Abstract

Hamartomas are benign tumors that contain a mixture of cell types appropriate for the tissue of origin but in abnormal amounts, patterns, and distributions. 1 Pulmonary hamartomas are the most common benign neoplasm of the lungs, with a reported incidence of 0.025% to 0.032% in adults. 2 Among all tracheobronchial hamartomas, only 1.4% are endobronchial, while tracheal hamartomas are much rarer, with fewer than 30 cases documented in the literature. 3 In this report, we review the clinical management of an adult patient with an incidental tracheal hamartoma discovered during routine lung screening.
Case Report
Approval was obtained from Vanderbilt University Medical Center Institutional Review Board (#212158). This study adheres and incorporates CARE case report guidelines.
A 69-year-old man with a 30-pack-year smoking history underwent routine lung cancer screening with a low-dose computed tomography (CT) chest scan. The patient reported no family history of cancers. Imaging demonstrated a 1.2-cm mass along the left tracheal wall at the level of the thoracic inlet ( Figure 1 ). Serial imaging was performed at 3-month and 6-month intervals without appreciable change in the appearance of the mass. An otolaryngology referral was made due to the possibility of malignancy given the patient’s smoking history. He presented to our clinic 14 months following the initial diagnosis without complaints of shortness of breath, wheezing, stridor, cough, difficulty swallowing, or hoarseness. We reviewed options of continued imaging surveillance vs endoscopic excision; the patient opted for surgery. Direct laryngoscopy was performed with a Dedo laryngoscope in the setting of intermittent endotracheal intubation. A 0-degree Hopkins rod endoscope was used for visualization. We identified the intraluminal mass projecting from the left lateral posterior