Abstract
Objective
This review aims to describe the methods used to assess the vocal quality and quality of life of children after airway reconstruction and their limitations.
Data Sources
A systematic review was carried out in 10 databases for articles published between 2000 and 2021 following the PRISMA guidelines (Preferred Reporting Items for Systematic Reviews and Meta-analyses).
Review Methods
Articles were included that described perceptual voice assessment with or without acoustic measures and/or voice quality impact questionnaires. Articles with no description of a specific voice assessment were excluded.
Results
A total of 12 studies were included, yielding 263 patients. The mean age at evaluation was 9 years. Follow-up varied from 5 months to 20 years with most patients being evaluated at least a year after surgery. Methods used to evaluate voice were perceptual, aerodynamic, and acoustic analysis and quality of life questionnaires. CAPE-V (Consensus Auditory Perceptual Evaluation–Voice) was the most used auditory-perceptual instrument (72.7%). Of the acoustic parameters, fundamental frequency and maximum phonation time were the most described (58.3%), and among the quality of life assessment questionnaires, pVHI (Pediatric Voice Handicap Index) was the most used (54.5%).
Conclusion
Multidimensional evaluations tailored to the individual child can be recommended after open airway surgery. CAPE-V scale, fundamental frequency, maximum phonation time, and pVHI are the most frequently used methods; therefore, their use may help broaden communication among authors. In the multitude of methods available, cognitive ability and degree of voice disturbance should be considered since they are the most important limiting factors in this population.
The success criterion of open airway surgery in children is primarily to achieve a patent airway and, consequently, the return to activities without respiratory restrictions. Currently, due to the improvement of surgical techniques, the high reported success rates of decannulation, and the longer follow-up time of children undergoing this type of surgery, voice quality has also been an important criterion of success, although considered secondary.1,2
Dysphonia occurs in varying degrees in more than half of children undergoing this procedure, causing social withdrawal and depression and negatively influencing social, emotional, educational, and occupational relationships. It has high repercussions on the lives of children and families, and long-term follow-up will increasingly uncover this as operated children enter the labor market; as such, this topic has gained importance in recent years.3,4 Measurements of the real impact of these operations on vocal quality are difficult due to the subjectivity of the perception of dysphonia, the variation of the impact according to the need for vocal performance, and the applicability in children during cognitive development. In addition, there is a difficulty in standardizing the assessments.
After decades of reports of success rates related to decannulation and breathing, it is essential that we assess the repercussions of these procedures on the quality of life of these children in the long term, and perhaps the most important handicap is related to voice and communication. 1 Considering the difficulty of evaluating vocal quality in highly altered voices, especially in children, it is important to establish which methods are used for this evaluation, the applicability and limitations of each one, in order to build a better follow-up strategy. Based on our experience, evaluating the voices of children is particularly challenging when they have multiple medical issues, have used a tracheostomy of extended periods, and/or have undergone major surgery. Cognitive ability to vocalize and perform demanded tasks varies greatly, and evaluation of distorted voices may require distinct analysis. The motivation for this review was to verify experiences from other airway teams that might help delineate better ways of characterizing voice and voice impact after major airway surgery. Verification of the previous achievements and difficulties could help improve and further validate the current protocol used for evaluation of postoperative voice outcomes and also contribute to ideas of future multicentric communication of such results. This systematic review aims to describe vocal quality assessment strategies for children undergoing airway reconstruction and their limitations.
Methods
This systematic review has followed the PRISMA recommendations (Preferred Reporting Items for Systematic Reviews and Meta-analyses).
Search Strategy
The bibliographic search was carried out in the following databases for articles published between 2000 and 2021: PubMed, PubMed PMC, BVC-Bireme, CINAHL, Scopus, Web of Science, Embase, Cochrane-OVID, ProQuest, and Medline. Specific descriptors and their synonyms were used according to the Medical Subject Headings and Embase Subject Headings: voice, voice quality, vocal quality, quality of life, laryngoplasty, airway remodeling, reconstructive surgical procedures, laryngeal reconstruction, airway reconstruction, laryngotracheoplasty, laryngotracheoplasty (LTP) OR laryngotracheal reconstruction OR cricotracheal resection, infant, newborn, infant, child, preschool, child and adolescent. The terms were associated with each other with the words AND and OR. A librarian assisted in the planning and development of terms for the computerized search. After the search, the references of each database were exported to the Rayyan QCRI program (https://rayyan.qcri.org/).
