Abstract
Objective
Vestibular impairment has been observed in patients with congenital hearing loss, but little is known about the vestibular anatomy and function of those in this group with inner ear malformations. This study aims to investigate the association between vestibulocochlear anatomy and vestibular function test results in children with inner ear malformations.
Study Design
Case series with chart review.
Setting
Pediatric patients with inner ear malformations presenting with bilateral profound hearing loss at a tertiary hospital from 1999 to 2017.
Methods
Ears were classified into subgroups based on anatomic abnormalities seen on computed tomography imaging. Cervical vestibular evoked myogenic potential (cVEMP), rotatory chair, and caloric test results were obtained and collated. Descriptive and inferential statistics were calculated.
Results
Of 82 ears, 29.3% had incomplete partition type II malformation, the most common type. The second-most common type was isolated vestibular organ anomaly (20.7%), which is not included in currently accepted categories. Most ears exhibited abnormal vestibular function. Abnormal vestibule volume was associated with a nonreactive cVEMP (P < .001). Radiologically abnormal lateral semicircular canals were associated with abnormal caloric and rotatory chair results (P < .001).
Conclusion
With a relatively large number of cases of isolated vestibular organ anomaly not only in our study but also in previous publications, we suggest that this category be added to the subsets of inner ear malformations. Abnormal vestibule volume was significantly associated with a nonreactive cVEMP finding. The majority of patients with hearing loss secondary to inner ear malformations have abnormal vestibular function test results.
Congenital hearing loss, which affects 3 children out of every 1000, 1 has long been linked to vestibular impairment.2,3 Inner ear malformations (IEMs) account for 20% of patients with congenital hearing loss, 4 but there is a paucity of data detailing vestibular anatomy and function in this specific population.
The most widely accepted theory on IEM is that different subtypes arise from various interruptions along a linear developmental model of inner ear organogenesis. 5 Having undergone several revisions, the latest classification has 8 subtypes based on cochlear morphology: complete labyrinthine aplasia, rudimentary otocyst, cochlear aplasia, common cavity, cochlear hypoplasia (CH), incomplete partition type 1 (IP1), IP2, and IP3.6,7 Though vestibular abnormalities are posited to have frequent concurrence with cochlear anomalies due to their closely interlocked embryologic development and anatomy, only 2 studies have examined the vestibular abnormalities in patients with IEM,8,9 and the association between vestibular malformation and vestibular function has not been well established. In our institute, we have routinely examined the preoperative vestibular function of cochlear implant candidates, including those with vestibular or cochlear anomalies. From these data, we explore the association between vestibulocochlear anatomy and vestibular function test results in children with IEM.
Methods
This case series with chart review was approved by the Institutional Review Board of the University of Tokyo. Charts were reviewed of all pediatric patients with IEM who had bilateral profound hearing loss and were candidates for cochlear implantation at the university hospital from January 1999 to October 2017. All patients had prior cervical vestibular evoked myogenic potential (cVEMP) testing, rotational chair testing, and caloric testing for routine preoperative evaluation. Those with incomplete records and results were excluded.
Vestibular Function Tests
Cervical Vestibular Evoked Myogenic Potential
Subjects were instructed to raise their heads from a supine position to activate the sternocleidomastoid muscle. The active electrode was placed on the superior half of the sternocleidomastoid muscle, the reference electrode on the upper sternum, and the ground electrode on the forehead. Electromyographic activity ≥150 μV confirms sufficient normal muscle activity. Stimuli presented through calibrated headphones (DR-531; Elega Acoustic) consists of 500-Hz tone bursts (95 dB nHL). Electromyographic signals were amplified with Neuropack Sigma (Nihon Kohden). cVEMPs were recorded twice in response to 100 stimuli and averaged. cVEMP findings were present when there was a reproducible short-latency biphasic wave, absent when there was none, and poor if asymmetry was noted.
Rotational Chair Test
Children were seated upright with heads bent down at a 30° angle. The rotational chair was accelerated to a maximum rotational velocity of 200 deg/s with a maximum acceleration of 300 deg/s2. The test was conducted twice in clockwise and counterclockwise directions, and eye movements were recorded by electronystagmography. The number of beats per rotatory nystagmus was measured and compared with those of previously published age-matched pediatric controls recorded in our laboratory. 9 Results were considered normal if the number was ≥23, decreased if <23, and absent if no nystagmus was elicited.
Caloric Test
Horizontal and vertical eye movements were recorded via electronystagmography after application of 4 °C water on an intact eardrum. Duration of induced nystagmus was compared with age-matched pediatric controls as published by Inoue et al 9 ( Table 1 ). Findings were recorded as normal if the duration of induced nystagmus was within normal limits of age-matched controls, decreased if >2 SD smaller than the average value at each age, or absent if no nystagmus was elicited.
