Abstract
Objective
Avoiding tracheal intubation by using general anesthesia with spontaneous breathing (GASB) is attractive for upper airway panendoscopy. The aim of this study was to estimate the incidence of adverse events during panendoscopy under GASB and to assess the practices of French anesthesiologists.
Study Design
Two-phase study: monocentric retrospective study and national survey.
Setting
University hospital center.
Methods
Patients who underwent a panendoscopy under GASB at the University Hospital of Angers between January 1 and December 31, 2014, were reviewed. Failure of GASB was defined as an episode of hypoxemia (SpO2 ≤88%) or the need for face mask ventilation with or without tracheal intubation. Then, we sent an electronic survey to all members of the French Society of Anaesthesia and Intensive Care.
Results
Among the 95 included patients, 22 (23%) experienced a failure of GASB: 3 tolerated hypoxemia, 15 had face mask ventilation episodes, and 4 were intubated. Three factors were associated with failure: obesity (odds ratio, 11.94; 95% CI, 3.20-44.64), history of difficult intubation defined as a Cormack score ≥3 (odds ratio, 6.20; 95% CI, 1.51-25.41), and laryngeal tumor (odds ratio, 2.81; 95% CI, 1.04-7.56). Among the 3930 members of the French Society of Anaesthesia and Intensive Care in 2018, 662 (16.8%) responded to the survey. The 2 preferred techniques to perform panendoscopy were intubation (62%) and intravenous sedation with spontaneous breathing (37%).
Conclusion
Although general anesthesia with orotracheal intubation remains the preferred technique for panendoscopy in France, GASB is an attractive alternative with a low failure rate. Risk factors for failure are obesity, history of difficult intubation, and laryngeal tumor.
Keywords
Panendoscopy is a common procedure, usually performed under general anesthesia (GA). Its main challenge is the need for anesthesiologists and otorhinolaryngologists (ORLs) to share the airways, to allow for oxygenation of the patient and a complete examination of the airways at the same time. Several anesthetic procedures are available to achieve these goals: apneic GA with intermittent face mask ventilation, GA with orotracheal intubation (OTI), GA with jet ventilation, and GA under spontaneous breathing (SB) without intubation. Each of these techniques has its own advantages, disadvantages, and possible complications.1-3
Thanks to the use of rapid-elimination anesthetic agents (eg, propofol and remifentanil) administered with brain or plasma target-controlled infusion,4,5 SB during GA is becoming easier to perform and appears to be an attractive technique for panendoscopy, as it optimizes the surgeon’s visibility by avoiding the presence of the endotracheal tube in the airways. However, the incidence of adverse events associated with this procedure is unknown, notably the rates of emergency or unplanned OTI and hypoxemia. Furthermore, SB does not protect the patient’s airway, making the procedures at risk for pulmonary aspiration. 6
Currently, there are no recommendations on the type of anesthetic procedure to apply for panendoscopy, and it is not known which procedures are the most commonly used by physicians. At the University Hospital of Angers, panendoscopies are usually performed under GA with the maintenance of SB. This study aimed to estimate the incidence of adverse events during panendoscopies in our center. In addition, we conducted a national survey to estimate the practices of anesthesiologists performing panendoscopies in France.
Material and Methods
We conducted a monocentric retrospective study assessing the incidence and predictive criteria for failure of panendoscopy under SB, and we distributed a survey regarding the anesthetic practices of panendoscopy in France.
Retrospective Cohort
The study was approved by the Ethics Committee of the French Society of Anaesthesia and Intensive Care (SFAR), which waived patient consent for this study according to French law (Institutional Review Board 00010254-2020-088). 7
Inclusion and Exclusion Criteria
Without any exception, all patients were included who underwent a panendoscopy under SB, for either diagnostic or therapeutic purposes (microsurgery or laser resection), at the University Hospital of Angers between January 1 and December 31, 2014. Patients for whom OTI or jet ventilation was planned were not included.
