Abstract
Objectives
The objectives of this study include characterizing the practice patterns and testing strategies of facial plastic and reconstructive surgery (FPRS) fellowship directors (FDs) secondary to COVID-19 and to quantify the impact of COVID-19 on FPRS fellowship training.
Study Design
Cross-sectional survey.
Setting
Online.
Methods
A survey was sent to all American Academy of Facial Plastic and Reconstructive Surgery FDs and co-FDs in September 2020. Descriptive analyses were performed.
Results
Of 77 eligible FDs, 45 responded (58.4%) representing a diverse group across the United States. All but 1 FD routinely screened patients for COVID-19 in the preoperative setting. FDs largely believed that universal preoperative testing was cost-effective (66.7%), improved patient safety (80.0%) and health care worker safety (95.6%), and was not burdensome for patients (53.3%). With regard to volume of cosmetic/aesthetic, reconstructive, facial nerve, and trauma surgery, FDs indicated largely no change in volume (34.9%, 71.0%, 68.4%, and 80.0%, respectively) or fellow experience (67.4%, 80.6%, 84.2%, and 80.0%). Half (50.0%) of the FDs reported decreased volume of congenital/craniofacial surgery, but 75.0% did not believe that there was a change in fellow experience. Overall, of the 15 responses indicating “worsened training” across all domains of FPRS, 14 were located in the Northeast (93.33%).
Conclusions
The COVID-19 pandemic has had the least impact on the volume of reconstructive procedures, facial nerve operations, and trauma surgery and a negative impact on congenital/craniofacial surgery volume, and it has accelerated the demand for cosmetic/aesthetic operations. Overall, the majority of FDs did not feel as though their fellows’ trainings would be adversely affected by the ongoing pandemic.
Keywords
The novel coronavirus 2019 (COVID-19) pandemic has had a profound impact across the health care industry, including the practices of facial plastic and reconstructive surgeons (FPRSs), plastic and reconstructive surgeons, oculoplastic surgeons, dermatologists, and otolaryngologist–head and neck surgeons (OTO-HNSs).1-7 At the height of the pandemic, federal, state, and local health agencies halted all “nonessential” surgery and outpatient services to help combat contagion. Many surgical societies, including those of OTO-HNSs and FPRSs, issued guidance echoing the need to stop elective procedures.8,9 Such actions posed unique challenges to residency and fellowship programs regarding the educational and clinical training opportunities of trainees.10,11 Surgical trainees have been disproportionately affected by the public health efforts to mitigate the epidemic, as they rely on operative experience to complete their training. 10 Even as operations resumed in later stages of the pandemic, some questioned the risk/reward aspects of allowing fellows/residents to assist in a procedure in which they were not required, given the desire to minimize exposure to workers and patients and utilization of personal protective equipment (PPE). 1
At first, the medical community was focused on controlling the epidemic. Now, 1 year since the World Health Organization first declared a global pandemic, the academic medical community has begun considering the implications of this crisis on residency and fellowship training.4,5 Understanding the effects is imperative to making sure that the next generation of surgeons will be well prepared to begin independent practice and determining whether there is a need for extending fellow training to compensate for time lost. While studies examining the specific training consequences of COVID-19 on residents and fellows are necessary,8,12 few have been done; to date, no such studies have been published regarding FPRSs.
This study aims to characterize the practice patterns and testing strategies of FPRS fellowship directors (FDs) in response to COVID-19 and to summarize the opinions of FPRS FDs regarding preoperative COVID-19 testing. Secondarily, we aimed to understand how the pandemic has affected patient willingness to undergo facial plastic surgery and case volumes among FPRSs. Finally, we strived to quantify the impact of the COVID-19 pandemic on FPRS fellowship training and highlight steps that FDs are taking to mitigate the effects of the pandemic on their trainees’ educations.
