Abstract
Objective
Treatment delays and suboptimal adherence to posttreatment surveillance may adversely affect head and neck cancer (HNC) outcomes. Such challenges can be exacerbated in safety-net settings that struggle with limited resources and serve a disproportionate number of patients vulnerable to gaps in care. This study aims to characterize treatment delays and adherence with posttreatment surveillance in HNC care at an urban tertiary care public hospital in San Francisco.
Study Design
Retrospective chart review.
Setting
Urban tertiary care public hospital in San Francisco.
Subjects and Methods
We identified all cases of HNC diagnosed from 2008 to 2010 through the electronic medical record. We abstracted data, including patient characteristics, disease characteristics, pathology and radiology findings, treatment details, posttreatment follow-up, and clinical outcomes.
Results
We included 64 patients. Median time from diagnosis to treatment initiation (DTI) was 57 days for all patients, 54 days for patients undergoing surgery only, 49 days for patients undergoing surgery followed by adjuvant radiation ± chemotherapy, 65 days for patients undergoing definitive radiation ± chemotherapy, and 29 days for patients undergoing neoadjuvant chemotherapy followed by radiation or chemoradiation. Overall, 69% of patients completed recommended treatment. Forty-two of 61 (69%) patients demonstrated adherence to posttreatment visits in year 1; this fell to 14 out of 30 patients (47%) by year 5.
Conclusion
DTI was persistently prolonged in this study compared with prior studies in other public hospital settings. Adherence to posttreatment surveillance was suboptimal and continued to decline as the surveillance period progressed.
Keywords
Despite significant advancements in diagnosis and treatment in recent years, the prognosis of head and neck cancer (HNC) remains poor, with an overall 5-year survival rate of 56% in whites and 34% in African Americans. 1 Early detection of symptoms and initiation of therapy, as well as careful posttreatment surveillance, have been shown to be vital for achieving optimal outcomes. Therefore, close monitoring of patients to reduce treatment delay and optimize adherence to posttreatment surveillance is an important aspect of HNC care.
Racial, ethnic, and income disparities in head and neck cancer outcomes exist and may be mitigated by close monitoring both during and after treatment. For example, a 2009 study by Gourin and Podolsky 2 investigated racial disparities between black and white patients with HNC at a single large institution in the South and found that black patients had significantly shorter follow-up periods compared to whites. Close monitoring in the treatment and posttreatment periods may help decrease loss to follow-up in such vulnerable populations. Monitoring may also play an important role in reducing delays and increasing patient adherence to radiation therapy. A 2017 study by Thomas et al 3 showed that low-income patients experienced disproportionately increased radiation treatment interruptions compared to patients insured by commercial carriers or Medicare.
We chose to study treatment delays and adherence to posttreatment surveillance in an urban safety-net hospital in San Francisco that serves a disproportionate number of racial and ethnic minorities and low-income patients. An understanding of these gaps will help delineate a potential role for a health information technology tool aimed at improving treatment planning and monitoring of patients with HNC in safety-net settings.
Methods
Population
We initiated this retrospective chart review as a readily accessible, rich source of existing data to document where gaps in care or loss to follow-up occur in HNC within an urban safety-net hospital in San Francisco. The UCSF Human Research Protection Program Institutional Review Board approved this retrospective review of patient data and waived the requirement for informed consent (#12-09658).
We identified all cases (n = 64) of biopsy-proven HNC between 2008 and 2010 from the electronic medical record. We excluded patients from this study if they presented with distant metastasis, were recommended palliative treatment as an initial treatment plan, or had no notes in the electronic medical record documenting a clinical encounter in the otolaryngology clinic.
Data Collection
Using REDCap, we created a measurement tool with structured fields for data abstraction. Five researchers were trained to ensure consistent coding through review of the variables, protocol, and data abstraction form. At least 2 researchers abstracted each patient record, and whenever present, discrepancies were noted and discussed to ensure agreement between abstractors. Data abstraction consisted of patient characteristics, disease characteristics, pathology and radiology findings, treatment details, posttreatment follow-up, and clinical outcomes including survival, recurrence, and development of a second primary tumor. Researchers consulted the National Center for Health Statistics’ National Death Index to supplement mortality data for patients no longer seen at this hospital.