Anesthetic Procedure
The anesthetic procedure was already under protocol in our unit in agreement with surgeons, and all patients have a trial in GA with SB for panendoscopies. Induction and maintenance of GA were performed with propofol and remifentanil via target-controlled infusion, after preoxygenation achieved an end-tidal oxygen concentration >90%, 8 associated with a reverse Trendelenburg position for obese patients.9,10 The brain target of remifentanil concentration was 2 ng/mL (according to Minto’s model) at induction. Propofol was then started with a brain concentration at 2 µg/mL (according to Schnider’s model) and, if necessary, a gradual increase of 0.5 µg/mL (usual final brain concentration, 3-5 µg/mL) to achieve narcosis compatible with the surgical procedure. A nasal oxygen catheter was then inserted (oxygen flow between 6 and 10 L/min was temporarily stopped in case of laser).
Procedural Failure Definition
Failure of the procedure was defined by the presence of at least 1 of the following criteria: hypoxemia (SpO2≤88%), 11 apnea episodes requiring face mask ventilation, or mechanical ventilation with OTI.
Data Collection
The following data were recorded via the electronic record: demographics, percutaneous oxygen saturation in ambient air, medical history, American Society of Anesthesiologists status, use of premedication, presence of difficult ventilation or intubation criteria, surgical parameters (indication, tumour size, location), per-procedure data (vital parameters, complications, time of the procedure, amount of anesthetics used), and postanesthesia care unit data.12-15
National Survey
Using Google Forms, we created a survey aimed to evaluate French practices on the anesthetic techniques used to perform panendoscopy. It included 11 single- or multiple-choice questions (Supplemental Table S2, available online). The estimated time to answer the questionnaire was 2 minutes. After agreements with the presidents of the French anesthesia group in ORL surgery (CARORL) and the SFAR, the survey was emailed to all members of the SFAR (doctors and residents). It was open from May to August 2018. We previously defined 2 groups of anesthesiologists according to their ORL activity rate: the ORL group by an activity rate of at least 50% in ORL and the control group by a rate <50%.
Statistical Analysis
Data are expressed as median and interquartile range for numeric variables with an asymmetric distribution and as mean and standard deviation for those with a normal distribution. Proportions are represented by the number and percentage of subjects. For comparisons of quantitative variables, we used t tests for those with a normal distribution and Wilcoxon tests for the others. The distributions were evaluated by the Shapiro-Wilk test (H0 normal distribution rejected if P < .05). For categorical variables, we used the chi-square or Fisher exact test (theoretical sample size <5). The odds ratios (ORs) of the presupposed risk factors for procedure failure were obtained by using chi-square tests with confidence intervals.
The significance threshold of the tests is set at a P value of .05. As the analyses were carried out for exploratory purposes, we did not correct for the alpha risk given the multiplicity of tests. The analyses are performed with SPSS Statistics (version 25; IBM) and JMP statistical software (version 11; SAS Institute).
Results
Retrospective Cohort
Between January 1 and December 31, 2014, 139 patients underwent a panendoscopy in the University Hospital of Angers, and 95 were included. Figure 1 shows the flowchart of patients’ inclusion. Note that 6 patients were not included because they needed jet ventilation for surgical reasons (eg, vocal cords (CV) immobility). Among them, 22 (23%) had a failure of the procedure: 3 tolerated hypoxemia, 15 required face mask ventilation, and 4 underwent OTI.
