Abstract
Objective
Examine the characteristics of recent head and neck (H&N) oncology fellowship graduates and assess their current perceptions of career alignment and satisfaction.
Methods
H&N fellowship graduates from American Head and Neck Society–accredited programs between 2015 to 2020 were surveyed. Two-sample t tests and analysis of variance tests were used to determine the effect of respondents’ demographics, fellowship characteristics, career preferences, and current practice on their degree of career alignment with expectations and overall job satisfaction.
Results
Fifty-eight fellowship graduates completed the cross-sectional survey. Of all respondents, 52 (89.7%) primarily preferred an academic job, of whom 5 (9.6%) went into private practice. Respondents in private practice, those treating general otolaryngology patients, and those who do not work with residents demonstrated significantly poorer job alignment and career satisfaction as compared with those in academic medicine, those treating only H&N patients, and those working with residents, respectively.
Discussion
The majority of graduating H&N fellows prefer a job in academic medicine; however, there may be an insufficient number of desirable academic positions available each year to meet such demand.
Implications for Practice
By setting realistic career expectations, preparing for a mixed scope of practice, and integrating resident involvement into private practice groups, H&N providers may ultimately find more fulfillment in their work. These findings could also be valuable to the American Head and Neck Society and fellowship programs in designing training and in planning for the number of available fellowship positions each year.
Keywords
Graduates of otolaryngology residency programs who are board eligible have the option of pursuing advanced training through a fellowship in head and neck (H&N) oncologic surgery. The number of American Head and Neck Society (AHNS)–accredited fellowship programs has grown over the last 2 decades in concordance with an increasing number of otolaryngology residency positions, with 50 programs currently available across the United States and Canada.1,2 Fellowship pursuance in general has also increased since the 1990s, whether out of desire or perceived necessity prior to entering a competitive job market. About 58% to 64% of fifth-year otolaryngology residents anticipate advanced training following graduation, and about 13% to 18% of fifth-year residents expect to complete a fellowship in H&N and/or microvascular surgery.3,4 However, for the newly graduated H&N oncology fellow in the current economic climate, there are uncertainties regarding the job application process and career expectations. While most H&N fellowship graduates tend to prefer a career in the academic setting over private practice, 4 this may not be an entirely realistic outcome if there is a limited number of academic positions available. It is unclear if these young physicians are joining the practices that they envisioned during training or finding fulfillment in their postgraduate positions. Through this study, we seek to examine the characteristics and experiences of recent H&N fellowship graduates and assess their current perceptions of career alignment and satisfaction.
Materials and Methods
We developed a survey that consisted of 17 multiple-choice and fill-in-the-blank questions addressing 4 basic categories: demographics, job application process, current practice, and quality of life perceptions. Respondents were asked to report their type of residency program, residency graduation year, geographic location of fellowship program, fellowship graduation year, whether they received microvascular training during fellowship, and their preferred career (academics, private practice, or either). Respondents were then asked about their experience applying to postfellowship jobs and the number of interviews they underwent prior to accepting a position. Current practice characteristics were assessed, such as geographic location, type and scope of practice, and interaction with other care providers, including residents. Finally, participants were asked to indicate how much they agreed or disagreed with the following statements: “My current practice matches the job I sought during training” and “I have an overall satisfaction with my current position.”
Approval was obtained from the Saint Louis University Institutional Review Board. Through the AHNS associate executive director’s office, H&N oncologists who graduated from an AHNS-accredited fellowship program between 2015 and 2020 were contacted via email and sent the electronic survey from June to July 2021. There were 230 working email addresses to which the survey was sent. To increase responses, the survey was also sent to the program coordinator at each AHNS-accredited fellowship program for distribution to previous fellows who graduated from 2015 to 2020. Multiple follow-up email invitations were sent, and participants were offered entry into a gift card raffle. Participation was voluntary and anonymous. The survey was designed to take ≤3 minutes to complete.
