Abstract
Objective
Increasingly, total thyroidectomy is offered as an ambulatory procedure. Most of the relevant outcomes research derives from academic centers, but most thyroid surgeries are performed in the community. The goal of this study is to evaluate the safety of total thyroidectomy performed as an ambulatory procedure in a community otolaryngology practice.
Study Design
Retrospective review and national database analysis.
Setting
A single community otolaryngology practice.
Methods
Adult patients undergoing total thyroidectomy by a single otolaryngologist between 2013 and 2019 were divided into 2 cohorts: planned ambulatory and planned admission. Charts were reviewed for demographics and surgical outcomes in the 2 groups. The Healthcare Cost and Utilization Project databases for New York and Florida between 2015 and 2016 were also analyzed to compare outcomes of thyroidectomy as an ambulatory surgery between different practice settings.
Results
A total of 99 total thyroidectomies were performed during the study time period; 66 of 99 (67%) were planned as ambulatory procedures and 33 of 99 (33%) were planned admissions. Five of the 66 (8%) planned outpatient surgeries required admission. Complications of vocal fold dysfunction, symptomatic hypocalcemia, and seroma formation were more commonly seen in the inpatient cohort. Only 2 ambulatory patients required admission after discharge. Nationally, odds of complication were higher for ambulatory total thyroidectomy at nonteaching practice sites, which is not duplicated in our study.
Conclusions
Ambulatory total thyroidectomy can be undertaken safely in the community in carefully selected cases.
Approximately 93,000 thyroidectomies are performed each year in the United States. 1 Increasingly, these procedures are performed on an ambulatory basis. 2 There is also a national trend toward surgical management of thyroid conditions by the otolaryngologist. 3 In 2013, the American Thyroid Association (ATA) released a statement on outpatient total thyroidectomy, providing guidelines for proper steps to be taken to perform ambulatory thyroid surgery safely. 2
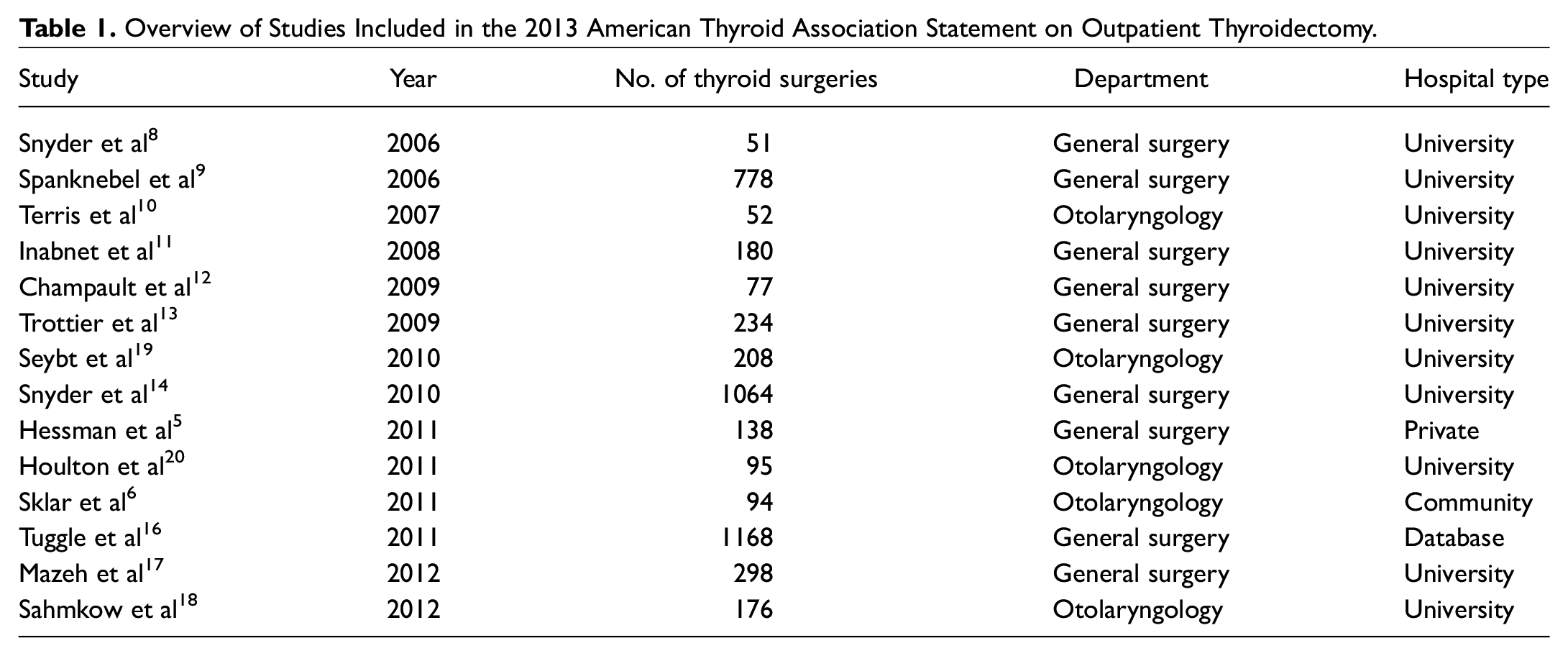