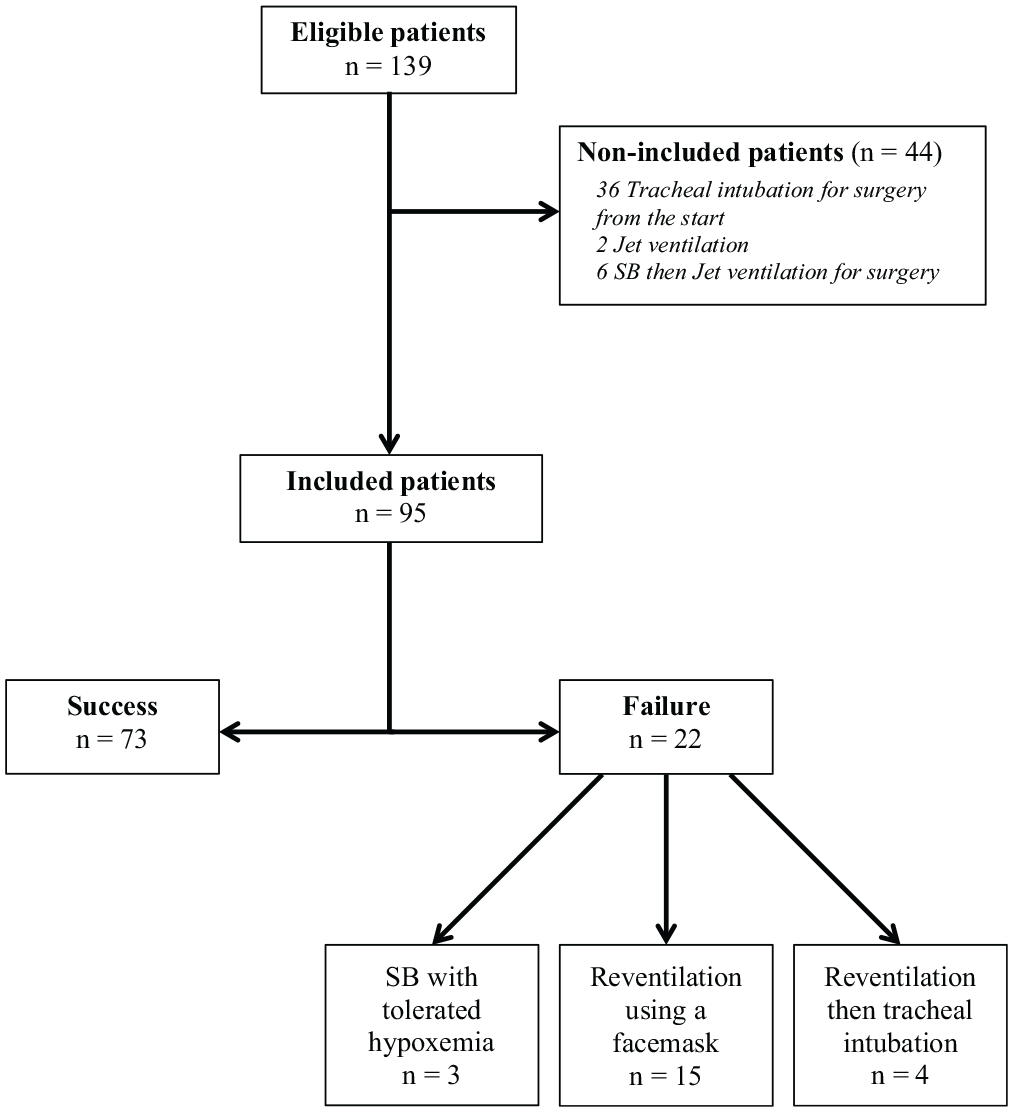
Flowchart of patients. SB, spontaneous breathing.
Characteristics of the patients and comparisons between the groups are presented in Table 1 . Patients were predominantly men >50 years old (86% of patients). The prevalence of failure was higher for obese patients (ie, with a body mass index >30 kg/m2; OR, 11.94 [95% CI, 3.20-44.64]) and those with a Cormack score ≥3 (OR, 6.20 [95% CI, 1.51-25.41]). The per-procedure data (Supplemental Table S1, available online) revealed that the laryngeal location of the tumor lesion was significantly more common in the failure group (OR, 2.81 [95% CI, 1.04-7.56]). In addition, doses of propofol and remifentanil, procedure duration, and length of stay in the postanesthesia care unit were significantly higher in failure group, in comparison with the control group. There were no hemodynamic complications per procedure with the drugs used. Furthermore, the mobility of the vocal cords, depending on possible tumor attachment, was not associated with a significant risk of SB procedure failure. Concerning surgical satisfaction in our cohort, about 92% of the procedures fully satisfied the surgeons (Supplementary Material).
