Abstract
Objective
Both tonsillar hypertrophy and obesity contribute to pediatric sleep-disordered breathing (SDB). Tonsillectomy addresses anatomical obstruction causing SDB; however, it may adversely affect the obesity profile postoperatively. Herein, we investigate posttonsillectomy body mass index (BMI) changes in pediatric patients.
Study Design
Retrospective case series.
Setting
Tertiary, pediatric urban academic center.
Methods
All patients undergoing tonsillectomy from January 1, 2016, to December 31, 2016, were included. Patients’ age, sex, surgical indication, and preoperative BMI were recorded. Postoperative BMI data were collected between March 1, 2016, and December 31, 2017. Statistical analysis was performed using a generalized regression model, using BMI percentile-for-age weight status.
Results
A total of 1153 patients were included (50% female), with age ranging from 2.0 to 19.5 years (mean [SD], 7.6 [4.0]). The majority (87.8%) had tonsillectomy for SDB. Of the cohort, 560 (48.6%) had available follow-up BMI data. The BMI percentile on the day of the surgery had a median of 65.8, and the BMI percentile on follow-up had a median of 76.4. The median time to follow-up was 197 days with a range of 50 to 605 days. Higher postoperative BMI percentile strongly correlated to higher preoperative BMI percentile (
Conclusion
We observed a significant increase in BMI percentile following tonsillectomy, which accounted for a significantly higher proportion of the cohort being classified as overweight or obese postoperatively. These findings necessitate greater preoperative counseling, closer follow-up, and adjunctive measures for obesity management in pediatric patients undergoing tonsillectomy.
Although the overall number of tonsillectomy procedures has declined over the past 2 decades with a paradigm shift in surgical indications from recurrent tonsillitis (RT) to sleep-disordered breathing (SDB), it is still one of the most frequently performed pediatric surgeries worldwide.1,2 With an estimated prevalence of 1% to 5% in pediatric patients, SDB represents a growing health concern in tandem with the childhood obesity epidemic in the United States. 3 It is known that tonsillar hypertrophy and obesity are major determinants of SDB in children and that these 2 factors share a close association as increased adiposity in the upper airway leads to increased opportunity for collapse. 4 Because of an ever-expanding body of literature implicating untreated SDB in a host of downstream morbidities ranging from behavioral problems and cognitive impairment to cardiometabolic disease in adults, tonsillectomy is still frequently performed as the first-line surgical treatment for SDB in the pediatric population.5-8
Previous studies examining the relationship between tonsillectomy and subsequent weight gain have produced mixed results, many with relatively small cohorts of patients. Some studies have shown no significant changes in body mass index (BMI) associated with surgical intervention, 9 while others reported meaningful weight gain after tonsillectomy,10,11 including a systemic review by Jeyakumar et al. 12 Several potential mechanisms for the observed acceleration in growth have been proposed, including increased secretion of growth hormone and catecholamines after resolution of SDB, decreased work of breathing leading to decreased net caloric expenditure, and altered appetite and caloric intake.13-15 Nonetheless, the effect of tonsillectomy and the underlying mechanisms behind clinically reported weight changes are poorly characterized. The purpose of the current study is to retrospectively observe a large cohort of pediatric patients following tonsillectomy, document changes in BMI, and investigate demographic and clinical factors associated with significant postoperative weight gain and propensity for the development of obesity.
Materials and Methods
Inclusion Criteria
After obtaining institutional review board (IRB) approval from the University of California, San Diego and Rady Children’s Hospital San Diego, we retrospectively identified children who underwent tonsillectomy with or without adenoidectomy at our tertiary academic pediatric hospital between January 1, 2016, and December 31, 2016. The follow-up period was defined as March 1, 2016, to December 31, 2017. Surgical indications included recurrent tonsillitis or the clinical diagnosis of SDB as characterized by obstructive abnormalities of the respiratory pattern or the adequacy of oxygenation/ventilation during sleep, which include snoring, mouth breathing, and pauses in breathing as reported by caregivers. 2 Those patients who had the diagnosis of obstructive sleep apnea (OSA) based on preoperative polysomnography (PSG) were also included in the broader definition of the SDB group. Tonsillectomies were performed with either monopolar cautery or wire snares with bipolar cautery used for hemostasis. We included patients between the age of 2 and 20 years in this study to analyze BMI change using the Centers for Disease Control and Prevention (CDC) BMI-for-age growth charts, which are used to assess growth in the United States among children and teenagers aged 2 to 20 years. 16 We excluded syndromic patients as well as those without complete weight or height data. Data collected from the electronic medical records included demographic information, surgical indications, and anthropometric measurements. We recorded patients’ BMI at the time of the surgery and any available anthropometric measurements within the electronic medical record system recorded during the follow-up period to obtain postoperative BMI data. The BMI was also recorded as percentiles according to the CDC growth chart.
