Abstract
Objectives
To determine if a Canadian voice center is meeting the recommended time to laryngoscopy for hoarseness per the clinical practice guideline of the American Academy of Otolaryngology–Head and Neck Surgery.
Study Design
Retrospective chart audit.
Setting
Tertiary referral Canadian voice center.
Participants and Methods
A total of 149 adult patients presenting with hoarseness over 6 months were included. Primary outcome measures were the time from onset of symptoms to laryngoscopy and the time from referral to laryngoscopy. Secondary outcome measures included patient- and disease-modifying factors, diagnosis, and clinical management. Analysis was performed to determine what factors were associated with meeting the guideline.
Results
Patients were evaluated by the laryngologist after 21.9 ± 37.6 months (mean ± SD) of symptoms. One-third (34.2%) of patients were seen within 3 months; 10.7% were seen within 4 weeks. Logistic regression showed that patients with neurologic symptoms (odds ratio, 4.04; 95% CI, 1.31-12.43;
Conclusion
It is an ongoing challenge for our Canadian voice center to meet the American Academy of Otolaryngology–Head and Neck Surgery’s clinical practice guideline for recommended time to laryngoscopy. Patients with more severe pathologies were consistently triaged more urgently. It is debatable whether this 4-week time recommendation is generalizable to a socialized health care system.
Hoarseness is a symptom that can have a significant impact on quality of life. Nearly one-third of the population will experience a voice disorder, yet only 5.9% will seek medical attention.1,2 The presentation of hoarseness can be challenging, as it is a symptom, not a diagnosis, and cannot be appropriately treated without a diagnosis. Laryngeal visualization is essential for diagnosis of the patient with dysphonia, and many physicians (primary care providers [PCPs], emergency room physicians, pulmonologists, and/or gastroenterologists) managing this symptom do not have the ability to perform laryngoscopy.3,4 Fortunately, symptoms rarely last >4 weeks, with most being caused by reversible pathologies (eg, acute laryngitis). 1 A small percentage (1%-3%), however, will have persistent symptoms secondary to more serious pathology.1,5 Glottic malignancies and vocal cord immobility present symptomatically early in their disease courses, yet both require prompt specialist evaluation and diagnosis. Failure of early recognition and direct laryngeal evaluation has an effect on quality of life and, more important, patient survival; therefore, guidelines were developed to streamline the recognition of serious pathology and expedite time to specialist assessment. 3
The American Academy of Otolaryngology–Head and Neck Surgery (AAO-HNS) recently released the updated clinical practice guideline (CPG) for hoarseness (dysphonia). This guideline consists of 13 evidence-based statements guiding the recognition, assessment, and management of dysphonia and was updated from the previous 2009 guideline.1,6 Notable changes from previous include a focus on rapid escalation of care (from PCPs to specialists) of the patient who is hoarse and a reduction in the time interval of symptom presentation to laryngoscopy (3 months reduced to 4 weeks).1,6 Continued recommendations of recognizing malignancy risk factors, the importance of subpopulations of voice users, prudent prescribing of medical therapy, as well as voice therapy options are also stressed. 1
Implementation of this CPG has been designed for a private-pay American health care system. However, the AAO-HNS CPG was meant to target otolaryngologists, PCPs, and any physician who may encounter a patient who is hoarse, stretching beyond the United States. Canada’s publicly funded single-payer universal health care system has a different delivery of health care, resulting in altered patient expectations with wait times and referral patterns. Most notably, Canadian patients are obligated to see a primary care physician first, and they require a referral to see a specialist. Presumably, this extra step creates a challenge for the otolaryngologist to meet the 4-week guideline. The aim of this study was to evaluate the feasibility of the CPG at our Canadian academic institution, focusing on the recommended time to laryngoscopy (statement 4B).
Materials and Methods
After consultation with the Institutional Research Ethics Board (University of British Columbia), this quality assurance project was deemed exempt. A retrospective chart audit was conducted that identified patients aged ≥18 years presenting over a 6-month period with the chief complaint of hoarseness or dysphonia. Patients were excluded if they were referred by another otolaryngologist with the assumption that these patients had already undergone laryngoscopy. All charts were reviewed by a single researcher. Demographic information, Voice Handicap Index–10 scores, diagnosis, previous management, and current clinical management were compiled. Patients’ presenting symptoms and risk factors were recorded, such as recent surgery or endotracheal intubation, previous head and neck radiation, smoking status, alcohol consumption, and professional voice user. Primary outcome measures were the time from onset of symptoms (ie, hoarseness) to laryngoscopy and the time from referral to laryngoscopy. Secondary outcome measures included patient- and disease-modifying factors, diagnosis, and clinical management.