Characteristics and Preoperative Data Stratified by Success or Failure of Panendoscopy With Spontaneous Breathing. a
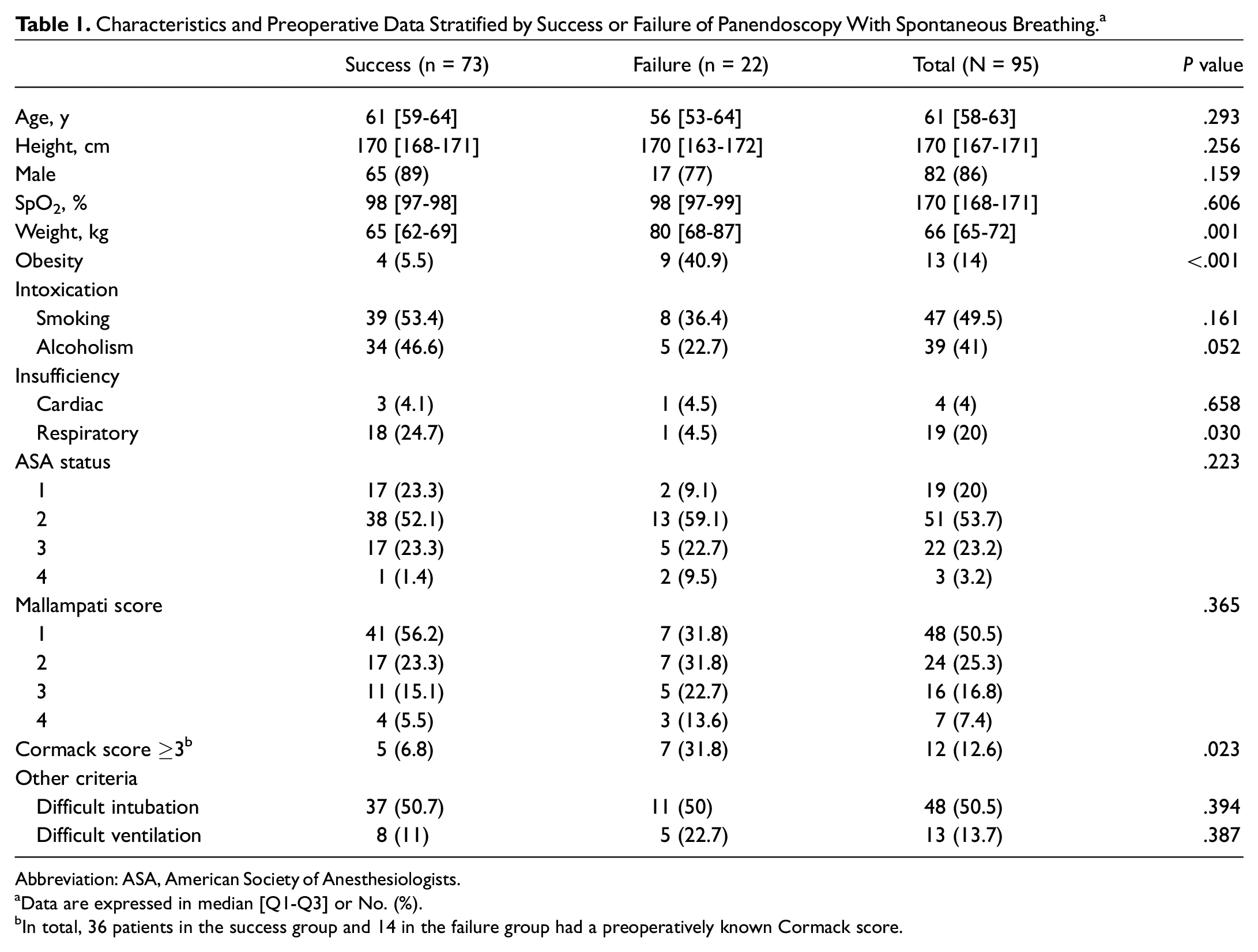
Abbreviation: ASA, American Society of Anesthesiologists.
Data are expressed in median [Q1-Q3] or No. (%).
In total, 36 patients in the success group and 14 in the failure group had a preoperatively known Cormack score.
