Abstract
Keywords
Introduction
Diabetic retinopathy (DR) occurs in approximately one-third of patients with diabetes. 1 In many countries, DR is a leading cause of preventable vision impairment and blindness in the working-age population. 1 Approximately one-third of patients with high-risk proliferative DR (PDR) will progress into severe vision loss within 3 years if not treated promptly. 2 In addition to medical management, patients with PDR could develop vision-threatening complications, including nonclearing vitreous hemorrhage (VH), tractional retinal detachment (TRD), and rhegmatogenous retinal detachment (RRD), 3 that require treatment with pars plana vitrectomy (PPV). 4 Within county-based and safety-net hospital populations, a large proportion of patients have long-standing and uncontrolled diabetes with limited access to preventative medical and retinal screening. Consequently, many patients commonly present with advanced PDR and vision loss secondary to its complications. 5
The rapid spread and development of COVID-19 into a global pandemic disrupted care in all health settings. In addition to increased rates of hospitalization and mortality from COVID-19 infections, the pandemic negatively affected the management of chronic medical conditions due to decreased access and increased patient fear and reluctance to seek out needed care in a timely manner. 6 In ophthalmology, the volume of routine clinic visits and surgeries, including vitreoretinal procedures and operations, was significantly decreased due to both lower clinic volume and patient no-shows and cancellations.7–9 Delays in care are associated with the increased complications and progression of DR reported during the COVID-19 pandemic.10,11
The COVID-19 pandemic disproportionately affected ethnic and racial minority groups, which make up a large proportion of populations relying on county-based and safety-net hospitals in the United States. 12 However, there have been few reports on the impact of the COVID-19 pandemic on vision-threatening diseases and outcomes in this patient population. This study examines the presentation and outcomes of patients with PDR who underwent PPV for PDR complications at 2 county-based safety-net hospitals in Los Angeles County, prior to and during the COVID-19 pandemic.
Methods
Study Design
This retrospective study was conducted at Harbor–University of California Los Angeles (UCLA) and Olive View-UCLA Medical Centers, 2 county hospitals in Los Angeles County, after receiving approval from the Harbor-UCLA Institutional Review Board (IRB) and Olive View-UCLA IRB committees. All study-related proceedings were performed in accordance with good clinical practice, the tenets of the Declaration of Helsinki, and the Health Insurance Portability and Accountability Act (HIPAA). Owing to the retrospective nature of the study, written informed consent was not required.
A comprehensive electronic health record review was performed for patients 18 years or older who underwent PPV for complications of PDR from March 20, 2018, to March 20, 2022, at either Harbor-UCLA or Olive View-UCLA Medical Center. A state of emergency was declared in California, with downsizing of elective procedures, on March 20, 2020, which was used as the cut-off date to separate the pre-COVID and post-COVID cohorts.
We collected baseline patient demographics (ie, age, gender, insurance type, ethnicity, primary language, established vs new patient, preoperative glycated hemoglobin [HbA1c]) as well as preoperative characteristics for all PPVs, including surgery request date, surgery date, indication for surgery (nonclearing VH, TRD, or TRD/RRD), prior treatment history such as panretinal photocoagulation (PRP) and/or intravitreal bevacizumab (Avastin; Genentech, Inc), best-documented visual acuity (VA), macular status (on vs off), and lens status (phakic, pseudophakic, or aphakic).
Patient presentation status was categorized as either established or new to the retina clinic. Patients lost to follow-up were defined as patients who did not return for scheduled follow-up visits for at least 6 months. Intraoperative characteristics collected included duration of surgery and surgical procedures performed (eg, membrane peel, air-fluid exchange, bimanual dissection, endolaser, or use of gas or oil tamponade). Cases of simultaneous cataract extraction plus intraocular lens (IOL) implantation with PPV (combined cataract extraction with IOL/PPV) and sequential cataract extraction with IOL followed by PPV (staged cataract extraction plus IOL/PPV) were noted.
Postoperative characteristics collected include VA at postoperative months 1 and 6, as well as any complications (VH), elevated intraocular pressure, or subsequent procedures (eg, bevacizumab, PRP, PPV) needed within the 6-month follow-up period. All eyes that underwent PPV were included for evaluation of surgery utilization, while repeat PPVs and/or eyes that did not have 6 months of follow-up were excluded from subsequent analyses, including preoperative, intraoperative, and postoperative outcomes. The electronic health record was last accessed on May 1, 2023, for the purposes of this study.
The primary outcome was VA at postoperative month 6. Additional outcomes included differences in preoperative, intraoperative, and remaining postoperative characteristics between the pre- and post-COVID groups.
Statistical Analysis
Categorical variables are described using frequencies and percentages. Continuous variables are described using means ± standard errors or medians with IQRs. Relationships between categorical variables were assessed using the Fisher exact test and χ2 test, and relationships between continuous variables were assessed using independent samples t tests and analysis of variance. Analyses were performed using JMP Pro 14 software (SAS Institute). P < .05 was considered statistically significant.