Selection Criteria
Articles were included that described perceptual vocal assessment with or without acoustic measures and/or impact of vocal quality on the quality of life in the pediatric population (up to 19 years of age) previously submitted to airway reconstruction. Only articles published in English were included. Articles that did not describe postoperative voice assessment, animal studies, and duplicates were excluded.
The entire search process was carried out by 2 independent evaluators, according to preestablished criteria per the Rayyan QCRI program, which eliminated duplicates and displayed the list of articles and abstracts for evaluators in a blind fashion. In case of discrepancies, a third evaluator was consulted for a final decision. After the database search, duplicates were removed, and the articles were selected by title and abstract and read in full. Data on postoperative voice assessment were extracted, in addition to the methodological characteristics of the studies, sample size and sex, language spoken in the country where the work was carried out, and advantages and disadvantages reported by the authors.
Results
A total of 389 articles were found in the databases, 142 of which were excluded due to duplicity, totaling 247 articles for selection. Of these, 228 were excluded after review of the title and abstract, and 19 were read in full. After the 19 articles were read, 6 were excluded because they did not specifically report the results of vocal evaluations in children in the postoperative period of laryngotracheal reconstruction, and 1 was excluded because it was an evaluation in an adult. A total of 12 studies were part of the review, including 263 patients ( Figure 1 ).
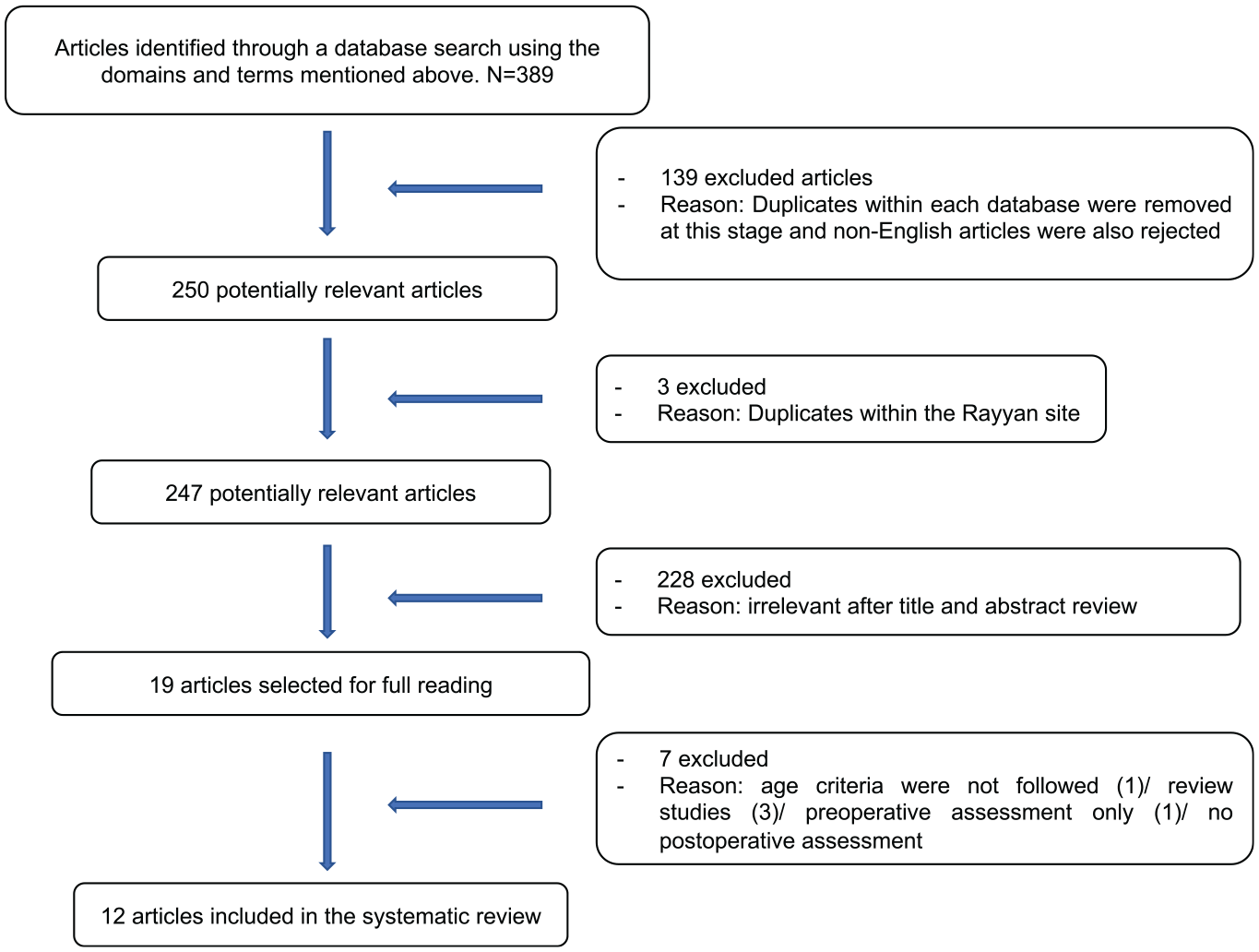
Flowchart with systematic revision search.
The studies were mostly cohort studies; 1 was an isolated case report of a single patient; and 2 were case-control studies. In 9 studies the mean age of the children evaluated was 9.2 years; in 3 studies, only the median age was reported, with a minimum age of 1 year and a maximum of 27 years (1 patient was 27 years old at the time of vocal analysis but 16 years at the time of surgery). The number of subjects in each study ranged from 1 to 55 cases. Sex was reported in 221 of the 263 patients and approximately half were male (53.3%). Only 1 study did not report the children’s sex. 5 Most articles were published in the last 8 years and the first was in 2009. Of the 12 articles, only 3 involved subjects that did not have English as their native language.2,6,7 The methodological and demographic characteristics of the studies included in this review are described in Table 1 .
Methodological and Demographic Characteristics of Studies.
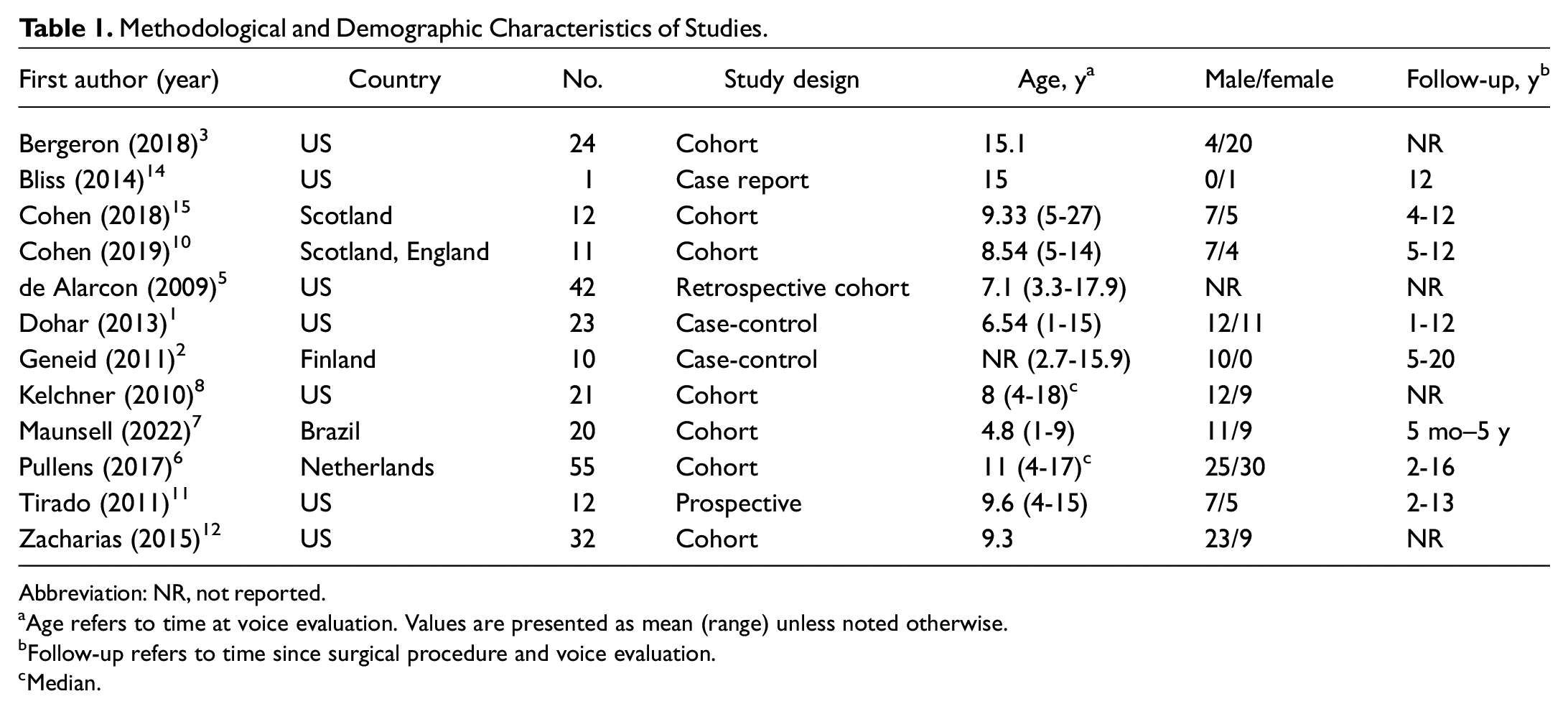
Abbreviation: NR, not reported.
Age refers to time at voice evaluation. Values are presented as mean (range) unless noted otherwise.
Follow-up refers to time since surgical procedure and voice evaluation.