Survey Results
Of the 3930 SFAR members in 2018, 662 (16.8%) responded to the survey. The respondents were located in 201 cities, including 15 foreign cities. The majority of the respondents were senior anesthesiologists (ie, at least 2 years of experience) working in a public structure. Of the 662 respondents, 97 (14.7%) mainly practiced in ORL surgery (ie, ≥50%). The characteristics of the ORL and non-ORL anesthesiologists are detailed in Table 2 . The 2 preferred techniques to perform panendoscopy were GA with OTI (62%) and intravenous sedation with SB (37%). SB was considered to be always feasible by 43% of the ORL anesthesiologists, as opposed to 27% in the non-ORL group (P = .002). The disadvantages and advantages of SB panendoscopy, according to the ORL and non-ORL anesthesiologists, are shown in Figure 2 . The risk of spasm with SB was considered present in a significantly higher proportion in the non-ORL group (42% vs 38%, P = .038). There were no other major differences between the groups.
Characteristics of the Respondents in ORL and Non-ORL Groups. a
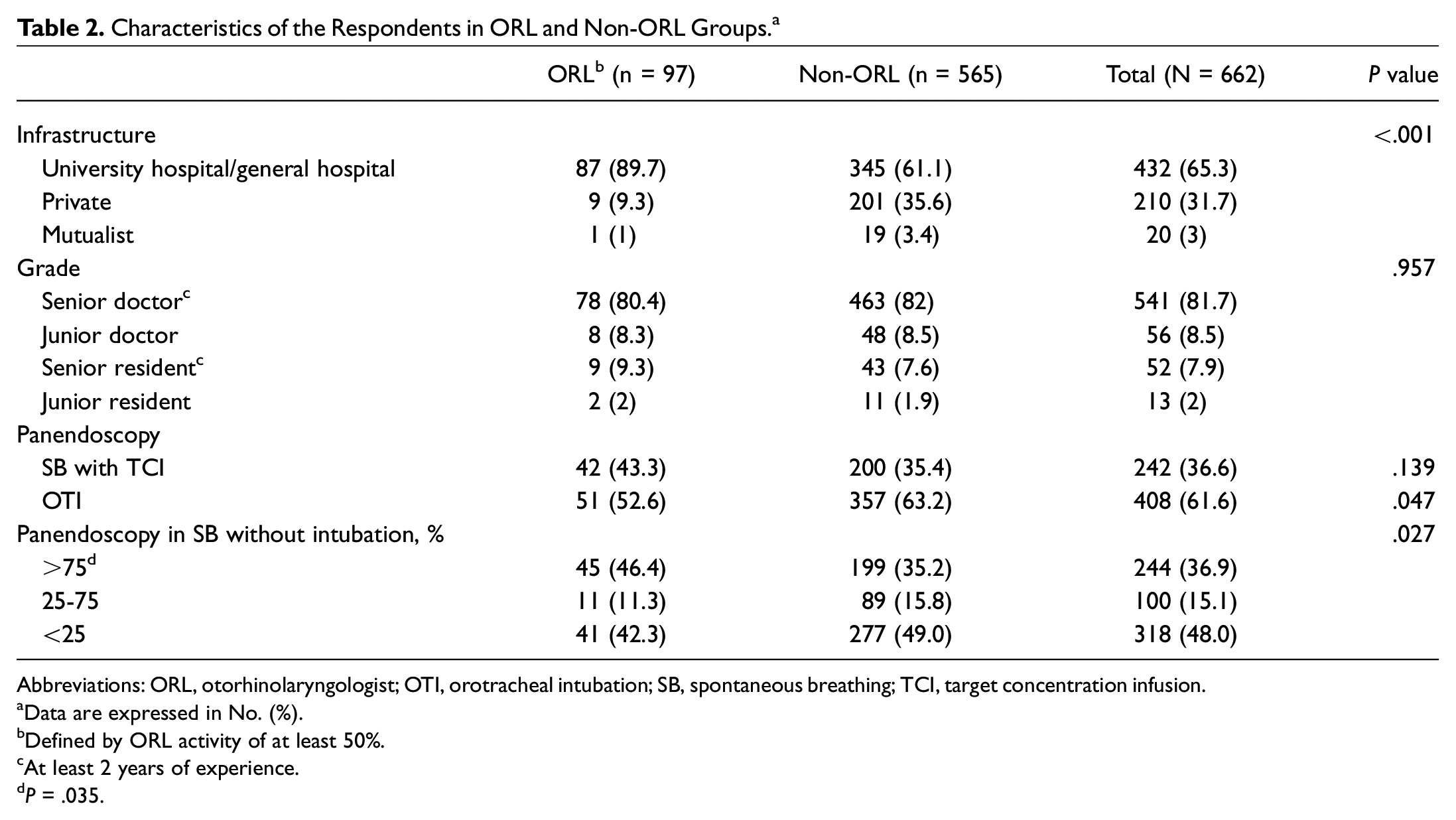
Abbreviations: ORL, otorhinolaryngologist; OTI, orotracheal intubation; SB, spontaneous breathing; TCI, target concentration infusion.
