Abstract
Objective
This study aims to assess trends in applicant-reported costs of the otolaryngology residency application process between 2019 and 2021 and evaluate the impact of application costs on number of interview offers.
Study Design
Cross-sectional study.
Setting
US allopathic and osteopathic medical schools.
Methods
Survey data from applicants were obtained from the Texas STAR database (Seeking Transparency in Application to Residency) for the years 2019 to 2021. Outcomes included total cost, interview cost, other costs, application fees, and number of interview offers. Simple and multivariable linear regression was used to identify novel predictors of cost and assess the correlation between cost and interview offers.
Results
Among 363 otolaryngology applicants, there was a 74% reduction in total costs and a 97% reduction in interview costs in the 2021 cycle vs the 2020 cycle. Significant predictors of total cost among otolaryngology applicants included the number of away rotations (P < .01), the number of research experiences (P = .04), and couples matching (P < .01). During the 2019 and 2020 application cycles, there was a significant association between applicant-reported total spending and number of otolaryngology interview offers (P < .01), which was not present during the 2021 cycle (P = .35).
Conclusion
Number of otolaryngology interview offers appears to be directly correlated with applicant-reported total costs regardless of number of applications or interviews attended, which may be a source of inequality in the application process. There was a drastic reduction in total costs, interview costs, and other costs during the COVID-19 pandemic, which was likely driven by virtual interviewing and the absence of away rotations.
The cost of medical education is a significant burden for medical students, residents, and physicians in the United States. The Association of American Medical Colleges reports that among graduates of medical school in 2021, 73% had education-related debt and the average debt was $203,062. 1 While much of medical school debt is attributable to tuition expenses, students accrue a reasonable amount during the residency application and interview process. 2 During the residency application process for competitive specialties, students often complete subinternships at away institutions, where they are responsible for expenses related to travel, temporary housing, and food. 3 This is followed by the Electronic Residency Application Service, where students pay a flat $99 fee for their first 10 applications and an additional fee per each extra application submitted (herein, application fee). 4 This is of particular importance in competitive specialties such as otolaryngology, where students submitted an average of 77 applications during the 2020-2021 cycle. 5 Prior to the 2020-2021 match cycle, applicants also accrued travel and lodging costs for their in-person residency interviews.
The high cost of the residency application cycle is important in the context of promoting diversity, equity, and inclusion (DEI) within the field of otolaryngology. Reducing this cost may help with the recruitment and retention of a diverse workforce that is better able care for an increasingly diverse patient population.6,7 There is valid concern that the high costs of residency application may serve as a barrier for students of lower socioeconomic backgrounds who are more frequently from marginalized communities. 8 In one survey of otolaryngology applicants, 28% reported that they had insufficient funds for the residency application process. 2
The COVID-19 pandemic resulted in major disruptions to the residency application process, including the cancellation of away rotations and in-person interviews, which were replaced with virtual alternatives during the 2021 application year.9,10 Virtual alternatives to interviews and in-person subinternships may help mitigate some of the cost-related barriers faced by otolaryngology applicants, although more research is needed to quantify the impact of these changes.
This study aims to assess trends in the cost of the otolaryngology residency application process from 2019 to 2021 with attention paid to the impact of COVID-19. We further hope to identify drivers of cost among otolaryngology applicants, assess differences in costs among specialties, and evaluate the impact that costs have on number of interview offers and match success. The results of this study may help inform future decision making to create a more affordable and equitable application process for otolaryngology applicants in future cycles.
Methods
Data and Sample
Data were sourced from the Texas STAR survey (Seeking Transparency in Application to Residency). The Texas STAR survey contains self-reported deidentified information from residency applicants for the 2018, 2019, 2020, and 2021 match years. 11 The Texas STAR survey is distributed to fourth-year medical students in the United States, including allopathic and osteopathic programs, by the dean of student affairs of the medical school between match day and April 10 of each application cycle. Applicants are instructed to report application data as they appeared on their residency application. Applicants were included in this study for the 2019, 2020, and 2021 match years, due to cost data not being available for the 2018 match cycle; overall survey response rates were 38%, 47%, and 40%, respectively. Participation in the survey was completely voluntary, use was explained to participants, and participation served as consent for data collection. This study was exempt from University of Michigan institutional review board approval.
Variables
Applicant-level variables were as follows: applied specialty, match status, USMLE board scores (in 5-point intervals; United States Medical Licensing Examination), honors society memberships, class ranking (cumulative quartile of medical school class), number of clerkship honors, honors in applied specialty, number of away rotations, research output, leadership experiences, volunteer experiences, research year, leave of absence, couples match, other degree obtained, and costs. Costs included total cost, application fees, interview costs, and other costs. Costs were reported in $500 intervals for the 2019 and 2020 application cycles and $100 intervals for the 2021 application cycle. Other costs were those associated with the application that were not application fees or interview-related costs; participants were instructed to include away rotation costs in this category. Demographic data such as age, sex, race, and home medical school were not collected to protect applicant confidentiality. USMLE scores and costs were centered for the analysis (ie, 220-224 was centered at 222 for USMLE scores and $5000-$5500 was centered at $5250 for cost).