Our outcomes of interest were agreement with the statements “My current practice matches the job I sought during training” (ie, “job alignment”) and “I have an overall satisfaction with my current position” (ie, “job satisfaction”), assessed on a 5-point modified Likert scale from strongly disagree to strongly agree. Outcome responses were analyzed as continuous variables and centered on 0 (neutral) with a range from −2 (strongly disagree) to 2 (strongly agree). Independent variables included sex, residency program type, fellowship program location, fellowship graduation year, microvascular training during fellowship, initial career preferences, number of job interviews, current practice location, practice type and scope, involvement with residents, and whether current practice was at the same institution as the fellowship program. For independent variables with 2 groups, a 2-sample t test was conducted to determine the effect of each independent variable on outcome statement agreement scores. For independent variables with >2 groups, a 1-way analysis of variance test was used instead. Results were reported as means, and all tests used a P value cutoff of .05.
Results
Demographics
Of the 230 distributed surveys, 58 (25.2%) were completed. Demographic information is shown in Table 1 . Roughly one-third (35.1%) of graduates practice in the same geographic region in which they attended fellowship, while the remainder (64.9%) went on to practice in a different region. While those in academic medicine were well represented across each fellowship graduation year, most private practice physicians were recent graduates: 5 of the 6 respondents (83.3%) who reported working in private practice graduated fellowship in 2019 or later. In terms of career preferences, of the 52 fellows who had preferred a position in academic medicine, 47 (90.4%) took jobs in academic practice while 5 (9.6%) took positions in private practice. Importantly, scope of practice was not strictly correlated with practice type; not all academicians saw H&N patients only, and not all of those in private practice saw general otolaryngology patients. Of those in academics, 9 (17.3%) reported a practice consisting of partial H&N and partial general otolaryngology, while 3 (50.0%) of those in private practice indicated seeing all or almost all H&N patients.
Demographic Information of H&N Fellowship Graduates, 2015-2020.
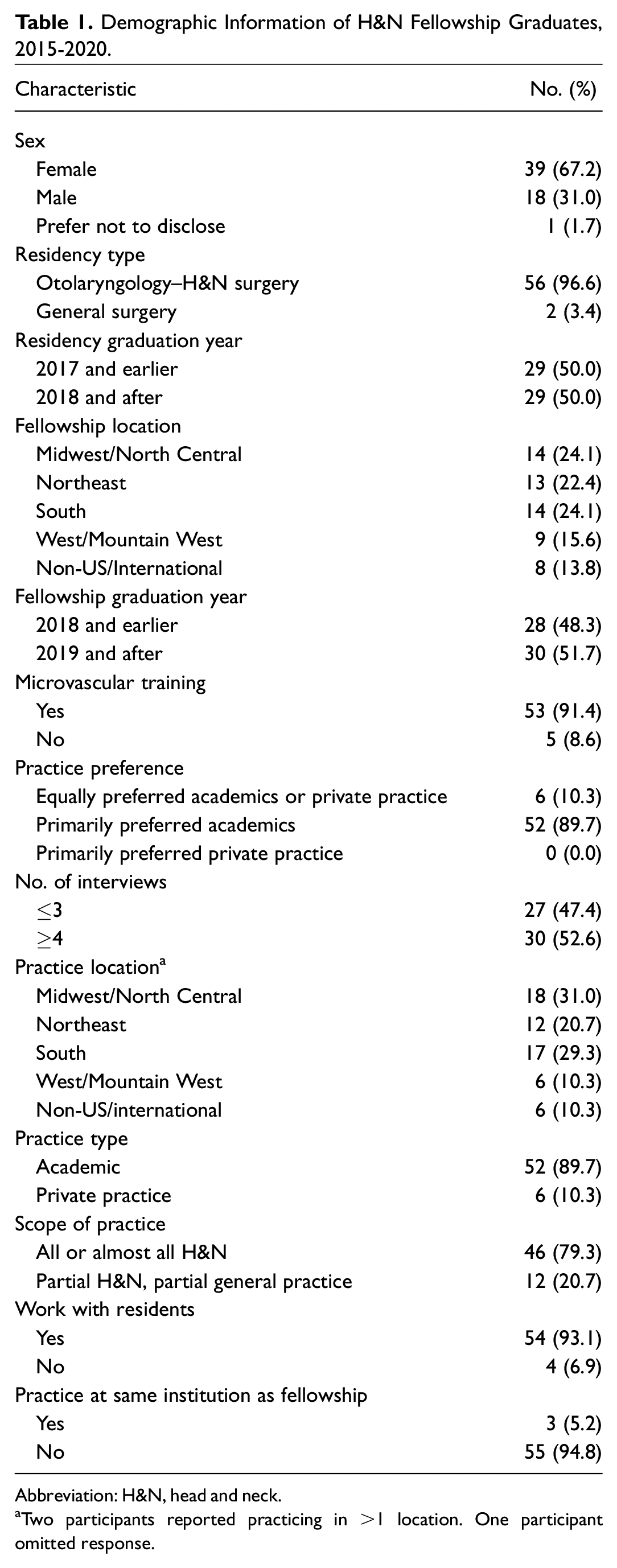
Abbreviation: H&N, head and neck.
