 Only the ischemia reperfusion pathway is prone to medical care, as the others present irreversible damages.
In the past few decades, many studies have evaluated the use of intra-arterial (IA) thrombolytic therapy by using tissue plasminogen activator (tPA) to restore vascular supply to the injured and ischemic body parts. Many results were published demonstrating the beneficial effects of thrombolytic therapy and its effectiveness in lowering the likelihood of requiring an amputation. 6 In a 2007 study by Bruen et al, 7 they have shown that the rate of amputations has gone down from 41% to 10%, when comparing patients who have not received thrombolytic therapy and patients who have received it, respectively.
Many therapeutic modalities have been studied such as heparin, 8 sympathetic blockade, 9 and even the administration of tPA intravenously, 10 but all of them failed to prove efficacious at a significant level of evidence in the treatment of frostbites.
We present an unusual and first case of tissue necrosis after angiographic evidence of restoration of vascular supply post IA tPA treatment.
Case Report
A 36-year-old male, who lived in the town of Kuujjuarapik, Quebec, was transported by plane, on March 15, 2017, to our tertiary care hospital in Montreal, which is a designated provincial center for severe cases of frostbites. The transport time took around 4 hours. He suffered frostbite injuries to both feet distal to midtarsal joints, with an estimated total body surface area around 4%. These injuries resulted from the patient travelling from his town to another by foot, with an outside temperature of mean −10°C. He was walking for 4 days covering around 60 km, where he was found in a ditch (Figure 1). He was taken to the closest hospital, and on physical examination, it was noted that both feet were hard to touch, pale and insensate. The levels of thrombi were at the distal two-thirds of the feet (Figure 2). Rewarming therapy started using water at around 40°C to 42°C, which was also continued on the plane that brought him to Montreal. The appearance of the feet changed to blue/grey after rewarming.

Patient on arrival to our institution.
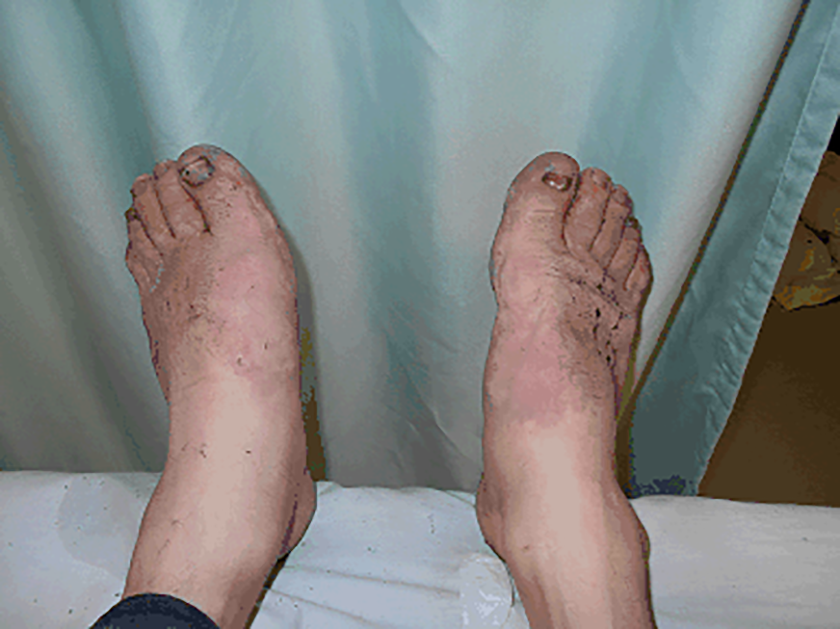
Feet prior to the commencement of rapid rewarming therapy.
On arrival, the decision was made to start thrombolytic therapy as, according to our algorithm, the warm ischemia period did not exceed 24 hours. The time between rewarming therapy and initiation of thrombolytic therapy was about 6 hours. Then, size 4F catheters were placed in the popliteal arteries bilaterally, where 1 mg/h of recombinant-tissue plasminogen activator (rtPA) was infused, and using 5F catheters, 30 mg/h of papaverine was infused. This makes it a total of 2 mg/h of rtPA and 60 mg/h of papaverine that were infused.
Immediately after initiation of thrombolysis, the feet recovered clinically up to the distal toes, they became clinically pink, with however presence of clear and hemorrhagic blisters. Saturation and pulses were taken on every toe and revealed normal values (saturation 98%).
The following day the thrombolysis catheter was bent and at risk of rupture, which required the removal of the catheter and cessation of thrombolytic therapy after about 9 hours (Figure 3). However, 12 hours after initiation of thrombolytic therapy (and 3 hours after its cessation), pedal pulses at the toes, which were present post thrombolysis, were lost. It should be noted that the angiography, at the time of cessation of thrombolysis, have demonstrated adequate perfusion of the toes and the patient did not receive any anticoagulation or antiplatelet therapy after catheter removal. Also, it was noted that during thrombolytic therapy, the patient was cooperative and his activity did not cause the removal of the catheter (Figure 4).
