Abstract

Syphilis is a sexually transmitted infection caused by the bacterium Treponema pallidum. Despite increased public campaigns for safer sexual practices, infection rates in the United States have shown a steady incline since 2000. 1 The clinical presentation of syphilis varies with stage of infection, transitioning from local lesions to more systemic symptoms. Due to the transient and inconsistent nature of its manifestations, diagnosis may be challenging, requiring synthesis of clinical, laboratory, and pathological findings.
The following case report describes a unique presentation of a syphilic ulcer masquerading as a head and neck malignancy with confounding clinical and pathological findings contributing to the difficult diagnosis.
Case Report
The patient was a 41-year-old man who emigrated from the Philippines 15 years ago. He had no significant medical history except for tonsillectomy. His social history included little alcohol consumption and no tobacco use. He is homosexual and reported oral sexual activity but no anal intercourse.
Initially, he presented to his primary care physician for a wellness exam with a sole complaint of sore throat. On physical exam, a large 3.0-cm × 1.0-cm ulcerated mass located on the posterior pharyngeal wall was identified ( Figure 1 ), and the patient was subsequently referred to a head and neck surgeon for evaluation. A biopsy of the mass was taken during laryngoscopy but was inadequate for histopathologic evaluation as it was largely necrotic. Due to this nondiagnostic material, positron emission tomography (PET)–computed tomography (CT) was performed, which showed bilateral hypermetabolic cervical lymphadenopathy and an intensely hypermetabolic mass in the right tonsillar region, concerning for malignancy. Given the patient’s demographics and location of the lesion, nasopharyngeal carcinoma and lymphoma were favored. Repeat biopsy was performed demonstrating reactive lymphoid tissue but no evidence of malignancy. Of note, scattered Epstein-Barr virus (EBV)–positive cells were observed in the tissue. Workup for potential infectious etiology was initiated with tissue culture and serology confirming EBV positivity. Rapid plasma regain (RPR) and subsequent fluorescent treponemal antibody absorption (FTA-ABS) test results were also reactive. Follow-up T pallidum immunostaining of the tissue highlighted a robust population of spirochetes ( Figure 2 ), consistent with the clinical diagnosis of syphilis.
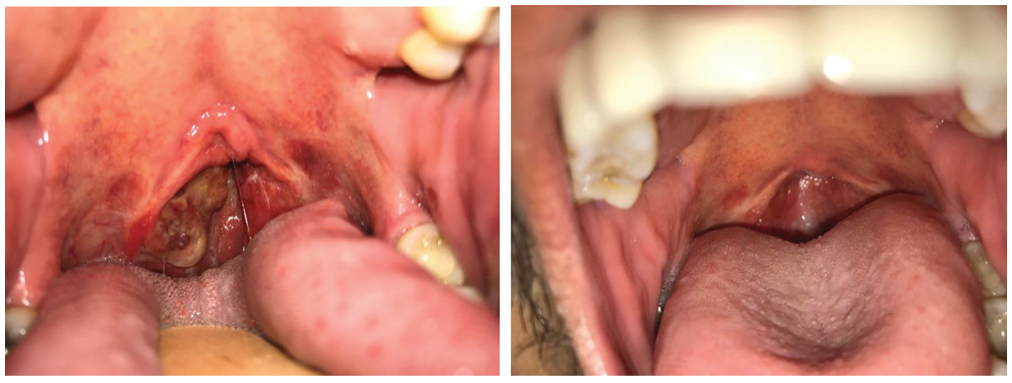
Gross photographs. Left, retropharyngeal mass on presentation. Note the exophytic and ulcerated appearance. Right, resolution of mass after treatment with penicillin.
