Abstract
Breast reconstruction with expander implant is the most common breast reconstructive procedure. Irradiated patients are seldom reconstructed this way because the tissue expansion is difficult and the complication rates are higher. Pneumothorax is a serious condition and can be seen as a complication to the operation. Literature is sparse; hence, the only study is by Schneider et al who found an incidence of 0.55%. The study focused on immediate reconstruction only and did not report the percentage of irradiated patients. We present a unique case of iatrogenic pneumothorax in a previously irradiated patient undergoing delayed reconstruction with expander insertion. This provides a new perspective to the complication, raising the question whether irradiated patients are at higher risk. As a plastic surgeon, it is important to be aware of this complication and to take account of radiation when selecting reconstruction method.
Introduction
In 2016, 109 256 women underwent breast reconstruction in the United States, 1 and expander implant accounts for 70% of the procedures. 2 The most common early complication is infection, ranging from 2.5% to 4.9%. 3 The rates of early complications are higher in the expander insertion than in the exchange procedure. 4
Pneumothorax is a serious and potentially fatal condition. Current standard of care includes consultation with a thoracic surgeon, a chest X-ray (CXR), and possibly insertion of a chest tube. If the patient is hemodynamically stable, the surgery can be continued. 5
Within breast surgery it is a known complication to breast augmentation, 6,7 but little literature exists regarding reconstruction surgeries. The only study is by Schneider et al who found an overall incidence of pneumothorax in immediate tissue expander reconstruction of 0.55% in 34 567 patients. 5 Pneumothorax is also a rare complication to lipoinjection to breasts. Thus, in a meta-analysis of 36 studies, a single case was registered. 8 We present a case of iatrogenic pneumothorax during delayed tissue expander reconstruction from The Department of Plastic Surgery and Burns, Rigshospitalet, Copenhagen University Hospital, Copenhagen, Denmark.
Case
A 32-year-old Caucasian woman was elected for delayed tissue expander–implant breast reconstruction to her right breast. She was a nonsmoker, had a body mass index (BMI) of 25 kg/m2, and her only comorbidity was unspecified oligoarthritis. Two years earlier she had been diagnosed with breast cancer and had undergone neoadjuvant chemotherapy, mastectomy, and axillary lymph node dissection. Additionally, she had received postmastectomy radiotherapy of 50 Gy in 25 fractions.
During the expander insertion, thin intercostals and serratus anterior were noticed, as well as a layer of fibrous tissue covering a tight pectoralis major. A sudden sound of air escaping the chest wall, a decrease in volume on the capnography, and a drop in saturation from 100% to 97% led to the discovery of a 2-mm defect in the intercostal fascia above the sixth intercostal, hence a pneumothorax was suspected. The injury was caused by the electrocautery, and it was unknown whether it involved the visceral pleura.
A superior anaesthesiologist was called to the operating room, and he consulted a thoracic surgeon. Since the patient remained respiratory and circulatory stabile, the surgery was continued.
Before the patient awoke, a CXR was taken, confirming the anticipated diagnosis of pneumothorax. However, it was so small that it did not need drainage (Figure 1). A second CXR 2 hours later (Figure 2) showed further development, and therefore, a chest tube was inserted (Figure 3). The tube was removed on the fourth postoperative day when air leak had resolved, and a control CXR showed complete expansion of the lung.
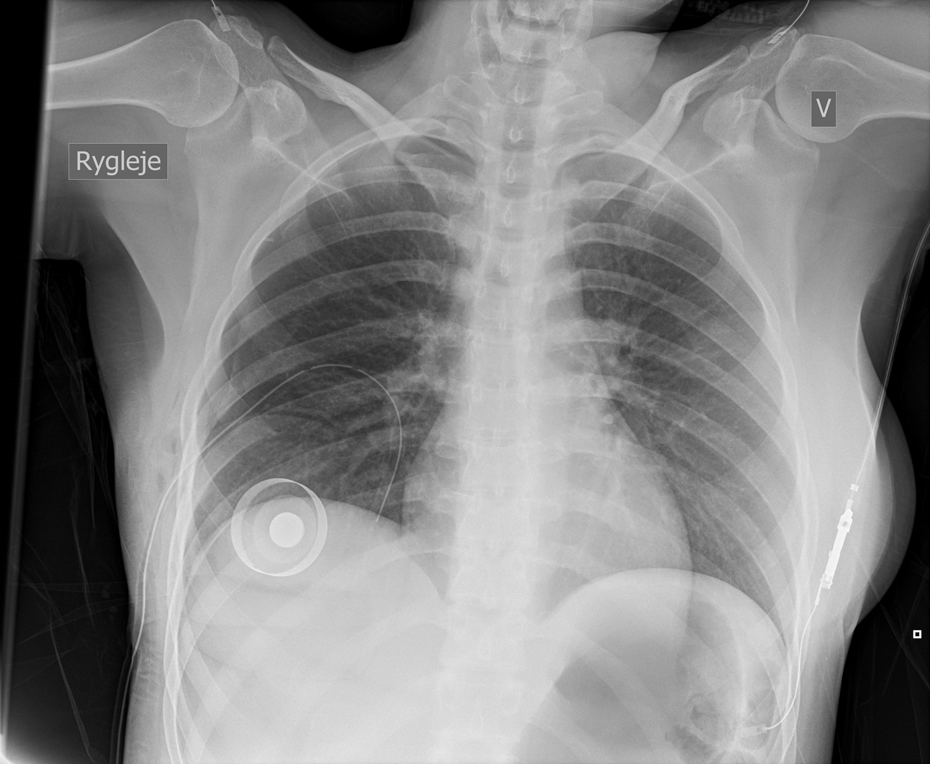
Chest X-ray taken just after the surgery showing a right-sided pneumothorax. The patient is lying down. You can see the expander and the pain catheter in the subpectoral pocket on the right side.