Statistical Analysis
Wilcoxon rank sum testing with Dwass-Steel-Critchlow-Flinger post hoc analysis was used to compare costs between the 2019 and 2020 application cycles and the 2021 application cycle. Applicant-level predictors of total cost among otolaryngology applicants were assessed via unadjusted ordinary least squares (OLS) regression ( Table 1 ). Analyses in Tables 2 to 4 were stratified into the 2019 and 2020 application cycles and the 2021 application cycle to better assess the impact of application and interview changes in the setting of the COVID-19 pandemic. Comparisons between surgical subspecialties and general surgery/nonsurgical specialties were obtained with OLS regression with least square mean estimations. Surgical subspecialties and nonsurgical specialties are outlined in Supplemental Table S1 (available online). Multivariable OLS regression adjusting for number of interviews attended and number of programs applied to was used to assess the impact of total cost on the number of interviews offers received among otolaryngology, surgical subspecialty, general surgery, and nonsurgical applicants. The impact that total cost had on match success was assessed with unadjusted logistic regression. All statistical analyses were carried out at a significance criterion of P < .05, and 2-sided testing was used. SAS version 9.4 (SAS Institute) was used for all analysis.
Simple OLS Regression of Applicant-Level Predictors of Total Cost Among Otolaryngology Applicants (N = 363).
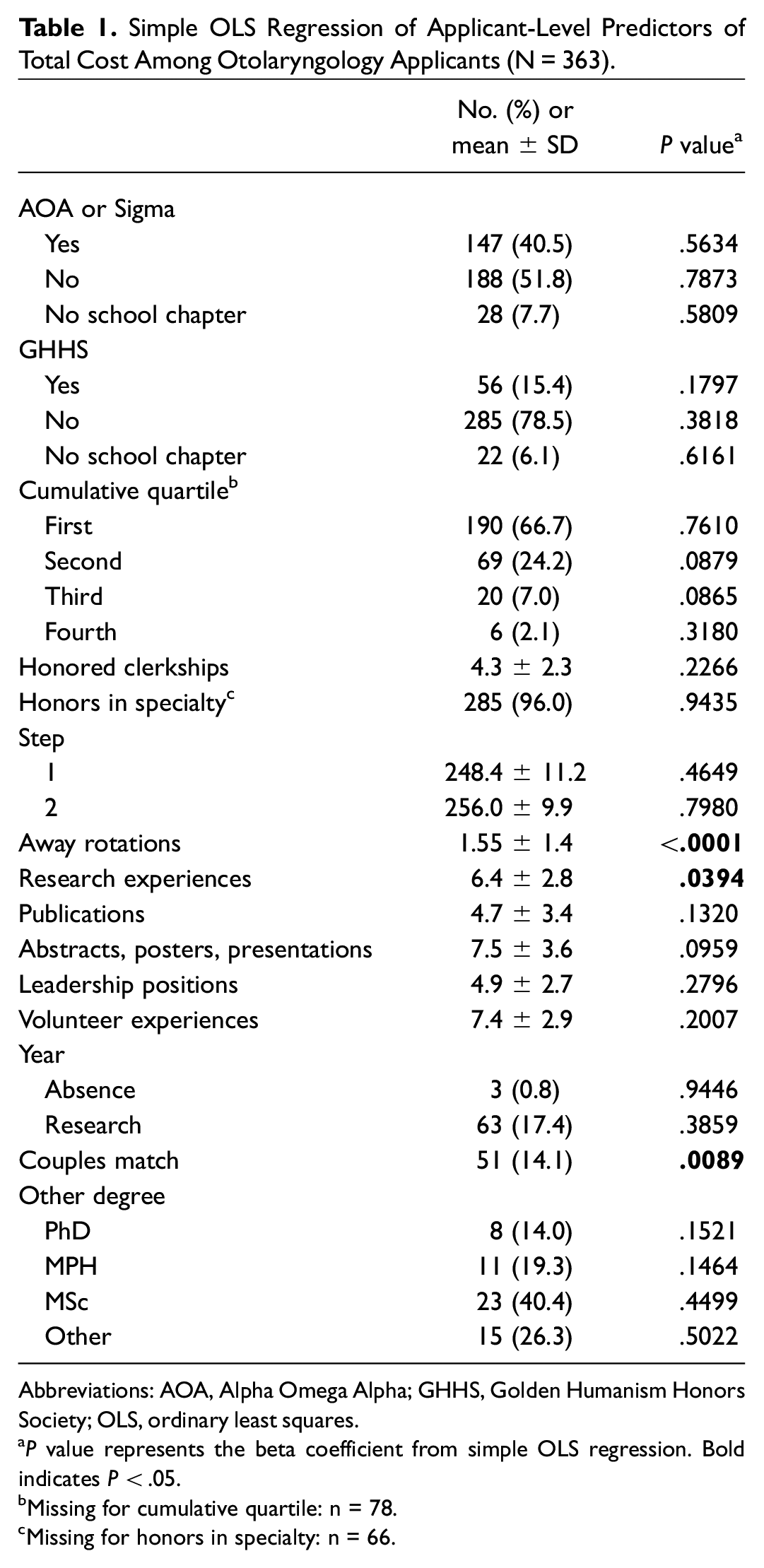
Abbreviations: AOA, Alpha Omega Alpha; GHHS, Golden Humanism Honors Society; OLS, ordinary least squares.
P value represents the beta coefficient from simple OLS regression. Bold indicates P < .05.
Missing for cumulative quartile: n = 78.
Missing for honors in specialty: n = 66.