Median.
Methods used for voice assessment after airway surgery were as follows:
Instrumental: rigid or flexible airway endoscopy, depending on the patient’s age
Auditory-perceptual: Consensus Auditory Perceptual Evaluation–Voice (CAPE-V); grade, roughness, breathiness, asthenia, strain (GRBAS); visual analog scale (VAS)
Aerodynamic/acoustic measurements: fundamental frequency, maximum phonation time, intensity, jitter, shimmer, noise-harmonic ratio, S/Z ratio, Dysphonia Severity Index (DSI)
Self-perception of quality of life and voice questionnaires: Pediatric Voice Handicap Index (pVHI), Pediatric Voice Outcome Survey (pVOS), Pediatric Voice Related Quality of Life (pVRQoL), Health Related Quality of Life (HRQoL), Health Utility Index Version 3 (HUI3), Impact on Family Questionnaire (IFQ), and pediatric quality of life (PedsQL)
All studies except one 2 used some kind of perceptual assessment, and CAPE-V was used in 72.7% (8 of 11). Two-thirds of the studies (66.6%) used >1 voice assessment method. The methods used by each author group are described in Tables 2 and 3 . Acoustic evaluations were also very common, used in two-thirds of the studies. Only 1 study did not use a quality of life questionnaire. 8 The most used questionnaires to report quality of life were pVHI (54.5%) and pVRQOL (45.4%). Table 4 lists the advantages and disadvantages of the methods reported by the authors.
Methods Used for Auditory Perceptual Assessment.
