Abstract

Intravascular papillary endothelial hyperplasia (IPEH), also known as Masson’s tumor, is a benign vascular lesion that was first described in 1923. It is characterized by exuberant endothelial cell proliferation and papillary formation within normal blood vessels and vascular malformations, often associated with thrombi. IPEH typically presents in the extremities, trunk, or head and neck within the skin and subcutaneous tissues. While there are several reports of IPEH within the oral mucosa, cases involving the neck are comparatively rare. We present a case of IPEH of the neck and discuss the clinical features and management of this lesion.
Case Report
A 53-year-old woman was referred to our department for an anterior neck mass. Prior to presentation, she underwent fine-needle aspiration (FNA) biopsy, ultrasound, and computed tomography scanning after the mass did not resolve with antibiotics. Ultrasonography and computed tomography scan were notable for a hypervascular solid mass measuring 3 × 2.5 × 1 cm anterior to the sternocleidomastoid muscle with a large inferior feeding vessel ( Figure 1 ). The outside biopsy demonstrated spindled epithelioid cells in a background of blood and was consistent with a benign vascular lesion. The patient was then seen at our institution.
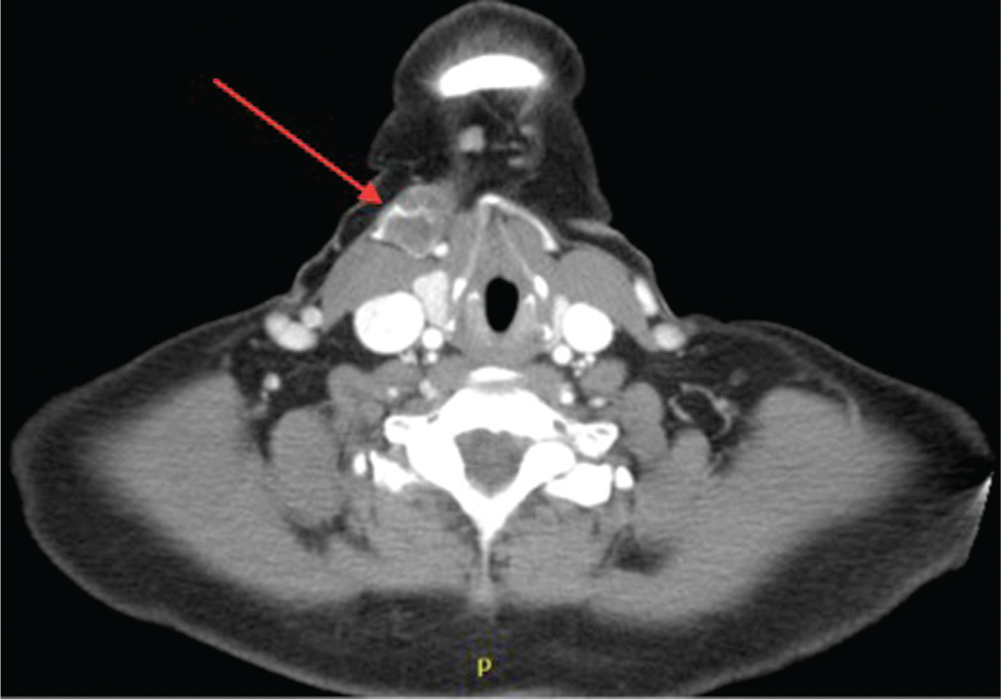
Large vascular lesion (arrow) of the neck with dilated vessels and heterogeneous and multiloculated appearance on computed tomography.
At our initial evaluation, the patient noted mild enlargement of the mass and discomfort following biopsy. She denied prior neck trauma and surgery, as well as voice, breathing, and swallowing changes. Her examination was significant for a mobile right neck mass without adherence to underlying tissues. There was no palpable lymphadenopathy or changes in the overlying skin. Flexible endoscopy demonstrated bilaterally mobile true vocal cords. The remainder of her examination yielded negative findings for other head and neck lesions.
Imaging and pathology were reviewed with the patient, and excision for definitive diagnosis and treatment was recommended. Intraoperatively, the mass was noted to be superficial to the platysma, bluish in color, well encapsulated, and hypervascular, with multiple feeding blood vessels and a large amount of clot within the capsule. All feeding vessels were ligated; the mass was completely excised and sent for routine pathologic evaluation.
At 2 weeks postoperatively, the patient was noted to have a small seroma, which was drained in office. She otherwise did well without recurrence of the lesion. Final pathology showed a 3-cm mass containing intravascular papillary endothelial hyperplasia consistent with IPEH ( Figure 2 ).
