Abstract
We describe an interesting case of a 57-year-old man who presented with a rare case of orbital tuberculosis masquerading as sarcoidosis. The varied presentation of orbital tuberculosis may only become evident once a tissue diagnosis is available. Therefore, the dilemma in diagnosis of this rare condition highlights the need for definitive diagnosis through tissue biopsy by a plastic surgeon.
Keywords
Introduction
Tuberculosis (TB) is still common in developing countries, but orbital TB is considered quite rare. Its varied presentations may cause difficulty in diagnosis and may only become evident once a tissue diagnosis is available. The disease process has been known to involve the bony orbital walls, soft tissue, or both. 1 The presentation can cause confusion in diagnosis in the absence of a tissue diagnosis. We present an interesting case of orbital TB masquerading as sarcoidosis.
Case
A 57-year-old male with a history of orbital sarcoidosis presented with a 2-week history of worsening left eye proptosis, orbital swelling, orbital erythema, and decreased visual acuity. He also complained of a 3-week history of worsening left-sided headaches. He stated he had painful extraocular eye movements, fever, and chills. He denied orbital discharge or diplopia. He had no traumatic history, no seizure history, and no loss of consciousness. There was no recent history of sinusitis or upper respiratory tract infection. He denied neck stiffness, photophobia, chest pain, cough, and palpitations. He had no abdominal, joint, or urinary symptoms.
His past medical history was significant for orbital and pulmonary sarcoidosis, which had been in remission. He had bilateral cataract surgery performed in 2013. In addition, he had hypertension. His home medications included methotrexate and folic acid. He had no known drug allergies.
On social history, the patient was born in Pakistan and moved to Canada almost 20 years ago. He had returned to Pakistan only once in that time. He received the bacilli Calmette-Guérin vaccine as a child, had no known TB exposures, and had multiple negative TB skin tests in the past.
On presentation, the patient was febrile with stable vital signs. Examination revealed left eye proptosis, periorbital swelling, and periorbital erythema. The left pupil had a sluggish response to light. Visual acuity in the right eye was 20/400 and in the left eye was 20/200. There was mild scleral erythema and the visual fields were intact via confrontation. He had diplopia in left lateral and inferior gaze, and he had lateral gaze ophthalmalgia in his left eye. The remainder of the neurological exam showed no abnormalities. Examination of the oral and nasal cavities showed no abnormalities, and a nasopharyngeal scope examination was normal. Cardiovascular, respiratory, and abdominal exams were non-contributory.
Lab work revealed a hemoglobin of 138 g/L and a leukocyte count of 7.8 × 109/L. His electrolytes were within normal limits. Blood cultures did not grow any organisms and chest X-ray was normal.
Computerized tomography (CT) scan of the orbit and head showed prominent soft tissue stranding and thickening in the extraconal space adjacent to the superior and lateral rectus muscles, likely representing a phlegmon. There was bony destruction adjacent to the stranding that involved the roof of the left orbit. The bony left orbital roof and sphenoid wing erosion were suggestive of osteomyelitis. The soft tissue thickening extended intracerebrally anterior to the left temporal lobe and inferior to the left frontal lobe. The findings were concerning for intraorbital infection with intracranial extension. There was abnormal extradural soft tissue in the left middle cranial fossa. There was no evidence of acute intracranial hemorrhage and no space-occupying lesions. There were no signs of midline shift, herniation, or hydrocephalus. There were no obvious large epidural or subdural collections.
Magnetic resonance imaging (MRI) of the head showed left globe proptosis. In addition, soft tissue thickening in the superior lateral quadrant of the left orbit was contiguous with the adjacent extraocular muscles extending to the left superior and inferior orbital fissures and anterior cavernous sinus. Pachymeningeal enhancement over the left cerebral convexity was noted. There was mild swelling of the left-sided preseptal and periorbital soft tissues.
The MRI findings were noted to carry a differential diagnosis of neoplastic etiologies including metastatic disease, infection, or lymphoproliferative disorders, such as sarcoidosis. Infection was a less favoured diagnosis.
The patient was started on a 6-week course of vancomycin and ceftriaxone to treat a potential infectious etiology. The patient was also started on steroid treatment to address the possibility of orbital sarcoid. His diplopia and lateral ophthalmoplegia resolved while on antibiotics and steroids.
The patient was discharged home with antibiotics and steroids but returned to hospital several days later for worsening periorbital swelling. The patient was afebrile, and his condition was otherwise stable from discharge. He had been compliant with his medications.
His examination revealed left periorbital swelling, and his exam was otherwise stable. A repeat CT scan (Figure 1) revealed worsening erosion to the superolateral wall of the left orbit with persistent intracranial extension. Both the intraorbital and intracranial components increased in size since the prior CT scan.
