Abstract
Objective
The uncinate process may play a role in the amount of irrigation penetrance. In this cadaver study, we aimed to investigate if the addition of partial uncinectomy provides better maxillary sinus irrigation penetrance than balloon sinuplasty (BSP) alone.
Study Design
Cadaveric study.
Setting
Simulation laboratory at the Mayo Clinic in Florida.
Methods
Five fresh-frozen human cadaveric heads (10 sides) were used to assess maxillary sinus irrigation penetration after 3 interventions performed sequentially: irrigation penetrance with no intervention, irrigation after BSP, and irrigation after BSP and partial removal of the uncinate. Penetrance was recorded with intrasinus endoscopy and scored by 4 blinded observers using a scale from 0 (no irrigation) to 5 (fully irrigated). The diameter of the maxillary ostium was measured before and after BSP. Internal consistency was evaluated with Cronbach’s alpha.
Results
Mean ostium size increased from 4.1 to 6.8 mm after BSP (P = .013). Cronbach’s alpha was 0.93. The median scores of irrigation penetration after no intervention, BSP, and BSP and partial uncinectomy were 2.5, 3, and 4, respectively. We found a significantly higher penetrance following partial uncinectomy plus BSP versus BSP alone (P = .008). Both interventions had a statistically significant difference in irrigation penetrance as compared with no intervention (P = .0001).
Conclusion
Maxillary sinus irrigation penetration increased from baseline after BSP. The addition of a partial uncinectomy to the balloon dilation of the maxillary sinus was associated with a statistically significant increase in irrigation penetrance scores as compared with BSP alone.
Chronic rhinosinusitis (CRS) affects 5% to 12% of the general population.1,2 It has a greater impact on social activities than other chronic conditions, such as congestive heart failure, chronic obstructive pulmonary disease, back pain, and angina. 3 The maxillary sinus is commonly involved in CRS. The maxillary sinus is predisposed to stasis due to the location of its natural opening, the presence of anatomic variations (eg, concha bullosa, septal deviation), and the presence of other sinonasal pathologies affecting mucous drainage. 4 Causes of maxillary sinus disease include odontogenic etiologies, inflammatory sinus disease, maxillary sinus atelectasis, mucocele, mycetoma, and antrochoanal polyp. 4 Some of these conditions may be amenable to balloon sinuplasty (BSP), which has become popular since its Food and Drug Administration approval in 2005. 5 In fact, Medicare data from 2012 to 2016 showed that BSP use increased from approximately 26% to 58% of all sinus procedures during that time frame. 6 Studies suggest that the rapid adoption of this procedure is likely associated with its higher patient satisfaction rates, fewer days of postoperative narcotic analgesics, and lower risk of scarring.5,7-10
Multiple studies have confirmed the safety of BSP and its role as a valuable addition to the surgical armamentarium for patients with CRS.7,8,11 Based on the American Academy of Otolaryngology–Head and Neck Surgery Foundation’s statement on balloon dilation, there was expert consensus on 3 main criteria for BSP: recurrent acute bacterial rhinosinusitis, hybrid procedures with endoscopic sinus surgery (ESS) in patients with CRS without nasal polyps, and persistent sinus symptoms of CRS without nasal polyps in patients with previous sinus surgery. 12
According to the current literature, the extent of irrigation penetration into the sinuses is associated with the size of the sinus ostium, the volume of irrigation device, head position, and nasal anatomy.13-15 Some of the major benefits of BSP are the increase in sinus ventilation and more effective delivery of topical medical therapy. A few cadaver studies in the literature have discussed nasal irrigation penetration of maxillary sinuses based on factors such as head position, sinus ostium size, and type of delivery device.13,16-18 Of the studies that specifically cite maxillary sinus penetrance, results have been conflicting. Brenner et al reported that maxillary sinus nasal irrigation penetrance decreased after BSP, suggesting that the anteromedial displacement of the uncinate process (UP) may have played a role. 16 Gantz et al, however, found a statistically significant improvement in irrigation penetrance in the maxillary sinus after BSP. 19 The purpose of this cadaver study is to add to our understanding of the effect of BSP on maxillary sinus irrigation and to investigate if the addition of a partial uncinectomy to the balloon dilation procedure provides better irrigation penetrance than BSP alone.
Methods
After Mayo Clinic Institutional Review Board approval (19-001535), 5 thawed fresh-frozen human cadaveric heads were used for this study. The handling, storage, and laboratory use of these specimens were performed in the dissection laboratory of the Simulation Center in the Mayo Clinic in Florida.