Results
During the pre-COVID period, 1068 PPVs were performed, of which 401 (37.5%) were for complications of DR (Figure 1). During the post-COVID period, 767 PPVs were performed, and 347 (45%) were for complications of DR. A total of 331 eyes in the pre-COVID group underwent PPV for the first time, and of those, 253 had at least 6 months of follow-up and were included in the subsequent analysis. A total of 306 eyes in the post-COVID group underwent PPV for the first time, and of those, 234 eyes had at least 6 months of follow-up and were included in the subsequent analysis.
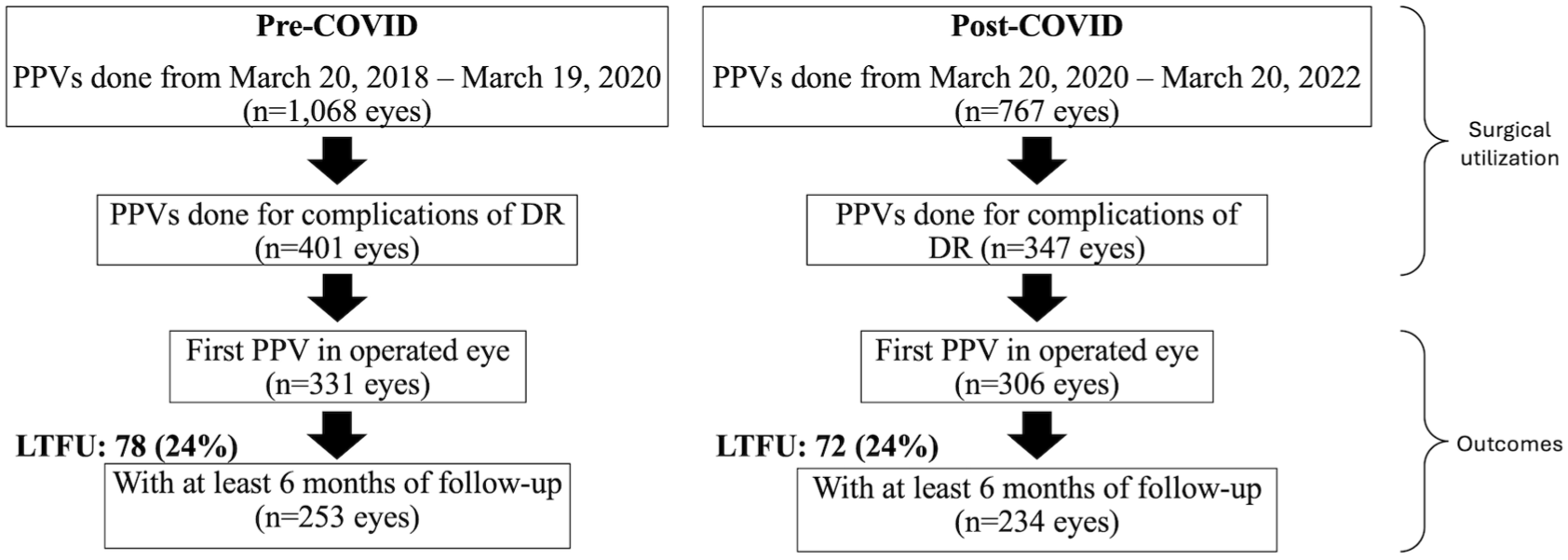
Patient data acquisition schematic. Abbreviations: DR, diabetic retinopathy; LTFU, long-term follow-up; PPV, pars plana vitrectomy.
Demographics
Demographics of patients who received an initial PPV for complications of PDR and had at least 6 months of follow-up are reported in Table 1. The median age was 52 years (IQR, 46-59), and 172 (39%) were women. A total of 388 patients (88%) reported their ethnicity as Hispanic/Latinx, and Spanish was the primary language for 337 (76%) patients. The median HbA1c within 3 months of surgery was 7.8 (IQR, 6.8-9.8). Given the county hospital setting for this study, all patients included had public insurance. There was no statistically significant difference in the above demographics between the pre-COVID and post-COVID groups (not shown).
Demographics of Patients Who Received an Initial Pars Plana Vitrectomy for Complications of Proliferative Diabetic Retinopathy.
