Abstract
The purpose of this report was to present the results of coverage of giant sacral sores with a gastrocnemius myocutaneous flap pedicled with femoral vessels after thigh amputation. Between June 1989 and April 2010, 10 patients with paraplegia having giant sacral pressure sores underwent early aggressive surgical debridement followed by surgical reconstruction with a gastrocnemius myocutaneous flap pedicled with femoral vessels after thigh amputation. The spinal cord injury was secondary to trauma in 8 patients and non-traumatic in 2 patients. The wounds measured between 8 cm × 26 cm and 26 cm × 30 cm. The post-operative course was uneventful in 8 patients. Partial flap necrosis occurred in 2 patients who were treated with skin grafts. The follow-up period ranged from 12 to 96 months. There was no recurrence of the sore in any patient. This technique may be a treatment option for the repair of huge sacral bedsores in the absence of other reliable methods for patients with paraplegia.
Introduction
Sacral pressure ulcers are very common in patients with paraplegia. 1,2 Giant sacral pressure ulcers are easily complicated by infections and sepsis, which result in proteinuria and subsequently systemic malnutrition. 3 Multiple techniques have been described to repair these ulcers, including reconstruction with rotation flaps, island musculocutaneous flaps, V-Y advancement flaps, gluteal thigh flaps, perforator flaps, and free flaps. 4 –13 However, despite successful flap closure, recurrence of the ulcer is common, especially in patients with paraplegia who are dependent on wheelchairs for mobility. 14 –16 Management of patients with large recurrent sacral pressure ulcerations can be complicated by the unavailability of local flaps, either because they have already been used or because the presence of adjacent lesions makes such flaps insufficient for complete coverage. In such cases, limb amputation with flap closure may be considered.
In this article, we present the results of the repair of giant recurrent sacral pressure sores in 10 patients using gastrocnemius myocutaneous flaps pedicled with femoral vessels after thigh amputation.
Patients and Methods
Ten patients (7 males and 3 females) received surgery over a period of 21 years (June 1989 to April 2010). The mean age of the group was 44.6 years (range: 34-60 years). All the patients had spinal cord injury (SCI): 3 patients were tetraplegic and 7 were paraplegic. In 8 patients, the SCI was secondary to trauma, and in 2 patients, it was non-traumatic (transverse myelitis). The duration of the ulcers ranged between 3 and 15 years. All patients had stage IV sacral pressure sores that extended to the bone. The sizes of the wound ranged from 8 cm × 26 cm to 26 cm ×30 cm. All ulcers were recurrent, and 6 patients had associated pressure ulcers. Limb-sparing procedures were difficult. The patient data are summarized in Table 1.
Patient Characteristics.
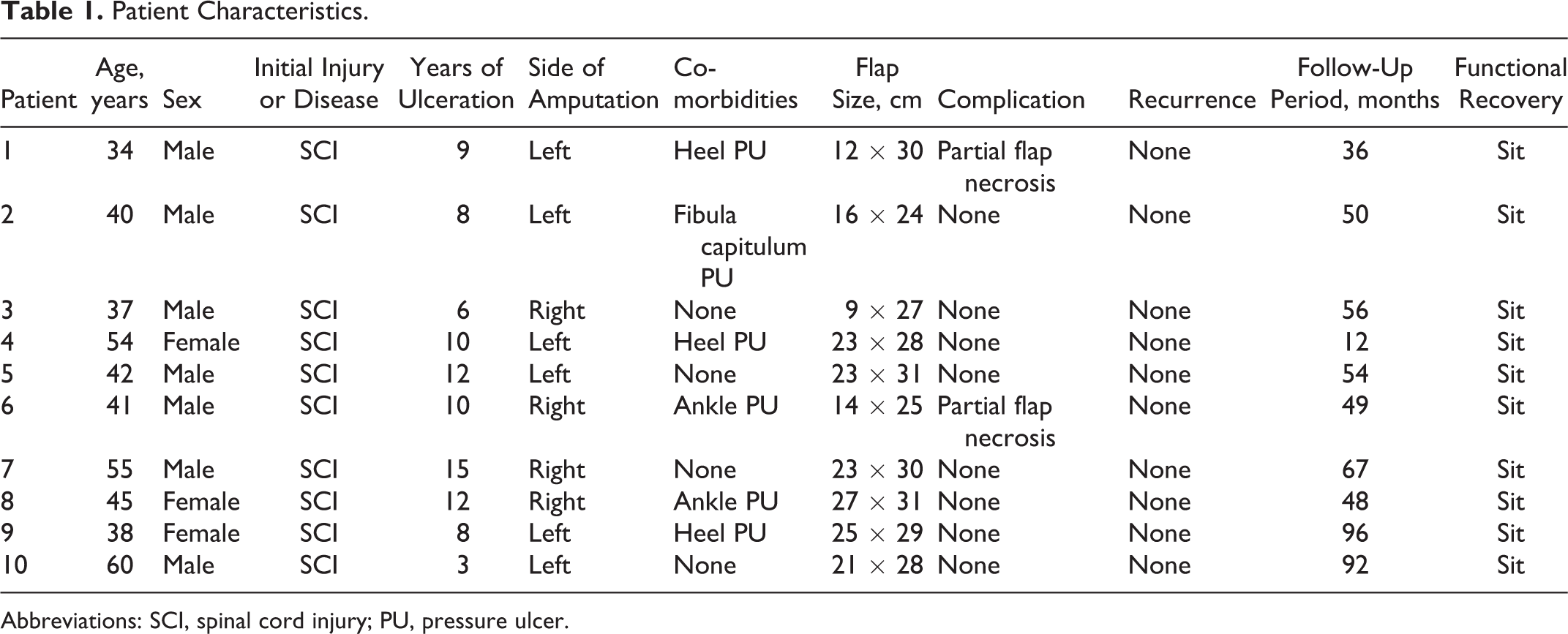
Abbreviations: SCI, spinal cord injury; PU, pressure ulcer.