Study Design
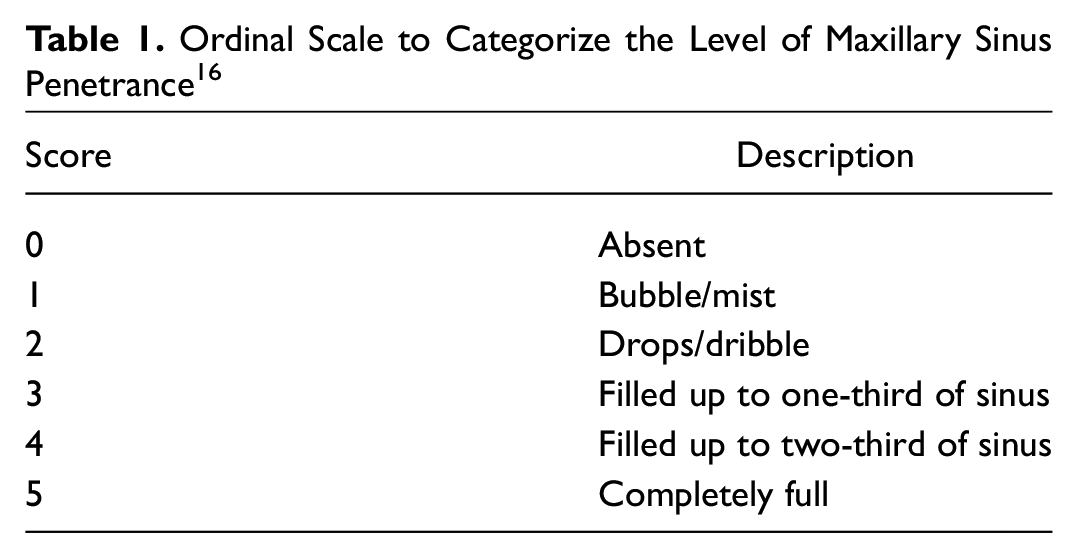
A cadaveric model was developed to assess maxillary sinus irrigation penetration: in physiologic conditions, after BSP alone, and following partial uncinectomy with BSP. A high-volume nasal irrigation system (NeilMed Pharmaceuticals, Inc) was used to irrigate a solution made of 5 mL of blue food coloring mixed with 240 mL of water (120 mL on each side). During each irrigation, the maxillary sinuses were endoscopically evaluated and recorded. Four independent observers graded the degree of penetration after each intervention, according to a previously described score system ( Table 1 ). 16
Ordinal Scale to Categorize the Level of Maxillary Sinus Penetrance 16
Study Protocol: Procedure Technique
A 0° endoscope was used to assess the nasal cavity for septal deviation, septal perforation, and evidence of previous sinus surgery or other anatomic abnormality that could alter the results of irrigation penetrance. Bilateral maxillary sinus trephinations were created by using a No. 11 blade scalpel to make a cruciate incision 2 cm below the infraorbital rim. Soft tissue was elevated from the underlying maxillary bone via a freer, and a handheld drill with a 4-mm burr was used to drill a small opening in the maxillary sinus.
The study protocol included 3 interventions on each maxillary sinus. One study investigator held the head of the cadaver in a 45° downward position to simulate the “head down and forward” position. In each intervention group, the right and left maxillary sinus ostia were irrigated while active observation and recording were performed with a 30° 4-mm rigid endoscope. All cadavers underwent video recording of maxillary sinus irrigation penetrance with no intervention, after BSP (intervention 1), and after subsequent partial uncinectomy (intervention 2). Interventions 1 and 2 were performed by a fellowship-trained rhinologist (A.M.D.). The following methodology describes the procedural component of this cadaveric model.
Intervention 1: With an endoscopic technique, a transilluminated guide wire was advanced through the natural ostium of the maxillary sinus. A 6-mm balloon device (Relieva Scout; Acclarent Inc) was then advanced over the guide wire and inflated to 12 cm H2O for 1 minute.
Intervention 2: With an endoscopic approach, the uncinate was outfractured with a maxillary seeker, and a cutting instrument was used to remove the lower one-fourth of the UP on both sides.
