Abstract
Introduction
Age-related macular degeneration (AMD) is a leading cause of blindness worldwide among individuals over 50 years of age. 1 In the late stages of the disease, macular neovascularization (MNV) may develop, resulting in vascular leakage, hemorrhage, and fibrotic scarring. 2 Although MNV has traditionally been characterized and diagnosed using fluorescein angiography (FA), optical coherence tomography angiography (OCTA) can provide detailed, noninvasive, 3-dimensional visualization of MNV, and clinical use is increasing. 2 Recent studies have used OCTA to characterize MNV features and morphologic changes after long-term antivascular endothelial growth factor (anti-VEGF) therapy.3,4 However, the characteristics of MNV after treatment with faricimab, a bispecific antibody inhibiting VEGF-A and angiopoietin-2 (Ang2), 5 are not well described in the literature. In addition, OCTA biomarkers suggestive of inadequate response to MNV treatment are poorly understood.
Methods
This retrospective case series evaluated 4 eyes from 3 patients with exudative neovascular age-related macular degeneration (nAMD) after aflibercept was switched to faricimab therapy due to inadequate control of exudation or limited treatment interval extension with other anti-VEGF agents. Clinical records were reviewed, including demographic data, treatment history, and ophthalmic examination findings. Multimodal retinal imaging, including structural OCT and OCTA, was analyzed to assess changes in MNV morphology and exudative activity before and after initiation of faricimab. Imaging findings were compared longitudinally across treatment visits.
Results
Case 1
A 67-year-old woman presented with several weeks of decreased vision in her left eye and was diagnosed with exudative nAMD. She was initially treated with intravitreal (IVT) ranibizumab. At the 1-month follow-up, subretinal fluid (SRF) was seen in the right eye, leading to a diagnosis of exudative nAMD. Treatment with ranibizumab was continued in both eyes. At the 5-week follow-up, persistent SRF in the right eye was noted, along with an enlarging pigment epithelial detachment (PED) in the left eye, prompting a treatment switch to aflibercept in both eyes. Despite 7 aflibercept injections administered at 4- to 5-week intervals and adjunct half-dose photodynamic therapy in both eyes, SRF persisted in the right eye (Figure 1C) and recurred in the left eye. Visual acuity (VA) gradually declined in both eyes during this period.