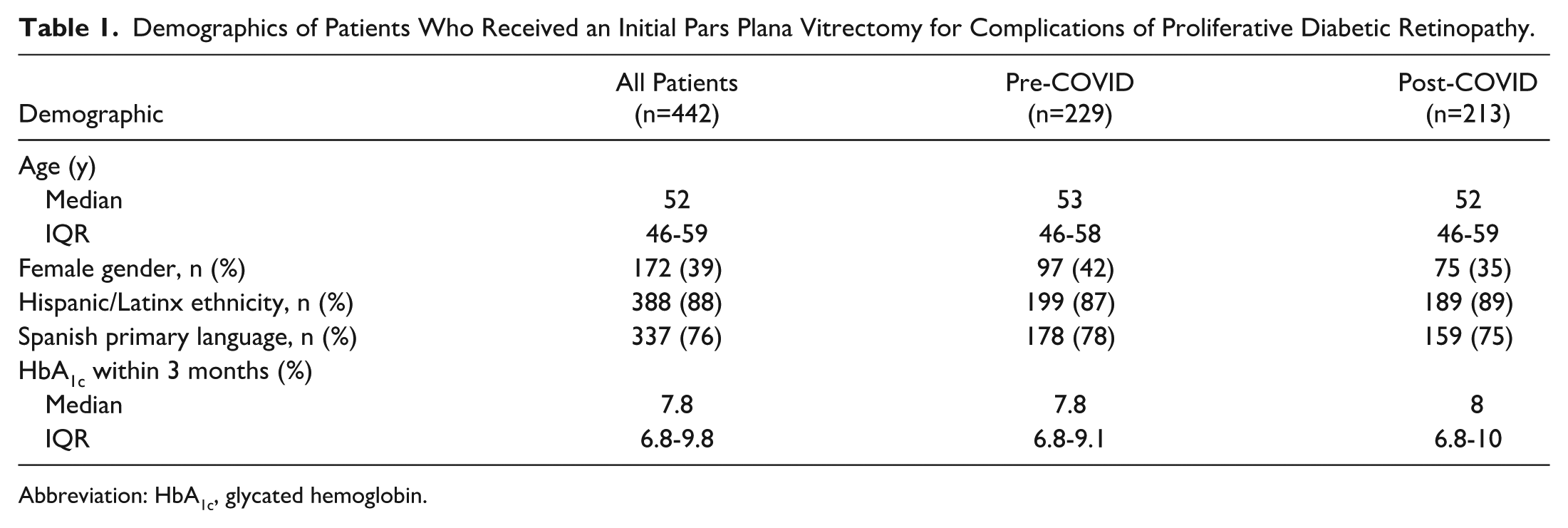
Abbreviation: HbA1c, glycated hemoglobin.
Surgery Utilization
The trend for the percentage of total PPVs done for complications of DR during the study period is shown in Figure 2A. The percentage trends for the surgical indications for all PPVs done for complications of DR are presented in Figure 2B. Of these cases, a greater proportion of PPVs done during the post-COVID period were for TRD (139 eyes [35%] vs 167 eyes [48%], respectively; P = .0009), and fewer were done for only nonclearing VH (178 eyes [44%] vs 116 eyes [33%], respectively; P = .0022) (data not shown).
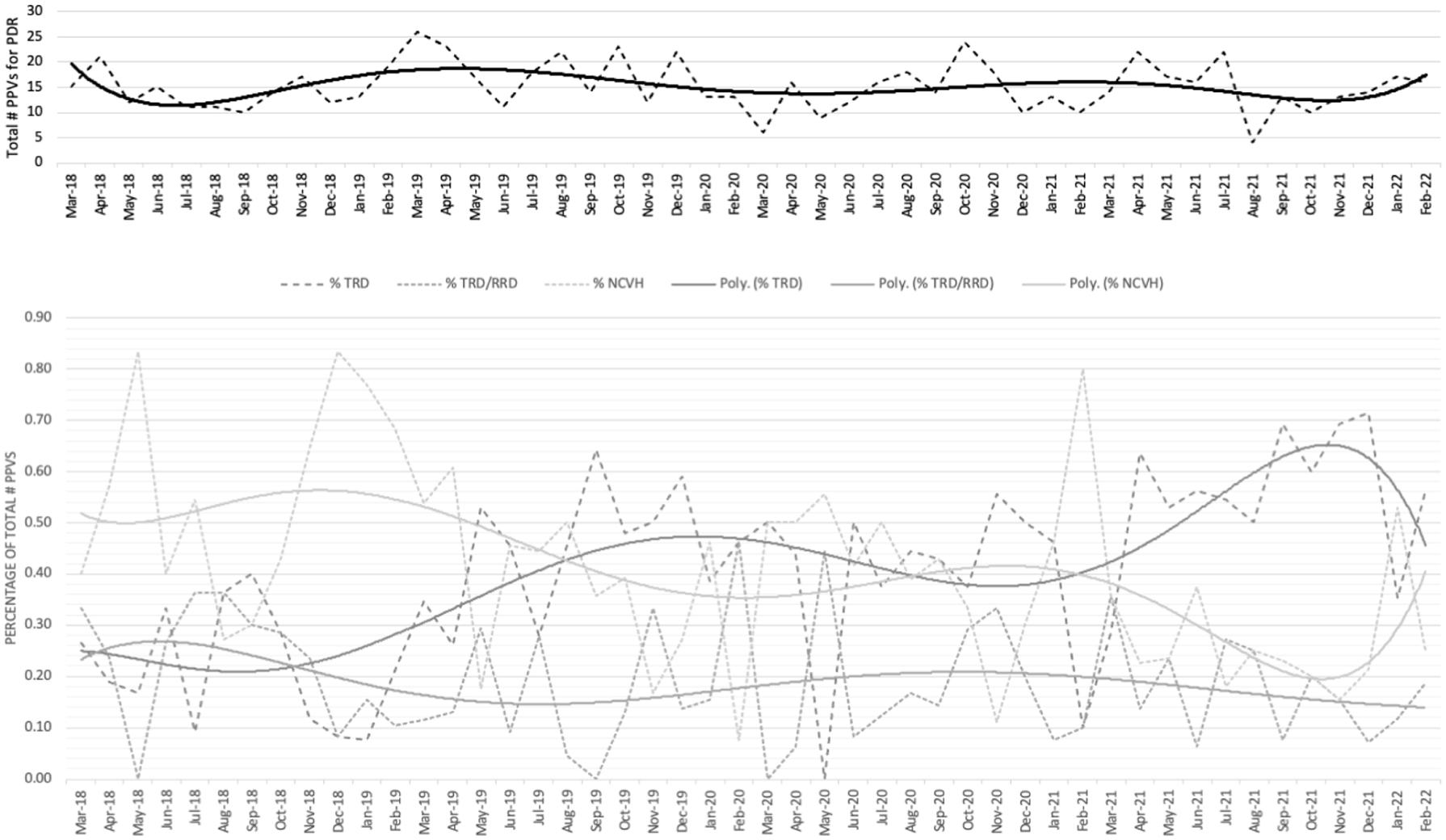
(A) Trend for percentage of total pars plana vitrectomies (PPVs) done for complications of diabetic retinopathy (DR) from March 20, 2018, to March 2022. (B) The percentage trends for the surgical indications of all PPVs done for complications of DR (dotted line indicates percentages, solid line indicates average trend). Abbreviations: PDR, proliferative DR; Poly., polynomial trendline; NCVH, nonclearing vitreous hemorrhage; RRD, rhegmatogenous retinal detachment; TRD, tractional retinal detachment.