aspect of the first tracheal ring ( Figure 1 ) and performed near-total resection using a variety of forceps and suctions. Specimens were sent for permanent pathology. They demonstrated a polypoid, benign cartilaginous, fibrous tumor covered by surface epithelium with squamous metaplasia consistent with a tracheal (chondroid) hamartoma ( Figure 1 ). A repeat CT scan performed at 1-year follow-up did not reveal evidence of recurrence. The interval was selected due to the slow growth of tracheal hamartomas.
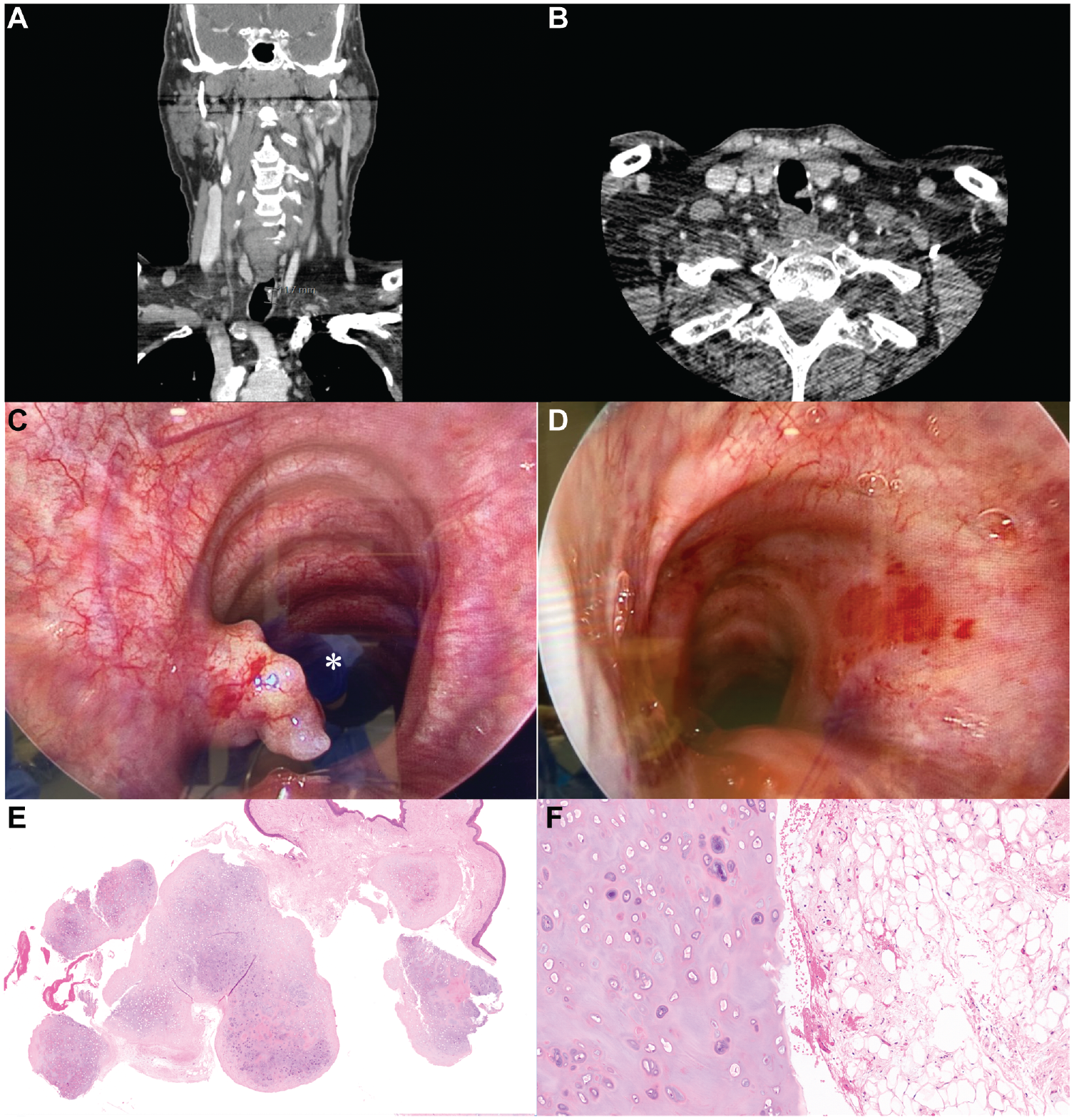
(A) Coronal and (B) axial computed tomography images showing a 1.2-cm endotracheal tumor. (C) Mass visualized on direct tracheoscopy.* (D) Post-resection. (E) Specimen on medium power (4×) and (F) higher power (10×). *Reflection artifact present.
Discussion
Primary tracheal tumors are rare, with a reported incidence of 2.6 per 1,000,000 people. In adults, only 10% are benign, while 70% to 90% are benign in children. 4 The differential for benign neoplasms of the trachea includes squamous papilloma, salivary pleomorphic adenoma, mucous gland adenoma, oncocytoma, hamartoma, and leiomyoma. 4 Tracheal hamartomas are composed of a mixture of cells in an abnormal distribution and have not been shown to exhibit malignant transformation potential. There have been fewer than 30 reported cases of tracheal hamartomas ( Table 1 ). Compared to pulmonary hamartomas, tracheal hamartomas are usually symptomatic secondary to intraluminal obstruction in the proximal airway. Shortness of breath and dyspnea are the most common presenting symptoms. Less common symptoms include stridor, cough, and chest pain. The overlap in symptoms with obstructive airway diseases may delay diagnosis, as demonstrated by 10 of 27 (37%) previous cases of tracheal hamartomas diagnosed initially as asthma.
Case Reports of Tracheal Hamartomas.