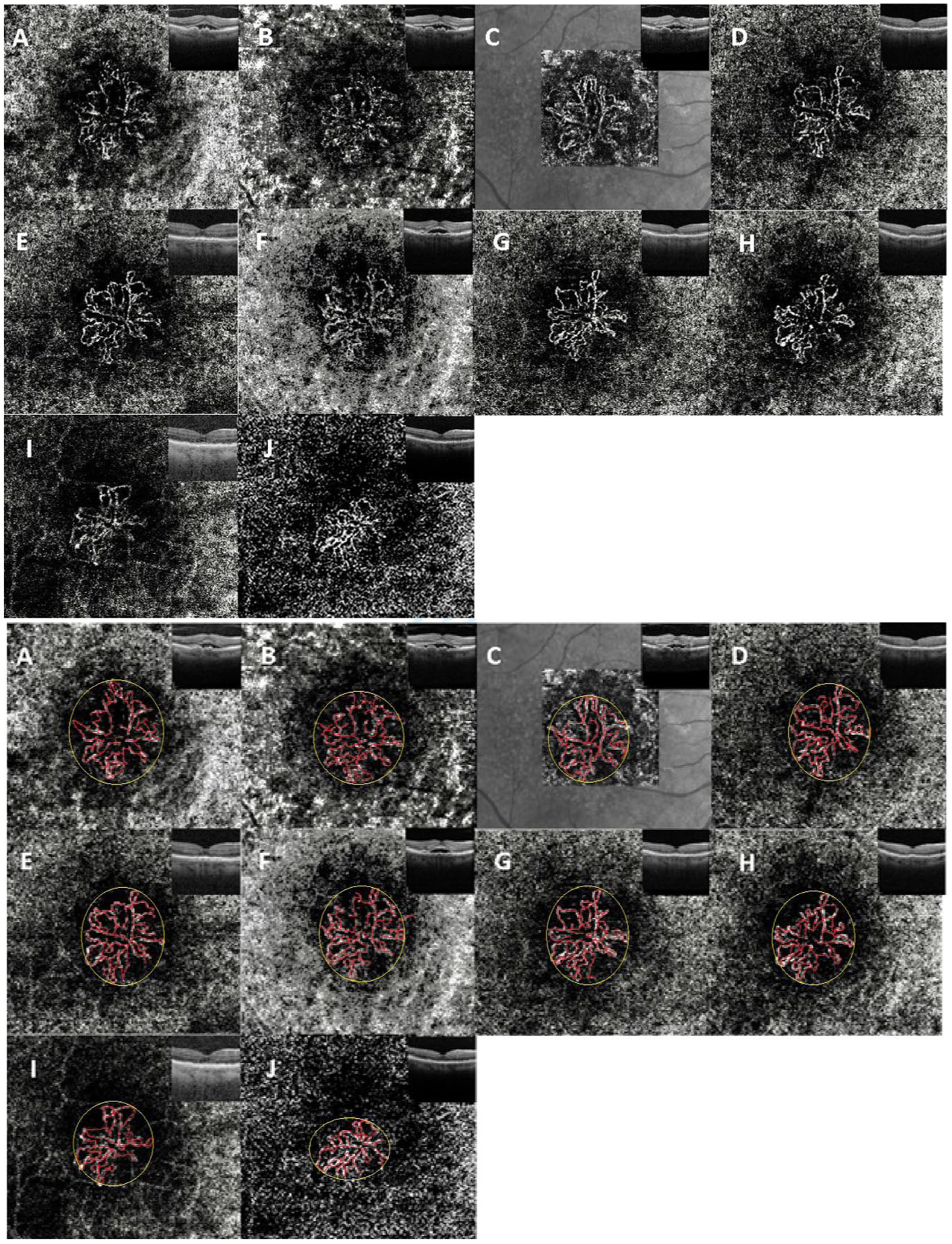
Case 1 (right eye). Top: Sequential optical coherence tomography angiography (OCTA) with corresponding structural OCT images obtained throughout the treatment course. Bottom: Sequential OCTA images with skeletonized vasculature highlighted in red and a yellow circular overlay detailing the progressive decrease in the area of macular neovascularization (MNV). (A) Two weeks after the third injection of aflibercept, OCTA shows a large MNV with prominent peripheral lacy vasculature and a surrounding dark halo. (B) OCTA at 5 weeks after the fourth injection of aflibercept and 6 weeks after half-dose photodynamic therapy shows a large MNV with increasing peripheral lacy vasculature. (C) Baseline MNV characteristics seen on OCTA immediately before the first faricimab injection (4 weeks after the seventh injection of aflibercept). (D) OCTA at 4 weeks after the first injection of faricimab shows significant reduction of lacy vasculature with persistence of the central MNV trunk and larger-caliber vessels. (E) Two weeks after switching back to aflibercept (6 weeks after the first faricimab injection), no significant changes are seen in lacy vasculature. (F) OCTA at 5 weeks after switching back to aflibercept (9 weeks after the first faricimab injection) shows recurrence of fine peripheral lacy vasculature with associated subretinal fluid recurrence. (G) Four weeks after the second faricimab injection, OCTA shows reduction of lacy vasculature with early consolidation of the MNV base. (H) OCTA at 8 weeks after the seventh faricimab injection shows further reduction of lacy vasculature with continued treatment at longer intervals. (I) Nine weeks after the 14th faricimab injection, OCTA shows sustained suppression of lacy vasculature, enlargement of central anastomotic vessels, and consolidation of the central MNV trunk. (J) OCTA obtained at the 3-year follow-up during continued faricimab therapy shows long-term MNV remodeling, characterized by sustained suppression of lacy vasculature and further consolidation of the central MNV trunk and anastomoses.
