Abstract
Objective
Laryngeal fractures are rare injuries; recent data describing these injuries and associated examination findings are limited. This study aims to describe injury etiology and outcomes associated with laryngeal fractures.
Study Design
Retrospective case series.
Setting
Academic tertiary center.
Methods
Patients with laryngeal fractures from 2005 to 2020 were identified in a retrospective chart review. Patient demographics, injury mechanisms, management, and voice outcomes were examined. Fracture type, radiologic, and endolaryngeal examination findings were analyzed for associations between fracture etiology and examination characteristics.
Results
Laryngeal fractures most commonly occurred at the thyroid cartilage. Fractures were most commonly due to sport-related injuries. Mechanism of injury was not associated with specific radiologic or endolaryngeal findings. Mechanism of injury was additionally not significantly associated with the need for intubation, surgical intervention, or tracheotomy. Fracture location was significantly associated with intubation requirement (P = .015), with 40% of patients with concomitant thyroid and cricoid fractures requiring intubation. Mechanism of injury significantly correlated with dysphonia at follow-up (P = .033). Mechanism of injury, fracture location, and surgical management were not associated with increased vocal fold injury or dysphonia.
Conclusion
There are no significant correlations between injury mechanism and fracture location, characteristics, radiologic findings, or endolaryngeal findings. These features emphasize the importance of a thorough and comprehensive laryngeal examination.
Laryngeal fractures are rare, accounting for <1 in 30,000 patients seen in emergency departments. 1 However, these injuries can be life-threatening and may require prompt identification and intervention. Motor vehicle collisions (MVCs) were historically the most typical cause of trauma to the larynx but have since decreased in incidence, likely related to auto safety features such as seat belts and airbags.1-3 More recent studies have demonstrated falls and blunt trauma as frequent causes of laryngeal injuries.4,5 Other common etiologies of blunt laryngeal trauma include sports and physical altercations. 6 Patients may present with a range of symptoms, such as dyspnea, neck pain, dysphonia, odynophagia, and hemoptysis, although these symptoms are nonspecific and patients may also be asymptomatic at presentation. 7 Laryngeal injuries and their long-term sequelae may even be overlooked as the severity of the symptoms does not always correspond with the extent of injury.
Laryngeal fractures are usually described via the Schaefer-Fuhrman classification system, which is based on clinical findings.1,8 With the advancement of diagnostic imaging and endoscopy, modifications to the original Schaefer classification combine clinical presentation and diagnostic findings from computed tomography (CT) and endoscopy to guide management. 9 The current workup for suspected laryngeal trauma consists of endoscopic examination and imaging to determine the severity of injury. 10 Laryngoscopy plays an essential role in the initial evaluation of patients with suspected laryngeal injury, as it allows the evaluation of mucosal injury and exposed cartilage and can provide real-time functional information such as vocal fold movement and phonation. Nevertheless, endoscopy is not always possible when massive edema is present. CT allows rapid and accurate detection of laryngeal injuries, minimizing the risk of airway compromise due to delayed treatment and hence preventing severe complications. However, radiologic diagnosis of fractures can be difficult, and diagnostic pitfalls exist, including variable and asymmetric ossification patterns11,12 and anatomic variants that can be confused for pathologic injury. 12 These challenges make prompt diagnostic evaluation with endoscopic and radiologic imaging an important part of the workup for suspected laryngeal injuries.
Due to the relatively rare incidence of laryngeal fractures, there remains a gap in the literature regarding diagnostic findings as they relate to outcomes and long-term management. Although some single-institution retrospective studies have described outcomes following laryngeal fractures,9,13-15 few studies have extensively compared endolaryngeal and radiologic findings with clinical outcomes. Herein we discuss the relationship between these findings through one of the larger known cohorts of patients with laryngeal fracture.
Methods
Approval for this study was obtained from the Institutional Review Board of Massachusetts Eye and Ear and Mass General Brigham. Retrospective chart analysis was performed on all patients presenting to Mass General Brigham from 2005 to 2020 with a diagnosis of laryngeal fractures. Patients who had laryngeal injury but no definitive fracture diagnosis were excluded, as were patients who presented with only hyoid fractures. Variables of interest included patient age, sex, mechanism of injury, management of injury, and voice outcomes.
Multidetector CT (Discovery 750 HD; GE Healthcare) was performed with 120 kV (peak) and 240 mA. Slice thickness was 2.5 mm for CT soft tissue neck, cervical spine, and angiography neck and 2 mm for CT larynx. For the majority of the studies (performed at our own institution), raw images were acquired in 0.625-mm increments and available for review as needed. Coronal and sagittal reformats were produced. Studies were variably acquired with or without intravenous contrast depending on the original ordering request submitted by the clinical service. For the available studies, breakdown of imaging technique is as follows: CT neck without contrast (33), neck with contrast (5), angiography neck (4), and C-spine (5) and magnetic resonance C-spine (1). The presence and absence of contrast did not affect analysis of fracture, edema, or hemorrhage. All images were uploaded to a PACS (picture archiving and communication system; Visage) for analysis. Additional reformats in nonstandard planes and/or 3-dimensional reconstructions were created at the PACS workstation by the radiologist as needed.