There are several publications on the safety of thyroidectomy as an ambulatory procedure, but such findings derive largely from academic centers. Today, thyroid surgery is commonly performed in the community by the otolaryngologist. 4 Of the 14 studies reviewed in the ATA statement, only 2 reflect nonacademic practice settings ( Table 1 ).5-18 Hessman et al 5 describe the outcomes of 72 patients who underwent total thyroidectomy by a single general surgeon at a private hospital in Portland, Oregon. They identified that male sex and Graves’ disease put patients at higher risk for unplanned admission in their cohort. Sklar et al 6 describe 94 outpatient hemithyroidectomies performed in a community hospital in Canada, of which 5 patients required unplanned inpatient stay. In a separate study, Ayala and Yencha 7 report 61 cases of successful ambulatory total thyroidectomy at a small low-volume hospital.
Overview of Studies Included in the 2013 American Thyroid Association Statement on Outpatient Thyroidectomy.
Ambulatory procedures may be of greater relevance to community practices because such practices tend to see less complicated cases and therefore have a higher number of patients suitable for ambulatory surgery. Moreover, patients are more apt to live near the community surgical facility, facilitating access in the event of an adverse postoperative event. The current body of literature disproportionately reflects academic settings, and more research is needed from the community to mirror current practice patterns.
The objective of this study is to evaluate the feasibility and safety of ambulatory total thyroidectomy in a community otolaryngology practice. We have previously demonstrated successful outcomes in diagnostic workup of thyroid nodules in our community thyroid practice by adherence to national guidelines and implementation of uniform protocols. 21 We hypothesize that by following the same principles we can achieve safety profile of ambulatory total thyroidectomy in community practice that is comparable to tertiary care setup.
Methods
Retrospective Chart Review
This is a retrospective review of all patients who underwent total thyroidectomy between 2013 and 2019 by a single otolaryngologist in a community practice based in southern Massachusetts, affiliated with Tufts Medical Center. A total of 99 patients were divided into 2 cohorts: planned ambulatory surgery (66/99) and planned admission (33/99) ( Table 2 ).
Criteria for Admission After Total Thyroidectomy.
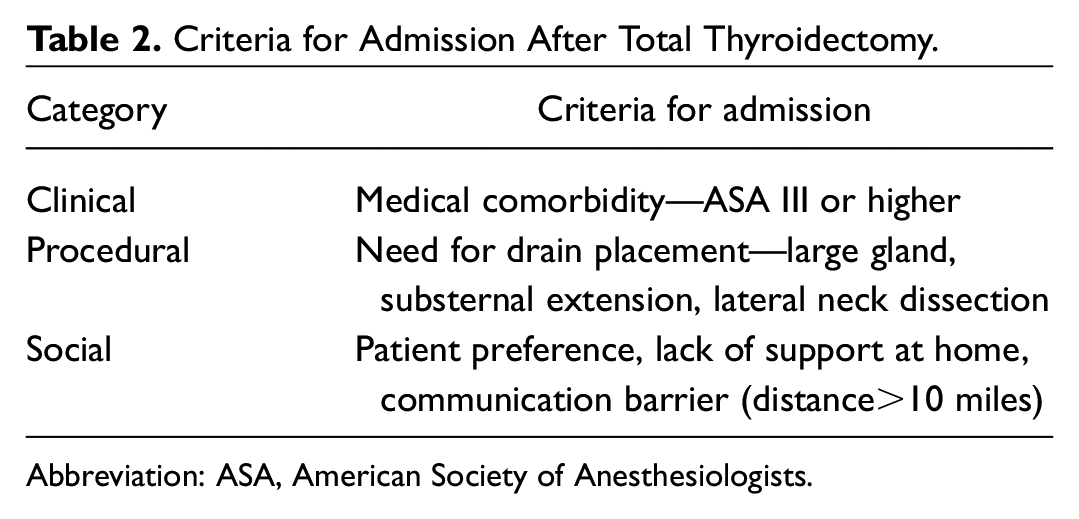

Abbreviation: ASA, American Society of Anesthesiologists.