BMI and Weight Classifications
Anthropometric measurements including height, weight, and BMI were collected at the time of the surgery. In our practice, we did not schedule routine follow-up appointment following tonsillectomy surgery. Families were instructed to observe the child after the 2-week recovery period for snoring or sleep-disordered breathing symptoms. If these symptoms did not resolve completely, they were instructed to contact the ear, nose, and throat (ENT) office for follow-up. All patients with preoperative PSG who demonstrated severe OSA were scheduled to undergo repeat PSG. The subsequent height and weight measurements were taken from available data recorded in the electronic medical record system whenever patients had any clinical encounter with any provider in the medical system during the postoperative period ending in December 31, 2017. If patients had more than 1 weight and height recording, the one closest to the surgery date beyond the 30-day postoperative period was used. BMI, a commonly accepted index for classifying adiposity in children and adolescents, is calculated as body weight in kilograms divided by height in meters squared. 17 Since BMI is both sex specific and age specific, obesity is calculated based on the CDC recommended cutoffs. Weight status is defined by the following: underweight (<5th percentile), healthy weight (5th to <85th percentile), overweight (85th to <95th percentile), obese (95th to <99th percentile), and morbidly obese (≥99th percentile).
Statistical Analysis
Baseline demographic and clinical characteristics were compared using Pearson’s χ2 and bivariate fit analysis for categorical and continuous variables, respectively. Baseline characteristics between patients with and without follow-up data were compared to demonstrate minimal selection bias. The primary outcome of interest was postoperative BMI percentile at follow-up. We studied the effect of SDB, age, sex, and the procedure on the postoperative BMI percentile distribution. A model is fit to explain (or predict) the BMI at follow-up (FU). The BMI on day of the surgery (DOS) enters the model as a covariate, together with SDB, age, and sex. The distribution of BMI is expressed by its percentiles. Therefore, it ranges from zero to 1. A generalized linear model is fit, and the model demands the specification of a distribution for the response and a link function. The β-distribution was chosen, together with the link logit, which are the standard choices for this type of response. JMP Version 14 (SAS Institute) was used to analyze the data, with 2-sided
Results
During the study period, 1153 patients who underwent tonsillectomy with or without adenoidectomy were included in the analysis ( Figure 1 ). The age range was from 2.0 to 19.5 years, with mean age of 7.6 ± 4.0 years and an equal distribution of males (577) and females (576). In this cohort, 995 patients had tonsillectomy with adenoidectomy, and 158 had tonsillectomy only without adenoidectomy. The majority of the patients (1012) underwent surgery due to SDB (87.8%), and 141 patients (12.2%) had the procedure done for the diagnosis of RT.