A switch from aflibercept to faricimab was subsequently made for both eyes, resulting in improvement in VA, complete SRF resolution, and near-complete resolution of the PED at the 4-week follow-up (Figures 1D and 2A). An attempt to revert to aflibercept at the 5-week follow-up led to recurrent SRF in both eyes (Figure 1F). Faricimab therapy was reinitiated, again achieving SRF resolution and improved VA in both eyes (Figures 1G and 2C), with a successful extension of treatment interval to 9 weeks by the 12th injection.
Sequential OCTA was performed throughout the treatment course (Figures 1 and 2). After treatment with faricimab, regression of fine lacy neovascular features and a decrease in MNV area were seen on OCTA, with persistence of the central vascular trunk and consolidation and peripheral anastomosis formation. Although similar short-term changes were seen on OCTA after aflibercept at 2 weeks (Figure 1D), fine lacy vasculature recurred in the right eye by the 5-week follow-up (Figure 1E) and in the left eye by the 2-week follow-up (Figure 2B). In contrast, faricimab-induced MNV morphologic changes appeared more durable and persisted at follow-up intervals of up to 9 weeks (Figure 1, H and I; Figure 2, E and F). Notably, faricimab was associated not only with prolonged regression of fine lacy vasculature but also with continued morphologic changes, characterized by greater central trunk consolidation and anastomotic maturation, despite stable structural OCT findings after exudation control (Figures 1J and 2G).
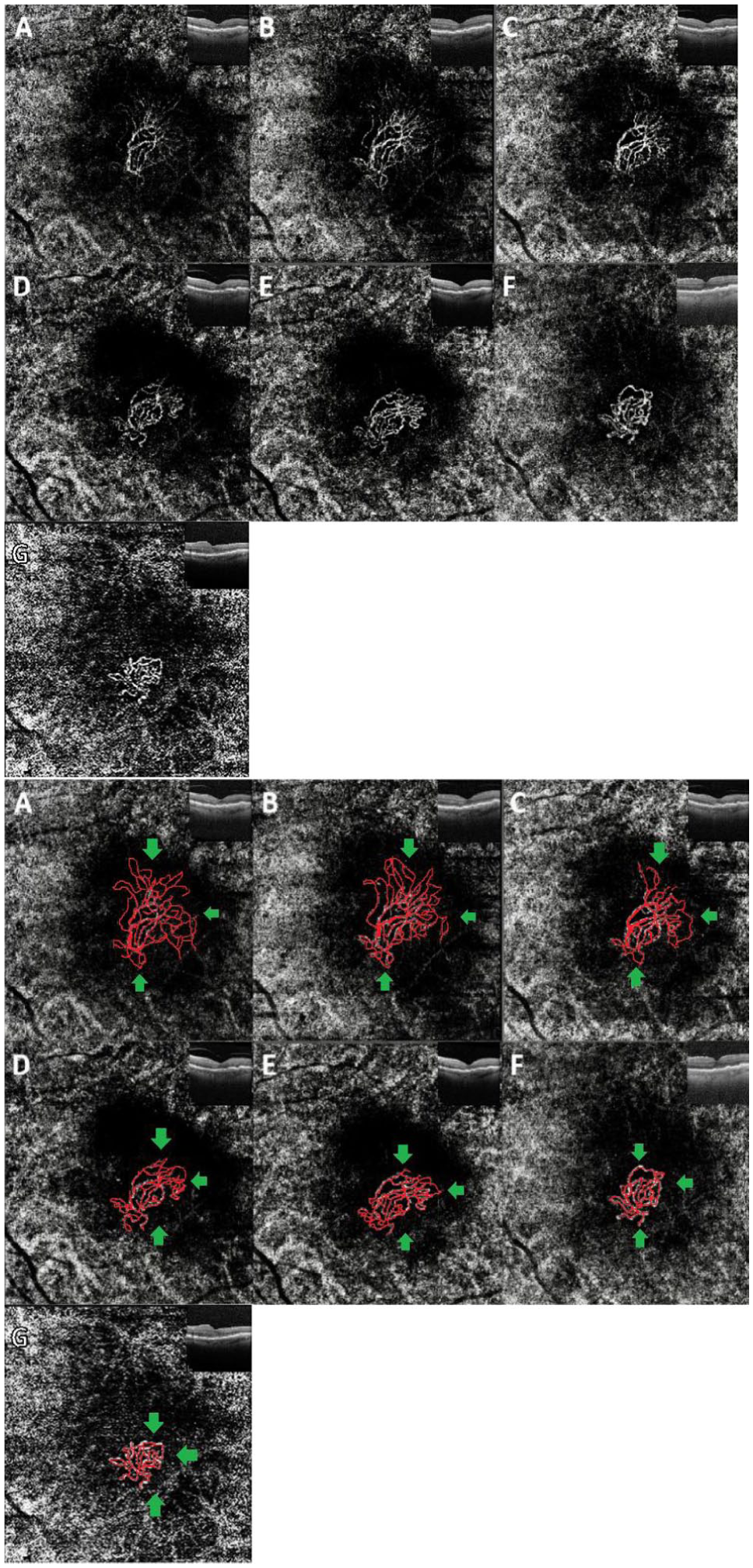
Case 1 (left eye). Top: Sequential optical coherence tomography angiography (OCTA) with corresponding structural OCT images obtained throughout the treatment course. Bottom: Sequential OCTA images with skeletonized vasculature in red and green arrows highlighting areas of peripheral lacy vasculature recurrence and regression. (A) OCTA obtained 4 weeks after the first faricimab injection shows a large macular neovascularization (MNV) with peripheral lacy