Data Analysis
We used descriptive statistics to report patient and disease characteristics, treatment details, surveillance outcomes, and clinical outcomes. Medians, as well as ranges wherever possible, were calculated for continuous variables. Number and percentages were calculated for categorical data. Observations were censored for all time-to-event analyses. We performed all statistical analyses using Excel (Microsoft, Redmond, Washington) and Stata (StataCorp LP, College Station, Texas).
Results
Patient Demographic and Disease Characteristics
Patient demographic and disease characteristics are depicted in Table 1 . Sixty-four patients met criteria for inclusion in this study. Fifty-three (83%) patients were men. At least 38 (59%) patients were of ethnic minorities, predominantly Asian and African American. Thirty-one (48%) patients were either uninsured or held low-income health insurance (Healthy San Francisco or Medi-Cal). There was a high prevalence of documented housing instability (n = 15, 24%), smoking (n = 54, 84%), alcohol abuse (n = 27, 42%), and other drug abuse (n = 19, 30%). Fifty (78%) patients had a Charlson comorbidity index greater than or equal to 3. 4
Patient and Disease Characteristics.
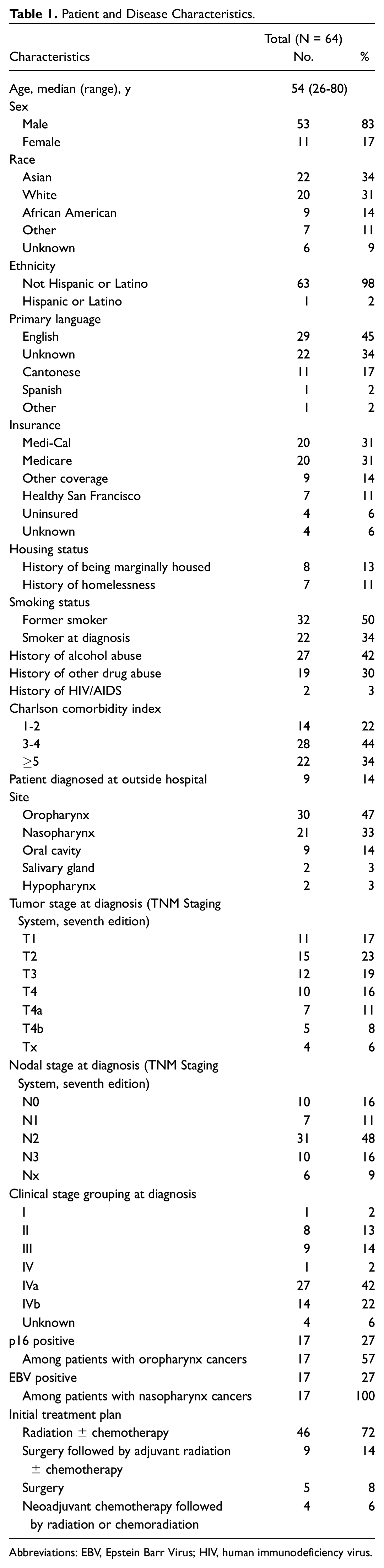

Abbreviations: EBV, Epstein Barr Virus; HIV, human immunodeficiency virus.
Most tumors were located in the oropharynx (n = 30, 47%), nasopharynx (n = 21, 33%), and oral cavity (n = 9, 14%). Of the oropharyngeal tumors, 57% tested positive for p16. It should be noted, however, that during this time period at our institution, not all oropharyngeal tumors were routinely tested for p16. Fifty-one (80%) patients presented with stage III or stage IV disease. The majority of patients underwent radiation ± chemotherapy (n = 46, 72%), while a smaller number had surgery followed by adjuvant radiation ± chemotherapy (n = 9, 14%), surgery alone (n = 5, 8%), or neoadjuvant chemotherapy followed by radiation or chemoradiation (n = 4, 6%).
