Abstract
Arterio-venous malformations (AVMs) are rare vascular anomalies due to the absent interposition of the capillary system between arteries and veins. Despite many AVMs being asymptomatic, pain, bleeding, functional impairment, and neurological compression can be observed, depending on the location of the lesion. Surgical removal of symptomatic lesions is the gold standard treatment. The vast majority of AVMs are sporadic, with only few familial cases reported. The pathogenics of the lesions are still elusive, although mutations in the PTEN and RASA1 gene have been identified. We report on an unusual presentation of an AVM occurring in similar anatomic locations and within concurring time spans, in a daughter and her mother. Both patients were negative for the known mutations.
Introduction
Arterio-Venous malformations (AVMs) are vascular lesions resulting from developmental disorders in the arterial–capillary–venous connection. This leads to direct contact between arteries and veins through a complex, tangled web of abnormal AV fistulae without the interpositions of a normal capillary network.
Arterio-Venous malformations can be observed at birth as a pale halo on the skin of the head and neck that enlarges during early childhood. 1 In other cases, AVMs can occur in internal organs mainly the brain, followed by the lung, the liver, and the gastrointestinal system.
The pathogenesis of this condition is still elusive. Reports of associations with PTEN and RASA1 mutations have been described. 2,3
Imaging, including ultrasound, magnetic resonance imaging (MRI), and angiography, has proved of pivotal importance in both diagnosis and the treatment of the lesions. 4 If untreated, AVMs can be complicated with bleeding, ulceration, and refractory pain. Symptoms usually depend on the site of the lesions and growth rate of the AVM. 5 In rare cases, lethal cardiac insufficiency can occur due to increased cardiac output. Surgical excision of the lesion still represents the gold standard treatment, often combined with preoperative embolization.
Case
An 18-month-old female was admitted to the Vascular Anomaly Clinic of our institution due to an extensive vascular lesion on the volar aspect of her left wrist (Figure 1). Personal medical history was otherwise unremarkable.
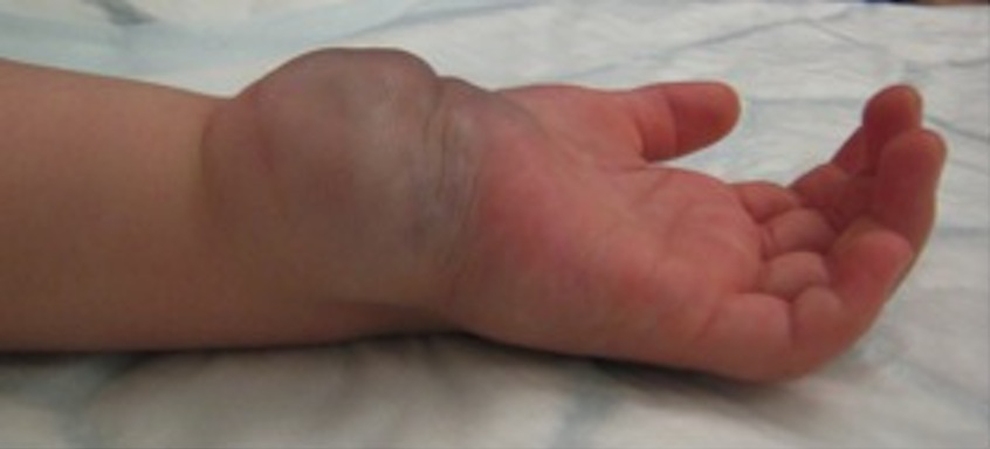
Clinical presentation of the lesion showing an extensive vascular lesion on the volar aspect of her left wrist.
The lesion had been present since birth and was growing with the child, without showing any signs of involution. Physical examination revealed a warm and pulsating mass.
Upon Doppler ultrasound imaging, a diagnosis of AVM was made. Due to the mother’s concern of increasing limitation of the use of the child’s left hand, as well as the potential aesthetic sequelae, surgical resection of the lesion was recommended.
Intra-operative findings revealed that the AVM spared the ulnar artery and nerve, as well as the superficial vascular arch of the wrist. Although tethered to, the lesion did not involve Guyon’s canal or its contents (Figure 2). Histopathology confirmed the diagnosis of AVM. The child’s post-operative course was uneventful.