We systemically reviewed all available radiology studies obtained closest to time of injury for fracture location and characteristics. A neuroradiologist (A.F.J.) with 14 years of subspecialty head and neck radiology experience reviewed all cases. The reviewer was blinded to the original reports, patient demographics, and clinical diagnoses. Studies were reviewed in reformatted “true” axial, coronal, and sagittal planes in bone and soft tissue algorithms. These views were standardized across all patients by generating reformatted images prior to review such that all axial images were parallel to the plane of the true cords and all coronal and sagittal images were orthogonal to these standardized axial images. A fracture was defined as a visible discontinuity involving a laryngeal cartilage, regardless of extent and displacement. Displacement was defined as a visible offset in the involved cartilage fragments on either side of a fracture. Fracture lines that course along the axial plane (parallel to the x-y plane of the CT scanner) are considered “transverse”; those that course primarily in a vertical trajectory (parallel to the z-axis, perpendicular to the axial plane) are considered “vertical”; and those that do not conform to either of these but have components along the axial plane and z-axis are considered “oblique.”
All available video recordings of direct flexible laryngoscopy and stroboscopy examinations were examined for vocal fold injuries and soft tissue edema and hematoma by one subspecialty-trained laryngologist. Patients who reported voice changes after the laryngeal injury as a primary complaint were classified as having dysphonia, and patients who reported no voice changes from baseline were classified as having normal voice. All patients were asked about the presence of dysphonia on review of systems.
Descriptive and analytic statistics were performed in this study. Demographic factors, mechanism of injury, and outcomes were analyzed with Fisher exact tests. All statistical analyses were performed through Stata 15.1 (StataCorp). Statistical significance was defined as a P value <.05.
Results
Patient Demographics
In our study, 56 patients with diagnosed laryngeal fractures were identified from 2005 to 2020. The mean age was 39.7 years (range, 16-66; mean ± SD, 39.7 ± 12.7). Fractures were more frequently identified in males (80.4%) than females (19.6%). The most common fracture site was the thyroid cartilage (n = 36, 64.3%), followed by cricoid cartilage (n = 10, 17.9%) and multiple sites involving the thyroid and cricoid cartilage (n = 10, 17.9%). Injury severity classified according to the Schaefer-Furhman scale revealed that the majority of injuries were grade II (62.5%). One patient had a grade IV injury. Most patients were treated conservatively (n = 36, 64.3%); 19 (33.9%) were treated surgically. Surgical management included open reduction internal fixation (n = 13, 23.2%) or open reduction internal fixation and suspension microlaryngoscopy (n = 6, 10.7%). These results are summarized in Table 1 .
Demographics and Injury Features (56 Patients).
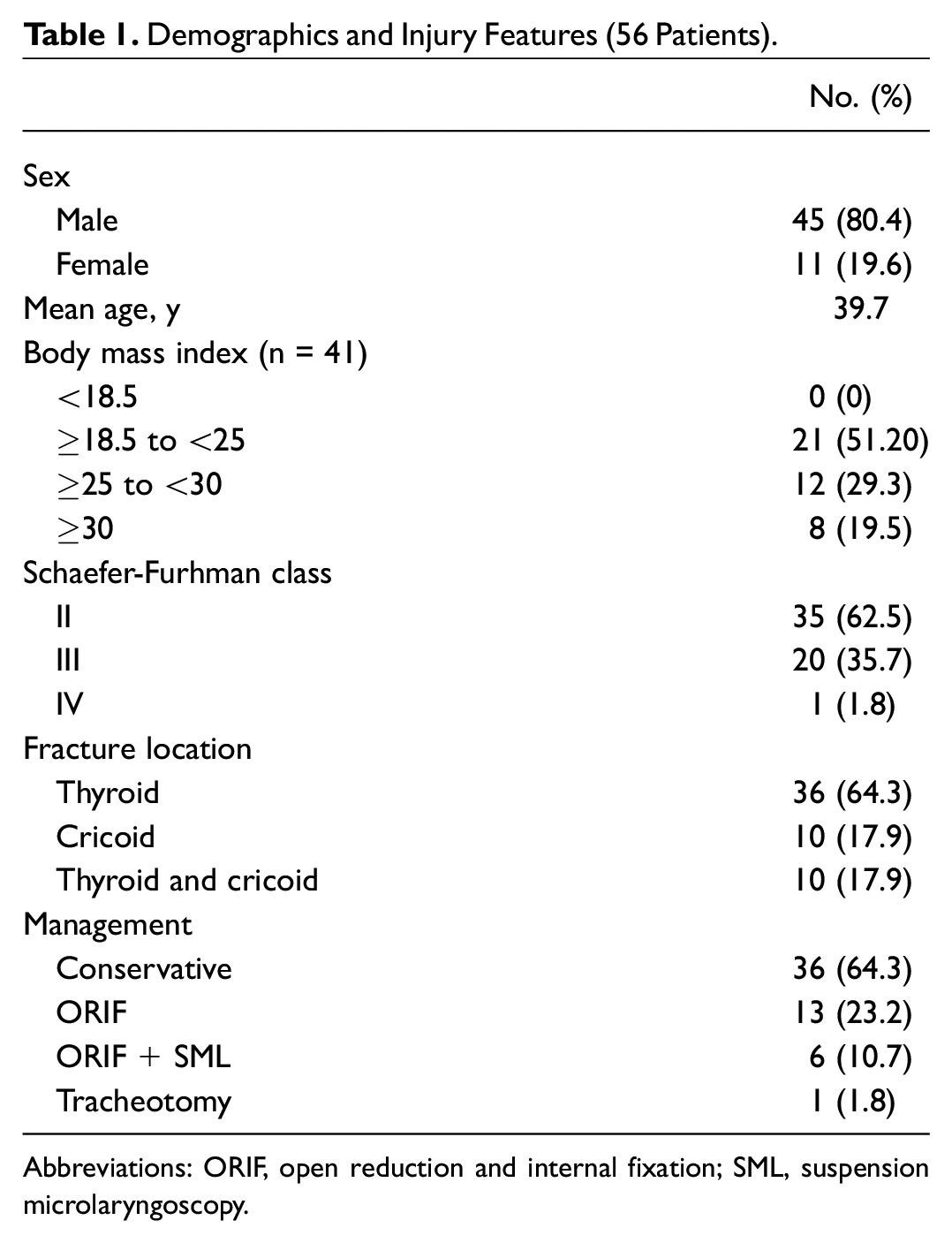
Abbreviations: ORIF, open reduction and internal fixation; SML, suspension microlaryngoscopy.