Median follow-up time, defined as the time from diagnosis to last attended otolaryngology clinic visit, was 2.6 years (range, 19 days to 8.1 years).
Pretreatment and Treatment Measures
We performed censoring for all time-to-event analyses. Among all patients, the median diagnosis to treatment initiation interval (DTI) was 57 days. This was most prolonged in patients undergoing definitive radiation ± chemotherapy (median, 65 days). DTI was shorter in patients undergoing surgery followed by adjuvant radiation ± chemotherapy (median, 49 days), patients undergoing surgery alone (median, 54 days), and patients undergoing neoadjuvant chemotherapy followed by radiation or chemoradiation (median, 29 days). For patients who required pretreatment dental extraction, the median diagnosis to dental extraction interval was 62 days. Forty-four (69%) patients studied completed treatment ( Table 2 ). Eleven patients failed to start treatment. Treatment completion status of 1 patient could not be ascertained due to incomplete information in the chart.
Pretreatment and Treatment Measures.
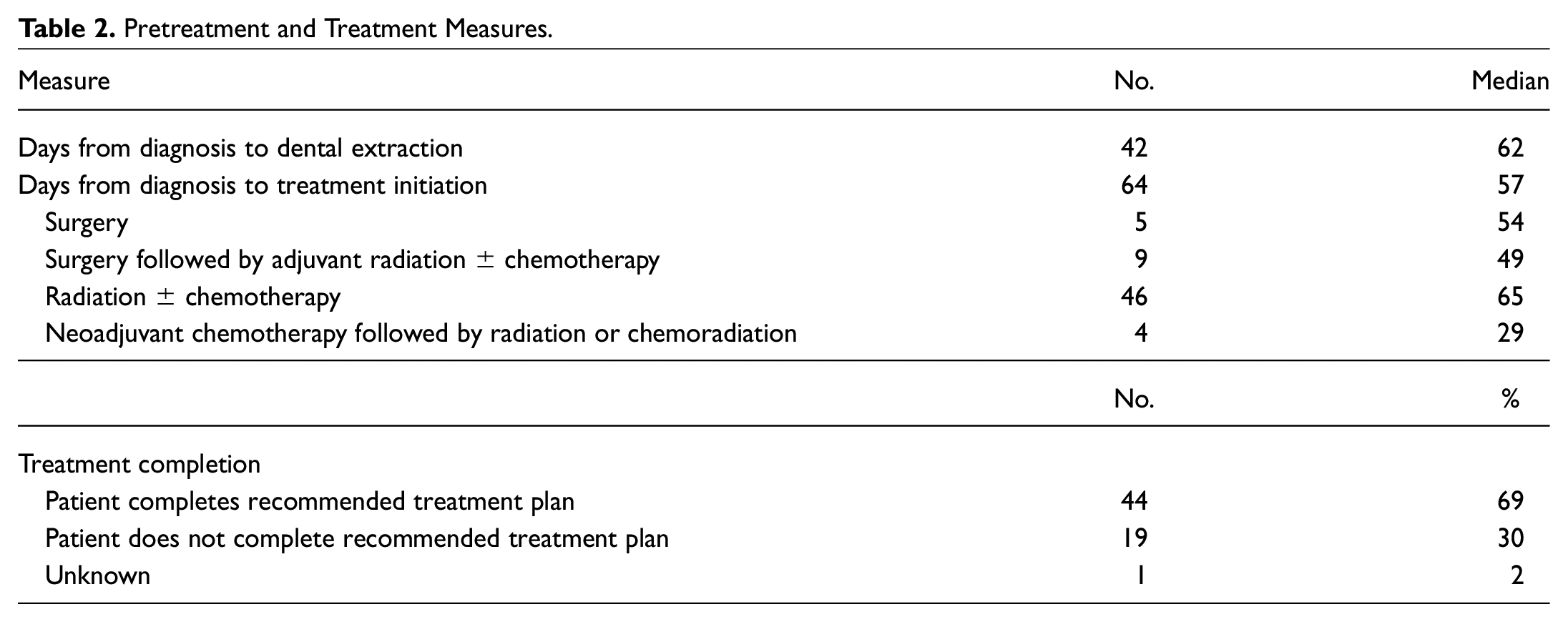
Fifty-five patients were recommended a treatment plan involving either primary or adjuvant radiation ( Table 3 ). The median radiation treatment length for all patients was 49 days (range, 2-67). Eighty-two percent and 80% of patients received the recommended dose and number of fractions of radiation, respectively.