In addition, the natural ostium of the maxillary sinus was measured with a disposable ruler via a transantral approach and a 30° endoscope before any intervention and after BSP. Following irrigation, each cavity was emptied, rinsed with clean water, suctioned to remove residual water, and left to dry before proceeding with the next intervention. Once all images and videos were recorded and labeled (according to cadaver number and procedure type), an ordinal accepted 5-point scale ( Table 1 ) was independently used by each observer to rate the amount of liquid that penetrated the maxillary sinus.
Statistical analysis was performed on SPSS software (version 25.0.0.0; IBM Corp). A paired t test was utilized to compare the ostium sizes before and after BSP. Additionally, an analysis of variance was performed to compare the effect of all procedures in irrigation penetration of maxillary sinuses. Cronbach’s alpha was also calculated to evaluate the interrater reliability.
Results
The mean ostial size of the maxillary sinus was significantly enlarged after BSP (4.1 to 6.8 mm, P = .013). The median score for maxillary sinus irrigation penetrance before any procedure was 2.5. After BSP, the median score was 3, and after partial uncinectomy plus BSP, the median score was 4 ( Figure 1 ). After intervention with partial uncinectomy, there was an observed increase in irrigation in the contralateral maxillary sinus after irrigation.
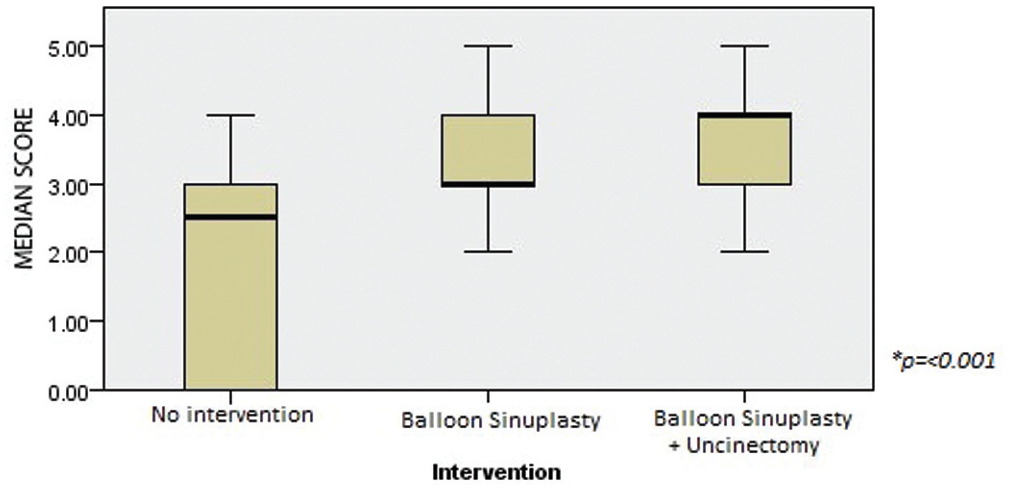
Maxillary sinus irrigation penetrance according to intervention. The ordinal scale maxillary sinus irrigation penetrance values are presented as median (line), interquartile range (box), and 95% CI (error bars).
There was a statistically significant difference in the irrigation penetrance of the maxillary sinus following BSP alone as compared with no intervention (3.2 vs 1.9, P = .0001). There was also a statistically significant increase in irrigation penetrance after partial uncinectomy and BSP versus no intervention (3.7 vs 1.9, P = .0001). There was a higher mean penetration score in the partial uncinectomy and BSP procedure as compared with BSP alone. This difference did meet statistical significance (3.7 vs 3.2, P = .008; Figure 2 ). Interrater reliability based on Cronbach’s alpha was 0.93. An alpha value >0.9 is considered to be excellent internal consistency.