Fracture Location and Mechanism of Injury
The most frequent mechanism of injury was sport related (n = 27, 48.2%), followed by assault (n = 13, 23.2%), falls (n = 10, 17.9%), and MVCs (n = 6, 10.7%). Two patients had laryngeal fractures resulting from gunshot wounds while hunting, and another did not have any clear inciting mechanism. These patients were excluded from subsequent analysis due to their extensive nature (pan-fracture) and missing data. Overall, fracture displacement was more common in the thyroid cartilage than the cricoid cartilage, although neither was associated with a specific mechanism of injury ( Table 2 ).
Mechanism of Injury and Fracture Characteristics. a
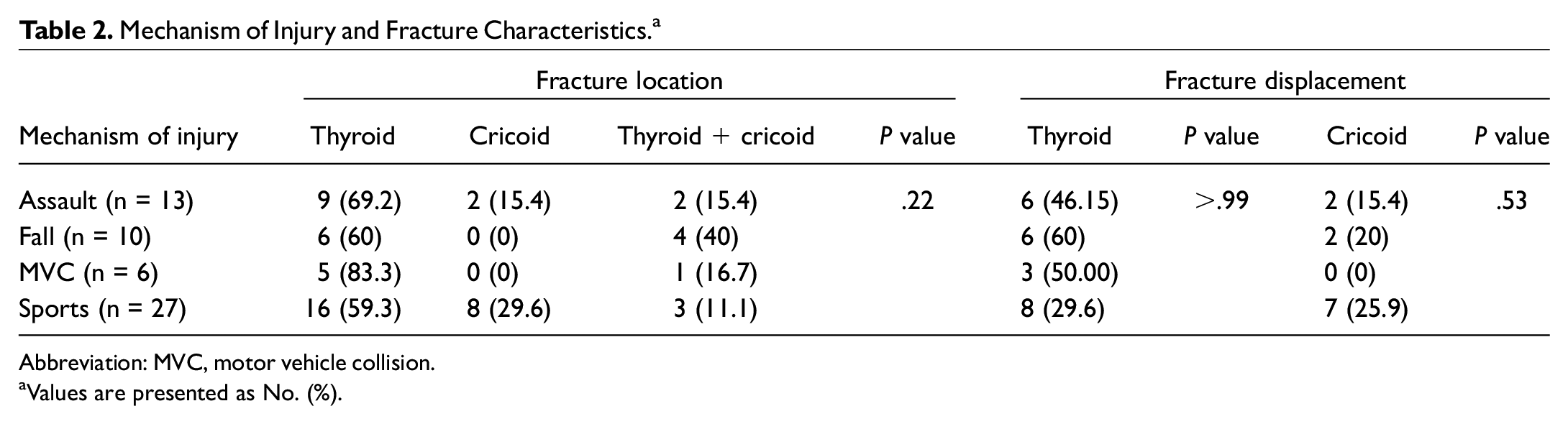
Abbreviation: MVC, motor vehicle collision.
Values are presented as No. (%).
Thirty-six patients (64.3%) in the data set had thyroid cartilage fractures. Of these patients, most thyroid cartilage fractures were vertical in orientation, occurring in 18 (50%) patients. Six (16.7%) had oblique fractures, 2 (5.6%) had transverse fractures, and 2 (5.6%) had complex fractures with vertical and oblique components. Ten patients (17.9%) had isolated cricoid fractures, of which 6 were vertical, 1 was oblique, and 1 was complex with vertical and oblique components. In the 10 patients with multiple thyroid and cricoid fractures, 7 thyroid fractures were vertical, and 7 cricoid fractures were also vertical. These findings are shown in Figure 1 .