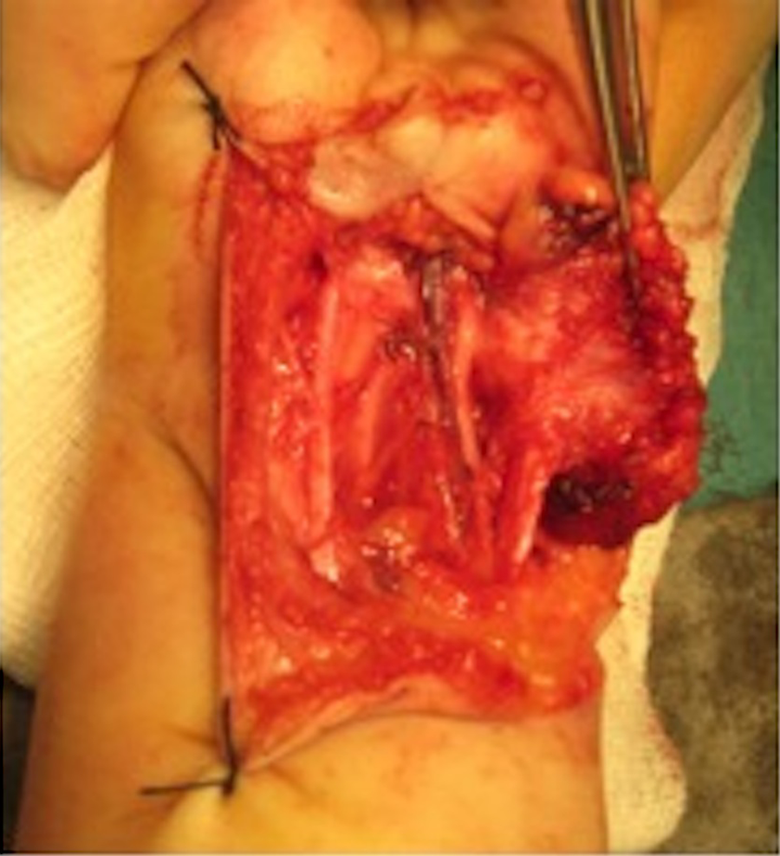
Intra-operative findings of the daughter’s lesion revealing sparing theulnar artery and nerve, as well as the superficial vascular arch of the wrist.
At the 1-year post-operative follow-up, the mother stated that she herself had been suffering a dull achy pain on the ulnar aspect of her own left hand, started around 2 years prior.
On examination of the mother’s hand and wrist, a soft and partially mobile 1 cm × 2 cm mass on the volar ulnar aspect of the mother’s left fifth metacarpal was palpated. No associated sensory or motor deficiencies were noted on the examination of the upper extremity. Ultrasound imaging indicated a vascular lesion (Figure 3), and MRI findings were suggestive of AVM (Figure 4).
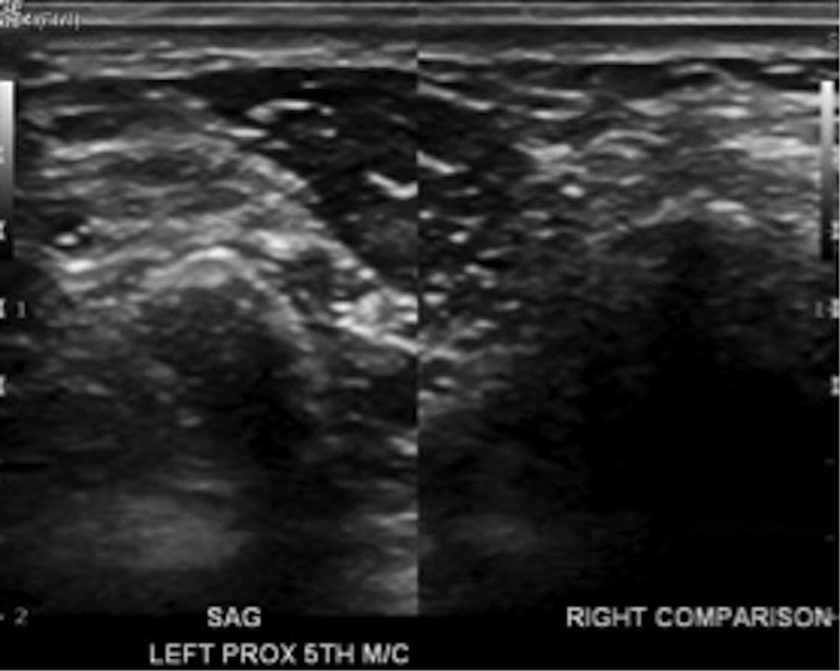
Ultrasound imaging of the lesion (mother’s).
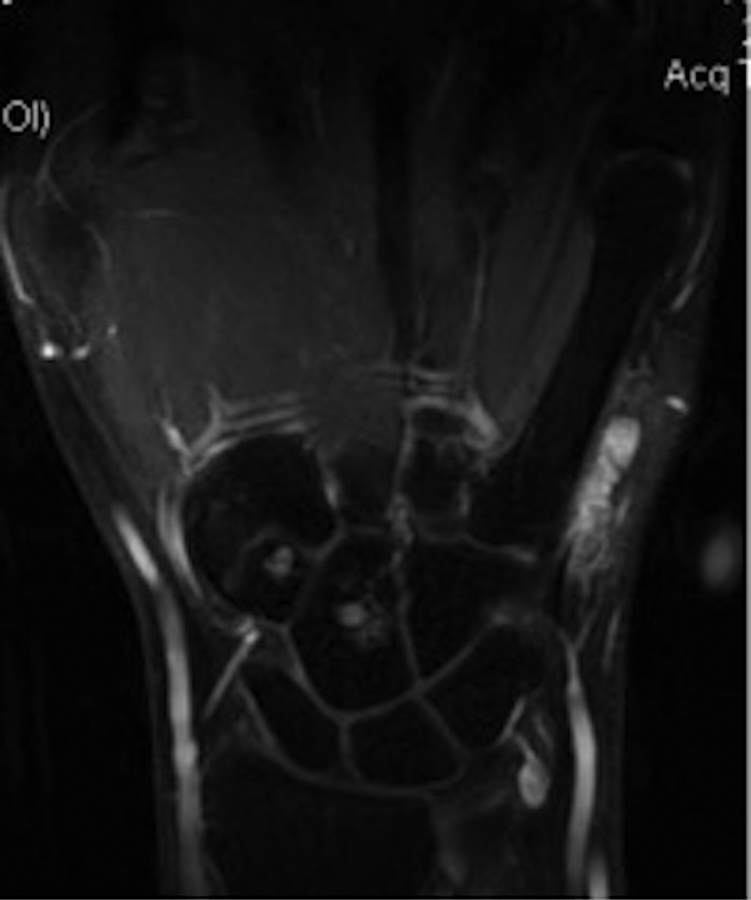
Magnetic resonance imaging (MRI) of the lesion (mother’s).
