Abstract

Keywords
Branchial cleft anomalies (BCAs) are a key diagnostic consideration in the evaluation of pediatric neck masses but uncommonly diagnosed in adult patients. 1 BCAs result from incomplete obliteration of embryologically derived branchial clefts or pouches and are named from the derivative cleft or pouch and the degree of obliteration.
Most BCAs are related to the second branchial arch, while lesions of the fourth branchial arch are most rare (1%-4% of branchial anomalies).1-3 Fourth BCAs are located adjacent to the thyroid gland, with an opening in the piriform sinus apex, and they often present with recalcitrant lower neck and/or chest infections. The infrequent incidence of fourth BCAs presents challenges in diagnosis and management.2,4 Here, we describe a case of a fourth BCA identified in an adult patient and managed with transoral robotic surgery.
Case Report
Presentation
This study is classified as exempt by the Massachusetts Eye and Ear Institutional Review Board. A 54-year-old woman presented to the head and neck surgery clinic for evaluation of antibiotic-refractory recurrent neck tenderness and odynophagia spanning several months. Her examination was notable for left anterior neck fullness with tenderness to palpation around the left thyroid lobe. Fiberoptic laryngoscopy findings were normal, as were neck ultrasound and thyroid function testing results. Subsequent neck computed tomography scan demonstrated abnormal soft tissue thickening and edema of the left piriform sinus extending anteriorly to the left thyroid lobe. Barium swallow revealed a thin, inferiorly directed tract arising from the left piriform sinus consistent with a fourth BCA ( Figure 1A ). The patient was counseled regarding a minimally invasive transoral approach with robotic assistance to identify and obliterate the tract without thyroid lobectomy.
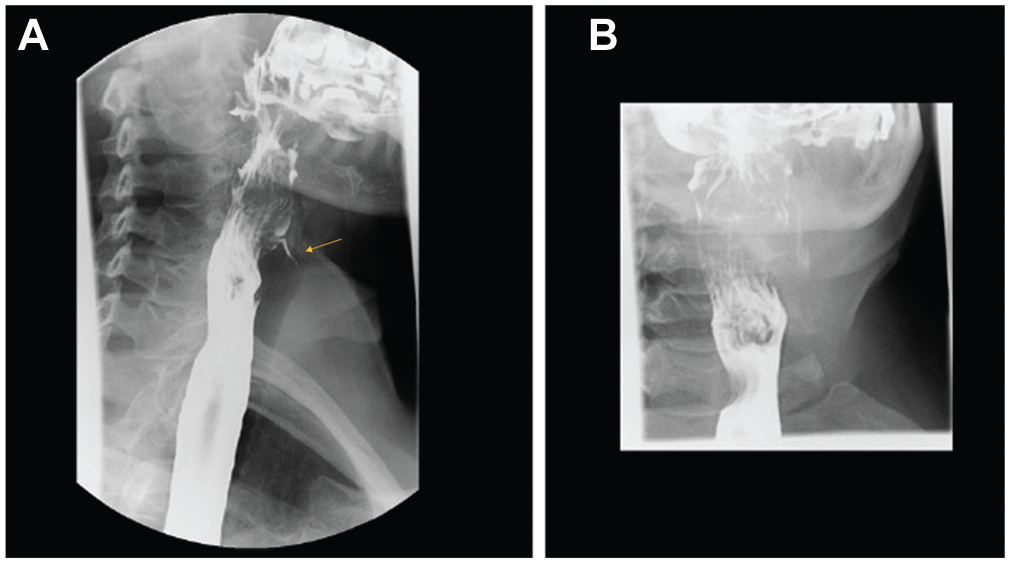
Modified barium swallow (A) before and (B) after transoral robotic cauterization of the fourth branchial cleft tract. Note the resolution of the thin inferiorly directed tract arising from the left piriform sinus, which resolved postprocedure (arrow).
Operative Intervention and Recovery
Following informed consent, the patient was brought to the operating room, positioned supine, and orotracheally intubated. The larynx was suspended with the flex retractor (Medrobotics Inc, Raynham, MA) with an endolaryngeal blade to gain access to the left piriform sinus. The da Vinci robot (Intuitive Surgical, Inc, Sunnyvale, CA) was docked with a 30° upgoing camera, and a Maryland dissector and monopolar electrocautery were advanced into the hypopharynx. The larynx was gently distracted to the right and the lateral piriform sinus mucosa distracted to the left, revealing a small tract at the piriform sinus apex ( Figure 2A ). Surrounding mucosa was cauterized with a silver nitrate stick advanced on the Maryland dissector ( Figure 2B ). The tract aperture was widened with monopolar electrocautery ( Figure 2C ), resulting in egress of purulent material. The entire length of the visible tract was then cauterized with silver nitrate. No obvious extension into neck was visualized. The surrounding mucosa of the tract was again cauterized with suction electrocautery by the bedside assistant. The area was copiously irrigated with saline, and the patient returned to anesthesia for emergence.