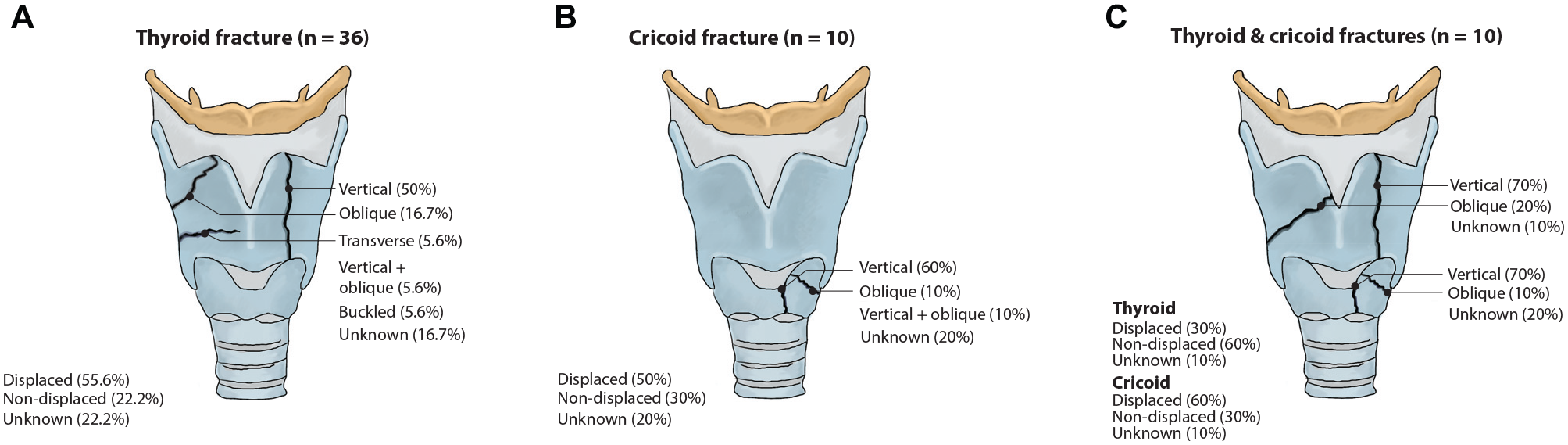
Laryngeal fracture types and fracture characteristics. Percentage of fracture displacement and fracture orientations in cohort categorized by type of fracture: (A) thyroid, (B) cricoid, and (C) concomitant thyroid and cricoid.
Among all mechanisms of injury, thyroid fractures were more common than cricoid fractures. Isolated cricoid fractures most frequently occurred in sport injuries, 29.8% of which were located in the cricoid. In the 10 patients who had falls resulting in laryngeal fractures, 4 (40%) had multiple thyroid and cricoid fractures. Thyroid and cricoid cartilage fractures were typically in the vertical direction, regardless of mechanism of injury. Assault and sport injuries resulted in complex thyroid cartilage fractures with vertical and oblique orientations. These findings are depicted in Figure 2 .
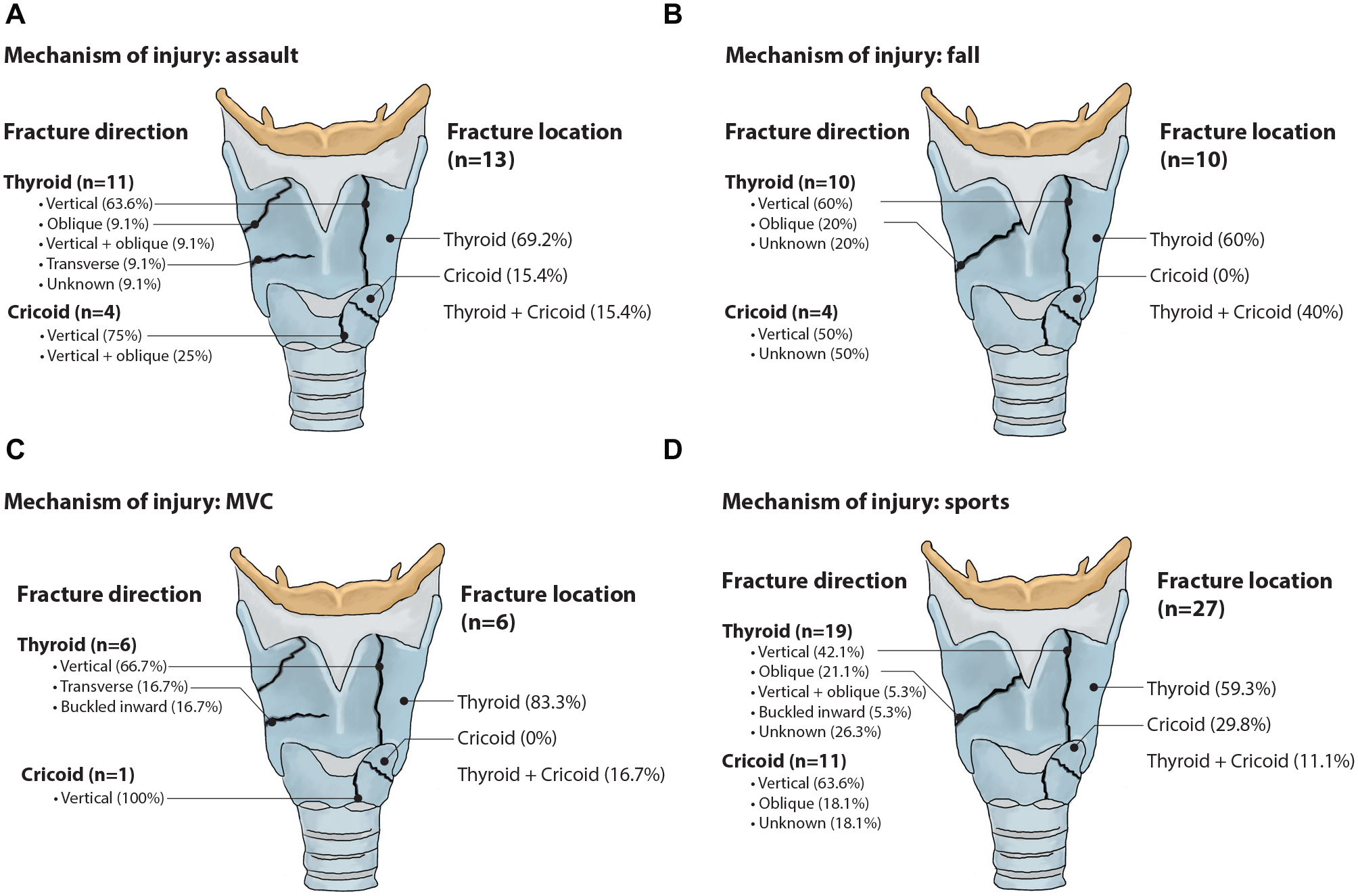
Mechanism of injury and fracture characteristics. Percentage of fracture orientations and fracture locations in cohort due to (A) assault, (B) fall, (C) MVC, or (D) sports. MVC, motor vehicle collision.
