Abstract
This is a case of plant thorn synovitis of the hand in an adult following a plum tree thorn injury, the first reported case in the hands in the past decade. The patient initially presented with persistent joint discomfort following removal of a retained plum thorn fragment from the skin overlyin the proximal interphalangeal joint of the left middle finger. Initial radiography and sonography imaging following the removal revealed no foreign bodies. However, the patient’s symptoms were worsening and refractory to anti-inflammatory and antibiotic treatment. An exploratory surgery was carried out, which revealed multiple plant thorn fragments within the synovium, each measuring approximately 1 mm in size. A synovectomy was performed and the patient recovered with full function. Our case of plant thorn synovitis is discussed along with a review of the current literature on plant thorn synovitis in the hands.
Introduction
Plant thorn synovitis, also known as plant thorn arthritis, is a rare and commonly overlooked cause of arthritic disease. This disease is attributed to a granulomatous inflammatory response to retained plant thorn fragments following a puncturing plant thorn injury. 1,2 However, the mechanism by which retained plant thorn material triggers this inflammatory response remains unclear. When the inflammatory response occurs adjacent to or within a joint, the patient develops signs and symptoms consistent with a typical inflammatory arthritis including erythema, joint swelling, warmth, and limited range of motion. 3-5 As the granulomatous response is localized to the injured joint, plant thorn synovitis typically presents as a monoarthritic disease. 4 To date, thorns from multiple plant species have been implicated in cases of synovitis and it is unclear if there are different risks associated with different plant species. 2
Due to its rarity, the knowledge surrounding plant thorn synovitis is limited to what is described in reported cases. Presentation is typically delayed, with one case reporting a median of 68.5 days between the time of the injury and the onset of joint pain. 2 There is no ideal diagnostic tool, and although ultrasound has been reported to be effective in visualizing fragments in some reported cases, most have been definitively diagnosed with plant thorn synovitis only at the time of surgical exploration. 5 Furthermore, treatment to date has not shown any promise with conservative or medical management. At present, surgical intervention is the only known definitive treatment, involving the open excision of plant thorn fragments and synovectomy. 3,6
Although there are many aspects of plant thorn synovitis that are not well understood, the main challenge is obtaining an accurate and timely diagnosis. Laboratory results only act to confirm an inflammatory process, often revealing an elevated erythrocyte sedimentation rate, white blood cells, and C-reactive protein. 6 Due to the often small size of retained plant thorn fragments and their radiolucent nature, diagnostic imaging such as radiography and ultrasonography have been used with varying degrees of success. 5,7 As a result, plant thorns often escape detection as a foreign body. 1,3,8,9 Here, we present a case of plant thorn synovitis of the hand in addition to a review of the current literature surrounding plant thorn synovitis in the hands.
Case
A 48-year-old woman, with a history of methotrexate-controlled psoriasis, was referred to plastic surgery clinic for concerns of retained foreign body near the proximal interphalangeal (PIP) joint of the left long finger. The patient had sustained a plum tree thorn injury to the ulnar aspect of her dorsal left long finger near the PIP joint 2.5 weeks prior. Following the injury, the patient had presented to a community hospital emergency department, where large thorn splinters were removed from the skin. The patient developed cellulitis following the removal and had been taking cephalexin orally for 2 weeks at the time of her consultation. Despite the antibiotic treatment, the patient reported persistent pain and decreased flexion in the left long finger PIP joint. Physical examination revealed mild erythema at the site of the initial thorn injury, with no pain elicited on axial joint loading and palpation of the volar aspect of the long finger. Collateral ligaments were stable with intact flexor and extensor functions. Consultation of radiographic and sonographic images of the hand post thorn extraction revealed no foreign bodies. The patient was given instructions to increase range of motion of her left hand to decrease PIP joint stiffness, and her course of cephalexin was extended. A tentative diagnosis of post-traumatic inflammation was made.
Five weeks postinjury, the patient was seen with persistent inflammation and pain of her left long finger PIP joint (Figure 1). Her symptoms were not improved by antibiotic use and the patient described joint stiffness and pain in the morning. At this point, a high-resolution ultrasound was ordered requesting a musculoskeletal radiology team, which revealed 5 small (1-2 mm) foreign bodies in the subcutaneous tissue. Due to the unfamiliarity with the diagnosis of plant thorn arthritis and the relatively superficial location of the foreign material, it was anticipated that the tiny foreign bodies would likely resolve spontaneously. The patient was asked to increase her dose of methotrexate, originally given to manage psoriasis, as a trial to decrease her inflammation.