Medical records were reviewed for patient demographics, indication for thyroid surgery, medical comorbidities, intraoperative findings, and postoperative courses. Primary end points were unplanned conversion to admissions group, surgical course, readmission rates, and complications, including vocal fold dysfunction, symptomatic hypocalcemia, seroma, or hematoma formation. Vocal fold dysfunction was defined as voice complaints with or without immobility or hypomobility of the vocal cord noted on flexible laryngoscopy on first postoperative visit at 7 to 10 days. Approval from the Tufts Medical Center Institutional Review Board was obtained for this study.
National Database Query
Concurrently, we analyzed cases of ambulatory total thyroidectomy reported in the Healthcare Cost and Utilization Project state databases for New York and Florida between 2015 and 2016. 22 Data were collected on rates of postoperative complications, including vocal fold paralysis, seroma/hematoma formation, and hypoparathyroidism, among 3 different practice settings: rural, urban nonteaching, and urban teaching.
Management Algorithm for Ambulatory Total Thyroidectomy
Patients are divided into planned admission or planned ambulatory cohort prior to the surgery ( Table 2 ). All surgeries, including planned ambulatory surgeries, are performed in a hospital setting.
Salient points of the surgical procedure and postoperative care are as follows. The proposed incision site is marked and infiltrated with 10 mL of 1% lidocaine with 1:100,000 epinephrine in the preoperative holding area approximately 30 minutes prior to skin incision. During surgery, the patient is placed in a semisupine, “beach chair” position to avoid venous congestion. Intraoperative monitoring of the recurrent laryngeal nerve is routinely used. At the end of the surgical resection, a forced Valsalva procedure is performed to ensure absence of bleeding. Gelfoam (Pfizer) soaked in thrombin is placed in the paratracheal gutters. Upper half of the strap muscles is loosely approximated with 3-0 Vicryl (Ethicon) sutures. Deep extubation is uniformly preferred. All patients receive 8 to 12 mg Decadron (Merck) and antiemetic drugs. No drains are used, and any unplanned placement of a drain results in conversion to admission group. Typical ambulatory management involves a combined 4-hour period of recovery in the acute postanesthesia care unit and step-down unit. The patient is monitored for nausea and vomiting, airway symptoms, ability to retain liquids, and any signs of neck hematoma. Postoperative calcium and parathyroid hormone levels are not routinely checked. Rather, patients are started empirically on calcium carbonate taper over a 3-week period. 23 Scripts for laboratory draws for calcium and parathyroid hormone level are provided with instructions for a blood draw 48 to 72 hours postsurgery. Patients are instructed in detail about symptoms of neck swelling and hypocalcemia. Patients are scheduled for follow-up at 7 to 10 days after surgery to survey the wound and assess the voice. At this time, calcium supplementation is discontinued if the calcium and parathyroid hormone (PTH) levels are in the normal range.
Statistical Analysis
For continuous variables, a Student t test was used for normally distributed data and the Mann-Whitney U test was used for nonparametric data. For categorical variables, either a Fisher exact test or χ2 test was employed. A result was considered significant at a P value of .05. The analysis was performed by using the GraphPad Prism version 8.0 software (GraphPad Software).