Mechanism of Injury and Endolaryngeal Findings
Available endolaryngeal examinations at the most immediate follow-up encounter postinjury were reviewed. The presence of edema and/or hematoma on examination was determined, and the location of soft tissue findings was categorized into supraglottic, glottic, and subglottic regions. Edema was most commonly seen with sport injuries, regardless of location or time of follow-up. For patients with sport-induced laryngeal injuries who had follow-up assessment between 1 week and 1 month, 35% had supraglottic edema, 40% had glottic edema, and 5% had subglottic edema. Of patients who had follow-up at >1 month, 42.9% had persistent supraglottic edema, and 28.6% had persistent glottic edema. No subglottic hematoma was seen in any patients after 1 month of follow-up. All other endolaryngeal edema and hematoma findings are described in Table 3 .
Mechanism of Injury and Endolaryngeal Examination Findings. a
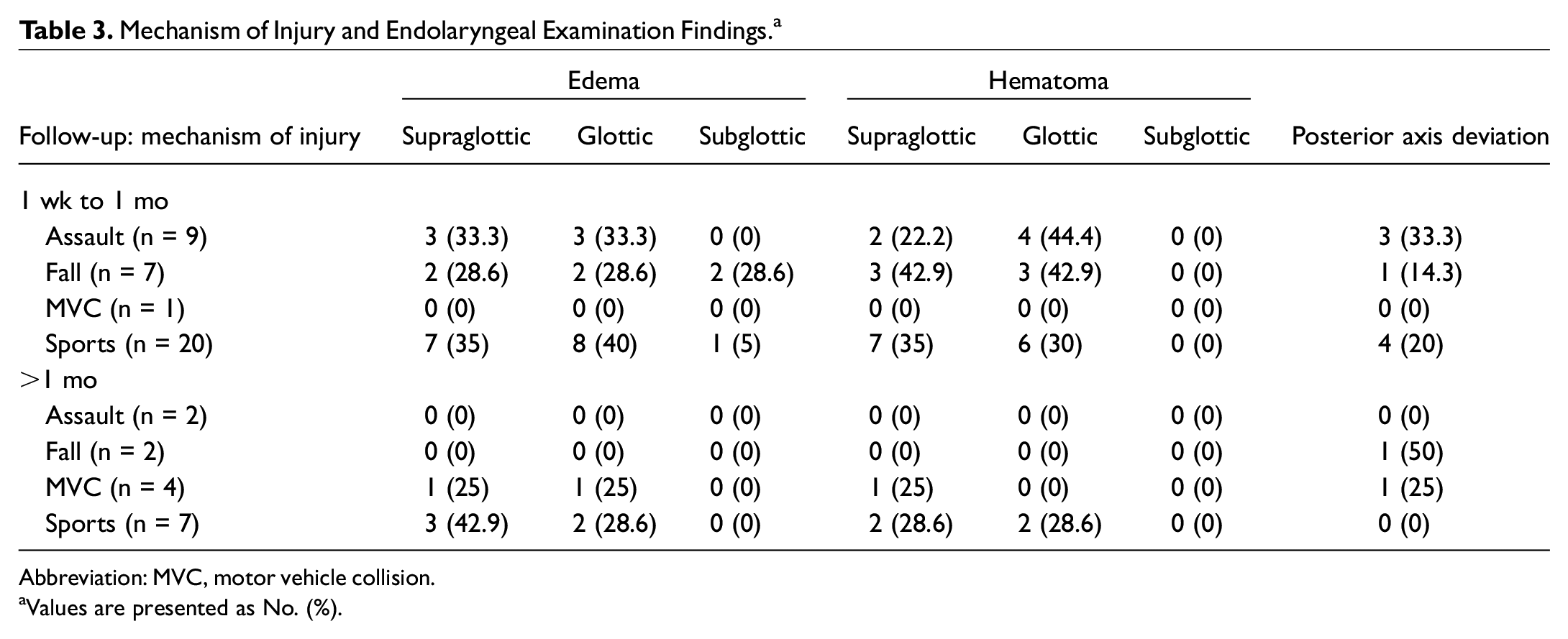
Abbreviation: MVC, motor vehicle collision.
