Abstract
Objective
We analyzed the incidence of facial nerve sacrifice during parotidectomy for metastatic cutaneous squamous cell carcinoma (CSCC).
Study Design
We retrospectively reviewed the charts of patients with cutaneous squamous cell carcinoma.
Setting
We used our CSCC institutional database, which includes patients treated at the University of California–Davis from 2001 to 2018.
Methods
We evaluated patients who presented with biopsy-proven head and neck CSCC who underwent parotidectomy as a part of surgical treatment. We assessed the frequency of facial nerve sacrifice required in patients with normal preoperative facial nerve function with metastatic disease to the parotid. We evaluated the association between sacrifice and high-risk tumor variables using multivariate analysis.
Results
We identified 53 patients with parotid metastasis and normal preoperative facial nerve function. Thirteen percent of patients required sacrifice of the main trunk of the facial nerve and 27% required sacrifice of a branch of the facial nerve. All patients who underwent facial nerve sacrifice had extracapsular spread (ECS). Perineural invasion (PNI) in the primary tumor (odds ratio [OR], 9.11;
Conclusion
Patients with regionally metastatic CSCC to the parotid gland frequently require sacrifice of all or a component of the facial nerve despite normal preoperative function. The likelihood of nerve sacrifice is highest for tumors with PNI and metastatic disease within the body of the parotid.
Nonmelanoma skin cancer is the most commonly diagnosed malignancy in the United States, with cutaneous squamous cell carcinoma (CSCC) representing about 20% of those cases. 1 It is estimated that there are 700,000 patients diagnosed with CSCC each year in the United States, and the incidence has been increasing worldwide.2,3 Most tumors are found within the sun-exposed areas of the head and neck.
Most CSCCs require only local treatment, but a subset of patients present with regionally metastatic disease. Although the overall incidence of regional metastasis is reported to be as low as 5% or less, certain tumor characteristics are associated with a greater risk of metastasis. 4 These include high-risk tumor location, greater diameter, increased depth of invasion, poor histologic grade, lymphovascular invasion (LVI), perineural invasion (PNI), and recurrent tumor.5-8 The parotid lymph nodes are the most common first echelon site of metastatic spread for CSCC of the head and neck. 9
Metastatic involvement of lymph nodes within the parotid gland poses a therapeutic challenge. Surgical resection via comprehensive parotidectomy is recommended with the goals of complete removal of tumor and preservation of nerve function. However, the involved nodal disease is often in close proximity or directly involving the facial nerve, and nerve sacrifice is sometimes necessary to achieve microscopic or gross total resection. This can be difficult to predict in the setting of normal preoperative facial nerve function, and there are limited data on what factors are associated with greater risk of nerve sacrifice. In addition, philosophies differ between surgeons on when to preserve the nerve in the setting of close or positive margins. 9
Our objective was to analyze the incidence of facial nerve sacrifice during parotidectomy for metastatic CSCC of the head and neck and to determine what tumor characteristics are associated with a higher risk of sacrifice.
Materials and Methods
We conducted a retrospective chart review of patients with CSCC treated at University of California–Davis. We received institutional review board approval from the UC Davis Comprehensive Cancer Center Scientific Review Committee to collect patient data by querying the electronic medical records of patients with biopsy-proven CSCC of the head and neck who were treated in the otolaryngology department between January 2001 and December 2018. The study population was composed of patients with resectable CSCC of the head and neck who underwent parotidectomy as part of their surgical treatment. We included patients who had pathologically proven metastatic disease to the parotid gland that was distinct from their concurrent or historical primary. This included patient with synchronous, historical, and unknown primary tumors. We excluded patients with distant metastatic disease and those with any preoperative facial nerve dysfunction. In our practice, facial nerve sacrifice was performed only when there was gross evidence of direct invasion onto or around the facial nerve. Close (<1 mm) but microscopically negative margins were generally tolerated if required to save facial nerve branches.