Results
In the 7-year period including years 2013 through 2019, the senior author performed a total of 99 total thyroidectomies and 106 thyroid lobectomies, yielding a total of 205 thyroidectomies, at an average of 29 thyroid surgeries per year. This would be considered an intermediate-volume surgeon. 24
Of these 99 total thyroidectomy patients, 67% (66/99) were assigned to the ambulatory surgery and 33% (33/99) were assigned to the admission group. There was a significant difference in median age of each cohort, as those undergoing day surgery were younger (55 years) than the inpatients (64 years), P = .02 ( Table 3 ). The ambulatory cohort also tended to have a higher proportion of malignant pathology (67% vs 54%) and smaller median nodule size (2.0 vs 2.9 cm) and lived closer to the surgical facility—average 7.1 vs 10.1 miles in the admission group. None of these differences, however, were statistically significant in univariate analyses.
Presenting Characteristics Stratified by Ambulatory vs Inpatient.
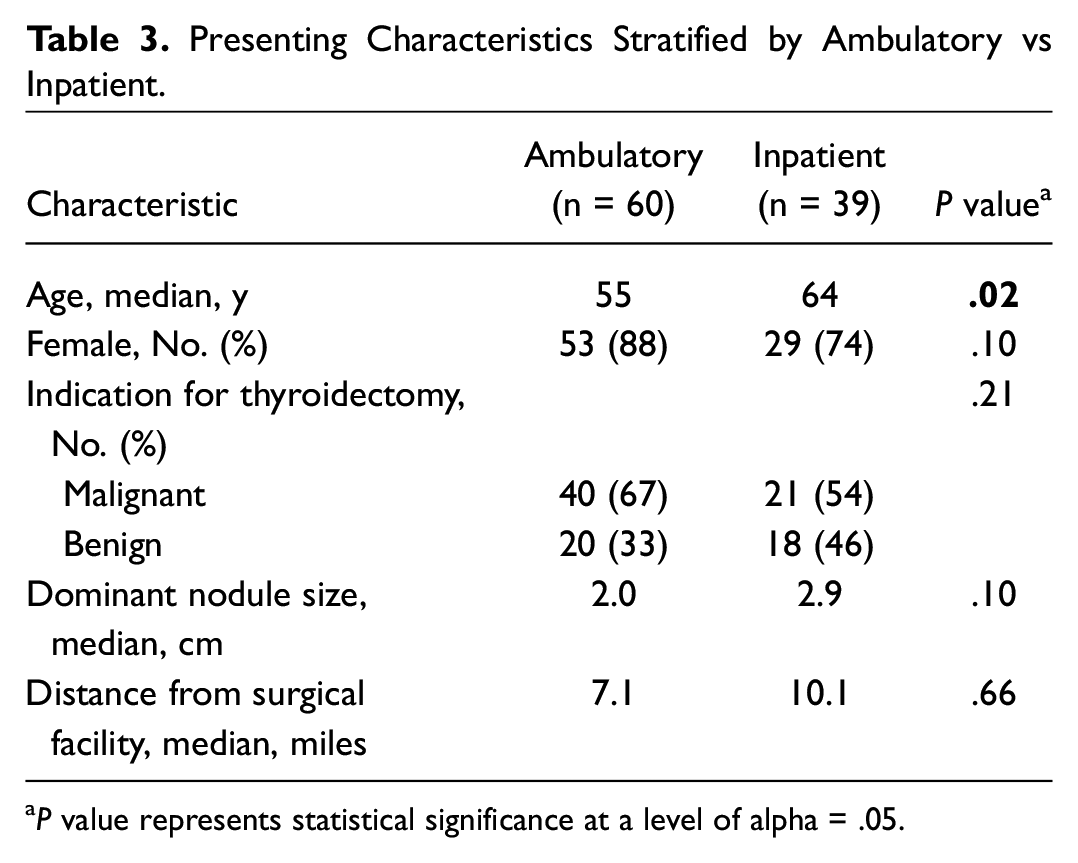
P value represents statistical significance at a level of alpha = .05.
Five patients planned for ambulatory surgery were admitted for unexpected reasons. Three patients had slow recovery from anesthesia, along with nausea and vomiting, and 2 patients had unplanned drain placement due to difficult dissection and excessive bleeding.
All surgeries were total thyroidectomies, except for 2 cases of subtotal thyroidectomy, in which residual thyroid tissue was left to preserve thyroid function in patients with benign disease ( Table 4 ). In 14 of 66 (21%) ambulatory patients and 7 of 33 (21%) inpatients, the total thyroidectomy was performed as a completion surgery; these are grouped with total thyroidectomy due to similar complication profile, specifically the risk of hypocalcemia. One patient had preexisting vocal cord paralysis on the contralateral (previously operated) side. A lateral neck dissection was performed concurrently with thyroid surgery in 8 (24%) inpatients.