In patients who received an initial PPV for complications of PDR and had at least 6 months of follow-up, there was no difference in the percentage of patients who were new to the clinic, established without loss to follow-up, or established with loss to follow-up (Table 2). The mean time between the surgery request date and the date of surgery was significantly longer in the post-COVID compared with the pre-COVID period (54 ± 2.7 vs 36 ± 2.6 days, respectively; P < .0001; Table 2). There was no pre-COVID vs post-COVID difference in the percentage of cases that had a previous surgery request submitted without surgery being done (owing to multiple possible factors, such as delays for medical clearance or patient no-shows).
Surgery Utilization.
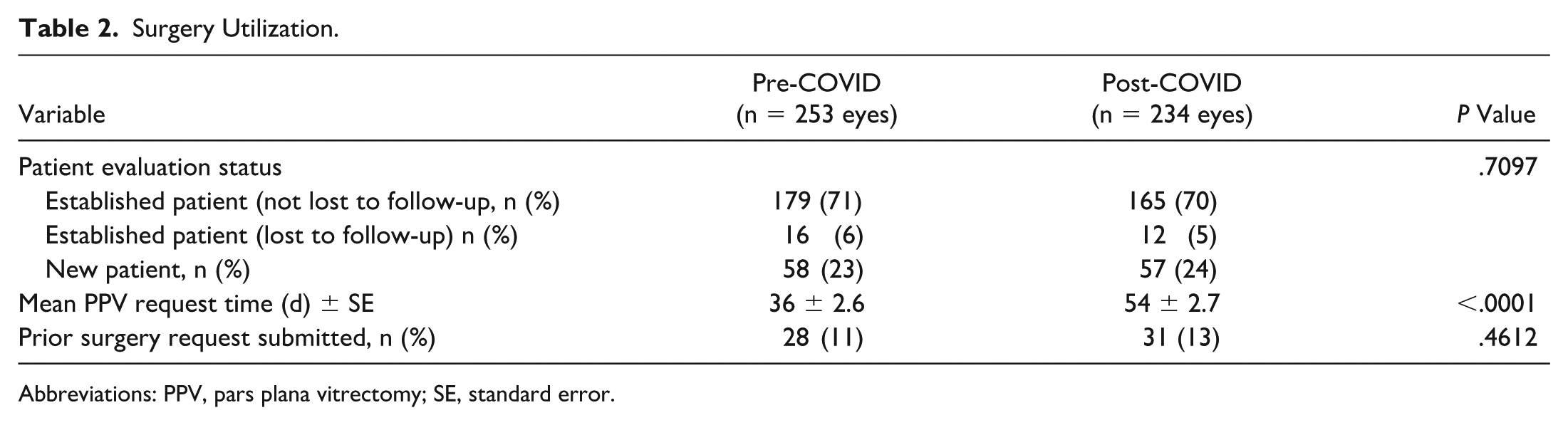

Abbreviations: PPV, pars plana vitrectomy; SE, standard error.
Preoperative Characteristics
In patients with at least 6 months of follow-up, more PPVs were done for TRD (115 [49%] vs 98 [39%]; P = .0206), and fewer were done for nonclearing VH (75 [32%] vs 105 [41%]; P = .0022) during the post-COVID compared with the pre-COVID period (Table 3). More eyes presented with macula-involving detachment during the post-COVID period (78 [33%] vs 59 [23%], respectively; P = .0001). There was no difference in lens status or the percentage of eyes receiving PRP or bevacizumab (excluding preoperative bevacizumab). There was also no pre-COVID vs post-COVID difference in the preoperative VA of the operated and fellow eyes.
Preoperative Characteristics.
