Abstract
Large diaphragmatic defects present a reconstructive challenge, often necessitating the use of synthetic materials. We report our experience reconstructing large diaphragmatic defects using human acellular dermal matrix (HADM). Patients unable to undergo primary repair of diaphragmatic defects from 2009 to 2013 were reconstructed using HADM. A chart review was performed to investigate immediate and late post-operative outcomes. Construct stability was assessed with repeat imaging. In addition, a literature review was performed to identify studies in which HADM had been used for diaphragm repair. Four patients required reconstruction of large hemi-diaphragmatic defects. All patients had chest tubes placed, which remained in situ from 4 to 10 days post-operatively. Two patients also had drains in dead space surrounding HADM; these were removed between 6 and 9 days post-procedure. Length of hospital stay ranged from 8 to 65 days. Post-operative complications were seen in 2 patients: surgical site cellulitis and failure of extubation due to persistent respiratory failure. There were no adverse events related to HADM, and all patients remained disease free without evidence of repair failure on radiographic follow-up, ranging from 14 to 62 months. The literature review identified 3 studies in which all diaphragms repaired with HADM remained intact without need for explantation despite common post-operative complications including fluid collections and surgical site infections. Diaphragm reconstruction with HADM is limited to a small number of patients and modest follow-up periods; the neodiaphragms appear durable in contaminated fields, without evidence of repair failure. Our results, and previously published data, indicate HADM is a reasonable option for diaphragm repair.
Introduction
The majority of acquired diaphragmatic defects result from trauma or surgical resection. Occasionally, defects may be too large or complex to allow for tension-free, primary closure, with definitive closure often necessitating the use of synthetic materials. 1 Concerns over contamination and visceral adhesions, however, preclude most synthetics in the setting of lung or intra-abdominal organ resection. 2,3 Polytetrafluoroethylene (PTFE; GORE-TEX® W.L. GORE & Associates, Inc.) is considered the gold standard for diaphragm repair due to its durable and anti-adhesion properties. However, as a foreign body, an inflammatory process will still be activated, and without host incorporation, it would require removal should infection arise. 4 Although autologous tissue reconstruction may avoid the shortcomings of synthetic materials, its use is restricted by prolonged operative time, defect size, and donor site morbidity. Human acellular dermal matrix (HADM) may offer an alternative and act as an adjunct to autologous reconstruction, though there are few reports of its use for diaphragm repair. 5 –7
Human acellular dermal matrix is an allogenic grafting material derived from cadaveric dermis and epidermis. All cellular components are removed, preserving the extracellular matrix and basement membrane. This provides a scaffold for vascular ingrowth and replacement with host connective tissue. 8 It is commonly used in breast reconstruction, 9 abdominal reconstruction, 10,11 and hiatal hernia repairs. 12 We report our initial experience using HADM at the Foothills Medical Centre (Calgary, Alberta) to reconstruct large diaphragmatic defects in 4 patients: 3 in the setting of combined chest wall and diaphragm resection for primary neoplasm and 1 for a chronic, traumatic diaphragm rupture.
Methods
Patients unable to undergo primary repair of diaphragmatic defects from 2009 to 2013 were reconstructed with HADM. Information was obtained from chart review to investigate immediate (infection, fluid collection, extubation, time to drain removal) and late post-operative outcomes (hospital length of stay, graft failure, infection). Construct stability was assessed with repeat imaging (CT or chest X-ray) and clinical examination, with repair failure being defined as evidence of neodiaphragm failure or need for neodiaphragm removal.
A literature review was performed to identify other studies in which HADM had been used to reconstruct diaphragmatic defects. Papers were included which used HADM for diaphragm repair and excluded if only used for chest wall reconstruction.