Methods
Survey Creation, Content, and Dissemination
This study was granted exemption from review by the Yale Human Investigations Committee. The Yale Qualtrics Survey Tool (Qualtrics) was utilized to create a cross-sectional survey, which contained 17 to 20 questions with inputted logic. Five questions gathered information on practice specifics, 7 on COVID-19 pre- and postoperative testing practices, 4 on the opinions of FDs regarding universal preoperative COVID-19 testing, and 4 on changes in operative volume secondary to the pandemic and its effect on fellow training.
The survey was emailed out via the American Academy of Facial Plastic and Reconstructive Surgery (AAFPRS) to all 51 FDs and 26 codirectors (77 possible participants) on August 30, 2020. A reminder email was sent September 19, 2020. The survey was closed on September 30, 2020. Descriptive analyses were performed.
Results
Survey Population
We received 45 completed survey responses, constituting 58.4% of all AAFPRS FDs and co-FDs. The respondents had a broad geographic distribution, and most had been in practice for >20 years (51.1%) or 16 to 20 years (26.7%). Practice composition showed that 95.6% were performing cosmetic/aesthetic surgery, 68.9% reconstructive, 42.2% facial nerve, 33.3% trauma, and 17.8% congenital/craniofacial. Practice setting included 20.0% in a solo practice, 33.3% in a small private group (2-5 members), and 44.4% in academics. Most (55.6%) operated in an ambulatory surgery center and 33.3% in a tertiary care center (Supplemental Table S1, available online).
COVID-19 Testing Protocols and Opinions
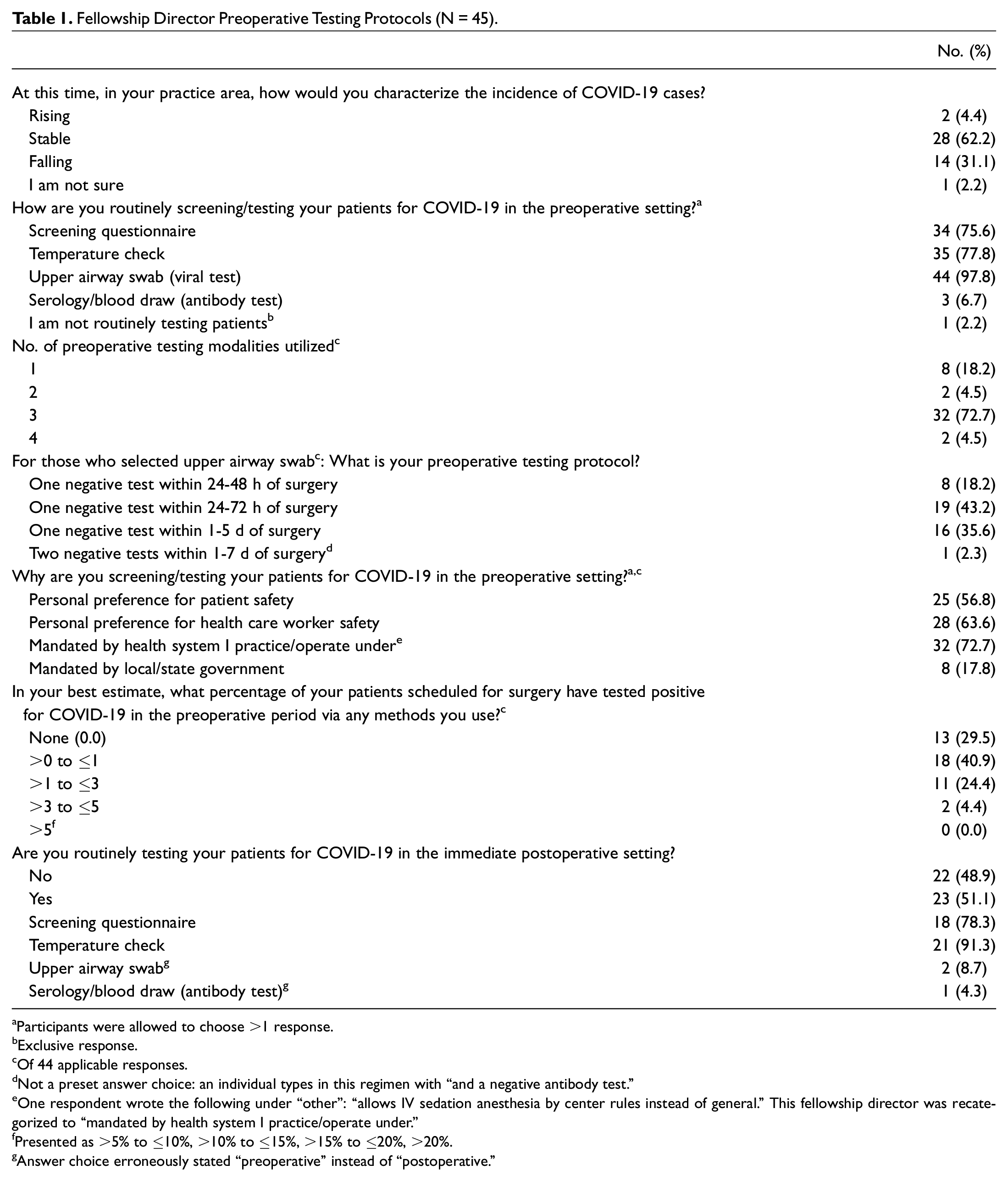