Operative Characteristics Stratified by Ambulatory vs Inpatient.
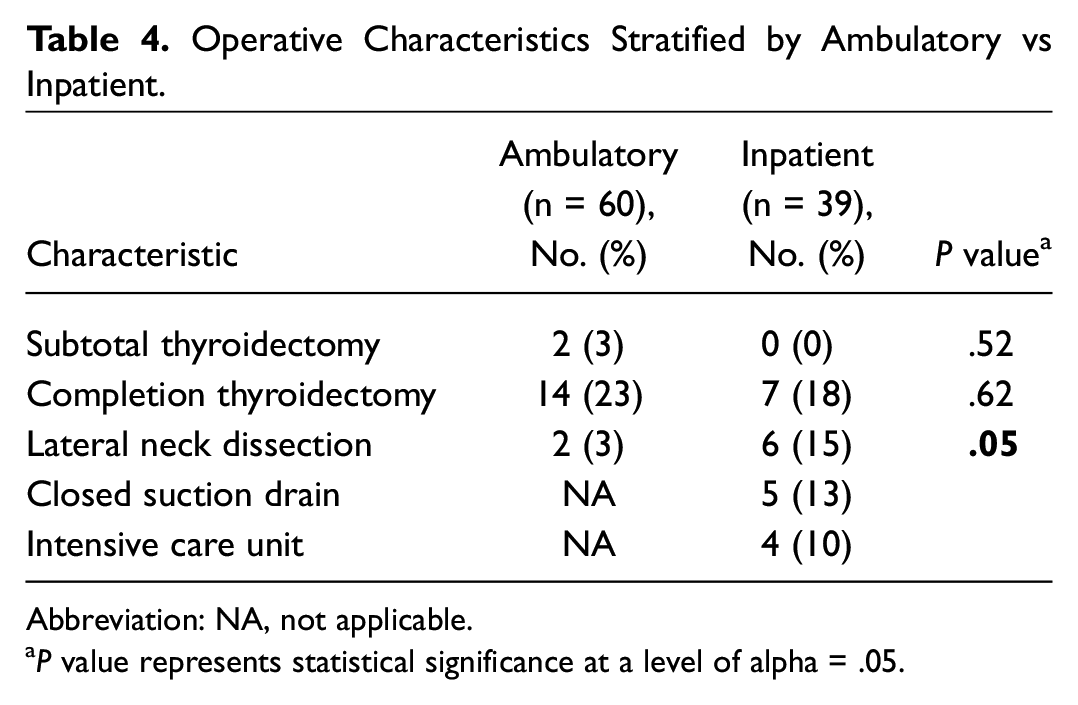
Abbreviation: NA, not applicable.
P value represents statistical significance at a level of alpha = .05.
No significant differences were found in rate of complications between the ambulatory and inpatient cohorts. Only 2 of 99 patients were readmitted after discharge ( Table 5 ). One patient from the ambulatory cohort required readmission on postoperative day 0, 8 hours after discharge due to significant anxiety and pain control issues at home. She was subsequently discharged after 23-hour observation. The second patient, from the inpatient cohort, was admitted on postoperative day 3 due to dehydration and chest pain, with negative cardiac workup, and was subsequently discharged after 2 days.