The patients were cachectic and anemic; moreover, they had malnutrition and a water–electrolyte imbalance. Whole blood, plasma, and human serum albumin were administered as required to ensure that the preoperative levels of hemoglobin were greater than 90 g/L and the preoperative level of plasma protein was greater than 50 g/L. Moreover, any fluid–electrolyte imbalance was corrected. We performed debridement and dressing changes preoperatively and prepared bacterial cultures from the wounds to ensure antibiotic sensitivity. We also performed electrocardiography, liver and renal function tests, and blood coagulation profiles preoperatively to ensure comprehensive patient assessment. Ethics approval for thigh amputation was granted by our institution. The procedure was discussed with both the patient and their family before surgery, and each patient accepted it. Informed consent was obtained from all patients prior to surgery.
Surgical Technique
The patients were placed prone on the operating table under general anaesthesia. Methyl blue was used to indicate the point at which the sacral pressure sore was to be resected. A vertical line was drawn along the middle of the back of the thigh, extending to the popliteal fossa; the line then curved forward to both sides and connected at the distal patellar edge. A second line was drawn from the anterior tibia downward to the ankle, and a ring was then drawn around the ankle joint.
The wound was washed intraoperatively with hydrogen peroxide and bromogeramine and any necrotic tissue was debrided as completely as possible. Any bone tissue in the wound (such as the apophysis of the sacrococcyx) was removed in small segments if it was found to be infected or if there was a chance that it would interfere with coverage by the flap. The incision was made along the described line, into the cutis, subcutis, and fascia. According to the flap design, a longitudinal incision was made at the anterior crura, and 2 circular incisions were made at the knee and ankle joint (Figure 1). The flap was freed under the deep fascia at the anterior tibia. The great saphenous vein was cut off in the proximal region of the flap, and the small saphenous vein was protected. When the flap was freed at the medial margin of the tibia, the medial head of the gastrocnemius muscle was cut at the point where it was attached to the tibia. The gastrocnemius and soleus muscles could be separated easily with the fingers. The gastrocnemius muscle, together with the skin, was freed from the inside out; the lateral head of the gastrocnemius muscle was cut from the fibula and then freed along its length under the deep fascia until a fairly large gastrocnemius myocutaneous flap including the front leg skin was obtained. The 2 ends of the gastrocnemius muscle attachment point were cut at the supracondylar femur. Nutrient vessels of the gastrocnemius muscle and the small saphenous vein were distinguished. The popliteal artery was cut at the point after which it branched into the sural artery, and it was ligated with the popliteal vein at the point of entry of the small saphenous vein. A pedicled gastrocnemius myocutaneous flap was created (Figure 2). An incision was made at the back of the thigh, and the proximal femoral vessel was freed until the vascular pedicle was long enough for the myocutaneous flap transfer. The vascular pedicle consisted of the sural vessels and the popliteal and femoral artery and vein. The lower extremity was amputated at the distal thigh. The gastrocnemius myocutaneous flap was transferred to cover the sacral wound through the femoral incision (Figure 3). The distal end of the muscle was sutured to the base of the defect with 3-0 Vicryl, and the skin island was sutured to the defect margins with 4-0 Prolene. The stump was closed primarily over a silicone drain that was removed between post-operative days 3 and 7.