At the time of survey completion, 62.2% of FDs indicated that COVID-19 incidence rates in their regions had been stable, and 31.1% indicated that they were falling. All but 1 FD was routinely screening patients in the preoperative setting for COVID-19. Of the 44 FDs who screened in the preoperative setting, 22.7% utilized 1 or 2 modalities of testing; 72.7%, 3 modalities; and 4.5%, 4 modalities. All 44 FDs who screened patients did so via upper airway swabs (100%). Of those who utilized an upper airway swab, the majority (97.7%) required 1 negative test. The preoperative screening practices of FDs are summarized in Table 1 .
Fellowship Director Preoperative Testing Protocols (N = 45).

Participants were allowed to choose >1 response.
Exclusive response.
Of 44 applicable responses.
Not a preset answer choice: an individual types in this regimen with “and a negative antibody test.”
One respondent wrote the following under “other”: “allows IV sedation anesthesia by center rules instead of general.” This fellowship director was recategorized to “mandated by health system I practice/operate under.”
Presented as >5% to ≤10%, >10% to ≤15%, >15% to ≤20%, >20%.
Answer choice erroneously stated “preoperative” instead of “postoperative.”
Of the 44 FDs who screened their patients in the preoperative setting, 72.7% stated that it was mandated by their health system; 63.6% said that it was a personal preference for health care worker safety; 56.8% indicated that it was a personal preference for patient safety; and 17.8% reported that it was mandated by the local/state government ( Table 1 ). In addition to testing in the preoperative testing, 23 (51.1%) of the 45 FDs stated that they screened patients in the postoperative setting in some capacity.
