Abstract
Objectives
Frontal sinus anatomy is complex, and multiple variations of ethmoid pneumatization have been described that affect the frontal outflow tract. In addition, the lumen proper of the frontal sinus may exist as 2 separate parallel cavities that share an ipsilateral outflow tract. This variant has not been previously described and may have implications for surgical management.
Study Design
Case series.
Setting
Tertiary rhinology practice.
Subjects and Methods
Cases with radiographic and intraoperative findings of separate parallel tracts within a unilateral frontal sinus were identified from a consecutive series of 186 patients who underwent endoscopic sinus surgery between May 2015 and July 2016. Data were recorded including sinusitis phenotype, coexisting frontal cells, and extent of surgery.
Results
Ten patients (5.4%) were identified with computed tomography scans demonstrating bifurcation of the frontal sinus into distinct medial and lateral lumens. All cases were treated with Draf 2a or 2b frontal sinusotomy with partial removal of the common wall to create a unified ipsilateral frontal ostium. Eleven sides had a coexisting ipsilateral agger nasi cell, 7 had a supra-agger cell, 8 had a suprabullar cell, and 1 had a frontal septal cell. There were no significant complications.
Conclusion
The bifurcated frontal sinus is an anatomic variant that the surgeon should recognize to optimize surgical outcomes. Failure to do so may result in incomplete clearance of the sinus and residual disease. The bifurcated sinus may occur with other types of frontal sinus cells and may be safely treated with endoscopic techniques.
The anatomy of the frontal sinus outflow tract (FSOT) is complex and poses a challenge to the endoscopic surgeon. Anatomic variations of the anterior ethmoid region may include several pneumatization patterns that displace the FSOT or encroach into the frontal sinus lumen.1-3 Failure to recognize and address these variants during endoscopic sinus surgery (ESS) can result in postoperative sinus obstruction and subsequent iatrogenic frontal sinus disease.1,4 Features of the most common FSOT anatomic variants have been recently described in the publication of the International Frontal Sinus Anatomy Classification. 2 These variants include supra-agger cells, suprabullar cells, supraorbital cells, and frontal septal cells. On the basis of this classification system, each of these variations has an implication for the surgical approach and the extent of surgery.
In addition to variations of the FSOT, the lumen of the frontal sinus can display a widely varied morphology. Studies of pneumatization have shown that the sinus may encompass the entire frontal bone and may extend far laterally over the orbit.2,3,5 Similarly, the sinuses may be asymmetric with 1 dominant frontal sinus crossing the midline.6,7 In addition, a single frontal sinus may consist of 2 individual compartments of approximately equal size, each with a distinct ostium within the frontal recess. We present a description of this distinct variant of frontal sinus anatomy along with recommendations for surgical management.
Patients and Methods
A case series with planned data collection was compiled from all surgical cases performed by a single surgeon at a tertiary rhinology practice between May 2015 and July 2016. All patients had preoperative computed tomography of the paranasal sinuses and preoperative nasal endoscopy. ESS was performed under general anesthesia using intraoperative image-guided navigation. Postoperative examination with nasal endoscopy was performed after each case, and patients were followed up to 12 months after surgery. Recorded data included sinusitis phenotype, coexisting frontal cells, extent of surgery, and complications. Cases without a bifurcated frontal sinus were used for comparison of radiologic findings. This study was approved by the institutional review board of Ochsner Clinic Foundation.
Results
A total of 186 patients representing 372 individual sides received ESS during the study period, of which 10 were found to have a bifurcated frontal sinus, resulting in a prevalence of 5.4% among patients and 3.2% among sides. There were 6 male and 4 female patients, with a mean age of 44.9 years (range, 25-67). Unilateral bifurcation was present in 8 patients and bilateral in 2 patients, for a total of 12 sides with a bifurcated sinus ( Figure 1 ). One patient had a diagnosis of cystic fibrosis, and polyposis was present in an additional 5 cases. The clinical presentation of cases with a bifurcated frontal sinus did not suggest any unique or distinguishing features, and mucosal disease was noted in both lumens without predilection. Ipsilateral FSOT variations were present as follows: 11 agger nasi cells, 7 supra-agger cells, 8 suprabullar cells, and 1 frontal septal cell. A similar frequency of FSOT variations was observed in the remaining 176 patients (352 sides) without a bifurcated frontal sinus, as presented in Table 1 .