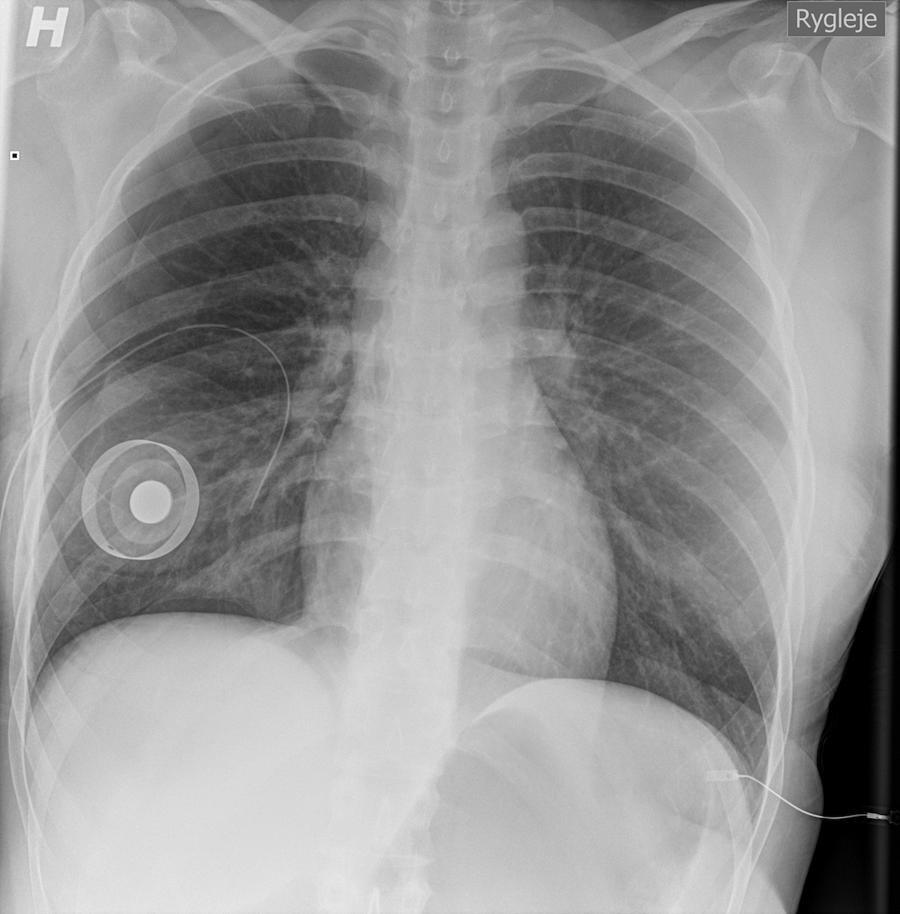
Chest X-ray taken 2 hours after the surgery shows further development in the right-sided pneumothorax. The patient is lying down.