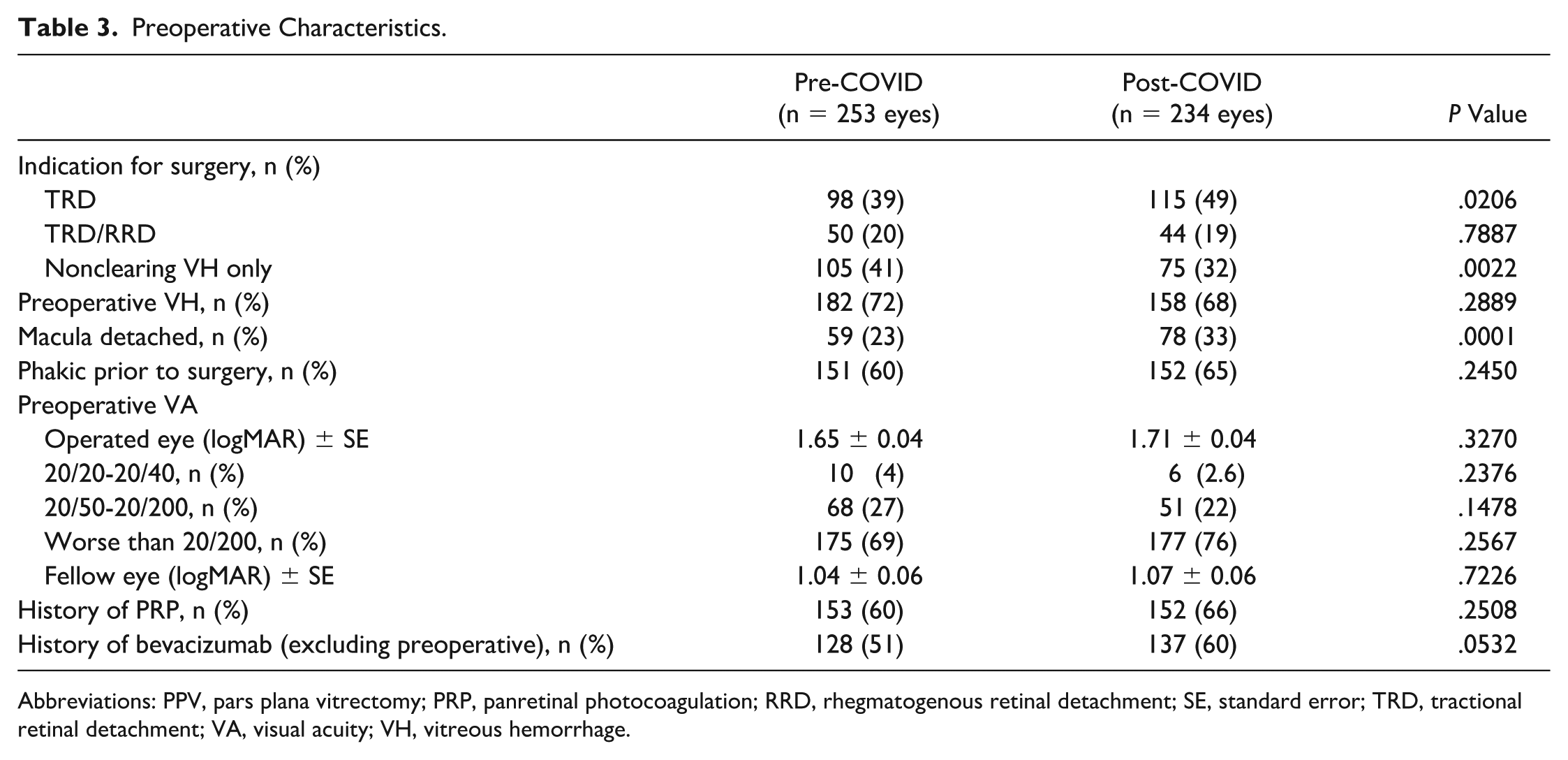
Abbreviations: PPV, pars plana vitrectomy; PRP, panretinal photocoagulation; RRD, rhegmatogenous retinal detachment; SE, standard error; TRD, tractional retinal detachment; VA, visual acuity; VH, vitreous hemorrhage.