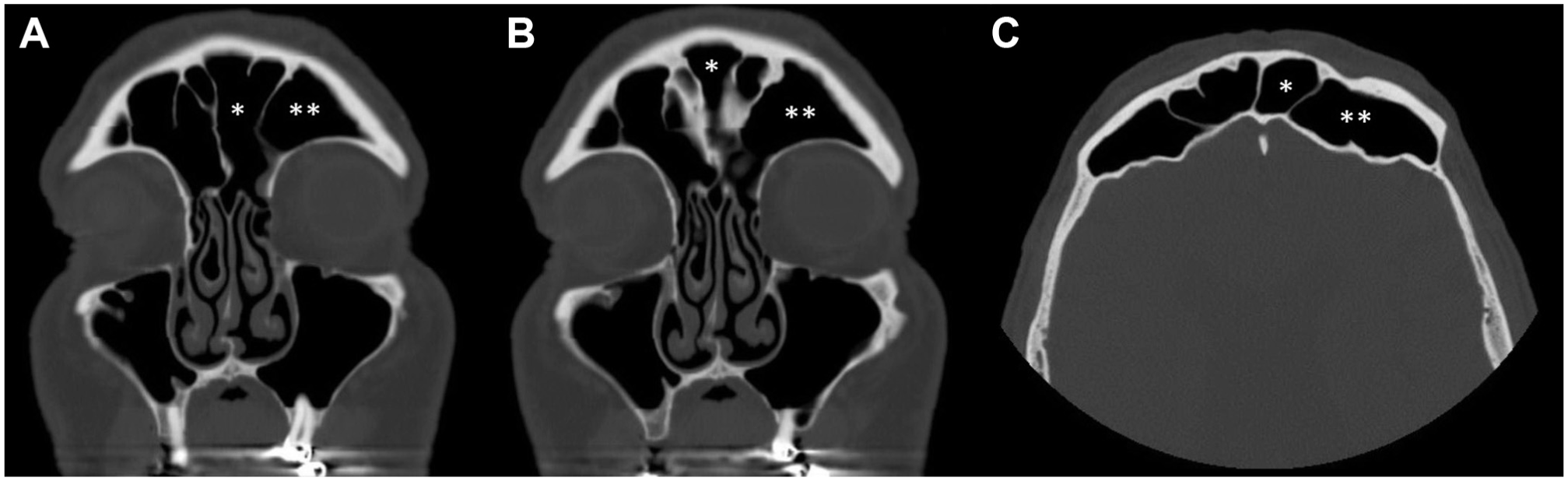
Computed tomography imaging in the axial (A, B) and coronal planes (C) of a patient with bilateral bifurcated frontal sinuses. Asterisks indicate the medial (*) and lateral (**) lumens of the left frontal sinus, each of which extends from the level of the frontal ostium to the superior extent of the frontal bone.
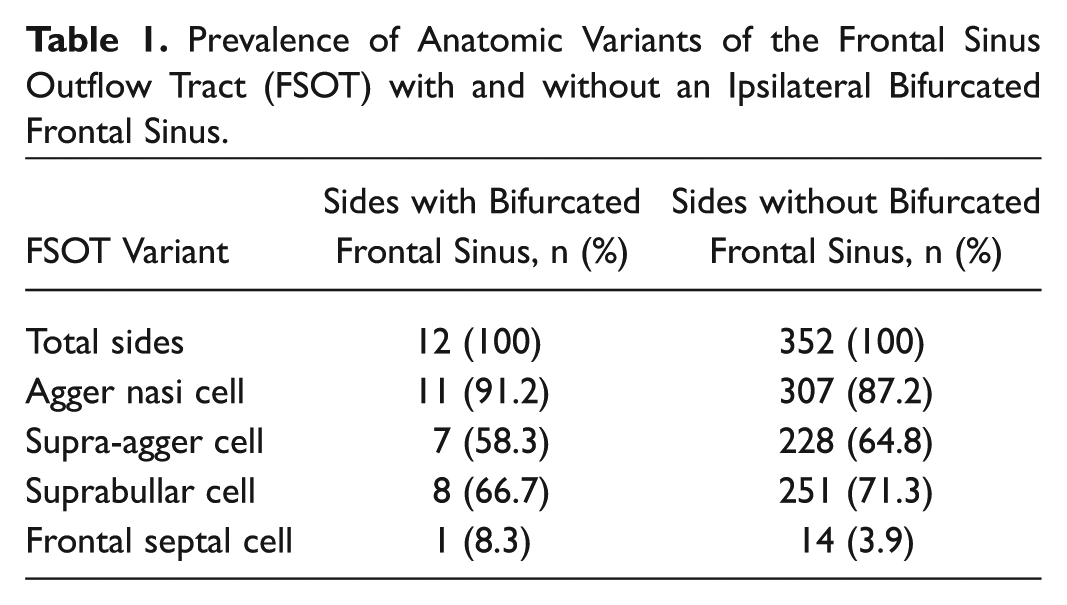
Prevalence of Anatomic Variants of the Frontal Sinus Outflow Tract (FSOT) with and without an Ipsilateral Bifurcated Frontal Sinus.
