Abstract
Introduction
Clinically detectable cases of systemic lymphoma with involvement of the iris are rare, with approximately 50 cases appearing in the PubMed database over the past 40 years. 1 Although diffuse large B-cell lymphomas are the most common subtype of lymphoma (25% to 30% of non-Hodgkin lymphoma cases), 2 fewer than 10 cases in which the iris was involved have been reported in the literature (Table 1).3–7 Systemic chemotherapy and radiation were used for treatment in those cases.
Cases Reports of DLBCL Involving the Iris.
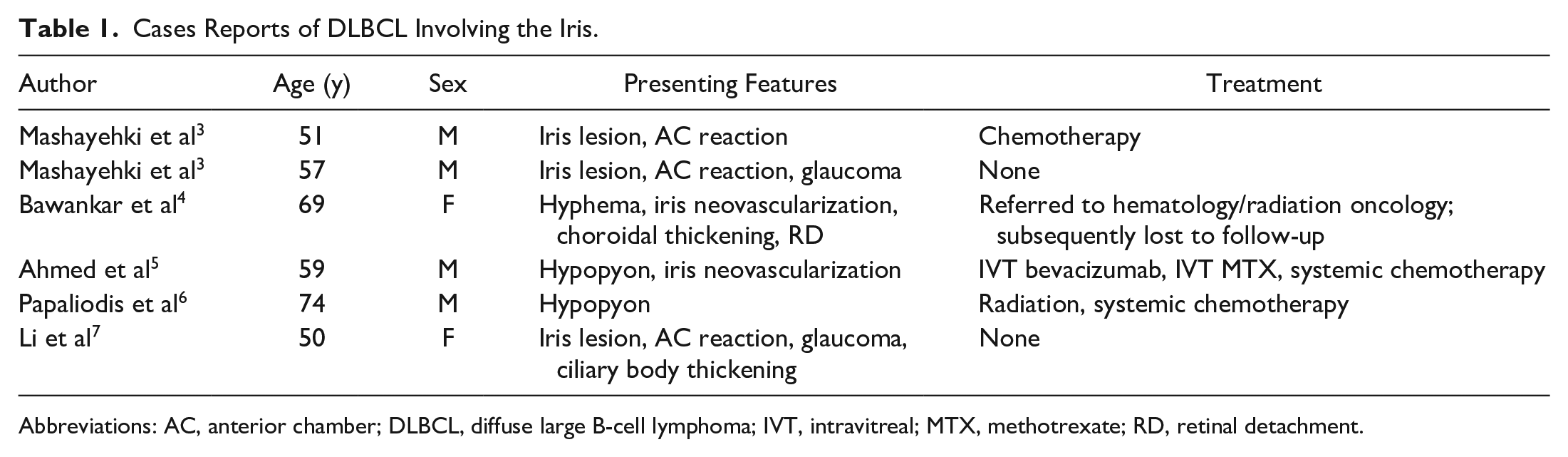
Abbreviations: AC, anterior chamber; DLBCL, diffuse large B-cell lymphoma; IVT, intravitreal; MTX, methotrexate; RD, retinal detachment.
We report a case of recurrent diffuse large B-cell lymphoma in the iris that was initially treated with intravitreal (IVT) chemotherapy and subsequent radiation for persistent disease activity. To our knowledge, no other cases have been reported in which IVT chemotherapy was used as the initial treatment.
Case Report
A 75-year-old woman with a history of treatment for diffuse large B-cell lymphoma was referred for evaluation of an iris lesion. She was initially treated with 6 cycles of chemotherapy comprising rituximab, cyclophosphamide, hydroxydaunomycin, vincristine, and prednisone for systemic disease.
A relapse occurred with secondary central nervous system involvement, and the patient was treated with salvage chemotherapy comprising 1 cycle of rituximab, etoposide, methylprednisolone, high-dose cytarabine, and cisplatin and 1 cycle of rituximab, dexamethasone, cytarabine, and cisplatin. Mobilization of the peripheral blood stem cells was performed after chemotherapy to ensure an adequate number of stem cells for transplantation. Autologous stem cell transplantation resulted in a good metabolic response.
Nine months after autologous stem cell transplantation, the patient was evaluated in the retina clinic. The visual acuity (VA) was 20/20 OD and 20/25 OS. A temporal iris mass was noted in the left eye with associated iris thickening (Figures 1A and 2A). A layered hyphema and white hypopyon (candy-cane hyphema) were present with 3+ cells in the anterior chamber. The vitreous was significant for 2+ cells and haze. Uveal involvement including the ciliary body was seen on imaging (Figure 2A). There was no posterior pole choroidal thickening on optical coherence tomography.