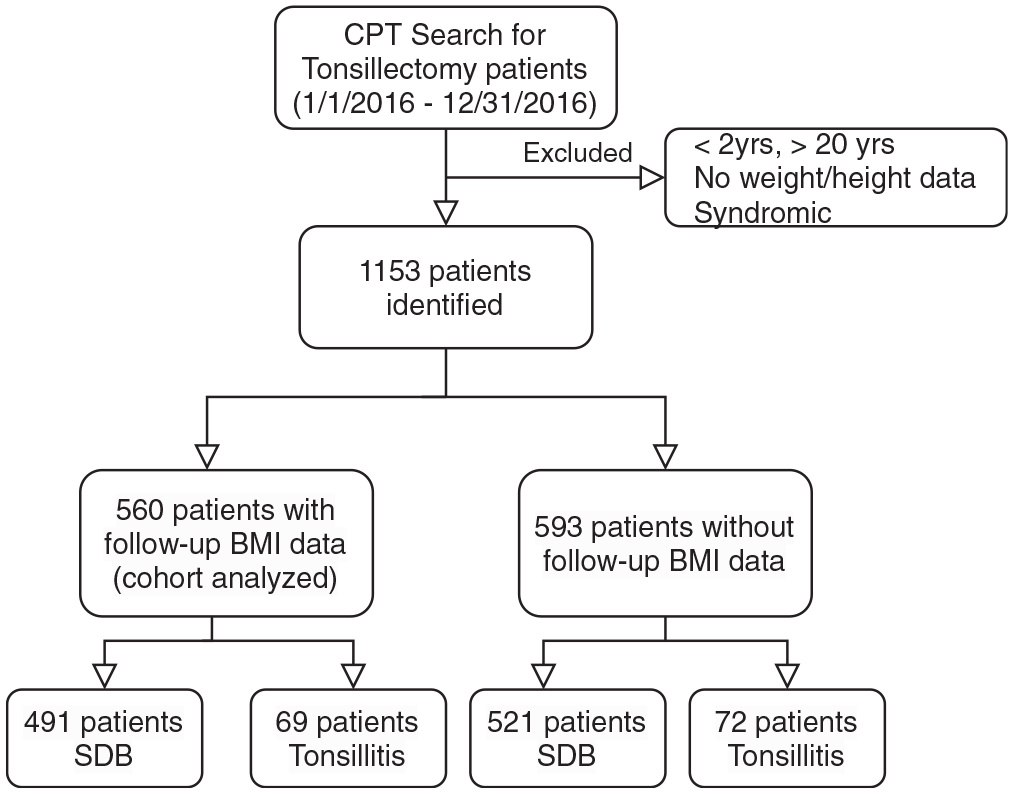
Inclusion criteria and patient selection algorithm. BMI: body mass index;
The RT population was significantly older compared to the children who underwent surgery for SDB and had more female patients ( Table 1 ). Also, the BMI profile of the 2 groups was significantly different, with the RT group representative of the general population, with most of the children in the normal weight range (67.4%) and a small percentage of the group being either obese (7.8%) or morbidly obese (2.8%). The SDB group BMI profile was shifted toward more obese (14.7%) or morbidly obese (7.6%) children.
Demographic Data and Physical Characteristics of the Cohort on the Day of Surgery.
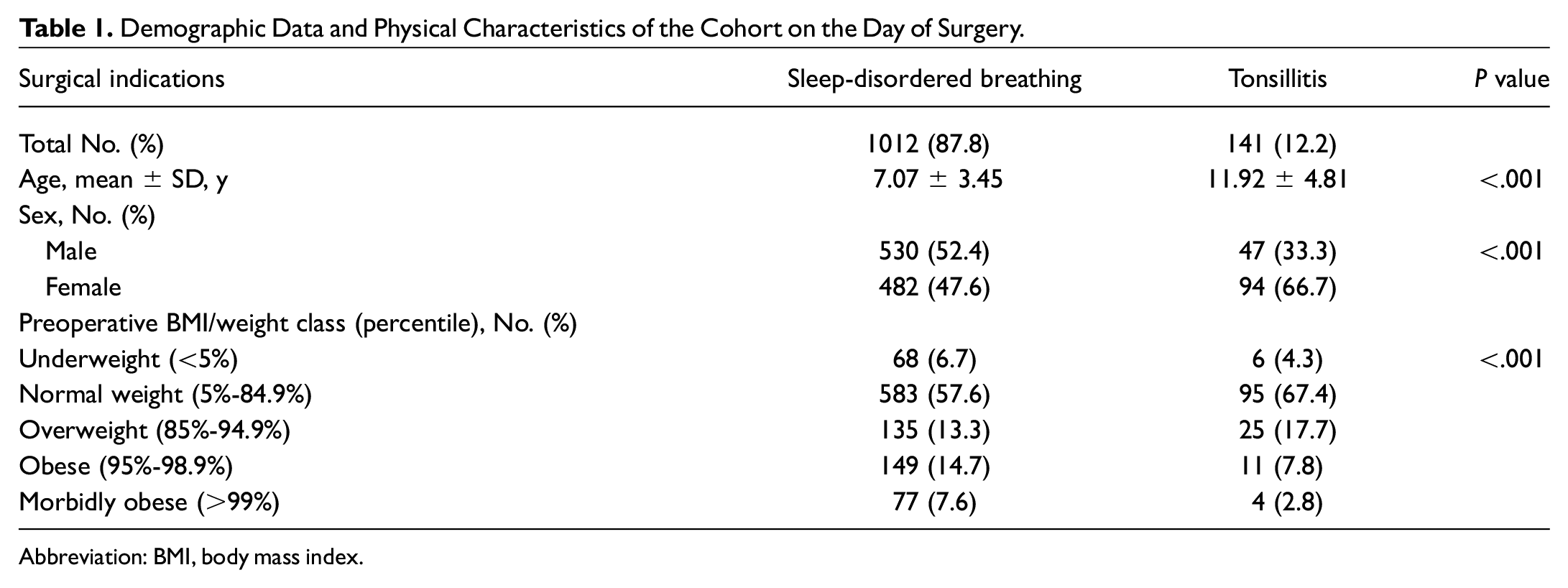
Abbreviation: BMI, body mass index.
Of 1153 total patients, 560 patients (48.6%) had follow-up anthropometric measurements, and 593 patients (51.4%) did not. Of the patients with follow-up data, 497 had tonsillectomy with adenoidectomy, and 63 had tonsillectomy only without adenoidectomy. Of these, 35 patients had tonsillectomy only for recurrent tonsillitis. We compared baseline characteristics of those with and without BMI follow-up data postoperatively. There was no significant difference between the 2 groups with regards to sex (