vasculature. (B) OCTA at 2 weeks after switching from faricimab to aflibercept (6 weeks after the first faricimab injection) shows increased lacy vasculature with enlargement of the MNV area. (C) Four weeks after the second faricimab injection, OCTA shows decreased lacy vasculature area with persistence of the central MNV trunk. (D) Six weeks after the fifth faricimab injection, marked regression of the lacy vasculature with progressive consolidation of the MNV trunk base is seen on OCTA. (E) OCTA at 8 weeks after the seventh faricimab injection shows further reduction of peripheral lacy vasculature, formation of anastomoses between larger peripheral vessels, and continued consolidation of the MNV trunk. (F) OCTA at 9 weeks after the 14th injection of faricimab shows near-complete elimination of lacy vasculature, consolidation of peripheral anastomoses, and stabilization of a persistent MNV trunk root. (G) OCTA at the 3-year follow-up during continued faricimab therapy shows long-term MNV remodeling characterized by further consolidation of peripheral anastomoses and persistence of the central MNV trunk root. Baseline OCTA performed before initiation of faricimab therapy was uninterpretable due to poor image quality.
Case 2
An 88-year-old woman was diagnosed with exudative nAMD in the left eye and was started on IVT bevacizumab therapy. After 4 injections, extension of the treatment interval beyond 8 weeks failed due to recurrent SRF. Therapy was subsequently switched to aflibercept; however, after 4 injections, the treatment interval could not be extended beyond 10 weeks. The patient was switched to faricimab and achieved successful extension of the treatment interval to 11 weeks by the third injection. Sequential OCTA was performed throughout the treatment course (Figure 3). With long-term faricimab therapy, regression of lacy vasculature at the margins of the MNV and consolidation of a persistent central MNV trunk were seen on OCTA. MNV morphology differed on OCTA despite the absence of significant changes on structural OCT.