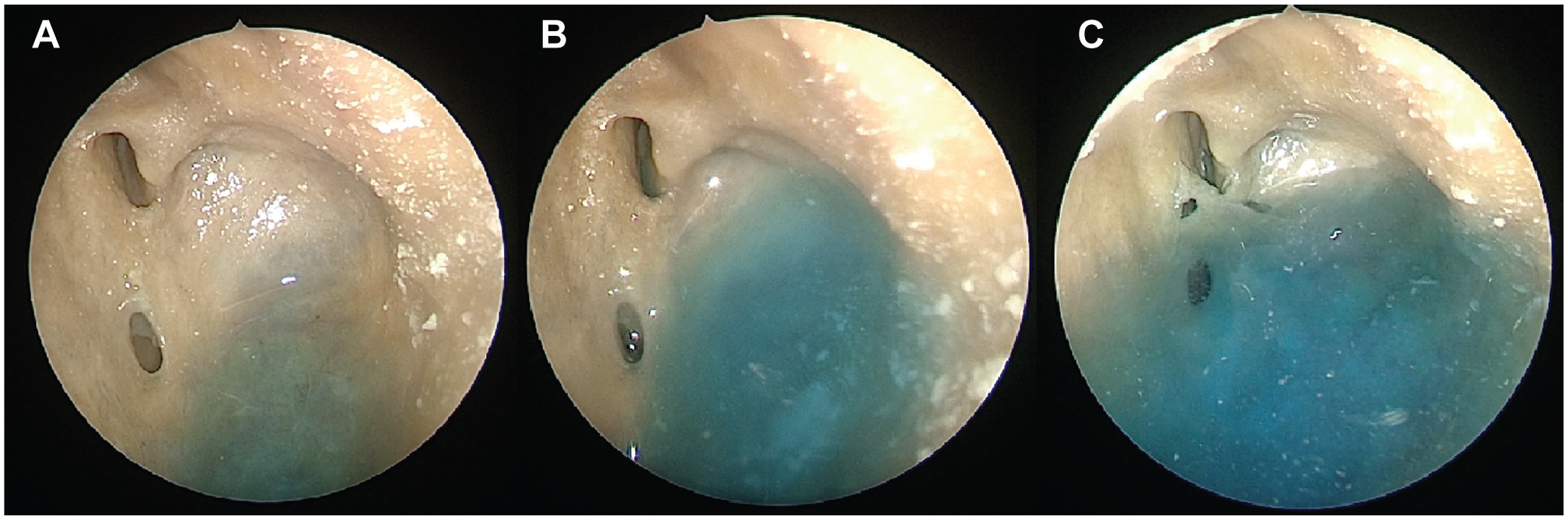
Representative images of the endoscopic view of the maxillary sinus irrigation penetrance (A) prior to any intervention, (B) following balloon sinuplasty dilation, and (C) following the addition of partial uncinectomy.
Discussion
The purpose of this study was to determine the difference in irrigation penetrance when a partial uncinectomy was added to the maxillary sinus BSP. We found a statistically significant increase in irrigation penetrance following BSP and partial uncinectomy versus BSP alone. Additionally, BSP with and without partial uncinectomy had increased irrigation penetrance as compared with no intervention. The results of this cadaveric study also indicated a statistically significant increase in maxillary ostium size.
The sinonasal anatomy modifications secondary to surgical techniques and their impact on sinus irrigation penetrance have been studied.16,19 For example, a recent study compared sinus irrigant penetration after BSP versus ESS in a cadaveric study. Although both procedures improved sinus penetrance, a significantly larger effect on the maxillary sinus was found after ESS relative to BSP. 19 A cadaveric study by Brenner et al noted different effects of balloon dilation depending on the sinus. According to their data, increased irrigation penetrance of the sphenoid sinus and decreased irrigation penetrance of the maxillary sinus occurred after the balloon dilation. Interestingly, their hypothesis for this finding involved the UP location and its possible role as a shield to ipsilateral maxillary sinus penetration. 16 We found an improvement in maxillary sinus irrigation penetrance in the BSP-alone and partial uncinectomy interventions. Our study supports the hypothesis by Brenner et al that location of the uncinate may affect maxillary sinus penetrance. Our results suggest that manipulation of the UP location by outfracturing or partial resection may be integral to maximal maxillary irrigation penetration. During our study, we also observed a trend toward increased retrograde irrigation of the contralateral maxillary sinus after partial uncinectomy. We noted this when preparing the maxillary sinus for the next intervention. Brenner et al suggested that blockage of the ipsilateral sinus by the UP may lead to more retrograde irrigation to the contralateral sinuses. 16
The UP is a thin bony plate that is a part of the lateral wall of the nasal cavity. Embryologically, it arises from the medial surface of the lateral cartilaginous capsule. 20 The UP is located at the most anterior point of the middle meatus, with the ethmoidal, maxillary, and frontal ostia behind it. Although the function of the UP is not well elucidated, it has been proposed that it acts as a conduit for the passage of mucous draining from the frontal, anterior ethmoid, and maxillary sinuses. 21 Removal of the UP is one of the initial steps of ESS, leading to better exposure of the ethmoid air cells and the maxillary ostium. 22
Multiple studies have reported that UP removal leads to a decrease in nasal resistance and a subsequent increase in airflow velocity in the surrounding area.22,23 Although no studies have evaluated the effect of partial uncinectomy after BSP, Singhal et al analyzed the impact of a specific sequence of dissections, including uncinectomy, on the irrigation of cadaveric sinuses. 13 The authors found no changes in the amount of irrigation with the initial removal of the UP. However, they noted significantly higher penetrance after the addition of surgical enlargement of the ostium diameter. 13
We performed a partial uncinectomy in addition to BSP rather than a total uncinectomy and surgical ostium enlargement. Our findings correlate with the increase reported by Singhal et al in the amount of penetrance after both techniques. The use of a partial uncinectomy instead of the total removal has been associated with a shorter operation and healing period in patients with localized maxillary sinus pathology. 24 In the case of BSP, this procedure is typically performed in office, with the goal of obtaining similar outcomes to ESS with shorter procedure times and quicker recovery periods. Previous studies have not found a superiority in symptom outcomes with BSP, and several long-term outcome studies have reported comparable results between traditional ESS and BSP in patients with maxillary sinus disease.25,26 In isolated maxillary sinus disease where postoperative medical therapy is warranted, our results indicate that limited resection of the uncinate provides a quick and effective way to maximize outcomes.