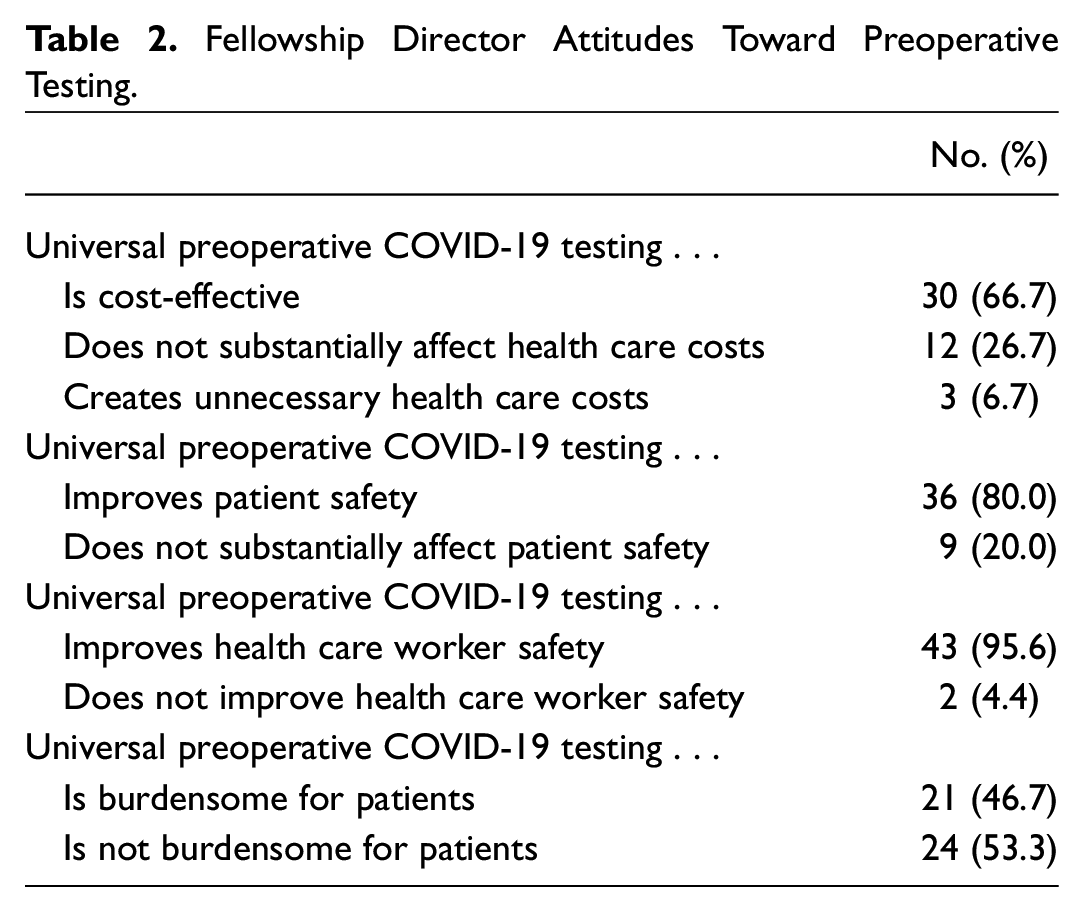
To understand opinions on universal preoperative COVID-19 testing, FDs were asked to complete 4 statements. Complete responses are shown in Table 2 . In short, 66.7% believed that universal preoperative testing is cost-effective; 95.6%, that it improved health care worker safety; 80.0%, that it improved patient safety; and 46.7%, that it was burdensome for patients.
Fellowship Director Attitudes Toward Preoperative Testing.
Impact of COVID-19 on Volume and Training
Cosmetic Surgery
Of those who performed cosmetic/aesthetic surgery (n = 43), 46.5% indicated no change in patient willingness to undergo surgery during the pandemic, though 34.9% and 18.6% indicated more and less willingness, respectively ( Figure 1A ). With respect to volume, 37.2% of FDs experienced an increase, 34.9% no change, and 27.9% a decrease ( Figure 1B ). Ultimately, 67.4% stated that, in their opinion, there was no change to their fellows’ training; 20.9%, that COVID-19 actually improved fellow training; and 11.6%, that it worsened the experience ( Figure 1C ).