Due to the persistent pain, the lesion was surgically excised. Intra-operatively, the mass was fully imbedded within the patient’s hypothenar musculature creating a crevice on the surface of the metacarpal bone to which it was tethered. Adjacent vessels and nerves were not involved (Figure 5). Histopathology confirmed the diagnosis of AVM. The mother’s post-operative course was uneventful.
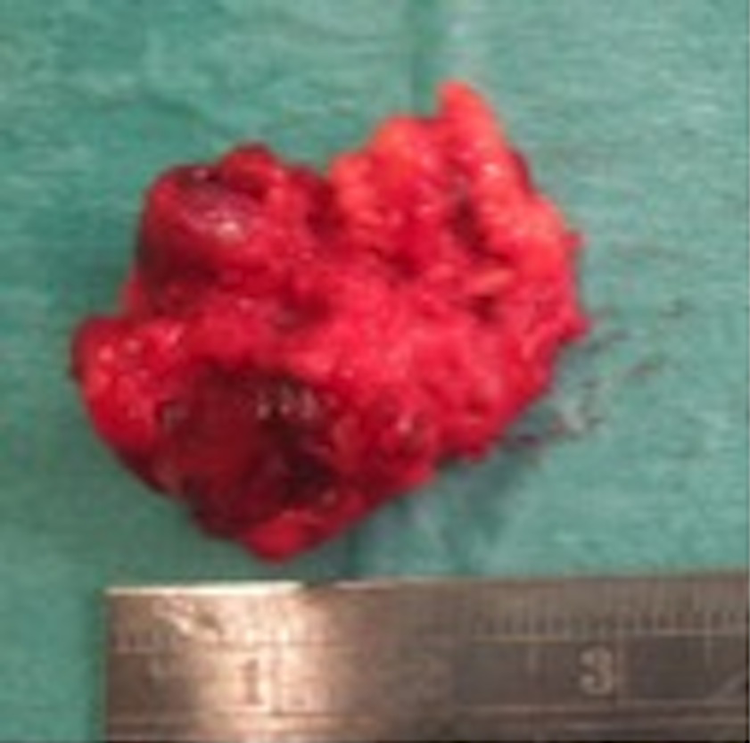
Intraoperative findings of the mother’s lesion showing the mass to be fully imbedded within the patient’s hypothenar musculature creating a crevice on the surface of the metacarpal bone to which it was tethered.
No recurrence of AVM was noted in either patient. Genetic investigations in both mother and daughter were negative for both PTEN and RASA1 mutations.
Discussion
The present report highlights the unusual presentation of a single AVM lesion, occurring in almost the exact same location and around the same period of time, in both a mother and child.
Each patient presented with a single lesion, but both were otherwise healthy. Of note, neither the child’s father nor her older brother ever presented with a history of vascular anomalies.
Familial cases of AVMs are usually extensive lesions, often associated with syndromic phenotypes, including hereditary hemorrhagic telangiectasia, Rendu-Osler-Weber syndrome, and Parkes Weber syndrome.
The recent discovery of associated mutations in PTEN and RASA1 genes has brought new light on the pathogenesis of the disease. Both genes are involved in the normal development of the vascular system; therefore, the aberrant angiogenesis resultant of mutations in those genes would likely explain the presence of AVM in those patients. Our cases, however, were negative for both mutations, which may confirm the hypothesis of the existence of other mutations still to be elucidated.
Interestingly, the timeline indicates that the lesions in both patients presented in a similar time span; being that the mother’s lesion started to become symptomatic coinciding with the pregnancy. This supports the promoting role of estrogen hormones in the lesion’s proliferation. Further studies are necessary to investigate the possible correlation.
This case illustrates that while AVMs most commonly present in the pediatric population, little is known on the subject of adult onset AVM-associated symptoms, especially during pregnancy and the effect this may have on a developing fetus.
Footnotes
Authors’ Note
All authors contributed equally to the writing and revision of the manuscript, and all approved the final version submitted for publication.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