Statistical analysis was performed with commercially available software (SPSS [v 25; IBM] and Microsoft Excel). Descriptive statistics were calculated for the 2 main outcome measures: duration of symptoms and referral time. The data were divided into 2 time points: ≤3 months (for meeting the old guideline) or ≤4 weeks or 1 month (for the meeting the updated guideline). In univariate analysis, Student’s unpaired
Results
Charts of 149 patients were reviewed. Demographic data of the study population are presented in Table 1 . Patients were seen by the Pacific Voice Clinic’s laryngologist 21.9 ± 37.6 months (mean ± SD) after onset of symptoms and 1.9 ± 1.7 months from time of referral.
Demographic Data for the Study Population (N = 149)
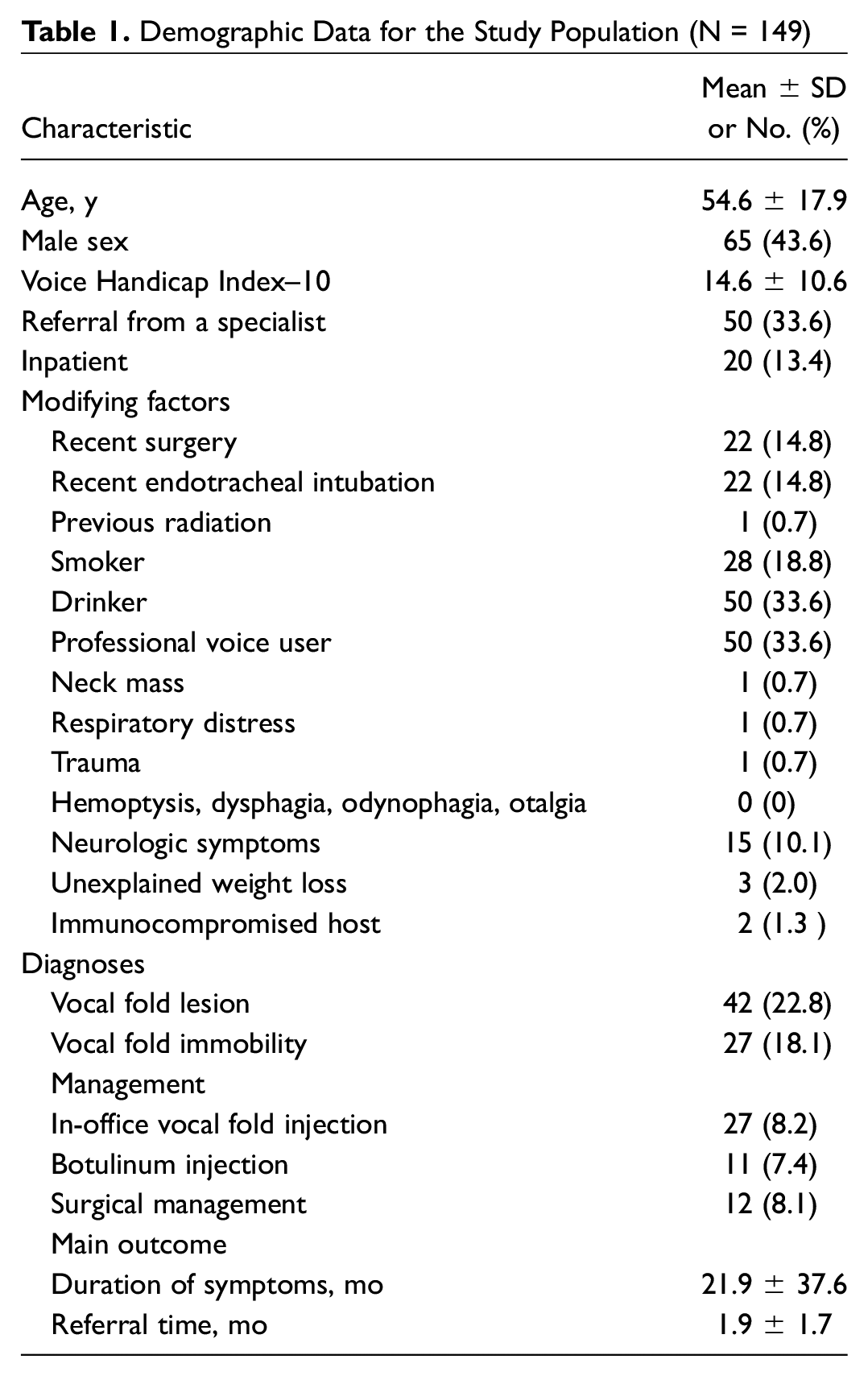

For the first main outcome measure of duration of symptoms, about a quarter of patients (34.2%, n = 51) were seen within 3 months, thus meeting the old guideline. About 10.7% (16 patients) were seen within 1 month of symptom onset (4 weeks), thus meeting the updated guideline. In univariate analysis (
Table 2
), similar variables were associated with meeting the 4-week and 3-month guidelines (respectively): recent surgery (
Univariate Analysis of Patients Seen Within 4 Weeks and 3 Months of Symptom Onset. a
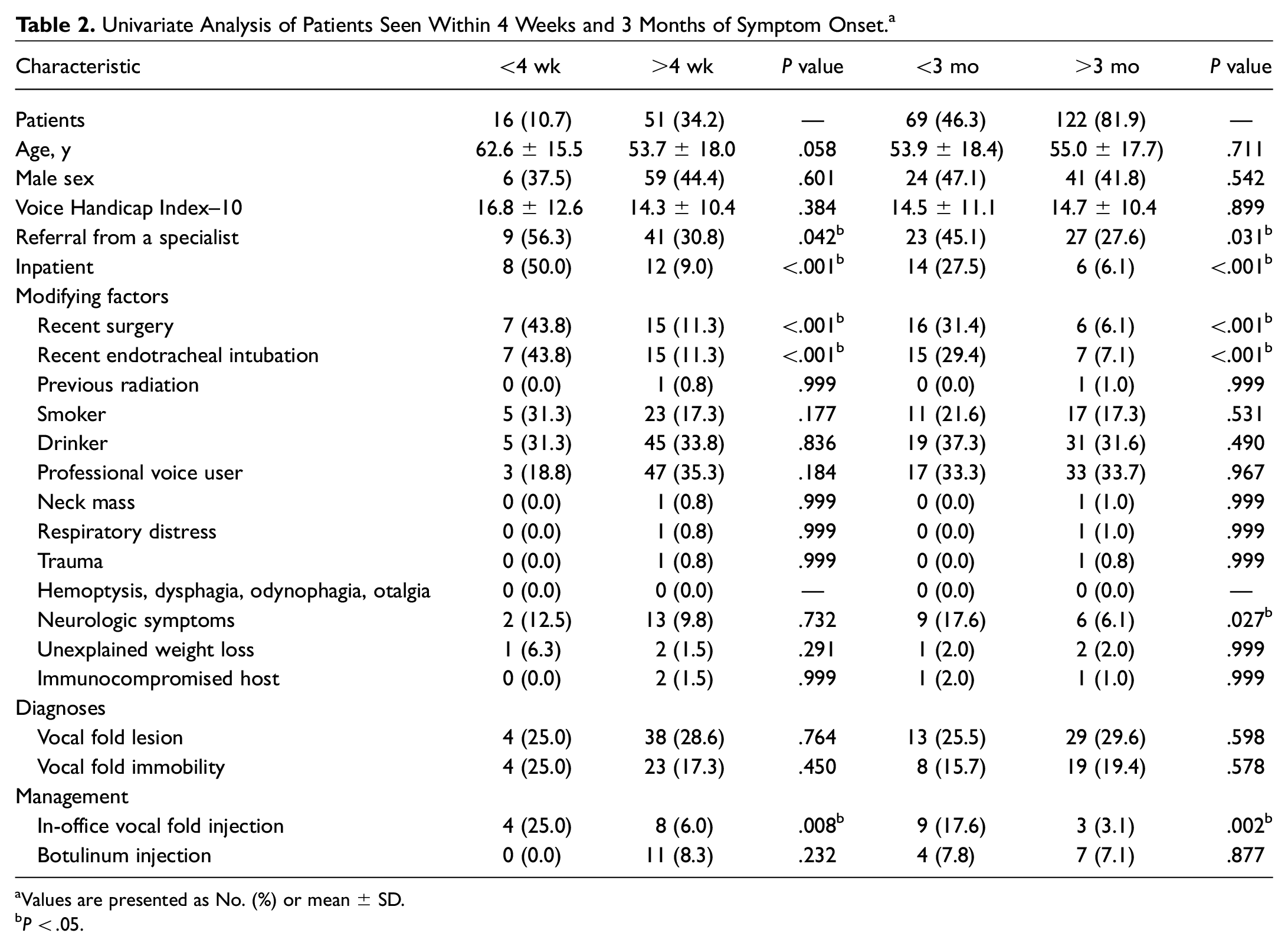
Values are presented as No. (%) or mean ± SD.