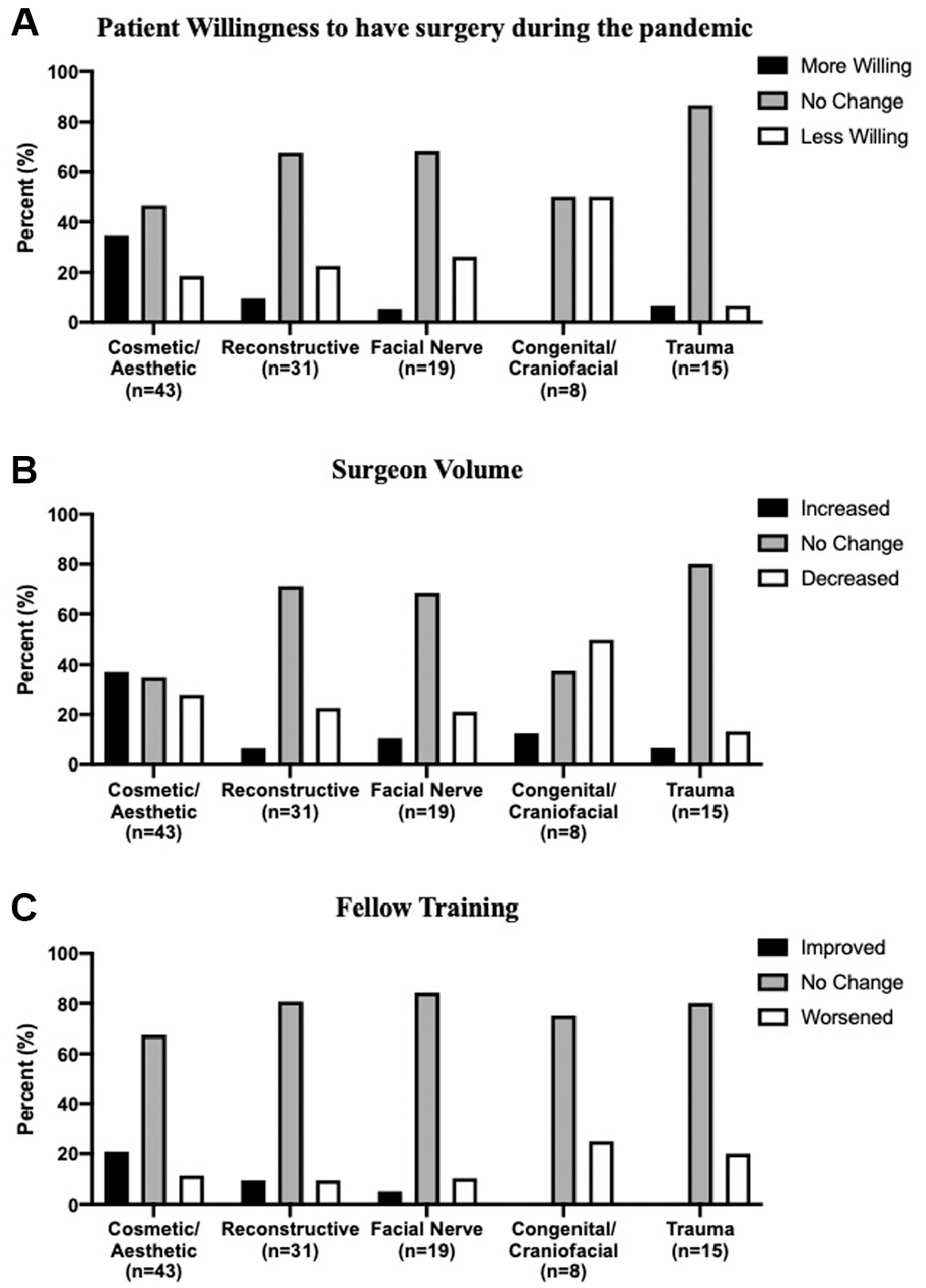
COVID-19–induced change in (A) patient willingness to have surgery, (B) surgeon volume, and (C) fellow training.
Reconstructive Surgery
Of those who performed reconstructive surgery (n = 31), 67.7% indicated no change in patient willingness to undergo surgery during the pandemic, though 22.6% indicated less willingness ( Figure 1A ). With respect to volume, 71.0% experienced no change and 22.6% a decrease ( Figure 1B ). Overall, 80.6% indicated that there was no change to their fellows’ training secondary to COVID-19 ( Figure 1C ).
Facial Nerve Surgery
Of those who performed facial nerve surgery (n = 19), 68.4% indicated no change in patient willingness to undergo surgery during the pandemic, though 26.3% indicated less willingness ( Figure 1A ). With respect to volume, 68.4% experienced no change and 21.1% a decrease ( Figure 1B ). Ultimately, 84.2% stated that there was no change to their fellows’ training secondary to COVID-19 ( Figure 1C ).