All patients underwent anterior ethmoidectomy and frontal sinusotomy, with either a Draf 2a (8 cases) or Draf 2b (2 cases) procedure. Intraoperatively, after removal of the bulla ethmoidalis, uncinate process, agger nasi cell, and superior ethmoid cells, parallel ostia characteristically appeared side by side at the level of the frontal beak, as confirmed by image guidance. The inferior portion of the common wall was then removed with 70° angled upward-cutting punches, to create a unified outflow tract. The common ostium was then enlarged in an axial plane using a Hosemann punch or similar instruments. Frontal sinus stenting was not used.
Postoperative care included routine debridement and topical steroids that initially consisted of high-volume budesonide-containing saline rinse. Subsequent nasal endoscopy at 3 months postoperatively typically demonstrated a well-mucosalized common FSOT with parallel distal lumens, which remained separated superiorly by a common wall ( Figure 2 ). No intraoperative or postoperative complications were encountered.
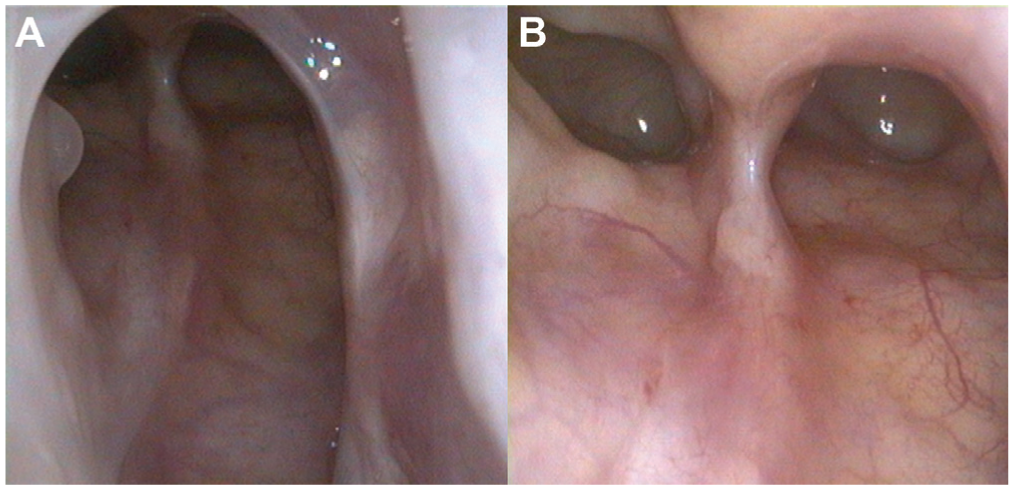
Endoscopic 70° view of a left-sided bifurcated frontal sinus 12 months after endoscopic sinus surgery. A common frontal ostium is well mucosalized inferiorly (A), while superiorly, the 2 parallel lumens remain partially divided by a common bony partition (B).
