Abstract
Melanoma is an aggressive disease that accounts for approximately 75% of skin cancer-related deaths. In the past, treatment options for patients with advanced stage melanoma have been limited with poor response rate and failure to improve overall survival (OS). Immunotherapy is a promising treatment that has been shown to improve OS and in cases produce durable remissions—a novel concept in the treatment of advanced melanoma. We report a case of advanced stage metastatic malignant melanoma of the scalp with a durable (31 months) response to ipilimumab immunotherapy. This is the first case study reporting long-term, progression-free response to ipilimumab in metastatic melanoma without side effects of therapy. This case adds to the evidence supporting early referral and initiation of ipilimumab in patients who can tolerate it, with the goal of producing a sustained treatment-free response and preserved quality of life.
Introduction
Melanoma is an aggressive disease that accounts for approximately 75% of skin cancer-related deaths. 1 The World Health Organization reports that the incidence of metastatic melanoma has increased over the past 3 decades—estimating 66 000 deaths worldwide every year are due to skin cancer, with approximately 80% due to melanoma. Most cases of malignant melanoma are diagnosed at an early stage when surgical excision can be curative. However, some patients have metastatic disease at presentation or develop metastases after their initial definitive treatment.
In the past, treatment options for patients with advanced stage melanoma have been limited with poor response rate and failure to improve overall survival (OS). Prior to 2010, median survival of patients with metastatic melanoma was approximately 7 months, and only 6% of patients survived to 5 years. 2 Chemotherapy with dacarbazine was the standard of care, although it had not been shown to improve patient survival. 2
Introduction and approval of immunotherapeutic and targeted agents between 2011 and 2013 has significantly changed the approach to treatment for those patients with advanced staged melanoma. 3 Both immunotherapy with ipilimumab (a monoclonal antibody targeting cytotoxic T-lymphocyte-associated protein 4 [CTLA-4]) and BRAF-targeted therapy with dabrafenib or vemurafenib have been shown to be effective. About 50% of melanomas will have a mutation in the BRAF gene, which activates the mitogen-activated protein kinase (MAPK) pathway. 1 These agents act by direct inhibition of the MAPK pathway. They have demonstrated antitumor activity in phase III trials in patients with advanced disease whose tumors have characteristic mutations in BRAF. 4 However, virtually every patient treated with an inhibitor of BRAF eventually has disease progression. 4
Immunotherapy is a promising treatment that has been shown to improve OS and in cases produce durable remissions—a novel concept in the treatment of advanced melanoma. 3 Ipilimumab is a monoclonal (anti-CTLA-4) antibody that acts by disinhibiting T-lymphocyte action, thereby allowing destruction of malignant cancer cells. 5 Ipilimumab has been shown in randomized controlled trials to improve OS in advanced melanoma with a median OS of 11.4 months. 3 However, only ∼11% of patients treated will respond (partially or completely) to therapy. 3,6,7 In addition, adverse effects are common and significantly limit its use. 3 Typically, response to ipilimumab develops slowly and there may be transient progression of disease before a response (disease stabilization or tumor regression) is observed, although durable remissions may result with approximately 22% surviving at 3 years. 8 Here, we report a case of advanced stage metastatic malignant melanoma of the scalp with a durable response to ipilimumab immunotherapy. To the best of our knowledge, there are no other case reports documenting response to ipilimumab exceeding that of 2 years, without adverse effect to treatment.
Presentation of Case
A 60-year-old woman presented to her family physician in the summer with a dark pigmented lesion on the crown of her scalp. The lesion had been present for at least 10 years, but recently her hairdresser noted that it had been changing and bled with minimal trauma. Over the course of a couple of months, the lesion grew vertically to become a palpable nodule. An excisional biopsy of the lesion was performed by general surgery on an urgent basis. The lesion was exophytic with mottled black coloring measuring 2.2 × 1.7 cm. Pathology showed an ulcerated malignant melanoma with vertical growth phase, characterized as lentigo maligna type. The tumor extended into the superficial subcutaneous tissue. Breslow depth was 10 mm, mitotic index was more than 10 mm2, and lymphovascular invasion and perineural invasion were present. Peripheral and deep resection margins were positive with multiple microsatellite nodules.