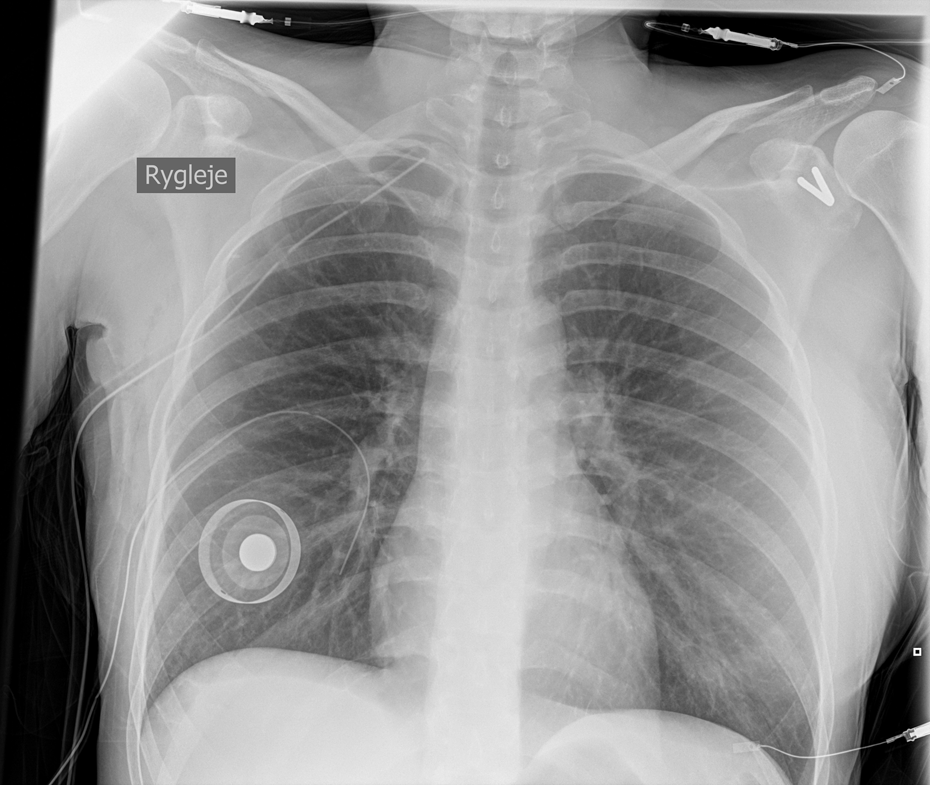
Chest X-ray taken after insertion of a chest tube in the apex of the lung. The patient is lying down.
The patient was discharged without further complications to standard expander filling at the outpatient clinic and had not developed further complications at follow-up 3 months later. The operator was an experienced superior plastic surgeon who had not previously caused an iatrogenic pneumothorax during this type of procedure.
Discussion and Conclusion
We have presented a unique case of iatrogenic pneumothorax as a complication to delayed breast reconstruction with insertion of a tissue expander in a previously radiated patient. We have described the patient’s full medical and surgical history, her BMI, the intraoperative discoveries and management, and follow-up.
The most common operative cause of pneumothorax is thought to be penetration of the pleura by a needle, during a regional rib block or injection of a local anaesthetic, 7,9 or as in this case, direct injury during dissection or cauterizing. Another suspected cause includes barotrauma due to air entrapment in the subpectoral pocket. 10 Iatrogenic causes related to general anaesthesia or pre-existing conditions may also precipitate pneumothorax, that is, high anaesthetic ventilation pressure, difficult intubations, and ruptured pulmonary blebs. 7
Previously irradiated patients are rarely chosen for this operation because the tissue expansion is difficult and there is an increased risk of infection and implant failure. 2,11,12 In contrast, a study by McCarthy et al on 1170 expander–implant reconstructions did not find radiation associated with greater complication rates. 13 However, the group of irradiated patients (10%) were highly select with good skin quality. If the patient is not a candidate for autologous tissue surgery, the expander–implant method does remain an option, small breast size and good skin quality after radiation being favorable. Furthermore, soft tissue coverage with lipoinjection before placement of the expander can help facilitate the reconstruction. 14
An important difference in immediate and delayed reconstruction is the presence of mastectomy scar tissue and, often, old seroma cavities, but it is not studied whether this is an actual risk factor. Likewise, it is not examined whether previous radiation poses a risk. Hypothetically though, both increase the risk of unintended perforation of the chest wall, because the tissue is harder and more friable. The one existing study on the matter by Schneider et al is on immediate reconstruction only and does not specify the causes of the pneumothoraxes nor previous irradiation in the study population, aside from in the 3 reported cases, of which all were iatrogenic and none had been irradiated. 5
Schneider et al comment that patients with low BMI may be at increased risk because of thin anterior intercostals. However, all 3 reported cases along with our case had normal BMIs ranging from 20.3 to 25 kg/m2. 5
Our case provides a new perspective to this complication, raising the question whether irradiated patients are at higher risk. We hypothesize that the previous radiation combined with mastectomy scar tissue in the operating field has contributed to an increased risk of chest wall perforation. However, we cannot conclude definitively on the matter due to lack of cases and literature. Further studies with specified causes and comparison of radiated versus nonradiated patients and immediate versus delayed reconstruction would be wish worthy in the future.
As a plastic surgeon, it is important to be aware of this serious, although very rare, complication to tissue expander placement for breast reconstruction. Radiation should be taken account for when choosing reconstruction method, and irradiated patients should have their operation performed by an experienced plastic surgeon.
Footnotes
Authors’ Note
The work originates from Department of Plastic Surgery and Burns, Rigshospitalet, Copenhagen University Hospital, Denmark. For this type of study, formal consent is not required. This article does not contain any studies with human participants or animals performed by any of the authors. Additional informed consent was obtained from all individual participants for whom identifying information is included in this article.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