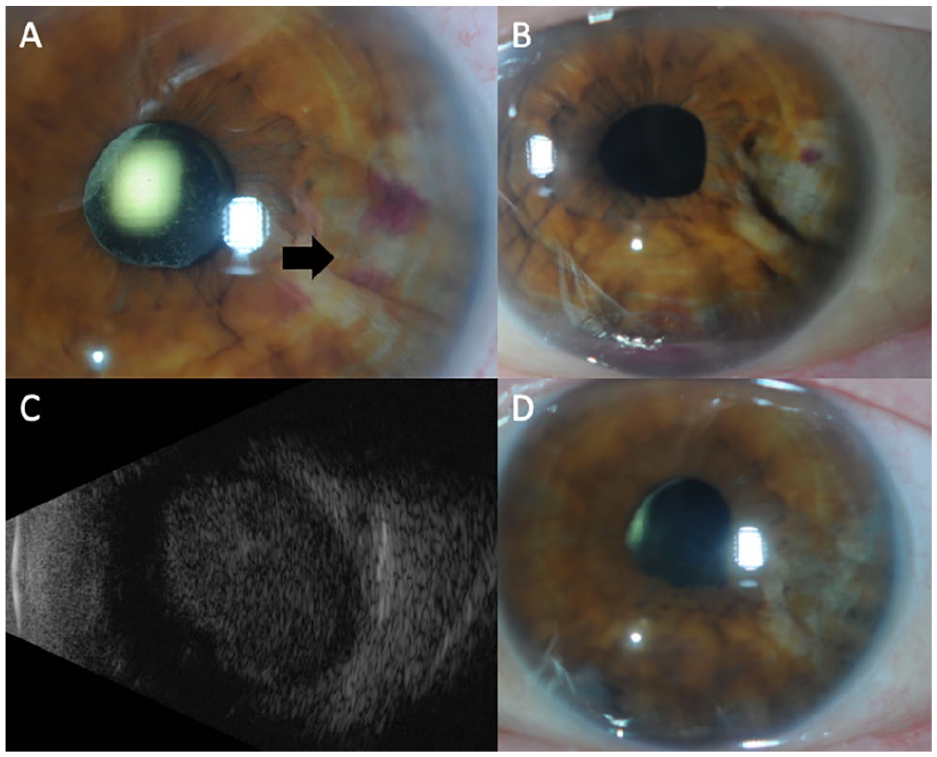
(A) Anterior segment photograph of the left eye shows a temporal iris mass with central hemorrhage overlying the lesion (arrow). (B) Remission of the iris mass with cavitation of the iris after intravitreal methotrexate therapy with evidence of a small hyphema. (C) B-scan ultrasound of the choroidal mass at the time of lymphoma recurrence; longitudinal scan at 6 o’clock. (D) Resolution of the iris mass after external beam radiation therapy.
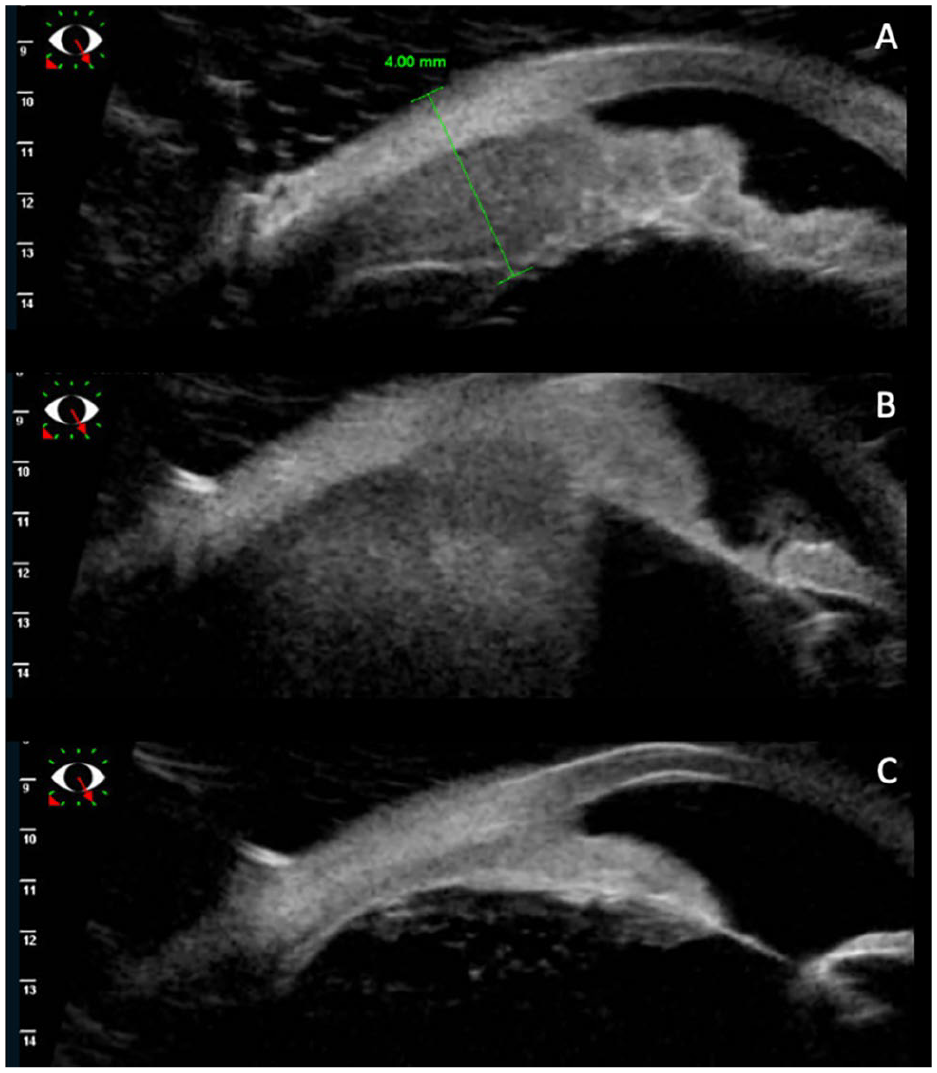
(A) Ultrasound biomicroscopy shows lymphoma involvement of the iris and ciliary body on presentation. (B) Progression of the iris lymphoma into the ciliary body at the time of lymphoma recurrence. (C) Resolution of the iris mass after external beam radiation therapy.