Postoperative Course in Ambulatory vs Inpatient Subjects. a
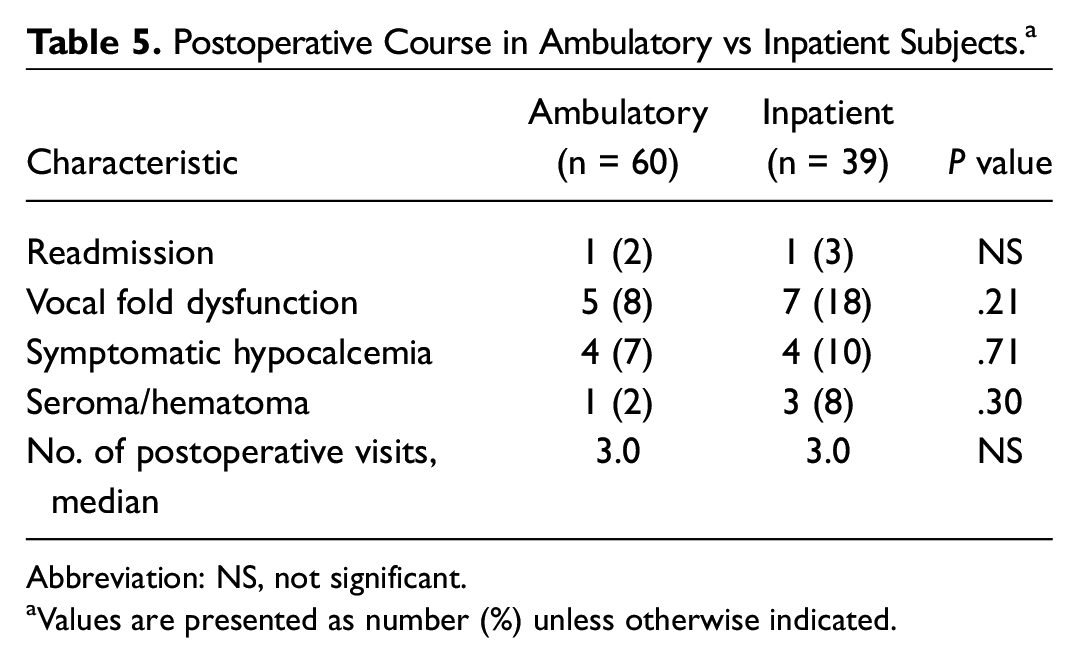
Abbreviation: NS, not significant.
Values are presented as number (%) unless otherwise indicated.
In both of our cohorts, we did not encounter any case of hematoma requiring decompression or drainage. There were 4 instances of postoperative seroma; 1 occurred in the ambulatory cohort and required aspiration in the office on postoperative day 3. Three such instances occurred in the inpatient cohort, between postoperative days 7 and 10, treated with needle aspiration in the office.
Of the recorded complications, vocal fold dysfunction was most common. On first follow-up visit, 5 of 66 (8%) patients in the ambulatory cohort complained of weak voice. In 4 patients, the dysfunction resolved on its own with full mobility of vocal cords documented at the 6-week postoperative visit by fiber-optic examination. One patient in the ambulatory cohort required voice therapy with complete return to normal voice quality and partial recovery of vocal cord mobility.
In the admission cohort, 7 of 33 (21%) patients had vocal cord dysfunction. This included 2 patients with malignancy with extensive bilateral nodal disease requiring unilateral recurrent laryngeal nerve sacrifice. Both these patients had elective tracheostomy placement for airway protection, as the contralateral recurrent laryngeal nerve had poor stimulation at the end of the case. Both were able to decannulated in <3 months. Another patient with malignancy had permanent vocal cord weakness at 3 months and underwent injection medialization. Four patients had hoarseness but good vocal fold mobility. One such patient required voice therapy, while the other 3 patients improved with time.
Symptomatic hypocalcemia with documented drop in PTH and calcium levels was observed in 4 of 66 (6%) ambulatory patients and 4 of 33 (12%) inpatients. This was managed on an outpatient basis with oral calcium supplemented with Rocalcitrol (Validus Pharmaceuticals) in all but 1 (from the inpatient cohort), who required intravenous calcium. Two patients, both from the admission cohort, developed permanent hypocalcemia requiring long-term oral calcium and Rocalcitrol treatment.
We analyzed data from the Healthcare Utilization Database for the states of Florida and New York between 2015 and 2016, during which time 12,755 total thyroidectomies were performed as day surgeries ( Table 6 ). In total, 2% (278/12755) derived from rural settings, 41% (5203/12,755) from urban nonteaching settings, and 57% (7274/12,755) from urban teaching settings. There were no instances of vocal fold paralysis in the rural settings; odds ratio (OR) for urban nonteaching was 7.36 (95% CI, 4.85-11.18; P < .001) vs 5.96 for urban teaching (95% CI, 3.95-8.99; P < .001). For postoperative hematoma/seroma, there was a significantly higher odds ratio in the rural setting (OR, 4.39; 95% CI, 1.73-11.12; P = .002) vs urban nonteaching (OR, 0.82; 95% CI, 0.53-1.27; P = .38) and urban teaching settings (OR, 0.742; 95% CI, 0.49-1.13; P = .17). Finally, for hypoparathyroidism, there were no recorded instances in the rural setting, but a higher odds ratio was seen for urban nonteaching (OR, 11.43; 95% CI, 6.12-21.31; P < .001) as compared to urban teaching (OR, 2.87; 95% CI, 1.34-6.14; P = .007).
