Abstract
Introduction:
The Fricke flap was originally described in 1829 as a laterally based flap from the temporal region that could be used to reconstruct potentially total lower eyelid defects. There have been a few minor modifications of this flap to allow for adjustments of the donor site scar, but none that address the sequelae of brow elevation and allow for reconstruction of a composite defect of the lateral canthus, lateral upper, and lower eyelids. We report our modification of the Fricke flap that allows for total reconstruction of these structures.
Clinical Report:
A 61-year-old male presented with composite defect of the lateral eyelids and canthus following resection of a basal cell carcinoma by Mohs technique. A Fricke flap was designed and modified to included elements of the above brow and below brow skin as an additional pennant flap. A “Y” shaped periosteal flap and inferior fornix conjunctival flap were also used to reconstruct the posterior lamella. Our surgical technique and follow-up are demonstrated.
Discussion:
Lateral eyelid and canthal reconstruction can be difficult to reconstruct with a single rotational flap from local sources. We describe our technique of modifying the Fricke flap to include an additional pennant of below brow skin that can be used to reconstruct the lateral eyelids and canthus allowing for a crisp lateral eyelid crease and acceptable donor site and aesthetic appearance.
Conclusions:
This is the first description of a modification of the Fricke flap that allows for total lateral eyelid and canthus reconstruction.
Keywords
Introduction
Full or partial thickness lateral canthal defects combined with upper and lower lateral eyelid defects can be extremely challenging to reconstruct with a satisfactory result. Resuspension of the lateral canthal insertion, creation of a crisp lateral canthal crease, and preservation of the aesthetic subunits of the lateral orbit are technical goals of reconstruction of this location. 1 Unsatisfactory reconstruction of this area can cause effacement of the lateral eyelid crease, scarring, adhesions, and narrowing of the palpebral aperture. The Fricke flap was originally described in 1829 as a laterally based flap from the temporal region that could be used to reconstruct the skin of the lower eyelid. 2 Because of its potential size, the Fricke flap can be used to reconstruct long defects of the lower lid. 1,3,4 In this article, we describe a case in which the Fricke flap was modified to reconstruct the entire lateral lid crease including lateral upper and lower thirds of the eyelids, as well as the lateral periorbital skin. To our knowledge, this modification of the Fricke flap has not previously been described.
Patient Description and Surgical Technique
This is a 61-year-old salesman who presented to our clinic immediately following resection of a large basal cell carcinoma from the lateral canthus using Mohs technique (Figure 1A and B). The tumour involved the lateral thirds of the upper and lower eyelids and lateral canthus. This was a full-thickness wound that also involved the canthal tendon and the underlying conjunctiva. The defect measured roughly 2 × 3 cm.
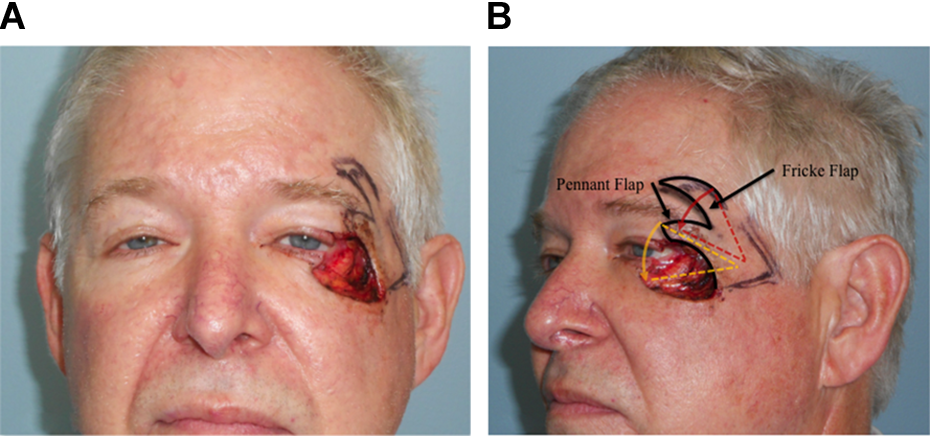
A and B, Preoperative frontal and oblique views of the eyelids defect demonstrating the Fricke flap and the modification of the flap with the below brow pennant flap. B, The flap outline and the arc of rotation for both components of the flap (red and yellow lines).