Discussion
The frontal sinus can pose a therapeutic challenge because of the intricate anatomy of the FSOT and the acute angle of approach relative to the nasal cavity. 2 In addition to variations produced by so-called “frontal cells” that extend from the ethmoid labyrinth, variations of the frontal sinus lumen may also be present, as described in this report. The presence of a bifurcated frontal sinus, in which 2 parallel lumens of relatively equal size are present, has important implications for the surgical approach. In particular, the surgeon must be certain to identify each of the ostia and ensure both that they are sufficiently patent and that the FSOT is confluent. Failure to identify and enlarge one of the ostia may risk postoperative stenosis and disease recurrence. Inadequate size of the frontal sinus ostium has been previously identified as the most significant risk factor for failure of frontal ESS. 8
The reasons for the presence of a bifurcated frontal sinus remain obscure. This variant may be seen in conjunction with several types of frontal cells, occurs in men and women, and may or may not give rise to mucosal polyposis. We encountered a prevalence of 5.4% among patients in the present series; in comparison, agger nasi and frontal cells have been reported in 78% to 98%6,7,9-11 and 20% to 33%11,12 of patients, respectively. One etiologic theory is that the more medial lumen arises as a frontal septal cell during ethmoid pneumatization. However, the aforementioned frontal septal cell, as recently described, is quite small when compared with the adjacent dominant frontal lumen. 2 By comparison, the cases in the present series each had 2 lumens of similar size, each with a distinct ostium. Whereas a small frontal septal cell may be clinically inconsequential, and therefore harmlessly neglected, the presence of similarly-sized medial and lateral lumens at the FSOT effectively doubles the mucosal surface that would be affected by frontal sinusitis. Therefore, each lumen with mucosal disease should be treated similarly, and addressing both components of the bifurcation is necessary to complete a frontal sinusotomy.
Although the extent of dissection within the frontal lumen is not accounted for in the Draf classification, fully addressing the bifurcation requires at least a Draf 2 procedure. In a Draf 2a procedure, the frontal sinus ostium is enlarged with preservation of the middle turbinate, whereas in a Draf 2b procedure, the entire frontal sinus floor is removed between the orbit and the septum, which necessitates resection of the anterior attachment of the middle turbinate. In cases of recalcitrant polyposis or hyperostosis, a Draf 3 procedure may be considered, in which a superior nasal septectomy is performed and the floor of both frontal sinuses is removed to unify the bilateral frontal sinus lumens. However, in the present series, a Draf 3 procedure was not required to address a unilateral bifurcated sinus.
The lateral lumen of a bifurcated frontal sinus can be differentiated from a supraorbital ethmoidal cell by its relation to the anterior ethmoidal artery (AEA). A true frontal sinus shares a posterior wall with the suprabullar recess or a suprabullar cell; in turn, the AEA resides in the coronal plane of the posterior wall of the suprabullar cell. 2 A supraorbital cell characteristically occurs at this location adjacent to the AEA, whereas a true frontal sinus lumen is separated from the AEA by 1 or more additional ethmoid cells.
We found intraoperative image guidance to be an indispensable adjunct to ensure identification and complete dissection in each of these cases. This was particularly true when one of the bifurcated ostia was not readily apparent, and an educated guess on the part of the surgeon would have been needed to decide whether the apparent ostium was the medial or lateral tract. Once both lumens were confirmed, we found that standard frontal surgical instruments were adequate for most cases with only occasional use of a high-speed drill. Routine stenting was not required in any case.
The present study is limited by the case series design and the single-institution setting. Although the prevalence of a bifurcated frontal sinus and FSOT variants described in this report are representative of a surgical cohort in a tertiary rhinology practice, it is possible that prevalence may differ among patients without chronic sinusitis requiring surgical management. Further study may examine the relationship between pneumatization of the frontal sinus and the development of clinically significant sinus disease. The effect of preferential treatment of specific sinuses, including a single lumen of a bifurcated sinus or other FSOT variations, on patient-reported outcomes may also be the subject of future study.
Conclusion
The bifurcated frontal sinus is an important anatomic variant that may coexist with other FSOT variations. The bifurcated sinus can be safely managed with endoscopic techniques. Intraoperative image guidance is beneficial to ensure that both lumens are identified and adequately addressed during surgery.
Author Contributions
Disclosures
Footnotes
Sponsorships or competing interests that may be relevant to content are disclosed at the end of this article.