Duration of Induced Nystagmus in 112 Age-Matched Pediatric Controls. a
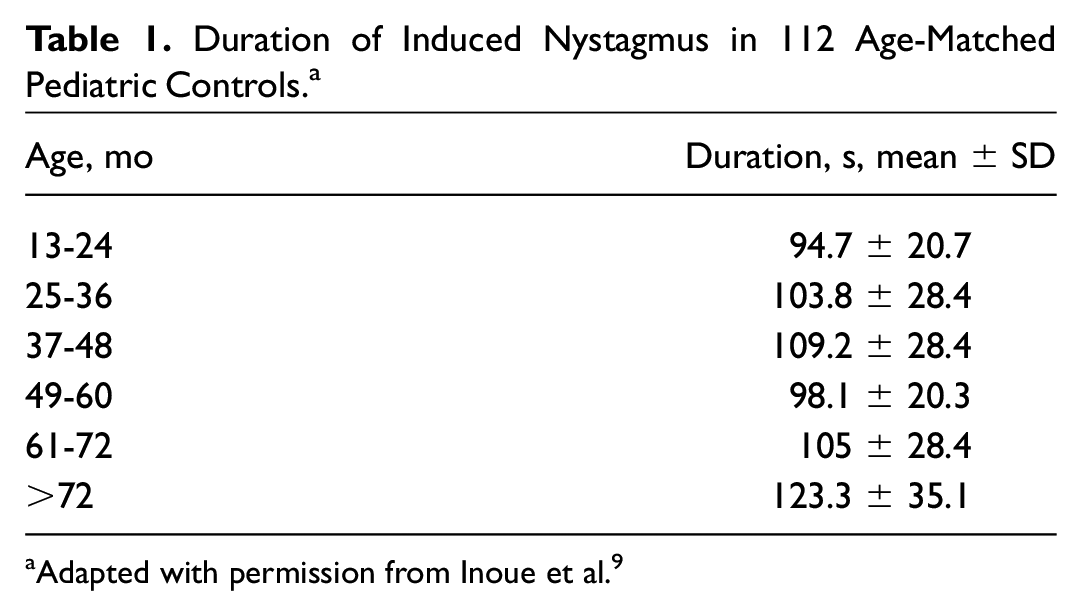
Adapted with permission from Inoue et al. 9
Vestibular Symptomatology
Age of achieving neck stability and age of initial independent walking were used as indicators of gross motor development. Delayed motor development was defined as attaining head control later than 4 months of age and achieving independent walking later than 15 months of age. 9 The average ages of patients with abnormal cVEMP, rotational chair, and caloric test results were compared with those of patients with normal test results.
Imaging Studies
High-resolution images were obtained with either a 4–detector row computed tomography (CT) scanner (0.5-mm width, 120 kV, 200 mA; Toshiba Aquilon 16) or a 320–detector row CT scanner (0.5-mm width, 120 kV, 100 mA; Toshiba Aquilon ONE), with reconstruction spacing of 0.1 mm. Evaluation of images was performed by 3 otologists at a GE Medical Systems Advantage Workstation, and measurements were made with images enlarged 10 times by using the hospital picture archiving and communication system.
The appearance of the semicircular canals (SCCs) was determined (normal, dysplastic, or aplastic). For the vestibule, the greatest craniocaudal (A), transverse (B), and anteroposterior (C) diameters were measured and approximate volume mathematically computed with the formula for ellipsoid volume: 4/3π× (A/2) × (B/2) × (C/2). The volumes were compared with age-matched vestibule volumes of pediatric patients with normal hearing, vestibular testing, and CT imaging findings. Cochlear malformations were classified according to the latest classification system. 7
Statistical Analysis
Descriptive and inferential statistics were calculated, including the association between vestibule volume and cVEMP, lateral SCC and caloric test, and lateral SCC and rotatory chair test. Descriptive summary measures for continuous variables were presented in terms of mean and standard deviation, and for categorical variables, summaries were presented in frequency counts and proportions. Chi-square test and Mann-Whitney U test were used to identify differences in outcomes and clinical predictors, as appropriate for the distribution of the data. All data were encoded in Microsoft MS Excel version 16 and statistical analyses performed with SPSS version 22 (IBM). All hypothesis tests used an α level of significance of 0.05.
Results
Out of 48 pediatric patients with IEM, 41 were included in the study. Seven were excluded due to incomplete vestibular test results. Each ear was treated as a single sample, for a total of 82 ears. The average age was 43 months (range, 12-196 months). There were 20 males and 21 females. The vestibular test results of 66 ears from 33 patients with GJB2 gene mutation were analyzed for comparison.