Values are presented as No. (%).
Interventions
Thirty-five patients (62.5%) were treated conservatively without the need for surgical intervention. Twenty-one (37.5%) required surgical management, 5 of whom were intubated in the field or in the emergency room. Another patient was intubated in the field and treated conservatively after airway stabilization. Of the patients who were surgically treated, most (n = 19, 90.5%) had injuries that were Schaefer-Furhman class III or above.
Notably, there was no significant association between mechanism of injury and intubation, tracheotomy, or surgical intervention ( Table 4 ). However, when the characteristics of laryngeal fractures were evaluated, fracture location was significantly associated with the need for intubation (P = .015). Specifically, there was a significant increase in the incidence of intubation for patients who had multiple thyroid and cricoid fractures (40%) when compared with isolated thyroid (5.6%) or cricoid (0%) fractures. There was no association between other laryngeal fracture characteristics and the incidence of tracheotomy or need for other surgical management. Schaefer-Furhman class was significantly associated with requiring intubation (P = .03), tracheotomy (P < .001), and surgery (P = .001).
Injury Characteristics and Interventions. a
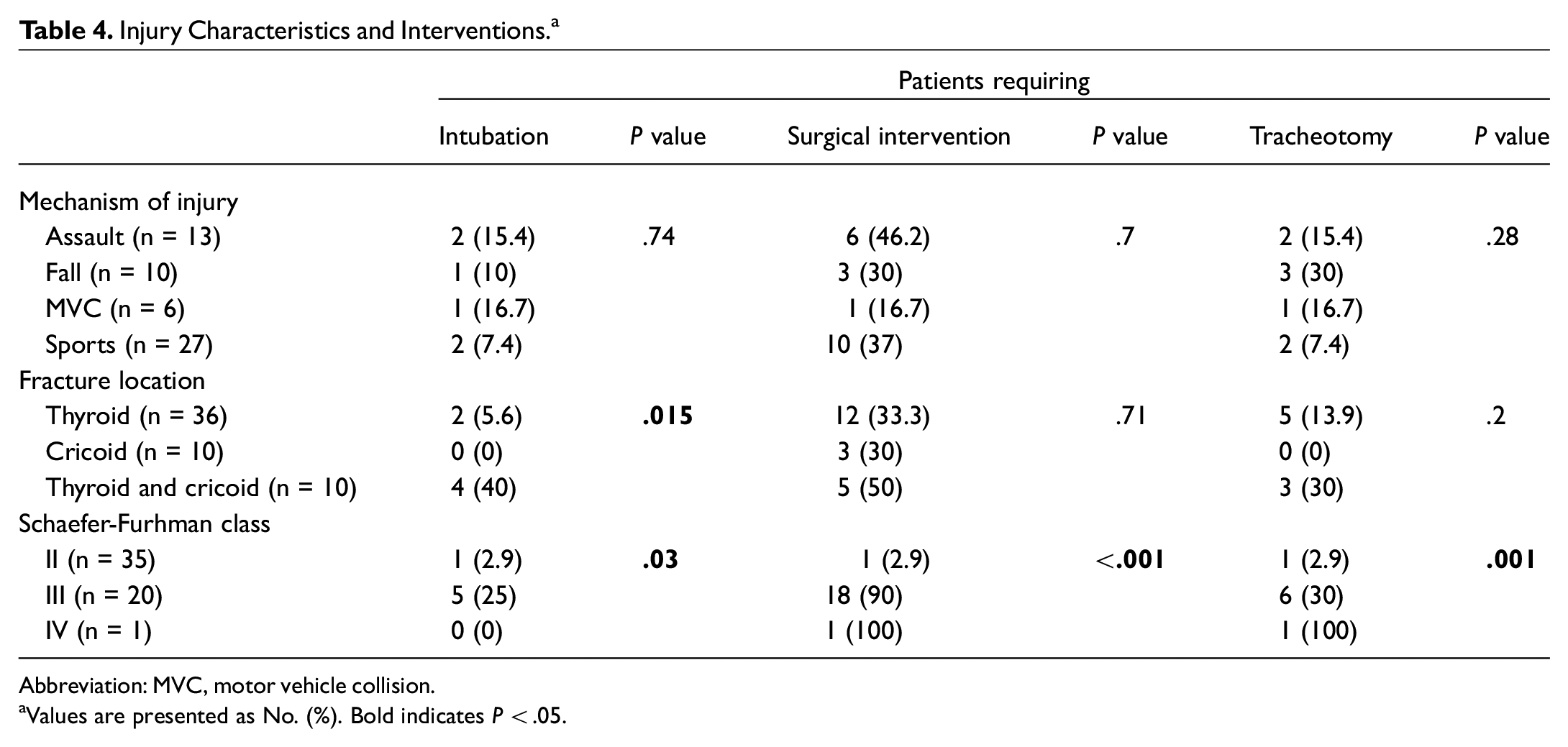
Abbreviation: MVC, motor vehicle collision.
Values are presented as No. (%). Bold indicates P < .05.