Adherence to Tumor Board Treatment Recommendations for Radiotherapy.

Adherence to Posttreatment Surveillance
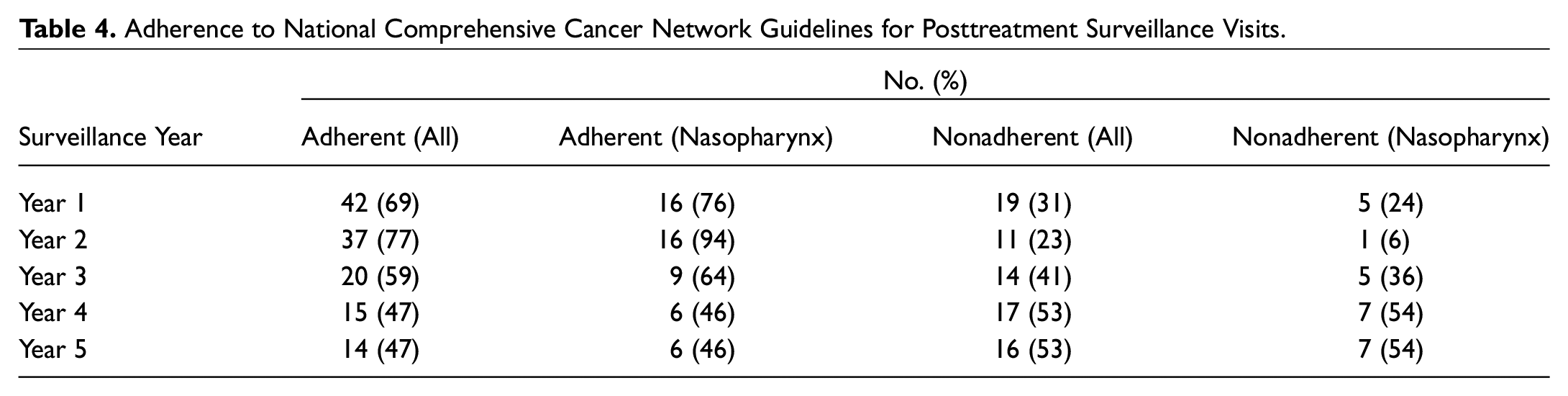
Table 4 displays adherence to posttreatment surveillance during the first 5 years after treatment completion. We defined adherence according to the National Comprehensive Cancer Network (NCCN) guidelines as follows for each year after treatment: at least 4 visits attended in year 1, at least 2 visits attended in year 2, and at least 1.5 visits attended annually in years 3 through 5. 5 Given anecdotally increased adherence to surveillance among patients with nasopharyngeal cancer, we examined this group of patients separately. For all cancers, we observed a decline in adherence as the surveillance period progressed. We observed a higher adherence in patients with nasopharyngeal cancers in years 1 through 3 of surveillance, which was no longer seen in years 4 and 5.
Adherence to National Comprehensive Cancer Network Guidelines for Posttreatment Surveillance Visits.
Clinical Outcomes
Twenty-eight (44%) patients died during the study period ( Table 5 ). Of these 28 deaths, 16 (57%) were attributable to HNC. Median time to death was 2.5 years (interquartile range, 1.2-6.0). One- and 2-year survival were 83% and 69%, respectively. Eight (13%) patients developed 1 recurrence, and 3 (5%) patients developed a second recurrence. Four (6%) patients developed a second primary cancer.
Clinical Outcomes (N = 64).