Cases
Case 1
A 76-year-old male underwent resection of a low-grade chondrosarcoma at the left costochondral junction. Resection included the costal margin, 3 ribs, mediastinum, pericardium, and hemi-diaphragm, leaving a ∼8 × 5 cm defect in the hemi-diaphragm; the skin and muscle anterior to the chest wall were salvaged. Bovine pericardium was used to repair the pericardial defect. An inlay technique was used for the diaphragm, in which the defect was bridged by suturing HADM circumferentially to the diaphragm with 0-polypropylene in an interrupted, horizontal mattress fashion. The chest wall was reconstructed with HADM using interrupted, 0-polypropylene placed through and around ribs and through the rectus abdominis and lateral chest wall muscles. The salvaged myocutaneous layer was closed primarily over the HADM chest wall construct, and a left-sided chest tube was placed intraoperatively and removed 9 days post-operatively. Their stay was complicated by worsening dementia and an upper gastrointestinal bleed secondary to oral NSAID use. He was discharged 19 days after surgery, and at 19 months, there was no evidence of repair failure.
Case 2
A 29-year-old male with synovial sarcoma of the right costal margin (Figure 1) underwent en bloc resection of skin, ribs 8-12, the lateral third of hemi-diaphragm (10 × 3 cm), a portion of the latissimus dorsi, 2 liver segments, and peritoneum (Figure 2). Human acellular dermal matrix was inlayed and secured using interrupted, 1-polypropylene around and through the remaining rib ends and hemi-diaphragm (Figure 3). Advancement of latissimus and overlying skin reconstructed the chest wall, while omentum was advanced to cover exposed liver. Two right-sided chest tubes were removed 4 days post-operatively. Two round Blake drains were placed in the dead space between the neodiaphragm and liver and were removed 6 days post-operatively. The patient developed a surgical site cellulitis, managed successfully with oral antibiotics, and was discharged 12 days after surgery. The patient underwent post-operative chemotherapy, and repair remained intact at 62-month follow-up (Figure 4).
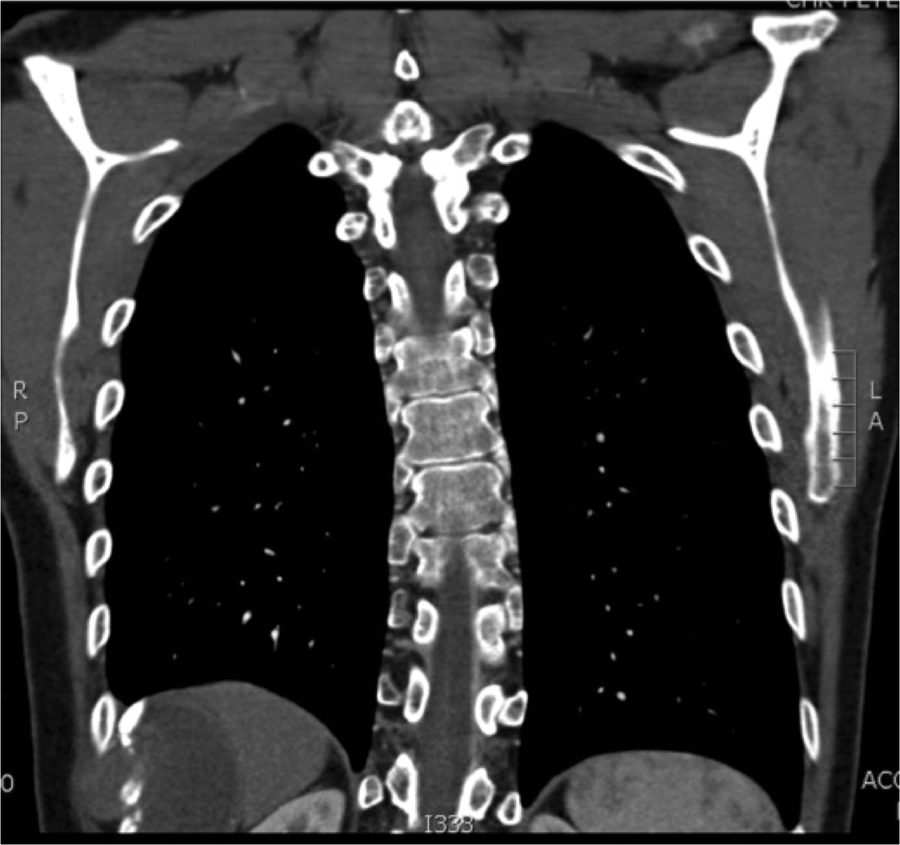
Preoperative chest CT, coronal slice, of case 2 with synovial sarcoma of right costal margin, invading chest wall, diaphragm, and liver.