Costs of the Surgical Subspecialty Application Process vs General Surgery and Nonsurgical Specialties. a
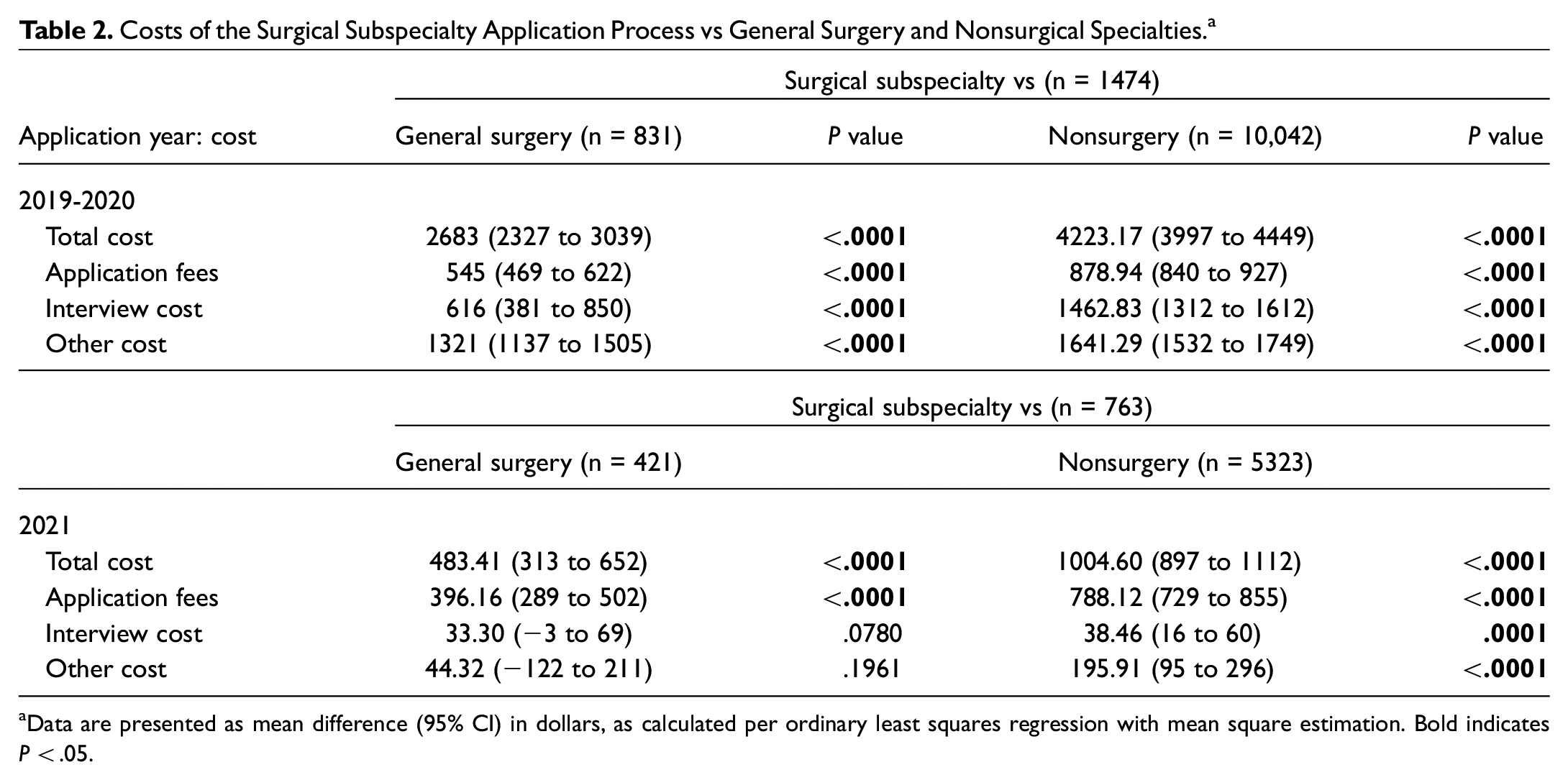
Data are presented as mean difference (95% CI) in dollars, as calculated per ordinary least squares regression with mean square estimation. Bold indicates P < .05.
Impact of Total Cost on Number of Interviews Offers Received. a
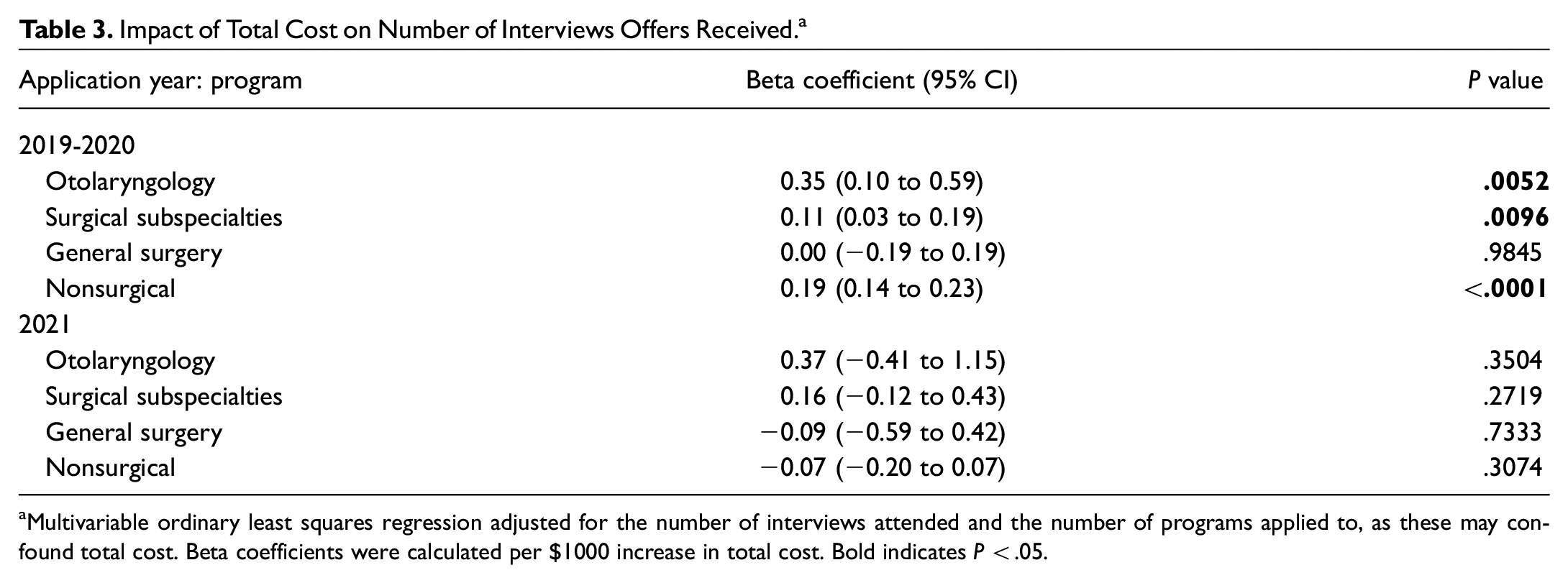
Multivariable ordinary least squares regression adjusted for the number of interviews attended and the number of programs applied to, as these may confound total cost. Beta coefficients were calculated per $1000 increase in total cost. Bold indicates P < .05.