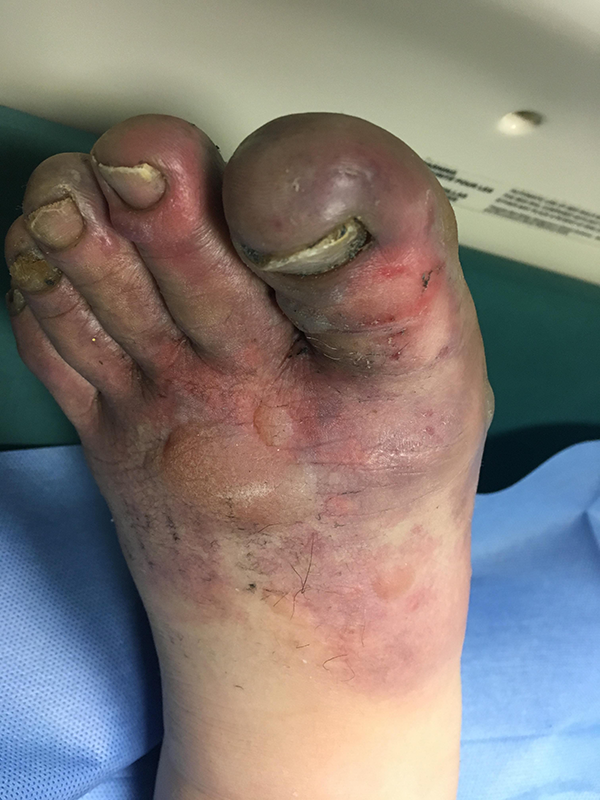
Nine hours after cessation of thrombolytic therapy.
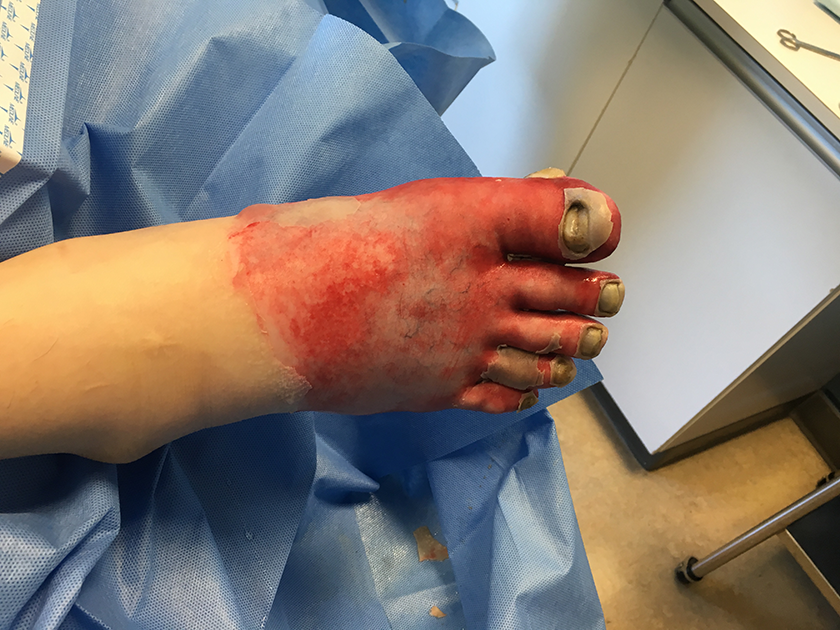
Deterioration of both feet.
The following days revealed a probably deeper frostbite that initially suspected with developing blistering and progressive necrosis of the toes to midfoot. An infection of his feet was also noted and the patient was started on intravenous antibiotics. Dressing was performed and an expectant approach was favoured. In addition, it was also noted that there was a progressive edema of the left lower limb, which required a Doppler investigation. The test showed a superficial thrombophlebitis, with no interference to the deep vasculature.
The conditions of both feet have worsened considerably and the color turned into black. The decision was made to amputate and the patient was transferred to the operating room on April 21, 2017. Debridement was commenced at the junction between healthy and necrotic tissues. On the right side, the amputation included the navicular bone and the 2 medial cuneiforms. The oscillating saw was used to resect the residuals at the distal cartilaginous surface of the tarsal bones. On the left side, the oscillating saw was used for the transmetatarsal amputation, at around two-thirds the distance distal to the metatarsals. The residual necrotic soft tissues were equally removed using a size 10 blade (Figures 5 & 6).