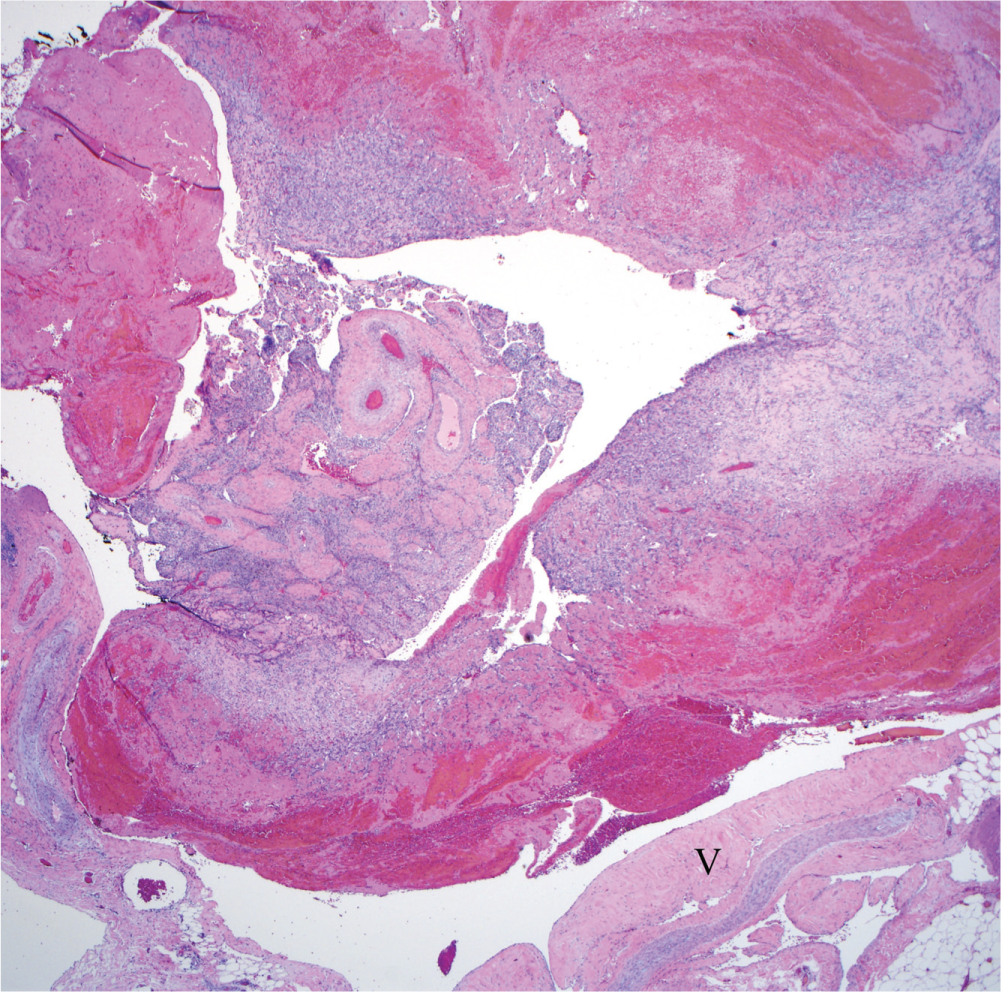
The intravascular endothelial proliferation is associated with an organizing thrombus and contains an intravascular arborizing vessel proliferation from the intimal wall of the vein (hematoxylin and eosin, ×40).
Discussion
IPEH occurs predominantly in the dermis and subcutaneous tissues of the head and neck and extremities, typically within the fifth decade of life, and has a slightly higher incidence among females. 1 The pathogenesis of IPEH remains poorly understood, and several mechanisms have been postulated. It is thought to be a benign neoplastic process involving proliferation of endothelial cells within vessel lumens, which subsequently undergo degeneration and necrosis. Alternatively, it may arise from thrombi or blood stasis with associated perivascular inflammation. 1
IPEH is categorized into 3 subtypes: type 1 (pure form) is the most common and occurs within dilated vascular spaces; type 2 (mixed form) develops in preexisting lesions; and type 3 (undermined type) is the least common and develops within traumatic hematomas. Despite multiple reports of IPEH within the oral cavity mucosa, there are <10 reported cases of IPEH within the lateral neck. 2
Though benign, IPEH may be difficult to distinguish from malignant tumors, owing to its appearance on imaging and its relative rarity. IPEH consistently demonstrates peripheral enhancement with central heterogeneity, 3 which may help differentiate it from other lesions. However, imaging alone is insufficient to diagnosis IPEH, which requires histologic analysis for confirmation.
Unfortunately, IPEH shares similarities with angiosarcoma that may be distinguished only microscopically. Histologically, IPEH is a well-encapsulated lesion with papillary fronds limited to intravascular spaces. 4 Necrosis, nuclear atypia, and atypical mitotic figures are uncommon. There are no irregular blood vessels or invasion of extravascular tissues. In contrast, angiosarcoma demonstrates abnormal endothelial cells, infiltrative vascular channels, and pleomorphic nuclei.
Another factor complicating accurate preoperative diagnosis of IPEH is the inadequacy of FNA cytologic analysis. IPEH may be mistaken for angiosarcoma and other malignancies, such as adenocarcinoma or adenoid cystic carcinoma, based on cytomorphologic features alone. FNA cytology has successfully diagnosed IPEH preoperatively in only 1 reported case. 5 In our patient, preoperative FNA confirmed the presence of a benign lesion; however, surgical excision was needed for definitive diagnosis, emphasizing surgical intervention as both a diagnostic and a therapeutic modality. Prognosis is excellent, and recurrence is rare, typically occurring only in the event of incomplete primary resection.
This article was exempt from review by the Institutional Review Board for Human Research at the Medical University of South Carolina.
Footnotes
No sponsorships or competing interests have been disclosed for this article.