For the cohort of 560 patients who had follow-up BMI data, the BMI percentile on the day of the surgery had a median of 65.8, while the BMI percentile at follow-up had a median of 76.4 with a range of 0 to 100 for both. The median time from the surgery to the subsequent BMI recording was 197 days with a range of 50 to 605 days. The weight class comparison between day of surgery and follow-up is demonstrated in Table 2 . Patients with SDB had the general trend of increased subsequent weight class distribution when compared to tonsillitis patients postoperatively.
Comparison of Weight Class on the Day of Surgery (DOS) and at Follow-up in Patients With Sleep-Disordered Breathing (SDB) and Tonsillitis. a
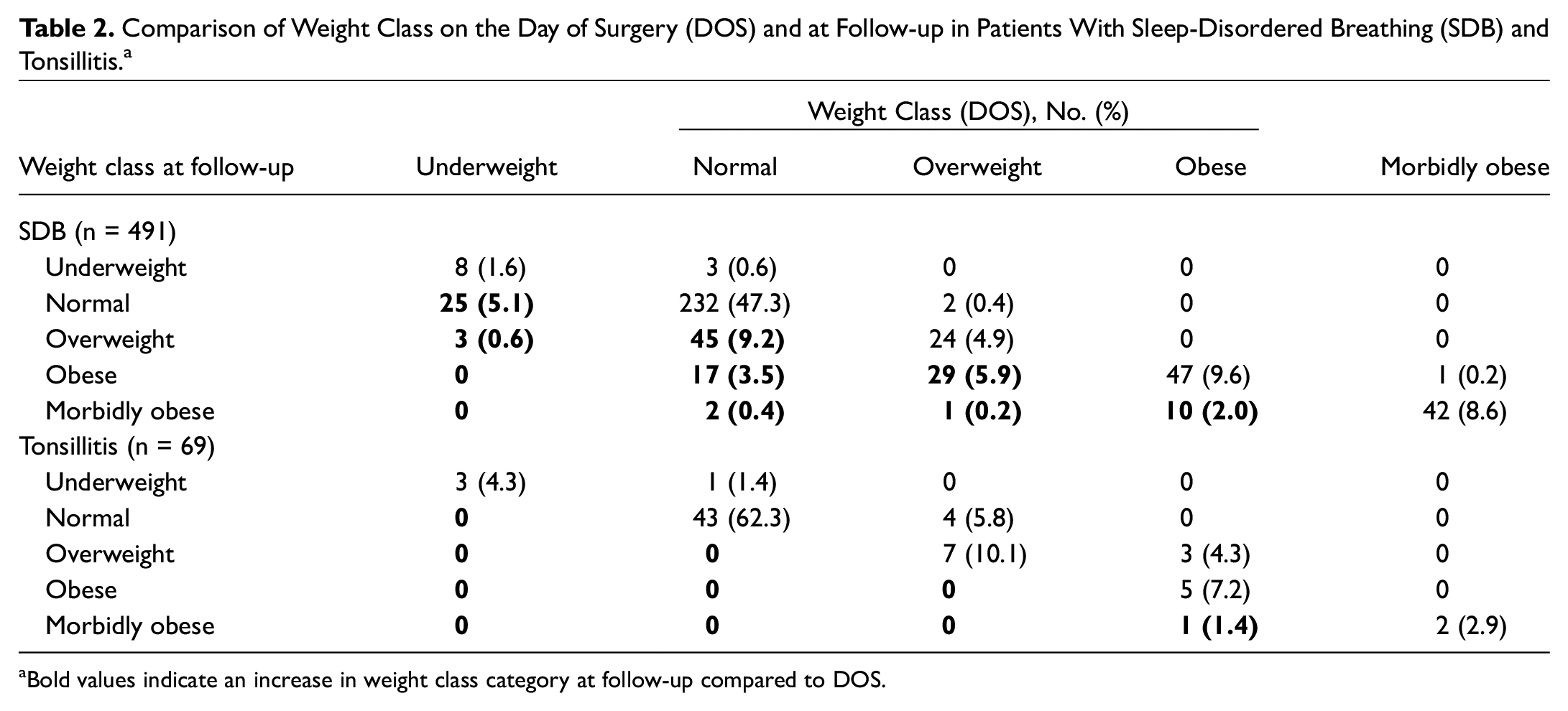
Bold values indicate an increase in weight class category at follow-up compared to DOS.
We performed a generalized regression model for follow-up BMI, adjusting it to initial BMI on the date of surgery, age, sex, and surgical indications (SDB vs RT). The generalized
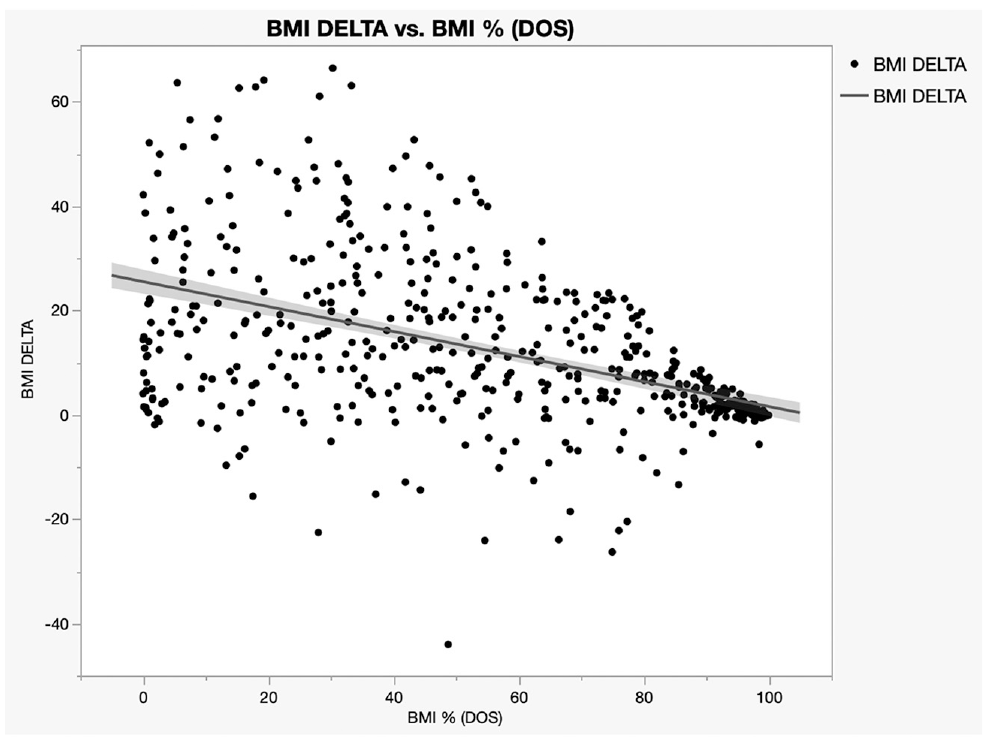
Body mass index (BMI) percentile on the day of the surgery (DOS) strongly predicts postoperative BMI percentile (
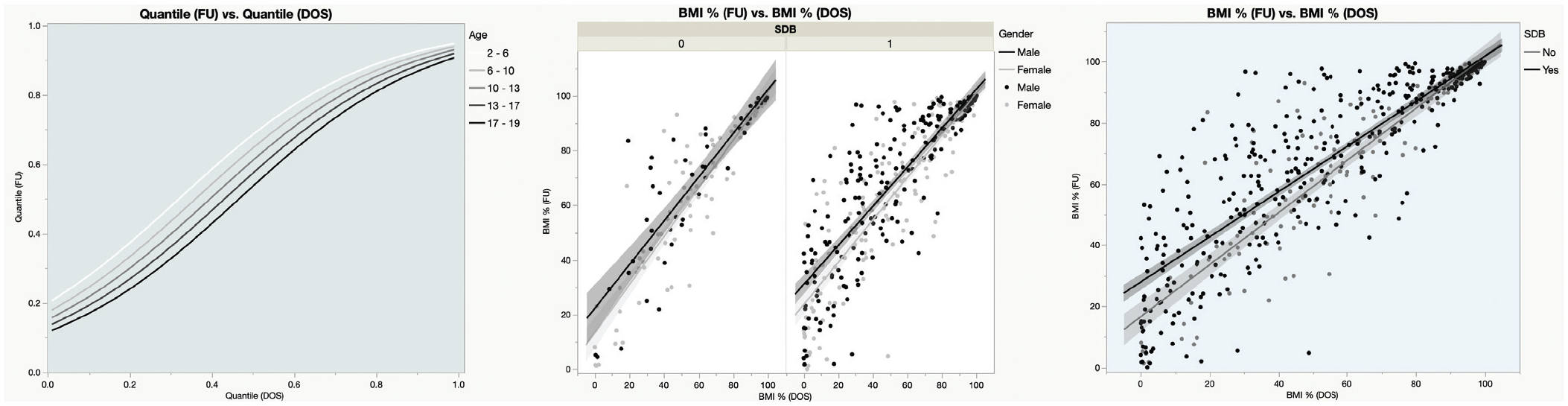