Impact of Total Cost on Odds of Matching. a
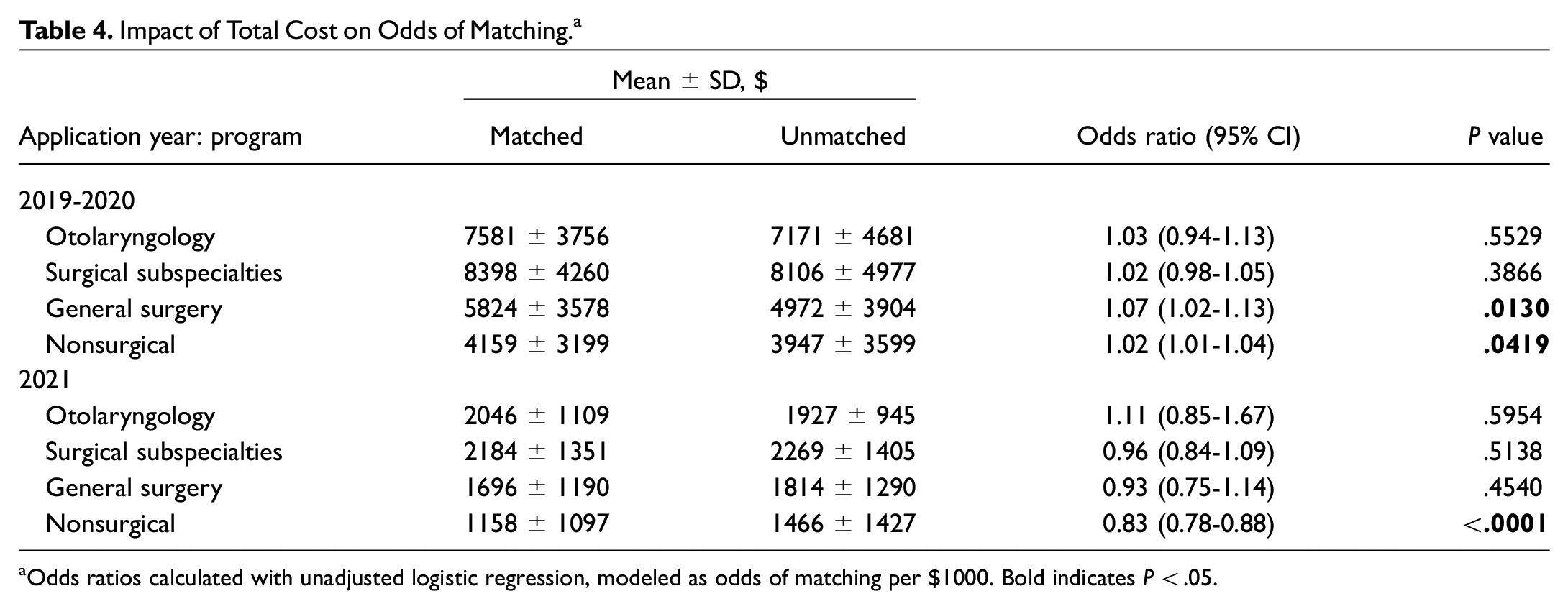
Odds ratios calculated with unadjusted logistic regression, modeled as odds of matching per $1000. Bold indicates P < .05.
Results
A total of 20,223 applicants completed the survey during the 2019, 2020, and 2021 application years. Of these applicants, 363 applied to otolaryngology. Among otolaryngology applicants responding to the survey, mean interviews received were 16.1 (SD, 9.3), mean interviews attended were 12.1 (SD, 5.0), and the match rate was 80.7%. Among all survey responders, mean interviews received were 16.4 (SD, 9.3), mean interviews attended were 12.3 (SD, 5.4), and the overall match rate was 87.3%.
Trends in Costs of Residency Applications
Among otolaryngology applicants, there was a 74% reduction in total costs ($7682 to $2013, P < .01), a 97% reduction in interview costs ($3593 to $105, P < .01), and a 74% reduction in other costs ($2551 to $667, P < .01) in the 2021 cycle as compared with the 2020 cycle. Application costs remained stable throughout the study period ($1519 to $1676 to $1644). There were no significant changes in total costs, interview costs, or other costs between 2019 and 2020 ( Figure 1A ; Supplemental Table S2, available online).