For the second main outcome measure of referral time, 81.9% of patients (n = 122) were seen within 3 months and 46.3% (n = 69) within 4 weeks. Univariate analysis showed the following variables being associated with being seen within 4 weeks: recent surgery (
Univariate Analysis of Patients Seen Within 4 Weeks and 3 Months of Referral. a
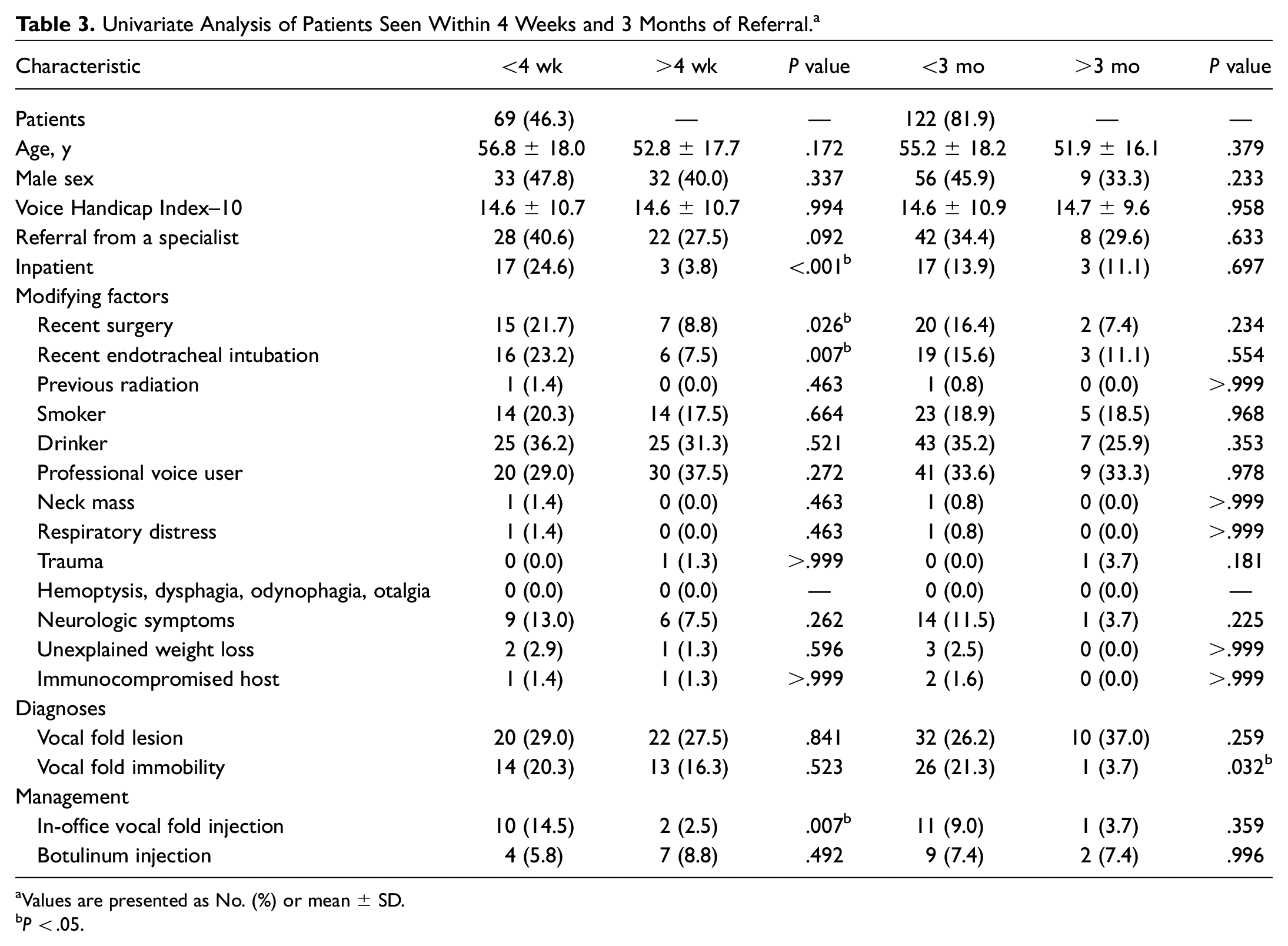
Values are presented as No. (%) or mean ± SD.
