Abstract
Case Report
This study was exempt by Vanderbilt University Medical Center Institutional Review Board (IRB #210379). A 19-year-old previously healthy man experienced an electrocution injury after contact with a homemade wood-carving device consisting of jumper cables, a car battery, and wires obtained from a microwave. He subsequently went into cardiopulmonary arrest requiring resuscitation and intubation. Initial exam was notable for electrical burns to lips and bilateral palms. The patient was extubated 3 days following the injury and reported throat pain without difficulty breathing. Two weeks after the accident, he developed progressively worsening dyspnea, which he self-managed with his father’s continuous positive airway pressure (CPAP) device. He reportedly visited external emergency departments a total of 6 times, over 3 months, for acute respiratory distress before presenting to our clinic for further management. On evaluation, he reported worsening dyspnea and dysphagia with an associated 20-lb weight loss. In-office laryngoscopy revealed bilateral vocal fold immobility with fixation in the paramedian position.
The patient was taken to the operating room for direct laryngoscopy and tracheostomy. Intraoperative assessment revealed normal mobility of bilateral cricoarytenoid joints without evidence of scarring. A 6-0 cuffless Shiley tracheostomy tube was subsequently placed given degree of respiratory distress and hope for the return of vocal fold function. Postoperatively, the patient reported improvement in his breathing and swallow. Unfortunately, his vocal fold motion showed no signs of improvement at 2-, 4-, and 12-month follow-up visits ( Figure 1 ). The patient was interested in undergoing cordotomy but was lost to follow-up.
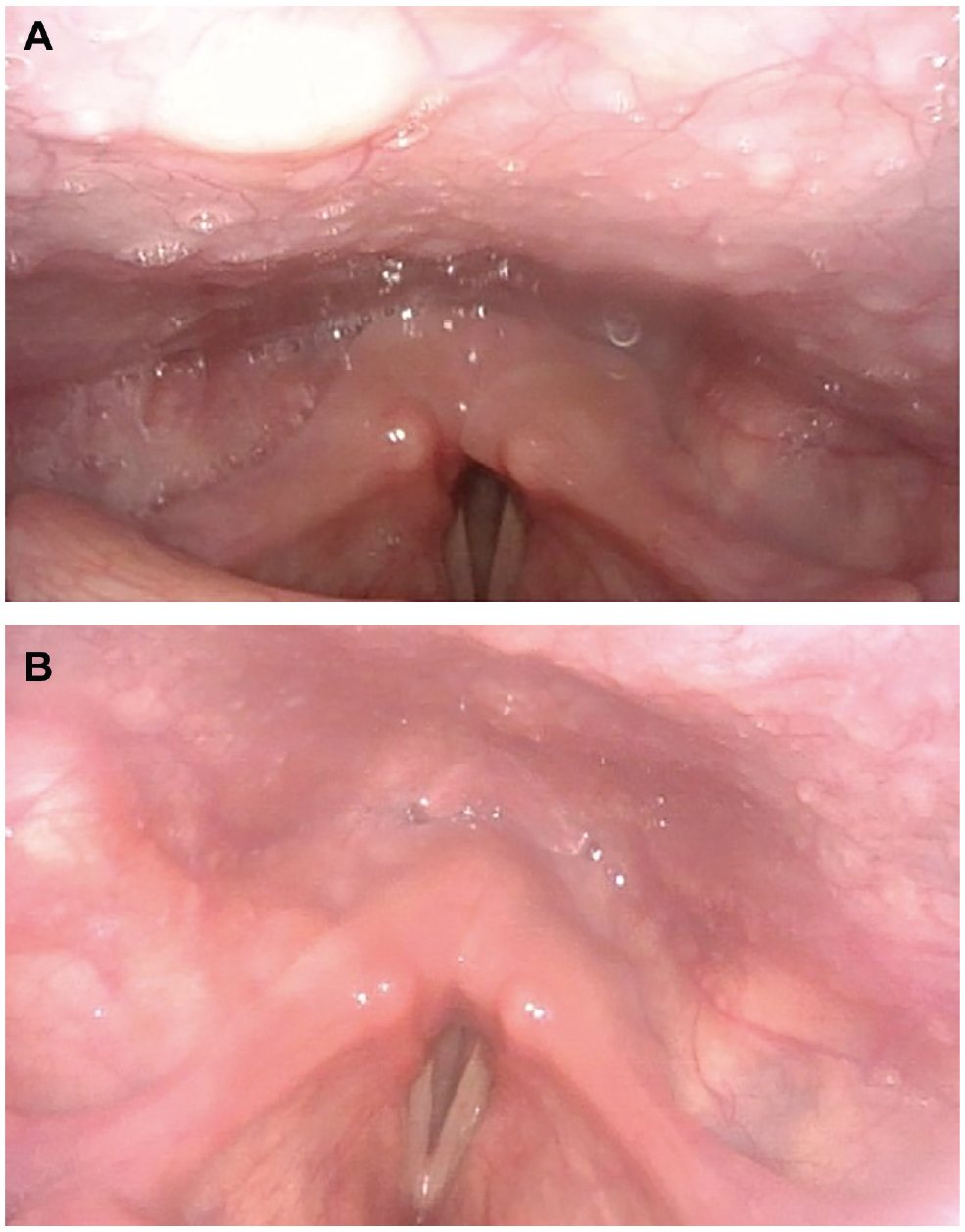
Laryngoscopy image from 2 months (a) and 4 months (b) posttracheostomy tube placement. Both images captured during full inspiration.
Discussion
Neurologic injury is common after electrocution injury and can manifest through a variety of presentations, including numbness, paresthesia, pain, tinnitus, and vision loss. 1 Notably, low-voltage electric shocks most often result in relatively minor and transient sequelae. In this article, we present the first case of a chronic recurrent laryngeal nerve (RLN) injury following an electrocution injury, review presumptive pathophysiology pertaining to this injury, and discuss subsequent management.