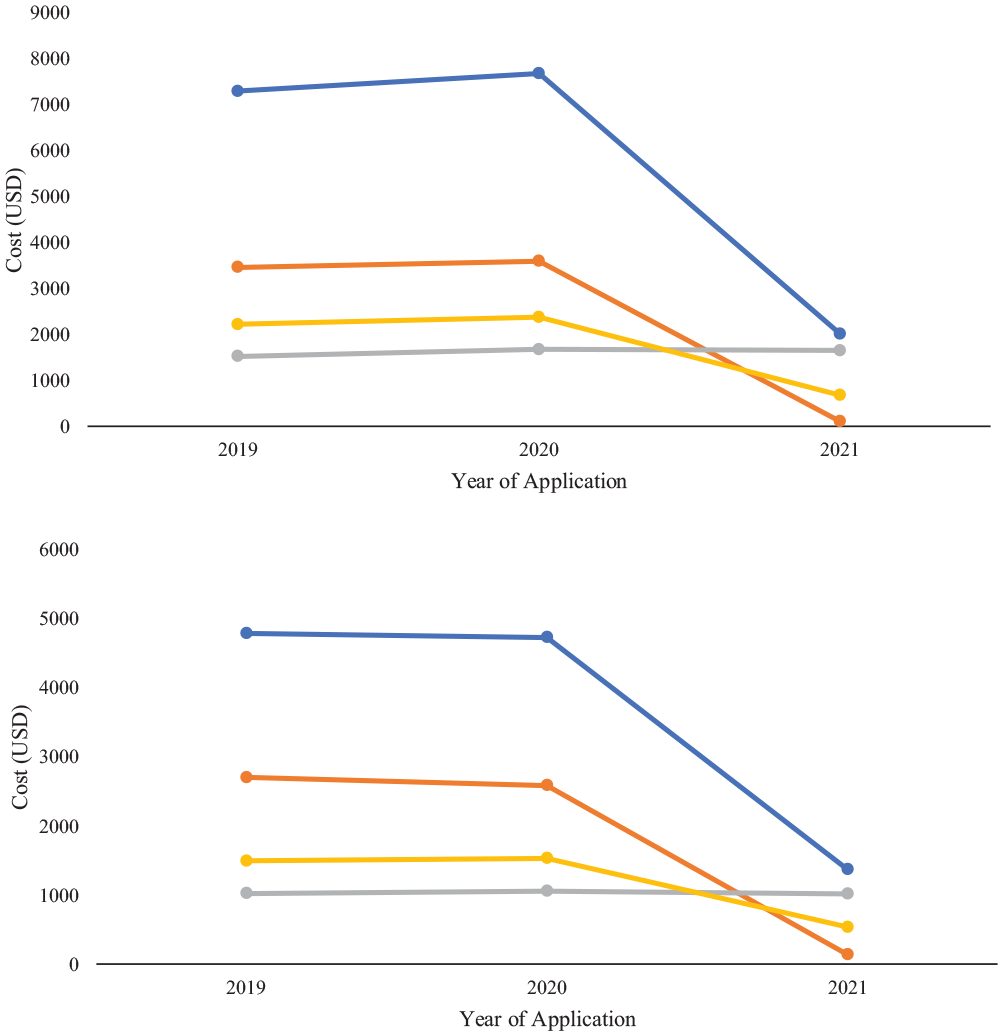
Top: trends in average cost among otolaryngology applicants between 2019 and 2021. Bottom: trends in cost among all applicants. Total cost, blue; interview cost, orange; application fees, gray; other cost, yellow.
Similar trends were reported among all applicants between 2020 and 2021: a 71% reduction in total cost (P < .01), a 94% reduction in interview costs (P < .01), a 64% reduction in other costs (P < .01), and a 3.6% reduction in application fees (P < .01). Between 2019 and 2020 there was a significant 4.4% decrease in interview costs (P = .02) and a 3.3% increase in application fees (P < .01) among all applicants. However, in the setting of our large sample size (n = 13,282), these differences represent small effect sizes ( Figure 1B ; Supplemental Table S3, available online).
Predictors of Total Cost Among Otolaryngology Applicants
Significant predictors of total cost among otolaryngology applicants included number of away rotations, number of research experiences, and participating in couples match, with applicants spending an additional $1622 per additional away rotation (95% CI, $579-$2663; P < .01), $163 per additional research experience (95% CI, $7-$329; P = .04), and an additional $1673 for couples match (95% CI, $422-$2925; P < .01). Other factors did not significantly affect total cost: honors society, class rank, clerkship and specialty honors, USMLE scores, research output, leadership and volunteer experiences, research year, leave of absence, or other degree ( Table 1 ; Supplemental Table S4, available online).
Comparison of Costs Among Specialties
During the 2019 and 2020 application cycles, applicants to surgical subspecialties reported higher total costs, interview costs, and other costs than applicants to general surgery and nonsurgical specialties ( Table 2 ). On average, applicants to surgical subspecialties spent $2683 (95% CI, $2327-$3039; P < .01) more than general surgery applicants and $4223 (95% CI, $3997-$4449; P < .01) more than applicants to nonsurgical specialties.
During the 2021 application cycle, applicants to surgical subspecialties reported higher total costs and application fees than applicants to general surgery ( Table 2 ). Furthermore, they noted higher total costs, application fees, interview costs, and other costs than applicants to nonsurgical specialties. On average, applicants to surgical subspecialties spent $483 (95% CI, $313-$652; P < .01) more than general surgery applicants and $1004 (95% CI, $897-$1112; P < .01) more than applicants to nonsurgical specialties in the 2021 cycle.