The ears were grouped according to the latest IEM classification, 7 except for 17 ears with an anomalous vestibular organ (consisting of at least a vestibule abnormality or an SCC abnormality) and normal cochleae, which did not fit into any of the predefined classifications ( Table 2 ). These were grouped separately into the category of vestibular organ malformation. The most frequent classification was IP2 (29.3%), in which the apical part of the modiolus is defective. 7 This is followed by isolated vestibular organ anomaly (20.7%) and IP1 (18.3%).
Types of Inner Ear Malformations.
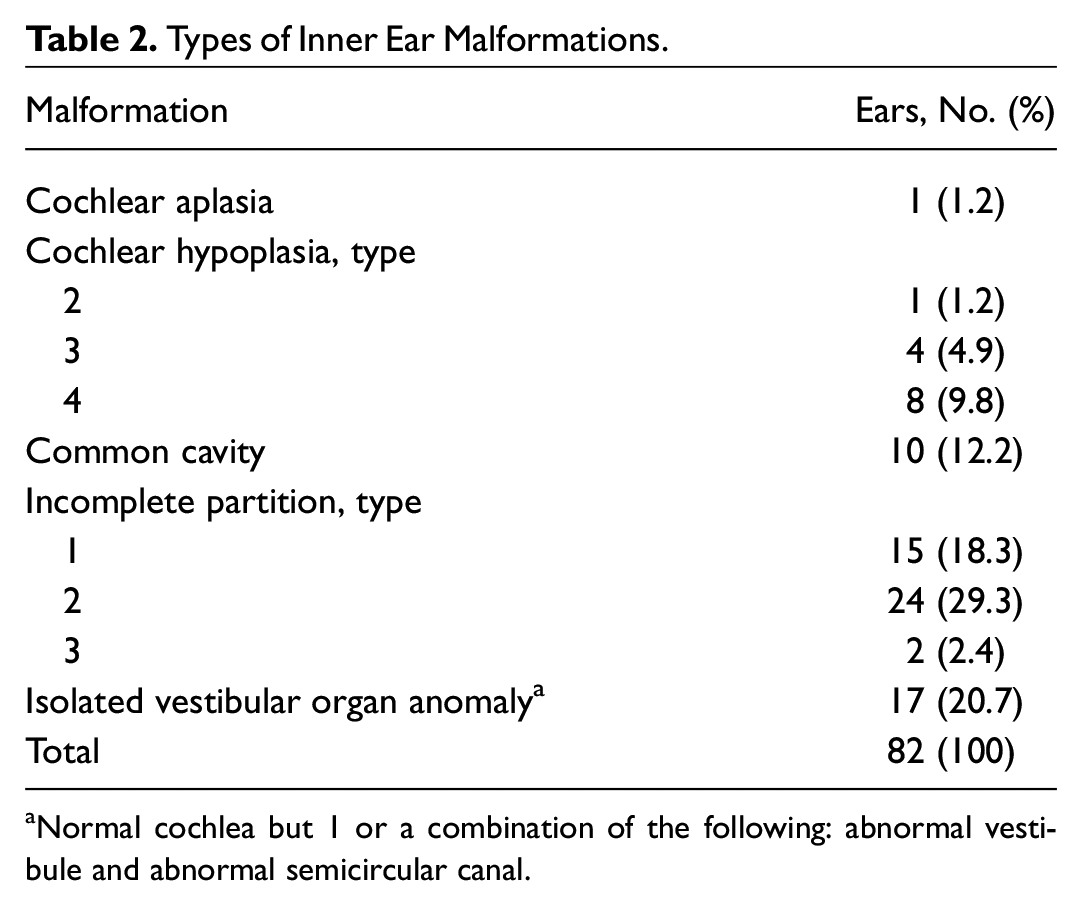
Normal cochlea but 1 or a combination of the following: abnormal vestibule and abnormal semicircular canal.
A total of 61 ears (74%) showed vestibular organ anomalies. Of these, 48 ears had abnormal vestibules, 45 had abnormal lateral SCCs, 27 had abnormal posterior SCCs, and 25 had abnormal superior SCCs. The CT imaging findings of the vestibular organs in various Sennaroglu classifications are tabulated in Supplement A (available online).
Among 65 ears with various cochlear malformations, 39 (60%) had coexisting vestibular organ malformation. Within the 8 subgroups of cochlear malformations, 5 groups had more ears with coexisting vestibular organ abnormalities than without. The CH type 3 (CH3) group had an equal number of normal and abnormal vestibules, and the IP2 and IP3 groups had more normal vestibules than abnormal ones. The IP1 and CH4 groups had dilated vestibules and enlarged cochlear basal turns. Patients with CH2, CH3, and IP3 had smaller cochlear basal turns and smaller vestibules.