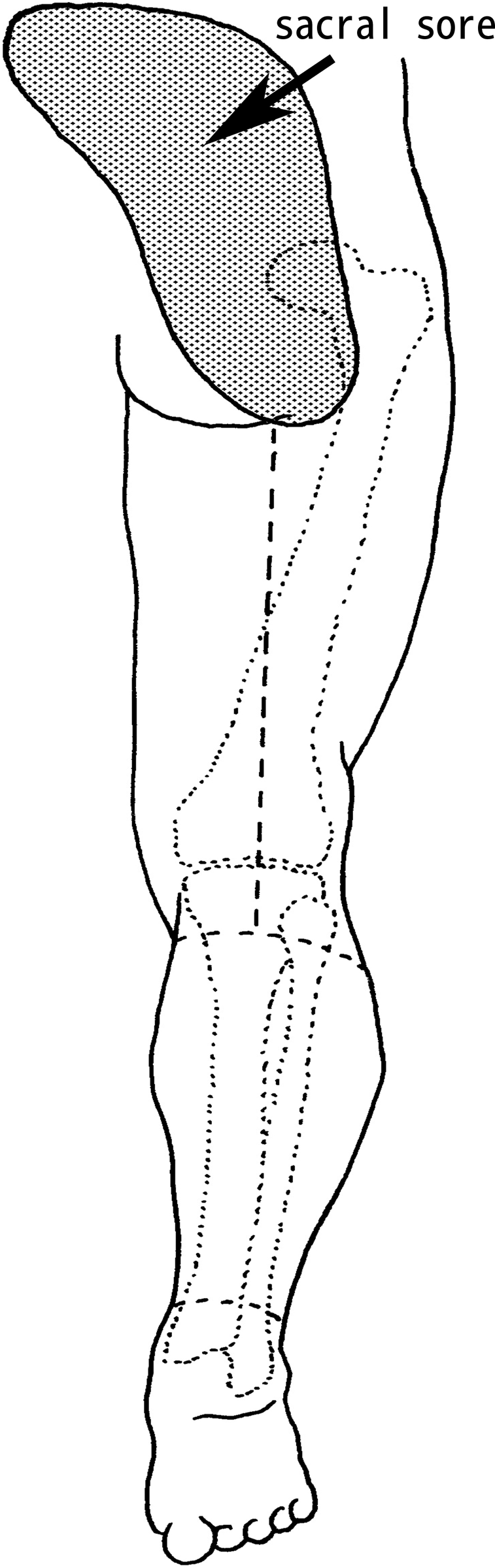
Demarcation for making the incision.
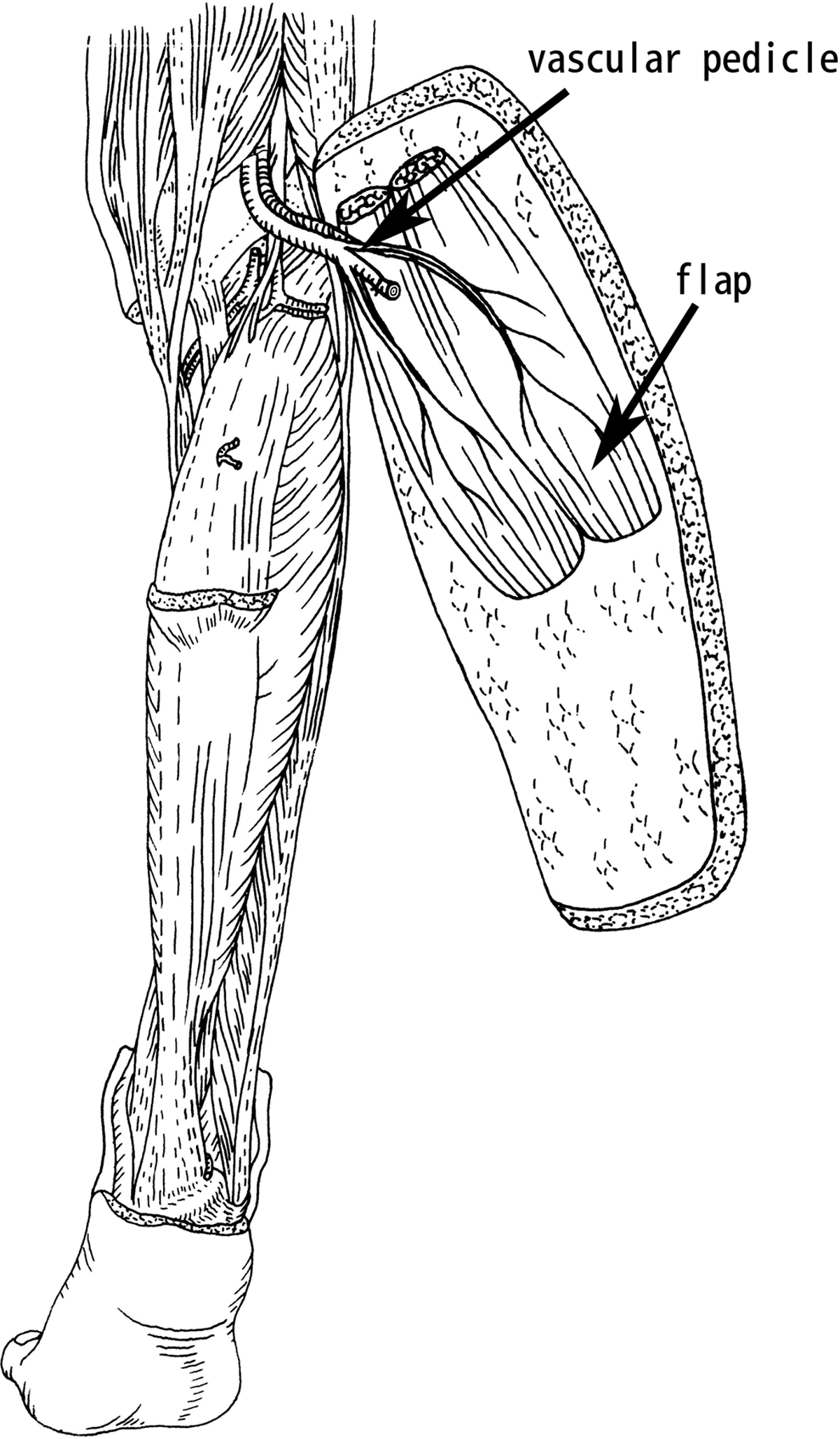
Raising of the gastrocnemius myocutaneous flap.