During the 2019 and 2020 application years, otolaryngology was the 10th-most expensive specialty to apply to, with an average total application cost of $7285 ( Figure 2 ). During the 2021 application cycle, otolaryngology was the eighth-most expensive specialty, with an average total application cost of $2013 ( Figure 3 ).
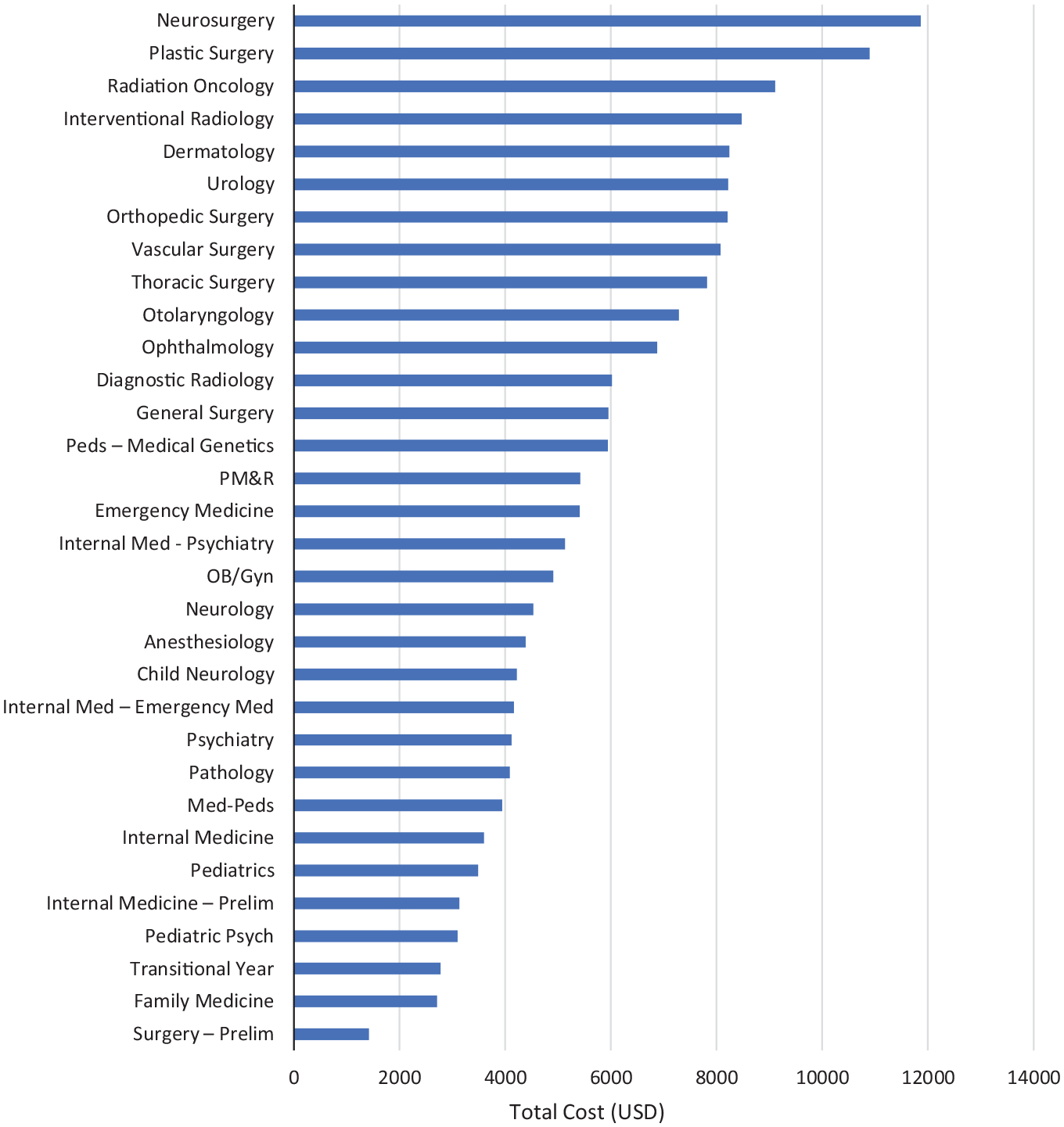
Average application cost by specialty: 2019-2020. PM&R, physical medicine and rehabilitation.