Two participants reported practicing in >1 location. One participant omitted response.
Job Application Process
Information on the timing of job applications, interviews, and offers for H&N fellows is listed in Table 2 . Notably, 10 graduates (17.2%) had started applying for attending-level jobs before the start of their fellowship, and 5 (8.6%) had already received a job offer going into fellowship. However, the majority of graduates were applying during the first half of their fellowship, interviewing during the second half, and receiving offers before they graduated. Four respondents (6.9%) started receiving job offers only after graduating fellowship.
Job Application Process for H&N Fellowship Graduates, 2015-2020. a
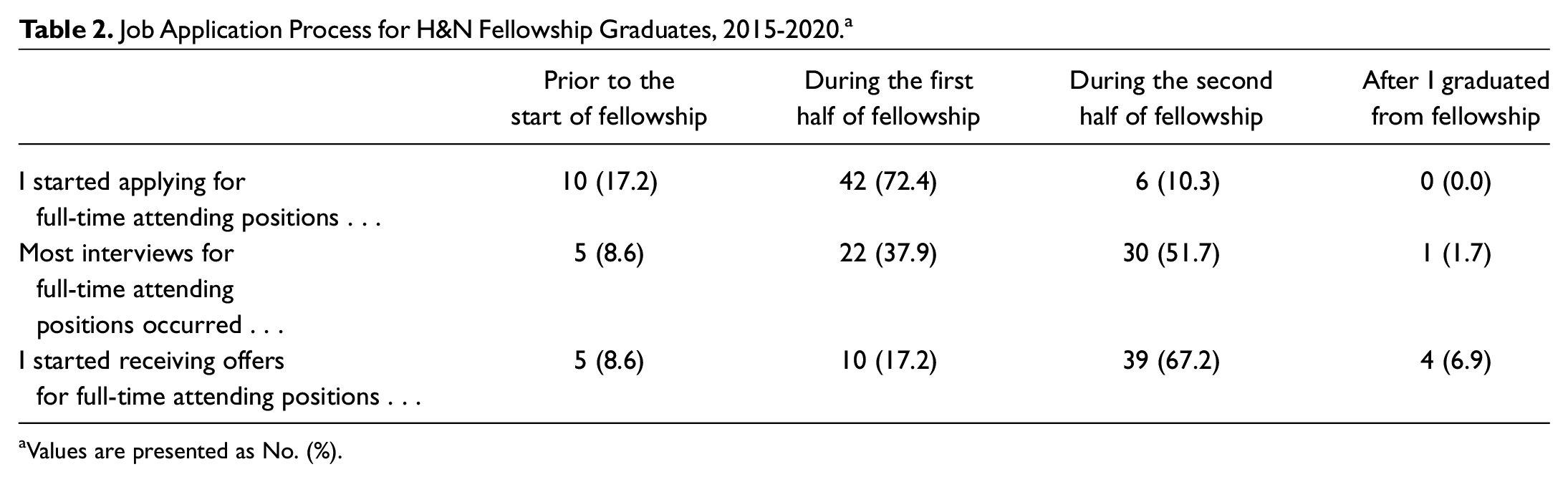

Values are presented as No. (%).
Current Practice Perceptions
Statistical analysis examining job alignment agreement scores showed that mean scores were significantly higher for respondents who graduated fellowship in 2018 or earlier (1.43 vs 0.90, P = .03), those currently in academic vs private practice (1.35 vs −0.50, P < .001), those seeing only H&N patients vs H&N and general otolaryngology patients (1.41 vs 0.17, P < .001), and those actively involved with residents (1.26 vs −0.25, P = .001; Figure 1 ). Similarly, mean agreement scores for job satisfaction were significantly higher for those in academic practice (1.23 vs −0.17, P < .001), those whose practice scope involves primarily H&N patients (1.30 vs 0.25, P < .001), and those working with residents (1.19 vs −0.25, P = .004; Figure 2 ). Sex, residency program type, fellowship location, microvascular training, number of interviews, practice location, and current position at the same institution as one’s fellowship were not associated with significant differences in agreement scores.
