Abstract
Reconstruction of massive soft tissue defects is challenging in the setting of polytrauma. We present a case report of a polytrauma patient with an open acetabulum fracture with a necrotizing wound that was managed with a hemipelvectomy and contiguous thigh and leg fillet flap. The harvest of the entire leg flap was utilized due to the presence of a high cervical spine injury that rendered the lower extremities non-functional. The patient’s tenuous medical status was normalized once the necrotizing wound was covered, and subsequent complications related to the flap were minimized. The patient currently enjoys a reasonable quality of life consistent with that of a C7 quadriplegic.
Keywords
Introduction
Reconstruction of large soft tissue defects in the setting of polytrauma are challenging to address, especially in the case of a contaminated or infected wound bed. Protocols have been described to treat severe open lower extremity fractures that include early aggressive and repeated debridement of necrotic tissue, fracture stabilization (usually with external fixation), early soft tissue coverage with local muscle flaps or free muscle transfers, 1 –4 and staged skeletal reconstruction. 5,6 Obtaining adequate soft tissue coverage with the use of vascularized local or free tissue transfer is associated with donor site morbidity but can be a potentially life-saving procedure for patients with pelvic trauma, large soft tissue defects, or uncontrollable sepsis of the lower limb. 7,8
Large free tissue transfers or pedicled local myocutaneous flaps are commonly troubled post-operatively with oedema of the transplanted tissue. 9 In addition to oedema, the post-operative course can be complicated by venous flap insufficiency, hematomas, hemorrhage, and infections 10,11 causing partial or total flap necrosis. Few strategies exist to mitigate flap congestion and mainly involve surgical re-exploration and application of leeches or compressive stockings, 12 but it seems the best answer is to avoid congestion if at all possible.
In this case we describe the use of a novel, contiguous fillet flap utilizing the entire leg soft tissue envelope to cover a massive traumatic defect of the pelvis and back. A similar fillet method has been described, 13 but we used a technique that preserved the venous outflow and lymphatic drainage of the distal end of the flap. This effectively minimized the flap oedema that has compromised previous attempts at this type of reconstruction.
Case Presentation
A 32-year-old man was involved in a high-speed motorcycle crash when he lost control at 120 km/h and was thrown off his vehicle, striking a bus shelter. He sustained multiple injuries, most notably a complete C7 ASIA (American Spinal Injury Association) A spinal cord traction injury, an open complex acetabular fracture, and a massive degloving wound to his lower back with extensive tissue loss (Figure 1). He had massive exsanguination from his back wound, followed by a traumatic cardiac arrest in the field, and was resuscitated with CPR before being transferred to Vancouver General Hospital. His retroperitoneal hemorrhage was emergently controlled surgically, and he was transfused more than 50 units of packed red blood cells. Soft tissue coverage of his open acetabular fracture and massive back wound was not possible initially; therefore, it was packed, and he was transferred to the intensive care unit for resuscitation. Over the next several days, due to his precarious respiratory status, he would not tolerate being in a lateral or prone position for an extended reconstructive operation, so definitive treatment of his wound was temporized by performing multiple bedside debridements, dressing changes, and blood transfusions. Bony exposure and osteomyelitic destruction of the left hemi-pelvis and acetabulum were evident, and the necrotizing nature of this infection led to his ongoing sepsis and deteriorating medical condition. It became clear that the necrotizing back wound was the primary threat to the patient’s life and only after the definitive coverage was obtained would his medical status stabilize.
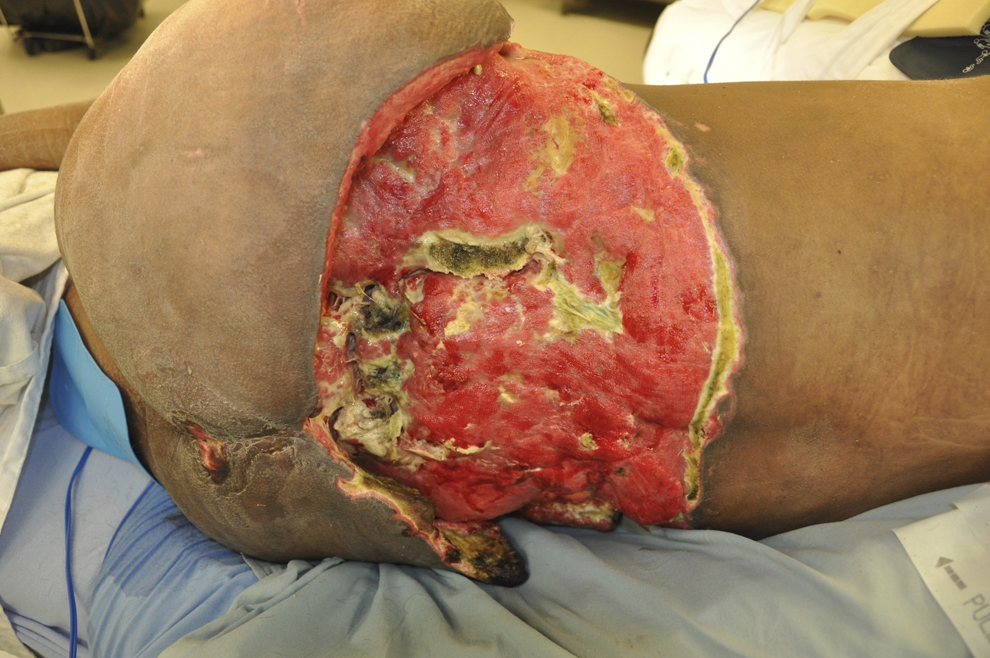
The large necrotizing back wound exposing the posterior pelvis and left acetabulum fracture.