An anterior chamber washout was performed, and aqueous fluid was sent for cytology. The results showed CD5-negative/CD10-negative large B-cell lymphoproliferation with CD43 positivity. CD19-positive B cells comprised 92% of the lymphoid subset. A positron emission tomography/computed tomography scan was performed, showing no evidence of disease outside the eye. Magnetic resonance imaging of the brain showed subtle thickening in the soft tissue of the anterior left globe.
A discussion with the oncology team led to the decision to begin with local therapy and to consider radiation if the response was minimal. The initial plan was to start combined therapy with IVT methotrexate and IVT rituximab. Because of a lack of insurance coverage, rituximab was not available; therefore, methotrexate monotherapy was initiated. Twice weekly therapy consisting of IVT methotrexate (400 mg/0.1 mL) was started. After 2 weeks, the injection interval was extended to once weekly for 4 treatments.
There was an initial reduction in tumor size with treatment (Figure 1B). The interval between injections was then extended to every 2 weeks, resulting in a new hyphema and a VA of 20/60. Ultrasound biomicroscopy showed enlargement of the ciliary body, which suggested extension of disease (Figure 2B), while a posterior examination showed an inferior choroidal mass (Figure 1C). The patient was referred to the radiation oncology service for external beam radiation (2000 cGY dose over 10 fractions) applied to the whole eye. After treatment, involution of the intraocular mass occurred (Figures 1D and 2C).
At 5 months, there was no evidence of ocular recurrence and the VA remained stable at 20/60. Unfortunately, there was further relapse of diffuse large B-cell lymphoma in the left thigh, and palliative treatment was commenced. The patient died 10 months after initially presenting to the retina clinic.
Conclusions
Iris lymphomas typically present with clinical signs and symptoms that may overlap with those of anterior uveitis.1,3 Other considerations on the differential include presumed tubercular or sarcoid granuloma.8,9 Features such as hyphema, abnormal iris vessels, and visible lymphoid infiltration of the conjunctiva, iris, or choroid can help differentiate iris lymphoma from anterior uveitis; however, a definitive diagnosis cannot be made without tissue sampling or aqueous cytology.1,3 Ultrasound biomicroscopy is valuable in identifying the extent of iris and ciliary body infiltration, while B-scan imaging can characterize choroidal thickening and is especially helpful when there is media opacity.
Once the aqueous fluid or tissue sample has been obtained, the diagnosis of iris lymphoma is confirmed based on cytomorphology and ancillary testing that includes flow cytometry, immunohistochemistry, and cytogenetics. 10 The differential diagnoses for iris lymphoma include benign reactive lymphoid hyperplasia, amelanotic iris nevi, amelanotic iris melanoma, juvenile xanthogranuloma, and autoimmune uveitis in the setting of autologous bone marrow transplantation. 1
In our case, the treatment options, which included initiation of IVT therapy with the option of adjunct radiation if required, were discussed with the patient. IVT therapy and radiation were both considered because of the localized area of recurrence. There had been no recurrence of lymphoma outside the left eye when the patient presented to the retina clinic. Fortunately, lymphoma is rather radiosensitive; however, most institutions would agree that low-grade extranodal marginal zone lymphoma is treated at a lower dose (20 to 24 Gy) while high-grade lymphoma (eg, diffuse large B-cell lymphoma) is treated at a higher dose (30 Gy).11,12 In cases of palliative radiation, lower doses are often used. This knowledge is derived from the treatment of choroidal lymphoma, which tends to be low grade.
Although our patient had a good initial response to IVT methotrexate, there was progression of disease involving the iris and ciliary body in addition to choroid involvement after the treatment interval was extended to every 2 weeks. External beam radiation therapy with a mean dose of 28.67 Gy for high-grade secondary choroidal lymphoma has been shown to be beneficial, achieving long-term regression in 96% of cases. 11 Previous case reports of iris and ciliary body lymphomas also show good outcomes after external beam radiation therapy, with no ocular recurrence, 3 as seen in our patient.
Footnotes
Ethical Approval
The authors’ institution does not require ethical approval for reporting individual cases or case series.
Statement of Informed Consent
The patient provided verbal informed consent, including permission for publication of all photographs and images included herein.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of the article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