Past medical history was significant for type II diabetes mellitus, hypertension, fatty liver disease, hyperlipidemia, and carpal tunnel decompression. There was no personal history of previous skin cancer and no family history of melanoma known. She is a farmer’s wife with blue eyes and reported many years of sun exposure and sunburns.
The patient was referred to plastic surgery for a wide local excision. Within a couple of weeks, her disease progressed locally with black, pigmented lesions involving the majority of the scalp in a spotted pattern. The total area measured more than 25 × 20 cm extending from the forehead to the occiput and bilateral parietal regions (Figure 1). Intraoperatively, it was clear the pigmentation had invaded deep to the prior excision site, actually involving the periosteum. The bone was exposed and a small periosteal flap was used to cover the exposed bone. Split thickness skin graft was harvested from the posterior and lateral thigh and meshed to cover the defect. Pathology from this procedure disclosed microscopic satellite nodules of malignant melanoma. Tumor thickness was 3.5 mm, with tumor invading the subcutaneous tissue and ulceration present. Deep resection margin was positive again for invasive malignant melanoma. A biopsy was also performed of a palpable left posterior triangle lymph node, which was positive for metastatic malignant melanoma with extranodal extension. Computed tomography (CT) showed multiple lymph nodes in the posterior cervical triangle bilaterally and left occipital region, but no distant metastases. TNM staging at this point was pT3a N1b M0.
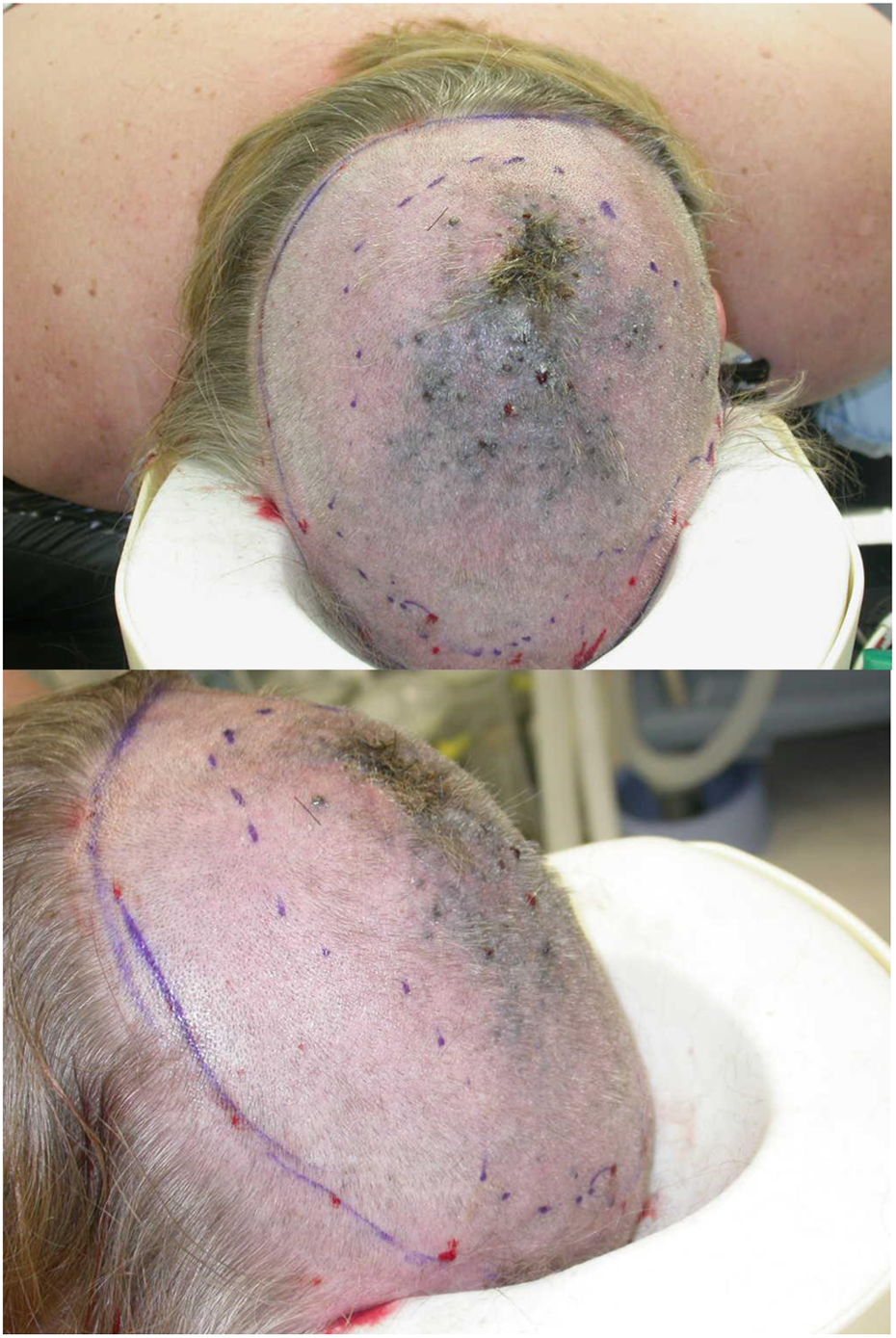
Intraoperative, prior to wide local excision and skin graft reconstruction.