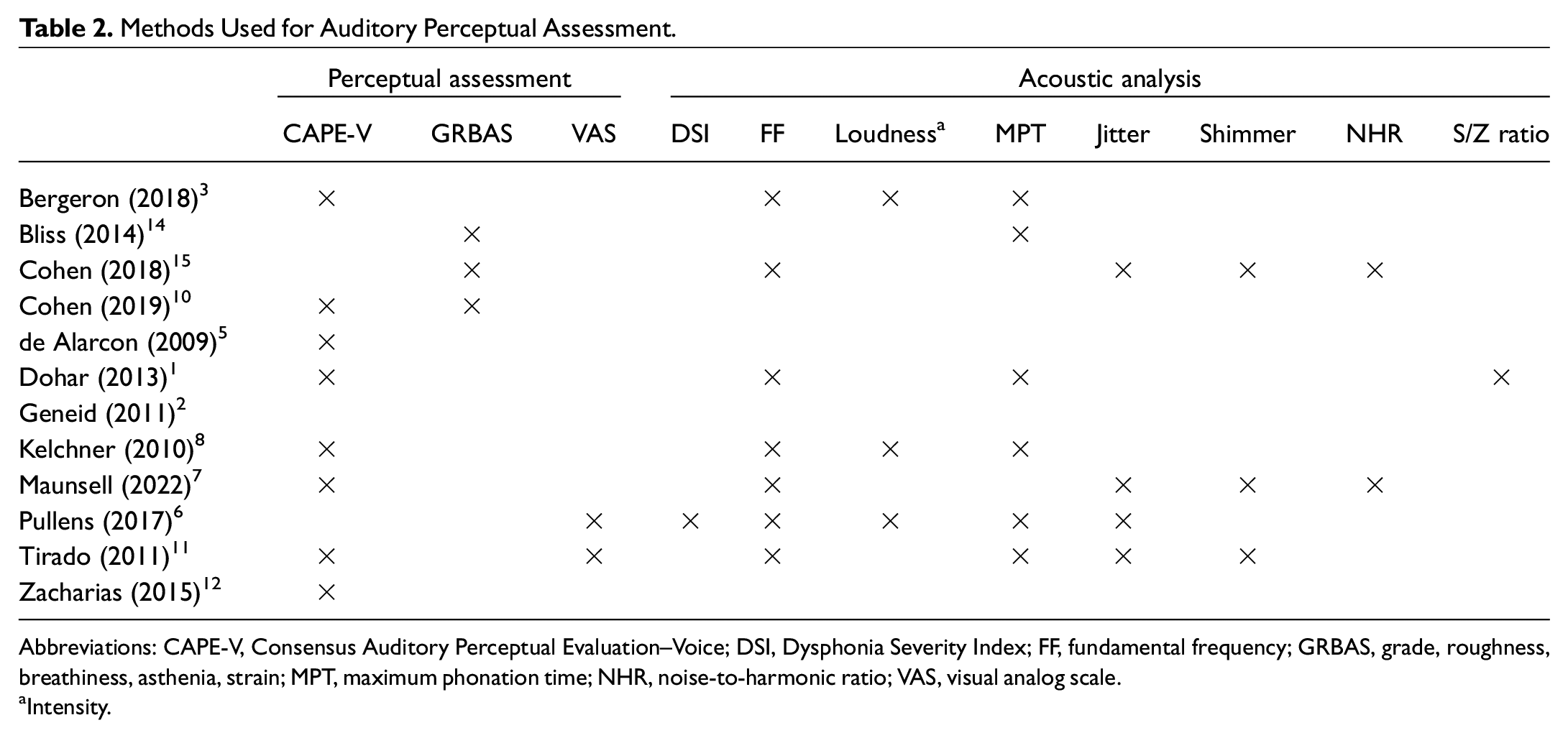
Abbreviations: CAPE-V, Consensus Auditory Perceptual Evaluation–Voice; DSI, Dysphonia Severity Index; FF, fundamental frequency; GRBAS, grade, roughness, breathiness, asthenia, strain; MPT, maximum phonation time; NHR, noise-to-harmonic ratio; VAS, visual analog scale.
Intensity.
Methods Used to Assess the Impact on Voice and Quality of Life.