Radiologic evaluation of the SCCs is shown in Figure 1 . Based on the mean vestibule volume of 54.4 mm3 and a standard deviation of 16.1 obtained from 15 age-matched pediatric control ears, cutoff values were estimated as follows: those <38.3 mm3 were considered small, 38.3 to 70.5 mm3 normal, and >70.5 mm3 dilated. This yielded 34 ears (41.5%) with normal vestibule volumes, 36 ears (43.9%) with dilated vestibules, and 12 ears (14.6%) with small vestibules. Mean vestibule volume was 75.5 ± 42.6 mm3. Figure 2 shows the various Sennaroglu subclassifications divided into varying vestibule volumes.
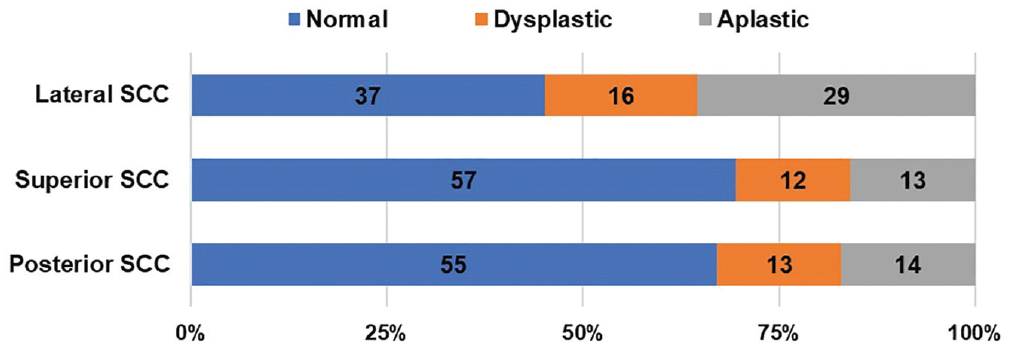
Radiologic characteristics of the semicircular canals (SCCs).
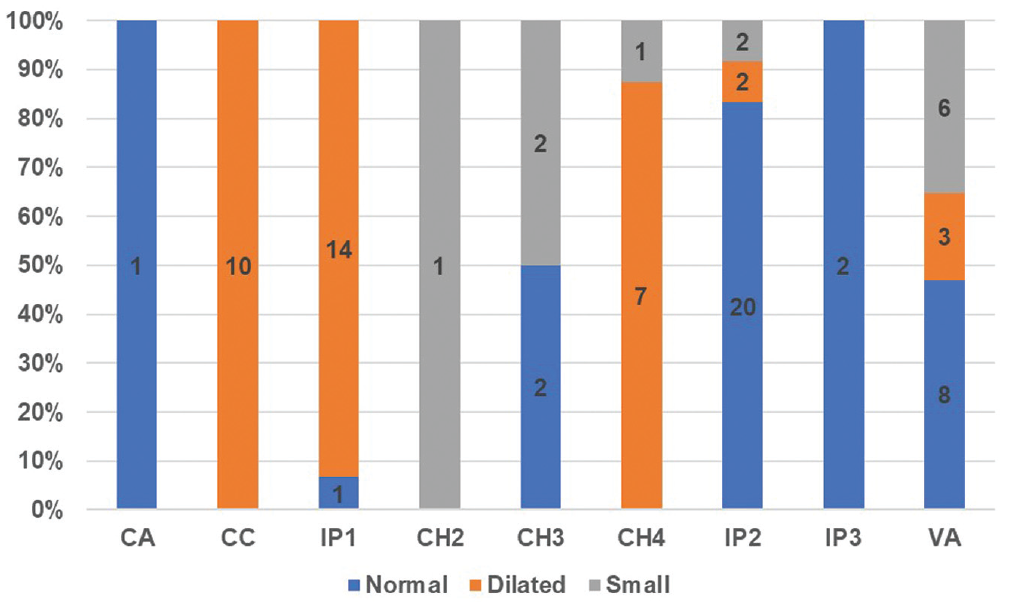
Vestibular volume in various Sennaroglu subclassifications. CA, cochlear aplasia; CC, common cavity; CH, cochlear hypoplasia; IP, incomplete partition; VA, vestibular abnormality.
Most of our population had an abnormal response on cVEMP testing (58 ears, 71%). On caloric testing, 23 (28%) had a normal response, 11 (13%) had a decreased response, and 48 (59%) had no response. Rotatory chair testing yielded 22 ears (27%) with a normal response, 28 (34%) with a decreased response, and 32 (39%) with no response. In comparison, in the GJB2 gene mutation group, 27% (18 of 66 ears) had no cVEMP response, 20% (13 of 66 ears) had an abnormal caloric response, and 2% (1 of 66 ears) had no rotatory chair response.
cVEMP test results in Sennaroglu subclassifications are shown in Figure 3 . Vestibular test results of each group of IEM are shown in Appendix B (available online). Figure 4 shows that all ears with small vestibule volumes and a majority of ears with dilated vestibules showed absent cVEMP response. Abnormal vestibule volume was significantly associated with a nonreactive cVEMP finding (odds ratio, 24.23 [95% CI, 6.231-94.233]; χ2[4, N = 82] = 30.09, P < .001). The caloric and rotatory chair test results were cross-tabulated with lateral SCC structural classifications ( Figure 5 ). All patients with dysplastic or aplastic lateral SCCs had abnormal results in the caloric and rotatory chair tests. The association between radiologically abnormal lateral SCCs and abnormal caloric and rotatory chair test results was statistically significant (P < .001 for both tests).