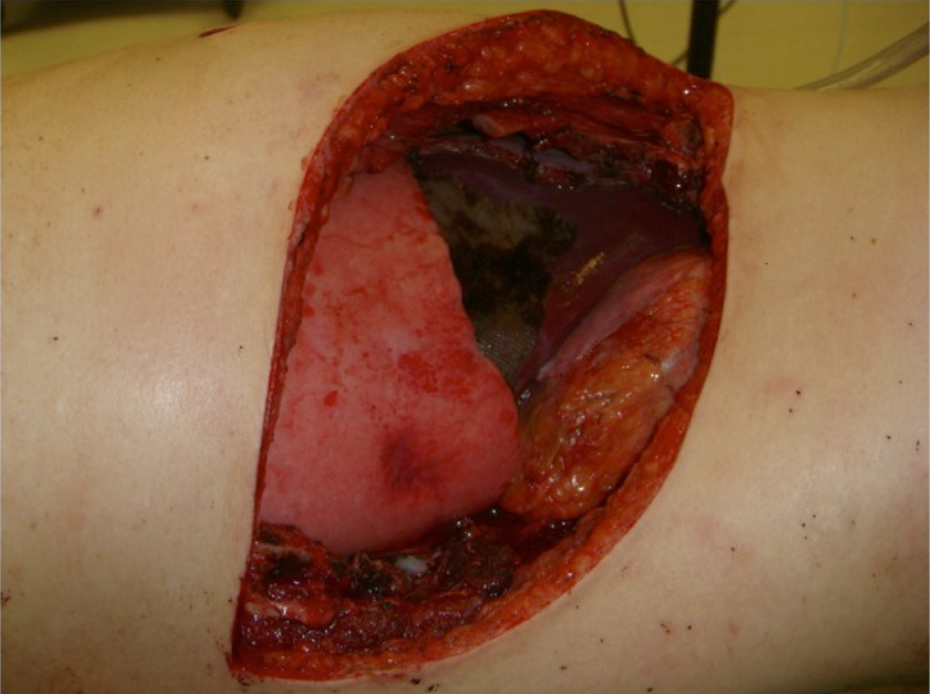
Case 2’s defect after surgical resection of portions of ribs 8-12, en bloc with the lateral third of hemi-diaphragm, overlying skin, portion of the latissimus dorsi, 2 liver segments, and peritoneum.
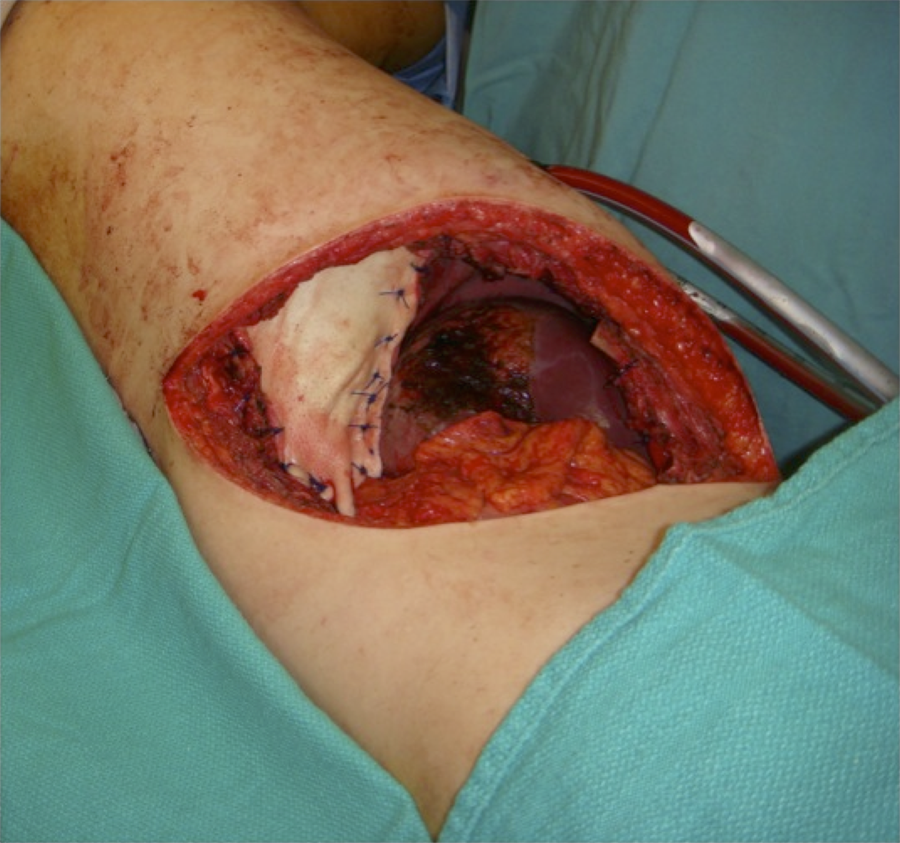
Human acellular dermal matrix inlayed and secured through the remaining rib ends and right hemi-diaphragm cuff.