Data are expressed in No. (%).
Defined by ORL activity of at least 50%.
At least 2 years of experience.
P = .035.
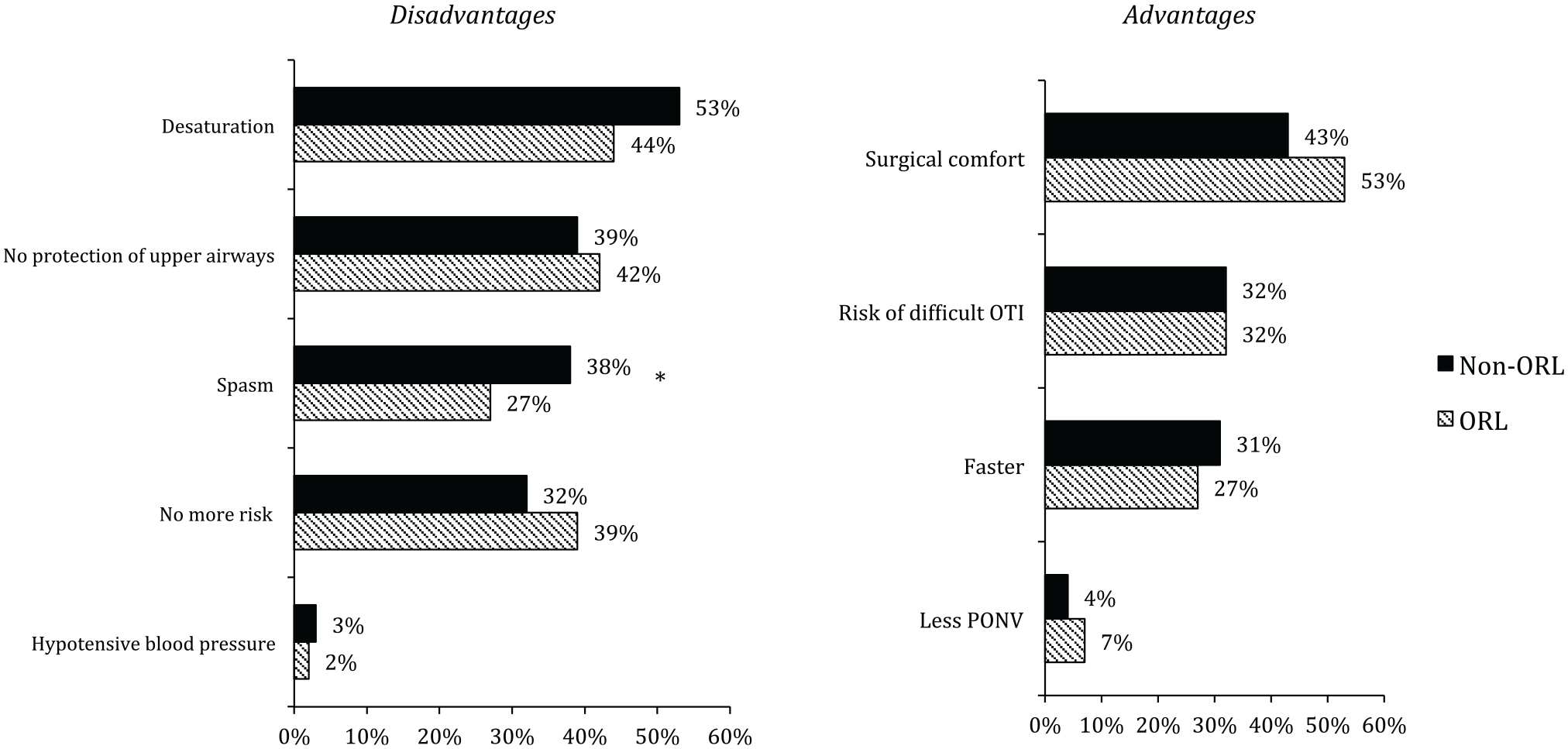
Disadvantages and advantages of the spontaneous breathing panendoscopy procedure according to ORL or non-ORL anesthesiologist groups. ORL group defined by an ORL activity of at least 50%. ORL, otorhinolaryngologist; OTI, orotracheal intubation; PONV, postoperative nausea and vomiting. *P = .038.