Body mass index percentage (BMI%) at follow-up (FU) vs BMI% on day of surgery (DOS) stratified by (A) age group (
Discussion
The effect of tonsillectomy on pediatric weight gain has been characterized to a limited extent in the current literature with conflicting results in the short-term postoperative period. Our study demonstrates that tonsillectomy is associated with significant postoperative weight gain in almost all children at our tertiary academic institution, with particularly increased risk in the younger, male, SDB, and preoperatively obese pediatric population.
Prior observational studies have been conducted in an effort to understand associations between tonsillectomy and weight gain. A study by Smith et al. comparing pediatric patients with OSA to patients with RT found that the BMI
In this current cohort, children with SDB had a higher propensity for obesity at the time of surgery as compared to children undergoing tonsillectomy for RT, which is consistent with our previously reported findings. 22 This gap in proportions of obese patients by surgical indication appears to increase with time following surgery ( Table 2 ). Existing research has not identified a causal relationship between tonsillectomy and weight gain in this subgroup, but in this observational study, we report a significant association between weight gain and the surgical indication of SDB. The underlying pathophysiology of the postoperative weight gain has been hypothesized but not yet elucidated. Systemic inflammation and increased circulating inflammatory factors are thought to be a component of OSA and SDB with the theory that correcting these imbalances with tonsillectomy may improve the overall health of the child.23-25 However, our data show that simply correcting the SDB may not reverse or correct the growth trajectory in obese children and may even accelerate it. Furthermore, the pervasiveness of residual OSA/SDB after surgical treatment has been reported as high as 72.8% in the literature. 26 In our practice, Lee et al 27 previously reported an overall rate of 53% complete resolution of OSA following tonsillectomy in obese patients, and 18% of the patients required additional intervention for their residual OSA in the form of nighttime airway support. The postoperative weight gain may contribute at least partially to the incomplete resolution of SDB and remains an important issue to be addressed in understanding the risk factors that predispose children to persistent SDB following surgery.