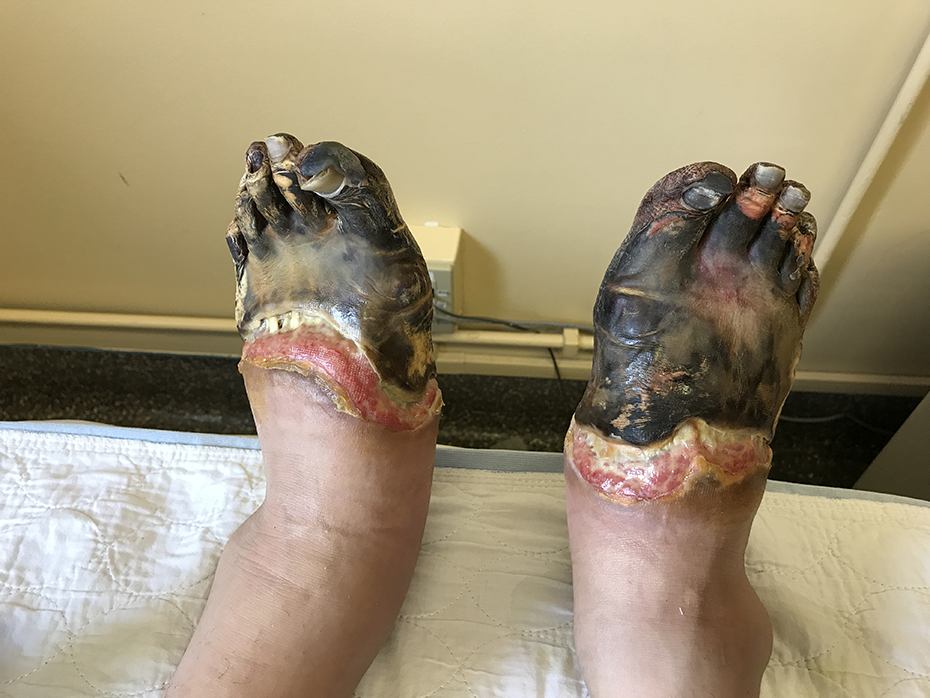
Full-thickness necrosis bilaterally.
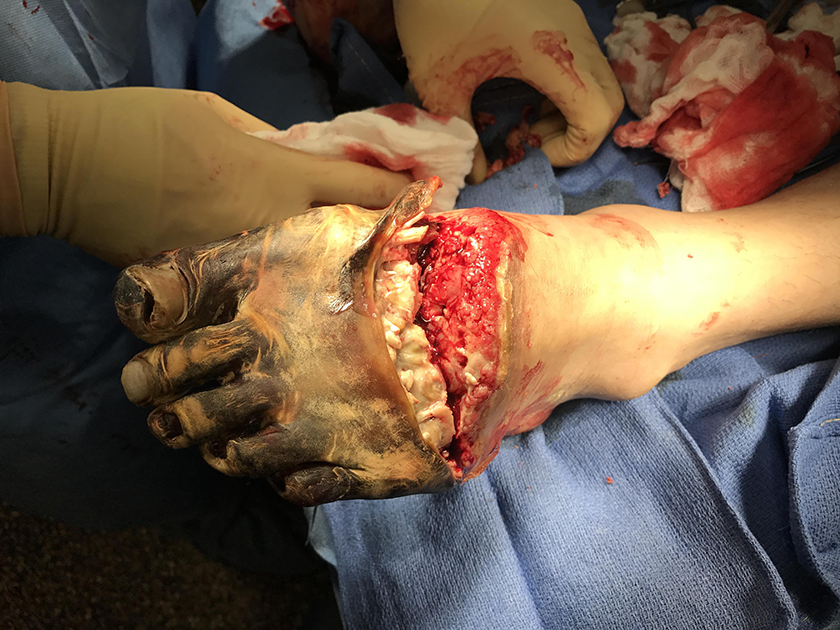
Bilateral amputations.
Discussion
Using IA tPA is demonstrated to have beneficial effects in the management of frostbites. In 1992, Skolnick was the first to report the use of IA tPA in 4 patients, where 1 of them required amputation. 11 More recent studies such as the study by Ibrahim et al in 2015, 12 implemented a protocol where severe cases of frostbites with angiographic evidence of vascular insufficiency and presented within 24 hours were given IA tPA (alteplase). They reported 3 cases, where posttherapeutic angiography showed considerable improvement, and noted that all patients returned to their previous functionality without any assistance. Another larger study in 2016 by Gonzaga et al 13 involved 62 patients. They used several thrombolytic agents, in addition to a vasodilator agent (papaverine) concomitantly. The results showed that 31.4% of the total number of digits affected were amputated.
Unfortunately, there are no definitive guidelines nor a clear set of indications for the use of thrombolytic therapy in severe cases of frostbites. Decisions using this type of therapy are subjective and depend on several factors, such as experience of the surgeon, availability of proper imaging modalities and thrombolytic agents at the institution, and so on.
In conclusion, the use of IA tPA has shown to be the most beneficial therapeutic modality for severe cases of frostbites, so far.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Statement of Human and Animal Rights
This case report was conducted in accordance with the Declaration of Helsinki, in regards to humans and animal research.
Statement of Informed Consent
Informed consent was obtained prior to performing the procedures, including permission for photographs included in this manuscript.