Congenital/Craniofacial Surgery
Of those who performed congenital/craniofacial surgery (n = 8), 50.0% indicated no change in patient willingness to undergo surgery during the pandemic, and 50.0% indicated less willingness ( Figure 1A ). With respect to volume, 37.5% experienced no change and 50.0% a decrease ( Figure 1B ). Overall, 75.0% stated that there was no change to their fellows’ training secondary to COVID-19, as compared with 25.0% who said it worsened the experience ( Figure 1C ).
Trauma Surgery
Of those who performed trauma surgery (n = 15), 86.7% indicated no change in patient willingness to undergo surgery during the pandemic ( Figure 1A ). With respect to volume, 80.0% experienced no change and 13.3% a decrease ( Figure 1B ). Ultimately, 80.0% stated that there was no change to their fellows’ training secondary to COVID-19 ( Figure 1C ).
Variations in Training Experience Based on Geography
Overall, of 43 FDs who practice cosmetics/aesthetics, 5 (11.6%) believed that fellows would experience “worsened training” secondary to the pandemic. Of these 5 FDs, 4 (80.0%) practiced in the Northeast, with 1 practicing in the Midwest. Similar trends were seen within the other domains of facial plastic and reconstructive surgery. Among all responses, the following believed that trainees would have “worsened training”: 2 (25.0%) of 8 practicing congenital/craniofacial surgery, 3 (20.0%) of 15 performing trauma surgery, 2 (10.5%) of 19 performing facial nerve operations, and 3 (9.7%) of 31 FDs practicing reconstructive surgery. Of these responders, 100% were located in the Northeast. Of the 15 responders indicating “worsened training” across all domains of facial plastic and reconstructive surgery, 14 (93.3%) were located in the Northeast.
Efforts to Improve Fellow Training During the COVID-19 Pandemic
All respondents were given an optional free response question, “How are you trying to mitigate any training challenges for your fellows due to the pandemic?” and 12 (26.6%) answered it. While the full list of unedited responses is presented in Supplemental Table S2 (available online), several general themes emerged upon review. First, FDs considered the risks and benefits of continuing to have fellows assist with surgery in the context of the service benefit to the patient. Second, FDs highlighted the importance of proper PPE and patient testing protocols to mitigate risks to patients and fellows. Third, 6 of 12 (50%) of respondents emphasized a greater use of online didactic materials (eg, lectures, webinars) to supplement fellow education. Last, FDs who implied presence at high-volume centers noted that the fellow experience was unchanged—that is, even with the decrease in operative volume induced by COVID-19, the program still performed more cases than the fellow was able to cover.
Discussion
The COVID-19 pandemic continues to have unprecedented societal implications across the world. For the medical community, the paramount concern is optimizing patient outcomes while keeping health care workers safe and minimizing contagion. In particular, FPRSs and OTO-HNSs have been found to be at greater risk for contracting COVID-19, as they commonly work in nasal, oral, pharyngeal, and respiratory epithelium and perform aerosol-generating procedures.1,3,5,13,14 As such, their respective societies have emphasized the need for proper PPE and the use of appropriate COVID-19 screening.1,9 While anecdotal evidence of trainees working without necessary PPE has surfaced, 4 our results suggest that FDs—generally considered experts in their fields by their colleagues and integral to advanced surgical training in facial plastic and reconstructive surgery—are making concerted efforts to comply with recommended PPE and universal precautions for their fellows, as well as preoperative screening protocols for their patients. In fact, all but 1 FD reported employing upper airway swabs to test for COVID-19 in the preoperative setting; moreover, the majority of respondents were using 3 separate tools preoperatively. A slight majority of FDs even continued to screen their patients for COVID-19 in the postoperative setting. Overall, our results suggest that FDs are compliant with national guidelines concerning preoperative COVID-19 screening.9,13,15-21
Interestingly, one-third of FDs estimated that none of the patients whom they screened preoperatively tested positive for COVID-19 prior to surgery, while the majority estimated that 0% to 3% of patients were positive in the preoperative period. As community prevalence of COVID-19 has fluctuated nationwide since our survey closed, the rates of preoperative positivity may have since changed. 22 Overall, we found that the majority of respondents believe that universal preoperative COVID-19 testing is cost-effective, enhances patient safety, and protects health care workers. Despite the perceived benefits of preoperative testing, 46.7% of FDs noted that universal testing was “burdensome” for patients. As such, FPRSs may benefit from working with the medical community to reduce the burden of preoperative testing on patients; vaccination programs and improvements in rapid-testing mechanisms are promising in this regard.