Vocal Fold Injury and Voice Outcomes
In our cohort, 34 patients had follow-up where the presence of vocal fold injury and voice outcomes were documented. Mechanism of injury was not associated with vocal fold injury. Most patients, regardless of mechanism of injury, did not have vocal fold paralysis. Vocal fold hypomobility was seen in all 4 patients with injury due to MVCs. Fracture location, Schaefer-Furhman class, and surgical management were not significantly associated with vocal fold injury. However, hoarseness and dysphonia were noted in 16 (47.1%) patients and were significantly associated with mechanism of injury (P = .033). Laryngeal fractures due to falls had the highest incidence of dysphonia (100%), and those due to sport injuries had the lowest (27.8%). These results are summarized in Table 5 .
Vocal Fold Findings and Voice Outcomes.
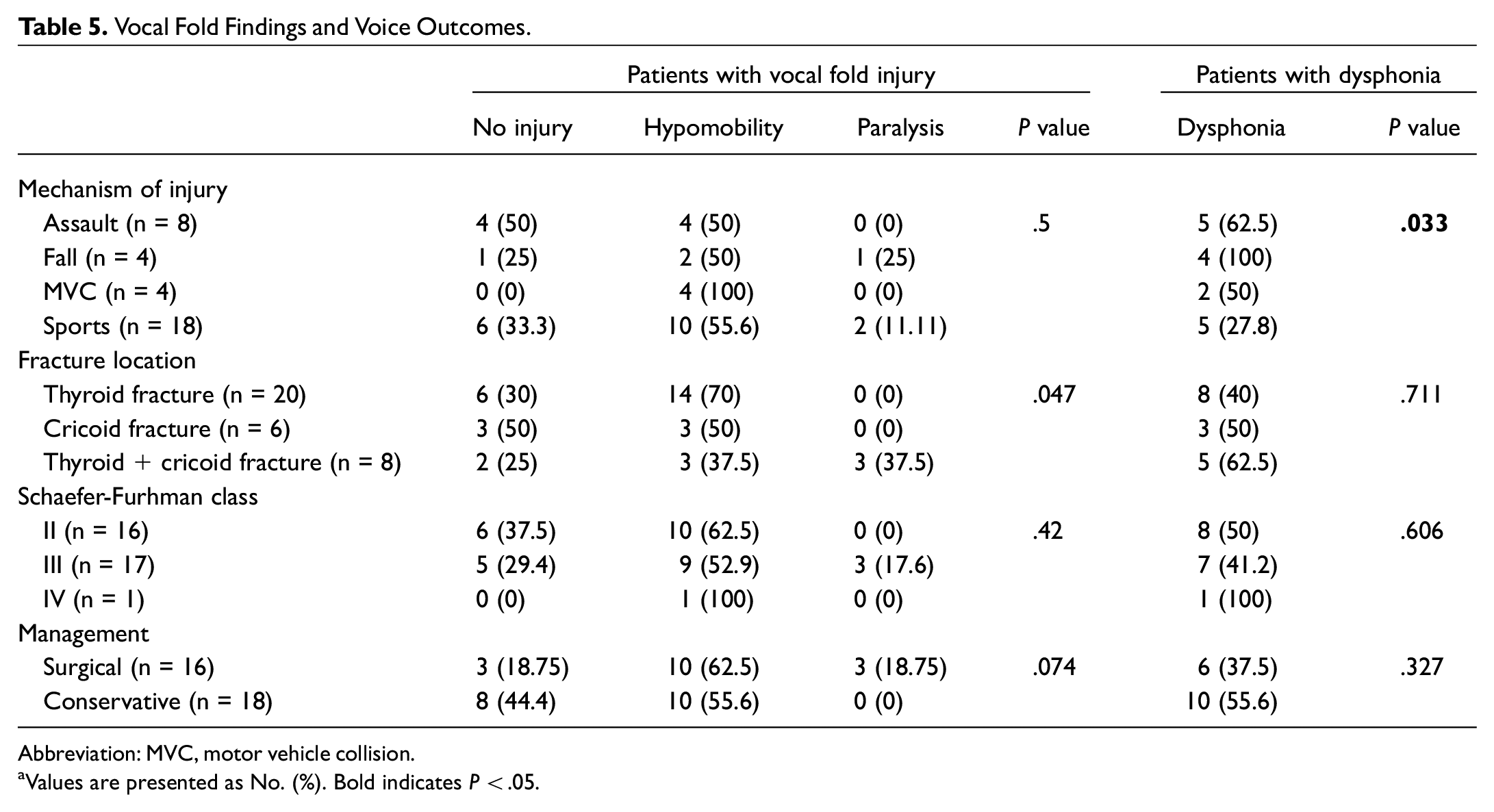
Abbreviation: MVC, motor vehicle collision.
Values are presented as No. (%). Bold indicates P < .05.