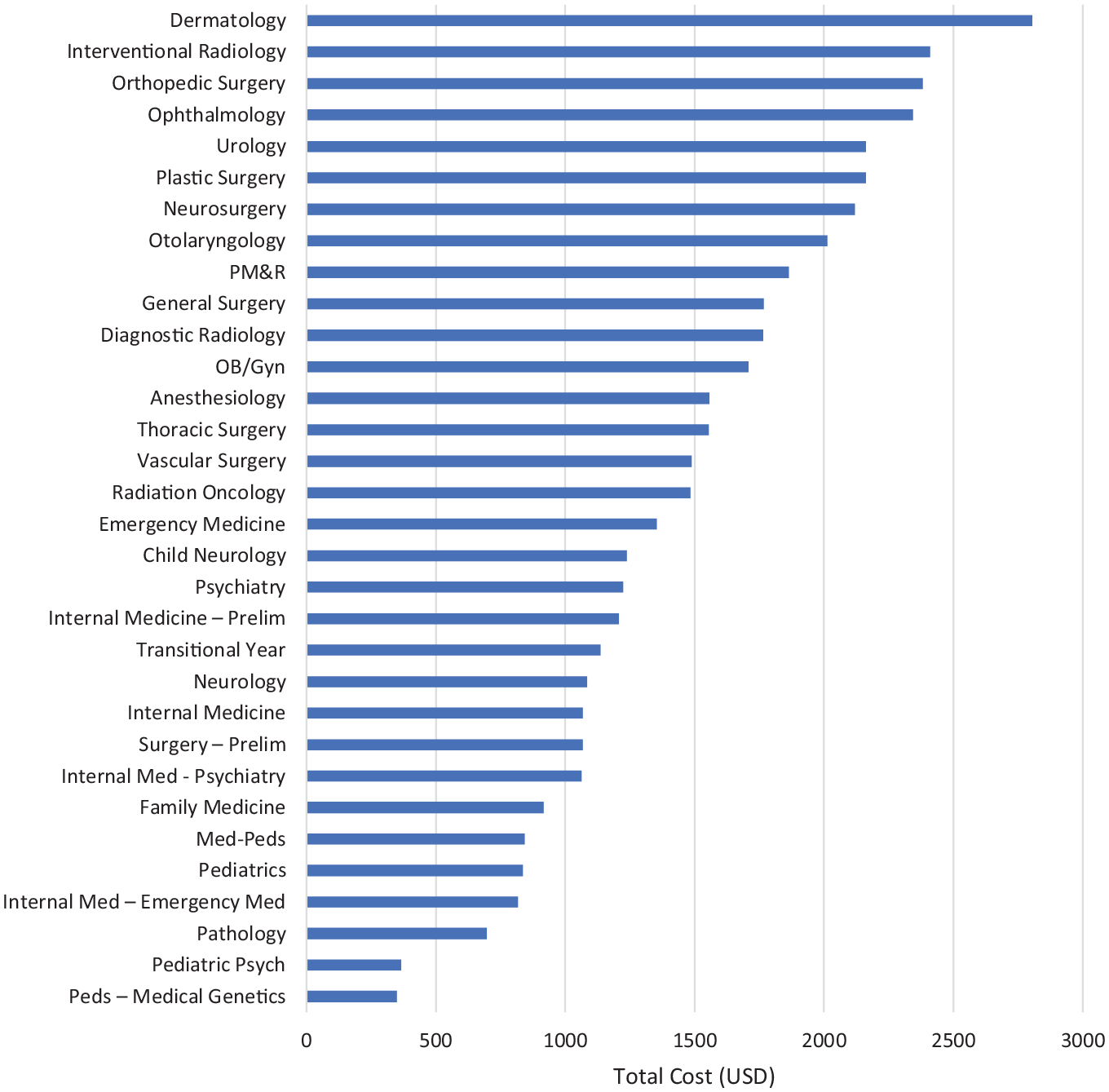
Average application cost by specialty: 2021. PM&R, physical medicine and rehabilitation.
Impact of Total Costs on Interview Offers and Matching
In OLS models adjusting for number of interviews attended and programs applied to, otolaryngology applicants on average received an additional 0.35 interviews (95% CI, 0.10-0.59; P < .01), surgical subspecialty applicants received an additional 0.11 interviews (95% CI, 0.03-0.19; P = .01) and nonsurgical applicants received an additional 0.19 interviews (95% CI, 0.14-0.23; P < .01) per $1000 spent in total cost. During the 2021 application cycle, there was no significant relationship between interview offers and total cost when adjusting for interviews attended and programs applied to among applicants to otolaryngology, surgical subspecialties, general surgery, or nonsurgical specialties ( Table 3 ).
Total costs were not significantly associated with odds of matching for otolaryngology applicants in either the 2019-2020 application cycle (odds ratio, 1.03 [95% CI, 0.94-1.13]; P = .55) or the 2021 application cycle (odds ratio, 1.11 [95% CI, 0.85-1.67]; P = .60) ( Table 4 ; Supplemental Tables S5 and S6, available online).
Discussion
In this study, we used the Texas STAR database to estimate trends in the cost of the otolaryngology residency application process, compare costs among specialties, and estimate the impact that the total cost of the application process had on obtaining interviews and matching. Our analysis showed a $5669 average total cost reduction for otolaryngology applicants during the 2021 application year, which was driven by a $3487 average decrease in interview costs and a $1884 average decrease in other costs. Average application fees remained stable. These findings highlight the significant savings that applicants experienced due to the implementation of virtual interviews and the cancellation of away rotations, which is consistent with previous findings from otolaryngology12,13 and other surgical subspecialties.14,15
We quantified several novel predictors of cost for otolaryngology applicants, including away rotations, couples matching, and number of research experiences. In this data set, otolaryngology applicants spent an additional $1622 per each additional away rotation. The cost of away rotations may be driving the association observed between total cost and number of interview offers received, as students completing away rotations may be more likely to get interviews at those programs.16-21 Applicants who participated in the couples match spent on average $1683 more than those who did not. This may be related to the general guidance to apply to a greater number of programs to improve the odds of match success when participating in the couples match.8,22 However, further study is warranted to better understand how doing fewer away rotations or applying to fewer programs affect match success among couples-matching students. Our finding regarding increased expenses with research experiences is likely related to the importance of research in a competitive application, with applicants with more research being more likely to obtain and therefore attend more interviews.16,23-26
Multiple studies have highlighted the high costs associated with applying to surgical subspecialties.2,14,27-30 Our study demonstrates significant cost savings for surgical subspecialty applicants during the COVID-19 pandemic, which appears to be driven by a lack of away rotations and interview-related travel. Our findings show that even though there were savings associated with the 2021 application cycle, surgical subspecialty applicants still reported higher costs than their general surgical and nonsurgical peers. In 2021, higher costs for surgical subspecialty applicants were driven by more applications submitted, likely reflective of higher competitiveness of the surgical subspecialties. In comparison with nonsurgical specialties, costs were higher in all categories, suggesting that there are additional costs perceived to be necessary to match into a surgical subspecialty.