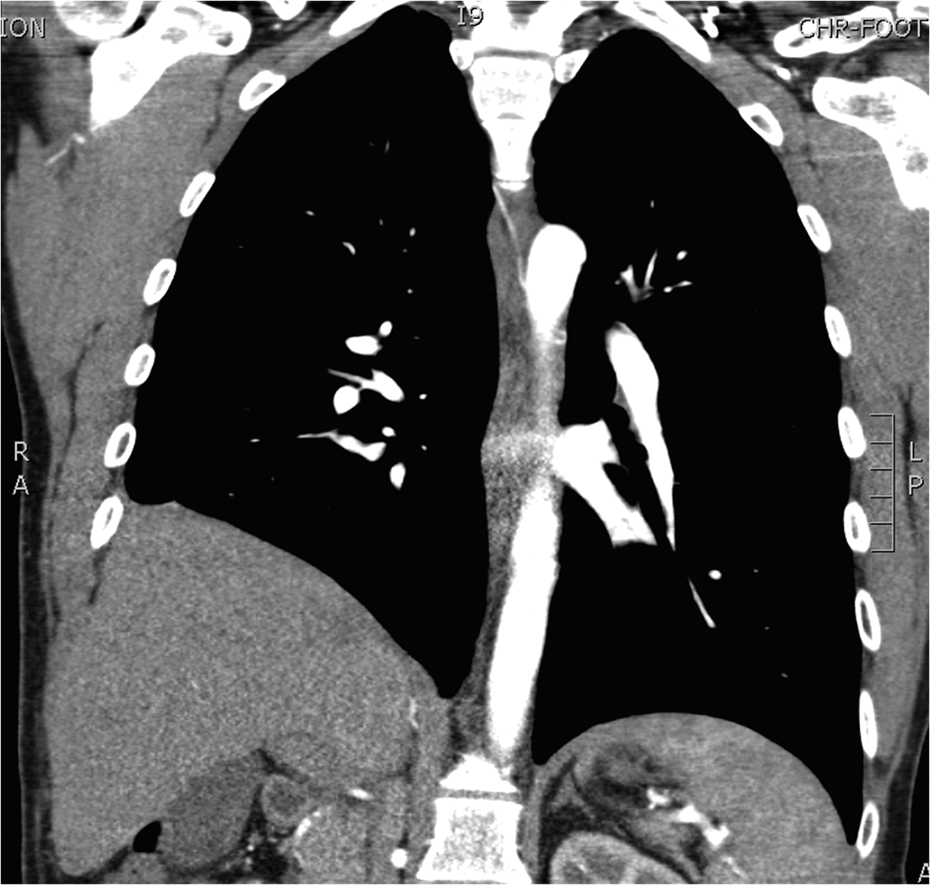
Post-operative chest CT, coronal slice, at 62-month follow-up. Human acellular dermal matrix sutured to remaining, cephalad rib ends posteriorly. Liver and retroperitoneal organs appear elevated without evidence of human acellular dermal matrix (HADM) diaphragm repair failure.