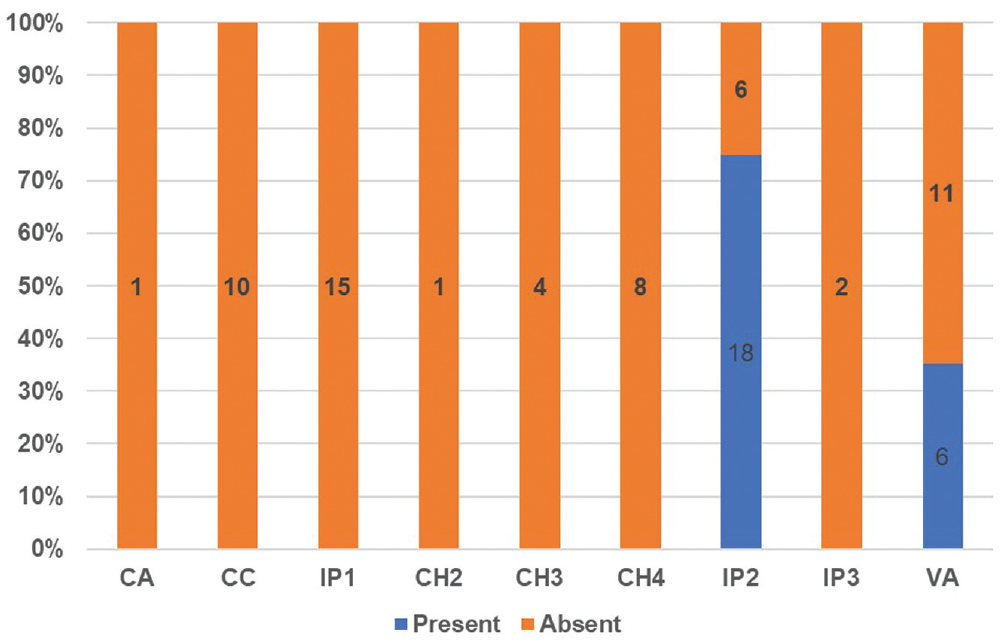
Cervical vestibular evoked myogenic potential test results of various Sennaroglu subclassifications. CA, cochlear aplasia; CC, common cavity; CH, cochlear hypoplasia; IP, incomplete partition; VA, vestibular abnormality
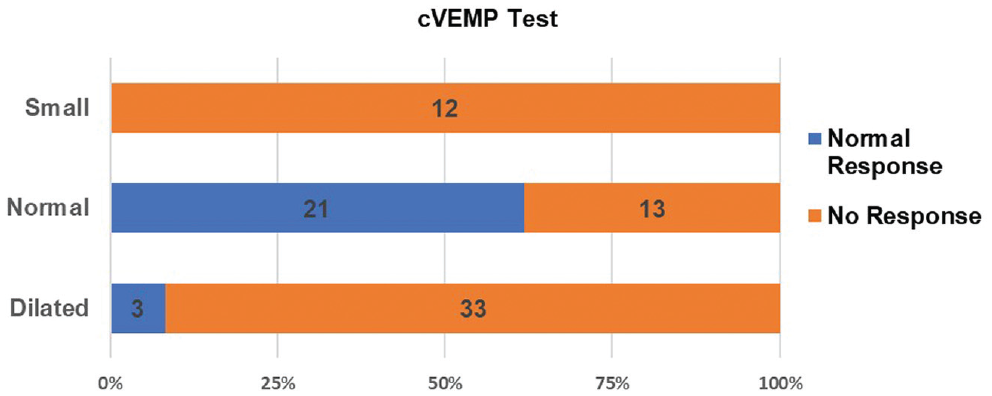
Comparison of vestibular volume with cervical vestibular evoked myogenic potential (cVEMP) results.