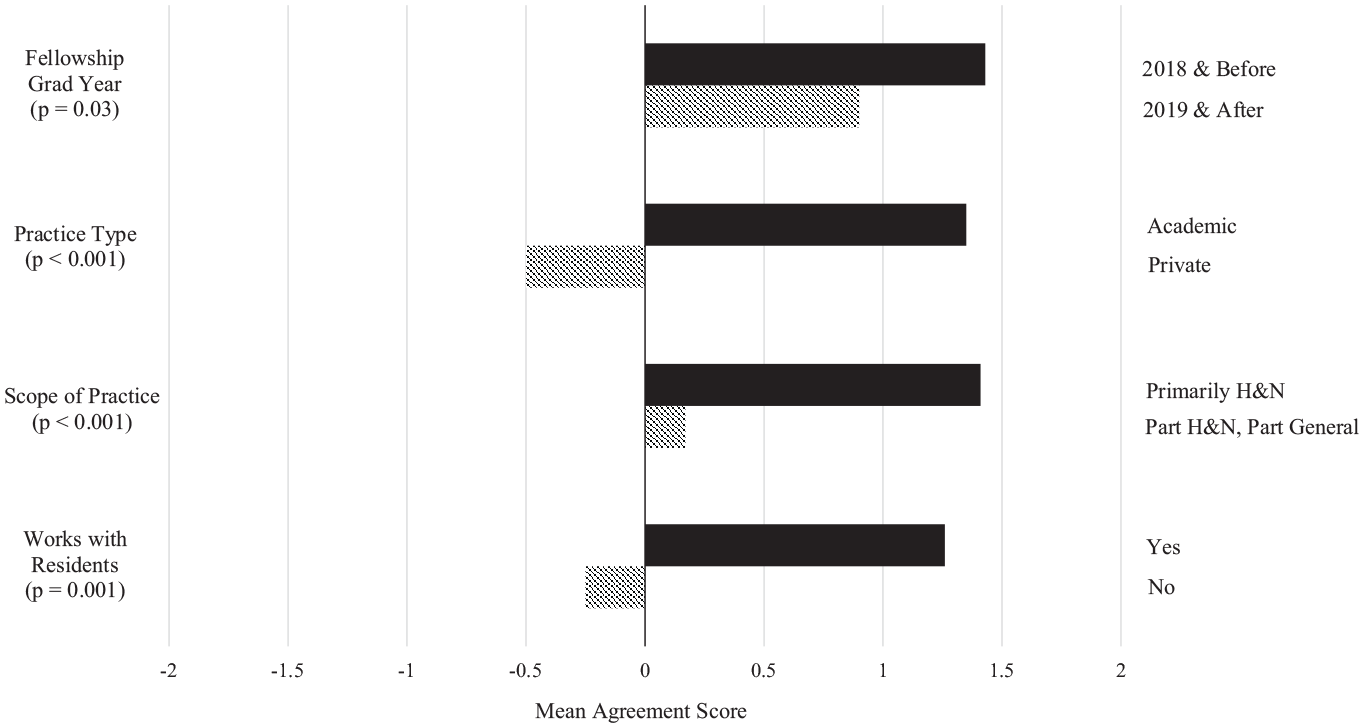
Mean agreement scores with “job alignment” by independent variable. Only variables that met statistical significance at a P value cutoff of .05 were included.