Clinical and pathologic factors were identified and recorded, including age at diagnosis, sex, primary vs recurrent tumor, primary tumor location, American Joint Committee on Cancer (AJCC) eighth edition pathologic T stage, histologic grade, LVI, PNI, both clinical and pathologic nodal status, metastatic nodal size, and extracapsular spread (ECS). Primary tumor location was categorized as “high risk” or “low risk” based on National Comprehensive Cancer Network (NCCN) criteria. 10 Metastatic nodal size was grouped into those less than or equal to 3 cm and those greater than 3 cm, consistent with AJCC thresholds for pathologic nodal staging. Histologic grade was recorded as either poor or moderately to well differentiated. We also identified extent of parotidectomy performed (superficial, total, or radical) and location of metastasis in the parotid (body or tail).
Statistical analyses were performed with SPSS (SPSS, Inc). Descriptive statistics were computed for clinical and demographic data. The significance of univariate associations between patient and tumor characteristics, including recurrent tumor, location of nodal metastasis within the parotid gland, nodal size, ECS, LVI, PNI, and histologic grade, with facial nerve sacrifice was assessed via χ2 analysis. A multivariate logistical regression was used to determine factors independently associated with nerve sacrifice. Statistical significance was defined as a
Results
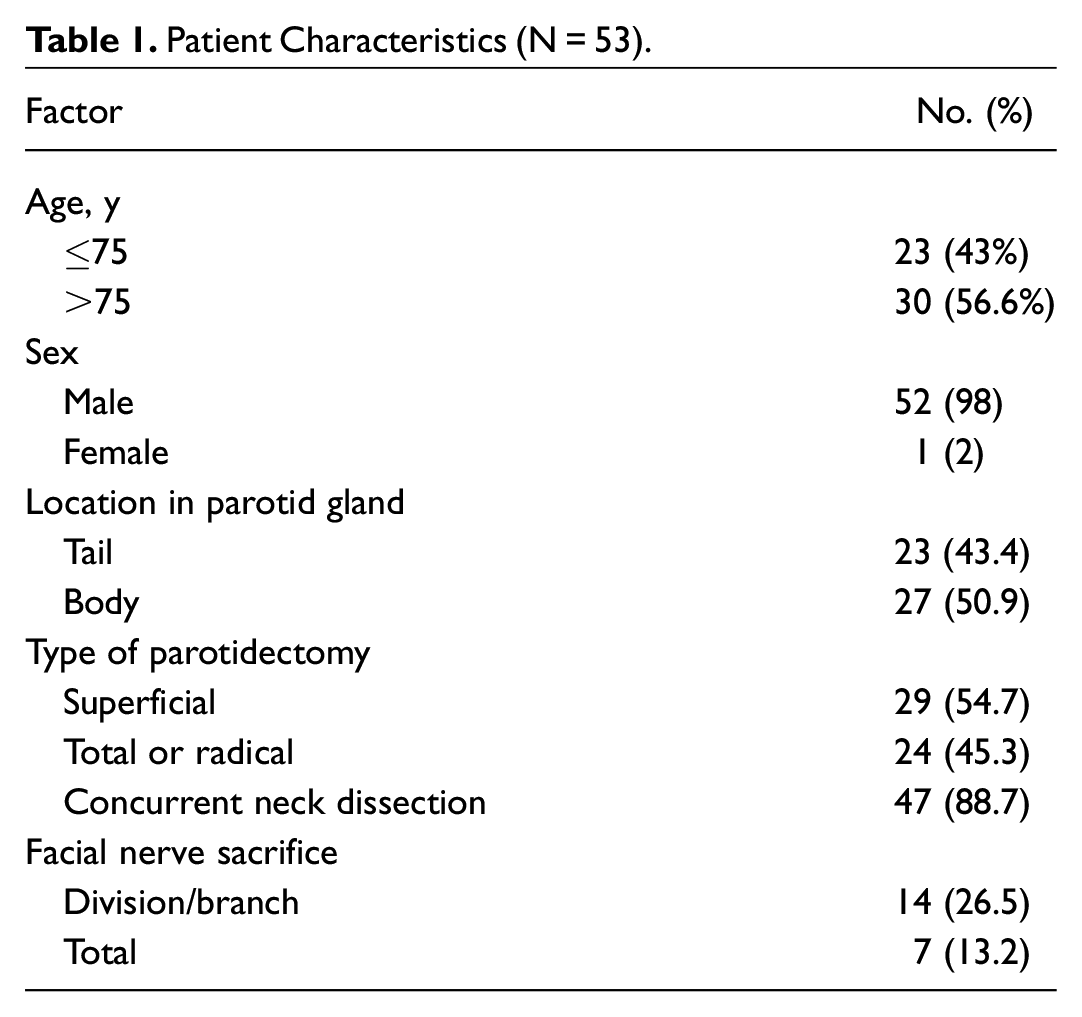
A total of 259 patients with advanced CSCC were identified. Of those, we identified 53 patients with both nodal disease in the parotid and normal preoperative facial nerve function. These results are summarized in Table 1 . We had complete data on the primary tumor in 46 of the 53 patients. The mean (SD) age of the patients analyzed was 75 (4.1) years, with the large majority being male (98.1%). Most patients (83.0%) were presenting with a recurrence from a previously treated CSCC. Despite patients having normal preoperative facial nerve function, 27% required sacrifice of a branch of the facial nerve and an additional 13% required total nerve sacrifice to achieve a negative margin resection. These results are summarized in Table 2 . The mean parotid node diameter was 3 cm, and 85% demonstrated ECS, which is reflected in the high proportion of patients with advanced nodal stage according to the AJCC eighth edition. Twenty-two patients (41.5%) had primary tumors with PNI, and 18 (34%) tumors had poorly differentiated histologic grade.