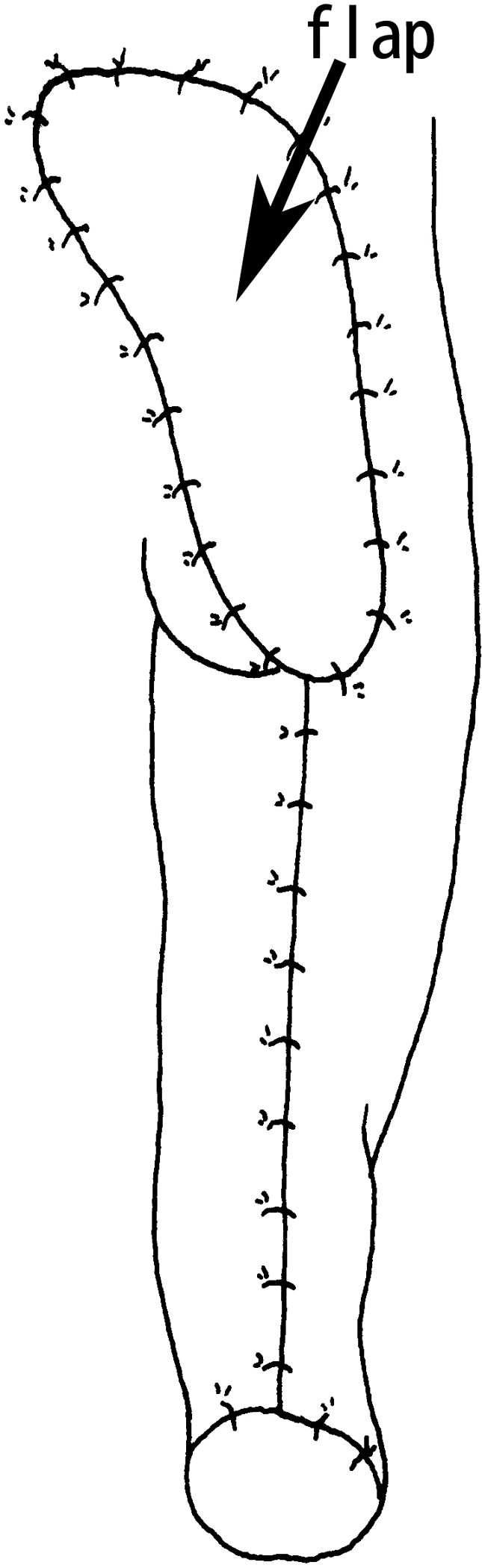
Covering the sacral bedsore with the flap.
Antibiotic and anticoagulant treatment and fluid replacement therapy were given after the operation, and the sutures were removed 14 days after the operation. The patient recuperated in the prone until the flap healed. Patients were allowed to sit but were kept off the operative site for 3 to 4 weeks after surgery.
Results
In all the cases, the patients underwent single-stage surgical reconstruction and good coverage of the defects was achieved. The area of the flap ranged from 9 cm × 27 cm to 27 cm × 31 cm. The post-operative course was uneventful in 8 patients. Partial flap necrosis (largest area approximately 2 cm × 2 cm) occurred in 2 patients who were subsequently treated with skin grafts. The patients underwent regular outpatient clinical follow-ups. The average follow-up period was 56 months (range, 12-96 months). No recurrent sacral pressure sores were noted in any patient (Table 1), and there were no complications at the amputation site in any patients. All patients were able to sit and independently perform their daily activities.