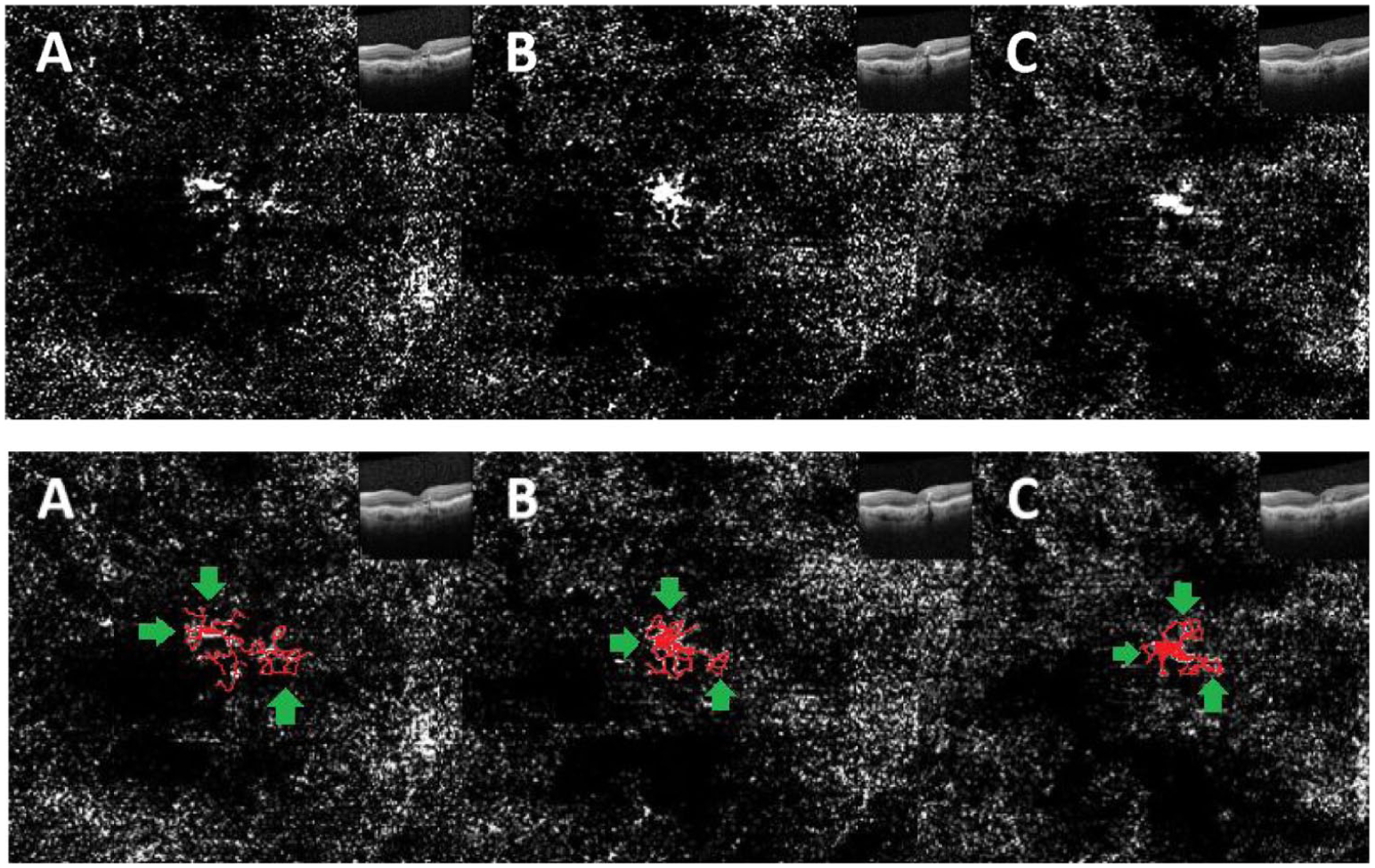
Case 2. Top: Sequential optical coherence tomography angiography (OCTA) with corresponding structural OCT images obtained throughout the treatment course. Bottom: Sequential OCTA images with vasculature skeletonization in red. Green arrows indicate areas of prominent peripheral neovascular regression. Increased density of central skeletonization delineates persistence and consolidation of the central macular neovascularization (MNV) trunk. (A) OCTA obtained 10 weeks after the third injection of aflibercept shows a focal MNV trunk with bordering lacy vasculature. (B) OCTA at 11 weeks after the fourth injection of aflibercept shows a decrease in peripheral lacy vasculature and persistence of the MNV trunk. (C) OCTA at 11 weeks after the second faricimab injection shows further reduction of lacy vasculature at the MNV border with persistence of the central MNV trunk.
