Abstract
Alar base resection is an essential part of rhinoplasty which is frequently utilized to narrow a wide nasal base or to correct excessive flaring of the lateral ala extending beyond the alar-facial groove. Multiple surgical techniques have been described in the literature including alar wedge excision, sill reduction, a combination of wedge and sill reduction, repositioning the alar insertion with a V-Y advancement flap, alar flap advancement, and multiple suturing techniques. The authors of this article propose a technique that can be used to correct excessive alar or sill reduction if encountered intraoperatively.
Introduction
Alar base resection is an essential part of rhinoplasty which is frequently utilized to narrow a wide nasal base or to correct excessive flaring of the lateral ala extending beyond the alar-facial groove. 1 Multiple surgical techniques have been described to narrow a wide nasal base, including alar wedge excision, sill reduction, 2 a combination of wedge and sill reduction, 2,3 repositioning the alar insertion with a V-Y advancement flap, 4 alar flap advancement, 5 and multiple suturing techniques. 6 Of these, alar wedge excision is currently the most frequently used, and multiple modifications have been described in the literature. 7,8
During rhinoplasty surgery, the decision for alar base reduction is usually taken toward the end of the procedure as tip de-projection and de-rotation may exacerbate alar flaring. A wedge incision is marked over the lateral alar border bilaterally (Figure 1). A caliper might be used to ensure symmetry of both sides. Small amount of local anaesthetic with epinephrine is first used to infiltrate the alar-facial groove, about 0.5 cm3 in each side, and excision of the wedge is then done using a number 15 blade without entering to the nostril from the side. Electrocautery is seldom used for bleeding control. A semilunar wedge excision with a shorter and less curved medial limb compared with the lateral limb is essential to avoid over-straightening the ala and to preserve its natural curvature. Care should be exercised to bevel the incisions inward to facilitate their closure. Alar wedge excision may be combined with nasal sill excision 3 to address a wide or a horizontally oriented nasal sill (Figure 2). Although uncommon, increased alar base width may be caused by a large nasal sill with no alar flaring, and in these cases, the sill alone is directly narrowed. Moreover, displaced lateral insertion of the ala might contribute to excessive alar flaring and increased nasal base width, and this is best corrected by repositioning with V-Y advancement. 9,10

Alar wedge excision.

Combined alar and sill excision.
Materials and Methods