Case Report
A sacral pressure sore developed in a 54-year-old woman who had a L1–L2 SCI accompanied by paraplegia after being crushed by a crane 10 years ago. Over the course of the past 10 years, she had undergone 6 operations for her recurrent left sacral pressure sore. She had a stage IV sacral pressure sore that extended to the bone, at which point she was referred to our care. The sore measured 22 cm × 27 cm. All local possibilities had been exhausted. The patient chose an aggressive surgical debridement followed by a flap-based surgical reconstruction. After the debridement of necrotic tissue in the sacral region, the skin and soft tissue defects were reconstructed with a gastrocnemius myocutaneous flap pedicled with femoral vessels after the left thigh amputation. The area of the flap was 23 cm × 28 cm (Figures 4 –9). The flap survived and her post-operative course was uneventful, with no complications at either the recipient or amputation sites. At the 12-month follow-up, the pressure sores had not recurred.
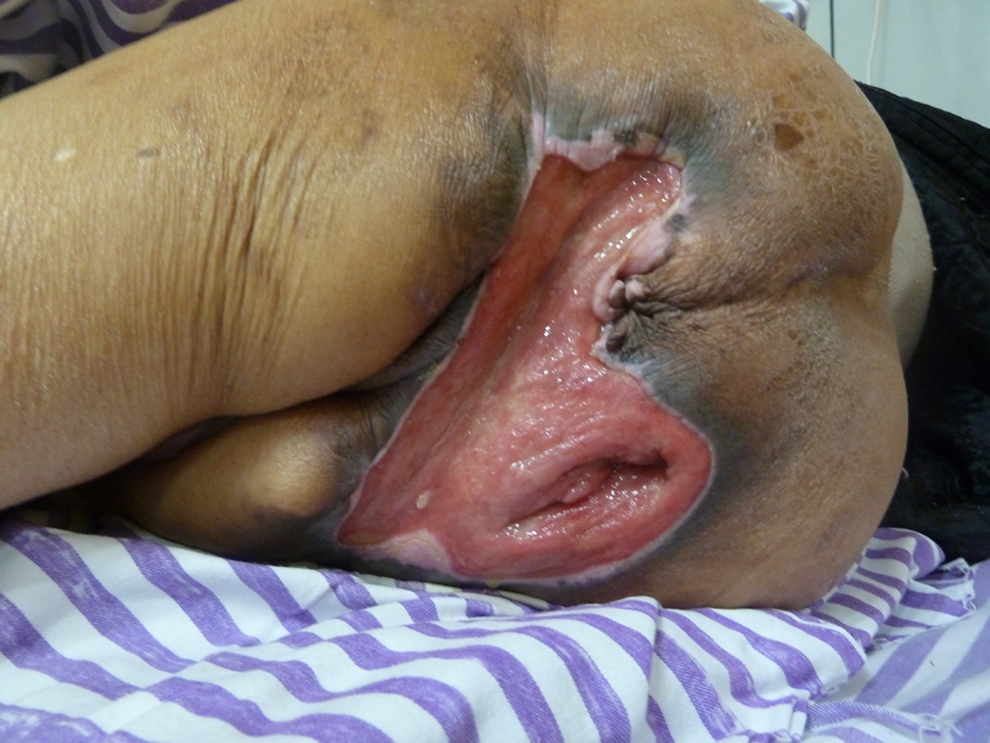
Preoperative appearance of patient 4.
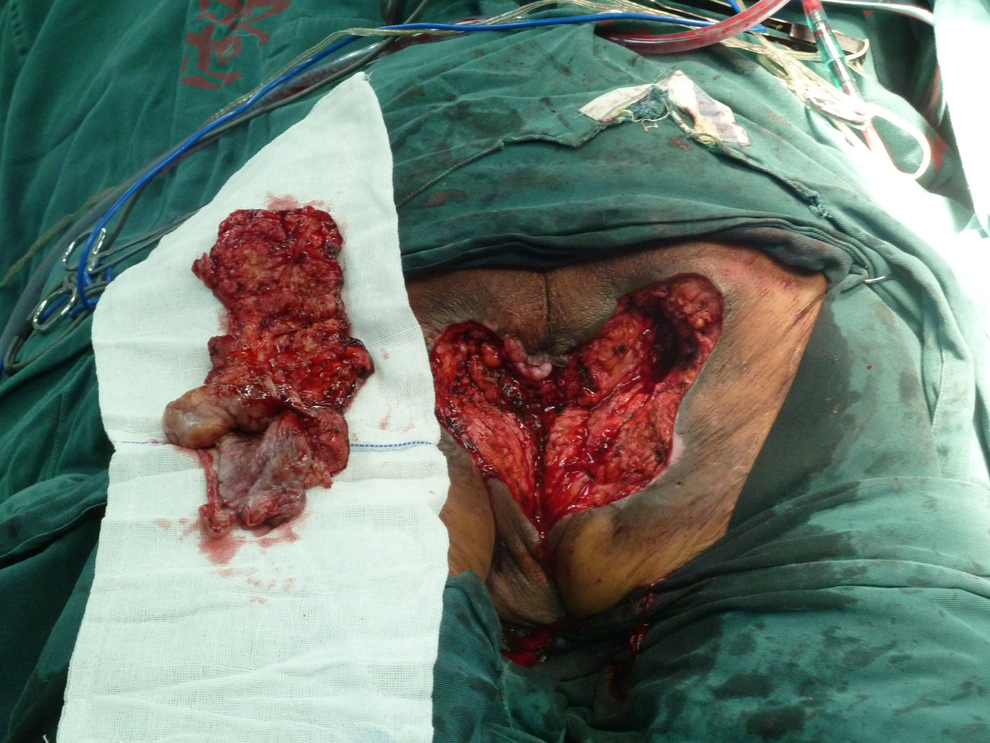
Complete excision of the bursa.