Case 3
An 85-year-old woman was diagnosed with exudative nAMD of the right eye and was started on aflibercept therapy. After 3 injections, recurrent SRF resulted in a failure to extend the treatment interval beyond 6 weeks. The patient was then switched to faricimab, and by the fourth injection, the treatment interval was successfully extended to 11 weeks. Sequential OCTA was performed throughout the treatment course (Figure 4). After faricimab therapy, OCTA demonstrated a decrease in lacy vasculature surrounding the MNV, with consolidation of a persistent central MNV trunk. Regression of this vasculature persisted at the 11-week follow-up and was maintained with extension to a 4-month treatment interval. MNV morphology differed on OCTA despite the absence of significant changes on structural OCT.
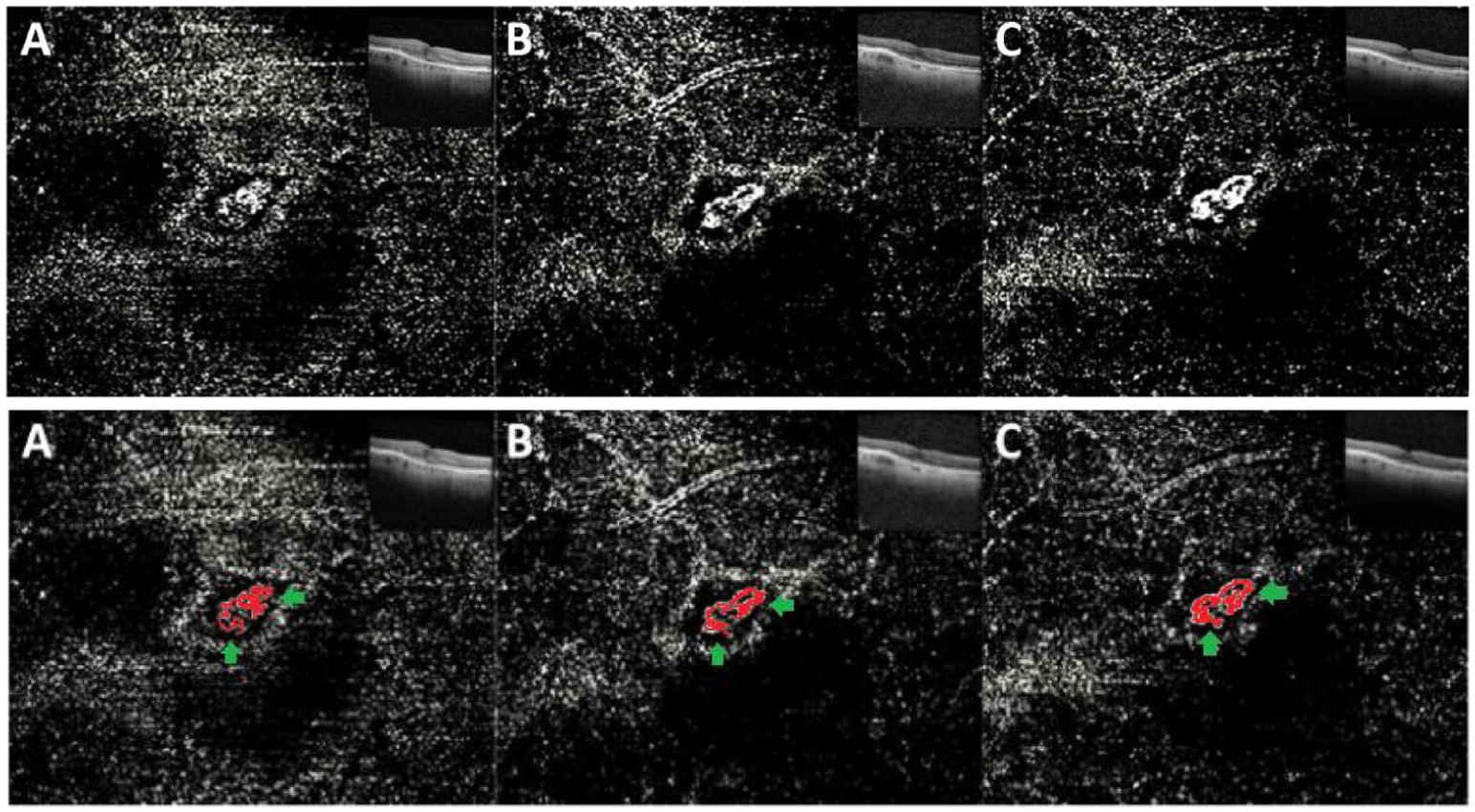
Case 3. Top: Sequential optical coherence tomography angiography (OCTA) with corresponding structural OCT images obtained throughout the treatment course. Bottom: Sequential OCTA images with skeletonized vasculature in red delineating the numerous capillary loops in the surrounding lacy vascular network and halo. Green arrows indicate areas of consolidation and regression, with an overall decrease in the number of capillary loops. Increased central skeletonization density indicates persistence and consolidation of the central macular neovascularization (MNV) trunk. (A) OCTA obtained 9 weeks after the second aflibercept injection shows an MNV trunk with a surrounding lacy vascular network and halo. (B) OCTA at 6 weeks after switching from aflibercept