The patient was marked preoperatively for a standard temporally based Fricke flap with one exception of our modification that included a pennant flap of skin from the upper eyelid which was located just along the undersurface of the brow (Figure 1B). This pennant was attached to the Fricke flap at the inferior lateral brow region. The operation was done under conscious sedation with a mixture of 1% epinephrine: 0.5% Marcaine, both with epinephrine, being used as local. The Fricke flap was incised and raised in the subcutaneous plane over the full temporal skin region. The lower pennant flap was raised to incorporate the orbicularis oculi muscle to preserve blood supply and to add bulk to the flap. This pennant flap was raised attached to the lower edge of the Fricke flap.
With the extended Fricke flap elevated, the middle and posterior lamella reconstructions were done. A medially based “Y” shaped periosteal flap was elevated with extensions incorporating the temporalis fascia (Figure 2). This flap was then rotated medially and anchored to the free edges of the remaining canthal tendon with 5-0 absorbable monofilament mattress suture. Because the conjunctiva was also missing, a laterally based conjunctival rotational flap was performed by lateral undermining and an inferior conjunctival back-cut. Final inset of the flap was done with 5-0 plain gut suture to bring the conjunctiva together and also to anchor the conjunctiva to the Fricke flap at the lateral palpebral aperture. The temporal supra-brow donor site was then closed directly in layers and the upper edge of the Fricke flap rotated into the upper eyelid defect for closure in similar fashion. The lower edge of the Fricke flap, which was the pennant flap, was rotated and inset into the lower eyelid defect with interrupted 6-0 prolene suture (Figure 3).
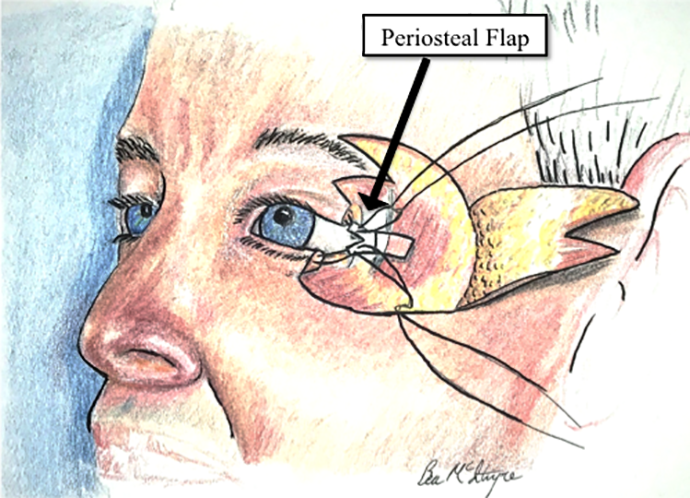
Demonstration of the periosteal flaps and inset into the lateral canthal tendon remnants.
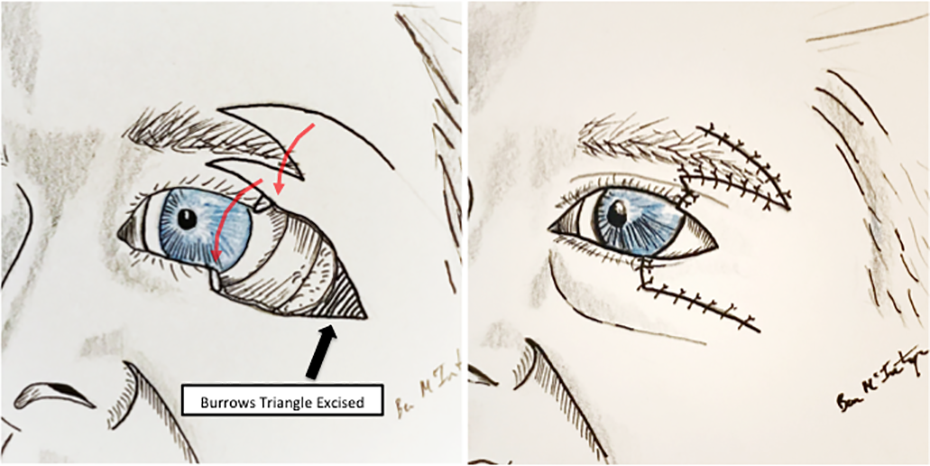
Demonstration of the modified Fricke flap markings, arc of rotation, and flap inset.
His sutures were removed at 7 days and time allowed for routine healing. At 3 months, he had a revision of the flap for pincushioning which was done by dermabrasion. His final result is shown at 6 months post-op (Figure 4A and B).