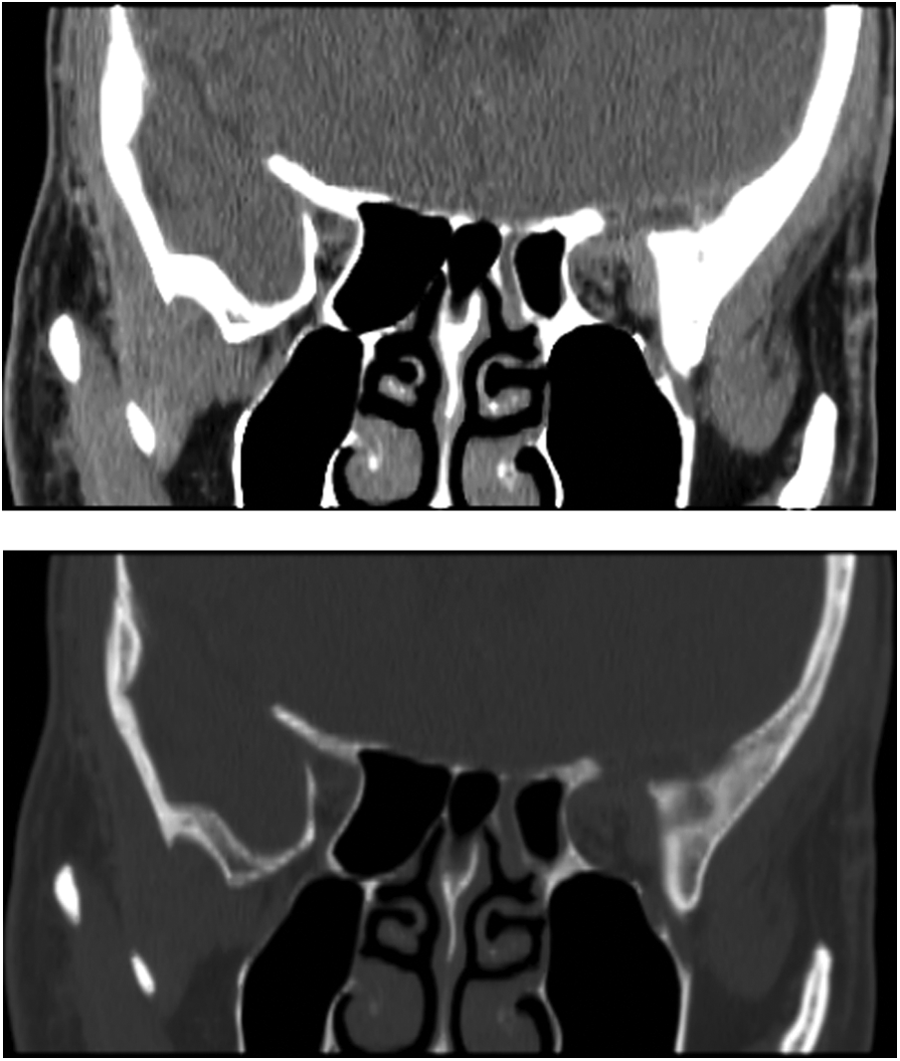
Computerized tomography scan of the orbits with (A) soft tissue and (B) bony views exhibiting left intraorbital soft tissue mass eroding the orbital roof.
Orbital tissue and bone biopsy were performed by a plastic surgeon for definitive diagnosis. There were no complications encountered during the operation. The specimen was sent for fungal culture, tissue culture, and mycobacterial culture.
The biopsy specimen was positive for TB with a positive 4+ acid-fast bacilli (AFB) seen on concentrated smear. In addition, microscopy was positive for mycobacterium TB complex by ribosomal RNA amplification. All other tests were negative. There was no evidence of pulmonary TB clinically or on chest X-ray.
The patient was started on isoniazid, rifampin, pyrazinamide, and ethambutol with pyridoxine for the treatment of his TB. On post-operative day 4, the patient still exhibited left-sided proptosis as seen in Figure 2. He continued prednisone therapy, antibiotic therapy was discontinued, and the patient was discharged home in stable condition.