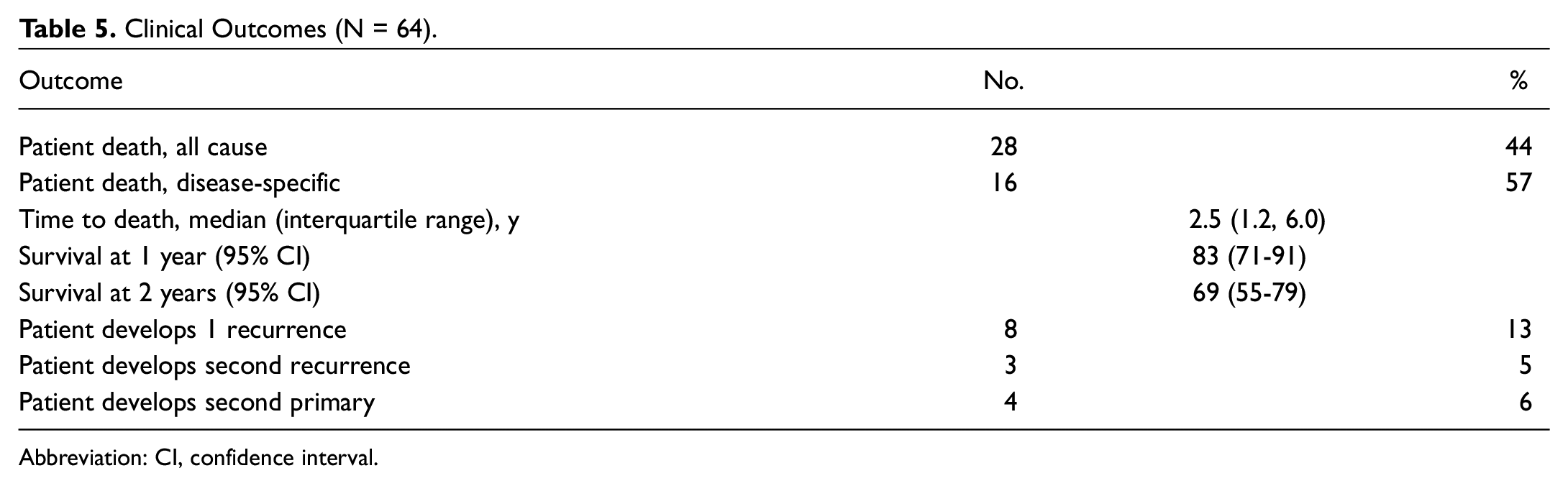

Abbreviation: CI, confidence interval.
Discussion
Our findings demonstrate that safety-net health systems need to be prepared to address a more socially and medically challenging population during and after HNC treatment compared to health systems that care for more advantaged populations. This patient population had a high prevalence of behavioral factors associated with poor HNC outcomes, such as tobacco use, alcohol and other substance abuse, and homelessness. Prior studies have demonstrated that these are risk factors for poor HNC outcomes. 2 This cohort also demonstrated a significant burden of medical comorbidities that can interfere with treatment completion and ability to adhere to posttreatment surveillance. With regard to disease characteristics, a greater proportion of patients in this population presented with advanced disease compared to national data. A 2009 National Cancer Database update reported a 42% prevalence of stage III and IV disease, whereas 80% of patients in this study presented with stage III and IV disease. 6
This study found a median DTI of 57 days among all patients. This is persistently prolonged compared to earlier studies conducted among similar populations. A study by Patel and Brennan 7 found a DTI of 48 days among 150 patients treated for HNC at John H. Stroger Cook County Hospital, an urban tertiary care public hospital in Chicago. A study among patients with oropharynx and nasopharynx cancer at the Zuckerberg San Francisco General Hospital and Trauma center, the same institution in our current study, found a DTI that ranged from 56 to 70 days depending on the tumor site. 8 A prolonged DTI has been shown to adversely affect survival—in a study of over 50,000 patients with HNC, a DTI of 61 to 90 days vs less than 30 days independently increased mortality risk on multivariate analysis. 9 This is especially relevant among a patient population in whom advanced stage at presentation, behavioral factors, and burden of medical comorbidities already limit the success of treatment.
