Abstract
Introduction
Norrie disease is an X-linked recessive retinal disorder characterized by retinal dysplasia and systemic findings of hearing loss and developmental delay. 1 Unfortunately, the disease is highly aggressive and results in retinal neovascularization and secondary tractional retinal detachment (RD) soon after birth, with poor visual outcomes. 2
A planned preterm delivery of a fetus at 34 weeks with a known NDP mutation tested by amniocentesis has been reported. 3 The infant had bilateral laser ablation and intravitreal bevacizumab in the left eye. Recently, at the 8-year follow-up, the patient had a visual acuity (VA) in both eyes of 20/80.3,4 Similarly, a case of preterm delivery of a fetus with familial exudative vitreoretinopathy (FEVR) whose siblings had severe congenital tractional RDs has been reported. 5
Here, we report a case of planned early-term delivery of a fetus with Norrie disease diagnosed based on positive NDP genetic testing on chorionic villus sampling 6 and total RDs noted on transabdominal fetal ophthalmic ultrasound.7,8
Case Report
A fetus had positive NDP genetic testing [c377 G>A; p.(C126Y); hemizygous] on chorionic villus sampling. An older brother with bilateral no-light-perception VA and developmental delay had been diagnosed with Norrie disease with the same genetic mutation in NDP. A preterm delivery at 34 weeks was planned for treatment of retinal dysplasia. A transabdominal ultrasound performed at 32 weeks found bilateral total RDs vs persistent fetal vasculature (Figure 1A). A confirmatory repeat ultrasound at 34 weeks showed total RDs (Figure 1B), and the decision was made to postpone the delivery until early term. The neonate was delivered at 37 weeks and the following day had an examination under anesthesia. Fluorescein angiography showed he had inoperable total RDs with very poor peripheral vascularization (Figure 1, C and D).
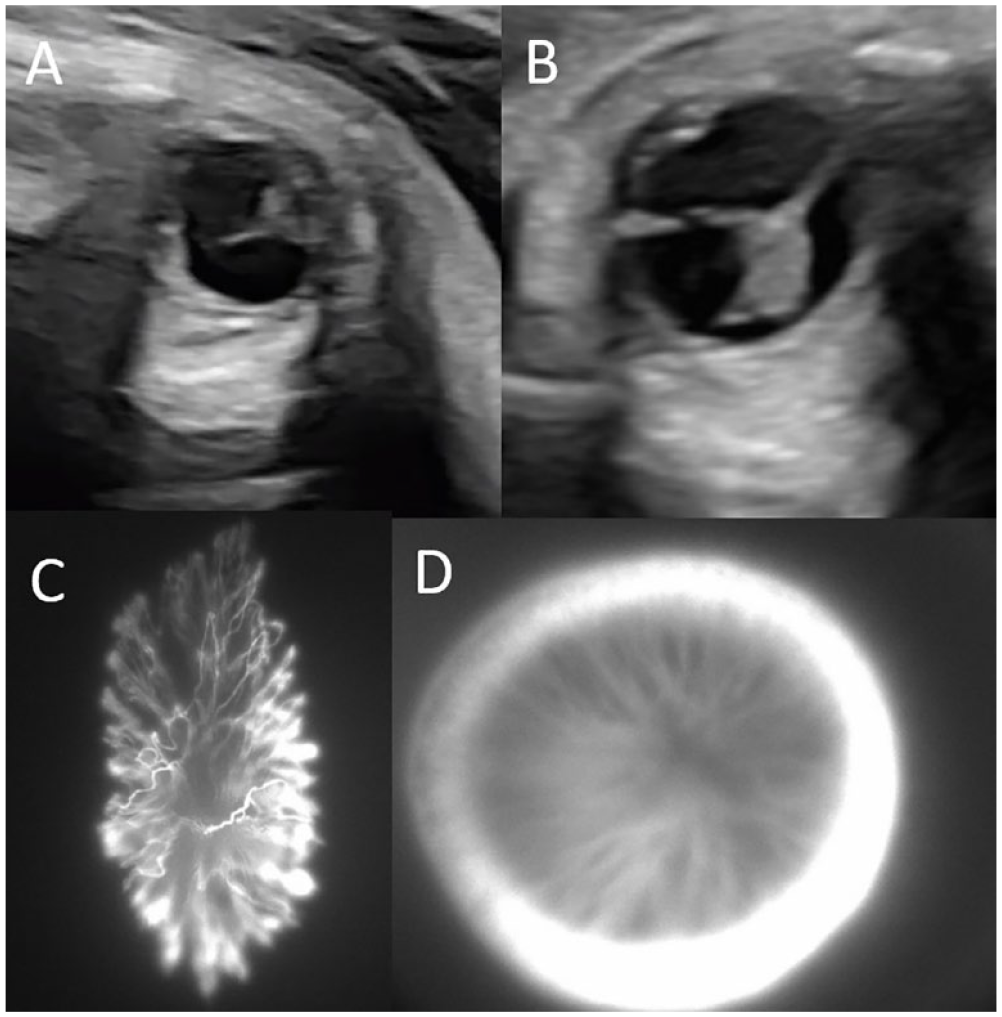
Retinal imaging in Norrie disease. (A) Transabdominal fetal ophthalmic ultrasound at 32 weeks found bilateral total retinal detachments (RDs) vs persistent fetal vasculature, as seen in this image of the left eye. (B) Subsequent transabdominal fetal ophthalmic ultrasound at 34 weeks confirmed a diagnosis of bilateral total RDs, as seen in this image of the right eye. Intraoperative fluorescein angiography of the left eye (C) and the right eye (D) 1 day after birth shows severe poor perfusion and inoperable total RDs.
The infant was seen in the pediatric ophthalmology clinic at 6 months of age and was noted to possibly wince to light in both eyes. The infant was comfortable, and both eyes were soft to palpation. He was enrolled in early intervention for low vision and will be evaluated for scleral shells.