Logistic regression for the 2 main outcome measures (duration of symptoms and referral time) and the 2 time frames (3 months and 1 month or 4 weeks) is displayed in
Table 4
. For the 4-week symptom time frame, patients who had recent intubation had an odds ratio of 6.04 (95% CI, 1.99-18.34;
Logistical Regression Model of Duration of Symptoms and Referral Time.
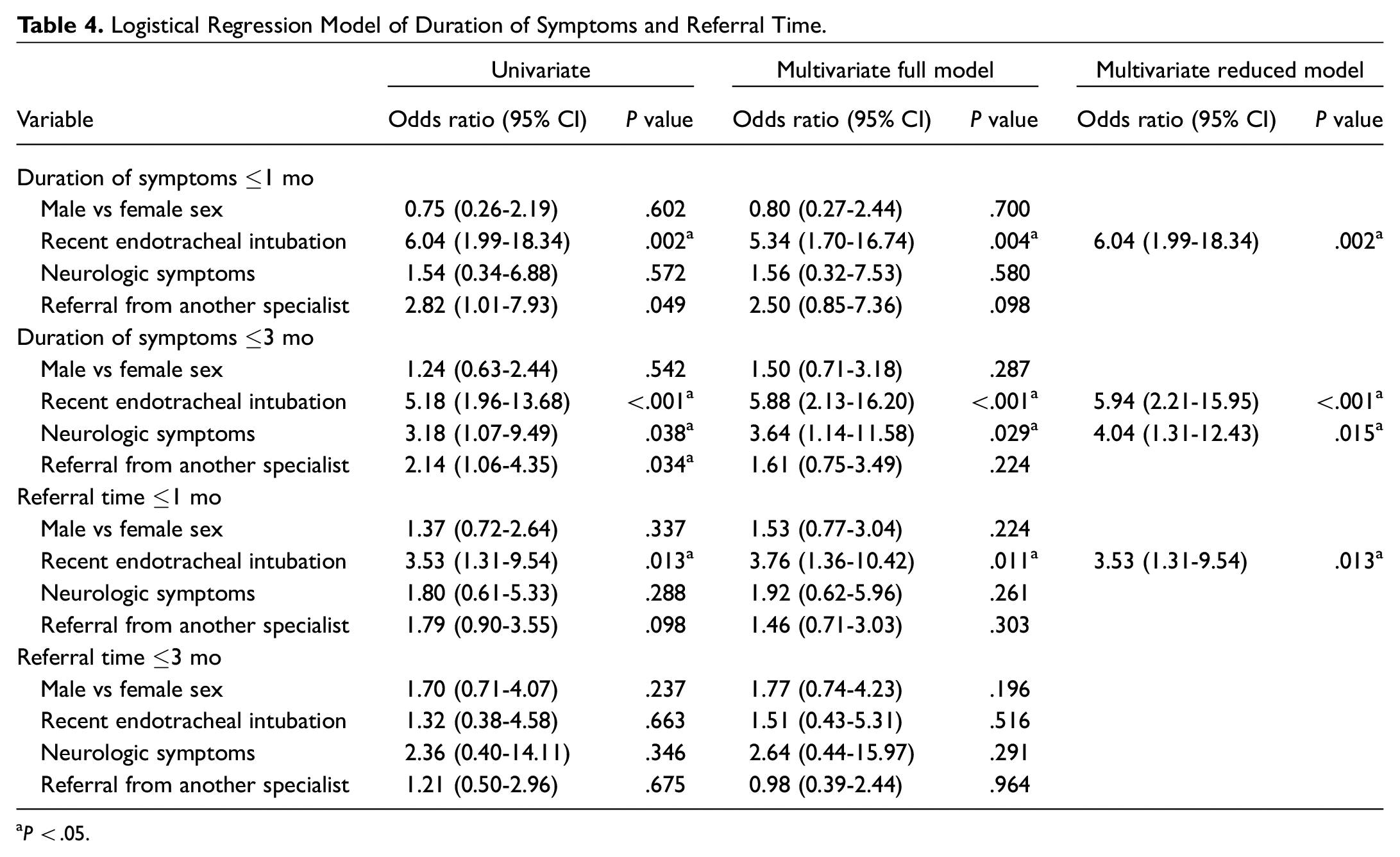
Discussion
The AAO-HNS CPG on hoarseness was developed through comprehensive literature review by experts in the field and endorsed by several American medical organizations. However, this guideline was created in a private-pay medical system. In the United States, although a large number of patients seek primary care initially, >70% of patients referred from primary care will be evaluated by an otolaryngologist within 4 weeks’ time, whereas almost 30% of self-referral patients will not be seen within 3 months. 7 Conversely, in Canada, all patients must first visit their PCPs before receiving a referral to specialist care, delaying time to laryngoscopy.