Odds Ratios (95% CIs) for Postoperative Complications Among Rural, Urban Nonteaching, and Urban Teaching Sites in the Healthcare Utilization Database for Florida and New York Between 2015 and 2016.a
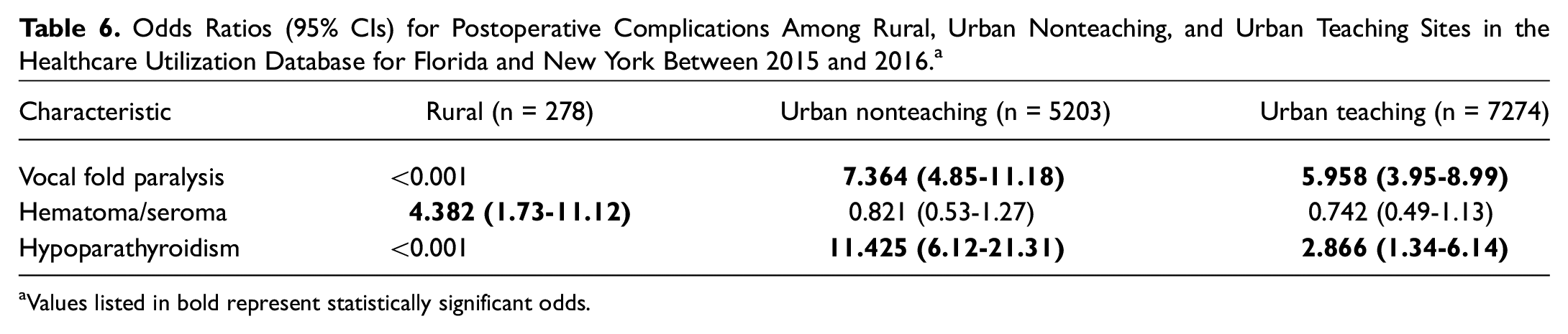
Values listed in bold represent statistically significant odds.
Discussion
Total thyroidectomy is performed at increasing rates by otolaryngologists, with the majority of the procedures taking place in the community setting. In this retrospective review, we analyze the results of 1 community thyroid surgeon as a representative sample of such practices. Two-thirds (66/99) of such total thyroidectomies done over a 6-year period were assigned to the ambulatory cohort based on criteria outlined in the ATA statement. 2
We compared the demographic data, surgical indications, and outcomes. The ambulatory cohort was younger (median age 55 vs 64 years) and had a higher proportion of female patients, consistent with well-described trends of more aggressive pathology and higher morbidity and mortality of thyroid cancer diagnosed in men.25,26 The older the patient, the greater likelihood of comorbid medical conditions necessitating admission; the more advanced the pathology, the greater the likelihood of lateral neck dissection requiring a drain and subsequent admission, as well as assignment to the admissions group. Although the ambulatory group had a higher proportion of malignant pathology, the malignant nodules were on average smaller than those operated on in the inpatient group. Larger goiters with pressure symptoms and substernal extension, as well as goiters with Graves’ and Hashimoto’s disease, were assigned to the admission group.
Our ambulatory cohort patients lived closer to the surgical facility (average 7.1 vs 10.1 miles) as compared to the admission cohort. For both cohorts, however, the median distance to the hospital was 8.2 miles. This highlights an important safety advantage of community practice compared to tertiary care (ie, the ability to serve patients close to home and quick access to the surgical facility in case of an adverse event). It also enables patients to be seen more frequently in postoperative follow-up, making close monitoring easier. The senior author operates at surgical facilities in 5 different towns, and most of the population served by these surgical facility lives within 5 miles, while the closest tertiary care center is more than 25 miles away for most of the population.