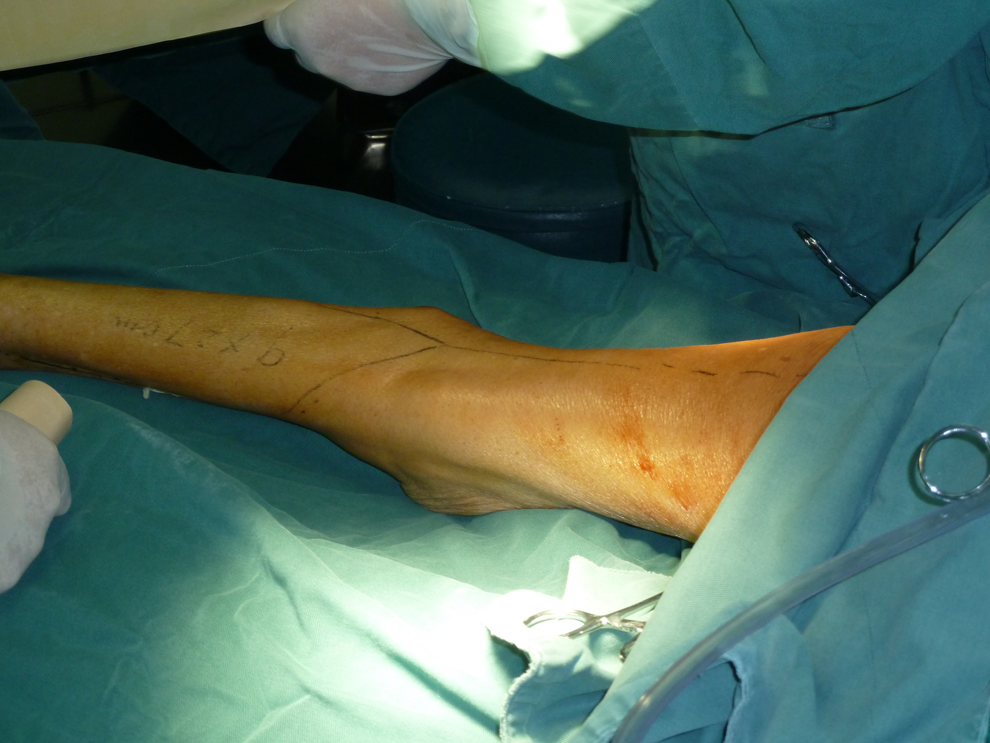
Flap design.
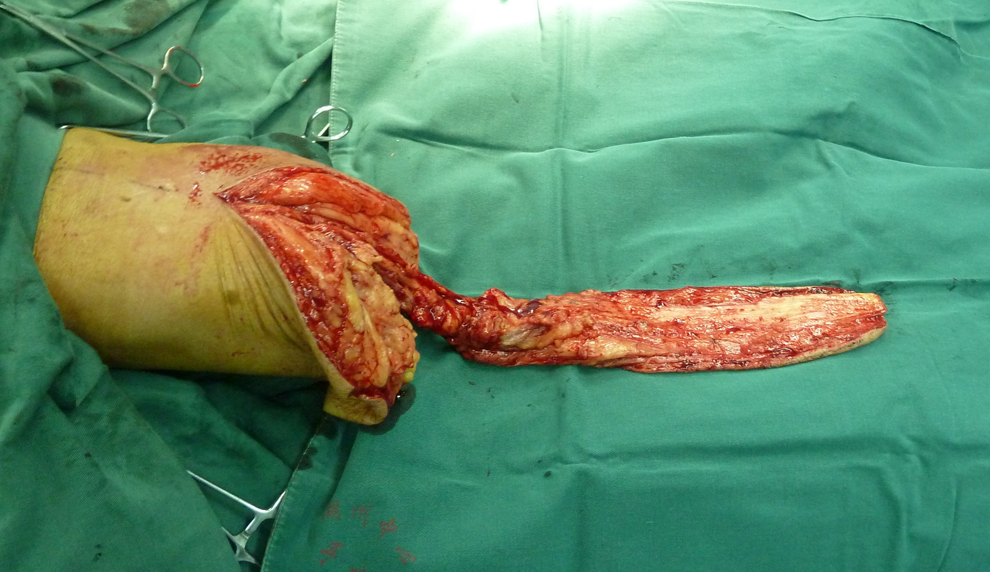
Raising of the gastrocnemius myocutaneous flap pedicled with the femoral vessel.