Case 3
A 73-year-old female on home oxygen presented with respiratory distress, secondary to restrictive lung disease from a traumatic, right hemi-diaphragmatic hernia following an MVC 40 years prior. Upon reduction of the right lobe of liver, gallbladder, stomach, colon, and omentum from the right chest cavity, a defect with minimal diaphragm cuff in the area of the IVC remained. The hemi-diaphragm was repaired with HADM inlay and secured with interrupted, horizontal mattress, 1-polypropylene sutures. Two right-sided chest tubes were removed 13 days post-operatively. The patient required post-operative ventilator support in the ICU for respiratory failure secondary to atelectasis and right-sided pleural effusions. She was discharged 65 days after admission, without supplemental oxygen therapy. There was no evidence of repair failure at 14-month follow-up.
Case 4
A 36-year-old female underwent resection of a right chest wall chondrosarcoma, with removal of the anterior portion of ribs 6-9, en bloc with the anterior third of hemi-diaphragm and overlying soft tissue. Two liver lesions undetected on preoperative imaging were also resected. A hemi-diaphragmatic defect of ∼10 × 5 cm was reconstructed with HADM inlay secured to rib ends and rectus fascia with 0-polyethylene. The chest wall defect was repaired with a pedicled TRAM flap. Two posterior chest tubes were removed by 7 days post-operatively. Two round Blake drains placed caudally to the neodiaphragm, and 1 intra-abdominally, were removed by 9 days post-operatively. The patient was discharged after 9 days, without evidence of repair failure at 25-month follow-up.
Results
Four patients required reconstruction of large hemi-diaphragmatic defects (average 9 × 4 cm): 3 in the setting of combined chest wall and diaphragm resection for primary neoplasm and 1 for a chronic, traumatic diaphragm rupture. None of the patients received radiation therapy. All patients had chest tubes placed intraoperatively, which remained in situ from 4 to 10 days post-operatively. Two patients also had drains placed in dead space surrounding HADM; these were removed between 6 and 9 days post-procedure. Post-operative complications were seen in 2 patients: surgical site cellulitis and failure of extubation due to persistent respiratory failure. Length of hospital stay ranged from 8 to 65 days. There were no adverse events related to HADM, and all patients remained disease free without evidence of repair failure on radiographic follow-up, which ranged from 14 to 62 months.
Results of our literature review yielded 3 papers in which HADM was used for diaphragm reconstruction. 5-7 Similar to our study, these are small, retrospective patient samples. Table 1 provides a comparison of patient outcomes in those papers to our study. The most common post-operative complication was peri-graft fluid collections, none of which required HADM removal. In all cases, the neodiaphragms remained intact at follow-up.
Comparison of Our Post-Operative Outcomes With the Current Literature, Following HADM Diaphragm Reconstructions.
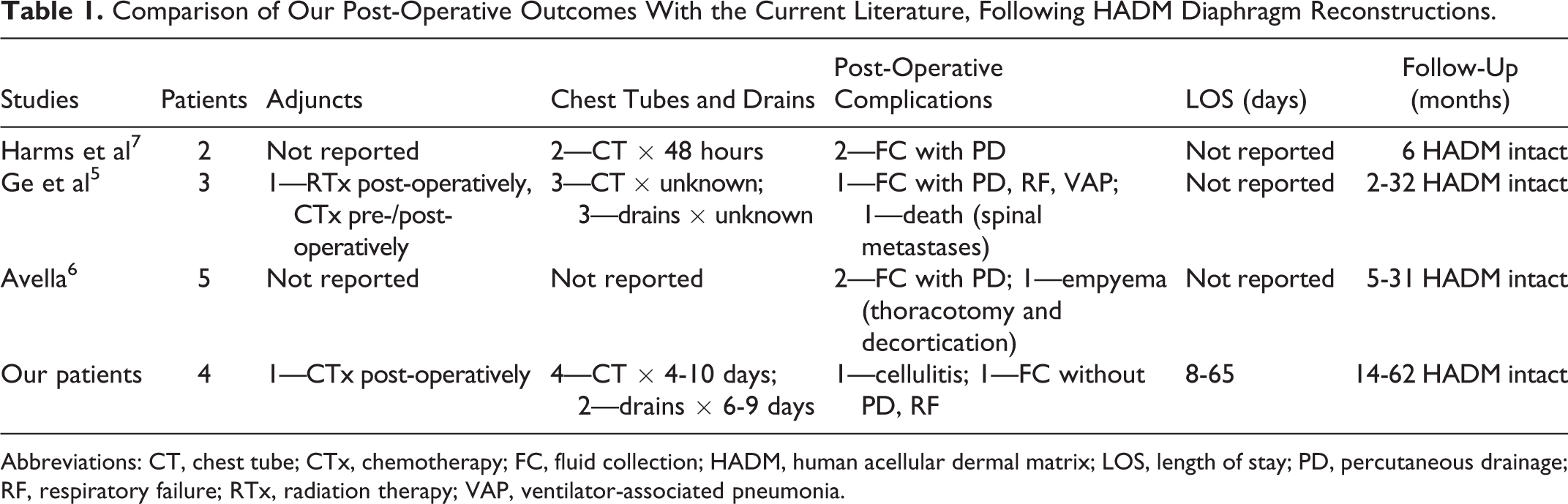
Abbreviations: CT, chest tube; CTx, chemotherapy; FC, fluid collection; HADM, human acellular dermal matrix; LOS, length of stay; PD, percutaneous drainage; RF, respiratory failure; RTx, radiation therapy; VAP, ventilator-associated pneumonia.