At the onset of the pandemic, the field of facial plastic and reconstructive surgery was substantially affected by the national moratorium on “nonessential” medical services, including elective surgery. 5 As hospitals, practices, and surgery centers have resumed services, many have questioned the effect that the pandemic has had on patient willingness to undergo surgery and operative case volumes. Our findings suggest that the pandemic has had the least impact on reconstructive procedures, facial nerve operations, and trauma surgery. This supports our hypothesis that the pandemic would have a lesser effect on these cases, as many of these operations are medically necessary and time-sensitive. 5 Numerous studies demonstrate the need for timely reconstruction in patients with acute or chronic facial palsy, 5 head and neck cancer reconstruction,23,24 and facial trauma25-28 to maximize long-term patient outcomes. Albeit in a small sample size (n = 8), we found that half of all respondents reported a decrease in patient willingness to undergo congenital/craniofacial surgery, as well as a decline in operative volumes. Our findings are consistent with a recent study of pediatric OTO-HNS fellowship training, which found that 86.3% of pediatric OTO-HNS FDs reported a decline in surgical volume. Of note, many craniofacial/congenital maladies also require timely intervention. Hence, examining the effects of delayed care induced by the pandemic for congenital/craniofacial cases may be an important area of future study. Finally, patient willingness and surgeon volume for cosmetic/aesthetic procedures were notably elevated, especially when compared with the other domains of facial plastic and reconstructive surgery. This supports recent reports of “pent-up” demand for facial plastic surgery during the pandemic.1,8,29-32 Moreover, we surmise that quarantine and stay-at-home orders, face mask mandates, and the rise in individuals working from home have likely created a unique circumstance favoring patients who wish to have privacy while recovering from cosmetic surgery. Others have noted a rise in patient concerns regarding facial appearance that are highlighted while using video-conferencing platforms, which may also be catalyzing surgery demand. 31
Many in the OTO-HNS community have speculated on the impact of COVID-19 on fellows’ training and preparedness.10,12 Some worry that reductions in operative volume may negatively affect fellowship training. 10 A recent study surveying pediatric OTO-HNS FDs supported this notion, with 77.2% reporting a “significant impact on overall fellowship training” in clinical and operative settings. 10 Moreover, the study found that 68.2% of pediatric OTO-HNS FDs reported a mild or moderate impact on their fellows’ abilities to become “well trained.” 10 A similar study among oculoplastic FDs reported that 94.4% of respondents predicted adverse effects on their fellows’ training. 4 In the same study, 75% of oculoplastic fellows themselves reported a decline in surgical confidence as a result of the pandemic. 4 Our findings are notable in that the majority of respondents did not feel that their fellows’ trainings would be adversely affected by the ongoing pandemic. This finding was true across all 5 studied domains of facial plastic and reconstructive surgery, with the majority of FDs noting “no change” or “improved” training. Overall, our findings suggest that the training of FPRSs, while undoubtedly affected, may not have suffered substantially as a result of the pandemic. This finding is important when determining the preparedness of the next generation of FPRSs. Notably, we found that the majority of “worsened fellow training” responses within the 5 facial plastic and reconstructive surgery domains came from FDs practicing in the Northeast. This finding may reflect the concentration of Northeastern facial plastic and reconstructive surgical fellowship programs in big cities that were devastated by the pandemic and/or differences in local and state regulations surrounding elective cases in the Northeast as compared with elsewhere. Any future increase in COVID-19 cases and/or lockdowns may cause the negative effects on fellow training to spread across the country.