This patient’s melanoma had a mutation in BRAF (V600E), and due to its aggressive nature, medical oncology recommended targeted therapy (dabrafenib) as first-line systemic treatment. On physical examination, at this time there were new, pigmented lesions that had developed involving the edge and center of the scalp graft (Figure 2). There was also palpable cervical adenopathy at this time. She tolerated dabrafenib therapy well, but unfortunately there was progression of disease after 3 months of treatment. Ipilimumab, a nontargeted immune checkpoint inhibitor, was initiated at this time as per the Regina Qu’Appelle Health Region’s protocol with 4 cycles of 3 mg/kg intravenously every 3 to 4 weeks. The patient responded remarkably well with complete resolution of cervical adenopathy and flattening/thinning of the pigmented lesions on the graft. No side effects of therapy were observed. Initial CT imaging showed no signs of distant metastasis, and clinically, the patient was asymptomatic. At 28 month follow-up from completion of immunotherapy, the patient was feeling generally well, with no indication of disease progression or adverse effects. Computed tomography scan of the brain, chest, abdomen, and pelvis at this time showed no obvious metastasis; however, the brain CT described a 0.3-cm focus of enhancement in the left parietal region, also seen on previous CT scan. It was apparently much smaller in comparison and was speculated as a regressing metastatic focus. At most recent follow-up at 31 months, the patient had maintained response to treatment and pigmented lesions had continued to regress.
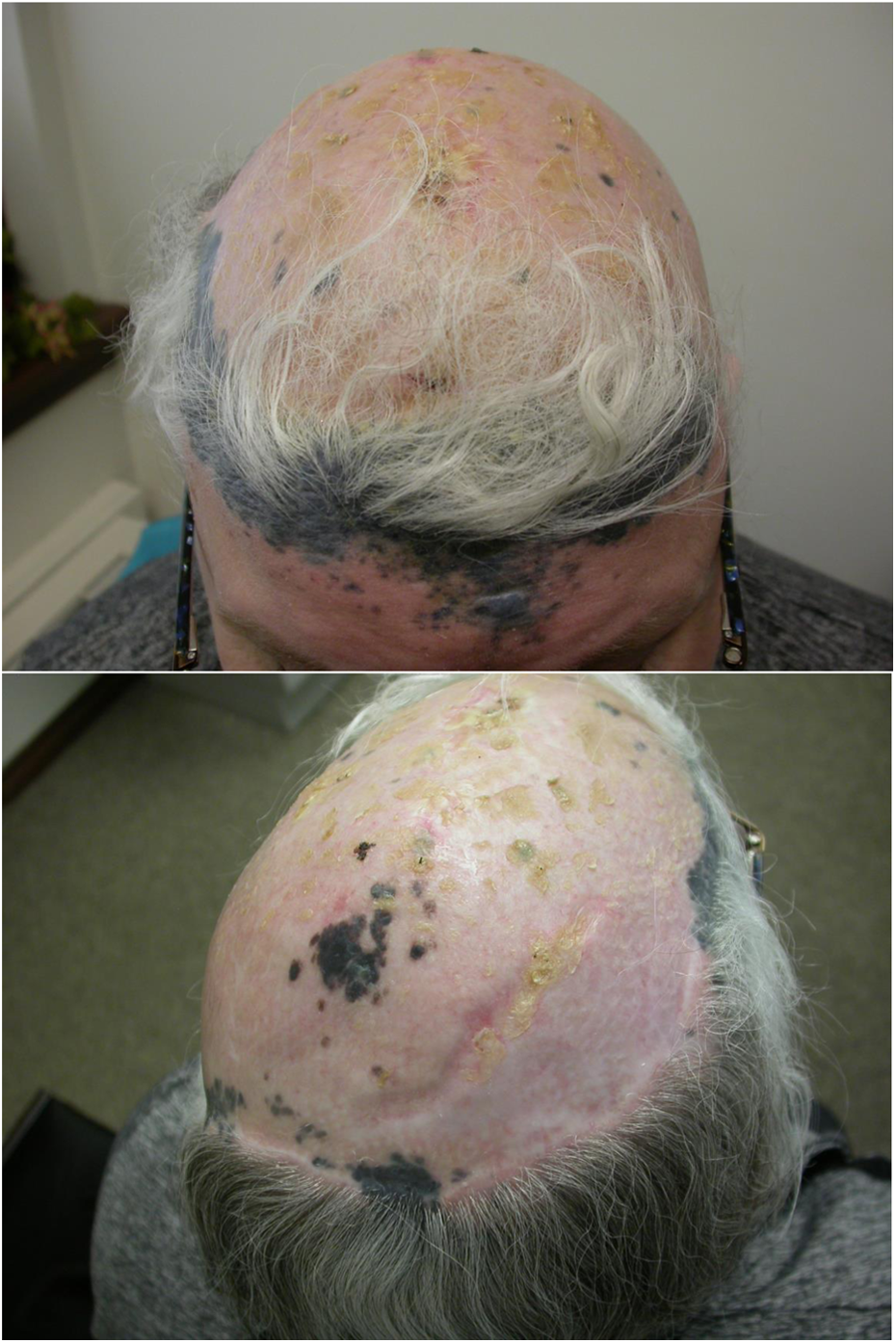
Follow-up at 8 weeks postoperatively.
Discussion
We report a case of a 60-year-old female presenting with advanced stage metastatic malignant melanoma of the scalp. Her disease was locally aggressive with rapid development of in-transit metastasis and lymph node invasion while undergoing therapy. This patient’s tumor had a BRAF mutation, which activates a mutant protein in the MAPK pathway that can be inhibited by the selective small-molecule kinase inhibitors vemurafenib and dabrafenib. 1 BRAF-targeted agents are typically recommended as initial therapy in those with aggressive and symptomatic disease based on the high rate of response to therapy and rapid onset of action. 3,8 Unfortunately, our patient failed initial therapy with dabrafenib, an effect that is known to occur due to developing tumor resistance, with the average duration of response being ∼6 months. 4