Discussion
Etiology of Injury
Historically, MVCs were often the most common cause of laryngeal injuries3,10 but have since decreased likely due to the implementation of motor vehicle safety features and air bags. 3 Our cohort provides a more recent assessment of laryngeal fractures wherein sport-related injuries were the most frequent cause of laryngeal fractures, followed by assault. It is important to note that a variety of injuries and accidents can result in laryngeal fractures, with some less obvious causes, such as a fall, high-velocity sport object (baseball, lacrosse ball, or hockey puck), or elbow to the neck. There was a trend that higher-velocity sport injuries, such as hockey puck trauma, resulted in more focal and less obvious injuries than those associated with assault and MVC. Clinicians need to have a high degree of suspicion in situations where individuals have sustained trauma of any kind to the unprotected neck. Delayed recognition and management of such injuries may lead to long-term voice, airway, and swallowing complications.14,16
Radiologic and Endolaryngeal Findings
Presenting symptoms of laryngeal injury are nonspecific, and patients are often asymptomatic. Thus, patients with suspected laryngeal injuries should be evaluated with imaging and endoscopy. CT is the preferred imaging modality for initial evaluation17-19 and can be especially useful in patients who have suspected laryngeal injuries. In our cohort, we did not see any laryngeal fracture patterns that correlated with a specific mechanism of injury. Isolated cricoid fractures were seen only in assault and sport injuries, but no mechanism of injury was predictive of multiple thyroid and cricoid fractures. Similarly, Buch et al did not see significant associations between mechanism of injury and fracture location or focality (multi- or single-site fracture) on CT imaging. 20 This suggests that regardless of pan-traumas from MVCs or isolated injuries to the neck from sports, CT should be obtained to diagnose and characterize laryngeal fractures and guide further management.
We additionally did not see any correlation between mechanism of injury and soft tissue findings on endolaryngeal examination. However, endolaryngeal examination remains a critical component of evaluation and follow-up of laryngeal fractures, as it allows timely identification of vocal fold injuries and soft tissue swelling. At >1-month follow-up after injury, few patients in this cohort had edema or hematoma on endolaryngeal examination, suggesting that patients generally do well after laryngeal fractures. Although our sample size is small, it is likely that patients who were lost to follow-up were asymptomatic with resolved soft tissue findings.
Interestingly, mucosal and soft tissue injury can be present contralateral to the side of fracture. Cases have been described where hockey players sustaining injury ipsilateral to local external soft tissue edema and cartilaginous fracture had contralateral vocal fold hemorrhage or mucosal injury of the vocal process.21,22 In our cohort, we did not find significant correlation between side of fracture and endolaryngeal findings. Multiple patients had significant injury at the contralateral endolarynx relative to site of injury. Three patients (1 fall downstairs, 1 collision with edge of table, 1 hockey puck strike) had laryngeal fractures on the left but sustained right vocal fold avulsion and had soft tissue findings predominantly on the right side on endolaryngeal examination. This supports previous observations that there may be multiple mechanisms of injury. Damage from the initial impact to the larynx is likely responsible for the laryngeal fracture. In addition, compression of the posterior larynx against the spine, with subsequent rebound injury as the laryngeal cartilage structures snap back into position, can avulse or dislocate the arytenoid, which likely explains the soft tissue injuries observed on the contralateral side. Thus, it is important to be cognizant that injuries may lead to contralateral mucosal and soft tissue findings and that endolaryngeal findings may be unpredictable and not necessarily match the side of injury.
Interventions
Our study showed that fracture location was significantly associated with intubation. When patients presented with concomitant thyroid and cricoid fractures, intubation was necessary in 40%. This may be attributed to an increased extent of endolaryngeal edema due to the presence of multiple fractures. Thus, a presentation of multiple laryngeal fractures may be more severe in nature. Unlike fracture location and number, mechanism of injury in our study was not predictive of needing airway intervention, although Randall et al found MVC-related injuries to be significantly associated with airway intervention. 7 Most patients in this cohort were treated conservatively, and most Schaefer-Furhman class III and IV injuries were managed surgically.
Vocal Fold Findings and Voice Outcomes
One of the goals of early detection and intervention on laryngeal fractures is the restoration of functional voice. Although there was a significant association between mechanism of injury and dysphonia, it is interesting that there was no difference in voice outcomes between surgically and conservatively treated patients. This suggests that surgical management, when appropriate, does not lead to a higher incidence of vocal fold injuries or worse voice outcomes. In our cohort, 5 patients had initial voice outcomes that were inadequate for functioning; 3 had improvement to being acceptable for functioning; and 2 returned to baseline prior to injury. In general, most patients seem to have minimal voice compromise at long-term follow-up. This is consistent with observations made in previous studies.14,23
Our study has several limitations, such as the small sample size and retrospective design. The small sample size is reflective of the relatively low incidence of laryngeal fractures. When outcomes were assessed, patients were often lost to follow-up. Due to the retrospective nature of our study, certain omissions in data or incomplete records were inevitable. The majority of radiologic studies were obtained at our own institution; however, some imaging studies obtained at the time of injury were performed at outside institutions, which may lead to variations in protocol and image quality. The geographic location of our center and overall patient demographic may have additionally resulted in bias toward certain mechanisms of injury (eg, a greater propensity for blunt vs sharp trauma at our institution). Our cohort may not be fully representative of patient presentation and management at other institutions. Further investigation including multi-institution studies will be helpful to fully understand the important mechanisms of injury, imaging findings, and voice outcomes for this rare pathology.
Conclusion
Laryngeal fractures occur via a range of mechanisms, from isolated focal impact or sport injury to MVC. A high degree of suspicion for the presence of laryngeal fracture must be maintained in anyone who presents with trauma to the neck. In cases where multiple laryngeal fractures are present, there is a greater associated need for intubation. Although surgical intervention is not always required, early identification of such injuries and full evaluation with imaging and endolaryngeal examination are necessary to avoid negative long-term sequalae.