The orthopaedic reconstructive and plastic surgery teams proposed the use of an amputation through the sacroiliac (SI) joint on the affected side that would generate an adequate soft tissue envelope in order to cover the wound. This leg was able to be sacrificed due to his high cervical spinal cord injury, and as the complexity of the pelvic and acetabular fractures rendered the limb essentially unreconstructable regardless. The one-stage contiguous fillet flap would be rotated on the external iliac vessels to cover the wound. To minimize the previously described complications of flap oedema and venous congestion, we planned to preserve the vessels and lymphatics around the popliteal fossa by keeping the contents of the popliteal fossa and the skin bridge in continuity.
Operative Technique
The tibia was mobilized proximally by releasing the gastro-soleus complex and identifying the neurovascular structures posteriorly (Figure 2). The anterior tibial artery was maintained in continuity by dividing the fibula as is standard in oncology procedures. We then dissected out the rest of the tibia subperiosteally and divided it at the ankle to remove it. The fibula was removed subperiosteally, and then the flap was divided distally circumferentially just above the ankle and the foot removed. This left the lower leg portion of the flap perfused on the 3 perforating vessels with intact lymphatics and venous drainage (Figure 3).
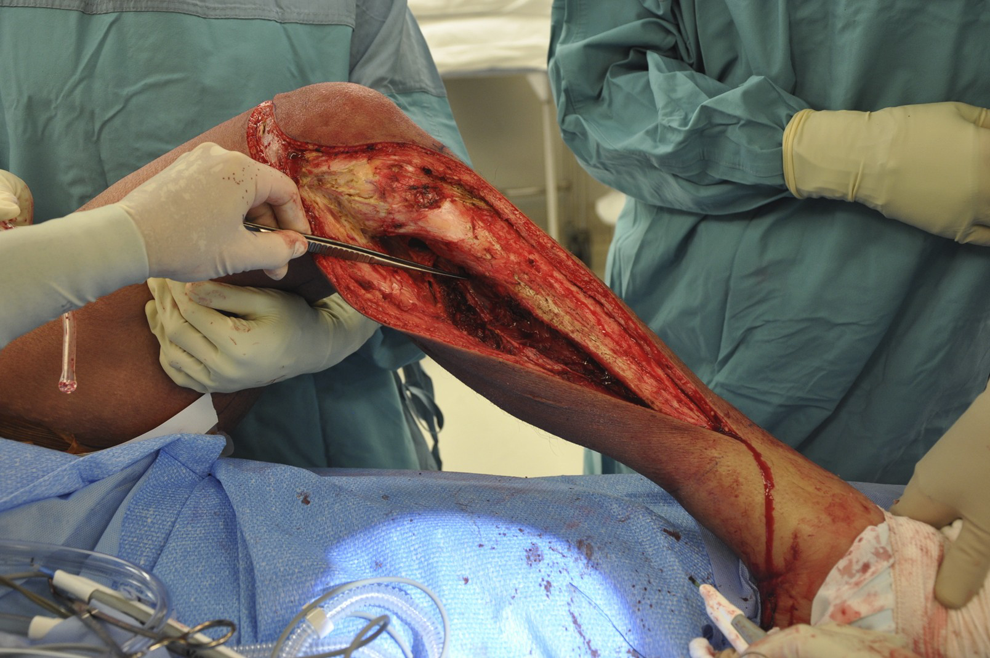
Mobilizing the neurovascular bundle of the proximal tibia prior to fibula excision.