Respondents’ justifications for not performing SB maintenance under GA are reported in Figure 3 . The ORL group less frequently reported a lack of skill in the technique (3% vs 10%, P = .015). The primary justification for not using the SB technique was its higher risk for practitioners in both groups.
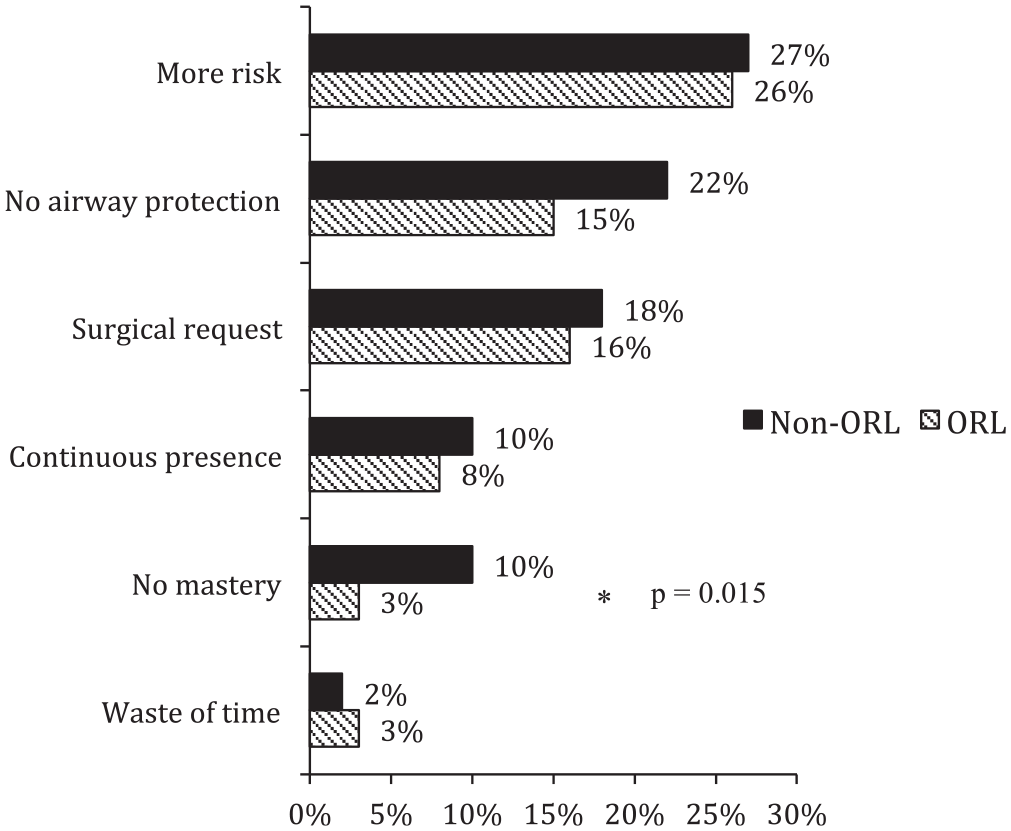
Justification for not using the spontaneous breathing procedure according to whether respondents were in the ORL or non-ORL group. ORL group defined by an ORL activity of at least 50%. ORL, otorhinolaryngologist. *P = .015.