Ipilimumab is often initiated as a second-line agent due to immune-related toxicity. Typically, response develops slowly with transient progression of disease before a response (disease stabilization or tumor regression) is observed. 9,10 Immune-related adverse events (irAEs) significantly limit its use as common complications of therapy include enterocolitis, hepatitis, dermatitis, and endocrinopathies, although other organ systems can be involved. 11 Typically, irAEs are transient but if persistent may be life-threatening and require discontinuation of therapy. 10
This is the first case report documenting progression-free response to ipilimumab exceeding that of 2 years, without side effects of therapy. Response has been maintained to date, with no new sites of metastasis or symptoms at most recent 31-month follow-up. This type of long-term response is seen in the minority of patients with advanced metastatic disease with average progression-free survival cited between 2 and 3 months. 3 There is a brief report that describes a cutaneous metastatic melanoma treated successfully with ipilimumab, although progression-free survival did not exceed 1 year and side effects of therapy were not commented on. 12 In addition, this patient was not treated with BRAF-targeted therapy and was started initially on ipilimumab without delay in systemic treatment.
There is increasing evidence supporting the long-term survival benefit of ipilimumab even in patients presenting late with advanced metastatic disease. Unique to immunotherapy, there is potential to produce a durable treatment-free remission in selected patients. 3,8 This case adds to the evidence for starting ipilimumab early in those able to tolerate it, with the goal of producing a sustained response and preserved quality of life.
Future randomized trials are needed to determine optimal treatment sequence for patients with BRAF mutant melanoma with the goal of prolonging the proportion of patients who experience long-term survival. Patients should be enrolled in clinical trials whenever possible.
Footnotes
Authors’ Note
The patient has given consent to use her de-identified information and images for educational purposes in the form of teaching, research, scientific meetings, and other professional journals.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