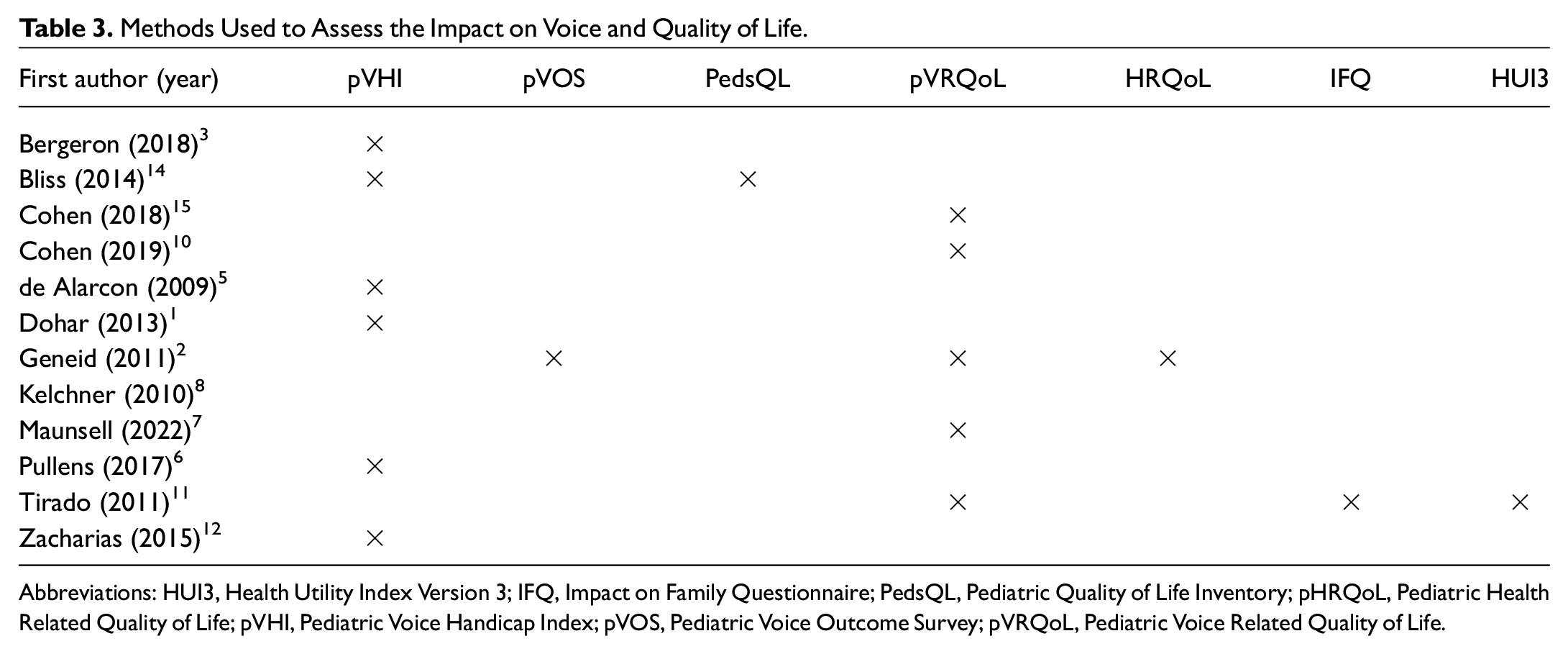
Abbreviations: HUI3, Health Utility Index Version 3; IFQ, Impact on Family Questionnaire; PedsQL, Pediatric Quality of Life Inventory; pHRQoL, Pediatric Health Related Quality of Life; pVHI, Pediatric Voice Handicap Index; pVOS, Pediatric Voice Outcome Survey; pVRQoL, Pediatric Voice Related Quality of Life.
Advantages and Disadvantages of Assessment Instruments.