Our patient exhibited burn injuries to his palms and lips, demonstrating a hypothesized mechanism of injury secondary to an electrical current traveling in a retrograde fashion from the upper extremities to the head and neck region. The nervous system has low resistance to the flow of exogenous electricity, which increases the susceptibility of the brain, spinal cord, and peripheral nerves to electrothermal injury. Aberrant electrical conductance results in hypoxia/vascular compromise, ultimately leading to nerve degeneration and subsequent death from electroporation- increased cell permeability due to exposure to an electrical field. 2 This presentation resembles hypoxic changes seen within the skin following lightning strike injuries, which cause endothelial damage and subsequent vessel occlusion. 3 Further injury may be attributed to free radical damage resulting in progressive demyelination, which can have a delayed presentation as seen in this case. Alternatively, RLN damage could have occurred at the initial electrocution injury with compensatory lateralization developing during the course of intubation. Progressive medialization of the deinervated vocal folds after extubation may have resulted in subsequent airway compromise.
Laryngeal electromyography (LEMG) is a modality useful for distinguishing between disorders involving upper/lower motor neurons, peripheral nerves, the neuromuscular junction, muscle fibers, and the laryngeal cartilages and joints. 4 Unfortunately, we were unable to obtain LEMG in this patient, although at the time of his initial surgery, both arytenoids were freely mobile on palpation. Standard treatment for patients with bilateral vocal fold paralysis is possible, but laryngeal pacing is a developing option that uses selective neurostimulation of the posterior cricoarytenoid (PCA) muscles to reverse the static conformation of the vocal cords and restore vocal fold mobility. Neurostimulation is possible because trauma to the RLN is likely to cause synkinetic reinnervation of the PCA muscles rather than complete denervation. 5 Although our patient was not a candidate for inclusion in the laryngeal pacing trial due to age, the technology has significant potential to affect how we manage patients with bilateral vocal fold in the future by optimizing respiration without sacrificing voice outcomes.
Persistent bilateral vocal fold paralysis following electrocution injury introduces a novel etiology to the literature. Utilization of diagnostic tools, such as LEMG, and further development of novel technologies, such as laryngeal pacing, have the potential to alter the management of patients with bilateral vocal fold paralysis.
Author Contributions
Disclosures
Footnotes
This article has been submitted for oral presentation at 2021 American Academy of Otolaryngology–Head and Neck Surgery Foundation Annual Meeting; October 3-6, 2021; Los Angeles, California.