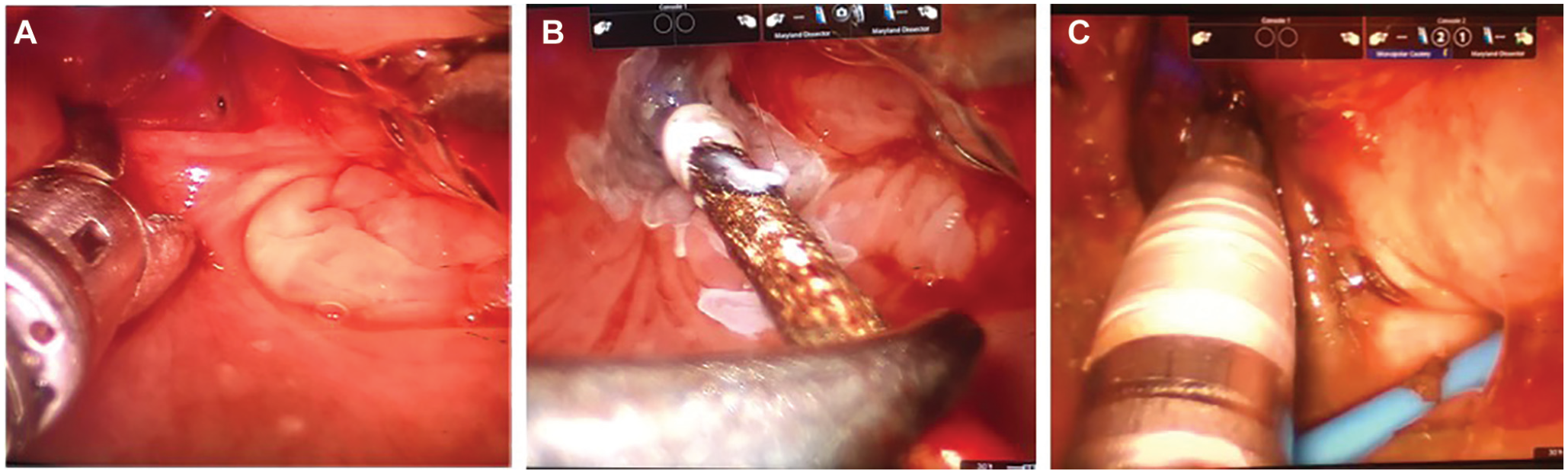
Robotic cauterization procedure. Operative exposure of the tract at the apex of the piriform sinus with (A) laryngeal distraction and (B) mucosal cauterization with silver nitrate. (C) Monopolar electrocautery is advanced into the tract opening, with cauterization of the entire length of the visible tract.
The patient had no immediate surgical complications during overnight observation. She had complete resolution of neck swelling and discomfort without any dysphagia. Repeat barium swallow performed 2 months postprocedure was without evidence of linear extravasation along the piriform sinus, consistent with surgical repair of a fourth BCA ( Figure 1B ). The patient continues to be asymptomatic 20 months postprocedure.
Discussion
In this case, we describe the identification of a fourth BCA in an adult patient successfully treated with a minimally invasive TORS obliteration procedure. Given the rarity of fourth BCAs, high clinical suspicion combined with appropriate diagnostic testing (barium swallow) was required for appropriate diagnosis and treatment. In this patient, the location of the fourth BCA, adjacent to the thyroid gland and within an opening in the apex of the piriform sinus, was consistent with known embryologic relationships and critical in the identification and management of this rare clinical entity.
A lack of consensus exists regarding optimal management of fourth BCAs; options include incision and drainage, open tract excision with repair, endoscopic cauterization, and open repair with partial thyroidectomy. 5 To our knowledge, this represents the first case of a fourth BCA managed with TORS endoscopic cauterization. Unlike endoscopic cauterization with microsuspension laryngoscopy, 3 the robotic procedure does not require balloon dilation of the sinus tract and allows for a stable intubated airway for the duration of procedure. Three-dimensional visualization is excellent, allowing for definitive identification and management of the sinus tract with bimanual instrumentation. We believe that the popularity of this technique will increase with growing access to robotic instrumentation.