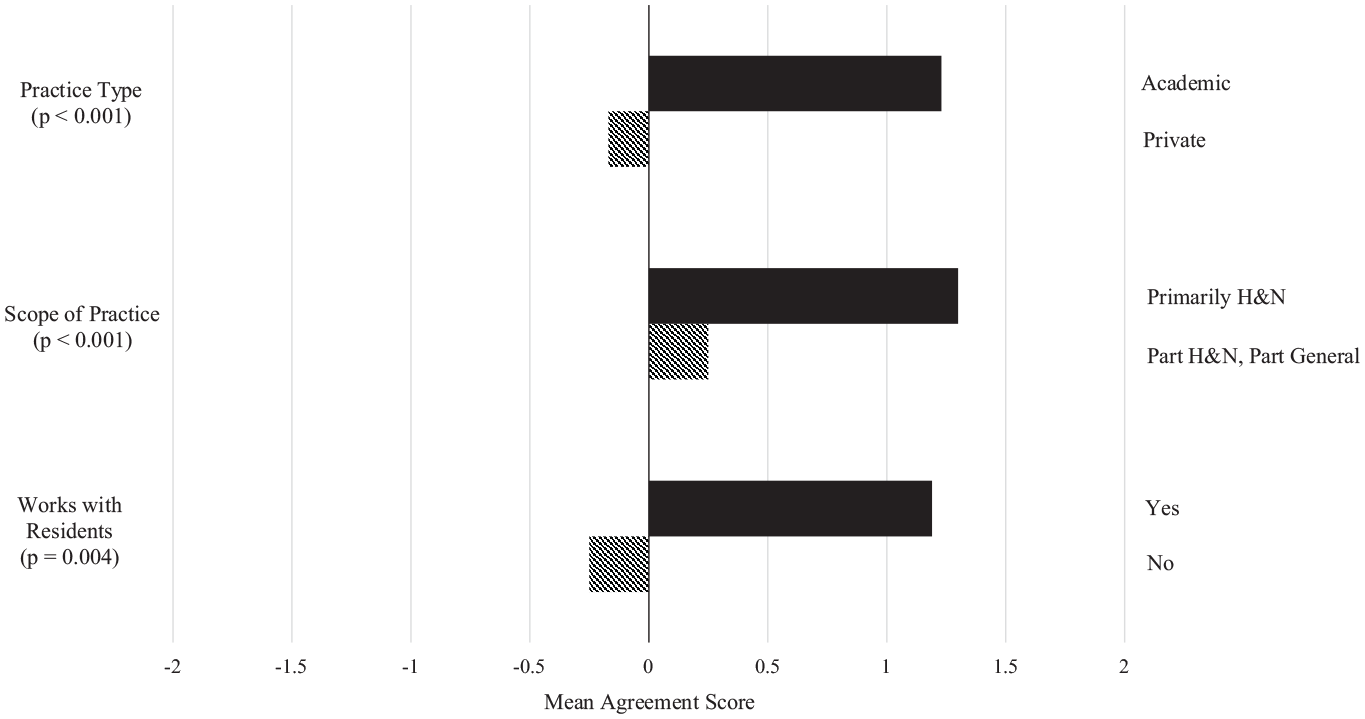
Mean agreement scores with “job satisfaction” by independent variable. Only variables that met statistical significance at a P value cutoff of .05 were included. H&N, head and neck.
Discussion
H&N oncology continues to be a top fellowship choice for otolaryngology residents, with roughly 9% to 29% of all residents choosing advanced training in this field.4,5 The majority of our survey respondents (89.7%) desired a job in academic medicine, as is the case for most other fellowship-trained physicians.6,7 Because nearly all H&N fellowships are 1 year in duration, it behooves the fellow to search for a job as early as possible. Approximately one-fifth (17.2%) of fellows were able to apply for jobs prior to the start of fellowship, all of whom received offers before the end of their training.
H&N fellowship graduates in private practice appear to be less satisfied with their career trajectory as compared with their counterparts in academic medicine. Most advanced H&N care has historically been performed at tertiary academic centers because of the complexity of oncologic and reconstructive surgery, lengthy postoperative hospital stays, and need for a multidisciplinary approach to patient care. There are often barriers to performing this type of care in private practice, such as greater financial constraints, more demanding call schedules, and less access to operating room time, which may lead to increased frustration and dissatisfaction among H&N physicians in these roles. These barriers, however, are not insurmountable; private multispecialty groups who are motivated and have a strong affiliation to a tertiary hospital are often capable of supporting the needs of a robust H&N practice.