Completion thyroidectomies were grouped with total thyroidectomies for this study as they have similar postoperative concerns, specifically the risk of hypocalcemia. Completion thyroidectomy represented 21% (21/99) of the volume of total thyroidectomies performed in this time period; two-thirds of completion cases (14/21) were managed on an outpatient basis. Some studies have reported higher rates of postsurgical complications after completion thyroidectomy vs primary operations. 27 While we did observe a higher complication rate in completion vs primary cases (33% vs 23%), most (12/14) of these cases were completed on an ambulatory basis, with a conversion rate of 2 of 14. Others have reported safe same-day discharge after completion thyroidectomy. 28
Vocal fold dysfunction was the most common surgical complication seen overall among our 99 thyroidectomy patients. In total, we observed 12 cases (12%) of any sort of dysfunction; most (9/12) were transient and resolved with time (7/9) or voice therapy (2/9). Three of 99 (3%) represented true unilateral vocal fold paralysis, 1 of which required additional surgical procedures. Others have reported a temporary paresis/paralysis rate of 5.2% and a permanent paresis/paralysis rate of 1.4%. 29 Our rate of transient vocal fold paresis may be higher than reported in academic literature owing to our preference for close postoperative follow-up with early flexible laryngoscopy on the first postoperative visit. The rate of vocal fold dysfunction was higher in the inpatient cohort. This is expected given the higher surgical complexity in patients with more advanced disease in the admission cohort. Similar findings were reported in a recent meta-analysis comparing ambulatory to inpatient thyroidectomies, noting over a 2-fold increase in risk of transient injury to the recurrent laryngeal nerve among inpatients. 30
Hypocalcemia is a well-known adverse event after thyroid surgery, and many measures have been described to prevent and treat this. A recent Cochrane review demonstrated that such management is not standardized, and high-quality evidence for treatment of postthyroidectomy hypocalcemia is lacking. 31 Our practice is to prescribe prophylactic calcium supplementation to all patients undergoing total thyroidectomy, regardless of planned admission or not. The rate of hypocalcemia was higher among inpatients (10%) than ambulatory patients (7%), although this was not a statistically significant difference in this small study. Importantly, the 4 ambulatory surgery patients who did develop symptomatic hypocalcemia did not require admission and were managed on an outpatient basis. Such care is enhanced by a close working relationship between otolaryngology and endocrinology in the community. It was also noted in meta-analysis that inpatients had an increased risk of transient hypocalcemia after inpatient surgery compared to outpatients. 30 This finding, in combination with reported increased risk of transient vocal fold paresis among inpatients, surely reflects increased surgical complexity of such cases.
The most life-threatening complication after thyroid surgery is neck hematoma, which in some studies has been shown to occur between 6 and 24 hours after sugery. 32 We did not have any incidence of early hematoma in either group. Our ambulatory patients are observed for 4 hours and discharged home, only after ensuring the absence of any collection in the neck. Four patients developed postoperative seroma that required needle aspiration in the office.
Using rural and urban nonteaching sites as a proxy for community practice, we found that ambulatory total thyroidectomy is performed nearly as frequently in the community as it is at urban teaching sites. The data do show higher odds of postoperative complication in nonteaching sites: with a higher incidence of vocal fold paralysis and hypoparathyroidism in urban nonteaching sites, as well as a higher incidence of hematoma/seroma in rural sites. We believe that the site is not a surrogate for quality, and the surgery performed by an experienced surgeon with strict adherence to guidelines can result in safe ambulatory total thyroidectomy in a community setting.
Limitations of this study include the retrospective nature of review and limited sample size. However, we feel that these data, derived from a community practice, provide an important contribution to the literature, as most of these procedures are performed in this setting.
While our review of the Healthcare Utilization Database provides some useful information, we found these data to be limited, as the information for the database is gathered from same-day discharge summaries. This analysis therefore fails to capture the complete postoperative course.
Conclusion
Total thyroidectomy in carefully selected cases is safe as an ambulatory procedure in the community setting, and strict adherence to the guidelines and procedures results in low complication rates. Geographic proximity of the surgical facility to patient’s home should further enhance the safety in the community setting.
Author Contributions
Disclosures
Footnotes
This article was presented at the AAO-HNSF 2019 Annual Meeting & OTO Experience; September 15-18, 2019; New Orleans, Louisiana.