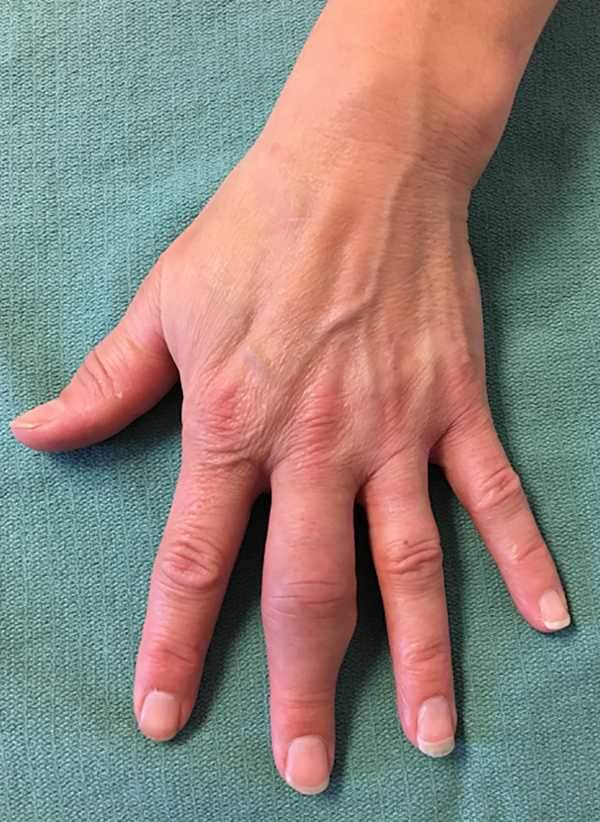
Five weeks postinjury from plant thorn puncture to the left hand.
Nine weeks postinjury, the patient’s symptoms had worsened, and the persistent inflammation and discomfort of the left long finger PIP joint now concurrently presented with increased joint stiffness on examination (Figure 2). Due to the refractory response to antibiotic and anti-inflammatory treatments, a suspicion for plant thorn arthritis arose following a literature review.
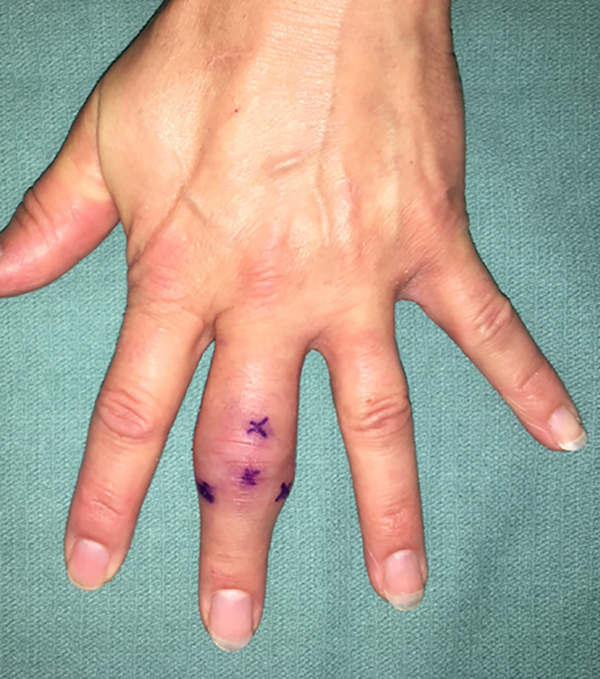
Nine weeks postinjury from plant thorn puncture injury.
Due to worsening symptoms, a decision to proceed with surgical exploration with excision of foreign body and possible synovectomy was made. For the purpose of surgical planning, a repeat ultrasound was taken and skin markings were made overlying the visualized foreign bodies by radiology (Figure 2).
Surgical Technique
Under general anaesthesia, with tourniquet control, a large Chevron incision was used to expose the full area over the dorsal aspect of the left middle finger PIP joint. Under loupe magnification, one foreign body 1 mm in size was extracted from the level of the extensor mechanism. The extensor mechanism was then longitudinally spilt to reveal synovium, which appeared to be extremely swollen and inflamed. A surgical microscope was then used to perform a meticulous removal of inflamed synovium and over 10 foreign bodies from within the synovium and synovial membrane (Figure 3). While under the microscope, an area of 2 mm × 2 mm of the PIP joint cartilaginous articular erosion was noted. After arthrotomy, the joint was thoroughly irrigated with an angiocatheter. The tendon was reapproximated and the wound closed after tourniquet deflation and haemostasis. A volar splint was placed with PIP held in extension.