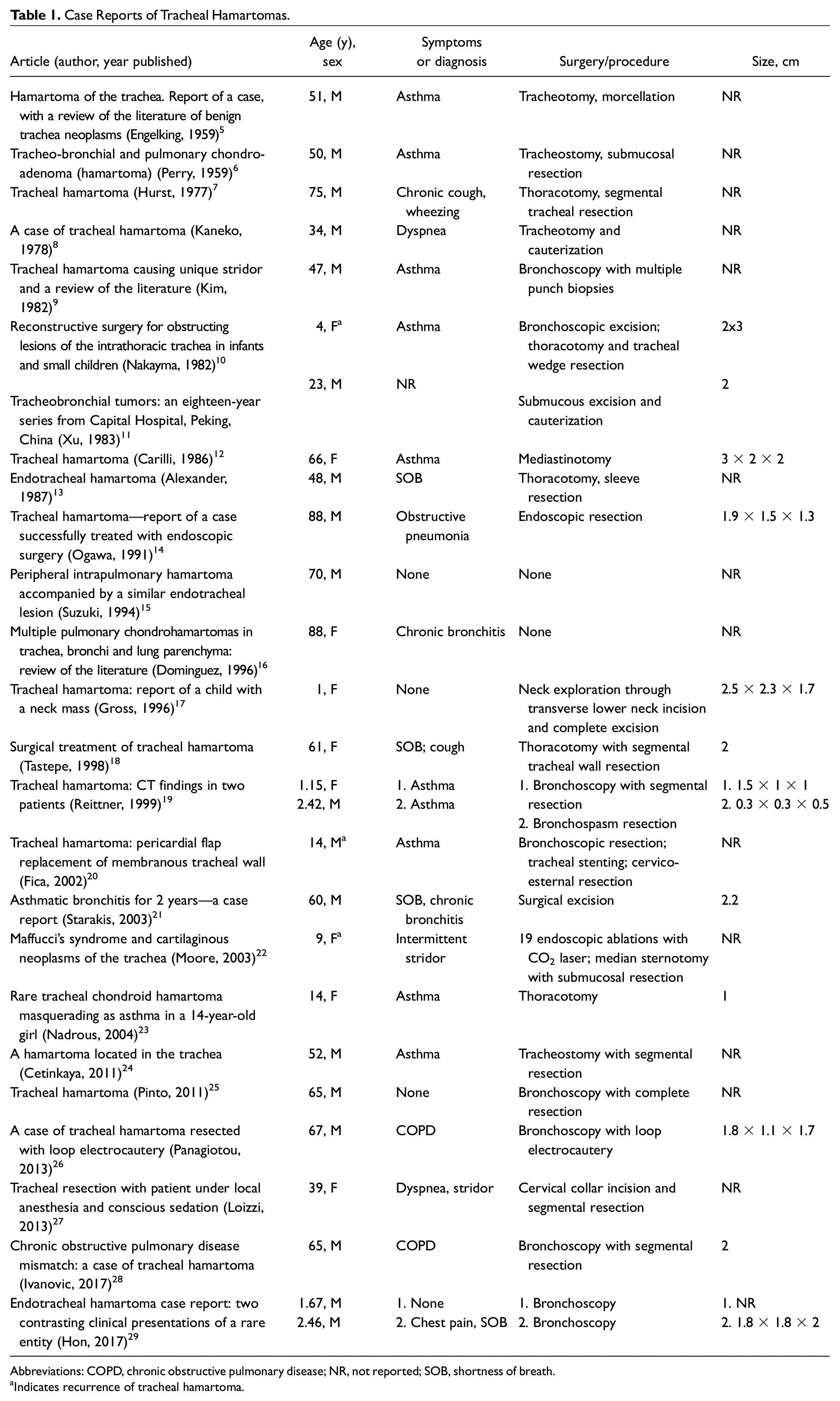
Abbreviations: COPD, chronic obstructive pulmonary disease; NR, not reported; SOB, shortness of breath.
Indicates recurrence of tracheal hamartoma.
Tracheal hamartomas may first be identified on CT scans of the neck or chest. Direct visualization requires endoscopic evaluation, at which time a biopsy can be performed to obtain a tissue diagnosis. In the literature, the average reported pathological or radiographical size of tracheal hamartomas is approximately 2 cm, ranging from 0.5 to 3.0 cm ( Table 1 ). Routine surveillance is acceptable for patients with a confirmed diagnosis and lack of symptoms. Surgery is the definitive management option for symptomatic patients and those with a clinical history concerning for underlying malignancy. The most common surgical intervention for excision is direct endoscopy with excision. Other surgical techniques include thoracotomy, mediastinotomy, transcervical approach with segmental resection, and CO2 laser ablation. Concurrent tracheostomy at the time or surgery may be necessary as observed in 4 of 27 (14.8%) reported cases.
Clinicians should consider the presence of tracheal hamartomas in patients with obstructive airway symptoms whose respiratory symptoms do not improve with standard therapies. Unrecognized tracheal hamartomas can lead to critical airway obstruction and early detection can prevent avoidable complications, including death. This article reviews key clinical characteristics and provides an overview of management to aid providers who may encounter this disease process.