Intraoperative Characteristics
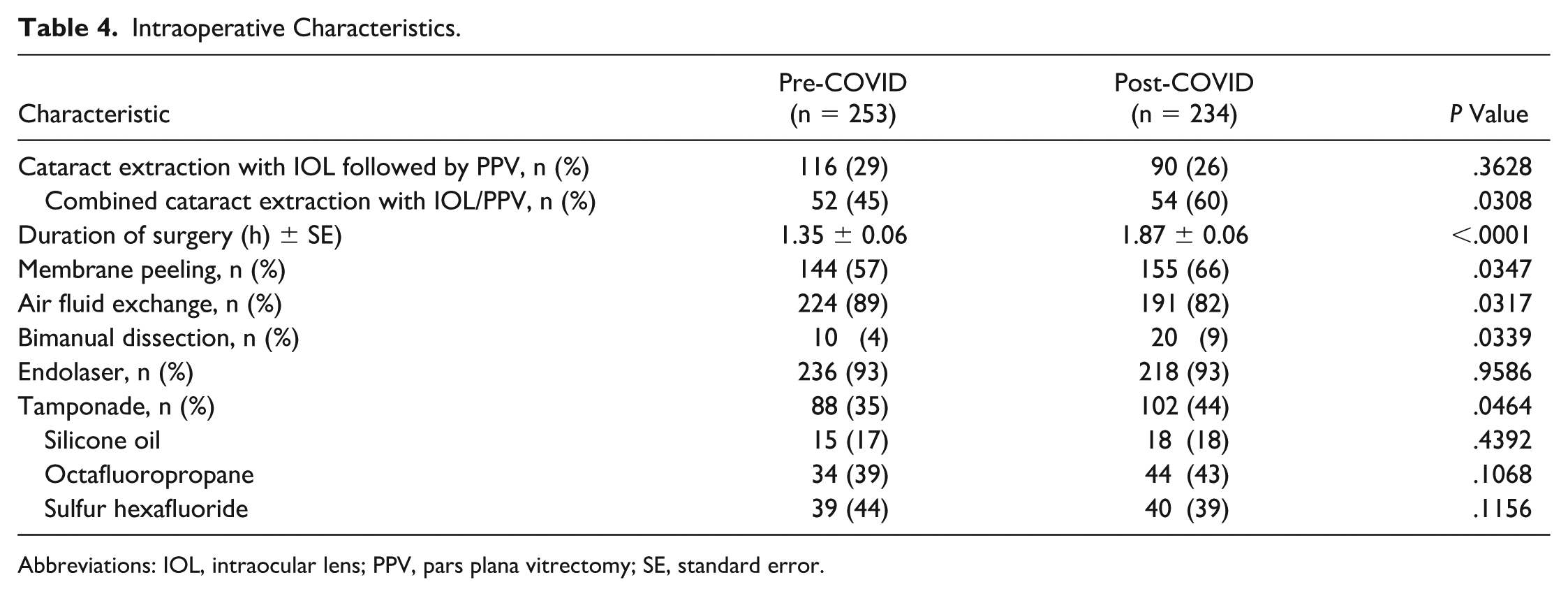
While there was no difference in the proportion of eyes that underwent cataract surgery around the same time as PPV, there was a greater proportion that received combined cataract extraction with IOL/PPV surgeries post-COVID (54 [60%] vs 52 [45%]; P = .0308) as opposed to staged cataract extraction with IOL/PPV surgeries (Table 4). The mean duration of surgery was longer in the post-COVID group, even after adjusting for combined cases (1.87 ± 0.06 vs 1.35 ± 0.06 hours; P = .0001).
Intraoperative Characteristics.
Abbreviations: IOL, intraocular lens; PPV, pars plana vitrectomy; SE, standard error.
Additionally, a greater proportion of cases used membrane peeling (155 [66%] vs 144 [57%]; P = .0347) and bimanual dissection (20 [9%] vs 10 [4%]; P = .0339) and fewer cases that used air-fluid exchange (191 [82%] vs 224 [89%]; P = .0317) post-COVID. During the post-COVID period, there was a greater proportion of cases in which gas or oil tamponade was used, though there was no difference when stratified by type of tamponade and no difference in the proportion of cases that used endolaser.
Postoperative Visual Acuity and Complications
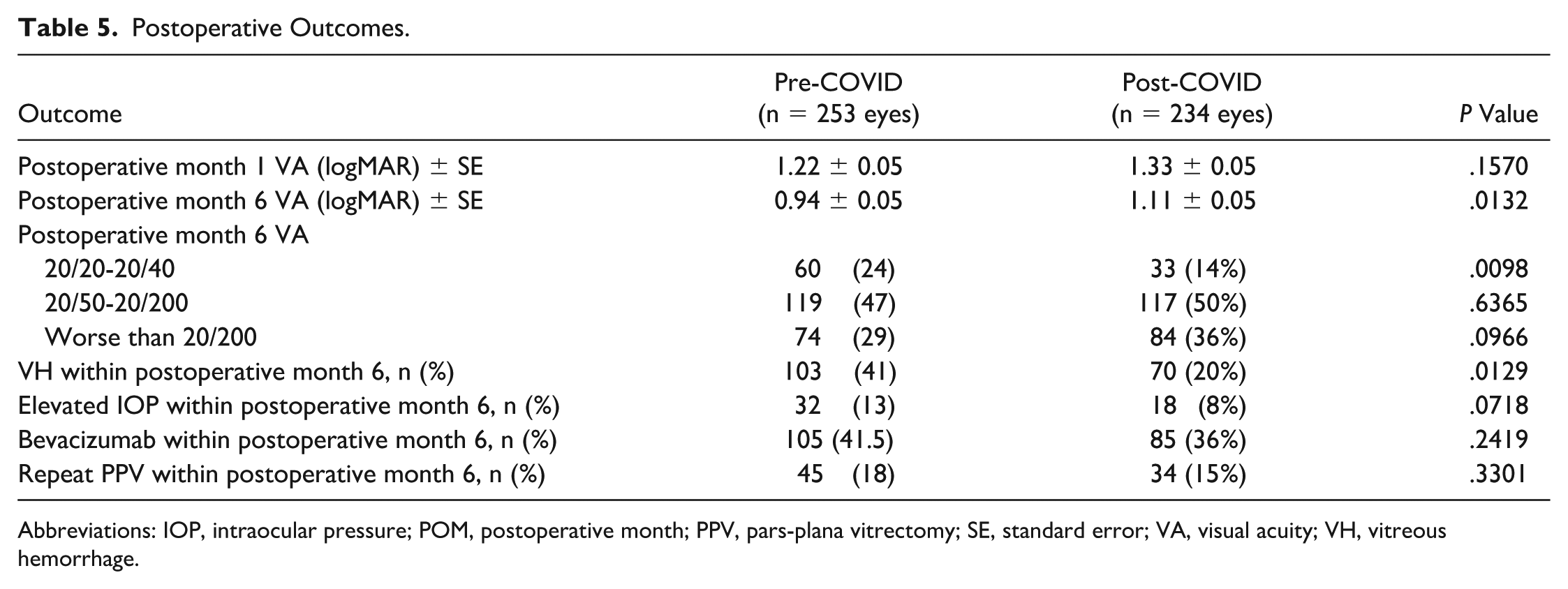
There was no statistically significant difference in mean VA between the 2 groups at postoperative month 1. The mean VA at postoperative month 6 was worse post-COVID compared with pre-COVID (1.11 ± 0.05 logMAR vs 0.94 ± 0.05 logMAR; P = .0132; Table 5), and when stratified by group, there were fewer patients post-COVID who had 20/40 or better vision (34 [14%] vs 61 [24%]; P = .0098). After accounting for preoperative characteristics, pre-COVID and post-COVID group status were no longer significantly associated with VA at postoperative month 6, while preoperative VA, macular status, duration of surgery, and time from surgery request to PPV remained significantly associated (Supplemental Table 1).
Postoperative Outcomes.
Abbreviations: IOP, intraocular pressure; POM, postoperative month; PPV, pars-plana vitrectomy; SE, standard error; VA, visual acuity; VH, vitreous hemorrhage.
Within 6 months, there were fewer incidences of VH (70 [20%] vs 103 [41%]; P = .0129) and no difference in incidences of elevated intraocular pressure post-COVID compared with pre-COVID (Table 5). There was also no difference in the proportion of eyes that required intravitreal injection or repeat PPV for postoperative complications in the 6 months following surgery.
Conclusions
This retrospective cohort study examines the visual outcomes of patients who underwent PPV for complications of DR and demonstrates worse visual outcomes at 6 months in patients who underwent PPV during the post-COVID period compared with the pre-COVID period. Numerous factors may explain this. The post-COVID cohort had significantly increased cases of TRD and macula-involving detachment, and there was an increase of almost 20 days between the surgery request date and date of surgery.