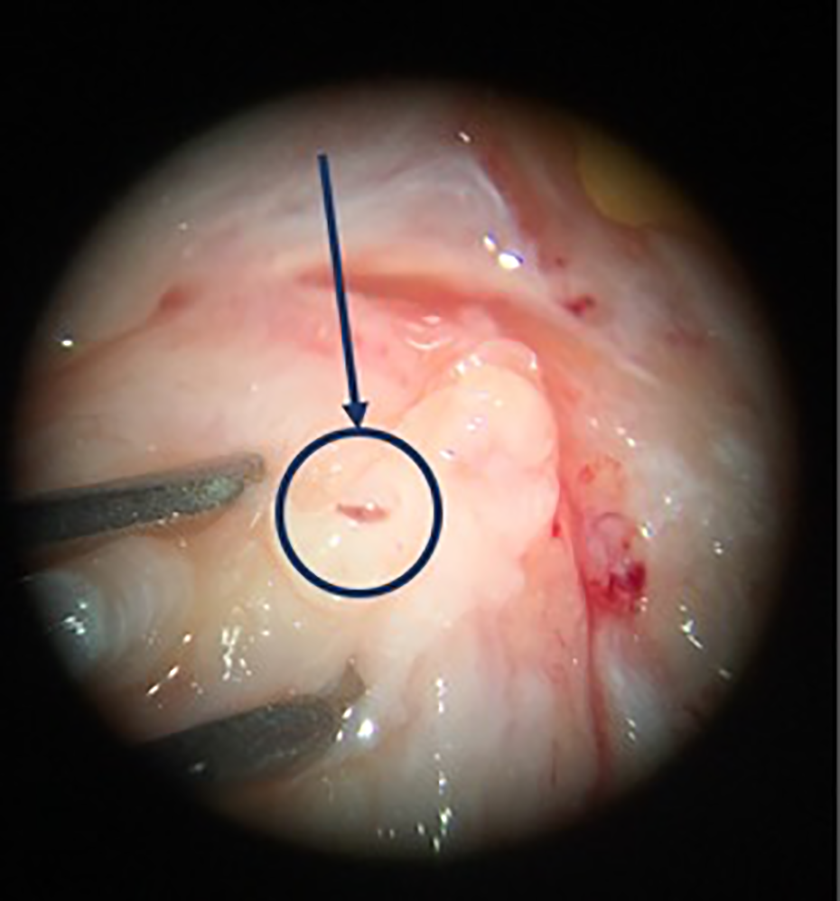
Intraoperative microscope visualization of plant thorn fragment within synovium.
At the 10-day postoperative follow-up, there was significant improvement in pain, erythema, and swelling of the joint (Figure 4). No complications were noted. Pathologic examination of the synovium revealed subacute inflammation with abscess formation and proliferative changes with focal foreign body giant cell reaction. The patient began hand therapy to range the affected finger at 4 weeks postoperatively. The last follow-up occurred 4 months postoperatively. An X-ray of the patient’s left hand taken on this visit revealed decreased joint space in the long PIP joint, though the patient was clinically asymptomatic with near full extension and flexion of the affected PIP joint (Figures 5 and 6).
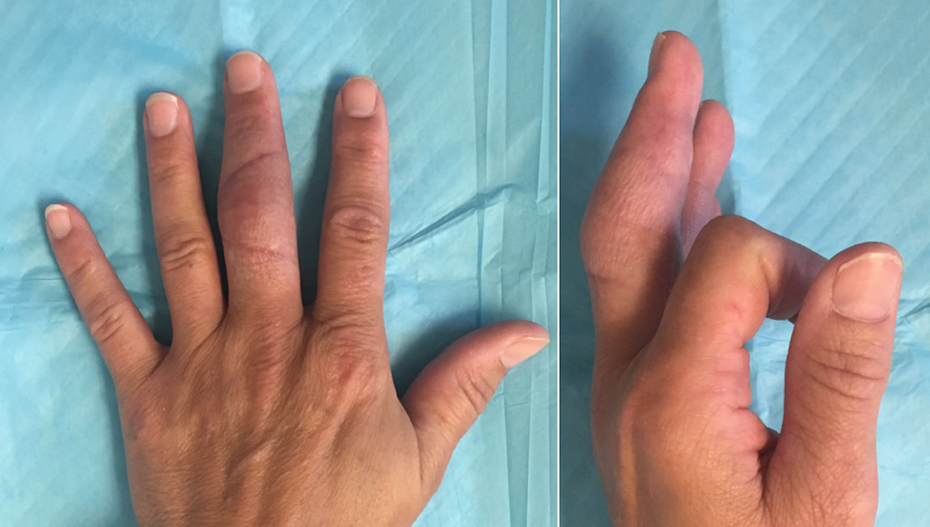
Synovectomy on postoperative day 10.