Given the morbidity of SDB and a host of downstream associated complications, tonsillectomy will likely remain the first-line surgical treatment for children in the foreseeable future. However, physicians need to be cognizant of the long-term implications of weight gain observed after surgery and be aware of such adverse impacts on children’s long-term health. Current standard-of-care practice does not dictate routine follow-up for most pediatric patients following tonsillectomy, except in high-risk patients such as those with documented severe OSA prior to surgery who require postoperative sleep studies. 28 Clinicians need to be aware of the propensity for postoperative weight gain in patients with SDB undergoing tonsillectomy and provide the appropriate counseling for patients and their families when reviewing surgical risks and benefits. For children with mild OSA, family-centered obesity treatment has been shown to improve and normalize the apnea-hypopnea index (AHI) without surgical intervention. 29 In light of the potential postoperative weight gain, weight management may provide a better overall health outcome in these patients when compared to surgical treatment. Furthermore, we should consider implementing follow-up in all patients 6 to 12 months postoperatively to identify those with worsening obesity and/or clinical signs and symptoms of recurrent/residual SDB. Last, given the prevalence of both SDB and obesity, we propose that the treatment of pediatric OSA/SDB should be approached in a broader multidisciplinary fashion similar to cleft and craniofacial clinics or aerodigestive teams. In order to achieve better long-term outcomes, multidisciplinary care should be provided to most children with sleep disorders rather than only those with genetic syndromes, complex comorbidities, or those who have failed surgical treatment. The team should involve otolaryngologists, pulmonologists, nutritionists, nurses, and social workers with appropriate counseling on healthy lifestyle changes and weight management before and after surgery.
Limitations to this study include some component of selection bias for patients with available follow-up data due to the retrospective nature of the study design. This bias was likely insignificant as a preliminary analysis demonstrated no significant differences in baseline variables investigated as potential predictors between those with and without available follow-up BMI data. We also do not have a “normal control” group where children with the same obesity profile were followed over time who did not undergo tonsillectomy. Second, our study characterized postoperative BMI changes within a relatively short-term follow-up period, and thus long-term effects of tonsillectomy on patients’ weight status cannot be derived from this study. There is variability in the measurements of height and weight among the various clinics; therefore, comparisons made between patients may not be consistent over the entire follow-up period. Due to the retrospective nature of the study design, the follow-up intervals range widely, making the BMI analysis less precise. However, Gerserick et al
30
demonstrated that greatest acceleration of BMI tends to occur very early in childhood, and the risk of obesity remains stable during school years and adolescence. Although the CDC growth charts are widely used clinically to classify childhood obesity, both BMI percentile and BMI
Conclusion
We observed a significant increase in BMI percentile following tonsillectomy, especially in younger, male, and obese patients undergoing surgery for SDB. The weight gain accounted for a significantly increased proportion of the overall cohort being classified as overweight or obese after surgery. Clinicians need to be aware of the propensity for postoperative weight gain in pediatric patients with SDB undergoing tonsillectomy and provide the appropriate counseling for patients and their families when reviewing surgical risks and benefits. In order to achieve better long-term outcomes, multidisciplinary care may be necessary for children with sleep disorders and obesity with emphasis on nutrition, healthy lifestyle changes, and weight management before and after surgery.
Author Contributions
Disclosures
Footnotes
This article was presented as a poster virtually at the American Society of Pediatric Otolaryngology (ASPO)/Combined Otolaryngology Spring Meeting (COSM) Annual 2021 Conference, April 7-11, 2021.