Additionally, more cases used intraoperative techniques such as bimanual dissection, membrane peeling, and gas or oil tamponade, suggesting a higher level of complexity in the post-COVID surgical cases. Interestingly, there were fewer incidences of postoperative complications post-COVID compared with pre-COVID. These findings suggest that during the post-COVID period, patients who underwent PPV for complications of DR presented with more severe disease and longer surgical wait times, which likely contributed to worse visual outcomes following PPV, despite lower complication rates.
Numerous studies have examined the effect of the COVID-19 pandemic on surgical outcomes in patients with RRD,13–15 but there are limited studies on outcomes in patients who undergo PPV for complications of PDR. In the present study, there was no difference in baseline VA between the pre-COVID and post-COVID cohorts. This may be due to the visually compromising nature of vitreous hemorrhage, even without TRD.
There was a significant improvement in postoperative vs preoperative vision in both groups, demonstrating that surgery was still of benefit in the majority of patients with complications of PDR, though the post-COVID cohort had worse VA overall at postoperative month 6 compared with the pre-COVID cohort. There were fewer patients in the post-COVID cohort who had 20/40 or better VA (14% vs 24%), and while direct comparisons with other studies that looked at visual outcome following vitrectomy for PDR are difficult, these percentages seemed to be within the range of those previously reported.16–19
After adjusting for preoperative and intraoperative characteristics, including preoperative vision, macular status, surgical duration, and time between surgery request and surgery, pre-COVID vs post-COVID status was no longer significantly associated with postoperative visual outcomes. Instead of COVID status alone, other significant differences between the pre- and post-COVID groups contributed to the differences in visual outcomes. Preoperative vision and macular status were independent predictors for visual outcome, which is consistent with a previously published study by Yorston et al that examined outcomes in 174 eyes following PPV for PDR. 17 Tractional disease was no longer significantly associated with visual outcomes after adjusting for surgical duration, which was found to be independently associated with worse visual outcomes even after controlling for combined cataract extraction with IOL/PPV cases.
In addition to anatomical pathology, functional pathology, such as degree of macular ischemia, could also affect visual outcomes. Longer surgical duration likely has multiple contributing etiologies, including greater complexity of cases and increased rates of intraoperative complications. Difference in primary surgeon is 1 factor that was not explored in this article, though vitreoretinal fellows would be expected to be at similar stages of training between the 2 cohorts, and year of fellowship was previously shown not to significantly influence outcomes or complications. 20 Surgical fellows starting during the post-COVID period may have had less surgical volume, but this was not associated with increased postoperative complication rates in this study.