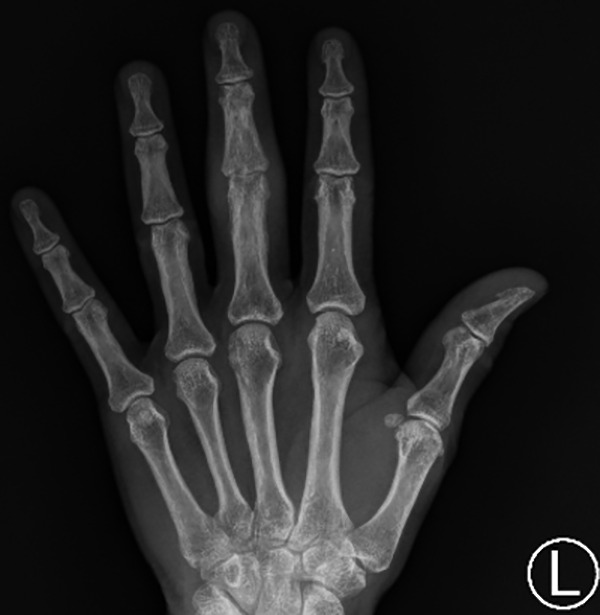
X-ray of the left hand on postoperative day 10 of synovectomy revealing decreased joint space.
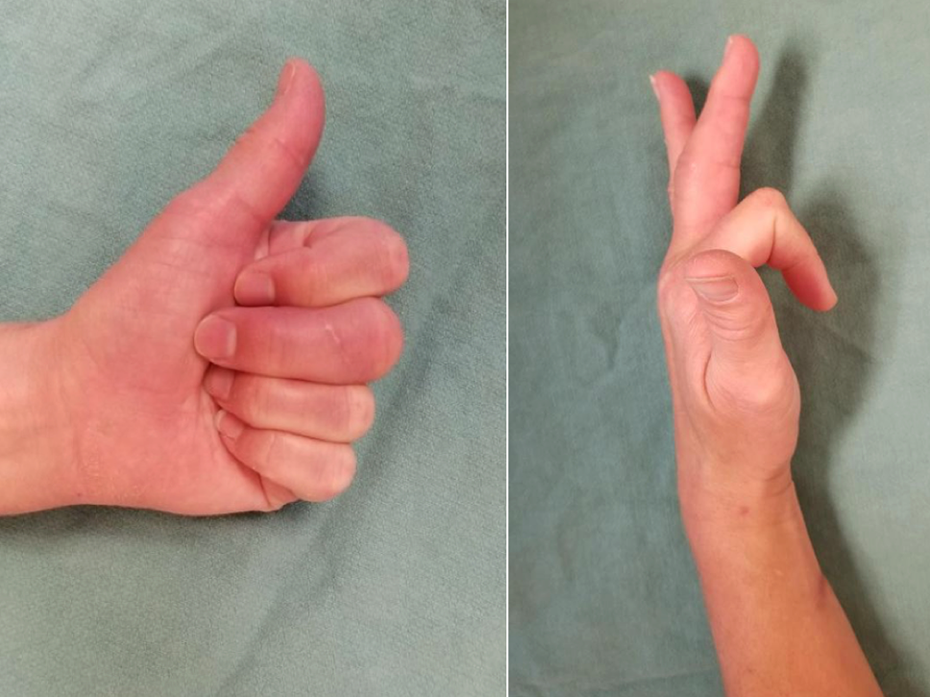
Range of motion at postoperative month 4.
Literature Review
A literature review was conducted by searching key terms: plant, thorn, arthritis, synovitis, hand, and foreign body in MEDLINE, EMBASE, and PubMED databases from 1975 to 2017.
Search Results
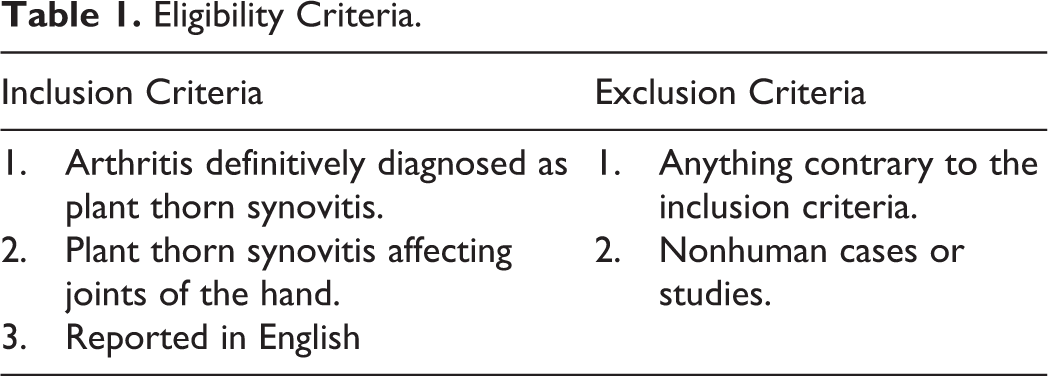
The initial search identified 153 titles. Initial screening of titles and abstracts were independently carried out by 2 authors. Papers with potential for inclusion, based on our predetermined criteria, underwent full-text review. These papers were included or excluded based on our eligibility criteria (Table 1). After full-text review, 6 reports were related to structures of the hand (Figure 7). All 6 relevant studies were case reports.