Similar to previous studies, DTI in this study was most prolonged among patients treated with definitive radiation therapy. 7 This is not surprising given the high level of care coordination required for patients undergoing definitive radiation for advanced cancer, which often involves multidisciplinary discussion between the otolaryngologist, radiation oncologist, oral and maxillofacial surgeon, and medical oncologist in a tumor board forum. A health information technology tool may be able to play a role in facilitating such multidisciplinary care coordination in a more timely fashion. The time from diagnosis to dental extraction was also observed to contribute substantially to DTI. This underscores the importance of expediting dental evaluation and extraction to decrease DTI. Given that untreated dental disease is more prevalent in racial/ethnic minorities and low-income patients, providing access to timely dental care is of particular importance in this population. 10
Interestingly, radiation adherence in this study compared favorably to previously published measures among similar populations. In a study by Patel et al 11 conducted at Stroger Hospital, 59% of patients undergoing radiation therapy received less than the effective dose of 65 Gray. In the present study, 82% and 80% of patients received the recommended dose and number of fractions of radiation, respectively. Institutional differences may account in part for this disparity. Most notably, patients in this study received their radiation treatment at a nearby affiliated academic tertiary care medical center. Nonetheless, the ability of this vulnerable population to achieve a relatively high radiation adherence warrants consideration of how support services may be adapted in a low-income setting to achieve favorable outcomes.
To our knowledge, this is the first study to investigate adherence to posttreatment surveillance in a safety-net population. At present, there are limited studies examining the impact of posttreatment surveillance on survival in HNC. One study by Deutschmann et al 12 demonstrated that adherence to posttreatment surveillance affected survival in HNC. However, other studies have suggested that routine surveillance may not contribute to a survival benefit.13,14 Nonetheless, surveillance visits are important in screening for and managing the complications of HNC treatment, as well as encouraging cessation of tobacco and alcohol. As such, adherence to a posttreatment surveillance schedule is currently acknowledged as a standard of care in HNC. 5 Adherence to surveillance visits may be especially difficult to achieve in a safety-net population. In this study, adherence was highest in the first 2 years of surveillance and declined as the surveillance period progressed. This may require more intensive tracking and follow-up with patients in later years. Posttreatment surveillance adherence was analyzed separately for nasopharyngeal cancer given anecdotally noted higher adherence among this population. Higher adherence to surveillance was noted in patients with nasopharyngeal cancer during the early surveillance period, which was no longer seen in later years.
This study has several limitations. As a retrospective chart review, this study is inherently prone to a number of biases. The median follow-up period was short at 2.6 years, which highlights the high rate of loss to follow-up in this population that struggles with substance use, housing instability, and medical comorbidities. In addition, particular institutional differences may limit generalization to other urban tertiary care public hospitals, although other hospitals serving a safety-net population likely face similar challenges. Future studies will be required to investigate patient- and system-related factors that contribute to treatment delays and poor adherence to posttreatment surveillance, as well as to elucidate how these gaps in care affect clinical outcomes.
Conclusion
This study characterized treatment delays and adherence with posttreatment surveillance that occur in HNC care delivered at an urban tertiary care public hospital in San Francisco. DTI was prolonged in this study, comparable to earlier studies conducted among patients with HNC in other public hospital settings. Adherence to radiation therapy compared favorably to previously published measures. Adherence to posttreatment surveillance was poor and continued to decline as the surveillance period progressed. Further study is needed to identify factors associated with delays and poor adherence, as well as associated clinical outcomes.
Author Contributions
Disclosures
Footnotes
Acknowledgements
We thank Dr Sue Yom and Dr Shane Lloyd from the UCSF Department of Radiation Oncology, as well as UCSF Academic Research Services, for their help collecting data.
Sponsorships or competing interests that may be relevant to content are disclosed at the end of this article.