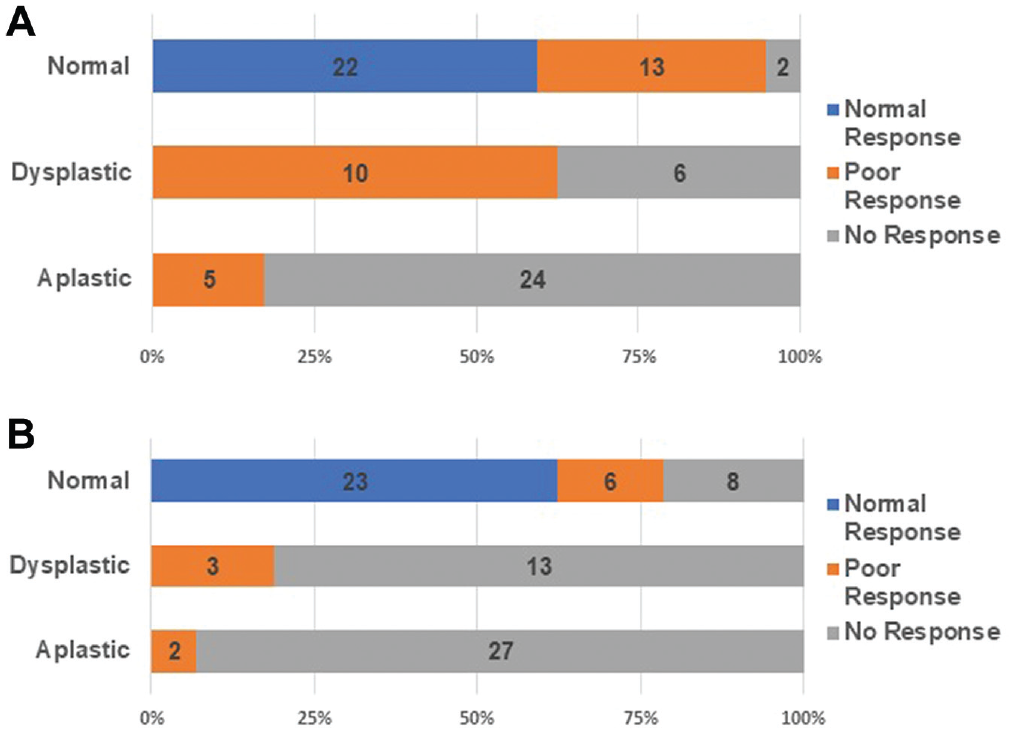
Association between lateral semicircular canal radiologic anatomy (normal, dysplastic, or aplastic) and (A) rotatory and (B) caloric test results (normal, poor, or no response).
Of the 41 children in this total population, head control and independent walking were delayed in 14 (34.1%) and 12 (29.3%), respectively. The average ages at which head control and independent walking were observed in patients with abnormal rotatory chair, caloric, and cVEMP test results were all significantly higher than those in patients with normal test results ( Table 3 ).
Age of Achieving Neck Stability and Independent Walking Between Patients With Normal and Abnormal Vestibular Test Results.
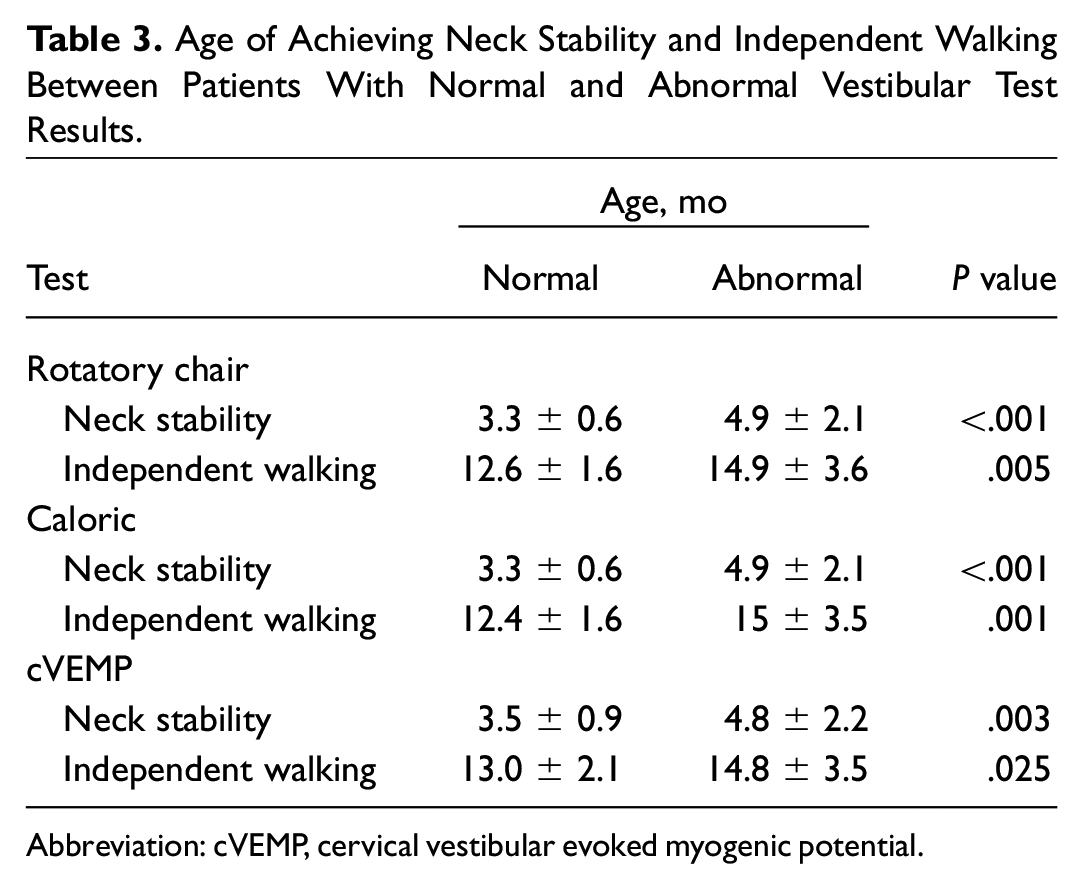
Abbreviation: cVEMP, cervical vestibular evoked myogenic potential.