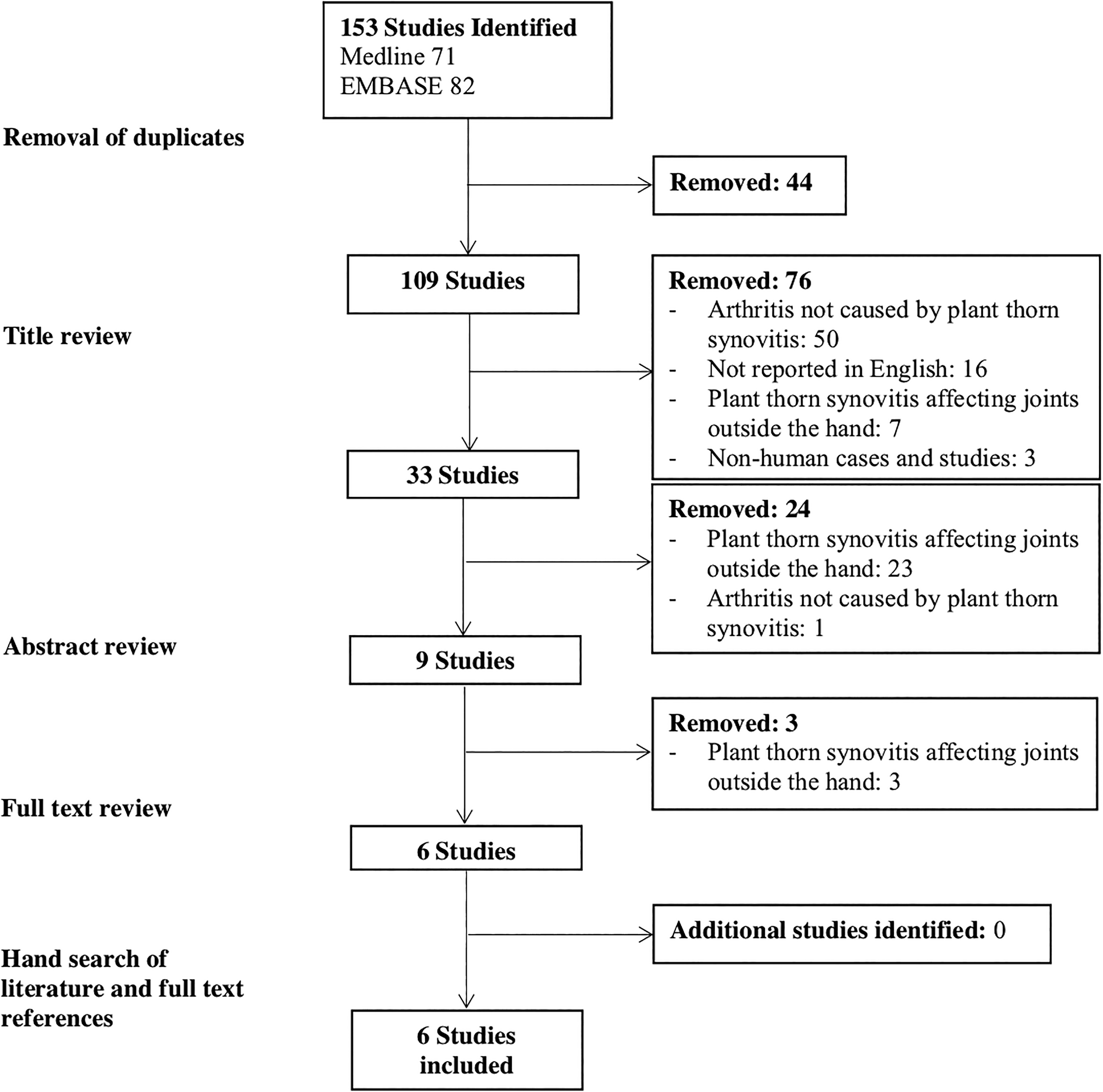
Flow diagram of study selection.
Eligibility Criteria.
Patient Demographic
Table 1 outlines the demographics from the included case reports. Ages of patients with published reports of plant thorn synovitis involving the hands ranged from 7 to 58 years, with a median age of 24.5 years. Both males and females were reported in the included cases. With the exception of 2, all patients were reported to have no significant past medical history. The 2 patients with a reported past medical history includes a 58-year-old female with insulin-dependent type 2 diabetes mellitus and a 10-year-old male with a history of psoriasis. 2,5
Presentation
Presenting symptoms described were largely consistent between the reported cases. These included swelling, erythema, decreased range of motion, and pain with range of motion at the affected joint (Table 2). Additional symptoms included one patient who developed additional nail and skin changes similar to psoriatic arthritis and another patient who developed fever. The time of initial symptom presentation ranged from 24 hours to 4 months after the injury (Table 3).