As defined by the Institute of Medicine, CPGs are “statements that include recommendations intended to optimize patient care that are informed by a systematic review of evidence and an assessment of the benefits and harms of alternative care options.” 8 Guidelines are one way of increasing implementation of evidence into practice. They can serve as a guide to best practices, a framework for clinical decision making, and a benchmark for evaluating performance. This CPG was based on the symptom of “hoarseness,” while the majority of the AAO-HNS CPGs are based on clinical disorders (eg, benign paroxysmal positional vertigo, adult sinusitis, Bell’s palsy). Hoarseness is present in a broad range of conditions, ranging from benign self-limiting diagnoses (eg, acute laryngitis) to life-threatening conditions (eg, laryngeal malignancy). 9 Failure of early recognition and direct laryngeal evaluation has a direct effect on quality-of-life measures and, more important, patient survival; therefore, the CPG aims to streamline the recognition of serious pathology and expedite time to specialist assessment. 10
One of the notable changes in the guidelines is the time to laryngoscopy after symptom onset (ie, 3 months decreased to 4 weeks). 1 The 3-month “safety net” was originally based on expert opinion, lacking objective evidence in the literature. 11 This may have been revised as this time frame could be interpreted as being prolonged, ultimately delaying diagnoses, and potentially increasing harm to patients with serious pathologies.9,12 The 4-week time frame was determined from recent evidence-based literature acknowledging that acute presentations need time to resolve, while also recognizing that after 4 weeks, quality-of-life measures begin to suffer.1,13 Furthermore, patients with voice disorders who are evaluated after 4 weeks incur higher health care costs. 14 Additionally, the new guideline continues to advise against the prescribing of antimicrobial, corticosteroid, and reflux therapy (recommendations 6-8) prior to direct laryngeal visualization. 1 This was noted to be inconsistently prescribed and documented in referral letters. In a recent commentary, Jotoi and Sah considered specialty bias to affect the validity of guidelines, suggesting that they generate increased referrals, lead to overdiagnosis and overtreatment, and contribute to increased health care costs. 15 However treatment of early-stage laryngeal pathology is associated with excellent outcomes, improved quality of life, and overall reduced health care expenditure, supporting the updated recommendation for early evaluation of patients with risk factors.1,6
In the current study, our Canadian voice center was not meeting the recommendation of laryngoscopy within 4 weeks of persistent hoarseness (statement 4B). This was suspected to be an area of deficiency and will continue to be an ongoing challenge for various reasons. Patients with dysphonia frequently delay presentation (88-119 days) to primary care, as they suspect that their symptoms will improve rapidly. 12 Furthermore, a recent analysis showed that nearly two-thirds of PCPs report feeling comfortable treating dysphonia for 6 weeks. 16 Although this initial management attempt may be sufficient for patients experiencing common benign etiologies, potentially serious conditions may be missed, leading to delay in diagnosis and treatment and to poorer outcomes.9,17,18 Last, patients encounter prolonged specialist wait lists, and laryngoscopy is delayed further. Only 10.7% of our patients were evaluated within the 4-week guideline and 34.2% at 3 months. However, a much higher percentage (46.3%) was seen within 4 weeks, and 81.9% were seen within 3 months from the time of referral. These findings suggest that although patients have a significant delay in presentation following symptom onset, once they receive a laryngology referral, they are evaluated in what we would consider an adequate time interval. Unfortunately, a physician can only control how quickly patients are seen once they seek medical attention.