Patient Characteristics (N = 53).
Tumor Characteristics.
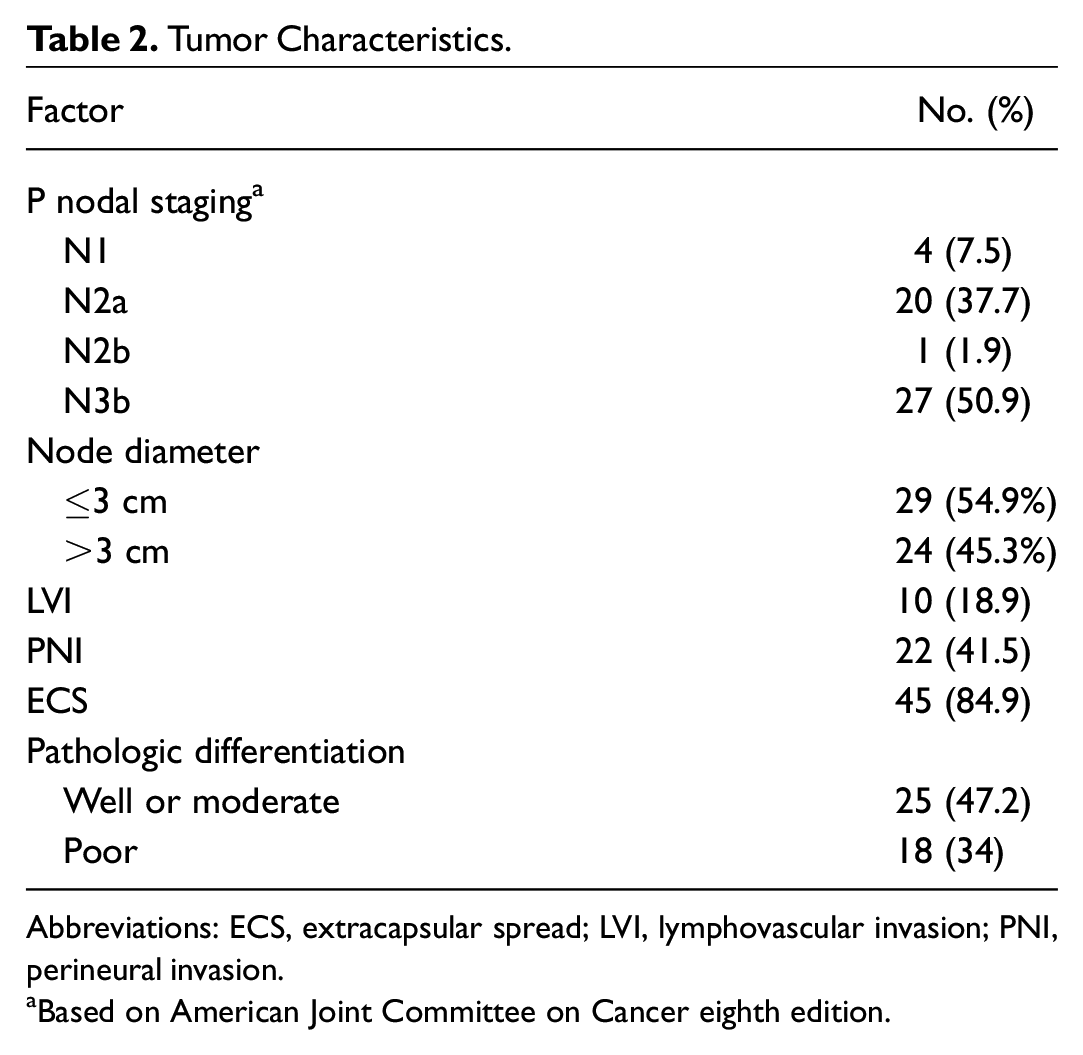
Abbreviations: ECS, extracapsular spread; LVI, lymphovascular invasion; PNI, perineural invasion.