Demographics and Clinical Characteristics of Reported Cases of Plant Thorn Synovitis.
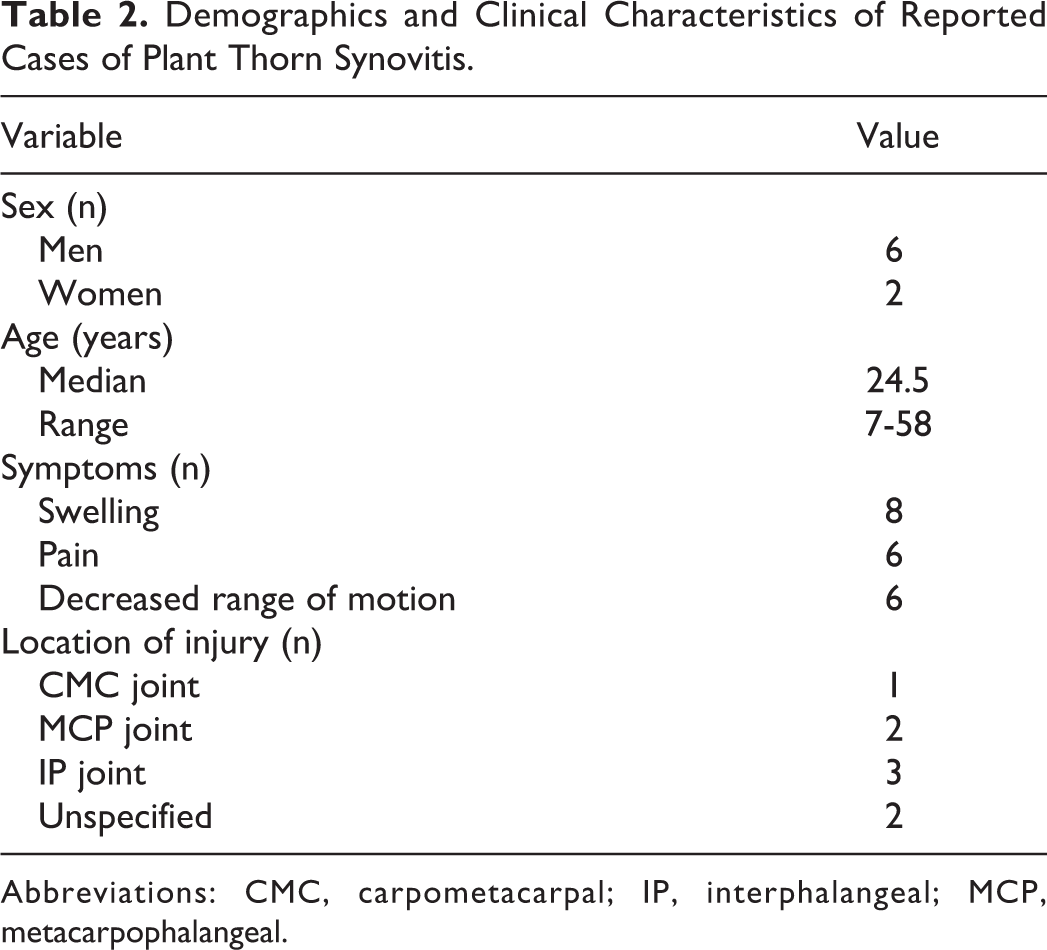
Abbreviations: CMC, carpometacarpal; IP, interphalangeal; MCP, metacarpophalangeal.
Summary of Characteristics, Imaging, Diagnosis, Treatment, and Outcome of Reported Cases of Plant Thorn Synovitis.