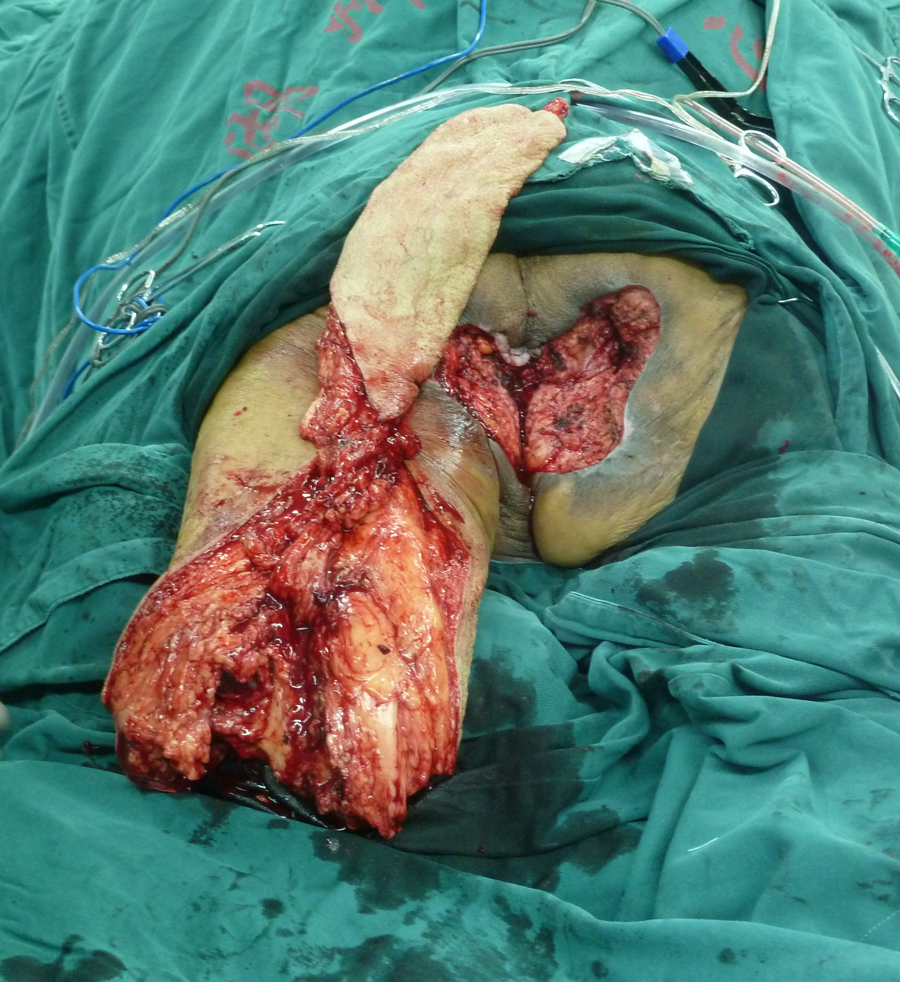
Transfer of the gastrocnemius musculocutaneous flap to the sacral wound through the femoral incision.