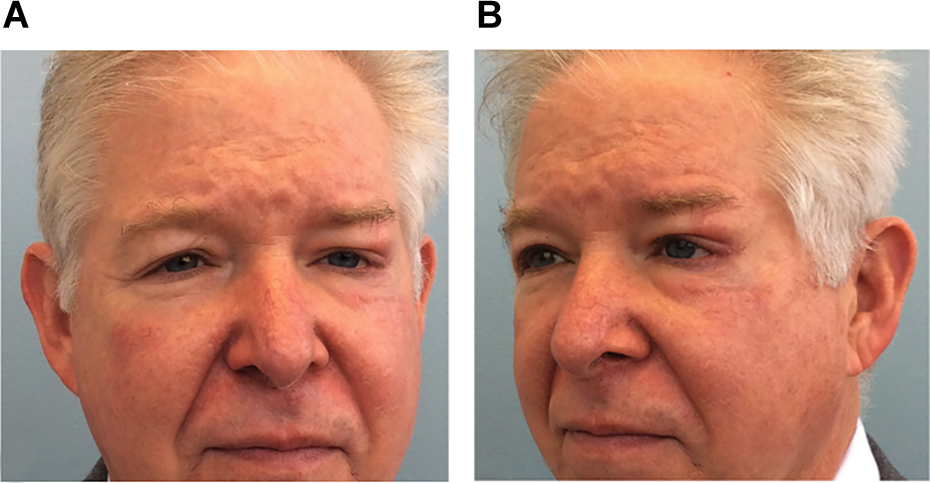
A and B, Postoperative frontal (A) and oblique (B) views at 6 months. Dermabrasion had been performed to improve the appearance of the scars.
Discussion
Mustarde, Tenzel, Tripier, and Fricke have all described flaps that can reconstruct 1 or 2 of the 3 mentioned areas of injury (lateral third upper eyelid, lateral third lower eyelid, lateral canthus) but not all 3. 5 -7 Both the Mustarde and Tenzel flaps rely on lateral periorbital skin as a source of donor tissue for eyelid reconstruction. When this skin has been resected, these flaps are no longer options for reconstruction. Additionally, it is difficult to bisect these flaps to recreate the lateral eyelid fissure without compromising the vascularity of these flaps. For similar reasons of blood supply, the Tripier flap cannot be used to reconstruct the lateral upper eyelid, lower eyelid, and canthus. For combination defects of this nature, cheek advancement flaps, combinations of flaps and skin grafts, and hard palate and cartilage grafts have all been described as options for reconstruction. 8 -13 We believe our modification of the Fricke flap, when possible, can offer a superior cosmetic result when compared with these other methods.
The Fricke flap has been modified previously by Barba-Gomez et al with an inferior extension of the flap into the central cheek. 4 Our modification of the Fricke flap differs in that this technique allows for recruitment of remaining upper eyelid skin for lower eyelid reconstruction and temporal skin for upper eyelid reconstruction and spares the central cheek as a donor site. There are many advantages of this operation. We were able to create a nice crisp lateral orbital fissure that had skin of similar complexion and thickness used to resurface this area. Brow elevation is minimized with this technique as the opposing forces of the upper flap inset and the above brow donor site offset the vectors of pull from each individual closure. The upper eyelid component of this flap can also be raised with orbicularis oculi muscle to maximize vascularity and to add to bulk in the lower eyelid if needed. The donor site and flap closure incisions were well concealed as they lined up nicely with the upper edge of the brow, the upper eyelid crease, and along the lash lines.
This patient had full-thickness defects that also required a “Y” shaped periosteal/temporalis fascia flap to recreate the canthal tendon. There was ample exposure to do this. This technique has been described elsewhere. 14,15 To recreate the posterior lamella, the conjunctiva was undermined and a lateral fornix advancement flap with backcutting of the inferior fornix was done to mobilize this tissue for a true, 3-layered reconstruction.
We acknowledge that this flap will likely require a second stage to fine tune the appearance of this flap with techniques, such as flap debulking, dermabrasion, and potentially z-plasty in the lateral canthus region. However, the overall appearance of this flap prior to second-stage revision is exceptional. The patient reported normal vision in his peripheral field of view. He also had a job in sales and noted that many of his customers did not notice the scarring in the lateral eyelid region.
In conclusion, the Fricke flap can be a versatile flap with a simple modification of an additional attached pennant flap that can allow for reconstruction of full-thickness defects of the lateral canthus including combination defects of the lateral upper and lower eyelids. This is the first such description of this modification of the Fricke flap. Our modification of this technique is relatively easy to perform and can create an overall exceptional result in an area that is otherwise difficult to reconstruct.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Statement of Human and Animal Rights
This article does not contain any experimental studies with human or animal subjects.
Statement of Informed Consent
Informed consent was obtained from the individual participant included in the study.