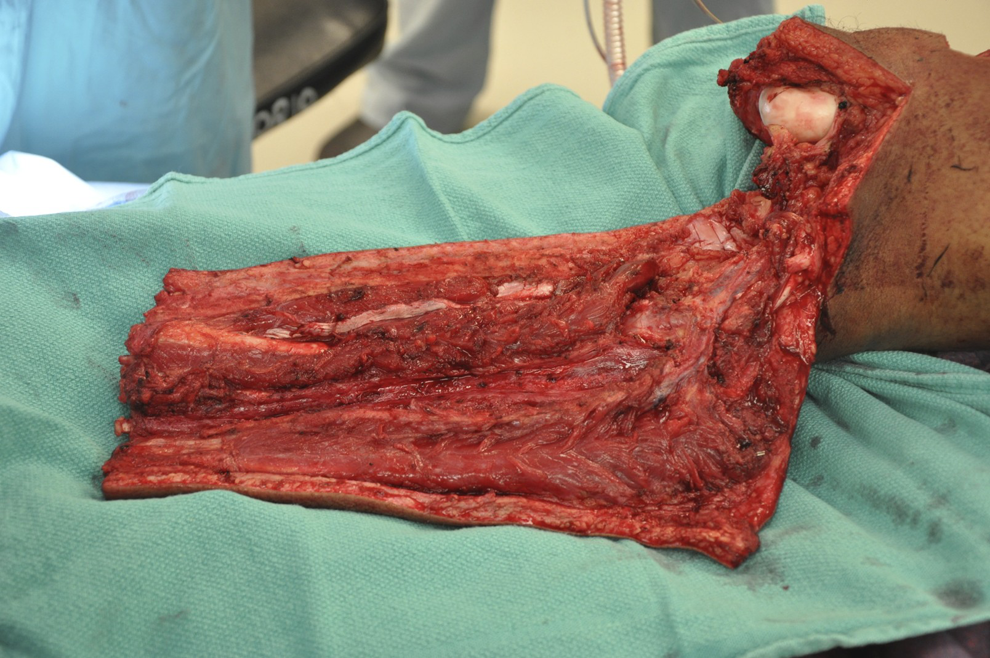
The lower leg fillet flap demonstrating the large skin bridge and preserved lymphatics of the popliteal fossa.
Dissection was then carried across the popliteal fossa, dropping the vascular, lymphatic, and neurological structures posteriorly off the back of the knee as a single unit with the skin bridge. Care was taken with the dissection through the popliteal fossa to maintain as much tissue as possible around the skin bridge and vessels, to avoid disturbing the lymphatic vessels.
This flap was then continued proximally as an anterior thigh flap with the quadriceps and anterior thigh skin all way up to the pelvic brim, dividing the profunda femoris artery. Mobilizing into the pelvis, we dissected the external iliac vessels to the least extent possible, again endeavouring to maintain lymphatic and skin contiguity across this junction. We amputated through the pelvic fractures and SI joint and trimmed off the ischium and the posterior acetabulum in order to improve the seating of the flap.
The flap was large, very well vascularized, and adequate to cover the defect (Figure 4).The wound was excised along its entire margin, and all necrotic tissue was debrided with a curette down to a bleeding base. The flap was trimmed to completely cover the defect of approximately 80 cm × 70 cm, and was inset and sutured into the wound (Figure 5).
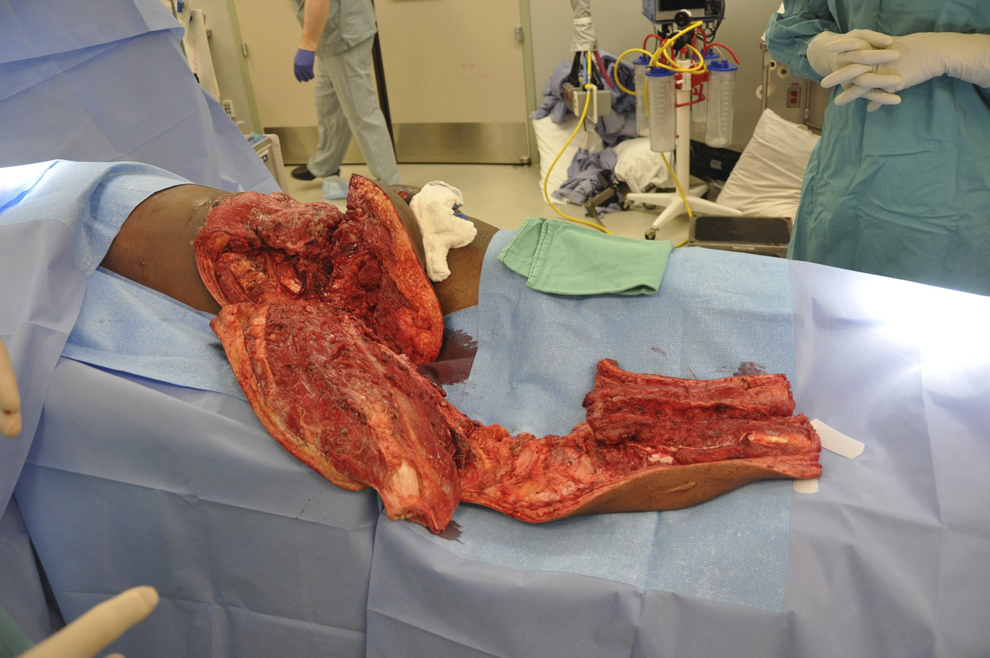
The entire leg fillet flap with the femur, tibia, fibula, and part of the left hemipelvis excised prior to insetting in the wound.