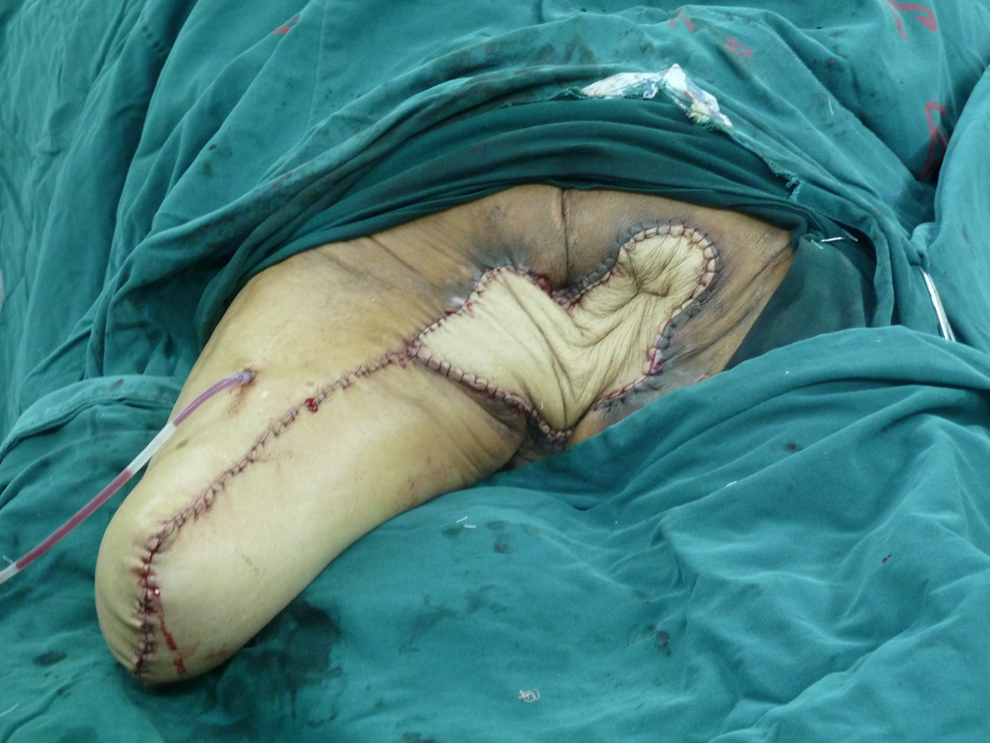
The sacral bedsore was successfully covered by the flap.
Discussion
The use of salvage flaps from amputated limbs is not a new concept. 17 –19 The amputated limb provides the surgeon with plenty of well-vascularized soft tissue that can be utilized effectively to reconstruct proximal pressure sores. Total thigh flap reconstruction is a formidable procedure that requires filleting the entire soft tissue of the thigh. 20 A variation of this is the island leg flap, in which the entire lower limb tissue can be raised as a flap supplied by the femoral vessels. 21 Hallock 22 described the use of a free gastrocnemius myocutaneous flap with a long venous pedicle to cover an ischial pressure sore in a patient with intact lower limbs; however, the flap size is limited with this procedure. Kierney 23 reconstructed recalcitrant pressure sores with hip disarticulation and inferiorly based rectus abdominis myocutaneous flaps; however, preservation of the ability to sit after rectus muscle transposition in patients with paraplegia has been questioned. 24 It is implicit that a significant number of patients with SCI show impairment in their ability to sit upright. 25 Sitting is an important function as it simplifies the performance of daily activities and improves social engagement. Therefore, preservation of this ability after flap reconstruction is an important point to be considered when planning the surgery.
In this study, we used a long pedicled gastrocnemius myocutaneous flap to repair giant sacral pressure sores in patients who underwent thigh amputation. The vascular pedicle consisted of the sural vessels and the popliteal and femoral artery and vein. With the upper thigh and hip joint conserved, the ability of the patients with paraplegia to sit and maintain their balance in a wheelchair and their daily life activities were not significantly impaired.
The 10 patients included in this study had sacral bedsore sores with extensive destruction to the muscle, bone, and supporting structures (grade IV), which was difficult to reconstruct. All these patients had recurrent sacral pressure sores, and all of them had undergone more than one flap reconstruction for the sacral defect. There were no reliable locoregional flaps that could be elevated from the buttocks or lower extremities. All recognized limb-sparing flap options had been previously used, had been disrupted during the design of other flaps, or were precluded because of a paucity of local soft tissue. We successfully repaired giant sacral pressure sores in these patients using gastrocnemius myocutaneous flaps pedicled with femoral vessels via thigh amputation. No recurrence was reported in any of the patients. All the patients were able to sit and perform their daily activities, indicating that the use of gastrocnemius myocutaneous flaps pedicled with femoral vessels is effective to repair huge sacral bedsores.
Although the surgical method used in this study is destructive, which may not be acceptable to either patients or surgeons, it has several advantages. First, the flap is large enough to cover giant sacral bedsores. Second, the vascular pedicle of the flap comprises femoral vessels, which are large and rich in blood supply and therefore improve the chances of flap survival. Thus, it could be used as a good alternative for reconstructing large sacral defects in cases where there are no other treatment options. Our findings indicate that this method is particularly applicable to patients with paraplegia having giant sacral bedsores, especially those with associated pressure ulcers in areas such as the heel, ankle, and fibula capitulum.
In addition to the destructiveness of the procedure, another limitation is that the scope of its applicability is relatively small. Moreover, apart from loss of the lower limb, if the operation fails, it is difficult to use other methods as a remedy. Therefore, the repercussions may be far worse than those of other myocutaneous flap transfers, and the indications for the operation should be carefully examined before performing it.
In conclusion, this technique should only be used for patients with SCI who have giant recurrent sacral pressure sores, especially in cases where there are no suitable flaps available to repair recurrent bedsores.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