To our knowledge, this study is the first to demonstrate an association between total cost of the residency application cycle and number of interviews obtained, controlling for the number of applications submitted and interviews attended. This finding was most profound for otolaryngology applicants, who received 0.35 additional interviews per additional $1000 spent.
Overall, this finding raises concern that cost may serve as a barrier for applicants from lower socioeconomic means, particularly because otolaryngology applicants have reported insufficient funds for the application process in the past. 2 However, the cost of residency applications is a fraction of the complete cost of medical education, and it is unclear how these costs influence choice of specialty. In the context of our finding of away rotations and research experiences driving costs among otolaryngology applicants, it is possible that these factors are in part responsible for the correlation between total costs and interview offers in the pre–COVID-19 application cycles. The absence of this association during the 2021 application cycle suggests that cost savings stemming from virtual interviews and the lack of away rotations may have helped mitigate the relationship between costs and interviews obtained.
With subsequent application cycles reintegrating away rotations and the possibility of a return to in-person interviews, it may be pertinent for programs to pursue novel strategies to mitigate the effects that high costs may have on obtaining interviews for otolaryngology applicants. Our findings that away rotations and research experiences predict total cost suggest that efforts in subsidizing or funding those experiences for medical students may be beneficial, especially for those from groups that are historically underrepresented in medicine (URiM). Multiple avenues of funding currently exist for students, including away rotation grants for URiM students funded by professional organizations and individual institutions.31,32 Additional funding for students exists in the form of funded research experiences as well as travel grants for conference attendance.32-35 These current approaches may help alleviate the burden of cost for some students, but given the large number of yearly applicants, the initiation of new funding programs or expansion of existing programs may help alleviate cost-related burden for additional students.
It is important to note that the shift to virtual interviewing may create new barriers and challenges to DEI goals in otolaryngology. 36 This includes challenges related to obtaining mentorship, which is important for the recruitment of a diverse profession alongside provider satisfaction and career growth.37,38 Given this, the discussion on how to alleviate cost-related burdens should be balanced with the ability to ensure adequate connection and mentorship in the field. Disruptive and systematic approaches to mentorship are emerging opportunities that may help alleviate the barriers of recruitment in the virtual setting. These include structured preclinical mentorship for URiM students alongside a continued proactive shift toward new age mentoring and near-peer and reverse mentoring.36,39,40
The primary limitation of our study relates to generalizability. Our sample comprised 363 US senior otolaryngology applicants, which represents 28.5% of the 1273 applicants cited by the National Resident Matching Program between 2019 and 2021.41-43 Additionally, we lacked sociodemographic data, thereby limiting our assessment of cost burden among applicants from different socioeconomic backgrounds. Due to this, we are unable to draw conclusions relating to the impact of application costs on applicants with limited socioeconomic means. This study is further limited by the potential for selection and recall bias. Our match rates for otolaryngology were 80.9% in 2019, 86.7% in 2020, and 72.2% in 2021, which overestimate the National Resident Matching Program–reported match rates of 77.4%, 73.6%, and 68.3% for US MD applicants, respectively. Given the potential for selection bias, our analysis of the impact of costs on match success should be viewed with caution.41-43 Furthermore, since the survey is filled out 8 months following the submission of the Electronic Residency Application Service application, there is potential for recall bias.
Despite these limitations, our study addresses a gap in the literature for stakeholders in the otolaryngology residency match process. It provides evidence of applicant-reported savings during the COVID-19 application cycle alongside novel predictors of residency application cost for otolaryngology applicants. These findings can provide information that may aid in determining how best to recruit the next generation of otolaryngologists without exposing students to unnecessary financial strain, which may serve as a barrier for students from lower socioeconomic backgrounds. Furthermore, these findings provide transparency for future otolaryngology applicants who can use them as an estimate of the costs related to the application process. Last, our study illustrates the need for further research into the impact of costs on the application process, especially as it pertains to influencing applicant decision making and behaviors alongside the potential ramifications that application costs have in achieving DEI goals in otolaryngology, both of which are critically understudied. A better understanding of how sociodemographic factors interplay with the match process is a vital next step in addressing equity in the recruitment of a diverse field of otolaryngologists.
Conclusion
There was a 74% reduction in total residency application cost among otolaryngology applicants during the 2021 application cycle, which was likely driven by virtual interviewing and the lack of away rotations. The high costs of the residency application process are an important consideration for surgical subspecialties, which had higher costs than general surgery and nonsurgical specialties regardless of application year. In the years preceding the COVID-19 pandemic, there was a significant association between total costs and interview offers obtained among otolaryngology applicants, controlling for applications submitted and interviews attended. These findings can help stakeholders in the residency application process identify areas of improvement to help mitigate cost as a potential burden to matching into otolaryngology.
Author Contributions
Disclosures
Supplemental Material
sj-docx-1-opn-10.1177_2473974X221119150 – Supplemental material for Cost of the Otolaryngology Residency Application Process: Comparison With Other Specialties and Equity Implications
Supplemental material, sj-docx-1-opn-10.1177_2473974X221119150 for Cost of the Otolaryngology Residency Application Process: Comparison With Other Specialties and Equity Implications by William J. Benjamin, Nicholas R. Lenze, Janice L. Farlow, Angela P. Mihalic, Lauren A. Bohm and Robbi A. Kupfer in OTO Open: The Official Open Access Journal of the American Academy of Otolaryngology-Head and Neck Surgery Foundation
Footnotes
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