Discussion
Large diaphragmatic defects can preclude tension-free primary repair, necessitating use of polypropylene or PTFE for reconstruction. 1 Unfortunately, in cases with concurrent resection of lung or abdominal viscera, synthetic grafts are prone to infection, requiring subsequent removal. 13 Further reports of erosion into adjacent organs have caused surgeons to seek alternatives. 2,3 Absorbable polyglactin, though useful in contaminated fields, requires replacement with a permanent mesh in a second operation. Similarly, PTFE is perceived as the gold standard for diaphragm repair, and like other durable synthetic meshes, its removal is often necessary in the setting of infection. 4 Reports of successful HADM use in abdominal reconstruction of contaminated fields 14,15 have led to its use in diaphragm reconstruction. Although the use of HADM does not prevent infection in contaminated fields, it may be able to endure the course of an infection and forgo removal. Human acellular dermal matrix was used for diaphragm reconstruction in 3 other studies, 5-7 in a similar inlay technique as previously described (“Case 1” section). All diaphragms repaired with HADM remained intact and did not require explantation despite common post-operative complications such as fluid collections and localized, surgical-site infections (Table 1).
Human acellular dermal matrix has been used in a variety of settings, including ventral hernia repair. Although we do not have significant experience in dealing with contaminated wounds, the general surgery literature suggests HADM use in complicated (contaminated defects at risk of infection, adhesions, and fistula formation) ventral hernia repair. However, despite showing short-term promise with respect to contamination, at long-term follow-up, high recurrence rates have lead it to be largely abandoned. 16 In light of these high recurrence rates, 2 issues should be addressed: adequate follow-up and unique nature of the diaphragm. With respect to follow-up, our shortest duration is 14 months, meeting the mean rate for ventral hernia repair failures of 13.4 months cited by Blatnik et al. 16 The laxity issues encountered in ventral hernia repair may be inconsequential in hemi-diaphragm repair. It is possible that HADM pliability is a favourable feature for simulating diaphragm function in a location that must counterbalance intra-abdominal and intrapleural pressures.
In cases of infection, HADM is associated with a high salvage rate compared to other synthetic materials. 15,17 In a 12-year follow-up of HADM in breast reconstruction, tissue analysis showed that graft volume was retained and HADM was integrated and organized into host collagen with little or no capsule formation or inflammation. 18 Unfortunately, there continues to be a paucity of information on long-term outcomes of HADM use. In addition to the lack of long-term effects and peri-construct fluid collections, 19 cost remains a barrier to widespread HADM use. However, this cost may be offset by increased operative time, secondary surgical revision, and staged reconstruction required with synthetic and autologous reconstruction.
Conclusion
Diaphragm reconstruction with HADM is limited to a small number of patients and modest follow-up periods. The neodiaphragms appear durable over time, and even in the setting of surgical site infection and fluid collection, without evidence of diaphragm herniation or repair failure. These results, in addition to previously published data, indicate HADM is a reasonable option for diaphragm repair.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