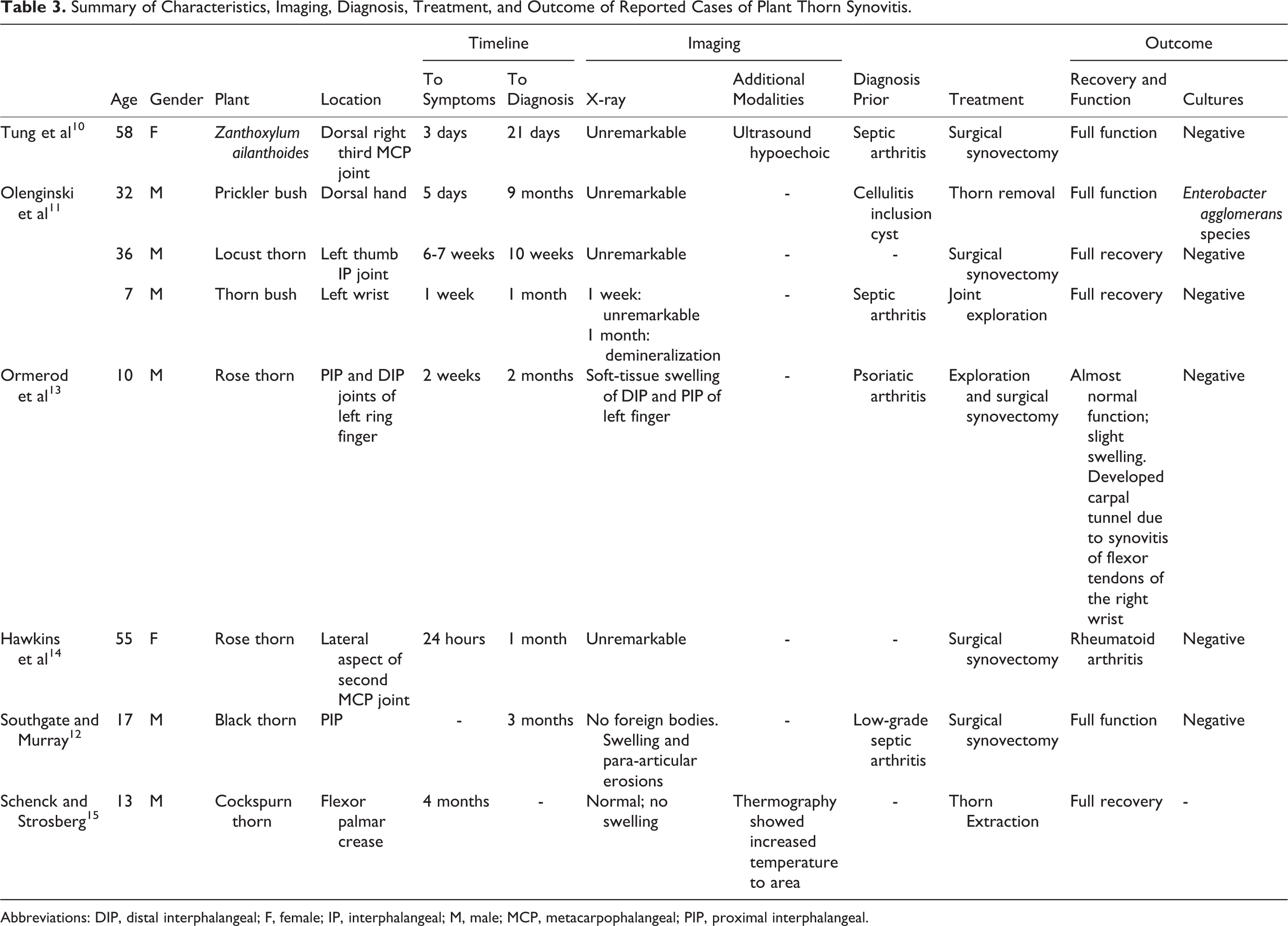
Abbreviations: DIP, distal interphalangeal; F, female; IP, interphalangeal; M, male; MCP, metacarpophalangeal; PIP, proximal interphalangeal.
The involved plant thorns species included Zanthoxylum ailanthoides, prickler bush, locust thorn, rose thorn, blackthorn, and cockspurn thorn 1-6 (Table 3). No discernable pattern of injury in the hand was noted, with equal distribution of interphalangeal joints and wrist joint injuries (Table 2).
Diagnosis
In all included cases, the diagnosis of plant thorn synovitis followed symptoms refractory to medical management. Infectious causes such as septic arthritis and cellulitis were the most common initial diagnoses. 10-12 In the diagnosis of a plant thorn as a foreign body, X-ray imaging was found to be ineffective in visualizing thorn fragments, while some cases reported visualization of fragments with ultrasound imaging (Table 3). 10-15
Treatment
Each reviewed case report of plant thorn synovitis ultimately underwent treatment with surgical exploration, removal of foreign material, and synovectomy if the synovium was shown to be compromised. With the exception of one patient who developed rheumatoid arthritis, all included cases reported a full recovery in the affected joint (Table 3). 10-15 Pathology investigation revealed synovium that was described as thickened, granulated, or lobulated from chronic irritation due to the foreign body. 11,12,14 All synovium was shown to be sterile with the exception of the case reported by Olenginski et al, which grew Enterobacter agglomerans. 11
Discussion
As reflected by the limited literature, plant thorns are a rare cause of arthropathy in the hands. The diagnosis is challenging and is often made on the basis of exclusion. 16 As plant thorn synovitis is an inflammatory response to retained fragments of plant thorns, it commonly progresses to arthritis due to inflammatory damage of periarticular structures. 16 Undiagnosed, it can evolve into an undifferentiated chronic arthritis. 6 However, this form of arthritis is unique in its potential for full recovery following a synovectomy, which is understood to be the only definitive treatment. 10,11,16 Our experience with this reported case reflects the diagnostic challenges and emphasizes the importance of a surgical approach in the diagnosis and treatment of this rare form of arthritis.