The risk factors for SB failure authenticated by respondents are reported in Supplemental Figure S1 (available online). The presupposed risk factors for SB failure were comparable between the groups, apart from the presence of >2 criteria for difficult ventilation, which appears to be a significant presupposed risk factor for failure in the non-ORL group (P = .034).
Discussion
Anesthesia with SB for panendoscopy was associated with a 23% failure rate, for which obesity, a history of difficult intubation, and laryngeal location of the tumor lesion were significant risk factors. GA with OTI seems to be the favorite method for panendoscopy by the majority of French anesthesiologists.
Spontaneous ventilation has potential advantages, including an open view of the larynx and the vocal cords’ mobility for the surgeon. We note that >90% of the procedures were completely satisfactory for the surgeons in our center. However, some studies reported that the conditions of panendoscopy for the surgeon remain unchanged with or without OTI. 16 According to our survey, SB is only an alternative method for panendoscopy, probably due to a lack of knowledge of the technique and the fear of associated adverse events. Indeed, we observe a substantial rate of failure in our cohort. This rate is mainly due to the need for transient face mask ventilation, which is a common event during procedures with low-dose sedation; yet, just 4% of panendoscopies required OTI. Interestingly, no inhalations, spasms, or severe adverse events (eg, myocardial infection) were recorded, contrary to the belief of the majority of our survey respondents.
Risk factors of failure were found in our cohort and are easily identifiable by the anesthesiologists taking care of these patients. During GA, the finding of hypoxemia in the obese patient is explained by several factors, such as the increase in oxygen consumption secondary to an increase in metabolic demand and cardiac output, 17 an increase in altered lung compliance by up to 35%, 18 or the decrease in residual functional capacity related to diaphragmatic ascent.19,20 In obese patients, there is an exponential relationship between body mass index and decrease in residual functional capacity. 21 In addition, a history of difficult intubation, defined by a Cormack score ≥3, was associated with a nearly 50% risk of SB procedure failure. Interestingly, obesity is not considered a risk factor for nearly one-quarter of the respondents. Similarly, a history of difficult intubation is not a risk factor for 80% of respondents. We therefore feel that it is necessary to communicate the identification of these risks to anesthetists and ORLs wishing to use this technique. We should be able to propose alternatives to the maintenance of SB for obese subjects and those with a difficult history of intubation or laryngeal tumor localization. Perhaps the use of first-line OTI for these patients is preferable, and the maintenance of SB is a guarantee of safety in case of intubation difficulties. One way to reduce the failure rate could be a change in the patient’s oxygenation technique. Instead of a nasal catheter, a possibility could be found in the use of high-flow oxygenation. This technique has especially shown its interest in intensive care. 22 Its use in SB panendoscopy procedures could avoid or delay the onset of hypoxemia that could lead to emergency OTI while preserving the visibility of the operative field. 23
Our study has several limitations related to its retrospective and monocentric nature, the lack of data about patients’ hospital outcomes, and the relatively small number of included patients. Concerning the survey, it is possible that the wording/understanding of the questionnaire was not perfect: we should have included the term “SB without intubation” to avoid confusion.
Conclusion
Anesthesia with SB is an attractive alternative to GA with OTI, with a relatively low failure rate and no severe complication. The identification of the population most at risk of failure—obese subjects, those with a problematic intubation history, and laryngeal location of the tumor lesion—could allow for better selection of patients who would benefit the most from this method.
Author Contributions
Author Contributions
Supplemental Material
sj-docx-1-opn-10.1177_2473974X211065015 – Supplemental material for Spontaneous Breathing for Panendoscopy? Retrospective Cohort and Results of a French Practice Survey
Supplemental material, sj-docx-1-opn-10.1177_2473974X211065015 for Spontaneous Breathing for Panendoscopy? Retrospective Cohort and Results of a French Practice Survey by Pierre Habrial, Maxime Léger, Fabienne Costerousse, Julie Debiasi, Renaud Breheret, Charles-Hervé Vacheron, Emmanuel Rineau and Sigismond Lasocki in OTO Open: The Official Open Access Journal of the American Academy of Otolaryngology-Head and Neck Surgery Foundation
Footnotes
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