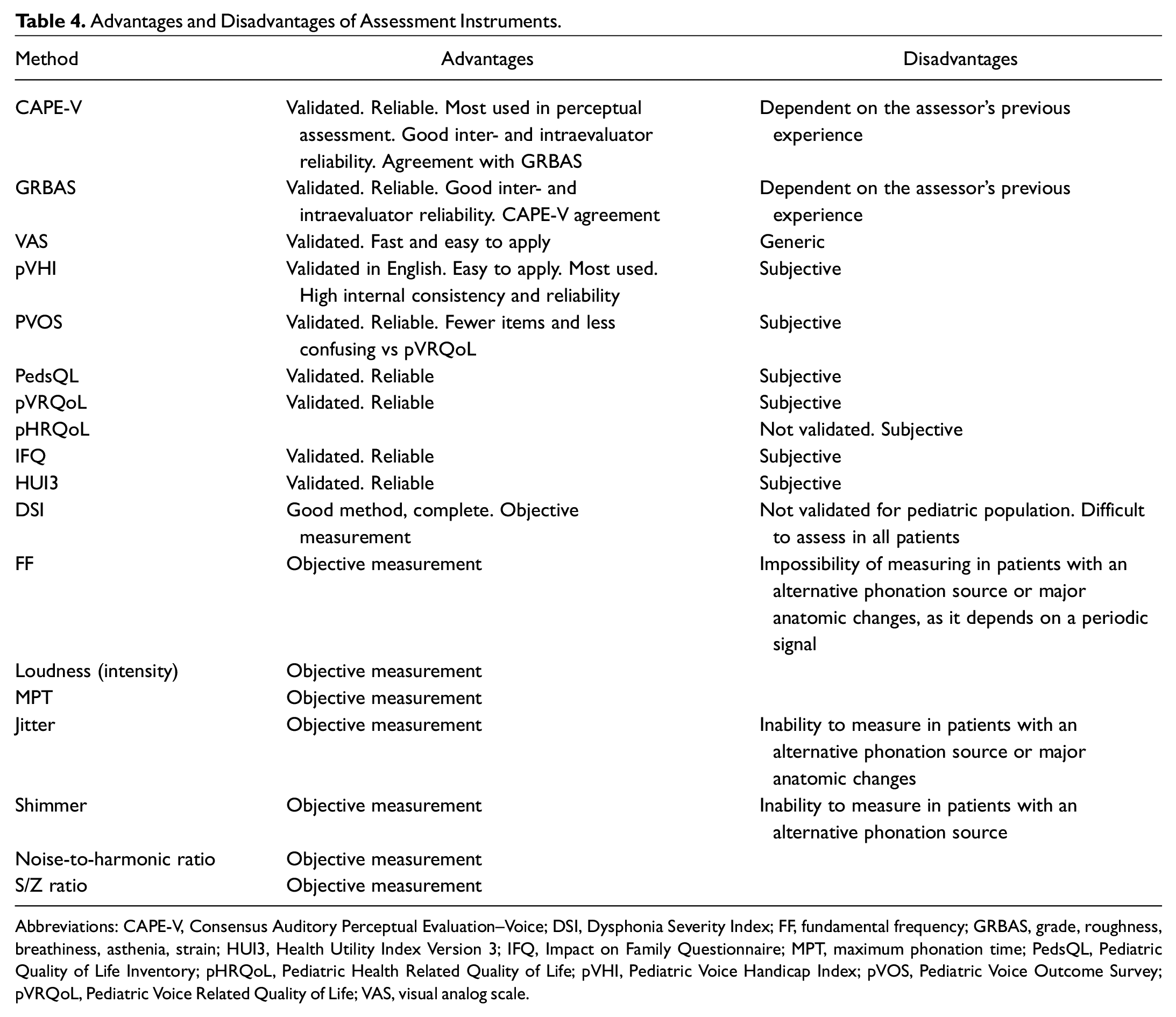
Abbreviations: CAPE-V, Consensus Auditory Perceptual Evaluation–Voice; DSI, Dysphonia Severity Index; FF, fundamental frequency; GRBAS, grade, roughness, breathiness, asthenia, strain; HUI3, Health Utility Index Version 3; IFQ, Impact on Family Questionnaire; MPT, maximum phonation time; PedsQL, Pediatric Quality of Life Inventory; pHRQoL, Pediatric Health Related Quality of Life; pVHI, Pediatric Voice Handicap Index; pVOS, Pediatric Voice Outcome Survey; pVRQoL, Pediatric Voice Related Quality of Life; VAS, visual analog scale.
Discussion
Postoperative vocal assessment is essential to address the permanent handicap associated with these surgical procedures and how this affects the family and the patients’ quality of life. In this context, a therapeutic and holistic approach should be established. As confirmed by many of the studies in this review, evaluating children’s voices with objective methods is always challenging. In this scenario of voices with high degrees of alteration, the concept of multidimensional voice assessment is particularly relevant. The multidimensional assessment should include endoscopic/otolaryngological assessment (image), perceptual assessment, acoustic assessment, and the subject’s self-perception, based on quality of life questionnaires, for example. 9 Although establishing a reproducible and effective methodology is desirable, it should probably be tailored to individual needs.