to faricimab shows a decrease in lacy vascular network surrounding the MNV trunk and resolution of subretinal fluid. (C) OCTA at 11 weeks after the third injection of faricimab shows a slowly consolidating MNV trunk surrounded by pruning of the lacy vasculature.
Conclusions
We report the morphologic changes in MNV observed on OCTA in 4 eyes from 3 patients with exudative nAMD who were refractory to aflibercept and subsequently treated with faricimab. In each of the eyes, faricimab was associated with a decreased area of MNV and regression of smaller fine lacy vasculature, accompanied by gradual consolidation of a central vascular trunk with anastomosis formation. Interestingly, these morphologic changes in MNV were evident on OCTA despite largely unchanged structural OCT findings and sustained absence of intraretinal fluid (IRF) or SRF. Conversely, enlargement of MNV on OCTA was associated with recurrence of IRF or SRF.
Two of the eyes that received longer-term faricimab therapy (up to 3 years) showed additional remodeling characterized by the formation of larger anastomotic vessels along the borders of the central vascular trunk, suggesting a potential cumulative effect of faricimab’s dual inhibition of VEGF-A and Ang2 compared with anti-VEGF monotherapy. Despite persistence of MNV at the final follow-up, all 4 eyes remained free of exudation, with faricimab administered at extended treatment intervals of 9 to 11 weeks. Although changes in MNV architecture were noticeable after the first faricimab injection, they became more pronounced with repeated longer-term treatment.