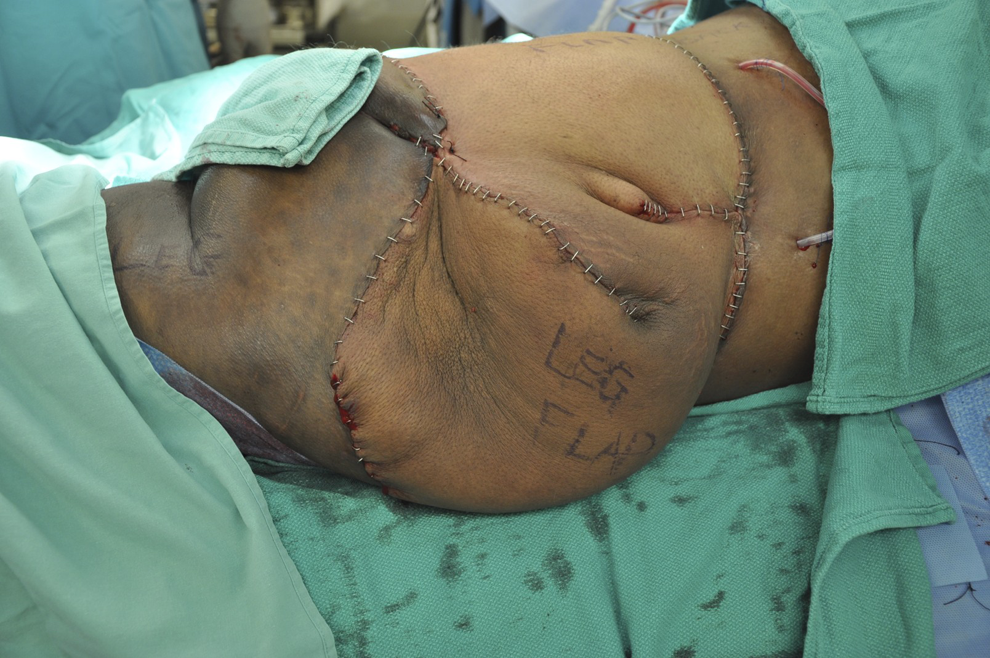
The flap has been inset into the wound with excess tissue trimmed.
Discussion
To our knowledge, the use of an entire leg contiguous pedicled fillet flap has not been used for coverage of a traumatic necrotizing wound. The use of a 2-component pedicled upper and lower leg fillet flap was previously reported for use in reconstruction of an extensive hemipelvectomy defect in a patient with a tumour 13 and for the coverage of large decubitus ulcers. 14 Only the popliteal vessels connected the upper and lower components in this report, and lymphedema was present in the lower leg component for the first 4 weeks post-operatively.
In this patient, the skin bridge and lymphatics around the knee were preserved in the reconstruction. This novel method was used for several reasons. Firstly, the size of the defect would have required the use of 2 or more free flaps involving a significant amount of donor site morbidity if the traditional latissimus flaps had been used. Secondly, we wished to minimize the post-operative swelling and lymphedema normally associated with large flaps by preserving the lymphatics of the distal flap. Thirdly, the leg had already been defunctioned by the large traumatic open acetabular fracture in addition to the patient’s high cervical spinal cord injury, so this tissue could be harvested without compromising the patient’s independence or mobility.
This report showcases that soft tissue reconstruction options exist even when injuries may initially appear non-reconstructable. On 24-month follow-up, the patient continues to do well clinically. He has been discharged home from a rehabilitation facility, is mobile in a motorized wheelchair, his flap has healed well, and he enjoys a reasonable quality of life. He expresses gratitude that his life was able to be saved.
Summary
There are many challenges when addressing large, life-threatening traumatic soft tissue defects. The specific combination of events in this patient with a large open acetabular fracture with an associated necrotizing back wound and the defunctioning of lower extremities from a high cervical spine injury led to the advent of using a large contiguous flap harvested from the affected leg. We addressed the problem of the large soft tissue defect with the contiguous leg flap and minimized lymphedema by preserving lymphatics and a skin bridge across the popliteal fossa. We feel his survival from such devastating injuries can serve as a reminder that this type of large soft tissue reconstruction option is available when the need arises.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