Auditory perceptual judgment is the gold standard for voice evaluation; however, this method can be subjective, and the results depend on the evaluator’s training and experience in altered voices. The CAPE-V scale, which uses an visual analog scale, was the most used. 10 Cohen et al correlated the perceptual assessment of voice in the view of physicians, using the GRBAS and CAPE-V scales, with the self-report of voice-related quality of life by family members/patients, establishing partial agreement between the medical assessment and parents. 10
Regarding the pediatric population, perceptual assessment reported by the family is extremely important to assess the ability to communicate. There is not always a direct correlation between family perception and quality of life 7 : a child and/or family with good communication skills can overcome the limitations of severe dysphonia and present fewer vocal complaints, for example. 11 Many of the questionnaires applied are subjective and dependent on the examiner’s experience. This is why it is extremely important that a qualified team perform the vocal assessment of these patients.
Quality of life questionnaires should be evaluated and discussed with the patient and family before settling for further surgical options to improve voice quality. Voice quality of life questionnaires are mostly adaptations from those applied to adult populations. Questionnaires validated for pediatric use are currently pVOS, HUI3, VAS, pVRQoL, pVHI, and IFQ. In the current review, pVHI was the most frequently used, as it is easy to apply, validated in English, and has reported high intra- and interevaluator reliability. 6 Endoscopic evaluation, although important, can be particularly difficult in these cases due to the anatomic distortions secondary to the surgery and aperiodicity of the tissues with difficult synchronization under stroboscopic light, a finding also described by Alarcón et al.5,12 In the current studies, endoscopic evaluation was not a method for voice evaluation.
Acoustic measures in the studies were the those traditionally reported for voice assessment. Acoustic analysis can complement information on laryngeal functioning based on stability and amplitude of the mucoondulatory movement and provide evidence on the coordination between phonation and breathing. These measurements are obtained in a noninvasive fashion, and the results obtained may indicate the evolution of vocal quality over time, as well as aspects of vocal effort or fatigue, considering the maximum phonation time. Children, nevertheless, may need conditioning for appropriate performance of vocal tasks.
The population of children undergoing open airway surgery is unique and very particular. Most of these children have undergone a period of tracheostomy and experienced a major limitation to socialization with multiple hospital admissions and general medical manipulation. As the child grows, voice performance becomes more important. Baker et al pointed out that from 5 years of age to adolescence, the focus of families would be on children’s participation in sports and other activities, and after adolescence, the main focus would be on vocal quality and soundness for communication and professional use, 13 justifying ongoing reevaluation of these patients’ voices in the long term. Long-term speech therapy follow-up may be required after laryngotracheal reconstruction, 1 and reassessments into the teen years and adulthood will help perceive more objective handicaps.
To our knowledge, this is the first systematic review to summarize the current methods used to evaluate this population. Despite that, there is a limitation as this review presents, as predicted, great heterogeneity of methods used among studies. This is not unexpected since there is great variation in patients and laryngotracheal stenosis. The variability in methods used to evaluate these voices does not allow us to definitively conclude the superiority of one method over the other. However, based on this review and our personal experience, it is extremely important that future studies consider an approach tailored to the individual child that should include an association of a perceptual evaluation, acoustic measures, and a quality of life assessment. Also, reassessment over time should help define the variation of the impact on quality of life as vocal demands shift from social to labor needs. Multicentric discussion among airway teams and populational reports may help define the ideal manner in which to report voice results in the future and evaluate greater populations.
Conclusion
Multidimensional evaluations tailored to the individual child can be recommended after open airway surgery. CAPE-V scale, fundamental frequency, maximum phonation time, and pVHI are the most frequently used methods to evaluate voice outcomes and therefore may help broaden communication among authors. In the multitude of methods available, cognitive ability and degree of voice disturbance should be considered since they are the most important limiting factors in this population.