Conclusions
Planned preterm delivery of infants with FEVR and Norrie disease has been reported.3 –5 Although the long-term outcomes of the patient with FEVR is not yet available, the patient with Norrie disease had an excellent outcome (20/80 OU) after laser ablation and intravitreal bevacizumab. Similarly, early-term delivery has been reported in a patient with Norrie disease who had immediate laser photocoagulation to the avascular retina with a bilateral VA outcome of 20/100. 9 All these cases highlight the potential for planned early-term or preterm birth in patients with congenital retinal vascular disorders for better long-term visual outcomes after treatment with panretinal photocoagulation and/or intravitreal bevacizumab than after pars plana vitrectomy. 2
There are 2 critical components to the diagnosis of Norrie disease in utero. First is accurate genetic testing with amniocentesis or chorionic villus sampling.3,6 Subtle differences in the genetic mutations in the Wnt pathway can result in FEVR or Norrie disease, which can require different treatment algorithms and prognoses.10,11 Second, fetal ophthalmic ultrasound is critical to identify whether there are RDs in utero.7,8 In our case, unlike in previously reported cases,3 –5 the patient had already developed bilateral total RDs in utero. Although we had initially planned on preterm delivery, once the bilateral total RDs were noted the decision was made to postpone the delivery to early term to optimize both fetal and maternal health.
Multicenter studies are warranted on the utility and safety of preterm or early-term delivery in fetuses with congenital retinal vascular disorders such as FEVR, Norrie disease, or incontinentia pigmenti, in particular if the fetus has evidence of an RD in utero. As seen in previous studies,3 –5 these infants with normally severe visual outcomes can have promising results with early intervention. Further use of fetal ophthalmic ultrasound screening in combination with genetic testing should be considered in patients with siblings or family members with a known history of retinal genetic disorders to identify at-risk fetuses for referral to centers with pediatric retina specialists.
Footnotes
Ethical Approval
The Duke Health institutional Review Board did not require review this case report of a single patient.
Statement of Informed Consent
Informed consent was obtained from the patient’s guardian for publication of the case report and accompanying images.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Dr. Justin received funding from the Heed Ophthalmic Foundation.