Although there is a paucity of literature on OCTA features of MNV in response to faricimab therapy, our findings align with those of previous studies assessing MNV remodeling after treatment with other anti-VEGF agents. Spaide reported that large-diameter central trunk vessels and anastomotic connections on OCTA are common features seen with long-term anti-VEGF therapy for MNV. It was hypothesized that anti-VEGF therapy preferentially induces regression of newly sprouting immature vessels while sparing larger, more mature vessels with sufficient pericytes. This selective pruning increases vascular resistance and blood flow in the remaining vessels, promoting arteriogenesis until levels of VEGF increase, at which point the cycle recurs with subsequent treatment. 3
The prognostic implications of residual MNV in patients with nAMD receiving ongoing treatment are not well understood. Recent studies4,6 have suggested that persistent blood flow in the setting of controlled exudation may confer a protective role against the development of geographic atrophy (GA). Dansingani and Freund 4 retrospectively assessed eyes receiving long-term anti-VEGF treatment for nAMD with type 1 MNV and minimal or no progression of GA. On OCTA, all eyes demonstrated mature, tangled vascular networks with persistent flow. The authors hypothesized that these vascular networks may compensate for reduced choriocapillaris function by providing oxygenation or nourishment to the retinal pigment epithelium (RPE) and outer retina, thereby mitigating the progression of GA. Similarly, Ichiyama et al 6 used OCTA to evaluate patients with nAMD in the remission stage and found persistent flow in MNV, with greater vessel density correlating with best-corrected VA (BCVA). Querques et al 7 compared fibrocellular and fibrovascular patterns of fibrosis in eyes with nAMD in remission and found that the patterns exhibited less neovascular lesion perfusion, greater RPE atrophy, lower BCVA, and reduced macular sensitivity. Furthermore, in subgroup analyses including only eyes with fibrovascular patterns, neovascular lesion perfusion density was inversely associated with RPE atrophy. Collectively, these findings suggest that preservation of perfused, mature MNV may be associated with more favorable structural and functional outcomes. Further research in nAMD is necessary to determine the optimal anatomic treatment outcomes.
The influence of combined Ang2 and VEGF inhibition on MNV morphology and fibrosis patterns, relative to VEGF inhibition alone, remains unclear. In our case series, the 2 eyes receiving long-term faricimab therapy developed mature, consolidated MNV networks resembling those previously described in the literature with traditional anti-VEGF agents.3,4 Although faricimab appeared to induce more durable regression of fine lacy capillary networks on OCTA compared with aflibercept, determining whether this effect reflects an enhanced molar binding capacity of anti-VEGF or the additional inhibition of Ang2 is not possible. 5
Joussen et al 8 hypothesized that dual inhibition of Ang2 and VEGF may facilitate vascular maturation and stabilization of perfused neovascular complexes while simultaneously suppressing vascular leakage. Additionally, preclinical studies in mouse models of MNV have demonstrated reduced fibrosis, 9 inflammation, and neurodegeneration 10 with combined VEGF-A and Ang2 inhibition compared with VEGF-A inhibition alone.
In conclusion, this case series described morphologic changes of MNV visualized on OCTA in 4 eyes with exudative nAMD after a transition from aflibercept to faricimab therapy. The central MNV trunk persisted in all eyes, with regression of fine lacy vasculature after treatment. Exudation was controlled despite the presence of residual MNV, and treatment intervals were successfully extended to 9 to 11 weeks. Further research is necessary to determine the optimal anatomic treatment outcomes for patients with nAMD and whether dual inhibition of Ang2 and VEGF-A pathways leads to differential MNV remodeling compared with VEGF-A inhibition alone.
Footnotes
Ethical Approval
This case series was conducted in accordance with the Declaration of Helsinki. Protected patient health information was collected and analyzed in compliance with the Health Insurance Portability and Accountability Act.
Statement of Informed Consent
Written consent was obtained from all patients for the publication of case details and clinical images.
Declaration of Conflicting Interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Dr. Chang has received consulting and speakers compensation from Genentech and Regeneron.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