A review of the current literature resoundingly supports the challenge of diagnosing plant thorn synovitis. Five additional case reports and 1 case series were found describing plant thorn synovitis in the hands. 10-15 Similar to this presented case, most reported cases consistently stated symptoms of joint inflammation—erythema, swelling, pain, and decreased range of motion in the affected joint (Table 1). However, this presentation is non-specific and mimics many common causes of arthritic diseases. This is reflected by the multiple cases where patients were initially misdiagnosed with conditions like septic arthritis. 10 This may especially be the case if the patient does not recall the initial thorn injury. In addition, the retained foreign bodies are often very small, measuring within millimetres, and have been reported to be missed on imaging. 17 Radiographic imaging presents limitations as plant thorns are radiolucent organic matter, making them essentially impossible to visualize. 7 A case report and literature review by Tung et al investigated the use of high-resolution ultrasonography for diagnosis, reporting the smallest fragment visualized to be 2.7 mm. 10 As a comparison, a number of fragments extracted from our patient measured approximately 1 mm. Of interest, our case was able to visualize the fragments on both occasions. The success in visualization may be attributed to a number of factors, such as prior to imaging the suspicion of a potential small foreign body was known and communicated to the radiologist, the radiologist and sonographer were specialized in the musculoskeletal system, and the ultrasound used was a high-definition ultrasound. Even with these advantages, surgical exploration revealed 5 additional fragments not visualized on imaging. As it stands with current imaging technology, there remains no consistently reliable imaging technique to include or exclude the diagnosis of plant thorn synovitis.
This challenge in diagnosis characteristically results in a lag of weeks to months before the diagnosis of plant thorn arthritis is made. 16 Although initial symptoms have been reported to be indolent and transient, the inflammatory process can cause significant sequelae. 6 Most commonly, the persistent inflammatory response damages the neighbouring articular structures, leading to arthritis. 6 In the case presented, there was intraoperative evidence of articular erosion accompanied by radiologic evidence of decreased joint space, only 3 months from the initial trauma. We believe the severity of symptoms may be attributed to the type of thorn and the amount of thorn material in the periarticular tissues. Presently, no successful medical management has emerged and the only effective treatment to date has been surgical excision of retained material and synovitis. Because of this, patients with undiagnosed plant thorn synovitis can progress to develop chronic arthritis. 5,16 The annual incidence of undifferentiated arthritis has been shown to range from 41 to 149 per 100 000 adults, comprising approximately 30% of all inflammatory arthritis. 18 As high as 50% of these chronic undifferentiated arthropathies do not achieve resolution in symptoms or diagnosis. 19 With these numbers in mind, it is important to consider that a subset of undifferentiated chronic arthropathies may be attributable to plant thorn arthritis.
Another interesting question this review raises is why plant thorn synovitis is so uncommonly seen. Based on past reported cases, any individuals with retained plant thorn fragments within the synovial tissue seem to be susceptible to developing plant thorn synovitis. No previously published studies have alluded to associated risk factors, whether that be patient characteristics, past medical history, or plant species. Interestingly, including our patient, 2 (25%) of 8 reported cases of plant thorn arthritis in the hands involved a patient with a history of psoriasis. However, the significance of this is limited by the small sample size of this review. As such, future studies are necessary to assess risk factors for individuals who go on to develop plant thorn synovitis.
Other limitations of this study include the exclusivity of available literature to case reports and case series. In addition, there is little current literature available, with the most recently reported case of plant thorn synovitis in the hands being from 2007.
In conclusion, due to its rare occurrence, in combination with diagnostic challenges, plant thorn synovitis is often excluded in the differential diagnosis of arthritic disease. However, with the potential of plant thorn synovitis to progress into a chronic arthritis, it is important to be aware of and maintain plant thorns as a differential for both acute and chronic undifferentiated inflammatory monoarthropathies. With the diagnosis commonly confirmed through surgical exploration, and definitive treatment being synovectomy, plant thorn synovitis is a unique arthritis as it is managed exclusively through surgical intervention. Therefore, it is important for surgeons especially to be aware of the condition and have a high index of suspicion for those with refractory arthopathy, especially following a plant injury.
Footnotes
Authors’ Note
Views expressed are the authors’ own and do not reflect the official position of the institution.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Statement of Human and Animal Rights
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2008 (5). Informed consent was obtained from all patients for being included in the study.
Statement of Informed Consent
Informed consent was obtained by the patient outlined in this manuscript. Additional informed consent was obtained from all patients for which identifying information is included in this article.