This is a retrospective review of 2 cases in which over-resection of lateral alar wedge excision took place and was identified and managed intraoperatively. The first case was encountered in 2007: a 17-year-old female with no comorbidities, Fitzpatrick skin type II of average thickness, underwent a rhinoplasty surgery in which excessive alar wedge resection combined with sill excision took place on the right side of the nose. The excised wedge which measured about 7 mm in width was put back in its place as a composite graft. The graft was then fixed in place using simple interrupted 6-0 Prolene suture. Reassessment led to the excision of a 4-mm-wide wedge, leaving about 3 mm of tissue medially as a composite graft. Incision was closed using 6-0 Prolene. The second case was encountered in 2014: a 23-year-old female with no comorbidities, Fitzpatrick skin type IV of average thickness, underwent rhinoplasty as well and the similar scenario was encountered, and the exact similar intraoperative management was performed, leaving a 2-mm composite graft in place (Figure 3). Postoperatively, both cases were instructed to apply topical antibiotic ointment (fusidic acid) for 2 weeks. Sutures were removed in the clinic after 1 week and patients were advised to apply sunscreen with SPF 30 for at least 6 weeks after surgery.
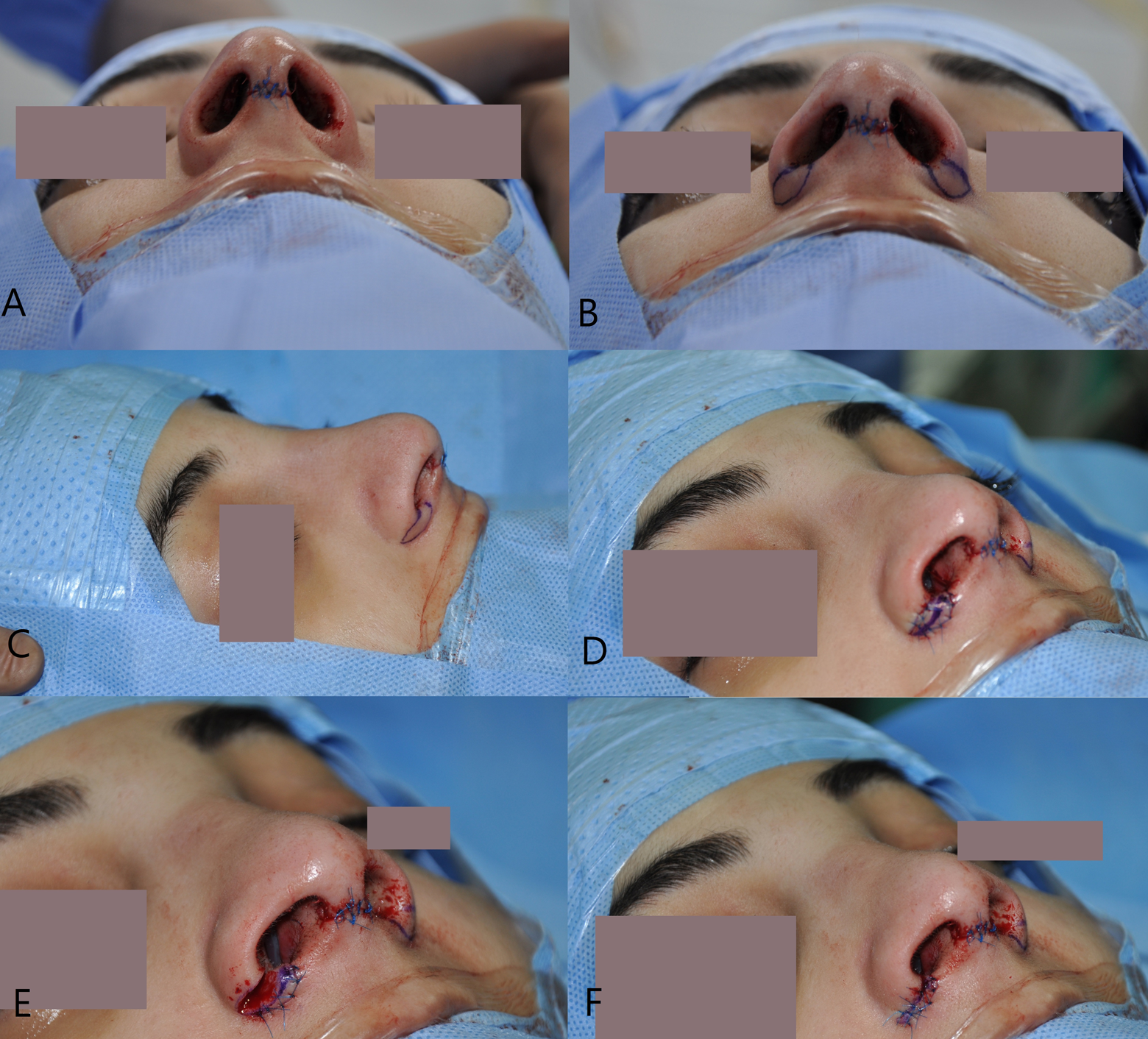
Surgical technique. A, Basal view before alar resection. B, Basal view showing the marking for a combined alar wedge and sill resection. C, Marking side view. D, The excised wedge was put back and sutured in place, remarking done. E, Re-excision of a smaller wedge, leaving 2 mm attached laterally as a composite graft. F, Final closure.
Results
Both cases were followed up for a year postoperatively. Excellent scar was achieved with no notable excessive scarring compared to uncomplicated alar wedge resection (Figure 4). Both patients were highly satisfied with results and no concerns regarding alar scar were expressed.
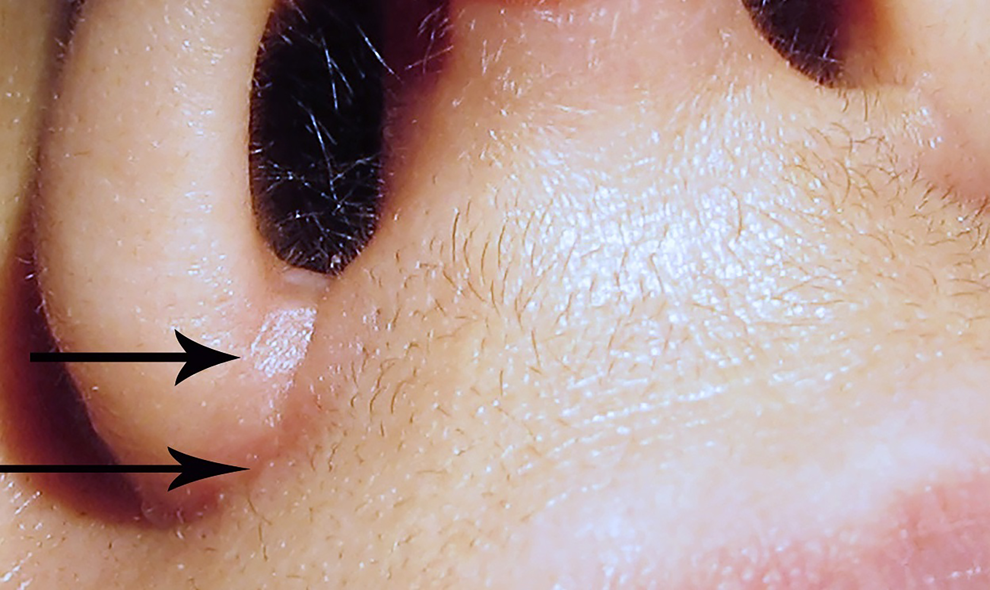
The resultant scar 12 months postoperatively. The arrows point to the 2 edges of the composite graft.
Discussion
Rhinoplasty surgery is occasionally accompanied with alar wedge resection, which is usually left to the end of the procedure. Rarely, surgeon may excise more tissue than needed, which is not usually evident until after closing the incision resulting in overly small nostrils. Careful assessment and precise measuring of the alar rim wedge to be excised should be exercised in all cases. However, even in the most experienced hands, overestimation of the wedge size to be excised may take place and is usually not recognized until the incision is closed.
We are unaware of any other intraoperative technique to overcome this issue. In both cases, patients were made aware of our concern that excessive scarring may occur. Interestingly, both composite grafts were taken completely and the resultant scars were not worse than the scars of uncomplicated cases. We would also advocate surgeons to making a habit of completing the alar resection and closing it unilaterally before moving to the other side.
Conclusion
In cases where excessive alar wedge resection is recognized intraoperatively, the excised wedge can be put back as a composite graft and a smaller wedge can be resected. Care should be taken to only excise one side at a time and reassess before moving to the other side.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