The effect of sinus ostial dilation on irrigation delivery was initially reported by Grobler et al. According to their study, a minimum ostial dimension of 3.95 mm effectively promotes adequate irrigation and drainage among sinuses. 27 In a balloon dilation study, Brenner et al found that an ostial size of 5 mm was associated with significant improvement in sinus penetration. 16 Our results are consistent with the findings of this study, as we noted that the enlargement of the maxillary ostium diameter after balloon dilation had a median size >5 mm and was associated with a higher maxillary sinus penetration score.
Irrigation devices and head position also play a role in sinus penetrance. Low-volume devices such as sprays, drops, and nebulizers have not shown consistent maxillary sinus penetration. In previous studies, nasal irrigations performed with high-volume devices (neti pots, squeeze bottles irrigators of at least 100 mL) were more effective in achieving maxillary sinus penetrance before and after ESS.18,28-31 Given this data and the methodology of other cadaveric balloon dilation studies, we chose to use a high-volume nasal irrigation system (NeilMed Pharmaceuticals, Inc). Head positioning is also known to affect sinus penetrance. In an evidence-based review, Thomas et al evaluated the distribution of topical medical therapies to the sinuses and the nasal cavity. When head position was analyzed, the “head down and forward” position was found to be optimal for sinus penetrance regardless of the irrigation delivery device. 14 Thanaviratananich et al also studied the effect of head positions based on the sinonasal target. According to their results, the “lying head back” position is recommended for frontal and ethmoid sinuses penetrance, while the “head down and forward” position is recommended for maxillary sinuses. 32 During our study, all our cadaver heads maintained a 45°“head down and forward” position to prevent any significant effect of head positioning on sinus penetration.
There are some limitations to our study. We had a relatively small sample size, which limits some of the statistical analysis. However, the interrater reliability was strong, and the sample size was similar to previous published cadaveric studies, which allowed us to compare the results of our study reliably.13,16-19,33 We did not perform the study with different types of delivery devices. Therefore, we are unable to determine if low-volume applications, such as sprays and mists, would have a similar benefit with the addition of the partial uncinectomy. Some authors have used computational fluid dynamics simulations or 3-dimensional printing sinonasal models to evaluate delivery systems.23,34 Further studies involving these technologies are needed to understand the role of partial uncinectomy in the irrigation penetration of the maxillary sinus. Regarding our finding of increased retrograde irrigation of the contralateral maxillary sinus after partial uncinectomy, additional studies based on quantitative measures of this phenomenon would add to our understanding of the benefit of partial uncinectomy with BSP. To our knowledge, no studies have examined symptom outcomes from the use of partial uncinectomy with BSP in the clinic setting. Future studies focusing on this will add value to the current literature that we have on this surgical technique.
Conclusion
Several factors affect irrigation penetrance into the maxillary sinuses, including the ostial size, irrigation device, head position, and nasal anatomy. This cadaveric study found that maxillary sinus irrigation penetration increased from baseline after BSP. The addition of a partial uncinectomy to the balloon dilation of the maxillary sinus was associated with a statistically significant increase in irrigation penetrance scores as compared with BSP alone.
Author Contributions
Disclosures
Footnotes
This article was presented at the 2020 AAO-HNSF Virtual Annual Meeting; October 13, 2020.