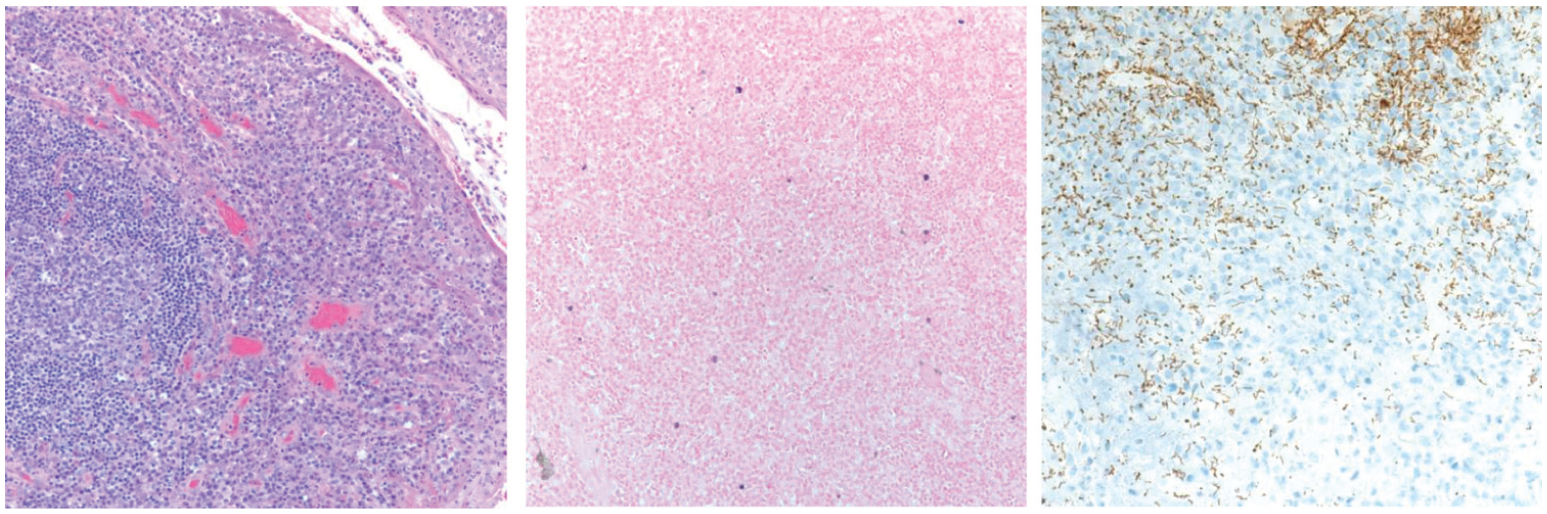
Histopathology. Left, hematoxylin and eosin–stained tissue demonstrating an intact lymphoepithelial architecture. Middle, scattered Epstein-Barr virus (EBV)–positive cells by in situ hybridization. Right, Treponema pallidum immunostain highlighting the characteristic corkscrew-shaped spirochetes.
Although the patient exhibited good clinical response with penicillin, concern for a simultaneous malignancy persisted. A follow-up fine-needle aspiration of the regressing lymphadenopathy showed no evidence of malignancy, confirming a purely infectious etiology of the mass.
Discussion
Oral involvement can be seen in all stages of syphilis, with lesions more commonly observed in patients with secondary disease. 2 As it is extremely rare for oral ulceration to be the sole manifestation of secondary syphilis, our patient most likely presented before disseminated disease developed. The chancre of primary syphilis appears at the site of inoculation and, therefore, is most often found on the genital and perianal regions. However, extragenital lesions can be seen in up to 31% of patients, the majority located on the mouth and lips. 3 Regardless of the patient’s elicited sexual history, an oropharyngeal chancre is still quite rare. Several case reports have documented the existence of these lesions but are described as “well-demarcated, grey-white plaque with central ulceration.” 4 This appearance is consistent with the typical chancre and grossly contrasts our patient’s polypoid and exophytic mass. The unusual gross appearance and location of this lesion in addition to the concerning imaging studies would favor a malignant over an infectious process. The patient’s demographics as a young Asian man also raises suspicion for nasopharyngeal carcinoma, which is more prevalent in that population. Although the histologic presence of dense lymphoplasmacytic infiltrate is characteristic of syphilis, the scattered EBV positivity further complicated a definitive diagnosis. Studies have shown a strong association between EBV and the development of both nasopharyngeal carcinoma and hematologic malignancies, such as extranodal NK/T-cell lymphoma, nasal type, Burkitt’s and Hodgkin’s lymphoma. 5
Crucial in elucidating this case were the positive laboratory results, improvement with antibiotics, and corroborating immunohistochemical stain highlighting T pallidum. While a synchronous malignancy still cannot be excluded, close clinical follow-up has shown no further suspicious findings.
This case demonstrates an unconventional presentation of a primary chancre and the ancillary findings that complicated the diagnoses. In sharing our experience, we hope to increase awareness regarding the resurgence of syphilis as well as the potential features that may hinder an appropriate and timely diagnosis.
This article was exempt from review by the Office of Research Compliance and Quality Improvement at Cedars-Sinai Medical Center.
Author Contributions
Disclosures
Footnotes
No sponsorships or competing interests have been disclosed for this article.