The majority of respondents in our study reported that during their fellowship training, they primarily preferred to find a position in academics upon graduation. Yet we found that nearly a tenth of H&N fellows ultimately went into private practice despite preferring an academic job. These findings suggest that the number of desirable academic positions available to graduates today may be insufficient or that the number of fellows graduating each year may be too many. Several decades ago, the AHNS faced a diminishing pool of H&N fellowship candidates, thought to be due to reimbursement policies, decreased interest from general surgery applicants, and the rise of other subspecialties (eg, endoscopic sinus surgery, facial plastics). 8 It now appears that the paradigm has shifted in the opposite direction. Lin et al 9 showed that while the number of H&N fellows has steadily risen at a rate of roughly 2 additional graduates per year since 1997, the number of graduates practicing in an academic setting has increased by only 1 per year. Academic opportunities available to the large body of yearly H&N graduates now appear limited, perhaps indicating a surplus of fellows graduating each year. This phenomenon may be more recent than imagined, as 5 of the 6 (83.3%) respondents in private practice graduated fellowship in 2019 or later. This could also explain the significantly lower agreement scores with job alignment seen in those who graduated fellowship more recently.
At the same time, concerns have been raised regarding the ability of otolaryngologist workforce numbers to keep up with increasing demand from an aging and growing population, which may be more pronounced in H&N surgery than in other subspecialties due to its older patient base.10-13 Though positions may be limited at high-volume academic centers in urban areas, graduating fellows may find more job opportunities in rural or socioeconomically disadvantaged communities, which often lack access to H&N cancer care.14-16 To avoid discouraging future trainees from pursuing a career in H&N, fellows and residents should instead be prepared through mentorship and open dialogue to consider a career outside of purely academics, which could modify expectations and ultimately increase overall career satisfaction.
H&N physicians whose scope of practice includes a substantial amount of general otolaryngology and those who do not work with residents reported significantly lower agreement scores with job alignment and job satisfaction. Miller et al 3 found that only 19% of all newly fellowship-trained otolaryngologists, including H&N oncologists, planned to include general otolaryngology as part of their practice. However, because of the need to build up a patient base early on and the relatively low reimbursement rates in providing H&N oncologic care, 8 treating general otolaryngology patients may be necessary for young H&N physicians despite the desire to care exclusively for patients with H&N cancer. Fellows who stay current in their skill set and knowledge of general otolaryngology may ultimately be better prepared and more content after training. The support provided by residents in the form of rounding on patients, performing bedside procedures, and taking primary call may also reduce the stress and time burden for providers. Active teaching of residents in the operating room or at the bedside may be an additional understated driver of career satisfaction.6,9,17 While working with residents is obviously more intrinsic to academic practice, private practice groups near major centers could consider collaborating with residency programs to have trainees rotate with them. This is being done at some institutions, and our study suggests that it has the potential to benefit H&N providers.
Though our study did not specifically address physician burnout, the factors associated with lower job alignment and job satisfaction scores may contribute toward the high rates of burnout previously reported for H&N surgeons as compared with other subspecialists.18-20 Kejner et al 21 found that H&N microvascular surgeons in private practice and those who had been in practice for <4 years demonstrated higher absolute, though not statistically significant, rates of emotional exhaustion and depersonalization vs those in academics and those in practice for ≥4 years, respectively. Lack of inpatient support was also a significant risk factor for burnout. 21 Studies conducted more than a decade ago indicated that despite moderate levels of professional burnout in H&N physicians, career satisfaction and congruence with career expectations remained high. 22 Our results suggest that recent H&N fellowship graduates may be experiencing declining job satisfaction and worse career alignment with expectations, which could lead to worsening burnout rates in the near future.
One major limitation of the study was its relatively small sample size. The response rate of 25.2% is not unexpected for this type of survey study; however, this precludes the ability to perform multivariable analysis, and these results may not be representative of all H&N fellowship graduates. There are H&N programs outside the AHNS whose fellows were not captured in the distribution of our survey. We also suspect that selection bias may contribute to the low number of private practice respondents, who tend to have lower engagement with research and are therefore less likely to respond to this type of survey.
Implications for Practice
Despite these shortcomings, the data presented could be valuable to the AHNS and fellowship programs in designing training and in planning for the number of available fellowship positions each year. By setting realistic career expectations, preparing for a mixed scope of practice early on after training, and integrating resident involvement into more private practice groups, H&N providers may ultimately feel more fulfilled in their work. Further studies with higher power are needed to identify other indicators of H&N career satisfaction and to determine whether these changes truly improve perceptions among providers or lead to reduced rates of burnout.