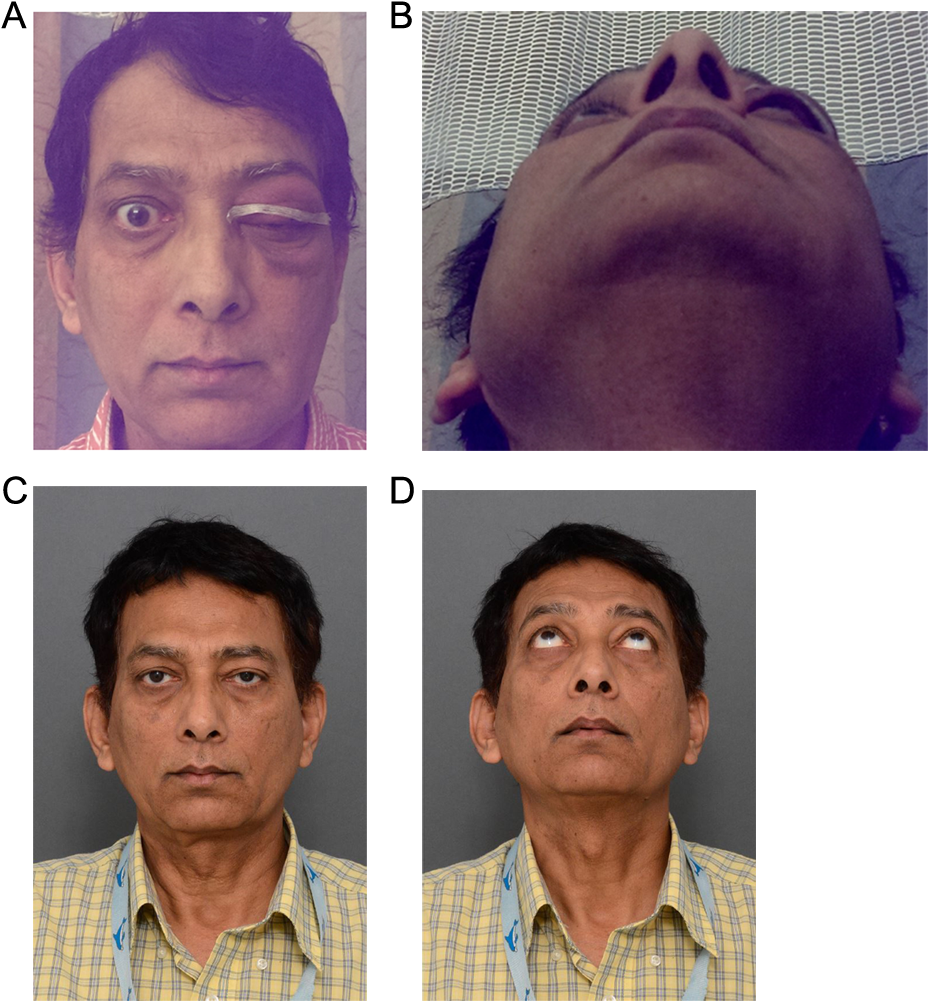
A, Frontal and (B) worm’s eye view of left eye proptosis on post-operative day 4, (C) frontal and (D) worm’s eye view of patient 18 months post-operatively.
Discussion
Although TB is uncommon in Canada, TB is a top infectious disease killer worldwide according to the World Health Organization. 2 In 2014, 9.6 million people fell ill with TB and 1.5 million died from the disease. 2 Nonetheless, orbital TB remains quite rare.
A review article by Madge shows only 91 documented patients with orbital TB in the English literature. Of all patients, 26 cases remained systemically well during their illness, and 53% of all cases had concurrent pulmonary TB. 1
The patient presented had orbital TB with bony erosion (see Figure 1), and Madge reported only 21 patients with similar findings. In addition to bony erosion, the presented patient also had intracranial extension. Only 6 other authors report intracranial extension such as demonstrated in our patient. 3 -8 The mean age of patients with orbital TB and bony erosion was 14 years, and our patient was significantly older at 57 years old. The mean duration of symptoms of these patients before presentation was 2 months (range: from 2 weeks to 7 years). All of these cases had radiological destruction, osteomyelitic changes, and erosion. Other features included proptosis, ophthalmoplegia, diplopia, a palpable mass, discharging sinus, or metachronous involvement of distant bones by TB. 1
The case presented describes a surprising outcome of orbital TB with bony erosion and intracranial extension, which initially masqueraded as orbital sarcoid. The initial misdiagnosis was aided by the previous history of orbital sarcoid, lack of significant risk factors for TB, and lack of pulmonary TB signs and symptoms.
Diagnosis of orbital TB is often clinical and can be confirmed through a biopsy with mycobacteria on culture. Radiologic findings may be suggestive, although inconclusive. 9 Histopathology may reveal granulomatous inflammation with sometimes caseation necrosis. Acid-fast bacilli testing may also be used, although the presence of AFB is often rare. 10 Nucleic acid amplification testing using polymerase chain reaction may also be used in the diagnosis of orbital TB. 11
Tuberculin skin testing (TST) may aid diagnosis as an ancillary tool but needs to be considered in context as 67% to 90% of healthy individuals in the Indian subcontinent may test positive. 11 Our patient had previous negative TST. The test results are stratified based upon the risk factors of the patient, but the false-negative rate for TSTs in proven TB cases is 10% to 20%. 12,13
Despite the difficulty in diagnosis, the management of orbital TB remains straightforward. The treatment of orbital TB is consistent with the treatment of pulmonary TB, which is a 2-month initial course of rifampicin, isoniazid, pyrazinamide, and ethambutol followed by a 4-month course of rifampicin and isoniazid. 14
Unfortunately, there is a general lack of data for the prognosis of orbital TB. No follow-up is yet available for the presented patient, although the majority of cases presented by Madge improved following initial treatment. Two cases of recurrence were reported, but no follow-up information was provided for 30% of cases. There have been 2 instances of death from spread to the brain from the orbit in the 1970s, 3,15 and no detailed radiologic imaging was used in those cases.
In summary, we present a rare case of orbital TB, which masqueraded as sarcoidosis. Although chest X-rays and TSTs should be included in the workup, orbital biopsy is essential for definitive diagnosis. Orbital TB is a rare condition, and orbital biopsy was essential for definitive diagnosis due to the lack of pathognomonic clinical features.
Footnotes
Statement of Informed Consent
The patient gave informed written consent for photographs and use of his medical information for publication.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