Based on American Joint Committee on Cancer eighth edition.
On univariate analysis (
Table 3
), tumors located in the body of the parotid gland were more likely to require facial nerve sacrifice when compared to tumors in the tail of the gland (
Univariate Association of Factors With Nerve Sacrifice. a

Abbreviations: ECS, extracapsular spread; LVI, lymphovascular invasion; PNI, perineural invasion.
Bold indicates statistical significance (
Factors Associated With Nerve Sacrifice: Multivariate Logistical Regression. a
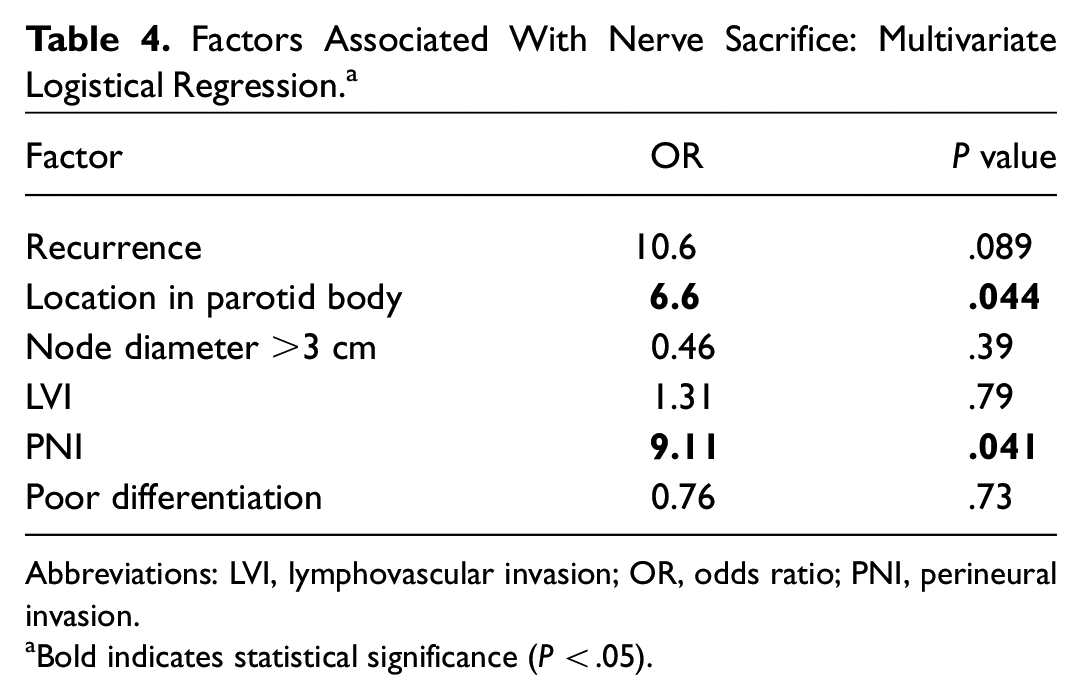
Abbreviations: LVI, lymphovascular invasion; OR, odds ratio; PNI, perineural invasion.
Bold indicates statistical significance (
Discussion
CSCC is the second most common type of nonmelanoma skin cancer and is increasing in incidence worldwide. The rate of metastasis remains low, but tumors with metastatic spread display more aggressive behavior, higher rates of recurrence, and worse overall prognosis.6,11 The most common site of metastatic spread from CSCC of the head and neck is the intraparotid lymph nodes.