The COVID-19 pandemic resulted in delays in surgical care and overall surgical utilization in numerous ways, with 1 significant factor being patient-driven care avoidance. 21 In 1 study of all patients with RRD at a tertiary academic center, there were significantly fewer patients who presented with a macula-sparing retinal detachment in 2020, and the time interval between symptom onset and presentation increased from 5.96 to 15.36 days. 13 In another multicenter study, the delay was increased to 22 days following the lockdown, leading to more epiretinal membrane proliferative vitreoretinopathy and lower single-surgery anatomic success rates. 14 In a study of patients with PDR, greater delay in appointments during the pandemic was associated with increased risk of requiring vitrectomy for proliferative complications, and patient-directed rescheduling was the main driver of care delays. 22 These studies suggest that, during the height of the pandemic, patients delayed seeking out medical care for vision-threatening conditions. This hesitancy may be a significant contributing factor to patients presenting with more severe disease on initial evaluation during the post-COVID period in this study.
While there was a 28% reduction in the total number of PPVs done in the post-COVID period compared with the pre-COVID period, with the greatest decline immediately following the lockdown, there was only an approximately 13% reduction in the number of PPVs done for PDR. PPVs for complications of PDR made up a larger proportion of cases being done post-COVID, which suggests that these surgeries were being prioritized when scheduled. Despite this, there was still an increase in wait time of almost 20 days between the surgery request date and the date of surgery. The delay itself was significantly associated with poorer visual outcomes, despite controlling for other preoperative characteristics and pre- vs post-COVID group status. While the etiology of this delay is likely multifactorial (eg, less operating room availability, patients testing positive for COVID, or patient/provider cancellation) and is not examined in this study, delays between presentation and surgery could lead to progressive retinal detachment and retinal damage, further compromising anatomic and visual outcomes. Similarly, in another UK study of 185 eyes, poor predictors of visual success included failure to attend clinic appointments and surgery delays. 16
Within the post-COVID group, there was an increased proportion of combined cataract extraction with IOL/PPV compared with staged cataract extraction with IOL/PPV. The increased use of combined cataract extraction with IOL/PPV post-COVID might reflect attempts to circumvent limited operating room availability and decrease surgery wait time. Postoperative VHVH is the most common complication after PPV for PDR and has been reported in 16% to 55% of cases.16,17,23,24 In this study, we found fewer incidences of VH in the post-COVID group compared with the pre-COVID group, which may in part be explained by the more frequent use of a long-acting tamponade agent in the post-COVID cohort. 25 While increased usage of a long-acting tamponade may be associated with more complex cases, it may also partially reflect attempts to decrease the risk of postoperative complications, leading to reoperation when operating room time is limited.
Strengths of this study include its large sample size and analysis of a patient cohort from 2 large county-based safety-net hospitals. Limitations include its retrospective nature and the potential for a variety of confounding variables. During the beginning of the pandemic, the criteria for deciding surgical necessity, such as for cases of VH, may have been influenced by COVID-19 itself and led to a preference for nonsurgical treatments.
While HbA1c levels reflect diabetes control, this study does not report on disease duration and time interval between symptom onset and surgery. Since the database used for this study includes all eyes that underwent PPV, patients who had surgery requests submitted but never received surgery were not included. Additionally, preoperative VA was obtained when surgery scheduling was initiated, and not immediately before surgery.
In conclusion, this study found that patients undergoing PPV for PDR presented with more advanced pathology during the post-COVID period and experienced worse visual outcomes after PPV compared with pre-COVID patients. These findings are multifactorial in etiology but are likely secondary to COVID-19–related delays in patient presentation and access to surgery. Interruptions in care during the start of the COVID-19 pandemic in this patient population have persistent effects on DR severity and surgical outcomes even 2 years after the COVID-19 lockdown.
Future studies with larger and more diverse study populations are warranted to improve the generalizability of these findings and examine outcomes in different patient populations.
Supplemental Material
sj-docx-1-vrd-10.1177_24741264251414110 – Supplemental material for Effect of the COVID-19 Pandemic on Presentation and Outcomes of Pars Plana Vitrectomy for Complications of Diabetic Retinopathy Within a County System
Supplemental material, sj-docx-1-vrd-10.1177_24741264251414110 for Effect of the COVID-19 Pandemic on Presentation and Outcomes of Pars Plana Vitrectomy for Complications of Diabetic Retinopathy Within a County System by Weilin Song, Reza Kianian, Judy Figueroa, Jack Benjamin Margines, Jiwei Sheng, Hamid Hosseini, Pradeep S. Prasad and Kirk Hou in Journal of VitreoRetinal Diseases
Footnotes
Acknowledgements
We would like to acknowledge David Peprah and Sayan Chatterjee for assistance with data collection.
Ethical Approval
Approved by the Harbor-UCLA IRB Committee and the Olive-UCLA IRB Committee.
Statement of Informed Consent
Due to the retrospective nature of this study, written informed consent was not required.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was generously supported by an unrestricted Research to Prevent Blindness grant.
Supplemental Material
Supplemental material is available online with this article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