Further examination of our results indicates that patients with more serious pathologies are being evaluated on a more urgent basis. Patients with dysphonia who had experienced endotracheal intubation or were exhibiting symptoms suggestive of a neurologic disorder were seen more urgently, suggesting that they had a diagnosis of vocal fold injury, paralysis, or dysfunction. These patients tend to be seen more urgently as they can be treated in office effectively with vocal fold injections to avoid aspiration. Similarly, inpatients or referrals from other specialists may have an associated convenience factor as the Pacific Voice Clinic is located within our academic institution. Interestingly, smoking, a known risk factor in head and neck malignancies, did not result in patients being evaluated earlier.18,19 We hypothesize that this may be due to patient reliability with smoking history, as patients have a tendency to underreport.
Only about 10% of patients with dysphonia evaluated by PCPs are eventually referred to otolaryngology. 7 A 2010 study found that the majority of PCPs are interested in learning more about voice problems, as treatment strategies are generally limited to antireflux and allergy management. 20 These physicians frequently manage hoarseness on their own before considering specialty opinion, leading to further delay in laryngoscopy. 16 For example, a recent survey of PCPs’ management of hoarseness revealed that many PCPs were willing to empirically prescribe reflux medication as primary therapy, even when gastroesophageal reflux disease symptoms were not present. 16 This practice opposes the AAO-HNS recommendations from 2009 and 2018. Interestingly, multiple studies found that 33% to 56% of patients with an initial nonspecific diagnosis of dysphonia from a PCP will have a revised final diagnosis following specialty evaluation.21,22 Most common referring diagnoses include acute laryngitis, nonspecific dysphonia, benign vocal fold lesions, and chronic laryngitis. 22 The updated guidelines recognize that gaps in knowledge exist and therefore encourage rapid escalation of care to an otolaryngologist with the technical ability and experience to visualize the larynx and arrive at definitive diagnoses.
The AAO-HNS guidelines are intended for use by AAO-HNS members and nonmembers, with the majority being located within the United States in a private-payer health care model. Outside North America, countries have adopted similar guidelines. The United Kingdom’s (NICE) suspected cancer pathway provides referral recommendations for symptoms with malignant potential. Specialist appointment within 2 weeks is recommended for patients who have persistent unexplained dysphonia and are >45 years of age or have a neck mass. 23 Rapid-access clinics have allowed for evaluation within 14 days for patients with suspected laryngeal cancer.23-25 With a health care delivery structure similar to the UK’s National Health Service, Canadian centers may benefit from a similar strategy.
We recognize that this study has some limitations. This is a single-institution study based on chart notes from a tertiary care academic laryngology practice. Included patients were evaluated during the first 6 months after the initiation of a new laryngologist’s practice, possibly lengthening the mean wait times. The type of patients assessed may differ from the population seen by a private practice otolaryngologist. The retrospective study design also introduces the possibility for recall and/or misclassification bias. Following the advice of our 2 consultant statisticians (J.S. and T.L.), since this was a hypothesis-generating pilot study, a Bonferroni correction factor was not calculated. Additionally, dichotomizing variables decreases the sensitivity in the data.
Conclusion
The recently updated AAO-HNS’s CPG on hoarseness continues to advocate for prudent diagnosis and management, while placing a new emphasis on rapid escalation of care to specialist evaluation within 4 weeks of symptom onset. We conducted a quality assurance investigation to evaluate if our Canadian voice center was able to meet this updated guideline’s recommended time to laryngoscopy, which was designed to be implemented in a private-pay health care system. Our results suggest the potential difficulty in the generalizability and application of the guideline to different economic models of health care delivery. Patients with more severe pathologies (eg, neurologic or postintubation dysphonia) were consistently seen more urgently; however, the minority of patients (10.7%) were evaluated within the revised 4-week recommendation. Challenges include prolonged time course for patients who delay seeking medical attention, delay in referral, and lengthy laryngology wait lists. Given these results, we recognize that only 2 of these 3 factors are within our control. The CPG is meant to be an educational resource for any physician who may manage dysphonia. Further PCP education, awareness of the updated guideline, and the creation of rapid-access laryngology clinics may be steps toward reducing wait times. This clinical audit will help our center to triage referrals more effectively and, more important, bring attention to the varied health delivery systems and access to specialist health care outside the United States.
Author Contributions
Disclosures
Footnotes
This article was presented at the AAO-HNS Annual Meeting, October 7-10, 2018; Atlanta, Georgia; and the Canadian Society of Otolaryngology–Head and Neck Surgery Annual Meeting; June 14, 2019; Edmonton, Canada.