Surgical resection of parotid metastases presents a unique challenge due to the close proximity of the intraparotid lymph nodes to the branches of the facial nerve. Abutment of involved lymph nodes to the facial nerve or ECS into the parotid parenchyma can necessitate sacrifice of all or branches of the nerve to achieve complete resection. In patients with intact preoperative nerve function, it can be difficult to predict those patients who will require sacrifice based on clinical exam and radiographic imaging alone. There have been no studies to date evaluating tumor characteristics associated with facial nerve sacrifice, and we sought to identify those features.
We found that despite normal preoperative facial nerve function, parotid metastasis in CSCC carries significant risk of facial nerve sacrifice. In our cohort, 27% of patients required resection of at least 1 branch or division, and an additional 13% required total nerve resection. Other studies have cited similar rates of partial or total nerve sacrifice (30%-40%) for CSCC with parotid metastasis.9,11,12
There are differing philosophies regarding nerve sacrifice in the setting of close margins to the nerve. Oncologic surgical doctrine would suggest a wide margin of normal tissue, as positive margins in CSCC have been associated with local recurrence. 13 Tolerating a close margin in the interest of nerve preservation has been advocated for when relying on adjuvant radiation for eradication of residual, microscopic disease. Iyer et al 14 reported no decline in local control or survival in patients in whom a positive margin was tolerated to preserve facial nerve function when patients were treated with adjuvant radiation. In large studies, the overall efficacy of postoperative radiation has been associated with improved outcomes in CSCC patients with high-risk features such as nodal disease or PNI.8,15 More data are necessary to determine the appropriate extent of surgery in patients with metastatic CSCC to the parotid.
Extracapsular extension into the parenchymal tissue makes achieving negative margins especially difficult. There was a remarkably high rate of ECS (85%) observed in our patients. We found that facial nerve sacrifice was required only in patients with ECS, as tumor was consequently invading the surrounding gland parenchyma and onto or around the facial nerve. Prior studies have also reported a high rate of ECS (70%) in metastatic disease to the parotid lymph nodes. 13 The rate of ECS observed within parotid lymph nodes is higher than that typically observed for metastatic disease to cervical lymph nodes in both mucosal and cutaneous SCC (50%-60%).16-18 The pathophysiological mechanisms driving this aggressive pattern of spread within the parotid as compared to cervical nodes remain unclear.
We found that metastasis within the parotid body vs the tail of the gland was an independent predictor of facial nerve sacrifice (OR, 9.1;
Our study also found that PNI identified in the primary lesion was independently associated with facial nerve sacrifice (OR, 6.6;
The results of our study are helpful for preoperative surgical planning in terms of predicting the likelihood of facial nerve sacrifice. Primary tumors with known PNI on diagnostic biopsy or preoperative imaging suggestive of extracapsular extension into the parotid parenchyma provide information for improved counseling on expected outcomes. If nerve sacrifice is anticipated, the surgeon can plan for adjunctive procedures such as nerve reconstruction, reanimation techniques, and eyelid augmentation.
Our study suffers from the intrinsic limitations of any single-institution, retrospective review, including potential errors in data acquisition from chart review. Many of our patients had resection of a historic primary lesion by an outside provider, and as such, we were unable to capture complete data on all original tumors. Our sample size was also limited given this unique cohort of patients, and we may be underpowered to detect association of other tumor factors with the incidence of facial nerve sacrifice. Despite these imitations, this is the first study to date evaluating factors associated with nerve sacrifice in metastatic CSCC and offers a novel set of data that can help inform head and neck surgeons.
Conclusion
Metastatic CSCC to the parotid gland frequently presents with ECS, and a high proportion of patients ultimately require sacrifice of 1 or more facial nerve branches. The likelihood of nerve sacrifice is highest in patients with nodal disease within the body of the parotid gland and in tumors with PNI. These findings can inform head and neck surgeons as they plan for parotidectomy in patients with regionally metastatic CSCC.
Author Contributions
Disclosures
Footnotes
This article was presented at AAO-HNS 2019 Annual Meeting & OTO Experience; September 16, 2019; New Orleans, Louisiana.