Last, our results indicate that FPRS FDs have embraced technology and online learning to supplement their fellows’ training. The use of virtual education has been lauded as a safe way to support trainee education during the pandemic.3,4,10 Continued innovation in virtual education mediums is promising and will likely play a larger role in trainee education moving forward.
There are several limitations to this study. First, as with any survey, this study is subject to recall bias, which may affect the accuracy of results. Second, while our response rate was robust, included a majority of all AAFPRS FDs, and was similar to related studies in other specialties,4,10 our results may be subject to response bias. Third, the timing of this study (August/September 2020) offers a snapshot of the evolving pandemic. As new “waves” of the virus have occurred nationally since our survey closed, 22 it is possible that the pandemic’s effect on fellowship training has been more negative than reflected in our results. Moreover, differences in local and state regulations and the varied impact of the virus on different areas of the nation may reduce the generalizability of our results. Last, the timing of our study allowed FDs to respond using experiences from 2 fellowship classes (2019-2020 and 2020-2021). While this is a strength of our study, it is also a weakness, as we are unable to distinguish nuances in the ways that the impact on fellowship training has evolved since the epidemic started. It is possible that the 2019-2020 fellowship class suffered disproportionately due to the restrictions of elective surgery in some locations during the early months of the pandemic. 10 However, fellows in the 2020-2021 class entered their fellowships in the middle of the pandemic, at which point the medical community was adapting to the “new normal.” Future studies surveying AAFPRS FDs may be beneficial in elucidating the ultimate impact on fellowship training, especially as we approach the final stages of the pandemic.
Notably, we did not survey AAFPRS fellows themselves about their experience during the epidemic. Future studies may benefit from incorporating the viewpoints of fellows, as well as from objectively comparing fellowship case logs and the job placement for fellows trained during the pandemic. Ultimately, understanding the experience of FPRS fellows during this time is critical not only to assist fellows affected by the ongoing pandemic but also to create initiatives to mitigate negative impacts on trainees during future epidemics and disasters.
Conclusions
Among respondents, the majority of AAFPRS FDs are in compliance with recommended preoperative COVID-19 screening protocols and believe that universal preoperative COVID-19 testing is cost-effective, enhances patient safety, and protects health care workers. Our findings suggest that the pandemic has had the least impact on the surgical volume of reconstructive procedures, facial nerve operations, and trauma surgery, as well as a negative impact on congenital/craniofacial surgery volume. Our results support recent reports of increasing demand for, and volume of, cosmetic/aesthetic operations. Overall, the majority of respondents did not feel as though FPRS fellows’ trainings would be adversely affected by the ongoing pandemic. Many respondents emphasized the importance of virtual education in supplementing fellow education during the epidemic. Lessons from this pandemic may serve as a foundation to prepare the AAFPRS and its fellows for any future crises that may arise.
Supplemental Material
sj-docx-1-opn-10.1177_2473974X211014130 – Supplemental material for Effects of COVID-19 on Facial Plastic and Reconstructive Surgery Fellowship Training and Director Practices
Supplemental material, sj-docx-1-opn-10.1177_2473974X211014130 for Effects of COVID-19 on Facial Plastic and Reconstructive Surgery Fellowship Training and Director Practices by Parsa P. Salehi, Sina J. Torabi, Yan Ho Lee and Babak Azizzadeh in OTO Open: The Official Open Access Journal of the American Academy of Otolaryngology-Head and Neck Surgery Foundation
Footnotes
Acknowledgements
We thank the American Academy of Facial Plastic and Reconstructive Surgery for approving this survey study for dissemination to the its fellowship directors and codirectors.
Author Contributions
Disclosures
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