Discussion
In this study, we classified all ears according to currently accepted types of IEM, and we explored the association between these anatomic abnormalities and vestibular function. We demonstrated that vestibule volume was closely related to cVEMP results. To our knowledge, this is the first study to show the relationship between anatomic patterns and vestibular function in IEM. We also explored the association between cochlear and vestibular malformation and found that anomalies of the cochlear basal turn and vestibule were closely related.
In our population of 82 ears, the most frequent type of IEM was IP2 (29.3%). Characterized by a normal proximal basal turn and a deficient interscalar septum between the upper 2 turns of the cochlea, this malformation was also the most common in previous studies.10,11 Second in frequency were ears with isolated vestibular organ anomalies (vestibule and/or SCC) without coexisting cochlear malformations (20.7%), which could not be classified into any of the currently accepted categories of IEM. While the classification of IEM was initiated by Jackler et al and revised several times by Sennaroglu and Saatci, comprehensively summarized categories of IEM have been created according to cochlear abnormalities. Vestibular abnormalities with no accompanying identifiable cochlear anomalies have been notably excluded.5,6 Because a relatively large number of cases of isolated vestibular anomalies have been reported not only in our study but in previously published articles (23%-36% of IEM cases),10,11 we suggest that this category of anomaly be added to the subsets of IEM to establish an all-encompassing classification system.
The majority of ears (74%) in our population showed vestibular organ anomalies. Furthermore, among 65 ears in the 8 groups with various cochlear malformations, the majority (60%) had coexisting vestibular organ malformation. Notably, however, the IP2 and IP3 groups had lower frequencies of abnormal vestibular organs, and the CH3 group had an equal number of normal and abnormal vestibular organs. The human labyrinth undergoes a number of complex changes during fetal life and attains an adult-equivalent size between 17 and 19 weeks’ gestation. 12 It becomes fully encapsulated by bone a few weeks later. We speculate that the CH3, IP2, and IP3 abnormalities may arise after the critical period of vestibular development.
The IP1 and CH4 groups, which had dilated vestibules, also had dilated or normal cochlear basal turns. Meanwhile, the CH2 and CH3 groups, which had small cochlear basal turns, also had small vestibules. These data suggest that vestibule volume may be related to cochlear basal turn size. The auditory part of the ear is known to evolve from vestibular organs. 13 As the embryonic origins of the cochlea and the vestibule are identical, they are affected by similar mechanisms, resulting in the similar trends of malformation.
There were 51 ears (62%) with SCC malformation. Among them, the most frequently affected was the lateral SCC. Embryologically, the superior SCC is the first SCC to form, achieving an adult size at 26 weeks, followed by the posterior and then the lateral SCC at 27 weeks. 14 Therefore, superior and posterior SCC anomalies are almost invariably associated with anomalies of the lateral SCC, while abnormalities of the lateral SCC may occur in isolation. 15 A study revealed that the type and severity of SCC malformation had no correlation with any specific audiologic outcome. 16 The independent development of individual SCCs in relation to the cochlea and vestibule, as well as the variability in hearing loss, suggests a more complex embryologic process than merely an arrest in development. 16
In our population, the majority of ears with IEM had abnormal vestibular function (71% with negative cVEMP result, 72% with abnormal caloric test result, and 73% with abnormal rotatory chair test result). Furthermore, abnormal vestibular function was associated with delayed achievement of head control and independent walking ( Table 3 ). A recently published study demonstrated an association among IEM, vestibular dysfunction, and delayed gross motor development and stressed the often-overlooked impact of the vestibular component of IEM. 11 A few other studies examined vestibular function in children with hearing loss, and the frequency of abnormal vestibular function test results in these studies ranged from 22.5% to 67.5%.8,17 This wide variability in vestibular function may be attributed to differences in etiology of the hearing loss.
To establish the reliability of our vestibular test results, we analyzed the results of our patients with a GJB2 gene mutation and radiologically normal inner ear anatomies and noted far fewer cases of abnormal vestibular function (27% with negative cVEMP result, 20% with abnormal caloric test result, and 2% with abnormal rotatory chair test result). This low proportion was similar to existing literature,18,19 supporting the reliability of our testing. These particular patients were selected as comparison since they also had profound hearing loss but normal radiologic anatomy and they had available vestibular testing data. Though patients who have normal hearing and vestibular function would be ideal, these patients do not readily undergo imaging studies.
We observed a clear association between abnormal vestibule volume and abnormal cVEMP function in cases of IEM. All ears with a small vestibule volume and a large majority of ears with dilated vestibules showed absent cVEMP response. In evaluating the size of vestibules, we used a novel method of computing for volume, instead of using 2-dimensional measurements such as length and width, as reported in previous studies.20,21 We obtained 3-dimensional quantitative measurements—craniocaudal, transverse, and anteroposterior diameters—and computed for vestibule volume using the formula for an ellipsoid. With this method, we demonstrated a significant association between vestibule volume and function.
In the current study, 38% of radiologically normal vestibules had abnormal cVEMP results ( Figure 4 ). Studies conducted on patients with cochlea-saccular dysplasia noted that the hair cells in the saccule could be abnormal even when the osseous labyrinth, membranous utricle, and SCCs were normal. 22 These findings imply that various factors other than structural abnormalities could affect vestibular function, including genetic abnormality, electrolyte imbalance, and vestibular neuropathy. 23
All patients with normal caloric and rotatory chair test results had radiologically normal lateral SCCs, and all dysplastic and aplastic lateral SCCs showed abnormal vestibular function test results. However, not all radiologically normal lateral SCCs had normal caloric and rotatory chair test findings; caloric and rotatory chair tests were abnormal in 14 and 15 of 37 ears, respectively, reiterating that structural integrity does not necessarily imply intact function.
Several cases of aplastic lateral SCCs showed some response, albeit poor, in rotatory chair (5 ears) and caloric (2 ears) tests. This was unexpected because, theoretically, cases of lateral SCC aplasia should show complete absence of response. While this may have been due to intrinsic errors in these diagnostic tests, another possible reason is that the ampulla of these ears may have been intact despite the absence of the bony canal. Brainstem structures of the vestibular pathway start functioning between 19 and 21 weeks, 24 long before complete ossification of the SCCs is achieved at 27 weeks. 14 If the arrest or interruption in development occurs after the ampulla has formed but before the bony lateral SCC has developed, some function could be present, resulting in a weakly positive vestibulo-ocular reflex.
This study is limited by the small population size. Furthermore, the sampling frame may not adequately represent all malformed inner ears, as our participants were limited to those who consulted at our institution for cochlear implantation, and patients with normal to moderate hearing loss were excluded. Additionally, the patient population had a wide age range, and this could influence our results. Some children were excluded from this study because they could not follow instructions or complete the examination. Finally, we could not assess clinical vestibular symptoms because these were not well documented in the chart. Correlation between vestibular function test results and patients’ clinical symptoms should be explored in a future study.
Conclusion
Among patients with IEM, isolated vestibular organ anomaly without coexisting cochlear malformations is the second-most frequent type of malformation, and this type is not included in currently accepted categories. With a large number of cases reported not only in our study but also in previously published articles,10,11 we suggest that this category be added to the subsets of IEM to establish an all-encompassing classification system for IEMs.
We showed a clear association between an abnormal vestibule volume and a nonreactive cVEMP finding and that majority of patients with hearing loss secondary to IEM have abnormal vestibular function test results.
Author Contributions
Disclosures
Supplemental Material
sj-docx-1-opn-10.1177_2473974X221128912 – Supplemental material for Vestibular Imaging and Function in Patients With Inner Ear Malformation Presenting With Profound Hearing Loss
Supplemental material, sj-docx-1-opn-10.1177_2473974X221128912 for Vestibular Imaging and Function in Patients With Inner Ear Malformation Presenting With Profound Hearing Loss by Alexander Edward S. Dy, Akinori Kashio, Chisato Fujimoto, Makoto Kinoshita, Yayoi S. Kikkawa, Yujiro Hoshi, Kazunori Igarashi, Tsukasa Uranaka, Shinichi Iwasaki and Tatsuya Yamasoba in OTO Open: The Official Open Access Journal of the American Academy of Otolaryngology-Head and Neck Surgery Foundation
Footnotes
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
